COVID-19: Symptoms, course of illness and use of clinical scoring systems for the first 42 patients admitted to a Norwegian local hospital
Main findings
Fever, reduced general condition, dyspnoea and cough were the most common symptoms among patients admitted to our hospital with COVID-19, and most patients had symptoms for at least one week before hospitalisation.
One of five patients had a critical course of illness.
Eight of nine patients with a critical course had a NEWS2 score of ≥ 5 on admission, while few patients in this group scored ≥ 2 on CRB-65 or qSOFA.
COVID-19 (coronavirus disease 2019) is caused by infection with the virus SARS-CoV-2 (severe acute respiratory syndrome coronavirus 2), which belongs to the coronavirus family. The first case among humans very probably arose at the beginning of December 2019 at a food market in Wuhan in Hubei province, China (1). The ability of the virus to spread rapidly became evident during the first part of the outbreak, when it spread from one city to much of China in 30 days (2). Within a short period of time, COVID-19 has caused a pandemic with infected persons on all continents (3). The first case of COVID-19 in Norway was identified on 26 February 2020, and in the course of a short period we have observed a dramatic increase in cases both in Norway and in many other countries (3).
The disease picture for COVID-19 shows great variation – from an asymptomatic course or mild cold symptoms to acute respiratory distress syndrome and death. It is estimated that four out of five experience mild symptoms, but that up to 20 % will require hospitalisation (2). In reports published so far, the percentage with a critical course (requiring intensive care treatment or dying) has been about 15 % of hospitalised patients (4), but with local variations (5, 6).
The variation may be due to differences in age composition, morbidity, social factors and the criteria for hospitalisation in the populations surveyed. Differences in culture, social structure and the healthcare system across countries and regions probably also play an important part, and it is therefore necessary to describe patients admitted to Norwegian hospitals with COVID-19. To our knowledge, data on hospitalised Norwegian COVID-19 patients have not previously been systematically reported and published. Fever and respiratory tract symptoms occur frequently, but at present we know less about what symptoms, clinical parameters and findings may predict a poor prognosis (7).
Whereas clinical tools such as the quick Sepsis-related Organ Failure Assessment (qSOFA), CRB-65 and National Early Warning Score (NEWS) are established clinical tools for other groups of patients with infectious disease, so far little has been written about their usefulness for patients with COVID-19. We present patient characteristics, symptoms, examination findings and experience of use of clinical scoring systems on admission for the first patients admitted with COVID-19 at a Norwegian local hospital during the first few weeks of the outbreak.
Material and method
This observational clinical qualitative study was conducted at Bærum Hospital, Vestre Viken. Bærum Hospital is a local hospital for a population of about 190 000 inhabitants of Viken county (8). The purpose of the study was to systematically survey features such as age, comorbidity and frailty, symptoms and examination findings and the course of illness of patients admitted with COVID-19. All hospitalised patients diagnosed with COVID-19 infection before or during their stay in hospital were included successively in the study. COVID-19 was confirmed on qualitative detection of nucleic acid from SARS-CoV-2 in specimens of laryngeal and pharyngeal secretion using real time polymerase chain reaction (RT-PCR) (9).
When reviewing patients' medical records we registered age, sex, comorbidity and frailty prior to the present illness, laboratory findings, results of radiological scans, self-reported symptoms, vital signs, need for respiratory support, intensive care treatment and death while in hospital. Comorbidity was surveyed using the Charlson Comorbidity Index (CCI) (10). The tool gives points for age and chronic diseases such as cardiopulmonary disease, diabetes mellitus, dementia and malignant diseases. The CCI score has proved to predict mortality and has been validated on hospitalised patients (11). Frailty was assessed by means of the Clinical Frailty Scale (CFS). The tool can be used to assess the vulnerability and frailty of elderly people, on the basis of their mobility, cognitive function and need for help in daily activities 14 days prior to the onset of acute illness (12) and it has been proposed to use it as support for assessing the treatment level needed during the COVID-19 outbreak (13). CCI and CFS scores were assigned by the last author on the basis of data in the patient's records.
In addition, NEWS2, qSOFA, CRB-65 and Systemic Inflammatory Response Syndrome (SIRS) scores on admission were calculated on the basis of the first clinical examination after admission. NEWS2 scores and as a rule qSOFA scores were noted in the records. For the other clinical scoring systems and in cases of missing total scores, the last author calculated the total score using figures noted in patient records.
In NEWS2, the physiological parameters respiratory rate, peripheral oxygen saturation, systolic blood pressure, pulse rate, level of consciousness/confusion and temperature are given scores of 1–3 points. In addition, two points are given if the patient receives supplemental oxygen. A total score of ≥ 5 indicates severe acute illness (14). In qSOFA, one point is scored for respiratory rate ≥ 22/min, systolic blood pressure ≤ 100 mm Hg and altered mental status (Glasgow Coma Scale (GCS) score <15) (15). A qSOFA score of ≥ 2 may be a predictor of a poor prognosis for patients with infection (15). CRB-65 is used to assess illness severity and has been validated on persons hospitalised with pneumonia (16). New-onset confusion, respiratory rate ≥30/min, low blood pressure (systolic < 90 mm Hg or diastolic ≤ 60 mm Hg) and age ≥ 65 years score one point each. Patients with a score of ≥ 2 are most frequently in need of hospitalisation (17). We defined systemic inflammatory response syndrome (SIRS) as that at least two of four SIRS criteria should be met (temperature > 38 °C or < 36 °C, pulse rate > 90/min, respiratory rate > 20/min or hypocapnia with pCO2 < 4.3 kPa, leukocytes ≥ 12 · 109/l or < 4 · 109/l) (15).
Severe illness was defined as requiring hospitalisation. Critical illness was defined as treatment in the Intensive Care Department or death in hospital up to 31 March 2020.
Statistical methods
We registered all data with the aid of EpiData version 4.4.3.1 (The EpiData Association, Odense, Denmark). Continuous variables were presented as average, median and range, and categorical variables as number and percentage. Data were processed in SPSS version 25.0 (IBM, Armonk, NY, USA).
Ethics
This is an observational qualitative study without intervention. The study used data that are routinely registered during a hospital admission. The only possible drawback was that reviewing patient records compromises patient's privacy protection. We did not actively obtain written consent, but patients were given the right of reservation, in that they received a letter with information about the study on or after discharge. The main purpose of the study was to monitor and evaluate the hospital's handling of the patient group, but we see that experience from the first patients admitted to a Norwegian local hospital could be of interest beyond this particular hospital during the ongoing outbreak. The study and publication of results of the study were approved by the data protection official of the health trust (20/02772–1). We have made a conscious choice not to comment on mortality rates or number of deaths. This is because of the proximity to real time, the interests of protection of privacy and the uncertainty implicit in a limited dataset.
Results
The first patient found to have COVID-19 was hospitalised on 9 March 2020. By 31 March, 43 patients with COVID-19 had been admitted to the hospital, while 23 patients were discharged alive after spending an average of 7.5 days in the hospital (Fig. 1). One asymptomatic patient with detected COVID-19 was tested solely because of exposure and was excluded from the analysis.

Patient characteristics
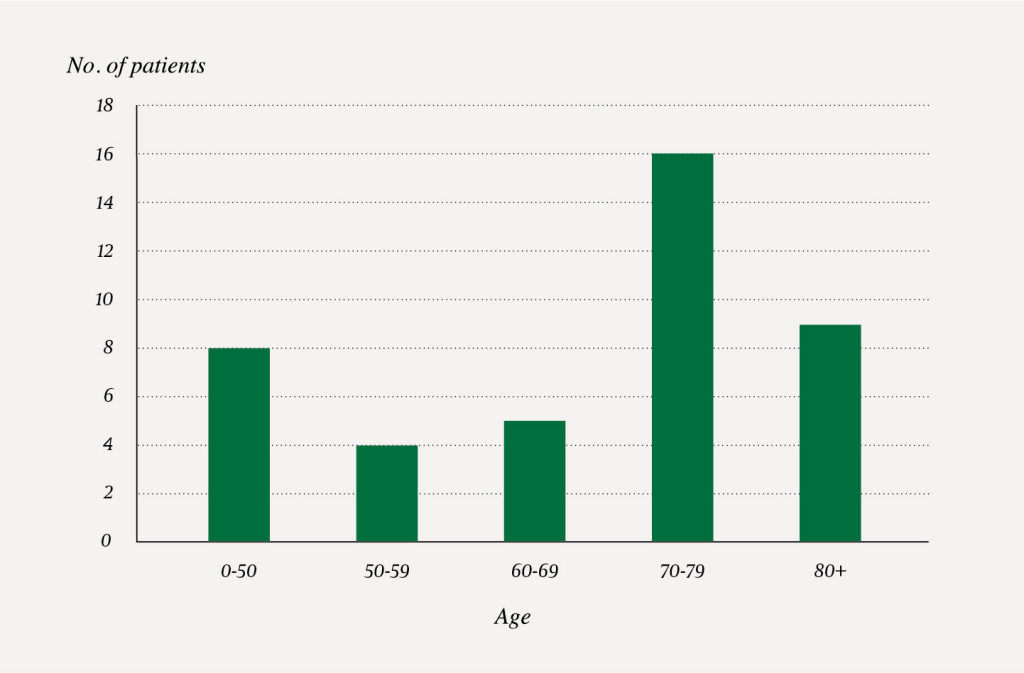
Table 1 and Figure 2 provide an overview of key characteristics of the patients. The median age was 72.5 years, and 28 of the patients were men. The majority of the patients were aged 70 or older and had good functional capacity. Nine patients were frail (CFS score ≥ 5). Diabetes mellitus was the most common comorbid condition (7 of 42 patients).
CFS = Clinical Frailty Scale, CCI = Charlson Comorbidity Index
Table 1
Characteristics of patients with detected COVID-19 infection admitted to Bærum Hospital in the period 9.3.2020–31.3.2020 (n = 42). Number (%) unless otherwise specified
| Variable |
Figures |
|
|---|---|---|
| Age (years) average (median, range) |
67.8 (72.5, 30–95) |
|
| Men |
28 (67) |
|
| CFS score, average (median, range) |
2.9 (2, 1–7) |
|
| CCI score, average (median, range) |
3.2 (3, 0–9) |
|
| CFS score ≥ 5 |
9 (21) |
|
| CCI score |
||
| 0–1 |
10 (24) |
|
| 2–4 |
22 (52) |
|
| ≥ 5 |
10 (24) |
|
| Diabetes mellitus |
7 (17) |
|
| Malignant disease |
6 (14) |
|
| Renal failure |
4 (10) |
|
| Chronic obstructive pulmonary disease |
3 (7) |
|
| Other1 |
7 (17) |
|
| Body mass index2 |
||
| < 20 |
3 (9) |
|
| ≥ 25 |
14 (44) |
|
| Smoking |
||
| Yes, currently |
2 (5) |
|
| Yes, previously |
9 (21) |
|
1Dementia, previous stroke, previous myocardial infarction or heart failure
2Data on height or weight were lacking for 10 patients
Symptoms and clinical findings
The median duration of symptoms prior to hospitalisation was seven days. Fever (79 %), reduced general condition (79 %), dyspnoea (69 %) and cough (67 %) were the most common symptoms reported by patients. Of 14 patients admitted with acute functional decline, falls or suspected stroke, three did not have fever, cough or dyspnoea.
A total of 17 patients had systemic inflammatory response syndrome at the admission examination, and 18 patients had a respiratory rate of ≥ 22/min. Only two patients had a qSOFA score of ≥ 2 on admission, seven had a CRB-65 score of ≥ 2, and 19 had a NEWS2 score of ≥ 5.
The average CRP in the first blood sample taken on admission was 64 mg/l. A total of 32 patients (76 %) had abnormalities on chest X-rays. The most frequent findings were patchy opacities in several lung sections and in both lungs (21 patients).
Course of the illness
The illness of nine patients (21 %) followed a critical course. Table 2 shows characteristics, symptoms and findings on admission of patients with severe and critical illness. The most striking differences were that critically ill patients had a higher NEWS2 score, higher CRP and lower lymphocyte count in comparison to their severely ill counterparts, and several had a respiratory rate of ≥ 22.
Table 2
Characteristics, symptoms and findings at the time of admission according to course of illness in patients with COVID-19 at Bærum Hospital in the period 9.3.2020–31.3.2020 (n = 42). Number (%) unless otherwise specified. qSOFA = quick Sepsis-related Organ Failure Assessment, NEWS2 = National Early Warning Score 2
| Severe illness (n = 33) |
Critical illness (n = 9) |
||
|---|---|---|---|
| Age (years) average (median, range) |
66.8 (71, 30–95) |
71.8 (77.0, 43–90) |
|
| Clinical Frailty Scale score1, average (median, range) |
3.1 (3, 1–7) |
2.1 (1, 1–5) |
|
| Charlson Comorbidity Index score, average (median, range) |
3.3 (3, 0–9) |
3.1 (3, 0–5) |
|
| No. of days with symptoms, average (median, range) |
7.4 (7, 0–18) |
7.2 (7, 3‒14) |
|
| Symptoms |
|||
| Cough |
22 (67) |
6 (67) |
|
| Dyspnoea |
20 (61) |
9 (100) |
|
| Fever |
25 (76) |
8 (89) |
|
| Reduced general condition |
25 (76) |
8 (89) |
|
| New-onset confusion |
6 (18) |
2 (22) |
|
| Gastrointestinal symptoms |
4 (12) |
2 (22) |
|
| Clinical findings on admission |
|||
| Body temperature < 36 °C or >38.0 °C |
18 (55) |
7 (78) |
|
| Body temperature (°C) average (median, range) |
37.8 (38.2, 36.4–39.1) |
38.0 (38.2, 35.8‒39.3) |
|
| Respiratory rate |
|||
| ≥ 22/min |
11 (33) |
7 (78) |
|
| ≥ 30/min |
1 (3) |
3 (33) |
|
| Systolic blood pressure < 100 mm Hg |
1 (3) |
0 (0) |
|
| Heart rate > 90 beats/min |
5 (15) |
3 (33) |
|
| SpO2 (%), average (median, range) |
95 (95, 88–100) |
91 (90, 87‒96) |
|
| Glasgow Coma Scale score ≤ 14 |
2 (6) |
1 (11) |
|
| CRB-65 score |
|||
| 1 |
14 (42) |
8 (89) |
|
| ≥ 2 |
6 (18) |
1 (11) |
|
| qSOFA score |
|||
| 1 |
12 (36) |
6 (67) |
|
| ≥ 2 |
1 (3) |
1 (11) |
|
| Systemic inflammatory response syndrome (SIRS) |
11 (33) |
6 (67) |
|
| NEWS2 score ≥ 5 |
11 (33) |
8 (89) |
|
| NEWS2 score, average (median, range) |
3.3 (3, 0–9) |
7.6 (8, 4‒10) |
|
| Laboratory values average (median, range) |
|||
| C-reactive protein (mg/l) |
52 (45, 3–168) |
106 (127, 16‒257) |
|
| Leukocytes (· 109/l) |
5.9 (5.5, 2.8–10.7) |
7.4 (6.7, 4.2‒11.1) |
|
| Lymphocytes (· 109/l) |
1.3 (1.1, 0.2–4.9) |
0.8 (0.7, 0.3–2.1) |
|
| Platelets (· 109/l) |
195 (193, 60–340) |
182 (177, 76‒261) |
|
| Creatinine (µmol/l) |
92 (83, 46–191) |
82 (82, 59‒109) |
|
| D-dimer (mg/l FEU) |
1.6 (1.0, 0.2–5.0) |
2.0 (0.9, 0.3–8.0) |
|
1Based on the patient's functioning 14 days prior to acute illness
Discussion
In line with earlier studies, we found that fever and respiratory tract symptoms were the most common symptoms in inpatients with COVID-19 (5, 6). Many patients had symptoms for 1–2 weeks before admission to hospital. Some patients appeared to experience a severe exacerbation of the disease late in the course, which distinguishes COVID-19 from other common infectious diseases. One of five patients had a critical course of illness. The percentage with critical illness was relatively high compared with European reported figures, which have been around 15 % (4). This may be due to a higher average age in our study or different admission practice. Continued monitoring of admission practice and course of illness may yield knowledge that can be used to provide advice to the general public and health personnel with regard to which patients should be examined in hospital.
In earlier studies, comorbidity has been associated with a severe course of illness and death (18–20). We found no clear difference between severely and critically ill patients. Only nine patients were aged 80 or more. This may be attributable to limited spread of infection in this age group during the first part of the outbreak. The spread of infection among the oldest patients may be less or delayed in Norway compared with, for example, Italy. Fewer older people live in institutions there, and more live in multi-generational homes or are cared for by younger family members. We expect that the proportion of severely ill older people and frail people who are admitted to hospitals will increase, with increasing spread of infection among the general public.
There is a need to identify clinical features and findings that can predict the course of illness and need for intensive care. CRB-65 and qSOFA scores of ≥ 2 are frequently used to predict a severe course in infection patients. In our study, these scoring systems did not appear very suitable for this purpose for COVID-19 patients, partly because few patients had compromised circulation systems. Eight of nine patients with a critical course had a CRB-65 score of 1, but this was mainly attributable to age.
Eight of nine patients with a critical course had a NEWS2 score of ≥ 5 on admission. Hypoxaemia is a frequent and serious finding in COVID-19 patients. In contrast to NEWS, NEWS2 includes oxygen saturation, need for oxygen treatment and a separate scale for patients with hypercapnia. The most frequently occurring individual findings in those who developed a critical illness were temperature < 36 °C or > 38.0 °C and respiratory rate ≥ 22/min. Whether NEWS2 score, individual elements in NEWS2 measured on admission or laboratory readings can be used to predict a severe course of illness should be investigated further in larger-scale studies.
One of five patients was admitted with new-onset confusion in the current history of illness, but this was not generally captured by the scoring systems. This may be because delirium symptoms often fluctuate, or because the scoring systems investigated are not appropriate for diagnosing delirium (21).
Limitations
Because of the low number, the results must be interpreted with caution. The dataset is based on a review of medical records, and imprecise or missing documentation may have affected the results for some of the variables. The study was conducted at only one hospital and during the first part of the COVID-19 outbreak in Norway. Several of the patients were young and fit without comorbidity, which we believe is due to the fact that the first phase of the COVID-19 outbreak in Norway featured imported cases. The proportion of elderly and frail patients may increase during the course of the outbreak in pace with ongoing spread of infection in Norway. The results can therefore not readily be generalised to other Norwegian hospitals or later phases of the outbreak. Indication for testing has been restricted for the general public since the outbreak started. Changes in test criteria during the study period may have affected admission practice.
Conclusion
Fever, reduced general condition, cough and dyspnoea were the most common symptoms of the first patients admitted to Bærum Hospital with COVID-19. Many patients had symptoms for 1–2 weeks before admission. One of five admitted patients had a critical course of illness. Few patients scored ≥ 2 on frequently used clinical tools such as CRB-65 and qSOFA, while the data may indicate that the NEWS2 score on admission may be a useful tool for identifying patients at risk of a very severe course of disease.
The article has been peer-reviewed.
- 1.
Wu F, Zhao S, Yu B et al. A new coronavirus associated with human respiratory disease in China. Nature 2020; 579: 265–9. [PubMed][CrossRef]
- 3.
World Health Organization. Coronavirus disease 2019 (COVID-19): situation report 51. https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200311-sitrep-51-covid-19.pdf?sfvrsn=1ba62e57_10 Accessed 20.3.2020.
- 4.
European Centre for Disease Prevention and Control. Coronavirus disease 2019 (COVID-19) pandemic: increased transmission in the EU/EEA and the UK – seventh update. https://www.ecdc.europa.eu/sites/default/files/documents/RRA-seventh-updateOutbreak-of-coronavirus-disease-COVID-19.pdf Accessed 31.3.2020.
- 5.
Guan WJ, Ni ZY, Hu Y et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med 2020; 382: NEJMoa2002032. [PubMed][CrossRef]
- 6.
Wang D, Hu B, Hu C et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA 2020; 323: 1061–9. [PubMed][CrossRef]
- 7.
Zhou F, Yu T, Du R et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 2020; 395: 1054–62. [PubMed][CrossRef]
- 8.
Statistisk sentralbyrå. Befolkning og kvartalsvise endringar, etter region, statistikkvariabel og kvartal: Asker og Bærum, 2019.
- 9.
Corman VM, Landt O, Kaiser M et al. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Euro Surveill 2020; 25: 2000045. [PubMed][CrossRef]
- 10.
Charlson ME, Pompei P, Ales KL et al. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373–83. [PubMed][CrossRef]
- 11.
Quan H, Li B, Couris CM et al. Updating and validating the Charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am J Epidemiol 2011; 173: 676–82. [PubMed][CrossRef]
- 12.
Rockwood K, Song X, MacKnight C et al. A global clinical measure of fitness and frailty in elderly people. CMAJ 2005; 173: 489–95. [PubMed][CrossRef]
- 13.
Myrstad M, Ranhoff AH. Acutely ill older people in the corona era. Tidsskr Nor Legeforen 2020; 140. doi: 10.4045/tidsskr.20.0227. [CrossRef]
- 14.
National Early Warning Score (NEWS) 2. Standardising the assessment of acute-illness severity in the NHS Updated report of a working party. Executive summary and recommendations. London: The Royal College of Physicians, 2017. https://www.rcplondon.ac.uk/file/8504/download Accessed 24.3.2020.
- 15.
Singer M, Deutschman CS, Seymour CW et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016; 315: 801–10. [PubMed][CrossRef]
- 16.
Spindler C, Strålin K, Eriksson L et al. Swedish guidelines on the management of community-acquired pneumonia in immunocompetent adults–Swedish Society of Infectious Diseases 2012. Scand J Infect Dis 2012; 44: 885–902. [PubMed][CrossRef]
- 17.
Lim WS, van der Eerden MM, Laing R et al. Defining community acquired pneumonia severity on presentation to hospital: an international derivation and validation study. Thorax 2003; 58: 377–82. [PubMed][CrossRef]
- 18.
Zhou F, Yu T, Du R et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 2020; 395: 1054–62. [PubMed][CrossRef]
- 19.
Huang C, Wang Y, Li X et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020; 395: 497–506. [PubMed][CrossRef]
- 20.
Remuzzi A, Remuzzi G. COVID-19 and Italy: what next? Lancet 2020; 395: 1225–8. [PubMed][CrossRef]
- 21.
Myrstad M, Neerland BE, Hagberg G et al. Vurdering av mental status hos akutt syke gamle. Tidsskr Nor Legeforen 2017; 137: 859. [PubMed][CrossRef]
Jeg er begeistret over hvor raskt Covid-19 tilfeller er beskrevet fra Bærum sykehus (1). En del pasienter ble meget dårlige. Med artifisiell intelligens av New York University er 3 funn fra pasienter fra Wenzhou, Kina vurdert som indikatorer for alvorlig klinisk forverring: ALAT, dype muskelsmerter og hemoglobinstigning (2). I vår artikkel om et anfall av idiopatisk kapillærlekkasje fant vi en betydelig økning i hemoglobin (hemokonsentrasjon) som vi tolket som forårsaket av plasmalekkasje gjennom kapillærene (3). Hemoglobin inngår ikke i de diagnostiske verktøy brukt til vurdering av pasientene i artikkelen. Hemoglobin er ikke notert i tabellene. Min tanke er at de tre parametre indikerer plasmalekkasje med hemokonsentrasjon, og begynnende kompartmentsyndrom. Fant man slike tegn som kunne varslet hvem som ble de sykeste pasienter?
Litteratur:
1. Håkon Ihle-Hansen, Trygve Berge, Anders Tveita med flere: Covid-19: Symptomer, forløp og bruk av kliniske skåringsverktøy hos de 42 første pasientene innlagt på et norsk lokalsykehus. Tidsskriftet 10. april 2020, doi: 10.4045/tidsskr.20.0301
2. Xiangao Jiang, Megan Coffee, Anasse Bari et al: Towards an Artificial Intelligence Framework for Data-driven Prediction og Coronavirus Clinical Severity. CMC, 2020(63,1): 537-551, CMC doi:10.32604/cmc.2020.010691
3. Ole Wilhelm Bøe, Kjell Sveen, Magne Børset, Kirk M. Druey: Raised Serum Levels of Syndecan-1 (CD138), in a Case of Acute Idiopathic Systemic Capillary Leak Syndrome (SCLS) (Clarkson’s Disease). Am J Case Rep 2018; 19:176-182,