Main message
Data from the Norwegian Patient Registry showed that 3.8 % of Norwegian children had been diagnosed with hyperkinetic disorder at 12 years of age.
The proportion of children with this diagnosis varied widely among counties.
A review of medical records showed that only half of the diagnoses were reliably documented.
There is a need to review the national guideline for evaluation and diagnostics, the requirements for medical recordkeeping, and the way in which the guideline is followed in clinical practice.
Hyperkinetic disorder is one of the most frequently used psychiatric diagnoses among children and adolescents in Norway (1). The condition is characterised by hyperactivity, impulsivity and inattention (2). In order to make the diagnosis, the symptoms must be present before the age of six and occur in multiple settings where the child spends time, i.e. both within the family and outside the home (2). The symptoms must also result in an obvious functional impairment in the child’s daily life (2). The diagnosis is defined in the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD-10), which is used to classify diagnoses in Norway and in most countries outside of North America (3). In the clinical section of the Official Guidelines for Coding and Reporting, the definition is brief and imprecise and does not include specific diagnostic criteria (3). However, diagnostic criteria have been developed for research use (2).
Data from the Norwegian Patient Registry for the years 2008–2011 showed that 3.4 % of Norwegian children had received the diagnosis from specialist health services at 12 years of age (4). In the age group 6–17 years, 3 % of the boys and 1 % of the girls were given medication to treat the condition (5). These percentages have been stable since 2010 (5). In population surveys that use questionnaires and clinical interviews to study a representative sample of children, the prevalence of hyperkinetic disorder is 1.7 % in children 7–9 years old (6) and 2.1 % in adolescents 13–15 years old (7). The differences in prevalence may be due to the fact that the population surveys set stricter requirements regarding functional impairment than those normally used in clinical practice (8).
The Norwegian Directorate of Health has prepared a guideline for assessment and diagnosis of hyperkinetic disorder (9). However, registry data have shown that use of the diagnosis in children varies widely by county (4). The discrepancy between population studies and registry data, as well as variations in use of the diagnosis by county, gives grounds for investigating the basis on which the diagnoses are made.
In this article, we present updated figures for the proportion of children and adolescents who are diagnosed with hyperkinetic disorder, for Norway as a whole and by county, as well as results from a national study of how hyperkinetic disorder is diagnosed and documented in medical records within specialist health services.
Material and method
National registry data
The Norwegian Patient Registry has personally identifiable data from 2008 to the present. In this study, we used data from specialist mental health services for children and adolescents, somatic hospitals and private contract specialists for the period 2008–2016. Hyperkinetic disorder was defined as one or more entries in the medical record of the diagnostic code F90 from ICD-10. This includes the diagnoses F90.0 Disturbance of activity and attention, F90.1 Hyperkinetic conduct disorder, F90.8 Other hyperkinetic disorders, and F90.9 Hyperkinetic disorder, unspecified.
As a general rule, hyperkinetic disorder is diagnosed from six years of age and older in Norway. We estimated the proportion of children who had received the diagnosis before turning 12 years old, for Norway as a whole and by county, using a Kaplan-Meyer analysis. We included everyone with a complete follow-up from six years of age in the Norwegian Patient Registry, i.e. children born in the years 2002–2010. For the county estimates, we calculated confidence intervals in order to compare the counties with the national average. If the entire confidence interval was under or over the national average, we categorised this as a significant deviation from the average. Because we made many comparisons (19 counties), we used strict confidence intervals (99.7 % based on Bonferroni correction). The analyses were performed in Stata 15 (StataCorp. 2017).
We also wanted to study potential changes in use of the diagnosis over time, so we estimated the proportion of children registered with the diagnosis within each calendar year for the period 2008–2016 by gender and age group. These calculations included everyone who was 6–17 years old in the relevant calendar year. The population data were obtained from the Norwegian Population Registry (10).
Review of medical records
The diagnostics study was conducted under the auspices of a research project on hyperkinetic disorders in the Norwegian Mother and Child Cohort Study (11). The participants were born in the years 1999–2009, and the study includes 112,700 children. Participants registered with an F90 diagnosis were identified by linking to the Norwegian Patient Registry. At the time of the linkage, the registry contained data for the years 2008–2012, and a total of 1699 children in the Norwegian Mother and Child Cohort Study were registered with the diagnostic code F90 during this period. Of the 1699 children, 1517 of them received the diagnosis from specialist mental health services for children and adolescents. The medical record reviews were limited to those children. The remaining 182 were registered with this diagnosis only at somatic hospitals and/or by private contract specialists.
Initially, the aim was to review the medical records of up to 30 children per county. In counties with more than 30 registered cases of hyperkinetic disorder, a random sample of the patients was selected. The aim was to review at least 500 medical records nationwide.
Specialists in clinical psychology, child psychiatry and clinical pedagogy developed a protocol for the review of medical records. Two specialists in clinical pedagogy, with extensive experience from specialist mental health services for children and adolescents within the specialist health service, used the protocol to survey the instruments and methods used in the evaluation, based on the assessment components recommended in the national guideline (9): developmental history, case history (anamnesis), questionnaires for determining symptoms and assessing functional level, psychiatric diagnostic interview (free-form or semi-structured), informant information, assessment of functional impairment, differential diagnostic assessment/evaluation, psychiatric medical assessment, assessment of cognitive skills, neuropsychological examination and assessment of executive functions. We also registered the diagnoses that were recorded in the multiaxial coding system which is used in specialist mental health services for children and adolescents. The protocol is attached as an appendix.
E-Table 1
Complete list of assessment components used in the assessment of hyperkinetic disorders in Norway. Survey based on participants in the Norwegian Mother and Child Cohort Study who were diagnosed with hyperkinetic disorder by specialist health services.
| Component | Conducted and documented (N = 540) | |
|---|---|---|
| Number | Percentage | |
| Survey of developmental history | 518 | 96 |
| Questionnaires for determining symptoms and assessing functional level | 478 | 89 |
| Child Behavior Checklist (CBCL) – one parent | 130 | 24 |
| Child Behavior Checklist (CBCL) – both parents | 249 | 46 |
| Barkley ADHD Rating Scale – parents | 283 | 52 |
| Brown ADD Scale – parents | 61 | 11 |
| Teacher Rating Form (TRF) – teacher | 364 | 67 |
| Barkley ADHD Rating Scale – teacher | 270 | 50 |
| Other specified questionnaires parents/teacher | 187 | 35 |
| Standardised psychiatric interview | 157 | 29 |
| Kiddie Schedule for Affective Disorders and Schizophrenia (K-SADS) | 64 | 12 |
| Development and Well-Being Assessment (DAWBA) | 97 | 18 |
| Other diagnostic interview | 18 | 3 |
| Informant information | 516 | 96 |
| School/kindergarten observation | 482 | 89 |
| Conversation with school teacher/kindergarten teacher | 490 | 91 |
| Observation of play in clinic | 296 | 55 |
| Other observation in clinic | 77 | 14 |
| Observation at home | 22 | 4 |
| Other informant information | 15 | 3 |
| Assessment of functional impairment | 416 | 77 |
| Differential diagnostic assessment/evaluation | 289 | 54 |
| Medical/neurological examination | 446 | 83 |
| Cognitive ability or developmental test | 344 | 64 |
| Wechsler Preschool and Primary Scale of Intelligence (WPPSI) | 95 | 18 |
| Wechsler Intelligence Scale for Children - Third edition (WISC-III) | 52 | 10 |
| Wechsler Intelligence Scale for Children - Fourth edition (WISC-IV) | 188 | 35 |
| Wechsler Abbreviated Scale of Intelligence (WASI) | 4 | 1 |
| Leiter International Performance Scale – Revised | 11 | 2 |
| Other cognitive ability or developmental test | 36 | 7 |
| Linguistic test | 131 | 24 |
| Språk 6–16 (‘Language 6–16’) | 67 | 12 |
| Illinois Test of Psycholinguistic Abilities (ITPA) | 19 | 4 |
| Reynell Developmental Language Scale | 41 | 8 |
| Test of Receptive Grammar – Second edition (TROG-2) | 19 | 4 |
| Clinical Evaluation of Language Fundamentals – Fourth edition (CELF-4) | 2 | 0 |
| Other specified linguistic test | 34 | 6 |
| Sustained attention test | 203 | 38 |
| Conners’ Continuous Performance Test (CPT) | 156 | 29 |
| Quantitative Behavior Test (QB Test) | 49 | 9 |
| Neuropsychological examination | 91 | 17 |
| Assessment of executive functions | 153 | 28 |
| Behavior Rating Inventory of Executive Function (BRIEF) – parent | 143 | 26 |
| Behavior Rating Inventory of Executive Function (BRIEF) – teacher | 132 | 24 |
After completing the medical record review, the specialist in clinical pedagogy assessed whether the child met the diagnostic criteria defined for research on hyperkinetic disorder, on the basis of all the material in the medical record (2). In case of doubt, both specialists reviewed the medical record and reached a consensus.
If the conclusion was that the diagnosis was not reliably documented in the medical record, the specialists would give one or more of the following reasons:
-
Discrepancy between information in the medical record and the diagnosis
-
Insufficient/missing information
-
Inadequate differential diagnostic assessment/evaluation
-
Diagnosis made solely for the purpose of trying out a drug
-
Tentative diagnosis, no further assessment available
-
Incorrect coding
In clinical practice in Norway, it has been common to use the diagnostic code F90 also when attention deficit is the dominant or only problem. In such cases, the diagnosis was regarded as having been documented if the child met the diagnostic criteria for inattention in ICD-10.
The regional ethics committee approved the use of registry data and the review of medical records (ref. 2010/2583 and 2013/594). The Norwegian Mother and Child Cohort Study is regulated under the Personal Health Data Registries Act and the Health Research Act. Participation is based on informed consent from the parents and includes obtaining data from health registries and hospital records.
Results
National registry data
Altogether 556,917 children had a complete follow-up from six years of age. The estimated proportion with hyperkinetic disorder at age 12 was 3.8 % (5.4 % for boys and 2.1 % for girls). There were significant differences among the counties (Figure 1), from 1.5 % in Vest-Agder to more than 5 % in Nordland, Rogaland, Hedmark and Sør-Trøndelag. The majority of counties showed a significant deviation from the national average.

There were 2.5 times as many boys as girls registered with the diagnosis upon turning 12 years of age for the entire country, with variations by county from 1.9 (Vest-Agder) to 3.7 (Aust-Agder). Average age when the diagnosis was first registered was 8.6 years for Norway as a whole, with relatively little variation among the counties (from 8.3 years in Møre og Romsdal to 9.0 years in Østfold).
The percentages of boys and girls registered with hyperkinetic disorder were relatively stable over time in all age groups (Figure 2). Most of the counties also showed stable percentages over time in the period 2008–2016. The exceptions were Aust-Agder and Nordland, where the percentages declined, while Sør-Trøndelag showed a slight increase.
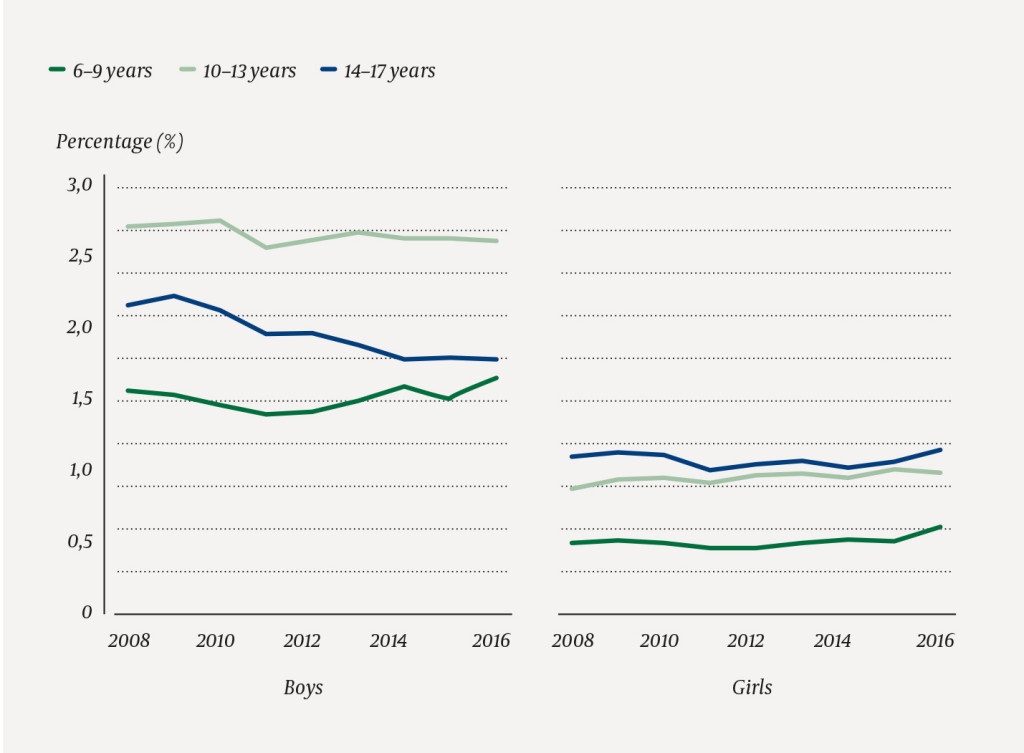
Review of medical records
We reviewed the medical records of 549 children, 405 (74 %) boys and 144 (26 %) girls, at 20 health trusts in 18 counties. Of these, 540 (98 %) had been diagnosed with hyperkinetic disorder by a doctor or psychologist. For the other nine children (2 %), the F90 diagnosis was probably registered in error, as we did not find any information indicating that the child had received the diagnosis.
The child’s age when first diagnosed with hyperkinetic disorder varied from 3 years to 11 years. For 392 (71 %) of the children, the reason for referral was suspicion of hyperkinetic disorder, while 137 (25 %) were referred for other reasons. Information about the reason for referral was missing for 20 (4 %) of the children.
For 538 (98 %) of the children, hyperkinetic disorder was registered as a diagnosis on axis I (clinical psychiatric syndrome) in the multiaxial coding system used by specialist mental health services for children and adolescents. A total of 462 (84 %) were scored on axis II (specific developmental disorders), and 456 (83 %) were scored on axis III (intellectual level).
Survey of the child’s developmental history was documented in 96 % of the cases in which a clinician had made the diagnosis (Table 2). A standardised questionnaire was used for 89 %. A standardised psychiatric interview was conducted for 29 % of the children. Informant information was obtained for 96 %, usually both from school or kindergarten observation and from conversations with the school teacher/kindergarten teacher (Table 2). Observation of play or other observation in the clinic was carried out for the majority of children. The aim of most of the observations was limited to uncovering symptoms of hyperkinetic disorder. An assessment of functional impairment was documented for 77 %.
Table 2
Assessment components used in the assessment of hyperkinetic disorder in Norway. Survey based on participants in the Norwegian Mother and Child Cohort Study who were diagnosed with hyperkinetic disorder by the specialist health service.
| Component | Conducted and documented | |
|---|---|---|
| Number | Percentage | |
| Survey of developmental history | 518 | 96 |
| Questionnaires for determining symptoms and assessing functional level | 478 | 89 |
| Standardised psychiatric interview | 157 | 29 |
| Informant information | 516 | 96 |
| Assessment of functional impairment | 416 | 77 |
| Differential diagnostic assessment/evaluation | 289 | 54 |
| Medical/neurological examination | 446 | 83 |
| Cognitive ability or developmental test | 344 | 64 |
| Linguistic test | 131 | 24 |
| Sustained attention test | 203 | 38 |
| Neuropsychological examination | 91 | 17 |
| Assessment of executive functions | 153 | 28 |
Differential diagnostic assessment/evaluation, i.e. assessment of alternative diagnoses or alternative explanations for the symptoms, was documented in 54 %. A cognitive ability or developmental test was carried out for 64 %. A complete list of the assessment components are attached in e-Table 1.
We concluded that hyperkinetic disorder was reliably documented in the medical records for 49 % of the children (Table 3). For the other 51 %, we concluded that the diagnosis was not reliably documented, but there were different reasons for these conclusions. For 38 %, there was a discrepancy between the information in the medical records and the diagnosis, i.e. the information indicated that the child did not meet the diagnostic criteria. Other important reasons were insufficient or missing information in the medical records (48 %) and lack of differential diagnostics (46 %). A total of 4 % of the children had received the diagnosis solely for the purpose of trying out a drug, and a diagnosis of hyperkinetic disorder was never assigned. A tentative diagnosis was made for 3 %, but we found no information about the final conclusion.
Table 3
Conclusion after medical record review for children with hyperkinetic disorder in Norway. Survey based on participants in the Norwegian Mother and Child Cohort Study who were diagnosed with hyperkinetic disorder by the specialist health service.
| Conclusion (N = 540) | Number | Percentage |
|---|---|---|
| Hyperkinetic disorder reliably documented | 263 | 49 |
| Hyperkinetic disorder not reliably documented1 | 277 | 51 |
| Discrepancy between information in the medical record and the diagnosis | 203 | 38 |
| Insufficient/missing information | 260 | 48 |
| Inadequate differential diagnostic assessment/evaluation | 251 | 46 |
| Diagnosis made solely for the purpose of trying out a drug | 21 | 4 |
| Tentative diagnosis, no further evaluation available | 17 | 3 |
1The sum of the numbers in the sub-categories exceeds 277 because giving multiple reasons was permitted.
Discussion
At 12 years of age, 1 of 19 boys and 1 of 48 girls were registered with hyperkinetic disorder in Norwegian specialist health services. The percentages of children with the diagnosis were stable in the years 2008–2016 for Norway as a whole. The percentages are slightly higher in Norway than in Sweden, Denmark and Finland (12), but correspond with the estimate of 3.4 % in a meta-analysis of 41 studies from 27 countries (13). The percentages receiving medication are at the same level as in Sweden and Denmark, but higher than in Finland (5).
As previously reported, there are substantial variations among the counties. The counties at the top have percentages that are four times as high as the county at the bottom. These variations cannot be explained by differences in gender distribution among those who receive the diagnosis or by the average age at the time of diagnosis. The most likely explanation is regional differences in diagnostic practice. Similar differences among counties have also been previously shown for autism spectrum disorder (4).
The findings from the medical record review indicate that hyperkinetic disorder is often less well documented than other chronic conditions, e.g. cerebral palsy (14). Nor does the Norwegian Patient Registry have information about who has ‘grown out of’ the diagnosis. We also know from previous studies that many children who meet the criteria for psychiatric diagnoses have not been in contact with specialist health services (6). Thus, we cannot use our findings to estimate the actual prevalence of hyperkinetic disorder in the child population in Norway.
From the medical record reviews, we concluded that the diagnosis had not been reliably documented in half of the cases. It is important to emphasise that we have not conducted an independent diagnostic assessment with our own clinical examination of the children. Symptoms consistent with hyperkinetic disorder were recorded for many children, but the information was too scant to reach a conclusion or there was a lack of differential diagnostic assessments. For the majority of those who did not have reliably documented diagnoses, however, there were clear indications that they did not meet the diagnostic criteria. This could indicate that some children are diagnosed with hyperkinetic disorder without actually having it.
Inadequate differential diagnostic assessment and evaluation was the most important reason that diagnoses were not reliably documented. Our assessments were based on all the information found in the medical record, and a lack of one or more assessment components did not automatically result in a conclusion of inadequate differential diagnostics. However, these inadequacies often occur because a standardised psychiatric interview with a broad survey of symptoms was not conducted. Another widespread deficiency in the differential diagnostics was that learning disabilities were not mapped or assessed. Cognitive ability and developmental testing was often not carried out even though learning disabilities were mentioned in both the referral and the anamnesis. In other cases, cognitive ability tests were conducted and clear indications of learning disability or delayed development were found, but the diagnostic assessment did not take this into account. Some medical records contained information about other circumstances in the child’s life that could help to explain the symptoms, such as divorce, serious illness of a parent, parental neglect, abuse or bullying. Learning disabilities, delayed development or difficult circumstances in the child’s life do not exclude the child from having hyperkinetic disorder, but there was often no discussion of what these problems meant for the child’s symptoms and functioning.
The national guideline provides little direction and does not set clear requirements as to what should be included in an assessment of hyperkinetic disorder. As such, it does not provide adequate guidance to those conducting the assessments. We believe this is one reason why many of the diagnoses are poorly documented in the medical records.
Another problem is the brief, imprecise definition of the actual diagnosis in ICD-10, which does not provide specific diagnostic criteria (3). All research on hyperkinetic disorder is based on the diagnostic criteria developed for use in research, and it is therefore important that these criteria are also used in clinical practice (2). Use of the research criteria was part of the diagnostic procedure at many of the institutions we visited. In our view, these diagnostic criteria should also be included in the national guideline, as they provide good and essential support for diagnosing the disorder.
In addition, our impression is that there is a need to improve the quality of the observations of children carried out by specialist health services. The reports from the school observations usually contained only information about the symptoms of hyperkinetic disorder and not information about other factors that could affect the child’s behaviour, such as the classroom environment, organisation of the teaching, and the interaction between the teacher and pupil. Unfortunately, there are no well-evaluated methods for observations of this kind.
Another important experience from the medical record review was that we seldom found information about how the children and parents perceived the problems, the type of help they needed and how they dealt with the diagnosis. It was the kindergarten or school that usually wanted the referral. Our protocol contained no formal survey of involvement from the parents and children. A lack of such information in the medical records makes it uncertain whether the families were given the opportunity for user involvement to which they are entitled (9).
The review of medical records had some weaknesses. We could not analyse the reasons for the county-wise differences because the number of participants per county was too small. Since we only visited clinics in specialist mental health services, we cannot comment on the diagnostics employed at somatic hospitals or by private contract specialists. Many medical records were reviewed by only one expert, which may have made the conclusions vulnerable to subjectivity. Ideally, two experts should have reviewed all the records.
The proportion of children with F90 diagnoses from the specialist health service is lower in the Norwegian Mother and Child Cohort Study than among the general Norwegian childhood population (15). Nonetheless, we believe that our findings are representative for how assessment and diagnosis of hyperkinetic disorder are carried out in specialist mental health services for children and adolescents in Norway.
Conclusion
Hyperkinetic disorder is one of the most frequently used psychiatric diagnoses among children. The registry data show that significant variations in use of the diagnosis among counties persist. The review of medical records shows that only half of the diagnoses are reliably documented. There is a need to review the national guideline for evaluation and diagnostics, the requirements for medical recordkeeping, and the way in which the guideline is followed in clinical practice. The guideline should be changed so that it sets a clear standard for how assessments are conducted. For example, standardised psychiatric interviews and cognitive ability and developmental tests should be mandatory components of the assessment. Moreover, sound, standardised methods for observations of children in schools, kindergartens and clinics should be developed.
- 1.
Reneflot A, Aarø LE, Aase H et al. Psykisk helse i Norge. Oslo: Folkehelseinstituttet, 2018. https://www.fhi.no/publ/2018/psykiskhelse-i-norge/ (12.10.2018).
- 2.
The ICD-10 classification of mental and behavioural disorders. Diagnostic criteria for research. Geneve: World Health Organization, 1993. http://www.who.int/classifications/icd/en/GRNBOOK.pdf (12.10.2018).
- 3.
International Statistical Classification of Diseases and Related Health Problems. 10th Revision. Geneve: World Health Organization, 1990.
- 4.
Surén P, Bakken IJ, Lie KK et al. Fylkesvise forskjeller i registrert forekomst av autisme, AD/HD, epilepsi og cerebral parese i Norge. Tidsskr Nor Legeforen 2013; 133: 1929 - 34. [PubMed][CrossRef]
- 5.
Furu K, Karlstad Ø, Zoega H et al. Utilization of stimulants and atomoxetine for attention-deficit/hyperactivity disorder among 5.4 million children using population-based longitudinal data. Basic Clin Pharmacol Toxicol 2017; 120: 373 - 9. [PubMed][CrossRef]
- 6.
Heiervang E, Stormark KM, Lundervold AJ et al. Psychiatric disorders in Norwegian 8- to 10-year-olds: an epidemiological survey of prevalence, risk factors, and service use. J Am Acad Child Adolesc Psychiatry 2007; 46: 438 - 47. [PubMed][CrossRef]
- 7.
Ford T, Goodman R, Meltzer H. The British Child and Adolescent Mental Health Survey 1999: the prevalence of DSM-IV disorders. J Am Acad Child Adolesc Psychiatry 2003; 42: 1203 - 11. [PubMed][CrossRef]
- 8.
Posserud MB, Ullebø AK, Plessen KJ et al. Influence of assessment instrument on ADHD diagnosis. Eur Child Adolesc Psychiatry 2014; 23: 197 - 205. [PubMed][CrossRef]
- 9.
ADHD/Hyperkinetisk forstyrrelse – Nasjonal faglig retningslinje for utredning, behandling og oppfølging. Helsedirektoratet. https://helsedirektoratet.no/retningslinjer/adhd (27.2.2018).
- 10.
Statistisk sentralbyrå: Tabell 07459. Alders- og kjønnsfordeling i kommuner, fylker og hele landets befolkning (K) 1986–2018. https://www.ssb.no/statbank/table/07459 (12.10.2018).
- 11.
Magnus P, Birke C, Vejrup K et al. Cohort Profile Update: The Norwegian Mother and Child Cohort Study (MoBa). Int J Epidemiol 2016; 45: 382 - 8. [PubMed][CrossRef]
- 12.
Atladottir HO, Gyllenberg D, Langridge A et al. The increasing prevalence of reported diagnoses of childhood psychiatric disorders: a descriptive multinational comparison. Eur Child Adolesc Psychiatry 2015; 24: 173 - 83. [PubMed][CrossRef]
- 13.
Polanczyk GV, Salum GA, Sugaya LS et al. Annual research review: A meta-analysis of the worldwide prevalence of mental disorders in children and adolescents. J Child Psychol Psychiatry 2015; 56: 345 - 65. [PubMed][CrossRef]
- 14.
Hollung SJ, Vik T, Wiik R et al. Completeness and correctness of cerebral palsy diagnoses in two health registers: implications for estimating prevalence. Dev Med Child Neurol 2017; 59: 402 - 6. [PubMed][CrossRef]
- 15.
Oerbeck B, Overgaard KR, Aspenes ST et al. ADHD, comorbid disorders and psychosocial functioning: How representative is a child cohort study? Findings from a national patient registry. BMC Psychiatry 2017; 17: 23. [PubMed][CrossRef]
Forfattarane skriv at "all forskning på hyperkinetisk forstyrrelse baserer seg på diagnosekriteriene som er utviklet til forskningsbruk, og det er derfor viktig at de også brukes i klinisk praksis". Vidare skriv dei at "vi mener det også bør inngå i den nasjonale retningslinjen, da diagnosekriteriene gir en god og nødvendig støtte i diagnostikken". Diagnosekriterier er heilt nødvendige for å sikre mest mogeleg like pasientgrupper i forskning, men diagnosekriteria er symptom og funn for å identifisere pasientar med ein sjukdom der me ikkje kjenner patologien som er årsaka til sjukdomen. Me har ikkje ein diagnostisk gullstandard med bakgrunn i patologi, og det vil være svært usannsynlig og eineståande innan medisinsk diagnostikk at diagnostiske kriterier basert på symptom har ein sensitivitet på 100 %. Det betyr at dersom diagnosen hyperkinetisk forstyrrelse berre skal brukast på dei som stettar forskningskriteria vil det medføre at nokre pasientar som høgst sannsynleg har hyperkinetisk forstyrrelse ikkje vil få diagnosen, og heller ikkje få eit relevant behandlingstilbod. Komorbiditet kompliserar og ofte diagnostiseringa, og diagnosen er ikkje alltid like objektiv. Denne gruppa som ikkje stettar forskningskriteria, kan ha like stort behov for hjelp, og etter mi erfaring like stor nytte av medikamentell behandling som dei som stettar forskningskriteria. Det er difor viktig med ei pragmatisk holdning til diagnosen for å sikre at alle med hyperkinetisk forstyrrelse får tilbod om hjelp og eventuelt prøvd medikamentell behandling. Systematisk utprøving av medikamentell behandling under nøye observasjon av effekt, og seponering ved manglande effekt er etter mi erfaring like uproblematisk og ufarleg for denne gruppa som ikkje stettar forskningskriteria som for gruppa som stettar forskningskriteria, der ein og vil oppleve manglande effekt av medikamentell behandling. For å sikre alle med hyperkinetisk forstyrrelse rett behandling er det etter mi meining viktig at forskningskriteria blir brukt som eit hjelpemiddel, og at å stette desse kriteria ikkje er eit absolutt krav for å stille diagnosen.
Vi takker Bjarne Bråtveit for kommentaren til artikkelen vår. Vi er enige med ham i at det ikke skal være et absolutt forbud mot å bruke diagnosen hyperkinetisk forstyrrelse selv om ikke alle diagnosekriteriene er oppfylt. Man bør imidlertid være svært forsiktig med å bruke diagnosen på personer som ikke tilfredsstiller diagnosekriteriene. Disse kriteriene er grunnlaget for alle studier som er gjort av hyperkinetisk forstyrrelse. Dermed utgjør de også grunnlaget for hvordan diagnosen skal brukes i klinisk praksis. Det finnes ingen klinisk diagnose som representerer noe annet enn den forskningsbaserte diagnosen. Hvis klinikere bruker diagnosen på andre enn de den opprinnelig er ment for, beveger de seg ut i terreng hvor det ikke finnes evidens for at behandling virker. I slikt terreng kan en «pragmatisk» holdning til diagnosen fort bli «slepphendt». Vi mener derfor at alle som utreder og diagnostiserer hyperkinetisk forstyrrelser må forholde seg aktivt til diagnosekriteriene og ha en solid begrunnelse for å eventuelt avvike fra dem.