Of all musculoskeletal pain, knee pain is among the most frequently occurring. The majority of the patients have an atraumatic knee disorder (1). Pain receptors cannot be detected in joint cartilage, but are abundantly present in other structures, including joint ligaments, the synovium, the subchondral bone and surrounding soft tissue. Experience shows, however, that there will often be doubt regarding the origin of pain in atraumatic knee disorders, even after a thorough examination.
Symptoms that often accompany knee pain include stiffness, knee locking, muscle weakness and instability. In an interview survey of persons who were older than 20 years and resident in Nord-Trøndelag county, one in every seven women and one in every ten men reported to have suffered from knee pain of at least three months' duration in the course of one year (2). There are grounds to assume that knee pain is reported more frequently than before, but this tendency applies to musculoskeletal disorders in general (3, 4).
Radiologically verified gonarthrosis increases in frequency with advancing age (5). Some studies support the notion that the frequency of knee pain also increases somewhat with age, but that the curve levels off around the age of 50 (6–8). Although it is commonly assumed that symptoms of gonarthrosis worsen over time, a prospective study of 1 753 patients with moderate gonarthrosis found that their knee pain remained unchanged over a six-year period, in spite of radiological progression (9).
As for other musculoskeletal pain, patients with knee disorders will as a rule first turn to a general practitioner (6, 7). Commonly, after undertaking a clinical examination, the GP will refer the patient for an MRI scan of the knees and/or to a physiotherapist. If the MRI scan indicates that the condition is operable, the patient will be referred to an orthopaedist and in many cases undergo arthroscopy.
Recent research has cast doubt on the justification for a narrowly biomechanical model of understanding for assessment of patients who suffer from knee disorders that have not been caused by an obvious trauma. It is claimed that current practice partly leads to overdiagnosis as a result of erroneous or over-interpretation of normal variants, and partly to treatment that is of doubtful benefit, which drives up the cost level and involves a risk of iatrogenic injury (10, 11). Figure 1 provides a schematic overview of precipitating and perpetuating factors in atraumatic knee pain with or without degenerative changes.
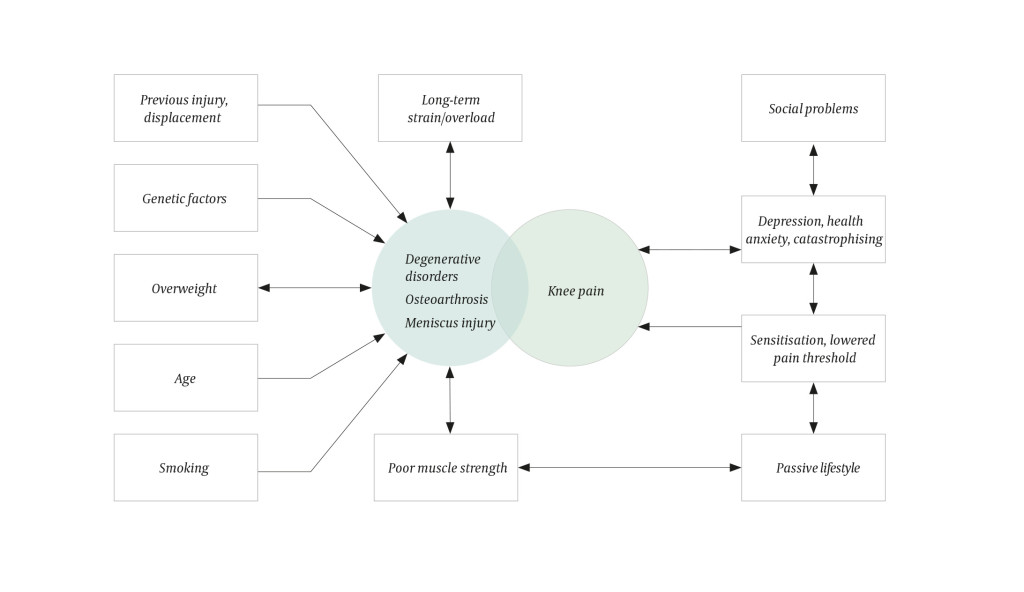
The objective of this article is partly to provide an overview of recent research on examination and treatment of atraumatic knee pain, and partly to elucidate the degree to which such research results have influenced the health services' approach to this large group of patients.
Method
This review is based on a selection of articles found through literature searches in Medline with the search terms 'knee AND (osteoarthrit* OR menisc*)' in titles and summaries, in combination with 'degenerative, psychol*, cognitive, radiogr*, MRI, arthrosc*, diagnos*'. Additional articles were identified through suggestions from the Mendeley reference programme and manual searches in lists of references.
The search was restricted to English-language articles on knee pain unrelated to trauma or septic or inflammatory arthritis, published over the last 20 years. It was concluded in September 2017. Altogether 889 articles were identified, of which 141 were reviews. The relevance of each article was determined by discretionary judgment on the basis of the title and summary. Of these 889 articles, 111 were retrieved in full-text versions. A total of 48 of these were included, of which 18 were reviews.
Knee pain and cognitive, mental and social factors
While a biopsychosocial model of understanding has gradually become accepted with regard to musculoskeletal disorders, knee disorders tend to be regarded as an expression of purely biomechanical dysfunction, often as a result of long-term or unaccustomed strain (5).
Patients with knee symptoms are a heterogeneous group, but numerous studies have shown significant mental comorbidity in chronic knee pain. Somewhat paradoxically, the incidence of anxiety, depression, difficult social conditions, poor coping, somatisation and catastrophising is highest in the group with sparse clinical and radiological findings (1), (12–15).
A study of functional impairment in patients with knee pain and radiologically verified osteoarthrosis found no association with the x-ray findings (osteophytes and reduced cartilage height), while high body-mass index, perceived helplessness, pain intensity and anxiety explained approximately 60 % of the variance (16).
One study compared a group that had significant gonarthrosis (Kellgren-Lawrence degree 3–4), but little pain, with a group with moderate gonarthrosis (KL degree 1–2), but strong pain. The latter group had increased sensitivity to sensory tests, interpreted as an expression of sensitisation (17).
After knee prosthesis surgery, a considerable minority reports persistent pain one year or more after the operation. This group is characterised by a higher pre-operative incidence of mental problems and catastrophising (18, 19). Such studies underscore that the causal relationships in chronic knee pain can be complex and that the treatment needs to take this into account (Figure 1).
Knee pain and radiological findings
In cases of typical symptoms of gonarthrosis (weight-bearing pain, transient morning stiffness), clinical findings (reduced mobility, crepitation, joint line tenderness) and risk factors (overweight, female sex and age > 40 years), a diagnosis of osteoarthrosis can often be made without any supplementary diagnostic imaging (20).
If such an examination nevertheless is undertaken, standing x-ray images should be made of both knees in three projections: lateral images, frontal images in semiflexion and skyline images of the patellofemoral joint (20). Classical x-ray findings in knees in cases of osteoarthrosis include pronounced medial joint space narrowing, osteophytes, subchondral sclerosis and subchondral cysts (21).
Lack of correspondence between radiological findings and knee pain has been frequently described. In a systematic review, the prevalence of radiologically verified gonarthrosis in patients with knee pain varied from 15 % to 76 % in different studies, while the proportion with knee pain among those who were diagnosed with arthrosis varied from 15 % to 85 % (22).
The association between radiological findings and knee function is also poorly documented (16). An emphasis on radiological findings at the expense of a clinical examination may cause periarticular disorders such as bursitis, tendinosis, regional myofascial pain conditions, pain transferred from proximal structures and neurogenic hyperalgesia to be overlooked (23).
Magnetic resonance imaging in cases of knee pain
In a study of participants in the age group older than 50 years and with no osteoarthrosis detected by radiology, an MRI scan showed at least one pathological finding in up to 97 % of those with knee pain and up to 88 % of those with no pain (24). In a study with randomly selected participants in the same age group, a meniscus injury was detected by an MRI scan in 35 % and in more than half of those older than 70 years (25). In the group with moderate to severe osteoarthrosis shown radiologically (KL degree 2–4), a meniscus injury was found in 82 %. However, only 39 % of those with a meniscus injury reported any knee symptoms.
The high prevalence and strong association between meniscus injuries and osteoarthrosis mean that an MRI examination rarely entails any diagnostic or therapeutic consequences in the age group older than 40 years, unless there are clinical indications of a more severe underlying disorder (26, 27).
In 2002, altogether 95 MRI scans of knees were undertaken per 1 000 inhabitants, increasing to 173 per 1 000 in 2013 (28, 29). The increase was strongest in the age group 50–59 years. Knee pain is currently the third most frequent indication for an MRI scan in Norway, after pain of the head and lumbar region. General practitioners account for 90 % of the referrals for MRI scans to private radiology institutes (29).
A review undertaken by the Office of the Auditor General concluded that the extensive use of MRI scans for knee pain lacked any documented beneficial effects, and there were also inexplicably large variations between the counties (29). The majority of Norwegian radiologists also agree that there is an overconsumption of MRI scans (29, 30). It is reasonable to assume that this also applies to MRI scans for the assessment of knee pain.
Poorly justified MRI scans are costly, may give rise to expectations of a referral to an orthopaedist and contribute to medicalisation (31). As a rule, an adequate clinical examination, supplemented by standing x-ray images will be sufficient to reveal the causal relationships, for the patient as well as the doctor.
Symptoms and findings for meniscus injuries
Mechanical symptoms such as popping, knee locking and catching are traditionally regarded as classical symptoms of meniscus injury with an indication for meniscus surgery. Recent studies cast doubts on this interpretation. In a randomised, placebo-controlled study of patients with knee pain that was degenerative in origin, the prevalence of mechanical symptoms was 49 % after arthroscopic meniscus resection and 43 % in the placebo group (32). In another study, it turned out that pre-operatively self-reported pain and functional impairment were not associated with structural knee pathology, including degenerative meniscus injury, detected by subsequent arthroscopy (33).
A positive McMurray test, a test in which the tibia is rotated with a simultaneous extension of the knee joint, is often regarded as one of the most reliable clinical signs of a meniscus injury. In controlled studies, on the other hand, inter-rater concordance tends to be low for this test (34). Nor have more recent clinical tests been shown to have a specificity that can reliably distinguish between meniscus injuries and other causes of knee pain (35, 36).
It is thus doubtful whether meniscus injuries can be distinguished from other pathology through detection of specific symptoms or clinical findings in patients with degenerative knee disorders.
Arthroscopy for atraumatic and degenerative knee disorders
In the last couple of decades, knee arthroscopy has become the most common orthopaedic procedure in countries for which there are available data, and this increase has been especially pronounced for middle-aged and elderly patients, among whom degenerative knee pain predominates (37). After two randomised studies showed that arthroscopic lavage and debridement of cartilage and meniscus tissue had no discernible effect on gonarthrosis, some countries have reported a reduction in the use of this procedure.
On the other hand, some increased use of arthroscopic meniscus surgery has been described during the same period (37). Since 2002, a number of randomised, controlled studies of this procedure have been conducted, in Norway as well as in other countries. The majority of the studies have been unable to show any better effect of arthroscopy than of physical exercise under the auspices of a physiotherapist, or placebo surgery (38, 39).
Partial meniscectomy increases the risk of developing radiologic gonarthrosis after one year (40) as well as later in the course of illness (41), although the clinical consequences of this are somewhat uncertain. The risk of pre- or post-operative complications in knee arthroscopy is low, but not negligible (42). The time has come to abandon the myth that arthroscopic surgery is a relevant intervention for the great majority of patients who suffer from atraumatic and degenerative knee disorders (11, 43, 44). We should expect that within a short time, knee arthroscopy will be restricted to indications where it will provide a proven benefit, primarily traumatic meniscus injuries in people younger than 35 years (10)
Conclusion
The 'standard model' applied in examination and treatment of atraumatic knee pain is out of step with new knowledge. Measures to reduce the use of MRI scans in atraumatic knee pain and a further reduction in the use of arthroscopy ought to be given especially high priority in health policy.
Although a conventional pathoanatomical model will not necessarily be irrelevant, the causal relationships in chronic knee pain are often multifactorial. Especially in cases where the symptoms and functional impairment cannot reasonably be related to findings made clinically and by diagnostic imaging, attention should be directed towards psychosocial components.
As a clinician, it is easy to assume a model of 'mechanical failure' and forget the wider context of which the knee symptoms are part (45). By disregarding such factors and continuing with our technically sophisticated, biomedically based diagnostics and treatment, we as healthcare workers risk imposing a further burden on the patient.
Patients may have unrealistic expectations regarding the benefits of diagnostic imaging and orthopaedic procedures (46). Communicating that a thorough clinical examination is often sufficient in cases of atraumatic knee pain is an important, but frequently challenging and time-consuming educational task. The patient should also be informed that 'low-tech' treatment principles – lifestyle change, active coping and individualised exercise therapy – have a documented effect on knee pain and functioning (47, 48). Such measures ought to constitute the mainstay of the approach taken by the health services to patients with atraumatic knee disorders.
I wish to thank May Arna Risberg, Jens Ivar Brox and Knut Arne Holtedahl for their useful comments.
MAIN MESSAGE
Atraumatic knee pain is only to a moderate degree associated with findings made by diagnostic imaging, and too many MRI scans are performed
Degenerative meniscus injuries are not normally associated with specific symptoms or findings
Knee pain may have causes other than osteoarthrosis or meniscus injury, including soft-tissue pain and pain secondary to underlying psychosocial stress
Self-care, activity-based interventions and weight loss, if appropriate, are the first choice. Arthroscopy is rarely indicated
- 2.
Svebak S, Hagen K, Zwart JA. One-Year Prevalence of Chronic Musculoskeletal Pain in a Large Adult Norwegian County Population: Relations with Age and Gender – The HUNT Study. J Musculoskeletal Pain 2006; 14: 21 - 8. [CrossRef]
- 29.
Riksrevisjonens undersøkelse av bruken av poliklinisk bildediagnostikk. Oslo: Riksrevisjonen, 2016. https://www.riksrevisjonen.no/rapporter/Sider/PolikliniskBildediagnostikk.aspx (5.1.2018).
- 46.
Fagerlin A, Sepucha KR, Couper MP et al. Patients' knowledge about 9 common health conditions: the DECISIONS survey. Med Decis Making 2010; 30 (suppl): 35S – 52S.
Takk for en flott artikkel, håper den blir lest av mange allmennpraktikere og ortopeder! Hilsen protesekirurg.
Å se hele mennesket ikke bare det vonde kneet er en kunst, men den er umulig å praktisere dersom en ikke har forstått at livet kan sette seg i kroppen for kortere eller lengre perioder (for eksempel i kneet) om vi liker det eller ei. Artikkelen din bekrefter bare at du har den egenskapen, å se hele mennesket. Det er en gave å ha som kliniker, når en jobber tett på mennesker med ulike helseplager.
Artikkelen formidler viktig kunnskap, som allerede har nådd mange av oss allmennleger blant annet gjennom Helsebiblioteket. Men vi og våre pasienter erfarer ofte et betydelig press fra fysioterapeuter for å få utført MR ved tilstander som beskrevet her. Det er viktig at denne kunnskapen også tilflyter den yrkesgruppen.
I sin oversikt over atraumatiske kneplager (1) hevder Holtedahl at magnettomografi (MR) brukes for ofte til undersøkelse av kneplager. Vi er ikke enig i disse betraktningene.
Artikkelen nevner ikke at benmargslesjoner (benmargsødem) er en viktig grunn til smerte ved osteoartitt og andre muskel-skjelettsykdommer, og at disse lesjonene sees hos 60-80% av pasienter med artrose, redusert brusktykkelse. I tillegg er de assosiert med sykdomsprogresjon og smerteintensitet (2). Histologisk sees høy benomsetning og økt vaskularisering som sannsynligvis er grunnen til MR-funnene (3). Det er også påvist økt nivå av smertefremkallende angiogene faktorer og proinflammatoriske cytokiner (interleukin-6) i benmargslesjoner.
Holtedahl fronter den tidligere forståelsen av osteoartitt som en ensartet sykdom, men mange nyere studier har etablert at sykdommen består av flere klinisk forskjellige fenotyper. I denne sammenhengen har ultralyd-og MR-undersøkelse en større klinisk betydning enn røntgenundersøkelse, siden disse er essensielle for vurdering av sykdomsaktivitet og medikamentell smertebehandling. Bisfosfonater kan, sannsynligvis via antiangiogene effekter, ha effekt på benmargslesjoner for eksempel ved transient osteoporose. En nylig randomisert placebokontrollert studie viste også klar reduksjon av størrelsen av benmargslesjonene hos pasienter med osteoartritt etter bisfosfonatbehandling (4). Reduksjon var forbundet med 80% reduksjon av smerter på VAS-skår og bedret funksjon på WOMAC-skår.
Røntgenologisk avsmalning av leddspalten er verken en mer sensitiv eller spesifikk undersøkelse for sykdomsprogresjon sammenliknet med MR (5). Benmargslesjoner kan ikke påvises på vanlig skjelettrøntgen, kun ved MR og ultralyd. Ressurser til og etterspørselen etter MR er presset, men å framholde at MR ikke har plass i utredning av knelidelser blir feil. Å begrense tilgang til MR vil redusere vår mulighet for meningsfull diagnostikk av utvikling av nye behandlinger, som er hardt tiltrengt ved osteoartritt.
Litteratur
1. Holthedahl R. Atraumatiske kneplager. Tidsksr Nor Legeforening. 2018;138(5):457-61.
2. Eriksen EF, Ringe JD. Bone marrow lesions: a universal bone response to injury? Rheum int. 2012;32(3):575-84.
3. Shabestari M, Vik J, Reseland JE, Eriksen EF. Bone marrow lesions in hip osteoarthritis are characterized by increased bone turnover and enhanced angiogenesis. Osteoarthritis and cartilage. 2016.
4. Varenna M, Zucchi F, Failoni S, Becciolini A, Berruto M. Intravenous neridronate in the treatment of acute painful knee osteoarthritis: a randomized controlled study. Rheumatology. 2015;54(10):1826-32.
5. Guermazi A. You can rely on radiography when managing OA, but not too much! Nature Reviews Rheumatology. 2017;13:394.
Fink Eriksen og Shabestari har kommentert oversiktsartikkelen om atraumatiske kneplager. Jeg noterer at en av forfatterne i tillegg til et professorat ved Universitetet i Oslo er daglig leder av en privat osteoporoseklinikk med over 2 mill. NOK i driftsinntekter i 2016, uten at dette er oppgitt.
Forfatterne hevder at benmargslesjoner kan påvises hos 60-80% av pasienter med gonartrose. Det nevnes ikke at opptil halvparten av benmargslesjoner viser spontan regresjon (1) eller at slike funn er vanlige også hos dem uten kneplager. Risiko for overdiagnostikk er betydelig ved ukritisk bruk av MR ved degenerative kneplager. En tverrsnittsstudie fra USA av personer over 50 år påviste benmargslesjoner på MR hos 59 % av dem med knesmerter og hos 50 % av dem uten smerter (2). En test som viser positivt funn hos halvparten av symptomfrie har ingen nytteverdi. Den samme studien fant en prevalens av bruskskade hos dem med og uten smerter på henholdsvis 72 % og 68 %, synovitt hos 38 % og 36 % og meniskskade hos 20 % og 25 %. Kun henholdsvis 9 % og 11 % hadde helt normale knær på MR.
Det hevdes videre at det å begrense tilgang til MR vil redusere muligheten for meningsfull diagnostikk og utvikling av nye behandlinger. Det vises i den forbindelse til en studie som viste god effekt av neridronate på knesmerter og benmargslesjoner (3). Studien er interessant, men med kun 56 pasienter som fullførte etter protokoll vil resultatene nødvendigvis måtte replikeres i større studier. Ifølge clinicaltrials.gov foreligger det ingen planlagte eller igangsatte studier av dette preparatet på denne indikasjonen. Det skal bemerkes at tilsvarende studier av andre bisfosfonater ved gonartrose ikke har vist sikre effekter verken klinisk eller radiologisk (4).
Situasjonen per i dag er altså at funn av benmargslesjoner på MR ikke får noen praktisk konsekvens før det foreligger effektiv medikamentell kausalterapi. Rutinemessig bruk av MR i den kliniske hverdag gir sjelden nyttig tilleggsinformasjon ved degenerative kneplager, og stående røntgenbilder er tilstrekkelig i de fleste tilfeller. Dette standpunkt er også i tråd med Helsedirektoratets anbefalinger.
1. Roemer FW, Guermazi A, Javaid MK et al. Change in MRI-detected subchondral bone marrow lesions is associated with cartilage loss: the MOST study. A longitudinal multicentre study of knee osteoarthritis. Ann Rheum Dis 2009; 68: 1461–5.
2. Guermazi A, Niu J, Hayashi D et al. Prevalence of abnormalities in knees detected by MRI in adults without knee osteoarthritis: population based observational study. BMJ 2012; 345: e5339.
3. Varenna M, Zucchi F, Failoni S et al. Intravenous neridronate in the treatment of acute painful knee osteoarthritis: a randomized controlled study. Rheumatology 2015; 54: 1826–32.
4. Davis AJ, Smith TO, Hing CB et al. Are Bisphosphonates Effective in the Treatment of Osteoarthritis Pain? A Meta-Analysis and Systematic Review. PLoS One 2013; 8: e72714.