Implementing a birth registry in a developing country – experiences from Georgia
MAIN POINTS
Previously reported perinatal mortality rates from Georgia are likely to have been underestimated.
The Caesarean section rate in Georgia in 2016 was 43.5 %, which is considerably higher than recommended as a measure to reduce mortality and morbidity.
Both birth weight and gestational age were lower in the Caesarean section group.
Population-based systematic registration of health events is vital for the development of tools to improve health care systems and health care services, and to provide a basis for research. A birth registry records data on pregnant women such as demographics, disease history, antenatal visits and treatment during pregnancy as well as data on the delivery and the newborn infant up to seven days after delivery (1). Several of the Nordic countries established birth registries for the purpose of epidemiological monitoring about 50 years ago in order to facilitate earlier detection of tragedies like the Thalidomide disaster (2).
National birth registries are vital parts of the health care system in many developed countries. Since establishing a birth registry requires a certain infrastructure and financial resources, they are rarely prioritised in less developed nations. Georgia is defined as an upper middle-income developing country, ranked 70 on the Human Development Index in 2016. The republic is located in the Caucasus region with a population estimated at 3 717 100 in 2016 (3). According to a 2014 census, 86.4 % of the population are defined as ethnic Georgians (4). Life expectancy at birth is 75 years and 56.3 % of the population lives in urban areas (5). The fertility rate in Georgia in 2015 was 2.3 (4). The current health care system was introduced in 2013 and includes a universal antenatal health care package. Additional health care services are made available through private health insurance and against out-of-pocket payment.
In Georgia, gynaecologists working either in hospitals or in antenatal out-patient clinics provide all pregnancy care. Basic antenatal care is covered by the state, thus coverage is high (88.3 %) (3) and follows the WHO recommendation with at least four check-ups per pregnancy. Currently, the new recommendations of eight check-ups is being implemented (6). 99.5 % of pregnant women give birth with qualified personnel present in one of the country’s 102 maternity wards (3). The officially reported perinatal mortality (PM) rate (13.8/1000) and the maternal mortality rate (36/100 000) (3) are higher than expected in a country ranked as high as Georgia on the Human Development Index , and where most women have adequate access to health care during pregnancy and delivery. Consequently, the Georgian health authorities, together with Georgia’s National Centre for Disease Control & Public Health, UNICEF and the University of Tromsø - The Arctic University of Norway initiated work to establish the national birth registry in 2014, with the ultimate goal of improving maternal and perinatal health. The Georgian Birth Registry was inaugurated on 1 January 2016, and is the first national birth registry ever to be established in a developing country. UNICEF provided initial funding while the University of Tromsø - The Arctic University of Norway, and Georgia’s National Centre for Disease Control & Public Health, provided technical assistance.
The aim of this article is to assess the quality of selected variables of the Registry and present preliminary results from the first year of registrations (2016).
Material and method
The Georgia Birth Registry
The Georgia Birth Registry uses a unique 11-digit personal identification number allocated to every citizen to link with data from the Service Development Agency at the Ministry of Justice (SDA), which is Georgia’s Civil Registry. A local Georgian IT-company (CiTi), created the entire registry system in 12 months, starting in September 2014. Training and piloting took place in the autumn of 2015 in the capital Tbilisi and several other cities. All clinics that provide antenatal, birthing or post-natal care have access to Internet, and Registry information is submitted online. Information is updated (or added) after every consultation related to spontaneous abortions, pregnancy terminations, antenatal check-ups or deliveries. Doctors or midwives at the respective health facilities are responsible for entering information on all 267 variables. The variables include information on maternal medical and pregnancy history, maternal and paternal characteristics, the current pregnancy, the delivery and on the newborn. Some variables (n = 40) are mandatory, e.g. women’s birth date and estimated blood loss, while the remaining are optional e.g. occupation, or reason for induced abortion.
Health care providers receive reimbursement from the government for each woman who follows the antenatal care programme guidelines, but only if complete information is entered into the Registry (introduced as a mandatory requirement on 1 May, 2016). The registry office, currently staffed by five full-time employees, is responsible for quality control. The Georgia Birth Registry automatically generates birth certificates and accommodates storage of all medical files on an integrated e-health platform.
Data handling and ethical considerations
The Georgia Birth Registry data are owned by Georgia. The University of Tromsø - the Arctic University of Norway has permission to use data for scientific purposes, but assumes no ownership. All personal identifiers (names and identification numbers) in the current dataset have been removed, and randomly generated numbers replace each personal identification number. The identification key has been deleted. The Regional Committee for Medical and Health Research Ethics of Northern Norway has approved the use of the data (2017/404/REK Nord).
Study sample and variables
The final sample comprised 53 236 newborns and 52 399 women. Exclusions are presented in figure 1.
Information on maternal age, number of deliveries, proportions of singleton and multiple births, mode of delivery, gestational age (GA), birth weight and sex of the newborn was extracted from the Georgia Birth Registry. Parity was not included due to substantial amounts of missing data.
The completeness of the birth registry was estimated by comparing the number of newborns in the Georgia Birth Registry with the number of newborns recorded in the Civil Registry. Missing information was calculated, with the expectance of 100 % representativeness for all variables, for each woman and each newborn infant.
Gestational age is primarily reported by last menstrual period (if certain) and secondarily by ultrasound estimate. Perinatal mortality rate was calculated by the number of stillborn infants + the number of live born infants who died before seven completed days / the total number of newborns. The number of perinatal deaths was extracted from the Ministry of Health and the medical department at the National Centre for Disease Control & Public Health because deaths occurring after hospital discharge were not registered in the Georgia Birth Registry at the time.
Statistical analysis
Descriptive statistics of continuous variables are presented as mean values with standard deviations (SDs). Frequencies and percentages are presented for categorical variables. Maternal and newborn characteristics are presented by reported or missing gestational age and by mode of delivery. We used the statistical software R (R Foundation for Statistical Computing, Vienna, Austria), version 3.4.0 for the statistical analyses.
Results
The total number of newborns reported to Georgia’s Civil Registry in 2016 was 56 695 while the total number registered in the Georgia Birth Registry was 53 254 (fig 1), thus the Georgia Birth Registry’s coverage of newborns was 93.9 %. For the selected variables presented in table 1 the following percentages of data were missing: maternal age (0 %); sex (0.4 %); gestational age days (28 %) and birth weight (0.4 %). There was a substantial proportion of missing data on gestational week (27 %) and for that reason we displayed maternal and infant characteristics (by both reported and missing gestational age) in table 1, to make sure that the two groups were comparable.
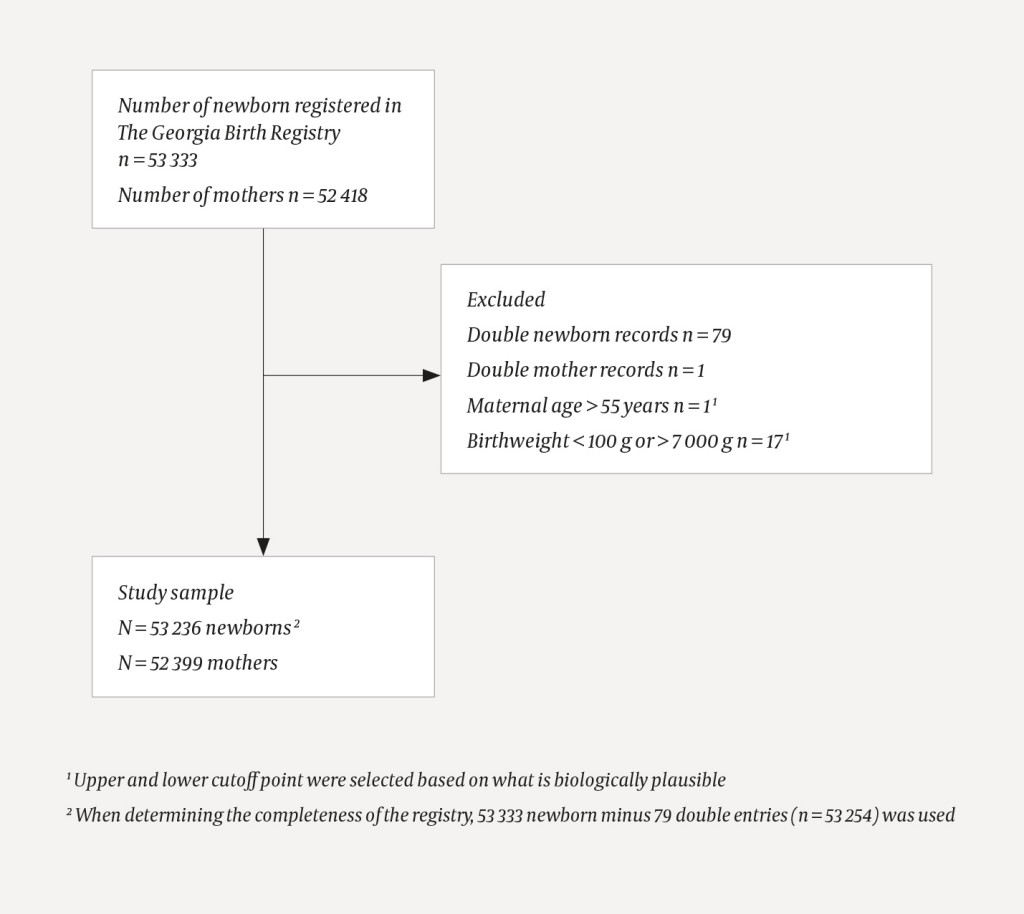
Table 1
Description of maternal and newborn characteristics by reported and missing data on gestational age from the Georgia Birth Registry in 2016.
| Gestational age reported | Gestational age missing | ||
|---|---|---|---|
| Maternal characteristics | |||
| Total number of birthing women, n | 38270 | 14153 | |
| Multiple births, % | |||
| No | 98.5 | 98.1 | |
| Yes | 1.5 | 1.9 | |
| Mode of delivery, % | |||
| Vaginal | 55.7 | 60.1 | |
| Caesarean section | 44.3 | 39.9 | |
| Maternal age (years)1, mean (standard deviation) | 27.1 (5.8) | 27.4 (5.8) | |
| Maternal age1 (years), % | |||
| <13–19 | 0.2 | 8.0 | |
| 20–24 | 28.3 | 26.5 | |
| 25–29 | 31.2 | 31.1 | |
| 30–34 | 20.5 | 21.6 | |
| 35–39 | 9.6 | 10.2 | |
| 40–44 | 2.3 | 2.3 | |
| >45 | 0.2 | 0.2 | |
| Newborn characteristics | |||
| Total number of newborn infants, n | 38839 | 14397 | |
| Multiple birth, % | |||
| No | 97.0 | 96.5 | |
| Yes | 3.0 | 3.6 | |
| Mode of delivery, % | |||
| Vaginal | 55.3 | 59.8 | |
| Caesarean section | 44.7 | 40.2 | |
| Sex, % | |||
| Male | 51.1 | 51.0 | |
| Female | 48.8 | 48.9 | |
| Undetermined | 0.1 | 0.1 | |
| Birth weight2 (g), mean (standard deviation) | |||
| Total | 3255 (610) | 3281 (592) | |
| Male | 3319 (622) | 3329 (602) | |
| Female | 3190 (587) | 3233 (574) | |
| Birth weight2 (g), % | |||
| <1000 | 0.8 | 0.7 | |
| 1000–1499 | 0.8 | 0.6 | |
| 1500–2499 | 5.6 | 4.9 | |
| 2500–4499 | 91.4 | 92.5 | |
| 4500–7000 | 1.3 | 1.3 | |
1Number of missing observations: 159 with reported gestational age and 37 with missing gestational age.
2Number of missing observations: 99 with reported gestational age and 127 with missing gestational age.
Newborns with missing information on gestational age were more likely to be delivered vaginally and were slightly heavier than newborns with reported gestational age (tab 1). Since there were no indications of lower birth weight among newborns with missing gestational age, we applied the same exclusion criteria to all newborn infants (fig 1).
The mean maternal age was 27.2 (standard deviation 5.8) years. A total of 51 568 singletons and 1668 multiples were born. The Caesarean section rate was 43.5 % of the total number of newborns. Of the 53 236 newborn infants, 51.4 % were males and 48.6 % females. There were 742 perinatal deaths registered in 2016, thus the total perinatal mortality was 14.8/1000 newborns, of which stillbirths contributed 10.5/1000. The mean gestational age (standard deviation) was 271.3 (14.2) days. Newborn males had a higher birth weight (standard deviation) than females, 3322 g (617) vs. 3202 g (583) respectively. Newborns delivered by Caesarean section had a lower gestational age, 269.1 (13.0) vs. 273.2 (14.9) days, and lower birth weight, 3233 g (625 g) vs. 3284 g (588 g), than those delivered vaginally (tab 2).
Table 2
Maternal and newborn characteristics by mode of delivery as recorded in the Georgia Birth Registry 2016.
| Vaginal delivery | Missing | Caesarean section | Missing | Total | Missing | ||
|---|---|---|---|---|---|---|---|
| Maternal characteristics | |||||||
| Total number of birthing women | 29820 | 22579 | 52399 | ||||
| Multiple birth, % | |||||||
| No | 99.1 | 97.5 | 98.4 | ||||
| Yes | 0.9 | 2.5 | 1.6 | ||||
| Maternal age (years), mean (standard deviation) | 26.4 (5.5) | 28.3 (6.0) | 27.2 (5.8) | ||||
| Maternal age (years), % | |||||||
| <19 | 9.6 | 5.9 | 8.0 | ||||
| 20–24 | 30.9 | 23.7 | 27.8 | ||||
| 25–29 | 31.9 | 30.2 | 31.2 | ||||
| 30–34 | 19.0 | 23.1 | 20.8 | ||||
| 35–39 | 7.3 | 13.1 | 9.8 | ||||
| 40–44 | 1.3 | 3.6 | 2.3 | ||||
| >45 | 0.0 | 0.3 | 0.2 | ||||
| Newborn characteristics | |||||||
| Number of newborn infants | 30084 | 23152 | 53236 | ||||
| Multiple birth, % | |||||||
| No | 98.2 | 95.1 | 96.9 | ||||
| Yes | 1.8 | 4.9 | 3.1 | ||||
| Sex, % | 126 | 70 | 196 | ||||
| Male | 50.3 | 52.2 | 51.4 | ||||
| Female | 49.7 | 47.8 | 49.6 | ||||
| Undetermined | 0.0 | 0.0 | 0.0 | ||||
| Gestational age (days), mean (standard deviation) | 273.2 (14.9) | 8883 | 269.1 (13.0) | 6004 | 271.3 (14.2) | 14887 | |
| Gestational age (weeks), % | 8603 | 5794 | 14397 | ||||
| 22–31 | 1.9 | 1.6 | 1.7 | ||||
| 32–36 | 4.6 | 8.6 | 6.4 | ||||
| 37–41 | 93.2 | 89.5 | 91.5 | ||||
| 42–45 | 0.4 | 0.4 | 0.4 | ||||
| Birth weight (g), mean (standard deviation) | 135 | 91 | 116 | ||||
| Total | 3284 (588) | 3233 (625) | 3262 (605) | ||||
| Male | 3345 (600) | 3293 (635) | 3322 (617) | ||||
| Female | 3226 (565) | 3169 (605) | 3202 (583) | ||||
| Birth weight (g), % | 135 | 91 | 116 | ||||
| 100–999 | 1.0 | 0.5 | 0.8 | ||||
| 1000–1499 | 0.6 | 0.9 | 0.7 | ||||
| 1500–2499 | 4.0 | 7.3 | 5.4 | ||||
| 2500–4499 | 93.5 | 89.4 | 91.8 | ||||
| 4500–7000 | 0.9 | 1.9 | 1.3 | ||||
Discussion
Our results indicate that the Georgia Birth Registry has a rate of completeness of 93.9 % in its first year compared with the numbers officially reported to Georgia’s Civil Registry. The first results from the Georgia Birth Registry show that the perinatal mortality rate in Georgia in 2016 was 14.8/1000, which is slightly higher than the officially reported rate of 13.8/1000 (3). The probable explanation for the discrepancy in numbers is that the Georgia Birth Registry records the number of infants born in Georgia annually, except home deliveries (-0.5 %), while Georgia’s Civil Registry records the number of newborn citizens.
This situation may occur in countries that do not have a well-functioning birth registry. Infants may be legally registered as citizens even if they are not born in Georgia, as long as one of the parents is a Georgian citizen (7). Parents may choose to do so because there are advantages to being Georgian, for example that Georgians may visit the Schengen area without a visa, a convenience not shared by any of the surrounding countries. Consequently, the true perinatal mortality rate is probably somewhere between 13.8/1000 and 14.8/1000, but closer to the latter.
The Caesarean section rate in Georgia is 43.5 %, which is 2 to 3 times higher than in the Nordic countries, where Caesarean section rates vary between 15 and 21 % (8). Although WHO no longer recommends a specific Caesarean section rate, proportions above 10 % are not associated with a reduction in maternal and perinatal mortality (9). The high Caesarean section rate is a governmental challenge because a caesarean delivery is more expensive than a vaginal birth, but it is also a burden for the women, since having one Caesarean section predisposes for Caesarean section in later deliveries (8).
The mean gestational age in Georgia is 271 days, 4 days shorter than in for example Norway (10). Newborns are much more likely to be delivered by Caesarean section in Georgia (where the mean gestational age in the Caesarean section group was only 269 days) than in Norway where the Caesarean section rate was 16.1 % in 2016 (11). If everything else was equal between the two countries, these differences could indicate that there is an association between high Caesarean section rates and lower gestational age. Unfortunately, our cross sectional design and the fact that we did not have access to reliable data on the clinical indication for performing Caesarean section in Georgia, restrict our possibility to do so. However, our results highlight that the causes and consequences of the high Caesarean section rate in Georgia need future attention.
The quality of the Georgia Birth Registry data is acceptable and in agreement with well-established international findings: i) the proportion of male newborns is slightly higher than the proportion of females (12); ii) higher birth weight among male compared to female newborns (13) and iii) 7 % of newborns had a birth weight <2500 g (14). The employees at the registry office perform continuous quality control of data in the Georgia Birth Registry. Additionally, there are several hundred built-in quality assurance measures e.g. ranges of acceptable values.
The Georgia Birth Registry has only been operational for one year, and system weaknesses are expected. Hospitals have reported some lack of motivation among staff to enter information into the Georgia Birth Registry as this is considered additional work without benefits to themselves or their patients. Therefore, there are substantial amounts of missing values for some optional variables, such as parity and number of fetuses. The birth weight variable also displayed inconsistencies with a disproportionate number of birth weights rounded off to the nearest hundred grams. Ideally the Wilcox and Russel method (or an adapted version) (15) should have been applied in order to double-check probable birth weight outliers routinely. Several major upgrades were implemented in the Georgia Birth Registry during May and June 2017. The same will apply to the Wilcox and Russel method as soon as sufficient data material is available.
During the development period, we discovered the importance of establishing national ownership of the final product. In addition, the Georgia Birth Registry has been dependent on a national and institutional initiative that has created enthusiasm and dedication among local and national health authorities that use the registry for statistics and quality improvement purposes. These are all prerequisites for the sustainability of a system such as the Georgia Birth Registry, a finding which finds strong support in The Lancet series “Civil registration and vital statistics” from 2015 (16).
Conclusion
The Georgia Birth Registry achieved 93.9 % coverage of newborns in its first year of operation. Selected core variables display reasonable agreement with established knowledge, however; important indicators, such as parity and gestational age, still need further improvement. The higher than previously reported perinatal mortality rate and the large proportion of Caesarean section need further attention.
UNICEF funded the creation of the birth registry system and the Georgian health authorities fund the on-going operation of the The Georgia Birth Registry. There are no conflicts of interest. We are grateful to Nino Berdzuli (Deputy Minister of Labour, Health and Social Affairs); Eka Pestvenidze (Deputy Minister Advisor at Ministry of Labour, Health and Social Affairs), Maia Kereselidze, Levan Kandelaki and Natalia Qachlishvili at the The Georgia Birth Registry office, and would also like to thank the rest of the staff at the National Centre for Disease Control & Public Health, and all the health clinics, for their patience and positive attitude. This article is part of the series ‘Global Health in the Era of Agenda 2030’, a collaboration between Norad, the Centre for Global Health at the University of Oslo and The Journal of the Norwegian Medical Association. The views and opinions expressed in the articles are those of the authors only.
- 2.
Folkehelseinstituttet. Medisinsk fødselsregister – Historiske røtter. https://www.fhi.no/hn/helseregistre-og-registre/mfr/medisinsk-fodselsregister--historis/ (14.6.2017).
- 3.
Gamkrelidze A, Kereselidze M, Tsintsadze M et al. Health care – statistical yearbook 2015 – Georgia. Tbilisi: National centre for disease control and public health, 2016
- 4.
National Statistics Office of Georgia. Statistical yearbook of Georgia. Tbilisi: National Statistics Office of Georgia, 2016.
- 5.
United Nations. Human Development Reports – Georgia: United Nations Development Programme 2016. http://hdr.undp.org/en/countries/profiles/GEO (7.6.2017).
- 6.
World Health Organization. New guidelines on antenatal care for a positive pregnancy experience. http://www.who.int/reproductivehealth/news/antenatal-care/en/ (7.6.2017).
- 7.
State Commission on Migration Issues. Acquisition of georgian citizenship. http://migration.commission.ge/index.php?article_id=165&clang=1 (14.6.2017).
- 9.
World Health Organization. WHO Statement on caesarean section rates. http://apps.who.int/iris/bitstream/10665/161442/1/WHO_RHR_15.02_eng.pdf?ua=1 (7.6.2017).
- 10.
Folkehelseinstituttet. Medisinsk fødselsregister (MFR) og Abortregisteret. Standardstatistikk. F6: Svangerskapsvarighet: 2016. Folkehelseinstituttet 2017. http://statistikk.fhi.no/mfr/ (30.10.2017).
- 11.
Folkehelseinstituttet. Medisinsk fødselsregister (MFR) og Abortregisteret. Standardstatistikk. F10c-2: Keisersnitt utført. Folkehelseinstituttet 2017. http://statistikk.fhi.no/mfr/ (30.10.2017).
- 13.
Kramer MS. Determinants of low birth weight: methodological assessment and meta-analysis. Bull World Health Organ 1987; 65: 663 - 737. [PubMed]
- 14.
United Nations Children’s Fund. Low birthweight: Country, regional and global estimates. Report. New York, NY: Unicef, 2004.
Artikkelen fortel om eit arbeid og initiativ som er svært viktig! Vil dette kunna overførast til andre land, f.eks i Afrika?
Ein liten detalj: 51,4% gutar og 49,6% jenter vert 101%. Det skulle vel vera 48,6% jenter?
Takk for at vi ble gjort oppmerksom på andelen gutter og jenter. Det skal selvfølgelig være 48,6% jenter.
Et slik nasjonalt fødselsregister kan i prinsippet overføres til alle land dersom noen kriterier er oppfylt. Det viktigste vil være at kvinnene i landet det gjelder oppsøker kvalifisert hjelp både før og under fødselen slik at data faktisk kan samles inn. Det må også være en viss statlig kontroll med disse helseytelsene slik at det kan innføres retningslinjer som alle må følge. Like viktig er det at dette er noe landet virkelig ønsker å opprette og drive selv på lang sikt.
Dessverre kjenner vi ikke spesifikt til forekomsten av disse kriteriene i afrikanske land, men det er flere land der som er sammenlignbare med Georgia på Indeks for menneskelig utvikling.