In Norway during the last decade we have seen a continuous increase in the number of organ donations from deceased donors. Despite this increase there is still a considerable imbalance between the need for and the number of available organs. The total potential for organ donations in Norway is not known.
In 2007, the Government adopted a target to achieve 30 donations per million inhabitants. The time limit for achievement of this goal has not been specified. In a report from 2008, the Ministry of Health and Care Services pointed to the need for intensified training of health personnel regarding the donation process and for improvement of the organisational framework within the health enterprises (1). Since 1992, the Norwegian Resource Group for Organ Donation (NOROD) has played a key role in the efforts to increase health workers’ knowledge and skills in this field, and the Directorate of Health has assigned the task of upgrading the training programmes to the group.
The doctors’ knowledge about organ donation, attitude to it and ability to relate to the potential organ donor and his or her next of kin may be decisive for obtaining consent to an organ donation (2) – (7). A review article published in 2009 (5) showed that specific skills in the person who provides information and inquires, as well as the timing of the inquiry, may have a greater effect on the likelihood that the next of kin will provide consent for an organ donation than legislation and regulations. Frequent contact with staff, good communication, the structure of the inquiry process and socio-emotional issues are key factors (7).
In 2006, Sanner showed that many Swedish anaesthesiologists felt that they had insufficient competence in clinical death diagnostics, and that more than half took a neutral stance when asking family members. A positive attitude to organ donation in the person who makes the inquiry leads to a positive answer far more frequently than a neutral stance (8).
There are no Norwegian studies available of how Norwegian intensive-care doctors and neurosurgeons perceive their encounter with the patient and his or her next of kin during the process of organ donation and how they relate to this situation. Neither has the need for training in medical treatment and communication in the context of organ donation been further investigated.
The purpose of our study was to investigate:
What experience doctors who have medically treated potential organ donors have had with respect to next of kin in this situation.
The doctors’ need for training in communication and medical treatment in the context of organ donation.
Material and method
A questionnaire-based survey comprising all doctors at the intensive-care units in all 28 donor hospitals and all neurosurgeons/trainee candidates in neurosurgery in Norway was undertaken in late autumn 2008 (first distribution and first reminder) and the winter of 2009 (second reminder). A questionnaire, which had been prepared by Margareta Sanner and colleagues in Sweden (3), was translated and adapted to Norwegian conditions by the authors.
The following background variables were identified: age, gender, specialisation (neurosurgery, intensive-care medicine/anaesthesiology, other specialisation, trainee) and place of work (local hospital, university hospital).
Experience of organ donation was mapped by two questions: «How many times have you treated a potential donor?» and «How many conversations have you had with the next of kin?» Response alternatives to these questions are shown in Figures 1 and 2.
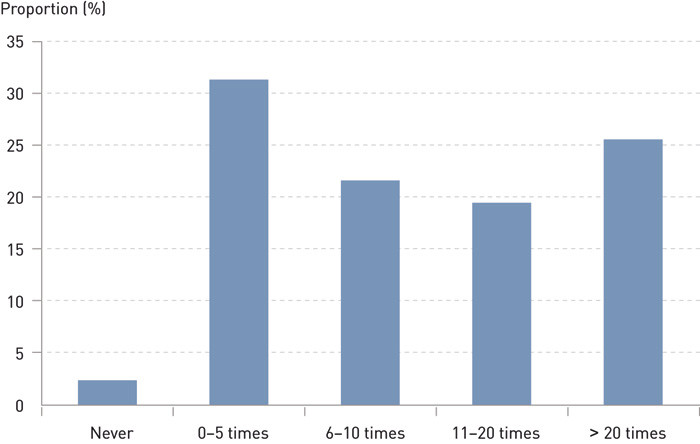
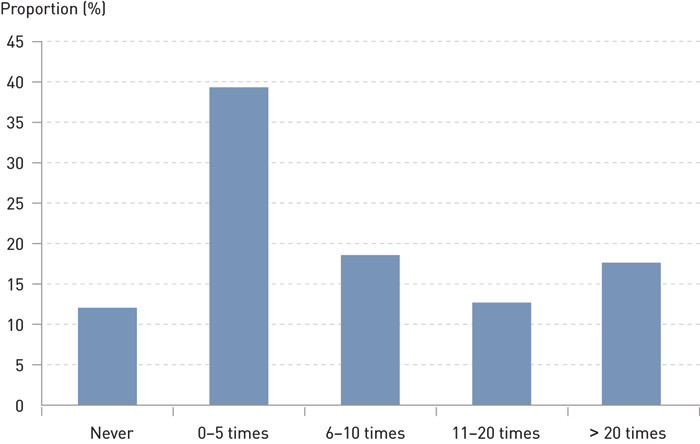
Key aspects of posing the question about organ donation were identified with three questions: «When do you usually raise the issue of donation, if the next of kin have not done so themselves?» (five response alternatives), «What attitude do you normally attempt to assume when asking the next of kin about organ donation?» (four response alternatives) and «Have you raised the issue of organ donation on a second occasion if you received a negative answer in your first conversation with the family members?» (four response alternatives). The response alternatives are shown in Table 1.
Table 1:
Reported practices among doctors in intensive-care units, neurosurgeons and neurosurgery trainees in matters related to organ donation. Distribution of responses in percentages.
| Questions and response alternatives |
Response distribution (%) |
| When do you usually raise the issue of donation, if the next of kin have not done so themselves? (N = 391) |
|
| After angiography |
9.5 |
| Time passes between the notification of death and the inquiry. |
15.3 |
| Simultaneously with the notification of death |
15.6 |
| When there is certainty that the patient will not survive. |
19.4 |
| It varies |
40.2 |
| Which attitude do you normally attempt to assume when asking the next of kin about organ donation? (N = 423) |
|
| Negative to donation |
0 |
| Cannot say¹ |
13.7 |
| Pro-donation |
44.0 |
| Neutral |
42.3 |
| Have you raised the issue of organ donation on a second occasion if you received a negative answer in your first conversation with family members? (N = 403) |
|
| Usually |
1.5 |
| Sometimes |
8.2 |
| Rarely |
21.6 |
| Never |
68.7 |
| [i] | |
[i] ¹ Those who have responded that they cannot say are those who have never been in this situation.
The respondents were asked to report their learning needs in four medical fields:
Identification of potential organ donors
Medical treatment of the donor
Clinical diagnostics of complete cessation of brain circulation
Carrying out the donation process
The response alternatives provided were «no need», «some need», «need» and «great need».
Learning needs pertaining to communication were reported in five fields:
Empathic communication
Listening
Breaking bad news
Obtaining consent for donation
Supporting the next of kin in crisis and grief
The response alternatives were identical to those for medical issues.
All respondents were asked whether they had attended NOROD courses.
The statistical analyses were carried out using SPSS. The sample was described by means of a descriptive analysis. We checked for any differences in responses according to the type of hospital where the respondents were employed.
The study has been reported to Norwegian Social Sciences Data Services.
Results
The sample
A total of 815 questionnaires (206 to local hospitals, 609 to university hospitals) were sent to doctors in the intensive-care units in donor hospitals, to neurosurgeons and trainee candidates in neurosurgery (29 per cent of which were women). Altogether 435 doctors returned a completed questionnaire. 30 questionnaires were returned because the addressee had left the hospital, and 20 doctors refused to participate, most of them because they were not involved in organ donation. The response rate amounted to 55.4 per cent, and was relatively similar for both genders as well as for local and university hospitals. The average age of the respondents was 45.9 years (standard deviation 10.2 years).
There was a large range with respect to the period of time the doctors had worked as specialists, from 0 – 35 years (median 5 years). Altogether 63.1 per cent were specialists in intensive-care medicine/anaesthesiology, 8.4 per cent in neurosurgery, 5.1 per cent had another specialty and 23.4 per cent were trainee candidates. A total of 34 per cent of the respondents had attended NOROD courses.
Experience from organ donation and practices in conversations with relatives
Figures 1 and 2 and Table 1 present the responses to the individual questions pertaining to the doctors’ experience with organ donation, conversations with next of kin and the practices the doctors reported using when asking for consent. More than half of the doctors had limited experience with organ donation. A total of 42.3 per cent assume a neutral attitude when asking the next of kin for consent. Those who have responded that they cannot respond are those who have never been in this situation. The majority (68.7 per cent) did not ask for organ donation a second time if they had received a negative response to their first inquiry.
Learning needs
In Figures 3 and 4 the learning needs within each response field are presented as well as the proportion who reported a need or a great need in the area. Nearly half of all doctors have a moderate to great need for training with regard to medical issues as well as communication.
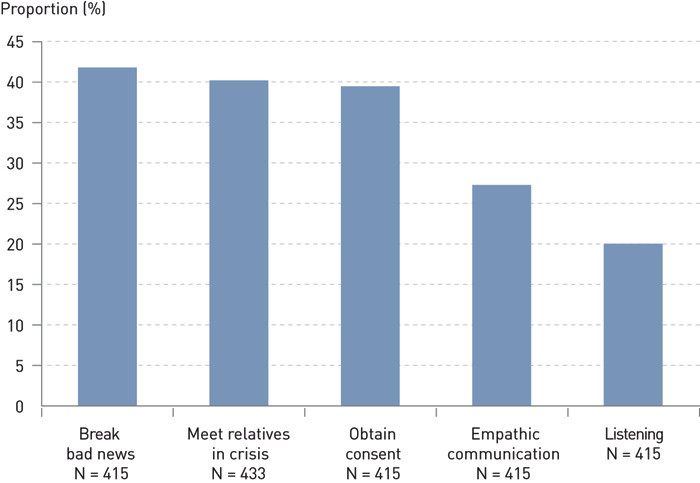
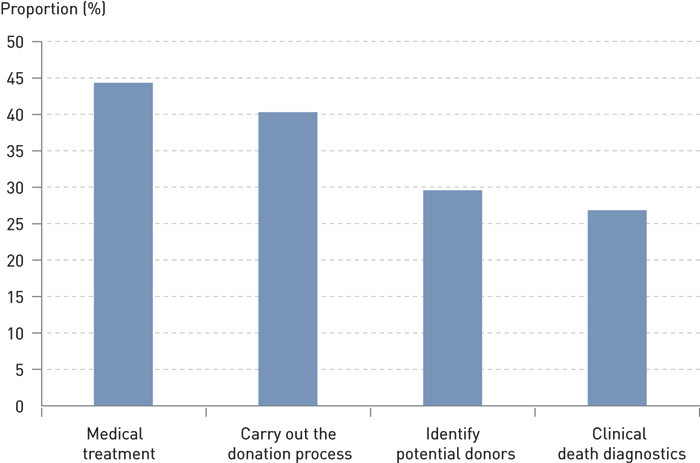
Discussion
The study shows that there is reason to assume that many doctors in Norwegian intensive-care units have little experience in treating potential organ donors and in communicating with the next of kin in potential donation situations. This may have an impact on practice, since skills and experience in these areas have been documented to be significant factors in identifying potential donors, treating the potential donor/the donor in an appropriate manner, attending to the relatives in this situation and obtaining consent for a donation (4) – (6).
Many doctors reported to have a considerable need for training with regard to medical issues as well as to communication with the next of kin. The learning needs were associated with deficiencies in terms of skills and experience. Another study from a Norwegian intensive-care unit in which considerable attention had been devoted to organ donation showed that the doctors were very confident about their own abilities in this area (6). Our findings indicate that this is not representative of Norwegian doctors in general. We found no differences between the 28 hospitals included in the study. Seen together, the studies appear to indicate that training in the field of organ donation is important, and that the needs are substantial.
Many doctor’s reports of how they communicate indicate that they do not have a form of communication which is commensurate with what we know can increase the likelihood of obtaining consent for organ donation. For example, research shows that some time should elapse between notification of death and any inquiries with respect to organ donation (5), but only 11 per cent of the doctors reported always allowing some time to pass between these two events, and more than 50 per cent responded that this would depend on the circumstances. It seems as though many doctors lack a strategy for communication with relatives and that they were not familiar with or did not follow evidence-based recommendations. Another Norwegian study shows that doctors find it difficult to practise evidence-based medicine – they prefer to consult with a colleague rather than seek advice from recent research literature (9). This appears to apply to organ donation as well – established practices within the department are continued. If routines are to be changed, new knowledge most likely needs to be supplied from outside.
Many of the doctors (42.3 per cent) responded that they assume a neutral attitude when asking for consent for donation of an organ. A neutral attitude is not recommended by research literature, nor by Norwegian political authorities. A directive from the Ministry of Health and Care Services instructs practitioners to ask the question about a donation «with the aim of obtaining a positive answer» (10). Furthermore, the directive states that «health personnel who are charged with this task vis-à-vis the next of kin must have good skills in empathy and communication».
Communicating a pro-donation attitude in an empathic manner can be learned. The literature also recommends that the inquiry about a donation can be repeated even though the next of kin initially have responded negatively. This requires great empathy. A rejection can be perceived as final or provisional. A quick rejection can be a rash, temporary answer given in the heat of the moment. This ought to be explored more closely, to allow the inquirer time to understand the implications of the response, as well as give the responder an opportunity to think through the matter. Exercises in communicating a pro-donation attitude and exploring temporary rejections have the potential to promote more considered decisions and open for opportunities to more frequently achieve positive responses (5).
Few doctors had attended NOROD’s training courses. Consideration should be given to how to better spread this training opportunity. Formalisation of a scheme involving teams consisting of a doctor and one or two intensive-care nurses who are responsible for donors should also be considered. As early as in 2003, it was pointed out in this journal that «much of the work associated with organ donation is undertaken as teamwork involving doctors and nurses» (11).
The limitations of this study are mainly associated with the low response rate. We received responses from a little more than half of all the doctors who were working in the intensive-care units of the donor hospitals in 2008 – 2009. There is reason to assume that the doctors who were most experienced and skilled are overrepresented, since they will probably have the greatest interest in participating. It is also conceivable that some of those who did not want to participate have responded that they were not involved in organ donation on a daily basis. This may indicate that the need for training is greater than indicated here. Another limitation is that the study has targeted the individual doctor’s self-reported practices, and not the institutional routines, organisation and training in each hospital department. In future studies, self-reporting ought to be linked to observation and registry data.
Conclusion
Our study indicates that there is a need to expand the opportunities for training to ensure that doctors have sufficient expertise in the field of organ donation. Information about training opportunities should be better disseminated and changes should be made to the organisation of skills development. One possibility would be for the entire intensive-care unit to increase their expertise, another would be build up expertise in separate teams consisting of the doctor and nurses who are responsible for the donor. The choice of solution will depend on a number of factors, such as the size of the department and the frequency of organ donations at the hospital.
Acknowledgement The Norwegian Directorate of Health contributed the funding for the distribution of questionnaires. We wish to thank the doctors who responded, as well as Tom Eide and Bjørn Lien for their detailed comments to the draft manuscript, and Thore Egeland for checking our statistical analyses.
Tabell
| Main message |
|
- 1.
Follesø G. Tiltak for å øke antall organdonasjoner – rapport fra en arbeidsgruppe nedsatt av Helse- og omsorgsdepartementet. Oslo: Helse- og omsorgsdepartementet, 2008: 1 – 31.
- 2.
Alnæs AH. Minding matter. Organ donation & medical modernity's difficult decisions. Doktoravhandling. Oslo: Universitetet i Oslo, 2002.
- 5.
Simpkin AL, Robertson LC, Barber VS et al. Modifiable factors influencing relatives’ decision to offer organ donation: systematic review. BMJ 2009; 338 (apr21 2): b991.
- 10.
Helse- og omsorgsdepartementet. Rundskriv I-6: Om regelverket som gjeld organdonasjon og samtykke. Oslo: Helse- og omsorgsdepartementet, 2008.
- 11.
Hanoa R. Organdonasjon i samarbeid med avdødes pårørende. Tidsskr Nor Lægeforen 2003; 123: 1110. [PubMed]