Human beings have unique characteristics that distinguish them from all other known organisms – a capacity for self-reflection, for designing sophisticated symbolic structures, for attaching metaphorical concepts to experiences and for building models and categories with the aid of the imagination. Nevertheless, the traditional scientific methodology of biomedicine fails to take account of the self-aware, meaning-seeking, purposeful and relational nature of humans (1). Doctors therefore lack theoretical understanding of how experiences associated with self-image, relations and values become «inscribed» in the body.
During the past decade, empirical documentation has demonstrated that experience – the information that an individual acquires during a lifetime of sensing and acting – is of fundamental biological relevance. Unfortunately, such experience does not lend itself easily to standardised interpretation; it is always an experience of something for someone, in a unique context (2). In this article, we attempt to exemplify the importance of subjective experiences for health. In so doing, we emphasize the need to revise the theoretical foundation of medicine, and the necessity of integrating this new knowledge into clinical practice, research, teaching and health policy.
Material and method
Many disciplines, including evolutionary biology, ecology, embryology and physiology, have investigated variable traits of organisms. For a long time this fragmented research resulted in differing views on the organism’s significance. In recent years, more emphasis has been put on understanding the integrity of the organism as a living whole, be it a bacterium or a human being (3). With this integrative understanding as our starting point, we present knowledge that reveals the interaction between the human body (biology) and life experience (biography) in the broadest sense.
The reference works we have selected substantiate the notion that the human organism is integrated with its surroundings and relational in its nature. We include studies from epidemiology, somatic and psychiatric clinical medicine, genetics, microbiology, immunology and neuroscience. We also include works from new, overarching disciplines such as neuro-endocrinology and psycho-neuro-endocrino-immunology, as well as analyses in the fields of biosemiotics, evolutionary biology, theory of science and philosophy. The complexity and breadth of the subject did not allow for systematic literature searches.
Results
Recognition of the fact that all organisms actively interpret meaningful signals from the external and internal environment can be found in the ecological works of the biologist Jakob von Uexküll (1864 – 1944) from the first half of the 20th century. His ideas gave rise to diverse fields of investigation, including work on animal behaviour by Konrad Lorenz (1903 – 1989), philosophical investigations of human action by Martin Heidegger (1889 – 1976), and current works in the field of biosemiotics. Biosemiotics (from the Greek semeion – sign) is the analysis of active communicative life processes mediated by means of signs, and thus entailing interpretation (4). Since all interpretation – irrespective of the level of consciousness – proceeds in a context coloured by previous experience, context and interpretation emerge as central concepts for understanding and explaining the organism’s observable phenotypes (4).
Genetic expression is influenced by experience
The science of «epigenetics», which is mentioned with increasing frequency in medicine (5), is concerned with the way experiences enable contextual «programming» of genetic material. Genes are regarded less and less as determinative templates. Instead they are looked upon as dynamic agents in an organism’s life, capable of responding to both external and internal stimuli. Accordingly, which part of the DNA becomes expressed – and under which conditions – will depend on experienced and interpreted impressions (6). It is therefore more appropriate to speak of genetic predisposition than genetic predestination (7).
In contrast to mutational changes in the DNA base sequence, epigenetics relates to temporary (relatively stable, but potentially reversible) changes in genetic expression without changes in the DNA. Several mechanisms, including DNA methylation, histone modification and non-coding RNA, can trigger or block gene expression. Until quite recently much of the literature focussed on epigenetic modifications occurring during pregnancy and early childhood. However, recent data suggest that these processes may be active from the time of conception – or even before – and throughout the individual’s lifetime. In addition, increasing evidence suggests that epigenetic «programming» can make a substantial contribution to the development of the complex, lifestyle related diseases so prevalent in our time (7) – (13). Epigenetic modifications have proved to be transmissible to future generations (11), although the practical consequences of these observations have yet to be determined. Still, the potentials are high, and some researchers claim that recognition of the epigenetic impact of social influence on the human organism will not merely change medicine fundamentally; it will also reshape the social sciences and the humanities (13).
Some scientists claim that epigenetic mapping is likely to provide answers to more questions relating to health and disease than genome mapping has done. In January 2010, the International Human Epigenome Consortium (IHEC) was launched for the purpose of mapping epigenetic marks in the genome. The journal Nature followed up with an expert commentary which stressed that the human genome is «singular and finite», while the epigenome is almost infinite, as it «changes in different states and different tissues» (14).
Convergent knowledge from several fields of research
Growing research activities in the last 10 – 20 years, at the interfaces between psychology, immunology, endocrinology, microbiology and the neurosciences, have resulted in studies which – with increasing levels of precision – contribute to a picture of the human biology as «saturated» with experience and interpretation (15, 16). In the following we present examples which show that, and to some extent how, existential experience can impact human physiology and create or exacerbate biological vulnerability in individuals:
Psychosocial stress during pregnancy may affect the unborn individual’s biological constitution through the mother’s hypothalamic-pituitary-adrenal axis (HPA axis) and epigenetic effects; a pregnant woman’s traumatic experiences in her own childhood may be reflected in both her own adult life (17) and in the HPA regulation of her unborn child (18). In addition, psychosocial stress in the woman represents a direct risk to the pregnancy outcome itself (19 – 21).
The chromosomes’ telomeres (stabilising ends) can be injured by certain types of experience. Several studies have found a relationship between chronically debilitating caregiver situations that a person cannot escape from (for example, being the caregiver for a seriously/chronically ill child or a close family member with longstanding Alzheimer’s disease), and shorter telomeres, which are regarded as an expression of early cell ageing (22 – 24).
Relational experiences appear generally to affect human immune systems, as reflected in an altered cytokine balance and a changed degree of inflammatory response (25). Humans subjected to stress where they are at risk of «losing face» (social evaluation threat) have, for example, been shown to «respond» with a pro-inflammatory cytokine balance (26). Similar responses have been found in experiences of unfairness at the workplace (27) and other experiences of threat, powerlessness and loss. Research also describes, with increasing precision, the physiological correlates of the emotions. Measured in terms of cortisol and cytokine levels, anger is for example associated with metabolic mobilisation, while the biology associated with fear and shame is characterized by physiological and social passivity (28). It has also been demonstrated that stressful caregiving responsibilities and conflict-filled relationships may lead to lowered antibody response to vaccines (29, 30).
New integrated stress research – the concept of allostatic overload
Long-term overtaxation of the physiological adaptability of human beings may lead to health impairment. This phenomenon, called «allostatic overload» (31) – (33), is a consequence of physiological «wear and tear» due to strong and/or persistent threats to an individual’s existence or integrity (the word encompasses both mental and physical aspects). The human body’s reaction to stressors, which in our culture can be classified as physical (e.g. undernourishment, overfeeding, malnutrition, pollution, lack of sleep, lack of exercise, infections, noise) prove to converge at the same biological «level» as stressors we would classify as psychosocial (e.g. a life characterised by threats, neglect, abuse, poverty or overwhelming caregiving burdens): Both categories of stress can contribute over time to the development of autonomic dysfunction, changes in the immune system, chronic low-grade inflammation, endocrine disruptions and accelerated cell aging, measured as telomere shortening (Box 1).
Allostatic overload may be quantified by measurement of autonomous, hormonal, immunological and genetic variables:
Cardiovascular readings (blood pressure, pulse rate etc.)
Lung function tests (PEF, spirometry)
Hormone levels (cortisol, DHEA-S, A, NA etc.)
Inflammation markers (CRP, IL-6, TNF, fibrinogen etc.)
Glucose metabolism (blood sugar, HbA1c)
Lipid metabolism (TG, HDL, LDL, etc.)
Obesity measures (WHR, BMI etc.)
Chromosome-related variables: telomere length and telomerase level
Biological parameters that form part of an evaluation of allostatic load in the scientific models and studies that have been discussed (32). Abbreviations: PEF – peak expiratory flow; DHEA-S – dehydroepiandrosterone sulphate; A – adrenaline; NA – noradrenaline; CRP – C-reactive protein; IL-6 – interleukin 6; TNF – tumour necrosis factor; HbA1c – glycosylated haemoglobin; TG – triglycerides; HDL – high density lipoprotein; LDL – low density lipoprotein; WHR – waist-hip ratio; BMI – body mass index
Chronic metabolic disturbances related to allostatic overload appear to contribute, at least partly through epigenetic mechanisms, to the development of the major, complex diseases of our time – cardiovascular disease, overweight, diabetes, chronic obstructive pulmonary disease, other immunological and inflammation-driven diseases, osteoporosis, depression, anxiety, so-called behavioural disorders, substance dependence and other complaints classified as psychiatric, cognitive complaints, adverse pregnancy outcomes in the form of premature births and low birth weight, pain syndromes and chronic fatigue etc. (31) – (37). The concept allostatic overload thus enables an entirely new understanding of composite pictures of biological defects and failures which have traditionally been perceived as concomitant, but different disorders and diseases; in other words so-called co- or multimorbidity (38). The overall degree of health hazardous stress, expressed in terms of loss of control and lack of mastery of one’s own life (39), can well be considered in light of the individual’s rank in the social hierarchy. In combination, epigenetics and the allostasis concept may contribute substantially to a deeper understanding of the social gradients in morbidity and mortality (40). The extent to which social gradients impact people’s health is well documented, for instance by the epidemiological Whitehall studies in England (41). Through the concepts of epigenetics and allostasis, the well-established epidemiological concept «social gradients in health», has acquired a pathophysiological counterpart, expressed in the term «the biology of disadvantage» (42).
Recent trauma research provides insight into how detrimental childhood experiences may lead to toxic stress (36) which is reflected in disturbed maturation of brain structure in the developing individual. Neuroimaging studies have linked such structural changes (gray and/or white matter alterations) to experiences of verbal abuse, harsh corporal punishment and sexual abuse (43). The plasticity and vulnerability of the brain appear to vary with the individual’s age; the detrimental potential of adverse experiences will depend on when they occur and how long they last (43).
The brain appears to remain receptive to relational effects throughout life. Fortunately, favourable brain changes can also occur, in response to experiences which promote healing and health (salutogenesis). A number of studies have documented structural changes in the brain associated with successful psychotherapy (44). On a more general level, a recent meta-analysis demonstrated that strong social relations provide as good protection against premature death as smoking cessation, and this statistical protection is numerically greater than the risk associated with, for example, obesity and physical inactivity (45). This protective effect is independent of age, gender and a number of other factors, and is therefore unlikely to be limited to sub-groups.
Discussion
Emerging knowledge of how experience «inscribes» itself in the human biology demonstrates how scientific methods pertaining to the natural sciences are currently being applied to develop new knowledge about issues traditionally regarded as «humanistic» in nature – for example how experiences of care or neglect, trust or treachery, belonging or loneliness, power or powerlessness, justice or injustice, can be linked to maintenance of health or development of disease. Experienced clinicians have long acknowledged the significance of these fundamental, existential living circumstances, but up to now biomedicine has lacked formal scientific concepts for relating to this interdependence in a consistent manner. The new research offers one means of integrating the natural sciences’ and the humanistic sciences’ understanding of human health and disease, and can, accordingly, challenge the notion of «two cultures» in science in general (46) and in medicine in particular (47).
Health-promoting work – a social responsibility and a medical task
The fact that experiences have a fundamental influence on human biology must be taken into account by a scientifically responsible medical community aiming to pave the way for promotion of public health. The creation of decent living conditions for today´s children and future generations is central in this connection (36, 37, 48). But also the health of adults needs to be considered from a perspective involving more than traditional «lifestyle factors» such as diet, smoking and exercise (40, 42). Doctors have an important responsibility to disseminate and further develop this broader knowledge. The significant impact of experiences on the body?s physiology will have to be reflected in future preventive medical strategies, particularly with respect to the complex disorders that are the most costly medical conditions in western societies today.
Medical theory that does justice to human nature
The recent developments in medical knowledge presented in this paper are incompatible with biomedicine’s traditional and pragmatic divide between body and mind (soma and psyche). Not only is the well-established theoretical distinction between somatic and mental disorders challenged (49, 50) and thereby the distance between psychiatric and somatic departments, but also the subdivision into somatic organ-based medical specialities. This last argument finds support in the work of an American research team that maintains that depression should be understood as a whole body disease, with both mental and physical causes and manifestations (51) which also have considerable clinical overlap with both cardiovascular disease and other disorders (52). A well developed professional ability to integrate biological and biographical information may prove particularly fruitful in encounters with patients who present complex and extensive expressions of disease that are resistant to treatment.
An integrated medical theory about human beings must take as its starting point that every individual is conceived with a given biological predisposition, which gradually becomes shaped by experience, understanding, interpretation and action, influenced by physical environmental factors and woven into relationships with significant others in a society with culturally constituted values (Fig. 1). We hardly need more empirical detail to claim with authority that (and suggest an explanation as to how) all these factors affect people’s health-related development. There is a need for a basic medical theory that recognises
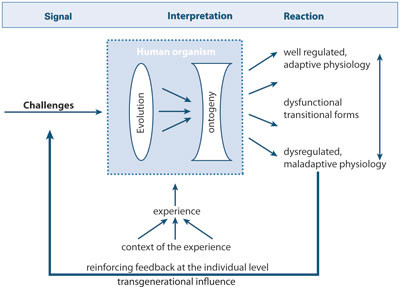
the status of the individual as a historically and culturally situated unique subject with inherited premises that are modulated by experience, individual and collective
the individual’s life-long development (ontogeny), where transgenerational (epigenetic) and evolutionary (phylogenetic) aspects also play a part (53, 54), and
Evidence-based medicine of the future
Medical doctors of the future must have access to theoretical models which acknowledge that every single human being incorporates both biological and historical experiences (1, 2, 52)(52–54), (58–60). Elaboration of such theoretical knowledge requires the development of a scientific terminology that conceptualises body and mind as undivided and interacting. Medical education and training must, accordingly, include the teaching of epistemology (theory of knowledge), a subject that is virtually unknown to today´s doctors.
The emerging empirical knowledge reviewed in the present paper must be integrated into the authoritative knowledge base of medicine. Only then can the patient’s subjectivity (and access to it) be given a necessary and verifiable status (60) – (62). Human subjectivity is not only absent from contemporary evidence-based medicine, it is in fact explicitly eliminated by the mathematical analyses performed during assembly of evidence. However, work with biographical data requires appropriate knowledge, training and organisational preparation (Box 2). In biographical work, as in work with biological data (63), there are inherent possibilities for interpretational error.
A concrete example of how knowledge about the health effects of experience can be incorporated in clinical practice is provided by the Kaiser Permanente Foundation in San Diego, California. The foundation has since 1993, in addition to recording their members´ (patients´) conventional medical histories, also systematically elicited and recorded their eventual trauma histories. On the basis of the resulting data and in collaboration with the Centers for Disease Control and Prevention (CDC) in Atlanta, a group of the foundation´s doctors have produced extensive scientific documentation of the clinical relevance of traumatic childhood experiences. This study is called the Adverse Childhood Experience Study (ACE Study) (62). There are currently more than 60 original publications from the ACE Study?s retrospective and prospective parts. The key findings have been summarised in a chapter in a recently published book (37).
Conclusion
Doctors in training are often told that the practice of medicine should be based on a «bio-psycho-social» model, according to which the patient should be «seen and treated as a person». Nevertheless, our experience is that many of our young colleagues have no clear idea of the practical biomedical relevance of biographical information. Hopefully, we have succeeded in demonstrating that a person’s life experiences have «hard» medical relevance, right down to the cellular and even subcellular levels. Lived experience, no less than microbes, smoking and nutrition, is thus of paramount biomedical relevance and should be acknowledged by medicine as such.
The authors are part of an interdisciplinary think-tank organized by the General Practice Research Unit at the Department of Public Health and General Practice in Trondheim. We thank the other members of the think-tank: Tor-Johan Ekeland, Irene Hetlevik, Edvin Schei and Arne Johan Vetlesen, and also Henrik Vogt, for constructive advice. The origin of this manuscript was Linn Getz’ contribution to a report on the future of Biomedicine commissioned by the Norwegian Medical Association ()
Conflicts of interest:
None
Tabell
| Key points |
|
- 1.
Lock M, Gordon DR. Biomedicine examined. Dordrecht: Kluwer Academic Publishers, 1988.
- 2.
Vetlesen AJ. Frihetens forvandling. Essays og artikler 2002 – 2008. Oslo: Universitetsforlaget, 2009.
- 9.
Vangen S, Nordhagen R, Lie KK. Gjensyn med Forsdahl-Barker hypotesen. Tidsskr Nor Lægeforen 2005; 125: 451-3.
- 11.
Godfrey KM, Gluckman PD, Hanson MA. Developmental origins of metabolic disease: life course and intergenerational perspectives. Trends Endocrinol Metab 2010; 21: 199 – 205.
- 14.
Abbott A. Project set to map marks on genome. Nature 2010; 463: 596 – 7.
- 23.
Damjanovic AK, Yang Y, Glaser R et al. Accelerated telomere erosion is associated with a declining immune function of caregivers of Alzheimer’s disease patients. J Immunol 2007; 179: 4249 – 54. [PubMed]
- 24.
Kiecolt-Glaser JK, Gouin JP, Weng N et al. Childhood adversity heightens the impact of later-life caregiving stress on telomere length and inflammation. Psychosom Med 2011; 73: 16 – 22.
- 37.
Felitti VJ, Anda RF. The relationship of adverse childhood experiences to adult medical disease, psychiatric conditions, and sexual behavior: implications for healthcare. I: Lanius RA, Vermetten E, Pain C (eds.) The impact of early life trauma on health and disease: the hidden epidemic. Cambridge: Cambridge University Press, 2010.
- 41.
UCL Research Department of Epidemiology and Public Health. Whitehall II Study www.ucl.ac.uk/whitehallII/ (201.2011).
- 42.
Adler NE, Stewart J, red. The biology of disadvantage: socioeconomic status and health. Ann N Y Acad Sci 2010; 1186 (temanummer med 13 artikler). www.nyas.org/publications/annals/Detail.aspx?cid=79be4d13-c2ef-4d4c-8249-09130fa910e7
- 43.
Andersen SL, Tomada A, Vincow ES et al. Preliminary evidence for sensitive periods in the effect of childhood sexual abuse on regional brain development. J Neuropsychiatry Clin Neurosci 2008; 20: 292 – 301. [PubMed]
- 46.
Snow CP. The two cultures. Cambridge: Cambridge University Press, 1998. Opprinnelig utgitt i 1959.
- 47.
Ulvestad E. Sameining av «dei to kulturane» i medisinen. Tidsskr Nor Lægeforen 2001; 121: 492-4. [PubMed]
- 52.
Kirkengen AL, Getz L, Hetlevik I. En annen kardiovaskulær epidemiologi. Tidsskr Nor Legeforen 2008; 128: 2181-4. [PubMed]
- 54.
Gilbert SF, Epel D. Ecological developmental biology. Integrating epigenetics, medicine and evolution. Sunderland, MA: Sinauer Associates Inc, 2009.
- 55.
Mazzocchi F. Complexity in biology. Exceeding the limits of reductionism and determinism using complexity theory. EMBO Rep 2008; 9: 10 – 4.
- 58.
Kirkengen A, Ulvestad E. Overlast og kompleks sykdom - et intergrert perspektiv. Tidsskr Nor Lægeforen 2007; 127: 3228-31. [PubMed]
- 60.
Kirkengen AL. Hvordan krenkede barn blir syke voksne. 2. utg. Oslo: Universitetsforlaget, 2009. English translation: Kirkengen AL. The lived experience of violation. How abused children become unhealthy adults. Bucuresti: Zeta Books, 2010.
- 61.
Ekeland T-J. Kommunikasjon som helseressurs. I: Ekeland T-J, Heggen K. Meistring og myndiggjering. Reform eller retorikk? Oslo: Gyldendal Akademisk, 2007.
- 62.
Centers for Disease Control and Prevention. Adverse Childhood Experiences (ACE) Study. www.cdc.gov/nccdphp/ACE/index.htm (20.1.2011).
- 63.
Ulvestad E. Feilbruk av diagnostiske laboratorietester – et beslutningsanalytisk perspektiv. Tidsskr Nor Lægeforen 2000; 120: 2294–8. [PubMed]
- 64.
Biomedisin – status, scenarier og anbefalinger. Oslo: Den norske legeforening, 2010. www.legeforeningen.no/asset/48795/1/48795_1.pdf