Long-term prognosis for patients admitted to a medical intermediate care unit
Main findings
Intermediate medical care patients are a very heterogenous group in terms of their age, comorbidity and long-term prognosis.
Patients older than 80 years can survive for a long time after treatment in an intermediate care unit and do not require significantly more resources, measured in hospitalisation time, when compared to other patients.
A serious infection at the time of admission is associated with an increased risk of death even many years later.
Akershus University Hospital, which functions as an emergency hospital for approximately 560 000 people, established a medical intermediate care unit in 2013. The unit treats patients who need monitoring or treatment beyond what can be provided in wards, but not the resources of the intensive care unit. It has ten beds and receives patients from the emergency department or internal medicine wards. The epidemiology and short-term prognoses for patients admitted to the unit in 2014 have been described in a previous article (1). The majority of the patients received stabilising treatment and were transferred to a ward, but some had to be transferred to the intensive care unit (1). Comparisons of data on long-term survival of patients who have been treated in intermediate care units are difficult to make, because hospitals organise their intermediate and intensive care units in very different ways, including across Norway (2, 3). A main objective of our study was to gain more knowledge about the patients' long-term prognoses and investigate whether there are any factors that can predict long-term mortality in this population.
Patients at an advanced age (> 80 years), with an underlying malignant disease or other comorbidity are often assumed to have a poor prognosis both in the short and long term. For these groups, discussions arise regarding the benefits of providing higher-level treatment than in the ward. Infections are thought to primarily affect the short-term prognosis, and if the patient recovers from the infection, the long-term prognosis will be unaffected. We therefore wished to investigate these prognostic factors in particular.
Material and method
All patients admitted to the medical intermediate care unit at Akershus University Hospital in 2014 and 2016 were prospectively included in the study. The year 2015 was not included due to resource shortages that had resulted in incomplete data. All the patients were followed until 31 December 2019. The admission criteria were identical in the two years in question: an unstable condition that might quickly require respiratory support with non-invasive ventilation or circulatory support with vasoactive drugs. The unit does not provide ventilation treatment, continuous haemodialysis or haemodynamic monitoring beyond measurement of arterial pressure. The indication for admission was not changed during the study period.
Two scoring systems were used in the study. APACHE III (Acute physiology, age and chronic health evaluation) is one of several systems used in intensive care units to score the degree of severity of illness. This scoring system includes a list of reasons for admission adapted to intensive care units, which is easier to use for the intensive-care patient population than the ICD-10 coding system. With minor adaptations, this list has been used in Norwegian intensive care units for more than 20 years (4). In our study, the reasons for admission were categorised according to the APACHE III list. A SAPS-II (Simplified acute physiological score II) scoring estimates the likelihood of death during hospitalisation based on 17 biochemical and physiological variables registered within the first 24-hour period in intensive care (5). The higher the score, the higher the degree of severity of the acute disease in question. The scale is non-linear and runs in theory from 0 to 163, but scores above 80–90 are extremely rare. Each value on the scale is associated with a likelihood of death during the hospitalisation period. For example, the average SAPS-II score was 38 in Norwegian intensive care units in 2014 (6).
The standardised mortality ratio (SMR) is the ratio between the observed hospital mortality and the expected average mortality in a patient population, estimated on the basis of SAPS-II. Values under 1 indicate a lower mortality than expected. A value below 0.7 is a quality indicator in Norwegian intensive care units (6). Comorbidity was identified with Charlson's comorbidity index, which weights 16 diagnostic groups, such as heart failure, chronic pulmonary disease, diabetes and cancer, on a point scale, where the total point score predicts the risk of death (7).
The patient data were continuously registered in the MetaVision (version 5.45.062, 2007, iMDsoft) patient records system. The following variables were registered: reason for admission as defined by APACHE III, age, sex, length of stay in intermediate care, degree of severity upon admission as defined by the SAPS-II score, comorbidity measured by Charlson's comorbidity index, whether infection was part of the issue in question, death during the intermediate care period and death during the observation period.
In this study, patients who were undergoing treatment or close follow-up for cancer were scored as having active cancer. Patients with previous cancer that was assumed to be cured, and patients with non-melanoma skin cancer were not registered as patients with active cancer.
The doctor in charge at the intermediate care unit registered whether an infection was the reason for admission in one of three response categories: 'yes, direct', 'yes, contributory', or 'no'. A contributory cause could be, for example, when a stable heart failure patient suffered decompensated heart failure because of an intercurrent infection. In the regression analysis, the categories 'yes, direct' and 'yes, contributory' were merged. Since the study included data from two separate years, the follow-up periods are of varying length, the longest of which was six years. Data on post-discharge mortality were retrieved from the National Population Register.
Descriptive statistics with percentages and averages are used for continuous variables. The survival of patients discharged alive from the medical intermediate care unit was studied with the aid of multiple logistic regression analysis, with the three-year mortality after discharge as the outcome variable, and age, underlying malignancy, comorbidity score on Charlson's index and infection as a direct or contributory reason for admission as explanatory variables. Three-year survival was chosen because all the patients in the study received at least three years of follow-up.
Sex was not an independent predictor of mortality and was removed from the model. The malignancy variable (leukaemia, lymphoma, and metastatic and non-metastatic cancer) is included in Charlson's index, and the total increase in mortality is therefore underestimated by the malignancy parameter in the model. However, this disadvantage is counterbalanced by the advantage inherent in using a known comorbidity index rather than a modified Charlson's index where malignancy is removed. Infection was included in the model because we have previously found this to be an independent predictor of short-term mortality (1), and we wished to investigate its effect also in the long term. The analyses were undertaken in R, version 3.6.1.
The study was submitted to and approved by the data protection officer at the hospital (13–062). It was considered to be a quality assurance study, and was therefore not submitted to the Regional Committee for Medical and Health Research Ethics.
Results
Altogether 2 170 unique patients who had stayed in the medical intermediate care unit were included, 1 118 in 2014 and 1 052 in 2016. Their average age was 63.8 years, the median age was 68.2 years. The oldest patient was 98 years of age. A total of 7 % of the patients died during their stay in the medical intermediate care unit. Of the 2 017 patients who survived their stay in intermediate care, 55 % were still alive three years later. Their average period spent in the intermediate care unit was 1.6 days, median 1.1 days, with 9.9 days of total hospitalisation time. For patients with malignancies, the average period spent in the intermediate care unit was 2.1 days, and 1.6 days for older patients over 80 years. Of a total of 333 cancer patients, 17 % per cent died in the intermediate care unit, and 23 % of the survivors were still alive after three years. Of the 466 patients who were older than 80 years, 12 % died in the intermediate care unit, and 28 % of the survivors were still alive three years later. A little more than one-half (54 %) of the patients in the intermediate care unit were registered with an infection as a direct (33 %) or contributory (21 %) reason for admission. The average SAPS-II score for the patients was 34, and the standard mortality ratio was 0.69. Reasons for admission ranked by frequency and group mortality are shown in Table 1.
Table 1
The ten most frequent reasons for admission and three-year mortality for patients admitted to the Medical Intermediate Care Unit, Akershus University Hospital, in 2014 and 2016.
|
|
Number |
Died during the stay, number (%) |
Died within three years after the stay, number (%) |
|---|---|---|---|
| Pneumonia |
319 |
43 (13.5) |
155 (48.6) |
| COPD |
263 |
24 (9.1) |
154 (58.6) |
| Sepsis |
252 |
29 (11.5) |
119 (47.2) |
| Poisoning |
221 |
0 |
31 (14.0) |
| Hyponatraemia |
172 |
2 (1.2) |
61 (35.5) |
| Other respiratory disorders1 |
87 |
8 (9.2) |
50 (57.5) |
| Heart failure |
80 |
11 (13.8) |
47 (58.8) |
| Gastrointestinal bleeding |
75 |
1 (1.3) |
38 (50.7) |
| Ketoacidosis |
72 |
1 (1.4) |
9 (12.5) |
| Acute renal failure |
52 |
4 (7.7) |
24 (46.2) |
| Other1 |
577 |
30 (5.2) |
216 (37.4) |
| Total |
2 170 |
153 (7.1) |
904 (41.7) |
1Restrictive pulmonary disorder, neuromuscular disease, other conditions
Table 2 shows the results of a regression analysis of death after three years for those 2 017 patients who were discharged alive from the intermediate care unit. Comorbidity, age, infection as a direct or contributory reason for admission, and malignancy as an underlying disorder are significant independent predictors of long-term mortality.
Table 2
Logistic regression analysis of 2 017 patients discharged alive from the Medical Intermediate Care Unit, Akershus University Hospital, with death after three years as the outcome variable and age, infection, comorbidity and malignancy as explanatory variables. All effect size estimates, both adjusted and unadjusted, had p-values < 0.001.
| |
|
Number |
|
Unadjusted effects |
|
Adjusted effects |
||
|---|---|---|---|---|---|---|---|---|
|
|
OR |
95 % CI |
|
OR |
95 % CI |
|||
| Age |
Numerical value |
2 017 |
|
1.06 |
(1.06 to 1.07) |
|
1.05 |
(1.04 to 1.06) |
| Infection |
No1 |
970 |
|
1 |
|
|
1 |
|
|
|
Yes, direct or contributory |
1 047 |
|
2.65 |
(2.2 to 3.2) |
|
1.49 |
(1.2 to 1.9) |
| Charlson's score |
01 |
559 |
|
1 |
|
|
1 |
|
| 1 |
504 |
|
4.03 |
(3.0 to 5.4) |
|
2.11 |
(1.5 to 2.9) |
|
| 2 |
408 |
|
6.91 |
(5.1 to 9.4) |
|
2.76 |
(2.0 to 3.9) |
|
| ≥ 3 |
546 |
|
14.34 |
(10.6 to 19.3) |
|
5.03 |
(3.7 to 7.1) |
|
| Malignancy |
No1 |
1 739 |
|
1 |
|
|
1 |
|
| Yes |
278 |
|
5.08 |
(3.8 to 6.8) |
|
2.05 |
(1.4 to 2.9) |
|
1Reference category
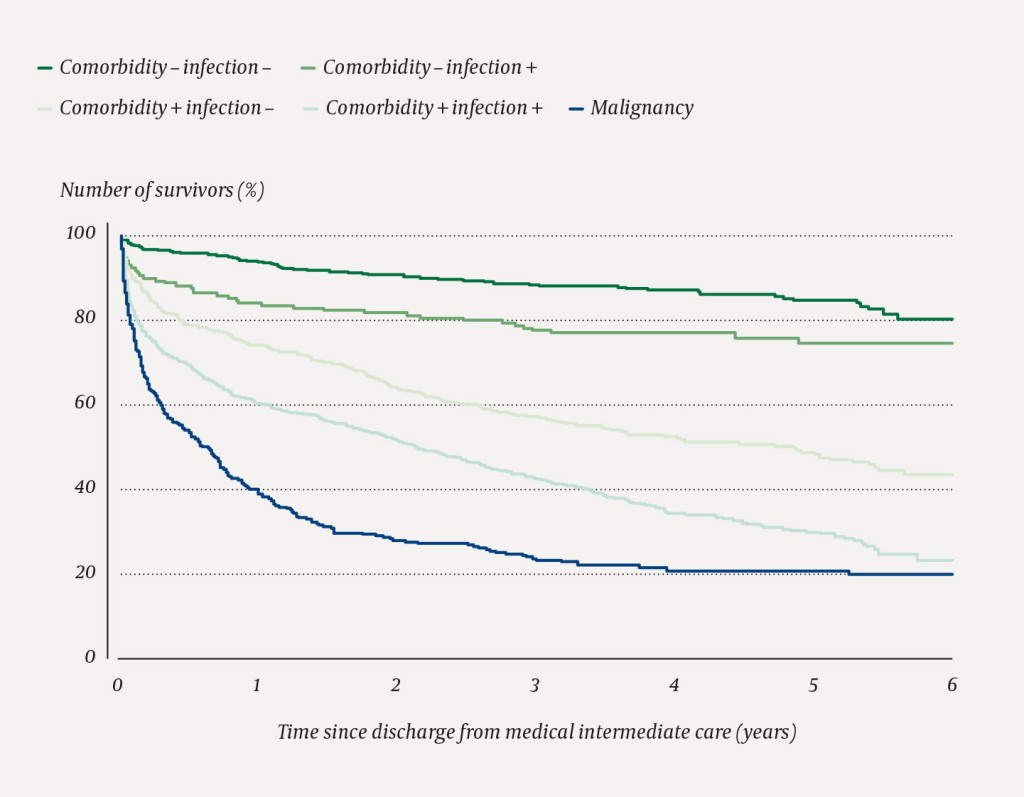
Figure 1 shows the survivors from the stay in intermediate care and their mortality in the subsequent years in a Kaplan-Meier curve. Group 1, consisting of 390 patients, had no known malignancy and no known comorbidity or infection. Their average age was 46 years, and typical reasons for admission were poisonings, rhabdomyolysis and seizures. Group 2, consisting of 169 patients, had no known malignancy or other comorbidity, but an infection. Their average age was 55 years, and typical reasons for admission were pneumonia and sepsis. Group 3, consisting of 499 patients, had no known malignancy or infection, but other comorbidity. Their average age was 65 years, and typical reasons for admission were heart failure, gastrointestinal bleeding and metabolic disorders. Group 4, consisting of 681 patients, had no known malignancy, but other comorbidity and infection. Their average age was 71 years, and typical reasons for admission were COPD, pneumonia and sepsis. Group 5 consisted of 278 patients with an underlying malignancy, with and without an infection. Their average age was 70 years, and they had typically been admitted for pneumonia, sepsis and hyponatraemia.
Discussion
The main finding in this study is that of all patients who were admitted to the medical intermediate care unit, 93 % were discharged alive from the unit, and of these, 55 % were still alive three years later. Of the cancer patients and patients older than 80 years who survived their stay, 23 % and 28 % were alive after three years, respectively.
Selecting patients for treatment beyond what can be provided in regular wards can be challenging. Doctors do not want to deprive their patients of the opportunity to receive organ support therapy that can enable them to survive an acute, reversible condition, but nor do they wish to provide treatment that at worst will simply prolong their suffering. These considerations are especially difficult with regard to very old patients who have serious underlying diseases or cancer. Here, we present survival data and factors that predict mortality within three years, and this may be helpful to clinicians in making these difficult assessments.
In the regression analysis, age, malignancy, comorbidity and infection emerged as independent predictors of mortality. Not unexpectedly, age was the most significant factor. More surprisingly, infection as a direct or contributory reason for admission was also an independent predictor of mortality. The five groups that are described in Figure 1 have significant differences in their disease trajectories. Patients with comorbidity, but with no malignancy, have a consistent mortality rate over the subsequent years both with and without infection, while for the group with malignancy, the curve drops off steeply with high mortality over the first eighteen months before flattening out.
The analyses have not differentiated between different forms of cancer. Cancer therapies are developing rapidly, however, and the long-term survival rate is considerable for many forms of cancer even at advanced stages. Oncological expertise is therefore required to assess the treatment level. However, medical factors other than the cancer prognosis are also essential in the assessment. More than one-half of the patients had an infection as their direct or contributory reason for admission. Infections are therefore a dominant reason for admission to an intermediate care unit.
Infections tend to be regarded as transient conditions that do not impact long-term survival. Sepsis is an independent predictor of mortality up to ten years later (8). The reasons why infections impact long-term survival have not been finally identified, but persistent organ dysfunction, immune dysfunction and immunosuppression have been suggested as explanations (9). Genetic factors influence mortality and increase the number of readmissions with an infection after sepsis (10, 11), and have an impact on the risk of developing sepsis (12). Another, more speculative explanation is that issues in the patient that cause the infection to take a serious course also predispose for mortality from other causes. For example, an increased risk of cardiovascular events has been found even many years after a case of pneumonia that required hospitalisation (13).
A total of 15 % of the patients in our cohort had a diagnosis of malignancy. Only very few studies have been undertaken of cancer patients in intermediate care units. A study from European intensive care units found, however, a similar proportion of patients with a cancer diagnosis (14). This indicates that Norway does not follow a more restrictive practice for providing treatment in intermediate care units to this patient group when compared to other European countries. A study of 2 439 cancer patients admitted to an intensive care unit in Jordan found similar survival rates as those in our cohort, with 23 % of the patients alive after one year and 14 % after five years (15).
For cancer patients and very old patients, there will often be a discussion about their ability to benefit from a hospital stay at a higher level than in the regular ward. In our dataset, the hospitalisation period in the intermediate care unit was no more than half a day longer for patients with cancer than for patients without, while the hospitalisation period for older patients was equal to that of the younger age groups. Resource use as measured in the length of admission was thus not significantly higher for these patient groups than for others, indicating that resource use is not in itself a valid argument for refraining from attempts at treatment. On the other hand, the patients in our study were preselected. Treatment in the intermediate unit had been withheld for many patients after a medical and ethical assessment made by the medical team, and a conversation with the patient/next of kin, and they were therefore not included in the study.
Age, male sex and serious comorbidity are independent predictors of long-term mortality after an admission for sepsis (15). In our study, sex did not emerge as a significant predictor. In a Spanish medical intermediate care unit, comorbidity and level of functioning prior to the admission were predictors of death after two years (16).
The reason for admission also has a considerable impact on mortality. In Table 1, we present the association between diagnosis and mortality for the ten largest diagnostic groups. The mortality varies considerably depending on the diagnosis, from 14 % for poisoning to 73 % for heart failure. The heart failure patients had the highest mortality both in the short and long term. Acute heart failure is known to have high mortality (17), but our figures are higher than what has been described previously. One possible explanation is that the heart failure patients in our unit were so ill that they had been transferred from the cardiac monitoring unit because they needed a higher care factor.
None of the patients who were admitted for poisonings died during the hospitalisation period, but three-year mortality in this group was 14 %, which underscores the serious prognosis and the risk of early death in this patient group.
The strength of our study lies in its prospective nature and its inclusion of a complete patient dataset for the study periods, with a high number of patients. The registration was uniform and was undertaken by a small number of persons affiliated with the unit. Its weakness is that the patients had already undergone a selection process in order to be accepted for admission to the intermediate care unit, meaning that the long-term survival in our study applies to a pre-selected population. The acceptance criteria for admission to the intermediate care unit may vary through the day, and specialists who are affiliated with the unit in the daytime tend to reject admissions that are accepted by less experienced doctors who are on duty at night. For patients with cancer, we have not differentiated by the degree of severity of the disease. This population is heterogenous, with considerable variation in terms of disease and prognoses. We have not investigated scoring tools that focus on frailty, e.g. the Clinical Frailty Scale (18), as a support tool in making decisions on treatment limitations. Such tools would have been of great interest also with regard to our population.
Patient groups treated in an intermediate care unit vary greatly in their long-term survival after three years. A considerable proportion of the patients with serious comorbidity or cancer, or aged above 80 years, survive for a long time after their hospitalisation. After an individual assessment, patients in this group should be given the option to receive stabilising organ support therapy in an intermediate care unit in line with other patient groups. Having a serious infection gives an increased risk of mortality even many years later.
The article has been peer-reviewed.
- 1.
Morland M, Haagensen R, Dahl FA et al. Epidemiology and prognoses in a medical intermediate care unit. Tidsskr Nor Legeforen 2018; 138. doi: 10.4045/tidsskr.17.0496. [PubMed][CrossRef]
- 2.
Torres OH, Francia E, Longobardi V et al. Short- and long-term outcomes of older patients in intermediate care units. Intensive Care Med 2006; 32: 1052–9. [PubMed][CrossRef]
- 3.
Mosevoll KA. Ill, but not ill enough. Tidsskr Nor Legeforen 2018; 138. doi: 10.4045/tidsskr.18.0224. [PubMed][CrossRef]
- 4.
Knaus WA, Wagner DP, Draper EA et al. The APACHE III prognostic system. Risk prediction of hospital mortality for critically ill hospitalized adults. Chest 1991; 100: 1619–36. [PubMed][CrossRef]
- 5.
Le Gall JR, Lemeshow S, Saulnier F. A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study. JAMA 1993; 270: 2957–63. [PubMed][CrossRef]
- 6.
Kvåle R. Norsk intensivregisters årsrapport for 2014. Bergen: Haukeland universitetssykehus, 2015. https://helse-bergen.no/norsk-intensivregister-nir/arsrapportar Accessed 24.3.2021.
- 7.
Charlson ME, Pompei P, Ales KL et al. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373–83. [PubMed][CrossRef]
- 8.
Linder A, Guh D, Boyd JH et al. Long-term (10-year) mortality of younger previously healthy patients with severe sepsis/septic shock is worse than that of patients with nonseptic critical illness and of the general population. Crit Care Med 2014; 42: 2211–8. [PubMed][CrossRef]
- 9.
Delano MJ, Ward PA. The immune system's role in sepsis progression, resolution, and long-term outcome. Immunol Rev 2016; 274: 330–53. [PubMed][CrossRef]
- 10.
Rautanen A, Mills TC, Gordon AC et al. Genome-wide association study of survival from sepsis due to pneumonia: an observational cohort study. Lancet Respir Med 2015; 3: 53–60. [PubMed][CrossRef]
- 11.
Genga KR, Lo C, Cirstea MS et al. Impact of PCSK9 loss-of-function genotype on 1-year mortality and recurrent infection in sepsis survivors. EBioMedicine 2018; 38: 257–64. [PubMed][CrossRef]
- 12.
Lu H, Wen D, Wang X et al. Host genetic variants in sepsis risk: a field synopsis and meta-analysis. Crit Care 2019; 23: 26. [PubMed][CrossRef]
- 13.
Corrales-Medina VF, Alvarez KN, Weissfeld LA et al. Association between hospitalization for pneumonia and subsequent risk of cardiovascular disease. JAMA 2015; 313: 264–74. [PubMed][CrossRef]
- 14.
Taccone FS, Artigas AA, Sprung CL et al. Characteristics and outcomes of cancer patients in European ICUs. Crit Care 2009; 13: R15. [PubMed][CrossRef]
- 15.
Feras IH, Lama HN, Awad A et al. Predictors of ICU admissions in patients with cancer and the related characteristics and outcomes: A 5-year registry-based study. Crit Care 2016; 44: 548–53. [CrossRef]
- 16.
Shankar-Hari M, Ambler M, Mahalingasivam V et al. Evidence for a causal link between sepsis and long-term mortality: a systematic review of epidemiologic studies. Crit Care 2016; 20: 101. [PubMed][CrossRef]
- 17.
Crespo-Leiro MG, Anker SD, Maggioni AP et al. European Society of Cardiology Heart Failure Long-Term Registry (ESC-HF-LT): 1-year follow-up outcomes and differences across regions. Eur J Heart Fail 2016; 18: 613–25. [PubMed][CrossRef]
- 18.
Rockwood K, Song X, MacKnight C et al. A global clinical measure of fitness and frailty in elderly people. CMAJ 2005; 173: 489–95. [PubMed][CrossRef]