COVID-19 cases reported to the Norwegian Institute of Public Health in the first six weeks of the epidemic
Main findings
By 12 March, 1 128 cases of laboratory-confirmed COVID-19 cases had been reported to the Norwegian Institute of Public Health.
The median age was 47 years, 64 % were men, 66 % had travelled abroad, 6 % were hospitalised at the time of reporting and < 1 % had died.
Between 13 March and 5 April 2020, 4 742 cases were reported. Their median age was 48 years, the proportion of men had fallen to 47 %, fewer had travelled abroad (18 %) and a higher proportion were hospitalised (15 %) or died (3 %).
An increase in numbers of persons with severe pneumonia of unknown aetiology was reported from Wuhan, China, on 31 December 2019. On 7 January 2020, a novel coronavirus, later named SARS-CoV-2, was identified by the Chinese health authorities as being the cause of the disease now known as COVID-19 (1). The virus spread rapidly; the World Health Organization declared the outbreak a Public Health Emergency of International Concern on 30 January, and a pandemic on 11 March 2020 (2).
Testing for SARS-CoV-2 in Norway was initially reserved for returning travellers from countries with widespread transmission and close contacts of confirmed cases. The first case of SARS-CoV-2 infection was confirmed on 26 February. At the beginning of the outbreak, advice concerning general infection control measures, such as good hand hygiene, cough etiquette, and staying at home in case of illness, was sharpened. On 12 March, extensive national control measures were implemented to reduce the spread of the virus and to maintain adequate treatment capacity in hospitals. These included closure of daycare centres, schools, cultural and sporting arrangements, hospitality services and businesses with one-on-one contact with customers (for example physiotherapists and hairdressers) and quarantining of persons returning to Norway from abroad (3).
At the same time, the criteria for testing were modified to ensure diagnosis of severe cases. Changes in test criteria, implementation of control measures and other important dates in the early stages of the COVID-19 outbreak in Norway are presented in Figure 1. From 13 March, the criteria for testing included patients with symptoms consistent with COVID-19 who were at increased risk of developing severe disease, patients in healthcare institutions with acute respiratory infection (ARI), and healthcare workers with ARI (Box 1).
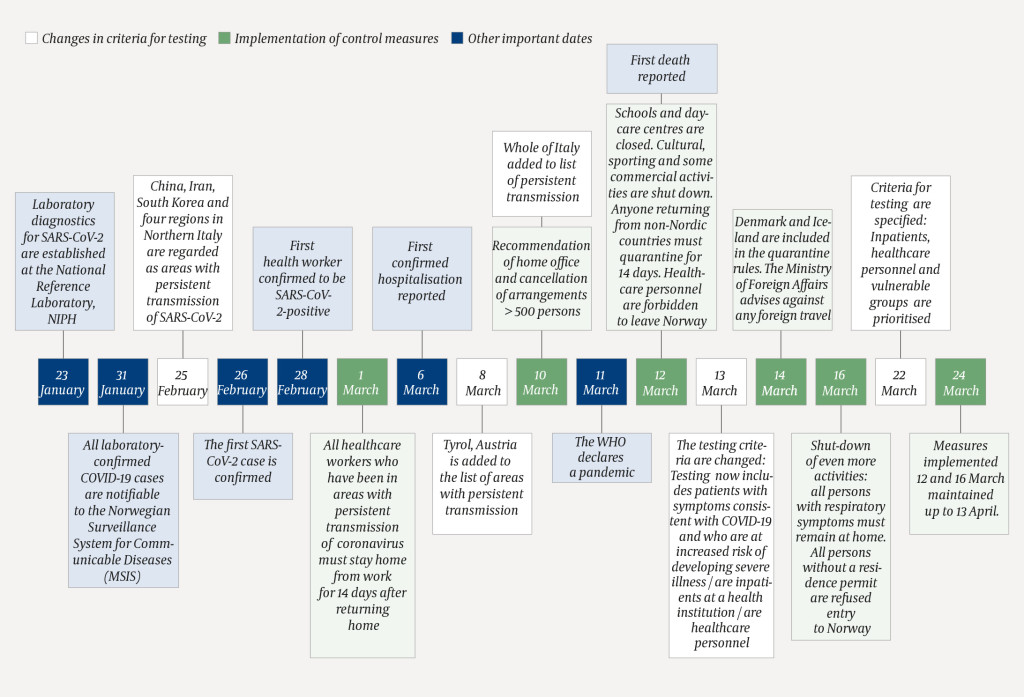
23 January–12 March
Persons with ARI (at least one of the following: cough, shortness of breath, fever (sore throat was included for some days in February)) who in the course of 14 days prior to the onset of symptoms fulfilled at least one of the following criteria:
has been in an area with transmission of COVID-19
has been in close contact with a confirmed case of COVID-19
has provided care for a patient, handled sample material from or in some other way had similar close contact with a person with confirmed COVID-19 (added 3 March), regardless of whether personal protective equipment was used (added 9 March)
has travelled outside the Nordic countries and is employed in the healthcare service (added 9 March)
has travelled outside the Nordic countries and is hospitalised in a healthcare institution (added 10 March)
13 March–5 April
Persons with ARI (at least one of the following: cough, shortness of breath, fever) who were:
in need of hospitalisation
hospitalised in/resident in a healthcare institution
employed in the healthcare service working in close contact with patients
members of a vulnerable group, even if their symptoms were mild (from 20 March changed to persons aged > 65 with an underlying chronic disease), who had had close contact with a person with confirmed COVID-19 (where contract tracing was indicated, applied until 19 March)
Testing was prioritised in this order from 22 March.
The Norwegian Institute of Public Health (NIPH) monitors the outbreak of COVID-19 in Norway and regularly publishes national statistics on SARS-CoV-2 testing and test results, the number of COVID-19 cases reported to the Norwegian Surveillance System for Communicable Diseases (MSIS), the number of confirmed cases hospitalised and in intensive care units (ICU)s and deaths associated with COVID-19 (4).
In this article we combine data from different surveillance to compare laboratory-confirmed cases of COVID-19 in Norway in the periods before and after control measures were introduced on 12 March and up to 5 April. We discuss how changes in criteria for testing and control measures may have affected the outbreak in the population and the surveillance findings.
Material and method
Laboratory diagnostics, criteria for testing and surveillance
Laboratory diagnostics for SARS-CoV-2 were established at the NIPH's National Reference Laboratory on 23 January. The primary test in Norway was a real-time reverse polymerase chain reaction (RT-PCR) test for detecting the E-gene (5), conducted mainly on nasopharyngeal and throat swab specimens. Given its high sensitivity (up to 99.9 %) and slightly lower specificity (about 80 %), the method may yield false positive results if many people with a low probability of being infected with SARS-CoV-2 are tested (6). Testing methods were established at most Norwegian medical microbiology laboratories within a few weeks. The test criteria for different time periods are shown in Box 1.
Most laboratories testing for SARS-CoV-2 reported daily numbers of tests performed, with data on test results and sampling dates, to the laboratory surveillance system at the National Reference Laboratory. A minority of laboratories reported the cumulative number of tests without exact sampling dates. Up to 30 March, our dataset contained information on the number of tests and number of positive tests, while from 1 April it contained information on number of persons tested and number who tested positive, in line with surveillance data published on the NIPH website.
Up to 5 April 2020, the chief municipal medical officers were required to notify all confirmed COVID-19 cases to the NIPH by phone (7)-(9). A confirmed case was defined as a person with confirmed SARS-CoV-2 infection regardless of the clinical picture. Data on age, sex, place of exposure, type of exposure, onset of symptoms if any, date of testing and hospitalization, if relevant, were collected. Type of exposure was defined as unspecified local transmission if the case had not been infected abroad or was not a close contact of a confirmed case, but where there was evidence of local transmission. For the remaining cases, type of exposure was classified as unknown.
The information was entered into the Outbreak Register, which was set up to provide a rapid overview of the outbreak, to enable the implementation of control measures and fulfilment of international reporting obligations. For the first 243 cases reported to the NIPH up to 9 March, the notifying chief municipal medical officers were also requested to complete a questionnaire with additional information on exposure and occupation, among other things. Data from the questionnaires were registered in the Outbreak Register. COVID-19-associated deaths were notifiable from 13 March (8). The data, including the first known death on 12 March, were entered in the Outbreak Register.
In addition to the notification by phone, all laboratory-confirmed cases of COVID-19 became notifiable to MSIS from 31 January 2020. Doctors and laboratories reported epidemiological, clinical and microbiological information using the standard MSIS notification form (8, 10, 11). The collection of data for the laboratory surveillance system, the Outbreak Register and MSIS took place in parallel (9).
Data processing and analysis
We included data on all cases reported to the Outbreak Register and MSIS up to 5 April 2020, with data on any deaths among these cases reported up to 7 May 2020. To maximize the completeness of case counts and variables, we linked MSIS data with Outbreak Register data using national identity numbers. In the event of discrepancies between the Outbreak Register and MSIS, MSIS data were prioritised, as MSIS was the primary data source used for surveillance. When there was no information on hospitalisation in the Outbreak Register, patients were assumed not to be hospitalised, unless other information was captured in MSIS.
We described cases in terms of demographic and geographic characteristics and disease severity for the whole period 26 February–5 April 2020, and divided it into periods A (up to 12 March) and B (from 13 March) on the basis of the test date. Population data were retrieved from Statistics Norway for use in calculating detection rates, defined as number of reported cases per 100 000 population (www.ssb.no).
From the laboratory surveillance system, we included data on all samples taken up to 5 April. The proportion of positive tests was calculated as the number of positive tests divided by the total number of tests. For some of the cases who were tested in early April and form part of the laboratory dataset, notification to MSIS and to the Outbreak Register only took place after 5 April. They are therefore not included in the data from these sources.
Excel and Stata SE 16.0 were used for data analysis. Maps were generated using QGIS version 3.10.0-A Coruña.
Ethical considerations
The data were reported to the NIPH pursuant to national legislation, and without the need for informed consent (7, 8, 12, 13). The project has ethical approval from the Regional Committee for Medical and Health Research Ethics (reference number 136964), and a privacy impact assessment was conducted and approved by the NIPH.
Results
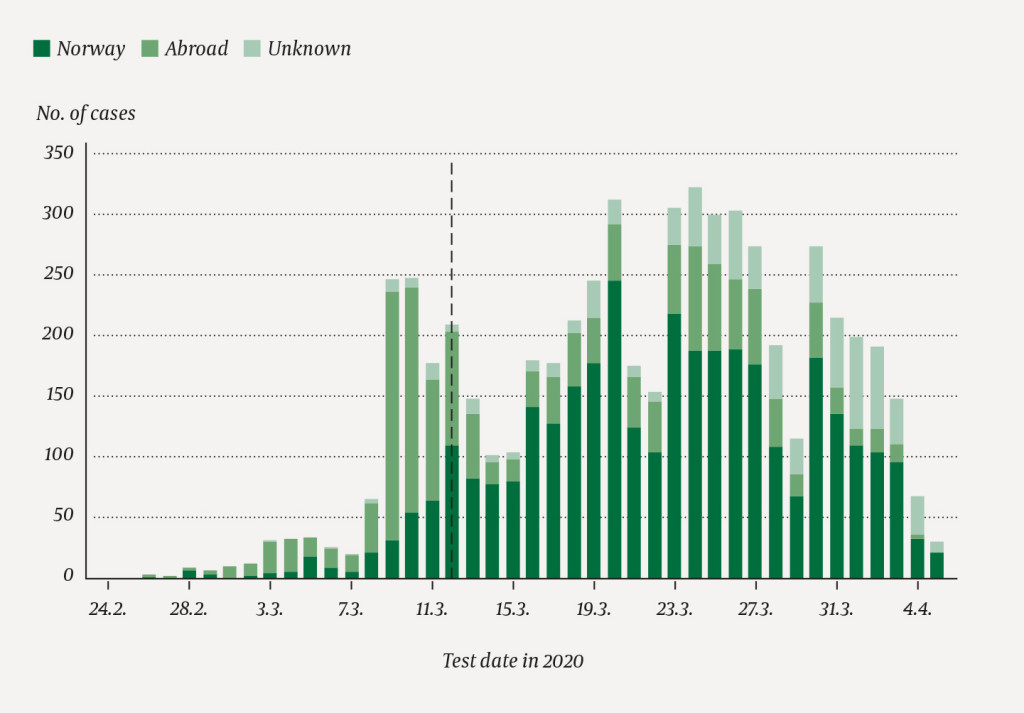
As of 5 April, 5 870 cases of COVID-19 were captured in the outbreak register and/or MSIS. Of these, 4 629 cases were registered in both registers, 1 125 cases were reported only to MSIS and 116 cases were registered only in the Outbreak Register. The first peak in the number of confirmed cases per day occurred on 9–10 March (Figure 2), while the majority of cases (4 742; 81 %) were detected after 12 March.
A total of 119 435 tests (2 225 per 100 000 population) were registered in the laboratory surveillance system as of 5 April, of which 6 203 (5 %) were positive for SARS-CoV-2. Test data with sampling date showed that the proportion of positive tests was highest in the period 8–10 March (11–17 %) (Figure 3), while the highest number of tests was registered in the period 16–20 March.
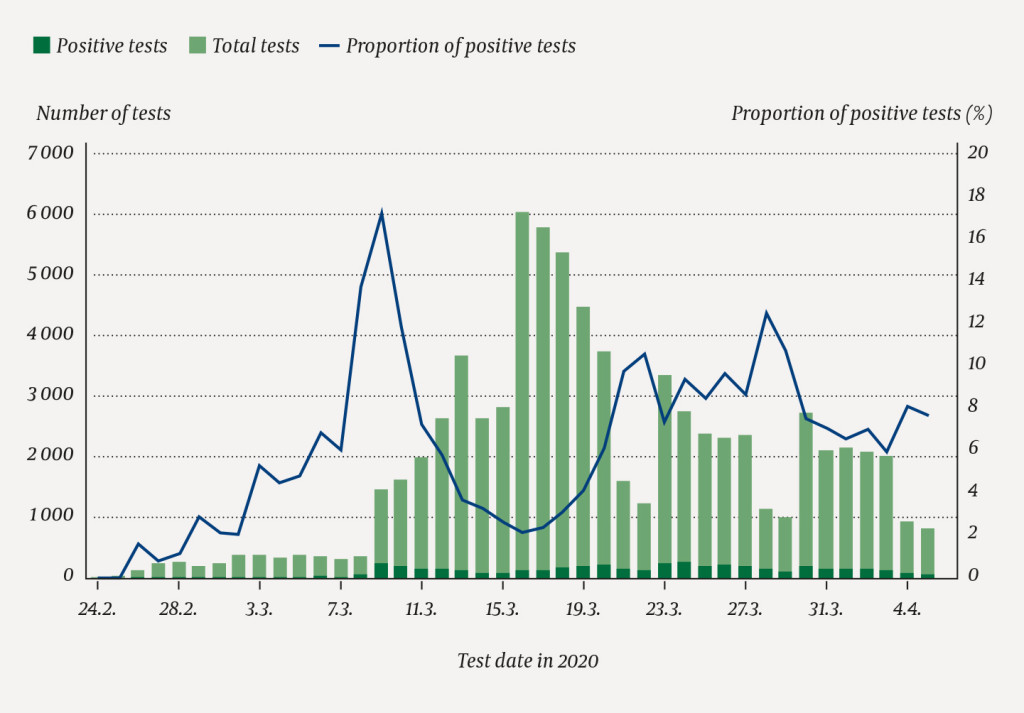
The median age of all cases was 48 years (range 0–102), and 2 939 (50 %) were men. The sex distribution changed over time, with males comprising 64 % of all cases in period A and 47 % in period B (Table 1). The median ages were 47 and 48 years in the two periods, and the proportion of cases aged 60 or over increased from 15 % to 29 % (Table 2).
Table 1
Description of COVID-19 cases by sampling period, Norway, 24 February–5 April 2020. No. (%) unless otherwise specified. Q1-Q3: lower quartile to upper quartile
| 24 February-5 April (n = 5 870) |
Up to 12 March (n = 1 128) |
From 13 March (n = 4 742) |
||
|---|---|---|---|---|
| Age (median, Q1–Q3) |
48 (33–60) |
47 (35–55) |
48 (33–62) |
|
| Sex |
||||
| Female |
2 931 (49.9) |
403 (35.7) |
2 528 (53.3) |
|
| Male |
2.939 (50.1) |
725 (64.3) |
2 214 (46.7) |
|
| Country of exposure |
||||
| Norway |
3 458 (58.9) |
331 (29.3) |
3 127 (65.9) |
|
| Abroad |
1 613 (27.5) |
747 (66.2) |
866 (18.3) |
|
| Unknown |
799 (13.6) |
50 (4.4) |
749 (15.8) |
|
| Type of exposure |
||||
| Foreign travel |
1 613 (27.5) |
747 (66.2) |
866 (18.3) |
|
| Close contact with confirmed case |
1 410 (24.0) |
218 (19.3) |
1 192 (25.1) |
|
| Unspecified local transmission |
1 357 (23.1) |
96 (8.5) |
1 261 (26.6) |
|
| Unknown |
1 490 (25.4) |
67 (5.9) |
1 423 (30.0) |
|
| Healthcare personnel |
||||
| Yes |
1 222 (20.8) |
61 (5.4) |
1 161 (24.5) |
|
| No |
2 293 (39.1) |
259 (23.0) |
2 034 (42.9) |
|
| Unknown |
2 355 (40.1) |
808 (71.6) |
1 547 (32.6) |
|
| In hospital at time of reporting |
||||
| Yes |
750 (12.8) |
63 (5.6) |
687 (14.5) |
|
| No |
4 710 (80.2) |
1 039 (92.1) |
3 671 (77.4) |
|
| Unknown |
410 (7.0) |
26 (2.3) |
384 (8.1) |
|
| Reported dead as of 7 May |
158 (2.7) |
5 (0.4) |
153 (3.2) |
|
| Time intervals, days (median, Q1–Q3) |
||||
| Symptom onset to testing (n = 4 882) |
4 (2–8) |
2 (1–4) |
5 (3–9) |
|
| Testing to reporting (n = 5 870) |
1 (1–2) |
1 (1–2) |
1 (1–2) |
|
| Symptom onset to hospitalisation (n = 312)1 |
7 (4–10) |
7 (5.5–9) |
7 (4–10) |
|
| Symptom onset to death (n = 145)2 |
13 (9–21) |
21 (9–27) |
13 (9–20) |
|
1Dates were available for 20 patients tested up to 12 March and for 292 patients tested from 13 March
2Dates were available for 5 patients tested up to 12 March and for 140 patients tested from 13 March
Table 2
Cases of COVID-19 reported to the Norwegian Institute of Public Health's Outbreak Register and/or Surveillance System for Communicable Diseases and number of tests and number of positive tests for SARS-CoV-2 per 100 000 population in Norway, 24 February–5 April 2020, by age group and testing period
| Age group |
24 February–5 April (n = 5 870) |
Up to 12 March (n = 1 128) |
From 13 March (n = 4 742) |
||||||
|---|---|---|---|---|---|---|---|---|---|
| Number of cases |
Number of cases |
Total number of tests per 100 000 |
Positive tests per 100 000 |
Number of cases |
Total number of tests per 100 000 |
Positive tests per 100 000 |
|||
| 0–9 |
61 (1.0) |
14 (1.2) |
94 |
2 |
47 (1.0) |
202 |
7 |
||
| 10–19 |
249 (4.2) |
42 (3.7) |
159 |
5 |
207 (4.4) |
242 |
25 |
||
| 20–29 |
784 (13.3) |
121 (10.7) |
208 |
14 |
663 (14.0) |
1,529 |
71 |
||
| 30–39 |
947 (16.1) |
180 (16.0) |
278 |
20 |
767 (16.2) |
1,959 |
83 |
||
| 40–49 |
1 109 (18.9) |
297 (26.3) |
306 |
34 |
812 (17.1) |
1 756 |
91 |
||
| 50–59 |
1 198 (20.4) |
310 (27.5) |
299 |
37 |
888 (18.7) |
1 507 |
99 |
||
| 60–69 |
708 (12.1) |
111 (9.8) |
184 |
14 |
597 (12.6) |
1 096 |
77 |
||
| 70–79 |
465 (7.9) |
43 (3.8) |
115 |
7 |
422 (8.9) |
913 |
76 |
||
| 80–89 |
270 (4.6) |
7 (0.6) |
147 |
4 |
263 (5.6) |
1 509 |
113 |
||
| 90+ |
79 (1.4) |
3 (0.3) |
208 |
9 |
76 (1.6) |
2 536 |
119 |
||
| Total |
5 870 (100.0) |
1 128 (100.0) |
212 |
17 |
4 742 (100.0) |
1 222 |
69 |
||
Cases were reported from all counties (Figure 4). Of the 5 071 cases (86 %) for whom the country of exposure was known, 3 458 (68 %) were infected in Norway and 1 613 (32 %) abroad. Imported cases were mainly from Austria (702; 44 %), Spain (348; 22 %) and Italy (171; 11 %). The remaining 370 cases (23 %) for which we had specific information about the country of exposure, had been infected in 45 different countries. The proportion of cases infected abroad decreased from 66 % to 18 % from period A to period B, while the proportion of cases infected in Norway increased from 29 % to 66 % (Table 1). Those who had been in Spain were older than the other travellers (median age 72 compared with 46 years), and a larger proportion were hospitalised (94 cases (27 %), compared with 97 cases (8 %)).
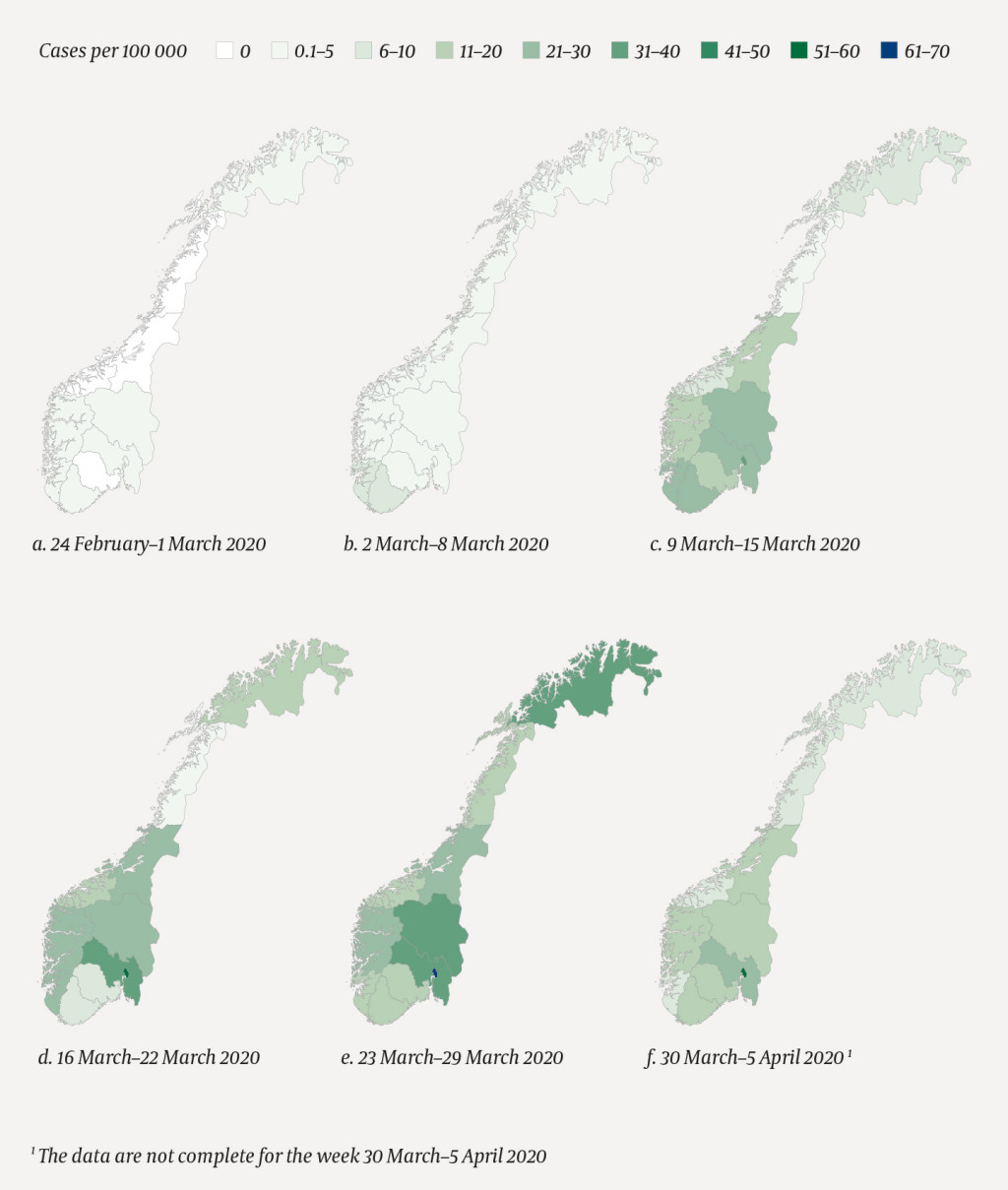
The date of reported symptom onset was available for 4 882 of cases (83 %). The earliest symptom onset date attributable to COVID-19 was 12 February. The median interval between onset of symptoms and date of specimen collection was 4 days, and it increased from 2 days in period A to 5 days in period B (Table 1). The median interval between testing and reporting was 1 day, and no difference was observed between the two time periods.
The first COVID-19 related hospitalisation was recorded on 6 March and the first death on 12 March. 750 cases (13 %) were hospitalized at the time when they were reported. The proportion of cases in hospital at the time of reporting increased from 6 % in period A to 14 % in period B. 158 deaths (3 % overall) were reported by 7 May. Five (<1 %) of the cases tested up to 12 March died, after which the proportion with fatal outcome increased to 3 %.
Discussion
During the first six weeks of the COVID-19 outbreak in Norway, approximately 2 % of the population was tested for SARS-CoV-2, 5 % of tests were positive, and 5 870 cases were reported to the NIPH.
The beginning of the COVID-19 epidemic in Norway occurred during the winter season's outbreaks of influenza and common cold. It was therefore necessary to have clear criteria for testing in order not to exceed testing capacity, even though COVID-19 diagnostics were in place early and were quickly scaled up. At the beginning of the outbreak, the strategy was to capture all introductions of COVID-19 to Norway, first and foremost related to foreign travel. The start of the outbreak in Norway coincided with extensive foreign travel activity in the winter holiday weeks, and many of the cases detected were men aged 40–60 who had been on skiing holidays in Italy or Austria.
During the days preceding 12 March, the proportion of cases who became infected in Norway increased and the number of cases with unknown source of infection rose (14). Norway was considered to have entered a new phase of the pandemic (14). When extensive control measures were introduced on 12 March, the criteria for testing were simultaneously shifted towards picking up cases of severe COVID-19, so that illness after foreign travel was no longer sufficient per se to qualify for testing. The restrictions imposed by the testing criteria may well have resulted in some infected persons not being diagnosed.
From 13 March the age distribution of the reported cases changed, and a higher proportion were hospitalised or died. In our data, hospitalisation was recorded at the time of reporting. The median time interval between onset of symptoms and hospitalisation and/or death indicates that some cases may have been hospitalised after the time of reporting or have died after 7 May. However, the total number of cases hospitalised is consistent with the numbers in the Norwegian Intensive Care and Pandemic Registry (15). Even though a history of travel was no longer among the prerequisites for testing after 12 March, a large number of cases who had travelled to Spain were reported in the weeks that followed. Many of them were probably tested because of high age and/or increased risk of severe illness, and not primarily because of their travel. This example reveals a bias in registered information about country of exposure, which was attributable to the testing criteria applying at the time.
The proportion of healthcare workers among cases was higher in the latter part of the study period, but this should be interpreted with caution because of incomplete data. Moreover, the type of exposure and nature of occupation (for example patient contact) of most health personnel was unknown. The numbers therefore cannot be used as a measure of how many were exposed at work. More reliable data can probably be acquired by improving the surveillance systems. We also found that after 12 March, the proportion of female cases exceeded that of males, possibly due to increased testing among healthcare workers and the elderly, both groups with a larger proportion of women (16).
The median interval between onset of symptoms and testing increased from 13 March. This may be because the testing targeted patients with severe disease, which takes some time to develop, or it may be a result of local practice and testing capacity. The discrepancy between numbers of positive tests and numbers of reported cases can be explained by the fact that some cases were tested repeatedly and were thus reported to the laboratory surveillance system several times. Furthermore, some cases tested up to 5 April were reported only after that date. However, there was very little delay between testing and reporting throughout the study period. Data reported to the Outbreak Register and MSIS are therefore considered to be a timely source of information on the status of the outbreak, also early in the epidemic. Case data were maximised by linking together data from MSIS and Outbreak registers, while data on testing from the National Reference Laboratory were important for understanding the fluctuations in the positivity rate in light of testing activity.
The number of cases registered in the three data sources will not represent the true number of persons infected with SARS-CoV-2 in the population. Only laboratory-confirmed cases are reported. The possibility that there was infection in Norway before 26 February cannot be ruled out, as a case with symptoms that could be attributable to COVID-19 was observed as early as 12 February, but only reported later. Moreover, the criteria for testing during this period were such that only those with symptoms met the criteria, and a large percentage of COVID-19 cases are asymptomatic, or only have mild symptoms (17, 18). Large-scale testing of asymptomatic or pre-symptomatic persons would have required significant resources, with increased risk of false positive and false negative test results. Although the discrepancy between number of registered cases and the true incidence of infections in the population is unknown, there is reason to believe that the incidence of infection in Norway during the study period was relatively low compared to many other countries (19). The seroprevalence (proportion of persons with antibodies) in Norway was estimated to be around 1 % in mid-April (20).
Conclusion
Access to timely surveillance data has been crucial for monitoring the epidemic. The compilation of data from various sources has contributed to a more comprehensive picture of the onset and development of the epidemic. Among the cases of COVID-19 reported to the NIPH in the first six weeks of the epidemic, differences were found in the distribution of age, sex, place of exposure and disease severity in the periods before and after 12 March, when extensive control measures were introduced. While some of these differences may reflect different phases of the epidemic, it is important to interpret the findings in the light of criteria for testing, testing activity, control measures and characteristics of the surveillance systems. Additional studies, information from more data sources and further development of surveillance systems are required to provide both broader and more detailed knowledge of the extent and evolution of the epidemic in Norway, where and in what contexts transmission occurs and who is at greatest risk of severe illness. Sound surveillance data which can be linked to various data sources are crucial for following up the current strategy, which is based on early detection of cases and local management by means of targeted measures.
The article has been peer-reviewed.
We would like to thank the chief municipal medical officers and medical microbiology laboratories for reporting cases and test results to the NIPH. We would also like to thank all those at the NIPH who have been involved in managing the outbreak. In addition we wish to thank Lisa Hansen for valuable input to the manuscript and Torstein Aune for his work on the laboratory surveillance data.
- 1.
World Health Organization. Novel Coronavirus - China. https://www.who.int/csr/don/12-january-2020-novel-coronavirus-china/en/ Accessed 3.4.2020.
- 2.
World Health Organization. WHO Director-General's opening remarks at the media briefing on COVID-19, 11.3.2020. https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19–11-march-2020 Accessed 3.4.2020.
- 3.
Regjeringen. Nasjonale tiltak. https://www.regjeringen.no/no/tema/koronavirus/nasjonale-tiltak/id2693684/ Accessed 1.5.2020.
- 4.
Folkehelseinstituttet. Statistikk om koronavirus og covid-19. https://www.fhi.no/sv/smittsomme-sykdommer/corona/dags--og-ukerapporter/dags--og-ukerapporter-om-koronavirus/ Accessed 27.5.2020.
- 5.
Corman VM, Landt O, Kaiser M et al. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Euro Surveill 2020; 25. doi: 10.2807/1560-7917.ES.2020.25.3.2000045. [PubMed][CrossRef]
- 6.
Folkehelseinstituttet. Molekylær diagnostikk av Sars-Cov-2. https://www.fhi.no/nettpub/coronavirus/testing-og-oppfolging-av-smittede/molekylar-diagnostikk/ Accessed 11.8.2020.
- 7.
FOR-2007-12-21-1573. Forskrift om varsling av og tiltak ved alvorlige hendelser av betydning for internasjonal folkehelse mv. (IHR-forskriften). https://lovdata.no/dokument/SF/forskrift/2007-12-21-1573 Accessed 4.6.2020.
- 8.
FOR-2003-06-20-740. Forskrift om Meldingssystem for smittsomme sykdommer (MSIS-forskriften). https://lovdata.no/dokument/SF/forskrift/2003-06-20-740?q=MSIS Accessed 4.6.2020.
- 9.
FOR-2020-01-31-92. Forskrift om endring i forskrift om allmennfarlige smittsomme sykdommer og forskrift om Meldingssystem for smittsomme sykdommer https://lovdata.no/dokument/LTI/forskrift/2020-01-31-92 Accessed 4.6.2020.
- 10.
Folkehelseinstituttet. Meldingskriterier for sykdommer i MSIS. https://www.fhi.no/publ/2017/meldingskriterier-for-sykdommer-i-msis/ Accessed 1.5.2020.
- 11.
Folkehelseinstituttet. MSIS meldingsskjema. Nominativ melding om smittsom sykdom. https://www.fhi.no/publ/2019/msis-meldingsskjema.-nominativ-meld/ Accessed 1.5.2020.
- 12.
LOV-2000-06-23-56. Lov om helsemessig og sosial beredskap (helseberedskapsloven). https://lovdata.no/dokument/NL/lov/2000-06-23-56 Accessed 4.6.2020.
- 13.
LOV-1994-08-05-55. Lov om vern mot smittsomme sykdommer (smittevernloven). https://lovdata.no/dokument/NL/lov/1994-08-05-55 Accessed 4.6.2020.
- 14.
Covid-19-epidemien: Risikovurdering og respons i Norge-Versjon 3. Oslo: Folkehelseinstituttet, 2020. https://www.fhi.no/publ/2020/covid-19-epidemien-risikovurdering/ Accessed 28.8.2020.
- 15.
COVID-19 Ukerapport - uke 19. Oslo: Folkehelseinstituttet; 2020. https://www.fhi.no/publ/2020/koronavirus-ukerapporter/ Accessed 4.6.2020.
- 16.
Statistisk sentralbyrå. Helse- og sosialpersonell. https://www.ssb.no/arbeid-og-lonn/statistikker/hesospers Accessed 18.5.2020.
- 17.
The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team.. The epidemiological characteristics of an outbreak of 2019 novel Coronavirus Diseases (COVID-19) - China, 2020. China CDC Weekly 2020; 2: 113–22. [CrossRef]
- 18.
Oran DP, Topol EJ. Prevalence of asymptomatic SARS-CoV-2 infection: A narrative review. Ann Intern Med 2020; 173: 362–7. [PubMed][CrossRef]
- 19.
European Centre for Disease Prevention and Control. Situation updates on COVID-19. https://www.ecdc.europa.eu/en/covid-19/situation-updates Accessed 1.9.2020.
- 20.
Tunheim GKA, Rø G, Steens A et al. Seroprevalence of SARS-CoV-2 in the Norwegian population measured in residual sera collected in April/May 2020 and August 2019. Oslo: Folkehelseinstituttet, 2020. https://www.fhi.no/publ/2020/seroprevalence-of-sars-cov-2-in-the-norwegian-population—measured-in-resid/ Accessed 11.8.2020.