Laparoscopic gastric bypass versus lifestyle intervention for adolescents with morbid obesity
Main findings
Adolescents who underwent laparoscopic gastric bypass surgery combined with lifestyle intervention had significantly greater one-year weight loss (31 %) than adolescents who received lifestyle intervention alone.
Surgery was associated with significant improvement in cardiometabolic risk factors, whereas lifestyle intervention was not.
A relatively high proportion of patients who underwent surgery had anaemia (10 %), iron deficiency (21 %) and low vitamin B12 levels (10 %) after one year.
Twenty out of 33 patients (61 %) had low blood glucose two hours after oral glucose tolerance testing.
Morbid obesity in adolescents is associated with an increased risk of comorbidities, including non-alcoholic fatty liver disease, type 2 diabetes, cardiovascular disease, mental illness, and morbid obesity in adulthood, as well as reduced life expectancy (1, 2). Effective treatment can therefore provide substantial benefits, both for the individual and for society (3).
Conservative treatment of morbid obesity in adolescents uses an interdisciplinary approach and family-based behavioural therapy to support changes in lifestyle habits related to diet and physical activity. This approach results on average in low to moderate levels of weight loss (4, 5).
In adults, bariatric (weight-loss) surgery has been shown to produce good results, with lasting weight loss and improvement in comorbidities, but also an increased risk of complications in the short and long term (6, 7). Prior to the start of the 4XL study in 2009, little was known about the effectiveness of bariatric surgery in adolescents and the associated complications (8). Eleven years later, the evidence base remains uncertain (3, 9).
The primary research question in the 4XL study was to clarify whether laparoscopic Roux-en-Y gastric bypass surgery (hereafter referred to as a gastric bypass) combined with lifestyle intervention is an effective and safe weight-loss treatment. This article compares the results of bariatric surgery and non-surgical treatment after one year.
Material and method
The 4XL study is an ongoing prospective clinical intervention study in patients aged 13–18 years who seek treatment at the Morbid Obesity Center, South-Eastern Norway Regional Health Authority, Vestfold Hospital Trust – a regional centre of excellence for the holistic and interdisciplinary treatment of morbid obesity in children, adolescents and adults. The study began in 2009, and the current analysis uses data from patients recruited in the period 8 October 2009–19 April 2018.
Children, adolescents and families with morbid obesity can be referred from either the primary or secondary healthcare services for treatment at the centre. At the first consultation, all families are informed about and invited to participate in the Vestfold Child Obesity Register ('Barnefedmeregisteret i Vestfold'), an opt-in prospective register, where personal information and biological material are collected for storage in a research biobank (4). Treatment is provided by an interdisciplinary team including a doctor, clinical nutritionist, nurse, specialist physiotherapist and health educator (appendix). The primary aim of the 4XL study is to clarify whether gastric bypass combined with lifestyle intervention provides greater health benefits than lifestyle intervention alone in the short and long term (1–10 years) and to survey complications after surgery.
As both the recruitment of suitable patients to the study and the dropout rate have been lower than expected, the study board has decided to analyse and publish the existing one-year data.
Participants
Patients who wish to undergo surgical treatment and who have completed at least one year of conservative interdisciplinary treatment in the Norwegian healthcare service without a satisfactory outcome can be referred for eligibility assessment for the 4XL study. Eligible patients undergo a standard length gastric bypass on a Roux limb (120 cm) in addition to standard lifestyle intervention (4). All anastomoses are performed using staples.
Inclusion criteria are age 13–18 years, BMI ≥ 40 kg/m2, or BMI ≥ 35 kg/m2 with at least one comorbidity, and Tanner stage 4–5 of pubertal development.
Exclusion criteria are BMI ≥ 55 kg/m2, significant risk of non-compliance, certain obesity syndromes, obesity caused by brain damage, and serious general illness.
The control group (those who receive lifestyle intervention) consists of patients who have not expressed a desire for surgery, but who have agreed to be included in the Vestfold Child Obesity Register, and who are undergoing conservative treatment at the centre over the same period. They must also meet the inclusion criteria for surgery (age, BMI). Some of the results following conservative treatment have been published previously (4).
Outcomes
The primary outcomes in this analysis are BMI and percentage weight loss one year after surgery/treatment start. Secondary outcomes are cardiometabolic risk factors (dyslipidaemia, inflammation, hypertension, dysglycaemia, fatty liver disease), early postoperative complications (graded from mild (grade I) to death (grade IV) within six weeks of surgery according to the Contracted Accordion Classification system), bone mineral density, anaemia, as well as various vitamin and mineral deficiencies (thiamine, vitamin B12, vitamin D, iron, calcium), and two-hour blood glucose after an oral glucose tolerance test. The primary outcomes were supplemented with measurement of waist circumference and body composition (fat percentage, fat mass, fat-free mass).
Measurements
Height is measured using a stadiometer (Seca 264, Seca, Hamburg, Germany), and weight and body composition are measured using bioelectrical impedance analysis (BC-418 Segmental Body Composition Analyzer, Tanita Corporation, Tokyo, Japan). Waist circumference is measured horizontally midway between the lowest rib and the iliac crest. Blood pressure is measured using Dinamap ProCare (GE Healthcare, Buckinghamshire, UK), and the average of three measurements is calculated. Smoking is self-reported (yes/no) upon inclusion.
Routine medical biochemical analyses are performed at the Department of Laboratory Medicine, Vestfold Hospital Trust. The laboratory is accredited according to the standard NS-EN ISO 15189. LDL cholesterol ≥ 2.8 mmol/L and non-HDL cholesterol ≥ 3.1 mmol/L were considered elevated, with an increased risk of cardiovascular disease (10). Normal glucose tolerance, prediabetes and type 2 diabetes are defined as HbA1c < 5.7 %, 5.7–6.4 % and ≥ 6.5 %, respectively (11). Hypertension is defined as systolic blood pressure ≥ 130 mm Hg or diastolic blood pressure ≥ 80 mm Hg (12). Bone mineral density (BMD z-score) and whole body bone mineral content (BMC) are measured via dual X-ray absorptiometry (DXA) with a Hologic Delphi W instrument (Hologic, Marlborough, MA, USA). Serum alanine aminotransferase values (s-ALT) above 34 U/L in boys and 24 U/L in girls were used as a surrogate marker for fatty liver disease (13).
Sample size
Based on our clinical experience, we expected an average weight loss of 25 % (10 BMI units) in the surgery group and up to 10 % (4 BMI units) in the lifestyle group (standard deviation (SD) 5). A total of 42 patients would need to complete the study (21 with surgery and 21 with conservative treatment) to provide more than 90 % power to detect such a difference (6 BMI units) with a significance level (alpha) of 0.01. The dropout rate was expected to be up to 30 %. We planned to include 50 patients in the surgery group to enable the incidence of serious postoperative complications to be assessed in addition.
Statistical methods
Treatment groups were compared prior to the start of treatment using t-tests, Mann-Whitney tests or Fisher's exact test. Changes from pre-treatment baseline to the one-year follow-up were analysed with paired t-tests or McNemar's test. The groups were compared after one year using analysis of covariance (ANCOVA), with adjustment for the baseline value of the dependent variable, unpaired t-tests, or logistic regression with the baseline value of the dependent variable as a covariate. P-values < 0.05 were considered statistically significant.
Ethics
The 4XL study has been approved by the Regional Committee for Medical and Health Research Ethics (REC) South-East (reference S-08584c 2008/14165) and recommended by the Data Protection Officer for Research and the Norwegian Centre for Research Data (project no. 21242). The Vestfold Child Obesity Register has been approved by the Regional Committee for Medical and Health Research Ethics (S-08742c 2008/19081), the Norwegian Centre for Research Data, has a concession from the Norwegian Data Protection Authority (20789 grh/rh) and has been recommended by a local Data Protection Officer. The Register's research biobank has been approved by the Norwegian Directorate of Health. The study was registered at ClinicalTrials.gov on 18 June 2009 (NCT00923819).
Results
A total of 510 adolescent patients began treatment at the Morbid Obesity Center, South-Eastern Norway Regional Health Authority, Vestfold Hospital Trust in the period 8 October 2009–19 April 2018 (Figure 1). Nineteen of 60 patients referred for surgery did not meet the inclusion criteria. The other 41 were eligible and underwent surgery, and 39 of these attended a one-year follow-up. A total of 139 patients began treatment in the lifestyle intervention group, of whom 96 attended a one-year follow-up. The patients in the lifestyle group who attended the one-year follow-up (n = 96) were slightly younger than those who did not attend (n = 43). There was also a tendency for those who did not attend to have higher bodyweight and a larger waist circumference (Table 1).
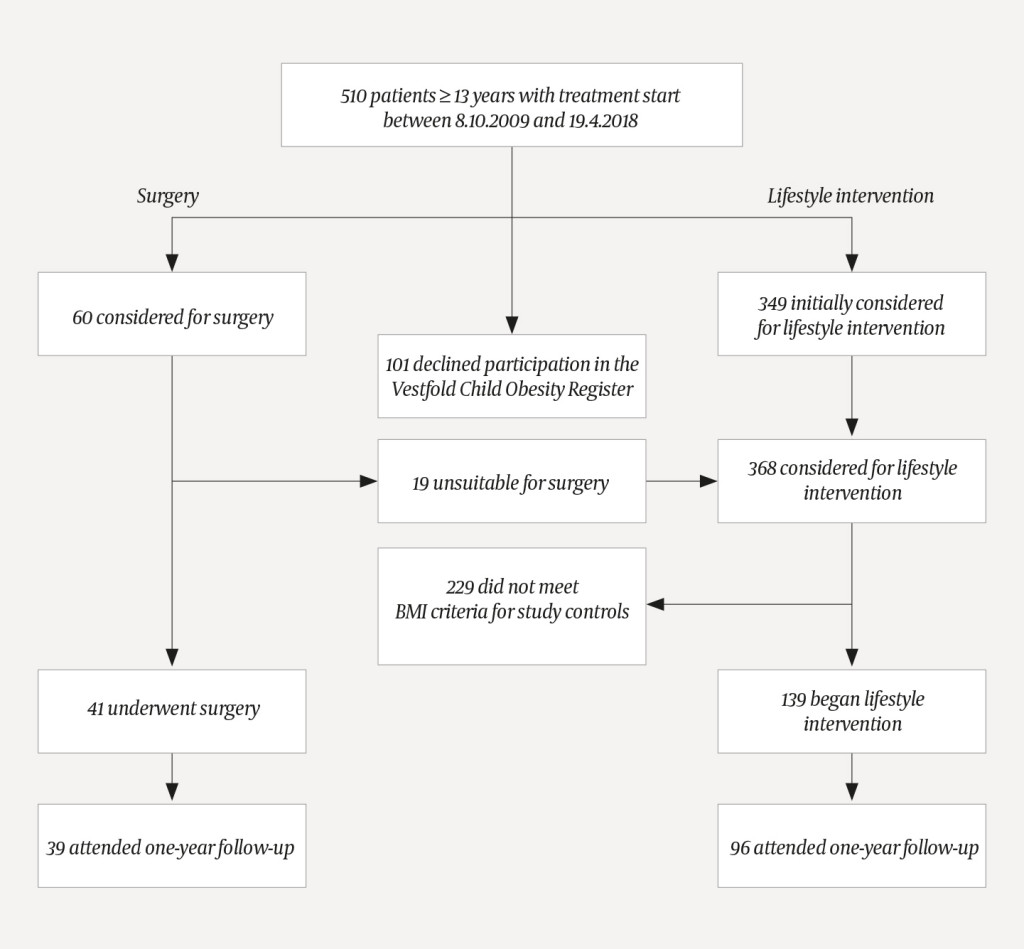
Table 1
Baseline characteristics of adolescents aged 13–18 years with morbid obesity who began lifestyle intervention treatment at the Morbid Obesity Center in Vestfold in the period 8 October 2009–19 April 2018. Data are presented separately for patients who attended and did not attend one-year follow-up. Values are presented as mean (SD) unless otherwise stated.
| Lifestyle intervention group who attended one-year follow-up | Lifestyle intervention group who did not attend one-year follow-up | ||
|---|---|---|---|
| Sex | |||
| Girls, number (%) | 55 (57) | 22 (51) | |
| Boys, number (%) | 41 (43) | 21 (49) | |
| Age (years) | 15.6 (1.3) | 16.1 (1.4) | |
| Anthropometry and body composition | |||
| Weight (kg) | 124 (20) | 130 (17) | |
| Height (cm) | 169 (9) | 172 (10) | |
| Body mass index (kg/m2) | 43.3 (4.1) | 44.0 (3.1) | |
| Waist circumference (cm) | 120 (13) | 124 (10) | |
| Fat percentage | 49 (6) | 49 (5) | |
| Fat mass (kg) | 61 (14) | 64 (11) | |
Before the start of treatment, patients in the surgery group (n = 39) were on average one year older and 2 BMI points heavier than those in the lifestyle group (n = 96) (Table 2). Gender distribution, mean waist circumference, fat mass, fat percentage and the percentage of patients with various cardiometabolic risk factors did not differ significantly between the groups (Table 2).
Table 2
Baseline characteristics of adolescents aged 13–18 years with morbid obesity who began treatment at the Morbid Obesity Center in Vestfold in the period 8 October 2009–19 April 2018 and who attended one-year follow-up. Values are presented as number (%) unless otherwise stated.
| Surgery + | Lifestyle intervention (n = 96) | P-value1 | ||
|---|---|---|---|---|
| Sex | ||||
| Girls | 25 (64) | 55 (57) | 0.56 | |
| Boys | 14 (36) | 41 (43) | ||
| Age (years) | ||||
| Median (from lowest to highest value) | 16.9 (14.2–18.0) | 15.6 (13.0–18.0) | < 0.001 | |
| Anthropometry and body composition, mean (SD) | ||||
| Body weight (kg) | 132 (14) | 124 (20)2 | 0.024 | |
| Height (cm) | 170 (8) | 169 (9)2 | 0.42 | |
| BMI (kg/m2) | 45.6 (4.4) | 43.3 (4.1)2 | 0.004 | |
| Waist circumference (cm) | 124 (11) | 120 (13)3 | 0.098 | |
| Fat percentage | 50 (6)4 | 49 (6)5 | 0.53 | |
| Fat mass (kg) | 66 (11)4 | 61 (14)5 | 0.075 | |
| Fat-free mass (kg) | 66 (10)4 | 63 (12)5 | 0.13 | |
| Cardiometabolic risk factors | ||||
| Hypertension | 8 (21) | 19 (20) | 1.00 | |
| Hypercholesterolaemia (non-HDL) | 22 (56) | 65 (68) | 0.24 | |
| C-reactive protein ≥ 3 mg/L | 31 (80) | 66 (70)2 | 0.39 | |
| Smoker | 8 (21) | 10 (10)3 | 0.18 | |
| Type 2 diabetes | 3/38 (8) | 1 (1) | 0.12 | |
| Prediabetes | 6/38 (16) | 14 (15)2 | ||
| Normal glucose tolerance | 29/38 (76) | 79 (84)2 | ||
| Fatty liver disease | ||||
| ALT > 24 U/L girls/> 34 U/L boys | 17/39 (44) | 43/95 (45) | 1.00 | |
1t-test, Mann-Whitney test or Fisher's exact test.
2n = 94
3n = 92
4n = 37
5n = 93
Primary outcomes
BMI decreased by an average of 14.1 (95 % CI 12.7 to 15.6) points in the surgery group and by 0.4 (−0.3 to 1.2) points in the lifestyle group. The estimated between-group difference after one year was 13.2 (11.7 to 14.7) BMI points. A total of 23 (25 %) and 13 (14 %) patients in the lifestyle group had a BMI reduction of at least 5 % and 10 % respectively, compared with 100 % and 97 % in the surgery group (Figure 2). Mean percentage weight loss was 30 % (27 to 33 %) in the surgery group compared with a weight gain of 1 % (−1 to 3 %) in the lifestyle group; observed difference 31 % (27 to 34 %), p <0.001 (Table 3).
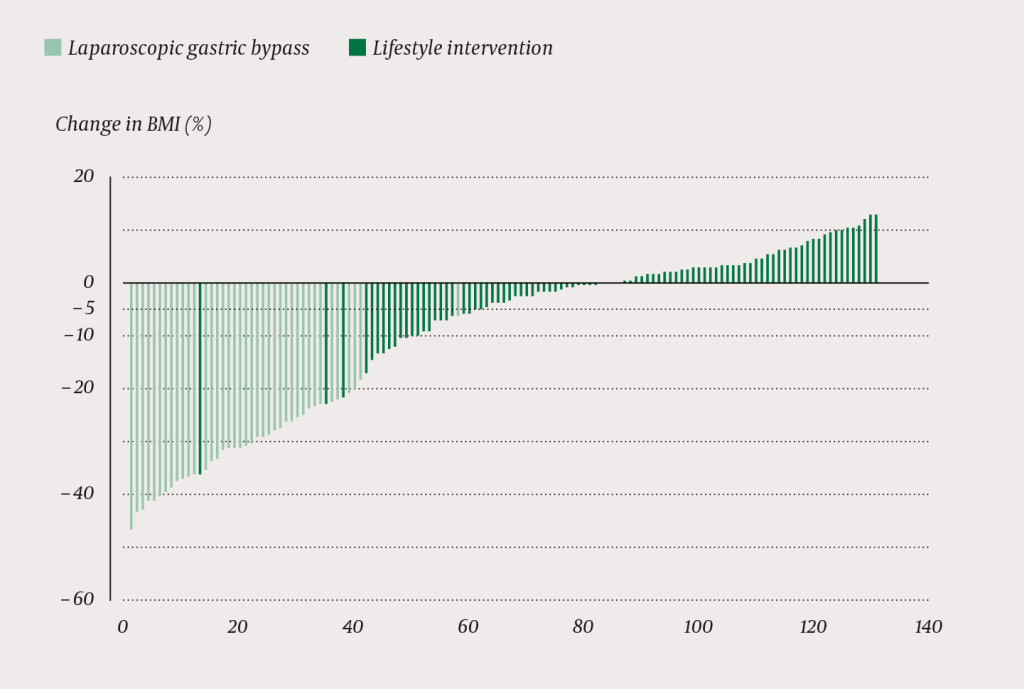
Table 3
Observed primary (BMI and percentage weight change) and secondary outcome measures at one-year follow-up and baseline-adjusted estimated differences or observed percentage differences between the groups. Included are adolescents with morbid obesity who began treatment at the Morbid Obesity Center in Vestfold in the period 8 October 2009–19 April 2018 and who attended one-year follow-up. Values are presented as mean (SD) unless otherwise stated.
| Surgery + | Lifestyle intervention (n = 96)1 | Between-group difference or odds ratio (95 % CI) | P-value2 | |||||
|---|---|---|---|---|---|---|---|---|
| Primary endpoints and body composition | ||||||||
| BMI (kg/m2) | 31.5 (4.4) | 42.7 (5.2) | 13.2 (11.7 to 14.7) | < 0.001 | ||||
| BMI change (95 % CI) | −14.1 (−15.6 to −12.7) | −0.4 (−1.2 to 0.3) | Not calculated | |||||
| Percentage weight change (95 % CI) | −30 (−33 to −27) | 1 (−1 to 3) | 31 (27 to 34) | < 0.001 | ||||
| Waist circumference (cm) | 95 (12) | 118 (13) | 26 (22 to 29) | < 0.001 | ||||
| Fat mass (kg) | 31.6 (9.7) | 58.2 (14.2) | 31.3 (27.2 to 35.5) | < 0.001 | ||||
| Fat-free mass (kg) | 60.7 (11.2) | 63.4 (11.5) | 6.0 (3.5 to 8.5) | < 0.001 | ||||
| Fat percentage | 35 (10) | 47 (7) | 14 (12 to 17) | < 0.001 | ||||
| Secondary endpoints | ||||||||
| Dyslipidaemia | ||||||||
| Total cholesterol (mmol/L) | 3.6 (0.7) | 4.4 (0.8) | 0.84 (0.63 to 1.05) | < 0.001 | ||||
| LDL cholesterol (mmol/L) | 2.0 (0.7) | 2.7 (0.8) | 0.82 (0.61 to 1.03) | < 0.001 | ||||
| HDL cholesterol (mmol/L) | 1.3 (0.3) | 1.2 (0.2) | −0.23 (−0.30 to −0.16) | < 0.001 | ||||
| Triglycerides (mmol/L) | 0.9 (0.3) | 1.5 (0.8) | 0.61 (0.35 to 0.86) | < 0.001 | ||||
| Non-HDL cholesterol ≥ 3.1 mmol/L | 5/38 (13 %) | 56/88 (64 %) | 0.06 (0.02 to 0.19) | < 0.001 | ||||
| LDL cholesterol ≥ 2.8 mmol/L | 4/38 (11 %) | 41/87 (47 %) | 0.08 (0.02 to 0.30) | < 0.001 | ||||
| Inflammation | ||||||||
| C-reactive protein (mg/L) (median/25–75 %) | 0.4 (0.1–0.8) | 4.0 (1.6–8.0) | 3.7 (1.9 to 5.5) | < 0.001 | ||||
| C-reactive protein ≥ 3 mg/L | 2/39 (5 %) | 56/91 (62 %) | 0.016 (0.003 to 0.077) | < 0.001 | ||||
| Hypertension | ||||||||
| Systolic blood pressure ≥ 130 mm Hg or diastolic blood pressure ≥ 80 mm Hg | 2/39 (5 %) | 13/89 (15 %) | 0.29 (0.06 to 1.41) | 0.13 | ||||
| Dysglycaemia and insulin | ||||||||
| Type 2 diabetes or prediabetes | 0/37 (0 %) | 13/86 (15 %) | NA | 0.010 | ||||
| HbA1c (%) | 5.3 (1.0) | 5.4 (0.5) | 0.11 (0.02 to 0.19) | 0.019 | ||||
| Fasting blood glucose (mmol/L) | 4.6 (0.8) | 4.9 (1.1) | 0.41 (0.20 to 0.63) | < 0.001 | ||||
| Insulin (pmol/L) | 58 (22) | 200 (172) | 129 (73 to 185) | < 0.001 | ||||
| Homeostatic model assessment of insulin resistance | 2.0 (0.8) | 7.7 (9.0) | 5.0 (2.5 to 7.4) | < 0.001 | ||||
| Fatty liver disease | ||||||||
| ALT (U/L) | 23 (11) | 35 (31) | 9 (1 to 16) | 0.025 | ||||
| ALT > 24 U/L girls/> 34 U/L boys | 8/38 (21 %) | 43/88 (49 %) | 0.20 (0.07 to 0.56) | 0.005 | ||||
1The majority of one-year values are based on data from at least 37 of 39 (95 %) patients in the surgery group (with the exception of insulin level and Homeostatic Model Assessment of Insulin Resistance (HOMA-IR), 36/39), and at least 88 of 96 (92 %) patients in the control group (with the exception of waist circumference, 81/96, insulin level and HOMA-IR, 85/96).
2Changes from pre-treatment baseline to one-year follow-up were analysed with paired t-tests. Between-group comparisons after one year were performed using analysis of covariance (ANCOVA) adjusting for baseline values of the dependent variable, unpaired t-tests, quantile regression or logistic regression with the baseline value of the dependent variable as a covariate.
Secondary outcomes
The percentage of patients with hypercholesterolaemia or elevated C-reactive protein (≥ 3 mg/L) fell significantly more in the surgery group than in the lifestyle group, all odds ratios (OR) < 0.09 (Table 3). All patients with dysglycaemia (type 2 diabetes or prediabetes) were normoglycaemic one year after surgery, and no normoglycaemic patients developed dysglycaemia after surgery. A total of 8 of 14 (57 %) patients with prediabetes in the lifestyle group became normoglycaemic, whereas 6 of 71 (9 %) normoglycaemic patients developed prediabetes.
Complications and adverse effects
Two early (<6 weeks) minor surgical complications were registered. There were no statistically significant reductions in mean haemoglobin, albumin or vitamins and minerals at the one-year follow-up, but 4 (10 %) patients had anaemia, 8 (21 %) had iron deficiency and 4 (10 %) had low vitamin B12. A total of 20 of 33 (61 %) patients had low two-hour blood glucose (< 2.8 mmol/L) after an oral glucose tolerance test (Table 4). Bone mineral content (BMC) and bone mineral density (BMD z-score) both decreased significantly, by an average of 3.5 % (BMC) and 0.5 standard deviations (BMD z-score), both p-values < 0.001 (Table 4). One patient had a BMD z-score < −2.0 (−2.1) after one year.
Table 4
Vitamins, minerals, albumin, haemoglobin, bone health and hypoglycaemia after 75 g glucose in an oral glucose tolerance test, prior to the start of treatment and after one year in adolescents with morbid obesity who underwent a gastric bypass in combination with lifestyle intervention at the Morbid Obesity Center in Vestfold in the period 8 October 2009–19 April 2018 and who attended one-year follow-up. Mean (SD) or number (%).
| Outcome measure | Baseline | One-year1 | Change (95 % CI) | P-value2 | |
|---|---|---|---|---|---|
| Haemoglobin and anaemia | |||||
| Haemoglobin (g/dL) | 13.7 (1.1) | 13.5 (1.5) | −0.19 (−0.50 to 0.11) | 0.21 | |
| Hb <12 g/dL girls/<13 g/dL boys | 1/39 (2.6 %) | 4/39 (10 %) | 0.63 | ||
| Albumin (g/L) | 41.9 (3.0) | 40.9 (3.6) | −1.0 (−2.02 to 0.07) | 0.067 | |
| Iron and iron deficiency | |||||
| Ferritin (µg/L) | 50 (30) | 47 (42) | −3 (−16 to 10) | 0.65 | |
| Ferritin <15 µg/L | 0/39 (0 %) | 8/39 (21 %) | NA | ||
| Vitamins, PTH and calcium | |||||
| Thiamine (nmol/L) | 165 (32) | 158 (33) | −7 (−16 to 2) | 0.14 | |
| Vitamin B12 (pmol/L) | 304 (126) | 467 (381) | 163 (48 to 278) | 0.007 | |
| Vitamin B12 < 150 pmol/L | 1/39 (2.6 %) | 4/38 (10 %) | 0.38 | ||
| Vitamin D (nmol/L) | 48 (20) | 48 (19) | 0 (−7 to 6) | 0.92 | |
| Vitamin D < 50 nmol/L | 23/38 (59 %) | 22/37 (56 %) | 1.0 | ||
| Calcium, albumin-corrected (mmol/L) | 2.39 (0.07) | 2.41 (0.05) | 0.013 (−0.009 to 0.035) | 0.24 | |
| Parathyroid hormone (PTH) (pmol/L) | 5.2 (1.8) | 4.7 (1.2) | −0.3 (−0.8 to 0.2) | 0.21 | |
| Secondary hyperparathyroidism | 3/39 (8 %) | 2/38 (5 %) | 1.0 | ||
| Bone health | |||||
| Bone mineral content, BMC (g) | 2 642 (283) | 2 590 (361) | –92 (–134 to −50) | < 0.001 | |
| Bone mineral density, BMD z-score | 1.19 (1.08) | 0.67 (1.07) | −0.51 (−0.66 to −0.36) | < 0.001 | |
| Hypoglycaemia | |||||
| Glucose after oral glucose tolerance test < 2.8 mmol/L | 0/37 (0 %) | 20/33 (61 %) | NA | ||
1All baseline and one-year values are based on data from at least 37 of 39 (95 %) patients (with the exception of serum glucose after an oral glucose tolerance test at one-year follow-up).
2Paired t-test or McNemar's test.
Discussion
The results from the non-randomised 4XL study show significantly greater one-year weight loss and improvement in cardiometabolic risk factors after gastric bypass combined with lifestyle intervention than after lifestyle intervention alone. However, the non-randomised study design, the relatively small number of patients who underwent surgery, and the short follow-up time preclude us from evaluating whether the benefits of weight loss outweigh the risk of long-term complications. Nor can we exclude the possibility that systematic differences between the treatment groups in both selection and dropout may have affected the outcomes, reducing the internal validity and generalisability.
As of 9 October 2020, only a single randomised controlled study had been published comparing the effects of lifestyle intervention to those of bariatric surgery in adolescents, and even this study featured a type of surgery (gastric banding) that is rarely used (14). The effects on BMI of laparoscopic Roux-en-Y gastric bypass surgery versus caloric restriction (low calorie diet) are being compared in an ongoing randomised controlled trial of 13–16-year-olds with BMI > 35 kg/m2. The results from this study may strengthen the existing evidence base (https://clinicaltrials.gov/ct2/show/NCT02378259).
Our results are consistent with findings from two non-randomised studies that showed approximately 30 % weight loss one and two years after gastric bypass surgery, respectively (15, 16). The Swedish AMOS study compared gastric bypass surgery with conventional treatment and showed 31–32 % weight loss in the surgery group versus 3 % weight gain in the control group (16). A US study showed approximately 30 % weight loss one and two years after bypass surgery (15). The significant improvement in cardiometabolic risk factors in the surgery group confirms findings from previous observational studies (16, 17).
Two (5 %) postoperative complications were recorded, which is in accordance with international experience (16, 18). The risk of long-term complications following bariatric surgery in adolescents is poorly documented (9) and has not been examined in the current analysis either.
Anaemia and vitamin and mineral deficiencies are known adverse effects after gastric bypass (7, 16). In the current study, mean levels of haemoglobin, ferritin, calcium, vitamin D and vitamin B12 had not fallen significantly after one year. However, at the one-year follow-up, a number of patients had anaemia, iron deficiency or low vitamin B12 levels (Table 4), and about 2 out of 3 patients (61 %) had two-hour hypoglycaemia after an oral glucose tolerance test (blood sugar < 2.8 mmol/L). The incidence of two-hour hypoglycaemia was higher than shown previously in adults (19, 20), and lower age is known to be a risk factor (21). No fractures were recorded, and bone mineral measurements did not show a decrease in (mean) bone density to below that expected for age. It is nevertheless concerning that gastric bypass surgery is associated with an increased fracture risk (22) and postprandial hypoglycaemia. Lifelong follow-up with diagnostic testing and use of preventive measures would seem to be necessary.
The 4XL study is ongoing, and a ten-year follow-up is planned. A particular strength of the study is that the intervention group is being compared with an actively treated control group, with both groups of participants fulfilling the same inclusion criteria. In addition, the study is being run by a centre with specialist expertise in family-based lifestyle interventions in adolescents, bariatric surgery and clinical research. The complexity of the assessment and follow-up of this patient group requires a seamless and close collaboration between healthcare professionals specialising in the treatment of childhood obesity and surgeons with expertise in bariatric surgery.
Weaknesses of the study include the relatively small number of patients in the surgery group, the long recruitment period and differences between the groups in baseline age (17 years vs. 16 years) and BMI (45.6 kg/m2 vs. 43.3 kg/m2). The latter, however, had little effect on the between-group difference in the change in the primary outcome measure, which was adjusted for baseline weight in the primary analyses, and further adjustment for age did not affect the results. Although the sample size was lower than planned (n = 50 in the surgery group), the dropout rate (5 %) was lower than expected (30 %). The study therefore had sufficient power to answer the primary research question on weight loss as soon as 39 patients had attended the one-year follow-up.
A recently published meta-analysis showed that health-related quality of life improved significantly after surgery in adolescents, especially in the first few years, but that few data are available on the long-term incidence of psychosocial and mental health problems (23). Long-term results from the AMOS study show that mental health problems do not necessarily decrease after gastric bypass surgery in adolescents, and that individuals who undergo surgery may have a greater need for psychiatric help than those who do not undergo surgery (24). Health-related quality of life, psychological status, eating behaviour and long-term complications are all topics for future analyses and publications from the 4XL study.
Our results confirm that laparoscopic Roux-en-Y gastric bypass can be performed with satisfactory weight loss, improvement of cardiometabolic risk factors and a low incidence of early postoperative complications. The study also indicates that the incidence of adverse effects and complications is similar in the short-term to that observed in adults (7), but the study is too small at present to be able to draw definite conclusions about the incidence and severity of complications. Little is known about the long-term effects and complications of weight loss surgery in adolescents (9). It is therefore difficult to know whether bariatric surgery should be offered to more young people with morbid obesity, or whether it is better to recommend waiting until adulthood. Arguments for obesity surgery in adolescence are the possibility of significant weight loss, improved quality of life and a reduced risk of future obesity-related disease. Arguments against are the risk of serious complications, anaemia, hypoglycaemia, vitamin and mineral deficiencies, and mental health problems.
We are grateful to all the patients and their families who participated in this study and consented to use of their data.
We also wish to thank all those working in the paediatrics section of the Morbid Obesity Center, South-Eastern Norway Regional Health Authority, Vestfold Hospital Trust. Special thanks to Nina Wahlmann Iversen and Berit Mossing Bjørkås for data management and quality assurance. Many thanks also to Martin Handeland who had the idea for the 4XL study and who was in charge of developing its design and the initiation of the study.
This article has been peer-reviewed.
- 1.
Must A, Strauss RS. Risks and consequences of childhood and adolescent obesity. Int J Obes Relat Metab Disord 1999; 23 (Suppl 2): S2–11. [PubMed][CrossRef]
- 2.
Llewellyn A, Simmonds M, Owen CG et al. Childhood obesity as a predictor of morbidity in adulthood: a systematic review and meta-analysis. Obes Rev 2016; 17: 56–67. [PubMed][CrossRef]
- 3.
Steinbeck KS, Lister NB, Gow ML et al. Treatment of adolescent obesity. Nat Rev Endocrinol 2018; 14: 331–44. [PubMed][CrossRef]
- 4.
Skodvin VA, Lekhal S, Kommedal KG et al. Livsstilsbehandling av barn og ungdom med alvorlig fedme – resultater etter ett år. Tidsskr Nor Legeforen 2020; 11: 901–7.
- 5.
Al-Khudairy L, Loveman E, Colquitt JL et al. Diet, physical activity and behavioural interventions for the treatment of overweight or obese adolescents aged 12 to 17 years. Cochrane Database Syst Rev 2017; 6: CD012691. [PubMed][CrossRef]
- 6.
Hofsø D, Fatima F, Borgeraas H et al. Gastric bypass versus sleeve gastrectomy in patients with type 2 diabetes (Oseberg): a single-centre, triple-blind, randomised controlled trial. Lancet Diabetes Endocrinol 2019; 7: 912–24. [PubMed][CrossRef]
- 7.
Jakobsen GS, Småstuen MC, Sandbu R et al. Association of Bariatric Surgery vs Medical Obesity Treatment With Long-term Medical Complications and Obesity-Related Comorbidities. JAMA 2018; 319: 291–301. [PubMed][CrossRef]
- 8.
Treadwell JR, Sun F, Schoelles K. Systematic review and meta-analysis of bariatric surgery for pediatric obesity. Ann Surg 2008; 248: 763–76. [PubMed][CrossRef]
- 9.
Ruiz-Cota P, Bacardí-Gascón M, Jiménez-Cruz A. Long-term outcomes of metabolic and bariatric surgery in adolescents with severe obesity with a follow-up of at least 5 years: A systematic review. Surg Obes Relat Dis 2019; 15: 133–44. [PubMed][CrossRef]
- 10.
Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and AdolescentsNational Heart, Lung, and Blood Institute. . Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report. Pediatrics 2011; 128 (suppl 5): S213–56. [CrossRef]
- 11.
American Diabetes Association. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2020. Diabetes Care 2020; 43 (Suppl 1): S14–31. [PubMed][CrossRef]
- 12.
Dong Y, Song Y, Zou Z et al. Updates to pediatric hypertension guidelines: influence on classification of high blood pressure in children and adolescents. J Hypertens 2019; 37: 297–306. [PubMed][CrossRef]
- 13.
Johansen MJ, Gade J, Stender S et al. The Effect of Overweight and Obesity on Liver Biochemical Markers in Children and Adolescents. J Clin Endocrinol Metab 2020; 105: dgz010. [PubMed][CrossRef]
- 14.
O'Brien PE, Sawyer SM, Laurie C et al. Laparoscopic adjustable gastric banding in severely obese adolescents: a randomized trial. JAMA 2010; 303: 519–26. [PubMed][CrossRef]
- 15.
Inge TH, Courcoulas AP, Jenkins TM et al. Weight Loss and Health Status 3 Years after Bariatric Surgery in Adolescents. N Engl J Med 2016; 374: 113–23. [PubMed][CrossRef]
- 16.
Olbers T, Gronowitz E, Werling M et al. Two-year outcome of laparoscopic Roux-en-Y gastric bypass in adolescents with severe obesity: results from a Swedish Nationwide Study (AMOS). Int J Obes 2012; 36: 1388–95. [PubMed][CrossRef]
- 17.
Black JA, White B, Viner RM et al. Bariatric surgery for obese children and adolescents: a systematic review and meta-analysis. Obes Rev 2013; 14: 634–44. [PubMed][CrossRef]
- 18.
Arafat M, Norain A, Burjonrappa S. Characterizing Bariatric Surgery Utilization and Complication Rates in the Adolescent Population. J Pediatr Surg 2019; 54: 288–92. [PubMed][CrossRef]
- 19.
Hofsø D, Nordstrand N, Johnson LK et al. Obesity-related cardiovascular risk factors after weight loss: a clinical trial comparing gastric bypass surgery and intensive lifestyle intervention. Eur J Endocrinol 2010; 163: 735–45. [PubMed][CrossRef]
- 20.
Pigeyre M, Vaurs C, Raverdy V et al. Increased risk of OGTT-induced hypoglycemia after gastric bypass in severely obese patients with normal glucose tolerance. Surg Obes Relat Dis 2015; 11: 573–7. [PubMed][CrossRef]
- 21.
Hofsø D, Birkeland KI, Holst JJ et al. Gastric bypass surgery has a weight-loss independent effect on post-challenge serum glucose levels. Diabetol Metab Syndr 2015; 7: 69. [PubMed][CrossRef]
- 22.
Paccou J, Martignène N, Lespessailles E et al. Gastric Bypass But Not Sleeve Gastrectomy Increases Risk of Major Osteoporotic Fracture: French Population-Based Cohort Study. J Bone Miner Res 2020; 35: 1415–23. [PubMed][CrossRef]
- 23.
Trooboff SW, Stucke RS, Riblet NB et al. Psychosocial Outcomes Following Adolescent Metabolic and Bariatric Surgery: a Systematic Review and Meta-Analysis. Obes Surg 2019; 29: 3653–64. [PubMed][CrossRef]
- 24.
Järvholm K, Bruze G, Peltonen M et al. 5-year mental health and eating pattern outcomes following bariatric surgery in adolescents: a prospective cohort study. Lancet Child Adolesc Health 2020; 4: 210–9. [PubMed][CrossRef]