Lifestyle intervention for children and adolescents with severe obesity – results after one year
Main findings
A lifestyle intervention for children and adolescents with severe obesity revealed moderate mean changes in body weight measures and body composition after one year.
We found large interindividual differences in changes in obesity parameters after one year of treatment.
There was a tendency for boys to show larger reductions in obesity parameters.
Obesity in children and adolescents is a major health challenge. Psychosocial complications are common in children with severe obesity, and cardiometabolic and orthopaedic complications may also occur (1). Moreover, childhood obesity is strongly associated with adult obesity, thus also with an increased risk of cardiovascular disease and premature death (2).
The most recent Cochrane review of family-based lifestyle intervention for children aged 6 to 11 years showed a small mean change of -0.06 in the BMI standard deviation score (body mass index z-score) (95 % CI -0.10 – -0.02) on follow-up after 6–36 months (3).
A similar review for adolescents aged 12–17 showed a mean change in the BMI standard deviation score of -0.13 (95 % CI -0.21 – -0.05) on follow-up after 6–24 months (4). These results underline the need for better treatment programmes, and more structured interventions have been sought (5). In these, a focus on the whole family is important, and both the number and duration of consultations appear to be correlated with therapeutic efficacy (6).
There are few specialist outpatient clinics in Norway that offer interdisciplinary, family-based intervention for children and adolescents with severe obesity. The Obesity Centre at Haukeland University Hospital, Bergen, and the Morbid Obesity Centre, South-Eastern Norway Regional Health Authority at Vestfold Hospital, Tønsberg, represent two of the largest. The centre in Tønsberg is additionally the regional centre of excellence of the South-Eastern Norway Regional Health Authority.
The purpose of this quality assessment project was to investigate changes in body weight measures (level of overweight as defined by the International Obesity Task Force (%IOTF-25), the BMI standard deviation score, waist circumference standard deviation score and body fat percentage measured by means of bioimpedance analysis (%BF-BIA)) after one year of family-based lifestyle intervention in two Norwegian specialist clinics. We also wanted to investigate whether the treatment centre, age, sex or initial BMI were associated with these changes. The analysis is limited to changes in measures of body weight and composition. These are relatively simple to measure, and the degree of their reduction is a good surrogate measure of improvement in obesity-related somatic and psychological diseases (6).
Material and method
Inclusion criteria were the same as the clinics' intake criteria: age ≤ 18 years, a BMI that corresponds to the International Obesity Task Force's definition of severe obesity (7), i.e. a BMI ≥ iso-BMI 35 in Bergen or 5 BMI units over iso-BMI 30 in Tønsberg, or BMI ≥ iso-BMI 30 in the presence of obesity-related comorbidity. Iso-BMIs are age- and sex-adjusted BMI percentiles that extrapolate the BMI 25, 30 and 35 cut-off points of overweight, obesity and morbid obesity in adults to children and adolescents. These lines are shown on the Norwegian BMI curves. Data were collected in the period 1.2.2012–1.10.2016 and included measurements at the start and all one-year follow-up measurements (9–15 months) taken in this period.
Intervention
Both clinics offer a two-year, family-based programme, combined with a follow-up in a primary health setting by a public health nurse or GP. The intervention period was personalised, i.e. shortened in the event of a good response at the one-year check-up or extended if it was considered to be clinically necessary. Interventions were based on national guidelines for the treatment of overweight and obesity in children and adolescents (8), as summarised in the appendix. Both programmes included conversations with a doctor or nurse specialist. In Bergen, the family also met a physiotherapist and a clinical dietitian in the course of the first month, while members of these professions were present at an interactive group meeting after three months in Tønsberg. Children were referred for assessment or follow-up by a psychologist or a child and adolescent psychiatric clinic when needed. The programme in Bergen was exclusively based on individual consultations, while the Tønsberg programme included two group meetings.
Anthropometric data
The participants' height was measured with a stadiometer (Seca 264, Hamburg, Germany) and recorded to the nearest 0.1 centimetre. Weight was measured to the nearest 0.1 kg and the percentage of body fat was obtained from bioimpedance analysis with an InBody720 (Biospace, Seoul, Korea) device in Bergen, and a Tanita Segmental BC-418 Body Composition Analyzer (Tanita Corp, Tokyo, Japan) in Tønsberg. Waist circumference was measured with a tape measure placed horizontally at the narrowest level or at the midpoint between the lowest rib and the iliac crest. All measurements at were taken by trained staff members (a medical assistant in Bergen and a nurse or doctor in Tønsberg).
The %IOTF-25 expresses the BMI as a percentage relative to the International Obesity Task Force's overweight criterion, calculated as 100 × (BMI/iso-BMI 25) (9), where BMI is the Body Mass Index of the child, and iso-BMI 25 is the IOTF cut-off value that defines overweight (iso-BMI 25). The degree of obesity was also determined using the IOTF reference curve as explained above, and categorized as normal weight, overweight, obesity of severe obesity (BMI ≥ iso-BMI 35). BMI standard deviation scores and waist circumference standard deviation scores were calculated using Norwegian growth references (10, 11).
Statistical analyses
Descriptive statistics are presented as means with standard deviations for continuous variables and as percentages for categorical variables. The treatment locations were compared by means of linear regression analysis with adjustment for age and sex. When analysing anthropometric changes after one year, we also included the baseline values in the model, as this is the generally preferred method (12). All models were checked by assessing the distribution of residuals and presence of spurious outliers. Changes in %IOTF-25, BMI standard deviation scores, waist circumference standard deviation scores and body fat percentage after one year of treatment were divided by the follow-up time interval in order to obtain an estimate of the annual change prior to the analyses (e.g. (BMI standard deviation score at follow-up minus BMI standard deviation score at baseline)/ time interval (years)). Fully adjusted linear regression analysis was carried out, with measures of bodyweight as outcomes, age at programme start (<12 years, an age limit widely used in published literature as the transition from child to adolescent), sex and treatment site as predictors. The data were analysed using IBM SPSS version 24 (International Business Machines Corporation, Armonk, New York, USA) and R version 3.2 (R Foundation for Statistical Computing, Vienna, Austria).
Ethics
The Bergen part of the study was assessed by the Regional Committee for Medical and Health Research Ethics of the Western Norway Regional Health Authority as a quality assurance project (REK 2016/1893), with advice from the Data Protection Officer, Haukeland University Hospital (2017/5132). The Vestfold Child Obesity Register is approved by the Regional Ethics Committee (S-08742c 2008/19081), the Norwegian Centre for Research Data, and has a concession from the Norwegian Data Inspectorate (20689 grh/rh). The Directorate of Health has approved it as a research biobank, and the local Data Protection Officer has given advice. The current analyses based on data from the Vestfold Child Obesity Register have been approved by the Regional Ethics Committee for South-Eastern Norway D (2019/911) and by the Data Protection Officer at Vestfold Hospital.
Results
A total of 416 of 568 children (73 %) who started treatment completed one year's follow-up and were included in the analyses, 181 from Bergen and 235 from Tønsberg. The children were 3 to 18 years old, and 219 (53 %) were girls. Demographic and anthropometric characteristics at the start of treatment and after one year are presented in Table 1. The participants from Tønsberg were on average one year older than those from Bergen, and had a higher %IOTF-25 and BMI standard deviation score after adjustment for age and sex. At follow-up after one year, in both treatment sites there was a significant decrease in all anthropometric variables adjusted for age, sex and initial value (Table 1).
Table 1
Demographic characteristics and changes in anthropometric variable after one year of family-based lifestyle intervention in children with severe obesity at two specialist clinics in the period 2012–2016. Data are presented as mean ± SD, mean (95 % CI) or %.
| Bergen (n = 181) | Tønsberg (n = 235) | ||
|---|---|---|---|
| Baseline | |||
| Proportion of girls (%) | 54.1 | 51.5 | |
| Age, years | 11.6 ± 3.4 | 12.9 ± 3.3 | |
| %IOTF-251 | 150.8 ± 14.5 | 161.2 ± 22.4 | |
| BMI standard deviation score2 | 3.07 ± 0.43 | 3.31 ± 0.61 | |
| BMI > IOTF-35 (%)3 | 77.9 | 78.3 | |
| Waist circumference standard deviation score4 | 3.05 ± 0.41 | 3.14 ± 0.51 | |
| Body fat percentage (BIA)5 | 43.0 ± 5.7 | 43.6 ± 6.7 | |
| Follow-up | |||
| Age | 12.6 ± 3.4 | 13.8 ± 3.3 | |
| %IOTF-251 | 148.0 ± 16.8 | 154.7 ± 23.6 | |
| BMI standard deviation score2 | 3.01 ± 0.51 | 3.22 ± 0.76 | |
| BMI > IOTF-35 (%)3 | 62.4 | 69.8 | |
| Waist circumference standard deviation score4 | 3.01 ± 0.76 | 3.04 ± 0.52 | |
| Fat percentage (BIA)5 | 41.6 ± 6.9 | 42.0 ± 7.5 | |
| Change after one year6 | |||
| %IOTF-251 | −2.76 (−4.21 – −1.32) | −5.42 (−7.02 – −3.83) | |
| BMI standard deviation score2 | −0.06 (−0.11 – −0.02) | −0.09 (−0.14 – −0.04) | |
| Waist circumference standard deviation score4 | -0.03 (-0.10–0.04) | −0.11 (−0.16 – −0.05) | |
| Fat percentage (BIA)5 | −1.33 (−2.14 – −0.53) | −1.36 (−1.94 – −0.77) | |
1Percentage above the International Obesity Task Force's overweight criterion for children and adolescents
2Body mass index (BMI) standard deviation scores, calculated with Norwegian growth charts as reference
3BMI ≥ IOTF-35 (%), percentage of children above the IOTF criterion for severe obesity in children and adolescents
4Waist measurement standard deviation score, calculated using Norwegian growth reference, n = 160 in Bergen and n = 228 in Tønsberg at the start (data missing for 21 and 7), and n = 138 and n = 203 on follow-up (data missing for 43 and 32)
5Fat percentage measured by bioimpedance analysis, n = 163 in Bergen and n = 221 in Tønsberg at the start (data missing for 18 and 4) and 149 and 229, respectively, at follow-up (data missing for 32 and 6)
6(Follow-up minus initial value)/follow-up interval: All one-year changes are statistically significant, adjusted for age, sex and initial value (p < 0.001)
The correlation between age, sex, initial value and treatment site and the change in anthropometric variables after one year are presented in Table 2. A negative regression coefficient in this table reflects a reduction in the parameter being analysed. A positive regression coefficient corresponds to an increase. Children less than 12 years old had a significantly larger mean reduction in BMI standard deviation score (0.13) and waist circumference standard deviation score (0.18) than those aged 12 or more. This was not observed for %IOTF-25 or fat percentage. Girls responded more poorly to treatment than boys for all parameters; for example, the mean reduction in %IOTF-25 was 3 % less in girls than in boys. Higher initial values were related to a larger reduction in %IOTF-25, waist circumference standard deviation scores and fat percentage, but not for BMI standard deviation scores. There was no statistically significant difference between the results of the treatment centres (Table 2). Individual changes in %IOTF-25 are shown in Figure 1.
Table 2
Anthropometric outcomes after one year of family-based lifestyle intervention (∆1) in children with severe obesity at two specialist clinics in 2012–2016, adjusted for initial values and other covariates. Non-standardised regression coefficients (95 % CI) adjusted for other covariates in the table
| Predictors | ∆1%IOTF-25 1 (n = 416) | ∆1BMI-standard deviation score2 (n = 416) | ∆1Waist circumference standard deviation scores3 (n = 341) | ∆1Fat percentage 4 (n = 378) |
|---|---|---|---|---|
| Age (< 12 years) | -0.51 | -0.13 | -0.18 | 0.51 |
| Sex (girls) | 3.02 | 0.19 | 0.16 | 2.76 |
| Baseline value (continuous) | -0.07 | -0.03 | -0.20 | -0.16 |
| Treatment site (Tønsberg) | -1.90 | -0.03 | -0.07 | 0.24 |
1Fat percentage measured by means of bioimpedance analysis
2Body mass index (BMI) standard deviation scores, calculated with Norwegian growth charts as reference
3Waist circumference standard deviation scores, calculated with Norwegian growth curves as reference
4Fat percentage measured by means of bioimpedance analysis
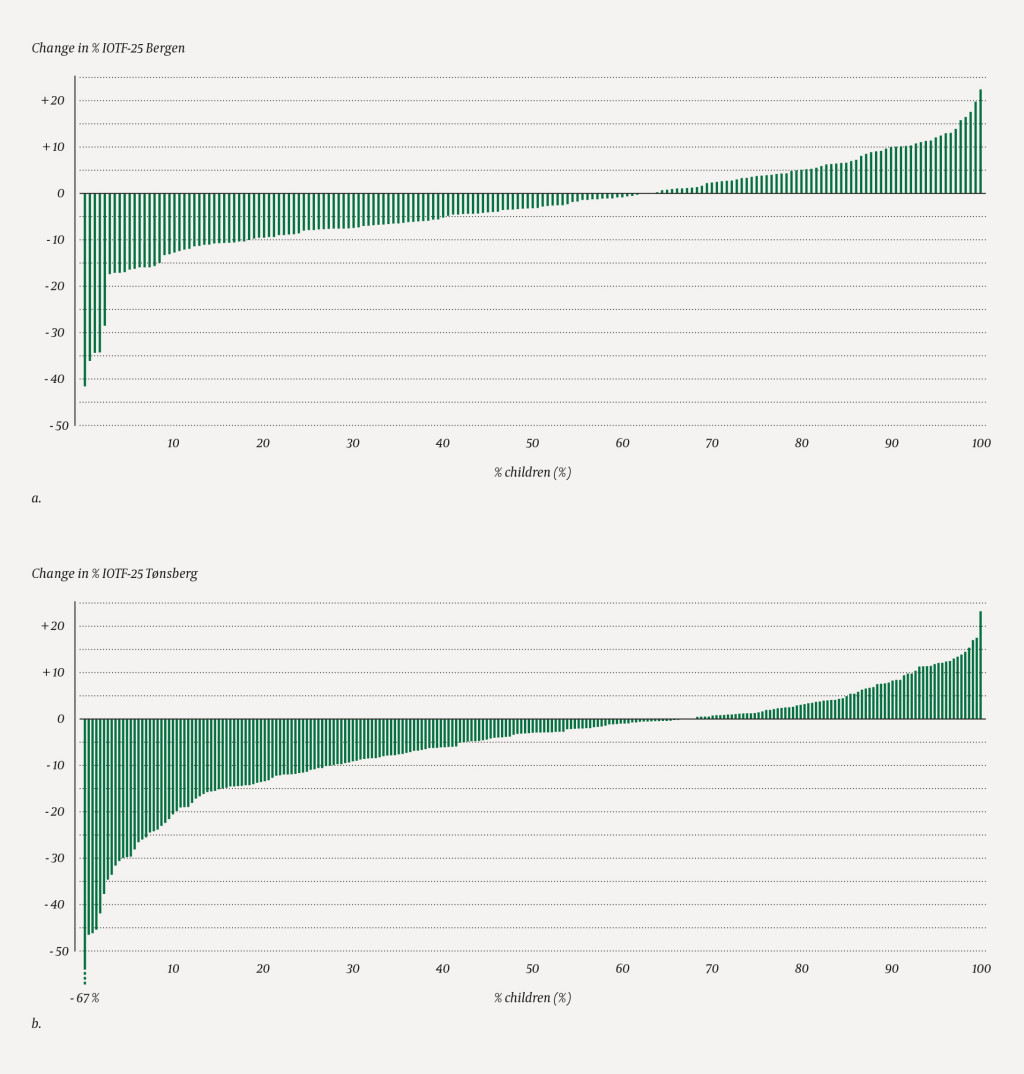
Of 416 included participants, 271 (65 %) reduced their %IOTF-25 and 228 (55 %) their BMI standard deviation score. Of the 325 children who were severely obese at baseline, 54 (17 %) changed their weight category to obesity and 8 (2 %) went from severe obesity to overweight. Of the 91 children who were obese at baseline, 8 (9 %) changed their weight category to overweight or normal weight, and 14 (15 %) became severely obese. The number of participants with a %IOTF-25 reduction of more than 5 % was 177 (43 %), and a reduction in BMI standard deviation score of more than 0.25 was observed in 95 (23 %) of participants.
Drop-out from treatment was 27 % (152 of 568). The individuals who dropped out in Bergen were significantly older (p < 0.01), and in Tønsberg those who dropped out had a significantly lower %IOTF-25 (p < 0.05) and percentage body fat (p < 0.01) (Table 3).
Table 3
Baseline values in children with severe obesity who completed one-year follow-up (included) after family-based lifestyle intervention at two specialist clinics in the period 2012–2016, compared to those who dropped out. Data are presented as mean ± SD or %
| Bergen | Tønsberg | |||||
|---|---|---|---|---|---|---|
| Included | Dropped out | Included | Dropped out | |||
| Age (years) | 11.6 ± 3.4 | 13.2 ± 3.2 | 12.9 ± 3.3 | 13.6 ± 3.3 | ||
| Sex (% boys) | 45.9 | 61.1 | 48.5 | 50.0 | ||
| %IOTF-251 | 150.8 ± 14.5 | 156.1 ± 15.3 | 161.2 ± 22.4 | 156.3 ± 21.9 | ||
| BMI standard deviation score2 | 3.07 ± 0.43 | 3.22 ± 0.44 | 3.31 ± 0.61 | 3.30 ± 0.64 | ||
| BMI ≥ IOTF-35 (%)3 | 77.9 | 87.0 | 78.3 | 76.5 | ||
| Waist circumference standard deviation score4 | 3.05 ± 0.41 | 3.10 ± 0.47 | 3.14 ± 0.51 | 3.16 ± 0.56 | ||
| Fat percentage (BIA)5 | 43.0 ± 5.7 | 44.5 ± 4.7 | 43.6 ± 6.7 | 42.0 ± 7.0 | ||
1Percentage of the International Obesity Task Force's overweight cut-off for children and adolescents
2Body mass index (BMI) standard deviation scores, calculated with Norwegian growth reference
3Percentage of children above the IOTF cut-off for severe obesity for children and adolescents
4Waist circumference standard deviation scores, calculated with Norwegian growth charts as reference
5Fat percentage measured by bioimpedance analysis
Discussion
We found moderate changes in mean weight and body composition, with large interindividual variations after one year of lifestyle intervention in children and adolescents with severe obesity and their families. The mean reduction in %IOTF-25 was 3 % in Bergen and 5 % in Tønsberg, and overall 2 of 3 patients showed a decline in %IOTF-25 in the intervention period. This is perceived as a positive change, as clinical experience indicates that the %IOTF-25 of children with severe obesity is generally increasing at the time of referral, which means that over time their BMI moves further above the overweight cut-off value (iso-BMI 25) on the BMI growth chart. In a pilot project conducted in Bergen in the period 2004–2010 with 32 children and adolescents, the %IOTF-25 increased on average 10 % during the two years before the start of treatment (from 152 % to 162 %), and 2 out of 3 patients showed an increase in %IOTF-25 prior to the start of the intervention (13).
A mean decline of 0.08 in BMI standard deviation score is comparable to the most recent Cochrane meta-analyses (3, 4). In Oslo, the Stor og Sterk treatment programme reported in 2011 a mean decline in BMI standard deviation score of 0.13 in 307 children and adolescents after one year (14). This study included patients with a lower degree of obesity and used BMI standard deviation scores based on the Centre for Disease Control and Prevention's BMI reference, which makes direct comparison difficult.
The results of a more intensive follow-up programme with family-based cognitive behavioural therapy for 49 children and their families showed a mean decline in BMI standard deviation score of 0.18 after 12 weeks of intervention (15). Although the mean change in our quality assurance project was small, our figures show wide individual variation. In all, 16.8 % achieved a lower BMI-defined weight class, while 3.4 % went up in weight class, a figure that must nonetheless be viewed in light of the fact that only 91 of 416 could increase their weight class.
Waist circumference is a less frequently used outcome measure. A study from the Netherlands found a change in waist circumference standard deviation score of −0.6 (95 % CI −1.2–0.0) in the course of a one-year family-based intervention in children and adolescents aged 8–17 years (16). This is a considerably larger decline than our findings of -0.03 and -0.11 in Bergen and Tønsberg, respectively. However, the standard deviation scores in this study were based on Dutch references, which may affect the basis for comparison. The change in fat percentage we found was fairly similar to that reported in the most recent Cochrane meta-analyses (3, 4).
BMI standard deviation scores have been widely used as outcome measures in research, but have nonetheless been regarded as unsuitable and potentially misleading for monitoring severe obesity (9, 17, 18). Measurements outside the reference range may lead to the deviation scores not adjusting well enough for age, sex or degree of obesity. Expressing the BMI as a percentage of an overweight cut-off has been proposed as a better measure (19). IOTF overweight cut-off points can be used in this way (%IOTF-25) (9).
As of today, there is no consensus as to how large a change in BMI standard deviation score should be regarded as clinically significant (20). Several studies have found a reduction in cardiovascular risk when the BMI standard deviation score was at least 0.25 units lower, even though this did not necessarily mean that the BMI was below the obesity cut-off (iso-BMI 30) (21, 22). Several studies have also found increased cardiovascular risk with increasing obesity (23), which indicates that weight stabilisation per se can be regarded as a satisfactory therapeutic goal. In our analysis, we found a reduction in BMI standard deviation score of more than 0.25 in 23 % of the participants. %IOTF-25 is a relatively new outcome measure, so there has not been discussion as to how large a change will be clinically significant. However, the IOTF cut-off points have been chosen to correspond to the cut-offs for overweight and obesity in adults. This means that a percentage reduction can be compared directly with a percentage weight loss or BMI reduction in an adult. A weight reduction of more than 5 % is regarded as clinically significant in adults (24). We noted that 42.5 % of participants had a %IOTF-25 reduction of more than 5 %.
We did not find any statistically significant difference in outcome measures between the treatment centres. However, there was a tendency towards a greater weight reduction in Tønsberg, which could be due to an increased exposure of the patients through group meetings, or somewhat larger staffing.
Boys had better weight developments than girls, which has been demonstrated in several earlier studies (25, 26). It is conceivable that biological and psychological differences play a part, and this should be examined more closely. A lower age (<12 years) was related to a larger reduction in BMI and waist circumference standard deviation scores, but did not affect the results for %IOTF-25 or fat percentage. This finding may be the result of a known limitation of standard deviation scores for children with severe obesity (9, 16, 17) and must therefore be interpreted with caution.
Children and adolescents with severe obesity are a very heterogeneous group, which is reflected in their response to intervention. The variation indicates a need for more tools to assist this patient group. It can be assumed that those for whom the standard intervention was unsuccessful require further action. This could be a closer follow-up, extended parental guidance, other approaches such as structured behavioural interventions with the aid of cognitive elements, supplementary treatment with drugs or more invasive measures such as a gastric balloon or weight-reducing surgery.
A substantial proportion dropped out of the programme (27 %), but this share was lower than that reported in most similar studies (27). Inconsistent findings make it difficult to conclude whether there were specific characteristics associated with individuals who dropped out, and also make it difficult to determine how any differences may have influenced the other results. This should be further investigated.
One of the limitations of this quality assessment project is that it only documents weight development over one year. We are therefore unable to say anything about long-term outcome of the programme. The data have been collected from quality registers and represent a retrospective analysis. It is therefore not possible to draw any definite conclusions about efficacy and which aspects of the therapy, if any, have been effective. However, the sample is large, reflects the real situation in the outpatient clinics and forms a basis for describing weight development during an intervention, which has not previously been done in Norway. We do not possess information about the number of consultations carried out at hospitals or in the primary health service.
Large interindividual differences in the development of body weight and body composition during treatment are evidence of the need for research to identify criteria for a successful intervention. This was also proposed by Mead et al. in a Cochrane review (3). Studies of this nature may potentially identify factors that are predictors for effective treatment, so that we are able to determine individual needs and adjust the therapy accordingly in the future.
Thanks to all patients and their families who have consented to our use of data. Thanks also to the staff at both centres, especially Nina Wahlmann Iversen at Vestfold Hospital. The article has been peer-reviewed.
- 1.
Neef M, Weise S, Adler M et al. Health impact in children and adolescents. Best Pract Res Clin Endocrinol Metab 2013; 27: 229–38. [PubMed][CrossRef]
- 2.
Twig G, Yaniv G, Levine H et al. Body-mass index in 2.3 million adolescents and cardiovascular death in adulthood. N Engl J Med 2016; 374: 2430–40. [PubMed][CrossRef]
- 3.
Mead E, Brown T, Rees K et al. Diet, physical activity and behavioural interventions for the treatment of overweight or obese children from the age of 6 to 11 years. Cochrane Database Syst Rev 2017; 6: CD012651. [PubMed][CrossRef]
- 4.
Al-Khudairy L, Loveman E, Colquitt JL et al. Diet, physical activity and behavioural interventions for the treatment of overweight or obese adolescents aged 12 to 17 years. Cochrane Database Sys Rev 2017:CD012691.
- 5.
Adab P. Treatment of obesity in adolescents: where should interventions focus? Editorial. Arch Dis Child 2017; 102: 689–90. [PubMed][CrossRef]
- 6.
O'Connor EA, Evans CV, Burda BU et al. Screening for obesity and intervention for weight management in children and adolescents: Evidence report and systematic review for the us preventive services task force. JAMA 2017; 317: 2427–44. [PubMed][CrossRef]
- 7.
Cole TJ, Lobstein T. Extended international (IOTF) body mass index cut-offs for thinness, overweight and obesity. Pediatr Obes 2012; 7: 284–94. [PubMed][CrossRef]
- 8.
Helsedirektoratet. Nasjonale faglige retningslinjer for primærhelsetjenesten. Forebygging og behandling av overvekt og fedme hos barn og unge. IS-1734. Oslo: Helsedirektoratet, 2010.
- 9.
Júlíusson PB, Roelants M, Benestad B et al. Severe obesity is a limitation for the use of body mass index standard deviation scores in children and adolescents. Acta Paediatr 2018; 107: 307–14. [PubMed][CrossRef]
- 10.
Júlíusson PB, Roelants M, Nordal E et al. Growth references for 0-19 year-old Norwegian children for length/height, weight, body mass index and head circumference. Ann Hum Biol 2013; 40: 220–7. [PubMed][CrossRef]
- 11.
Brannsether B, Roelants M, Bjerknes R et al. Waist circumference and waist-to-height ratio in Norwegian children 4-18 years of age: reference values and cut-off levels. Acta Paediatr 2011; 100: 1576–82. [PubMed][CrossRef]
- 12.
Vickers AJ, Altman DG. Statistics notes: Analysing controlled trials with baseline and follow up measurements. BMJ 2001; 323: 1123–4. [PubMed][CrossRef]
- 13.
Linde SF, Assmus J, Danielsen Y et al. Two years obesity intervention program in children and adolescents: The importance of age at enrollment. 22nd European Congress on Obesity (ECO2015), Praha, May 6–9, 2015. Obes Facts 2015; 8 (suppl 1): 231.
- 14.
Kolsgaard ML, Joner G, Brunborg C et al. Reduction in BMI z-score and improvement in cardiometabolic risk factors in obese children and adolescents. The Oslo Adiposity Intervention Study - a hospital/public health nurse combined treatment. BMC Pediatr 2011; 11: 47. [PubMed][CrossRef]
- 15.
Danielsen YS, Nordhus IH, Júlíusson PB et al. Effect of a family-based cognitive behavioural intervention on body mass index, self-esteem and symptoms of depression in children with obesity (aged 7-13): a randomised waiting list controlled trial. Obes Res Clin Pract 2013; 7: e116–28. [PubMed][CrossRef]
- 16.
Vos RC, Wit JM, Pijl H et al. Long-term effect of lifestyle intervention on adiposity, metabolic parameters, inflammation and physical fitness in obese children: a randomized controlled trial. Nutr Diabetes 2011; 1: e9. [PubMed][CrossRef]
- 17.
Woo JG. Using body mass index Z-score among severely obese adolescents: a cautionary note. Int J Pediatr Obes 2009; 4: 405–10. [PubMed][CrossRef]
- 18.
Løkling HL, Roelants M, Kommedal KG et al. Monitoring children and adolescents with severe obesity: body mass index (BMI), BMI z-score or percentage above the International Obesity Task Force overweight cut-off? Acta Paediatr 2019; 108: 2261–6. [PubMed][CrossRef]
- 19.
Flegal KM, Wei R, Ogden CL et al. Characterizing extreme values of body mass index-for-age by using the 2000 Centers for Disease Control and Prevention growth charts. Am J Clin Nutr 2009; 90: 1314–20. [PubMed][CrossRef]
- 20.
Reinehr T. Lifestyle intervention in childhood obesity: changes and challenges. Nat Rev Endocrinol 2013; 9: 607–14. [PubMed][CrossRef]
- 21.
Ford AL, Hunt LP, Cooper A et al. What reduction in BMI SDS is required in obese adolescents to improve body composition and cardiometabolic health? Arch Dis Child 2010; 95: 256–61. [PubMed][CrossRef]
- 22.
Reinehr T, Lass N, Toschke C et al. Which amount of BMI-SDS reduction is necessary to improve cardiovascular risk factors in overweight children? J Clin Endocrinol Metab 2016; 101: 3171–9. [PubMed][CrossRef]
- 23.
Skinner AC, Perrin EM, Moss LA et al. Cardiometabolic risks and severity of obesity in children and young adults. N Engl J Med 2015; 373: 1307–17. [PubMed][CrossRef]
- 24.
Williamson DA, Bray GA, Ryan DH. Is 5% weight loss a satisfactory criterion to define clinically significant weight loss? Obesity (Silver Spring) 2015; 23: 2319–20. [PubMed][CrossRef]
- 25.
Holm JC, Gamborg M, Bille DS et al. Chronic care treatment of obese children and adolescents. Int J Pediatr Obes 2011; 6: 188–96. [PubMed][CrossRef]
- 26.
Most SW, Højgaard B, Teilmann G et al. Adoption of the children's obesity clinic's treatment (TCOCT) protocol into another Danish pediatric obesity treatment clinic. BMC Pediatr 2015; 15: 13. [PubMed][CrossRef]
- 27.
Skelton JA, Beech BM. Attrition in paediatric weight management: a review of the literature and new directions. Obes Rev 2011; 12: e273–81. [PubMed][CrossRef]