Delirium and cognitive impairment among older patients in Norwegian emergency departments
Main message
On World Delirium Awareness Day, 14 March 2018, we examined 118 patients ≥ 75 years in Norwegian emergency departments to identify delirium and other forms of cognitive impairment
17 per cent showed signs of delirium, and 30 per cent showed signs of other forms of cognitive impairment
All types of departments and all hospitals received patients with symptoms of delirium and/or cognitive impairment at the time of the examination
Delirium is an acute change in attention, awareness and cognition that arises in association with physiological changes such as illness, injuries or surgery Box 1) ((1). Delirium may affect anybody, but advanced age and cognitive impairment significantly increase the risk (2). The prognosis for delirium is serious, with high mortality, increased need for nursing home care and increased risk of dementia (3). Patients with delirium also have an elevated risk of hospital complications, and delirium contributes to prolonged hospitalisation and increased costs (2, 4). Dealing with the condition may be challenging for healthcare personnel (5) and a frightening experience for the patients (6) and their next of kin (7).
-
A disturbance in attention (i.e. reduced ability to direct, focus, sustain, and shift attention) and awareness (reduced orientation to the environment).
-
The disturbance develops over a short period of time (usually hours to a few days), represents a change from baseline attention and awareness, and tends to fluctuate in severity during the course of a day.
-
An additional disturbance in cognition (e.g. memory deficit, disorientation, language, visuospatial ability or perception).
-
The disturbances in Criteria A and C are not better explained by another pre-existing, established, or evolving neurocognitive disorder and do not occur in the context of a severely reduced level of arousal, such as coma.
-
There is evidence from the history, physical examination, or laboratory findings that the disturbance is a direct physiological consequence of another medical condition, substance intoxication or withdrawal (i.e. due to a drug of abuse or to a medication), or exposure to a toxin, or is due to multiple aetiologies.
Since delirium is a serious condition that by definition has a somatic cause, it is crucial to recognise delirium and aim treatment at correcting all reversible causes (2). International studies indicate that one in every ten elderly patients in emergency departments suffer from delirium (2), and close to one-half of all patients with hip fractures develop delirium during the course of their illness (12). The condition is also very common among intensive-care and end-of-life patients (13, 14). Because delirium is both very common and serious, it is unfortunate that this condition goes undetected in more than 60 per cent of all cases (15, 16).
Impairment of cognitive functions is a prominent symptom of delirium, but cognitive impairment is also observed in dementia and not infrequently in depression, and this may complicate differential diagnostics. Such underlying cognitive impairment is also a prime risk factor for delirium. Since delirium has a serious prognosis (3), and patients with cognitive impairment are more vulnerable than other patients to complications during hospitalisation (17), it is crucial to detect both delirium and other forms of cognitive impairment at the earliest possible stage of the hospitalisation period to permit initiation of targeted treatment and effective environmental interventions (18). Today, symptoms of delirium or cognitive impairment are not routinely identified or documented in Norwegian hospitals (19).
In recent years, delirium researchers worldwide have marked World Delirium Awareness Day (WDAD) to improve knowledge about delirium among healthcare personnel and laypeople (20). Inspired by Italian and British point prevalence surveys of delirium (21, 22) we took the initiative to undertake a similar survey on WDAD in 2018. The objective was primarily to identify the prevalence of delirium, secondarily other forms of cognitive impairment. We conducted the survey in the emergency departments (EDs), since the prevalence of these conditions has not been investigated in Norwegian EDs before and because the EDs receive a broad range of patients. Clinicians in many departments may thus relate to our findings.
Material and method
We conducted a point prevalence survey of delirium and cognitive impairment in patients ≥ 75 years who arrived in Norwegian EDs between 08:00 and 22:00 on 14 March 2018. A geriatrician or doctor with long-standing experience in geriatric medicine assessed the patient for delirium using the validated 4AT screening tool (see appendix) and registered the patient's age and gender, the time of admission and the department (internal medicine, surgery, orthopaedics and 'other'). A total of 13 doctors participated, distributed among Helgeland Hospital (Mo i Rana), Levanger Hospital, St Olavs Hospital, Trondheim University Hospital, Førde Central Hospital, Vestfold Hospital, Kongsberg Hospital, Bærum Hospital, Diakonhjemmet Hospital, Oslo University Hospital Ullevål and Akershus University Hospital.
Diagnostics
4AT was developed in the UK and has been translated into a number of languages, including Norwegian (23, 24). The test consists of four items, and the patient may obtain a score of 0–12 points. A score of 4 or above should arouse suspicion of delirium, a score of 1–3 should arouse suspicion of cognitive impairment without active delirium, while a score of 0 indicates a low likelihood of cognitive impairment or delirium (24). 4AT is a validated screening tool for delirium with a sensitivity of 87–93 per cent and a specificity of 70–91 per cent (15, 16, 23).
In the first item, the examiner investigates whether the patient is normally alert and aware of his or her surroundings. Normal alertness returns a score of 0, anything else a score of 4. Item 2 consists of a brief orientation test, in which the patient states his or her age, date of birth, place of the examination and the current year. Depending on the responses, the patient scores 0, 1 or 2 points. Item 3 is an attention test, in which the patient is asked to name the months of the year backwards (December–November–October etc.). Correct naming of seven months returns a score of 0, less than seven months scores 1 point and untestable patients score 2 points. In item 4, the examiner consults the medical history, information from next of kin and patient records to assess whether there are any indications of acute changes or fluctuations in the patient's cognition, attention or awareness. If this is the case, the patient is given a score of 4 points.
Ethics
Relevant patients were asked to participate and received an information leaflet which described the content and purpose of the study. Patients who appeared to understand the content of the study and agreed to participate signed the consent form. If the doctor deemed the patient incapable of giving consent, he or she obtained consent from a next of kin. Patients who were incapable of giving consent and had no next of kin were not included. The project was approved by the Regional Committee for Medical and Health Research Ethics, Northern Norway (2017/2420).
Statistics
We present dichotomous and nominal data as integers and percentages and continuous data as averages and standard deviations. We used SPSS version 25 for descriptive statistics and Excel version 2016 to create graphs.
Results
A total of 140 patients ≥ 75 years arrived in the EDs in the ten hospitals between 08:00 and 22:00 on 14 March 2018. Of these, 118 patients (84 per cent) were included in the project. Ten patients did not wish to participate, and four patients were unable to provide consent. Four patients were not asked to participate, and four patients were unable to participate for various reasons. Average age was 83.5 years (standard deviation 6.1), and 63 (53 per cent) were women. The majority were admitted to departments of internal medicine (63 per cent), while 15 per cent, 13 per cent and 9 per cent were admitted to surgical, orthopaedic and other departments respectively.
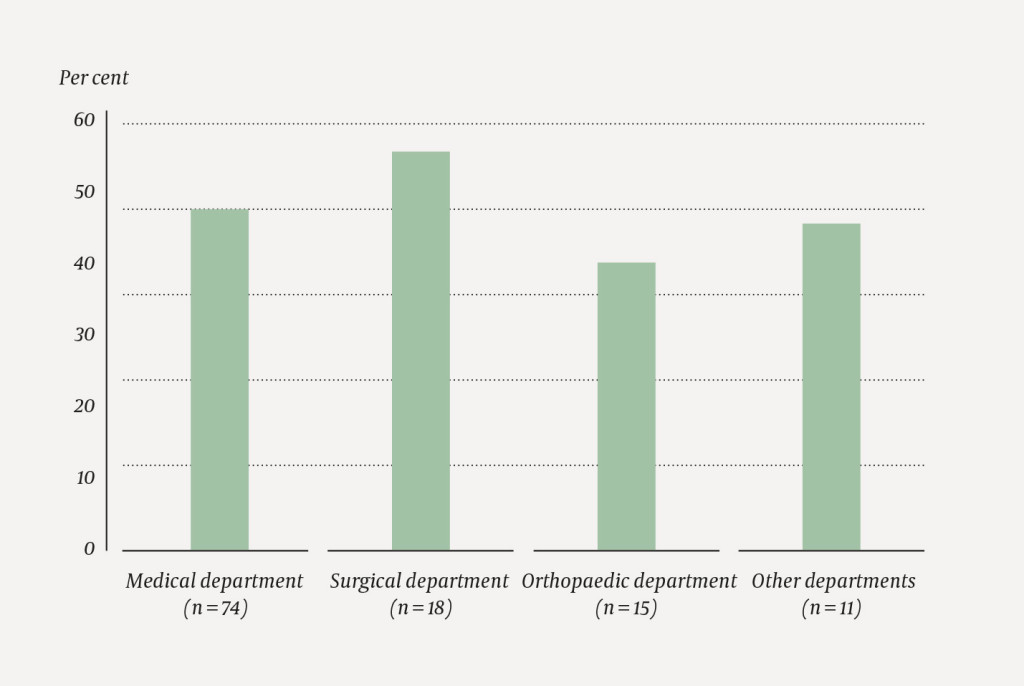
Twenty of 118 patients (17 per cent) had delirium identified by 4AT. We found signs of cognitive impairment in 36 further patients, resulting in 56 patients (47 per cent) with signs of some form of cognitive impairment. Eight of ten hospitals received patients with delirium, and all hospitals received patients with signs of cognitive impairment. Figure 1 shows that patients with delirium and/or cognitive impairment accounted for a major proportion of the elderly patients in medical, surgical, orthopaedic and other types of departments on that day.
Discussion
In this point prevalence survey among patients ≥ 75 years in ten Norwegian EDs, 17 per cent showed findings consistent with delirium, while another 30 per cent showed findings consistent with other forms of cognitive impairment, as determined by the 4AT screening tool. All categories of departments received patients with delirium. All participating hospitals received patients with signs of delirium or other types of cognitive impairment.
The prevalence of delirium was somewhat higher than in equivalent studies from other countries, where a prevalence of approximately 10 per cent was found in EDs (8–11). One likely reason is that whereas we included patients ≥ 75 years, these studies had an inclusion threshold of 65 years. Norwegian emergency departments also have a more selected group of patients than similar departments in other countries, to which patients may turn directly, as they would to an A&E centre. The prevalence of cognitive impairment at 47 per cent is approximately the same as in other studies, which identified cognitive impairment in approximately one-half of all elderly patients in emergency departments (25, 26).
Patients with cognitive impairment are at a high risk of developing delirium and other complications during hospitalisation (17). Since delirium is associated with a poor prognosis (3), complications, extended hospitalisation periods and increased costs (4), it is crucially important that the hospitals maintain a focus on prevention and appropriate management of delirium. A meta-analysis concludes that close to one-half of all cases of delirium can be prevented with the aid of simple, but personnel-intensive measures such as orientation, a focus on hydration and nutrition, patient activation, mobilisation and good sleep hygiene (18). Such interventions also have a documented effect on manifest delirium, in contrast to psychotropic drugs, which should not be used as a routine (2). We are concerned, however, that conditions such as overcrowded wards, corridor patients, short hospitalisation periods and low staffing all contribute to an increased prevalence and suboptimal treatment of delirium.
Since delirium is common, associated with a long series of negative outcomes and largely preventable, we believe that better prevention and management of delirium would have a major positive effect on patient safety in Norwegian hospitals. We call for a proactive stance with regard to delirium and cognitive impairment and we believe that including these conditions as focus areas in the patient safety programme would be a natural choice (27). Our results illustrate that patients with both delirium and other kinds of cognitive impairment are admitted to most types of departments, underpinning the assertion that concrete plans for management of patients with delirium and cognitive impairment ought to be available in all departments that treat elderly patients, and not be regarded as a concern only for geriatrics departments.
We also recommend the introduction of procedures for examination for delirium and cognitive status in EDs (4, 25, 26). This will help identify patients with delirium, and since delirium is a sign of illness, it will most likely lead to more thorough diagnostics and better treatment. Recognition of delirium will also reduce the risk of the condition being misinterpreted as dementia. Early identification of patients with cognitive impairment will also enable the staff to provide adapted information, initiate targeted measures to prevent delirium and other complications (17, 18), and improve discharge planning for these patients. Recognition of delirium may also identify patients who will need closer follow-up after discharge. Since delirium is underdiagnosed (15, 16), we recommend using a standardised screening tool. 4AT can provide a meaningful score also for patients who are unable to answer questions, and the tool provides an indication of whether patients without delirium may have underlying cognitive impairment.
Strengths and limitations
The key strengths of this study are its use of a validated screening tool for delirium and that it was conducted in ten different hospitals by doctors with long-standing experience of work with elderly patients. However, the dataset is relatively small and restricted to the date in question. We wish to emphasise that 4AT is a screening tool and must therefore not be used as a basis for final diagnoses such as dementia or mild cognitive impairment. Other limitations include non-registration of other risk factors for delirium, such as frailty, multimorbidity, polypharmacy or known cognitive impairment.
Conclusion
On World Delirium Awareness Day, 14 March 2018, altogether 17 per cent of all patients ≥ 75 years referred to a sample of Norwegian emergency departments showed signs of delirium, and another 30 per cent showed signs of other forms of cognitive impairment. All hospitals and all categories of departments received patients with signs of delirium and/or cognitive impairment, thus underpinning the view that all departments that treat elderly patients ought to have procedures and competence to provide optimal care for patients with delirium and cognitive impairment.
The authors wish to thank Dag Ole Aanderbakk, Eva Herløsund Søgnen, Dyveke Gleditsch, Tine Reiten, Ane Victoria Idland and Leiv Otto Watne for their help with the data collection.
- 1.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (DSM–5). Washington DC: American Psychiatric Publishing, 2013.
- 2.
Marcantonio ER. Delirium in hospitalized older adults. N Engl J Med 2017; 377: 1456–66. [PubMed][CrossRef]
- 3.
Witlox J, Eurelings LS, de Jonghe JF et al. Delirium in elderly patients and the risk of postdischarge mortality, institutionalization, and dementia: a meta-analysis. JAMA 2010; 304: 443–51. [PubMed][CrossRef]
- 4.
Inouye SK, Westendorp RG, Saczynski JS. Delirium in elderly people. Lancet 2014; 383: 911–22. [PubMed][CrossRef]
- 5.
Meagher DJ, Leonard M, Donnelly S et al. A longitudinal study of motor subtypes in delirium: relationship with other phenomenology, etiology, medication exposure and prognosis. J Psychosom Res 2011; 71: 395–403. [PubMed][CrossRef]
- 6.
Instenes I, Gjengedal E, Eide LSP et al. "Eight days of nightmares ... " – Octogenarian patients' experiences of postoperative delirium after transcatheter or surgical aortic valve replacement. Heart Lung Circ 2018; 27: 260–6. [PubMed][CrossRef]
- 7.
Morandi A, Lucchi E, Turco R et al. Delirium superimposed on dementia: A quantitative and qualitative evaluation of informal caregivers and health care staff experience. J Psychosom Res 2015; 79: 272–80. [PubMed][CrossRef]
- 8.
Elsayem AF, Bruera E, Valentine AD et al. Delirium frequency among advanced cancer patients presenting to an emergency department: A prospective, randomized, observational study. Cancer 2016; 122: 2918–24. [PubMed][CrossRef]
- 9.
Émond M, Boucher V, Carmichael PH et al. Incidence of delirium in the Canadian emergency department and its consequences on hospital length of stay: a prospective observational multicentre cohort study. BMJ Open 2018; 8: e018190. [PubMed][CrossRef]
- 10.
Kennedy M, Enander RA, Tadiri SP et al. Delirium risk prediction, healthcare use and mortality of elderly adults in the emergency department. J Am Geriatr Soc 2014; 62: 462–9. [PubMed][CrossRef]
- 11.
Sri-on J, Tirrell GP, Vanichkulbodee A et al. The prevalence, risk factors and short-term outcomes of delirium in Thai elderly emergency department patients. Emerg Med J 2016; 33: 17–22. [PubMed][CrossRef]
- 12.
Juliebø V, Bjøro K, Krogseth M et al. Risk factors for preoperative and postoperative delirium in elderly patients with hip fracture. J Am Geriatr Soc 2009; 57: 1354–61. [PubMed][CrossRef]
- 13.
Ely EW, Shintani A, Truman B et al. Delirium as a predictor of mortality in mechanically ventilated patients in the intensive care unit. JAMA 2004; 291: 1753–62. [PubMed][CrossRef]
- 14.
Hosker CM, Bennett MI. Delirium and agitation at the end of life. BMJ 2016; 353: i3085. [PubMed][CrossRef]
- 15.
O'Sullivan D, Brady N, Manning E et al. Validation of the 6-Item Cognitive Impairment Test and the 4AT test for combined delirium and dementia screening in older Emergency Department attendees. Age Ageing 2018; 47: 61–8. [PubMed][CrossRef]
- 16.
Hendry K, Quinn TJ, Evans J et al. Evaluation of delirium screening tools in geriatric medical inpatients: a diagnostic test accuracy study. Age Ageing 2016; 45: 832–7. [PubMed][CrossRef]
- 17.
Bail K, Berry H, Grealish L et al. Potentially preventable complications of urinary tract infections, pressure areas, pneumonia, and delirium in hospitalised dementia patients: retrospective cohort study. BMJ Open 2013; 3: e002770. [PubMed][CrossRef]
- 18.
Hshieh TT, Yue J, Oh E et al. Effectiveness of multicomponent nonpharmacological delirium interventions: a meta-analysis. JAMA Intern Med 2015; 175: 512–20. [PubMed][CrossRef]
- 19.
Watne LO, Wyller TB. Delirium – framleis underdiagnostisert. Tidsskr Nor Legeforen 2018; 138. doi: 10.4045/tidsskr.18.0118. [PubMed][CrossRef]
- 20.
iDelirium. The International Federation of Delirium Societes. www.idelirium.org (13.12.2018).
- 21.
Bellelli G, Morandi A, Di Santo SG et al. "Delirium Day": a nationwide point prevalence study of delirium in older hospitalized patients using an easy standardized diagnostic tool. BMC Med 2016; 14: 106. [PubMed][CrossRef]
- 22.
Ryan DJ, O'Regan NA, Caoimh RÓ et al. Delirium in an adult acute hospital population: predictors, prevalence and detection. BMJ Open 2013; 3: e001772. [PubMed][CrossRef]
- 23.
Bellelli G, Morandi A, Davis DH et al. Validation of the 4AT, a new instrument for rapid delirium screening: a study in 234 hospitalised older people. Age Ageing 2014; 43: 496–502. [PubMed][CrossRef]
- 24.
Evensen S, Forr T, Al-Fattal A et al. Nytt verktøy for å oppdage delirium og kognitiv svikt. Tidsskr Nor Legeforen 2016; 136: 299–300. [PubMed][CrossRef]
- 25.
Pendlebury ST, Klaus SP, Mather M et al. Routine cognitive screening in older patients admitted to acute medicine: abbreviated mental test score (AMTS) and subjective memory complaint versus Montreal Cognitive Assessment and IQCODE. Age Ageing 2015; 44: 1000–5. [PubMed][CrossRef]
- 26.
Reynish EL, Hapca SM, De Souza N et al. Epidemiology and outcomes of people with dementia, delirium, and unspecified cognitive impairment in the general hospital: prospective cohort study of 10,014 admissions. BMC Med 2017; 15: 140. [PubMed][CrossRef]
- 27.
I trygge hender. https://www.pasientsikkerhetsprogrammet.no (13.12.2018).