Use of snus and smoking tobacco among pregnant women in the Agder counties
The use of snus is unique to Norway and Sweden, since the sale of snus products is prohibited in the EU. Sweden has been granted an exemption from this sales ban.
A number of studies undertaken in recent years indicate that the use of snus during pregnancy may have detrimental effects during pregnancy and affect the newborn child (1) – (2). This has been documented in particular by large population studies on data from the Swedish Medical Birth Register. Use of snus during pregnancy increases the risk of stillbirth, premature birth and reduced birthweight (3) – (5), and is also associated with preeclampsia as well as cleft lip and palate and apnoea in newborns (6) – (8).
Since the use of snus is a phenomenon virtually specific to Sweden and Norway, few high-quality and large-scale studies are available from other countries. However, the findings are partly confirmed by studies from countries where other kinds of smokeless tobacco are used, including India (9, 10) and South Africa (11).
Over the last decade, the use of snus has tripled in Norway, and the frequency of use has increased especially among young women (1). In 2014, altogether 4 % of Norwegian women used snus on a daily basis, whereas 3 % were occasional users. In the age group 16 – 24 years, a total of 18 % of women were snus users, and in the age group 25 – 34 years 16 % (12). While fewer young people today take up smoking, there has been an increase in the use of snus, including in resourceful communities such as students, athletes and military personnel (13).
Among young women, the use of snus is a relatively recent trend. Should they become addicted, they may face difficulties in quitting the habit when becoming pregnant. Snus is recommended by many as a substitute for smoking as a harm reduction strategy, since snus has less health risks than smoking tobacco and is also associated with a decreased smoking prevalence (14) – (17). The risk, however, is that the use of snus may increase in groups that otherwise would not have taken up tobacco use (18). This may lead to an higher number of young women being snus users when they become pregnant.
To date, the use of snus has not been registered in the Health card for pregnant women. This may be taken as a signal that the use of snus during pregnancy has less health risks than smoking. The extent to which this problem area is addressed by midwives and GPs during pregnancy care is unknown (19).
The use of snus by pregnant women has not been surveyed previously in Norway, with the exception of a non-representative sample in the Mother and Child Cohort Study (1). The extent to which snus users quit during pregnancy is unknown. Sørlandet Hospital has used electronic birth records for a number of years, in which both snus use and smoking are registered. Since 2014, all Norwegian maternity wards have registered smoking as well as snus use in their electronic birth records, but so far, only smoking habits are reported to the Medical Birth Registry (20).
In this study, we wished to investigate trends in the use of snus and smoking tobacco among women who gave birth at Sørlandet Hospital during the years 2012 – 14. Since we assumed that snus would be considered less harmful than smoking tobacco, our hypothesis was that the proportion that quit using snus would be lower than the proportion that quit smoking during pregnancy.
Material and method
The material encompasses anonymised data for all births in the years 2012, 2013 and 2014 at the three maternity wards of Sørlandet Hospital Trust in Flekkefjord, Kristiansand and Arendal respectively, a total of 10 583 births.
Information on the women’s use of snus and smoking tobacco prior to and during their pregnancy, and on their level of education, as well as the children’s birthweight and Apgar score was retrieved from the Partus electronic birth record. In the record, the use of snus and smoking tobacco has been registered as «on a daily basis» and «occasionally» before the pregnancy, during the first trimester (as registered in the check-up in the 18th week) and during the third trimester (as registered in the admission interview at the maternity ward), respectively.
Data retrieval was undertaken by Sykehuspartner and transferred to SPSS, version 21, in which descriptive statistics were used. The proportion of users who quit using snus and smoking tobacco respectively was estimated from the time before pregnancy to the first trimester and from before the pregnancy to the third trimester. Significance values for the differences were estimated by a two-sample test of the proportions.
The study was approved by the Regional Committee on Medical and Health Research Ethics (2014/654 REK Sør-Øst).
Results
The material encompassed 10 583 births at Sørlandet Hospital. Use/non-use of snus was recorded in the births records of 98.8 % of the women prior to pregnancy, of 96.9 % in the first trimester and of 95.9 % in the third trimester. The equivalent response rates for smoking tobacco amounted to 98.4 %, 99.4 % and 97.0 % respectively. The total proportion of pregnant women who used snus on a daily basis or occasionally amounted to 4.9 % prior to pregnancy, 2.4 % in the first trimester and 1.7 % in the third trimester. The corresponding proportion who used smoking tobacco amounted to 19.1 %, 10.7 % and 8.0 % respectively (Table 1).
Table 1
Users of snus and smoking tobacco during pregnancy. Collated data for 2012 – 14. N = 10 583
| Snus |
Smoking tobacco |
||||||||||||||||
|
|
Occasionally |
Daily |
Sum of occasionally + daily |
Occasionally |
Daily |
Sum of occasionally + daily |
|||||||||||
| Number |
(%) |
Number |
(%) |
Number |
(%) |
Number |
(%) |
Number |
(%) |
Number |
(%) |
||||||
| Before pregnancy |
174 |
(1.6) |
351 |
(3.3) |
525 |
(4.9) |
443 |
(4.2) |
1 577 |
(14.9) |
2 020 |
(19.1) |
|||||
| 1st trimester |
119 |
(1.1) |
141 |
(1.3) |
260 |
(2.4) |
192 |
(1.8) |
946 |
(8.9) |
1 138 |
(10.7) |
|||||
| 3rd trimester |
86 |
(0.8) |
90 |
(0.9) |
176 |
(1.7) |
135 |
(1.3) |
705 |
(6.7) |
840 |
(8.0) |
|||||
Tendency over time
From 2012 to 2014 there was a near-doubling in the use of snus prior to pregnancy – from 3.6 % to 6.8 %. The corresponding proportions for the first trimester was from 1.7 % to 3.4 % and for the third trimester from 1.2 % to 2.1 %. Regarding smoking, there was a reduction from 19.9 % to 18.6 % prior to pregnancy, from 11.8 % to 9.8 % in the first trimester and from 8.7 % to 7.2 % in the last trimester (Figure 1).
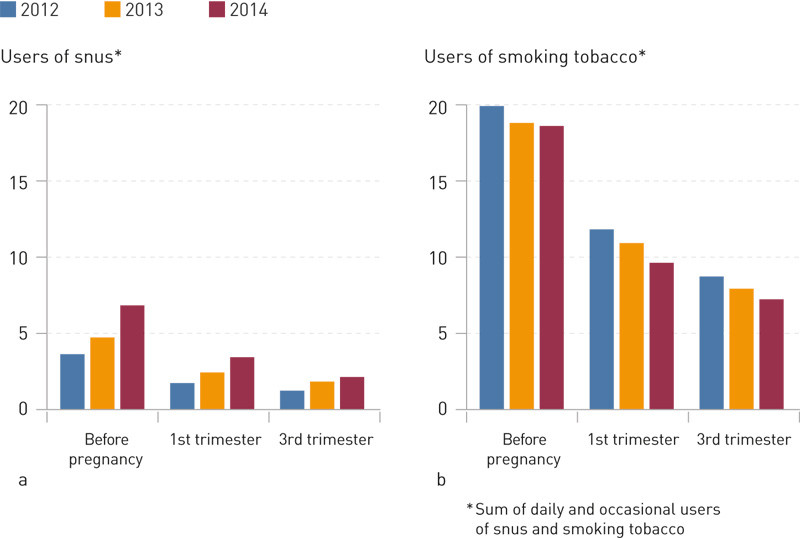
Age groups
The use of snus was most prevalent in the age group 16 – 24 years, in which 12.2 % used snus before pregnancy, 7.1 % during the first trimester and 4.6 % in the third trimester (Figure 2). In the same age group, the proportion of smokers amounted to 32.7 %, 22.4 % and 15.4 % respectively.
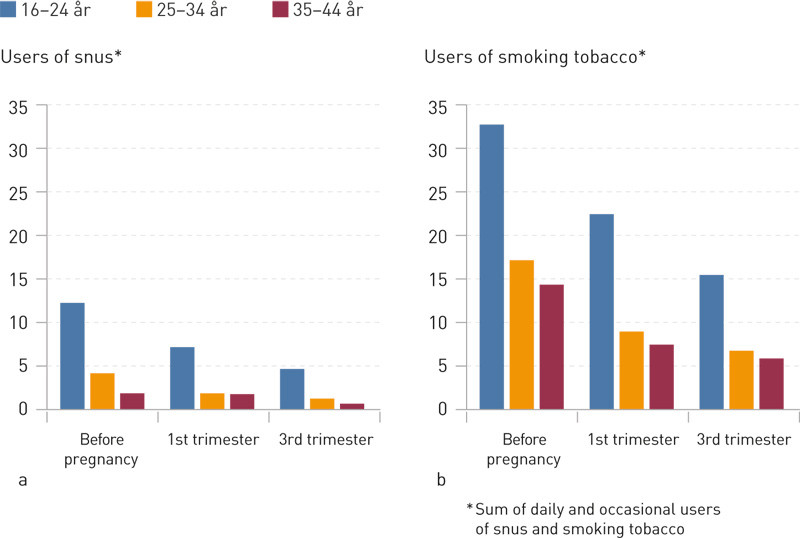
In the age group 25 – 34 years, altogether 4.1 % used snus prior to pregnancy, 1.8 % in the first trimester and 1.2 % in the third trimester. The proportion of smokers in this age group amounted to 17.1 %, 8.9 % and 6.7 % respectively.
Education
There was a marked educational gradient in the use of smoking tobacco, but this was less clear in the case of snus. Among those who used snus prior to pregnancy, those who had upper secondary as their highest level of education were in a small majority.
Only few women with education at the university or university college level used snus or smoking tobacco during pregnancy when compared to those with less education (Figure 3).
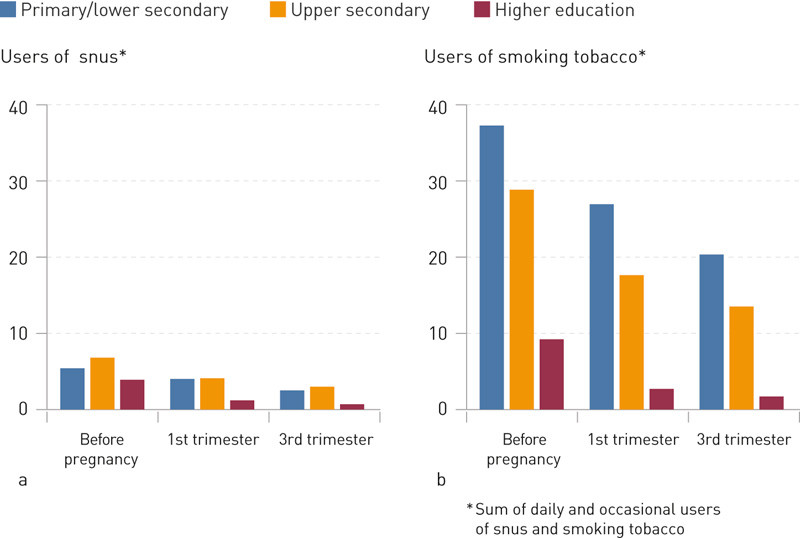
Changes during pregnancy
Out of 522 women who had used snus prior to pregnancy, altogether 300 (57.5 %; 95 % CI 53 – 62 %) had quit by the first trimester and 364 (71.4 %; 95 % CI 66 – 74 %) by the third trimester. Out of 2 015 women who used smoking tobacco before their pregnancy, altogether 910 (45.2 %; 95 % CI 43 – 47 %) had quit by the first trimester and 1 141 (58.0 %; 95 % CI 54 – 59 %) by the third trimester.
The proportion of pregnant women who quit using snus during their pregnancy was significantly higher than the proportion who quit smoking (p < 0.001). Altogether 42.4 % of those who used snus prior to pregnancy and 54.8 % of those who smoked continued to do so during the first trimester, and 28.6 % and 42.0 % respectively also continued during the last trimester.
Birthweight and Apgar score
The average birthweight for children of mothers who had been daily or occasional smokers during the last trimester amounted to 3 331 grams, compared to 3 533 grams in the group of non-smokers. This average reduction of 202 grams in birthweight was statistically significant (p < 0.001).
No significant difference in birthweight was found in children of mothers who had used snus when compared to children of non-users. Nor could any difference in Apgar score be found in children whose mothers had used snus or smoking tobacco during the last trimester when compared children of non-users.
Discussion
In the period from 2012 to 2014 there was a near-doubling in the use of snus among pregnant women in the Agder counties. The proportion of snus users who quit during their pregnancy was significantly higher than that of smokers. This may indicate that quitting snus is easier than quitting smoking.
Consistency with other studies
The use of snus in the Agder counties has been below the national average, while the use of smoking tobacco has been above the average (12). In our population as well, i.e. pregnant women in the Agder counties in the years 2012 – 2014, the use of snus was below the national average: 5 % compared to 7 % in the country as a whole. By 2014, however, the use of snus prior to pregnancy had increased to 7 %, equal to the national average.
The proportion of smokers among pregnant women in the Agder counties was higher than the national average: 11 % compared to 7 % in the country as a whole at the start of pregnancy, and 8 % compared to 4 % at the end of pregnancy (20). The proportion of pregnant women who used snus in our study was approximately equal to the one in Sweden. According to figures from the Swedish Medical Birth Register, the proportion who used snus prior to pregnancy in 2012 amounted to 3.5 %, compared to 3.6 % in the Agder counties, 1.2 % and 1.7 % respectively in the first trimester and 0.7 % compared to 1.2 % in the last trimester (21). This indicates that the extent of the problem may be on the same scale as in Sweden.
We found a statistically significant reduction in the birthweight of children whose mothers had used smoking tobacco towards the end of pregnancy, but no difference for those who had used snus when compared to non-users. These figures are not corrected for socioeconomic factors. The effect of snus on foetal growth has been less studied than the effect of smoking tobacco. A large-scale study from the Swedish Medical Birth Register showed that the risk for the child to be small for gestational age at birth, was lower in the case of snus use than in case of smoking at an early stage of pregnancy (adjusted OR 1.26; 95 % CI 1.09 – 1.46, compared to 2.55: 95 % CI 2.43 – 2.67) (5). Other studies also indicate that the use of snus has less effect than smoking on foetal growth (11, 22). It is debated whether this might be associated with the toxic effects of combustion products, such as the carbon monoxide level in the blood of smokers, in addition to the possible effects of nicotine (23).
Validity
The strength of this study lies in the large size of the studied population and the high response rates (ranging from 96 to 99 %). A weakness in this study is its possible element of underreporting. The response rates were at their lowest in the third trimester, and they were lower for snus than for smoking.
If the Partus health record in previous consultations had registered that the woman did not smoke or use snus, the midwife may have found it irrelevant to ask this question again, which may have given rise to underreporting. Moreover, we may assume that questions regarding tobacco use may be perceived as a taboo issue for a pregnant woman, and hence difficult for her to answer honestly, which also may contribute to missing or incorrect information. Prevailing regulations emphasise that registration of snus use and smoking habits shall be voluntary, and that written information must be presented on the purpose of the reporting to the Medical Birth Registry (20).
Lifestyle counselling and prevention
Among young women, the use of snus is a relatively new occurrence. The time and age gradients indicate that in the years to come, many more women might be snus users when they become pregnant. Our study indicates that 42 % of those who used snus prior to their pregnancy continued to do so through the first trimester and 29 % through the third trimester.
A portion of snus results in a somewhat higher uptake of nicotine in the bloodstream than a cigarette, and stays there longer (1). Nicotine quickly passes through the placenta barrier, and the concentration is 15 % higher in the foetal plasma than in the mother’s (24). Since no lower threshold to foetal injury is known, this represents a potential public health problem.
The Health card for pregnant women has been revised, now also calling for registration of snus use. This implies that harmful effects from the use of snus will tend to be included in the advice given to pregnant women from their first check-up in antenatal care, in the same way as warnings against the use of smoking tobacco.
The proportion of smokers in our study was especially high in the age group 16 – 24 years, in which 22 % smoked during the first trimester and 15 % in the third trimester. This indicates that smoking remains the largest tobacco-related problem in pregnancy, in particular among the youngest women.
We found a marked education gradient when it came to the use of smoking tobacco, but this was less distinct in the case of snus. This is consistent with the declining difference in the use of snus between educational groups, as opposed to previously, when the use of snus was most common in groups with higher levels of education (1). This indicates that the increase in the use of snus has reached younger age groups and those with the lowest levels of education. In our study, the prevalence of snus use was approximately identical in those with primary/lower secondary and those with upper secondary as their highest level of education. In this group 4 % used snus in the first trimester and 3 % in the third trimester, but only 1 % of those with higher education used snus during their pregnancy.
This has a bearing on how preventive measures should be targeted: Advice on the harmful effects of snus use should be provided to young girls at the earliest possible stage, for example in the context of consultations on contraception.
Conclusion
There was a near-doubling of snus use among pregnant women from 2012 to 2014. The proportion of women who quit using snus was significantly higher than of those who quit smoking during their pregnancy. The study confirms that the use of snus is increasing among pregnant women in the Agder counties and should this trend continue, it may represent a potential public health problem.
We wish to thank the Research group for primary doctors in the Agder counties for their peer guidance. The first author has received a grant from the Norwegian Medical Association’s research committee for general practice.
MAIN MESSAGE
From 2012 to 2014 the use of snus among pregnant women in the Agder counties nearly doubled.
The proportion that used snus before pregnancy and quit during pregnancy was higher than the proportion that quit smoking.
Of those who used snus or smoked before pregnancy, altogether 29 % of the snus users and 42 % of the smokers continued this habit throughout pregnancy.
- 1.
Helserisiko ved bruk av snus. Oslo: Nasjonalt folkehelseinstitutt, 2014. www.fhi.no/publ/2014/helserisiko-ved-bruk-av-snus/ (1.7.2016).
- 12.
Statistisk sentralbyrå. www.ssb.no/royk/ (1.7.2016).
- 13.
Lund KE, Tefre EM, Amundsen A et al. Røyking, bruk av snus og annen risikoatferd blant studenter. Tidsskr Nor Legeforen 2008; 128: 1808 – 11. [PubMed]
- 19.
Universitetet i Tromsø. Nyheter. Snusing kan forårsake dødfødte barn. 8.6.2012. https://uit.no/nyheter/artikkel?p_document_id=306019. (1.7.2016).
- 20.
Medisinsk fødselsregister. www.fhi.no/hn/helseregistre-og-biobanker/mfr/medisinsk-fodselsregister---helsere/ (1.7.2016).
- 21.
Tobaksvanor bland gravida. Medicinska födelseregistret 1973 – 2012. Artikelnr 2013-12-16. Stockholm: Socialstyrelsen, 2013.
- 24.
Luck W, Nau H, Hansen R et al. Extent of nicotine and cotinine transfer to the human fetus, placenta and amniotic fluid of smoking mothers. Dev Pharmacol Ther 1985; 8: 384 – 95. [PubMed]
Artikkelen Bruk av snus og røyketobakk hos gravide i Agder i Tidsskriftet nr. 16 (1), leiarartikkelen i same nummer og Folkehelseinstituttets risikovurdering av snus frå 2015 som vert sitert, nemner ikkje auka risiko for astma hos barnet som ein effekt av nikotinbruk under svangerskapet.
Det er godt dokumentert at røyking under svangerskapet aukar risikoen for astma hos barnet (2). Vidare, bestemors røyking medan ho gjekk gravid med mor, auka risikoen for astma hos barnebarnet om lag like mykje som mors røyking under svangerskapet (3). Vi har her å gjere med epigenetiske effekter over generasjonane. I placenta og lungevev frå foster frå røykande mødre er det påvist epigenetiske endringar som var spesielt hyppige i gen som hadde relasjon til astma og immunsystemet (4).
I ein eksperimentell studie førte perinatal nikotineksponering til astma ikkje berre hos avkommet, men også hos F2-generasjonen, altså hos ‘barnebarna’ til dei nikotin-eksponerte dyra (5, 6). Effektene av nikotin på lungeutviklinga hos ulike dyreartar (mus, rotte, sau, ape) er svært like, og verknaden på mennesket er neppe annleis (2). Dei molekylære mekanismane for at nikotin fører til astma er kjende (7,8,9). Dette aukar sannsynlegheita for at nikotin i fosterlivet kan føre til astma også hos menneskebarn. Dette blir understreka i to nylege kommentarartiklar i førande tidsskrift (2, 8).
Nikotineksponering i svangerskapet kan med stor sannsynlegheit vere årsak til astma hos kommande generasjonar. Gravide bør derfor unngå alle former for nikotintilførsel, også snus.
Litteratur
1. Rygh E, Gallefoss F, Reiso H. Bruk av snus og røyketobakk hos gravide i Agder. Tidsskr Nor Lægeforen 2016;136:1351-1354.
2. Spindel ER, McEvoy CT. The Role of nicotine in the effects of maternal smoking during pregnancy on lung development and childhood respiratory disease. Implications for dangers of e-cigarettes. Am J Respir Crit Care Med 2016;193:486-94.
3. Li YF, Langholz B, Salam MT et al. Maternal and grandmaternal smoking patterns are associated with early childhood asthma. Chest 2005;127:1232-41.
4. Chhabra D, Sharma S, Kho AT et al. Fetal lung and placental methylation is associated with in utero nicotine exposure. Epigenetics 2014;9:1473-84.
5. Rehan VK, Liu J, Naeem E et al. Perinatal nicotine exposure induces asthma in second generation offspring. BMC Med 2012;10:129.
6. Leslie FM. Multigenerational epigenetic effects of nicotine on lung function. BMC Med 2013;11:27.
7. Liu J, Sakurai R, Rehan VK. PPAR-γ agonist rosiglitazone reverses perinatal nicotine exposure-induced asthma in rat offspring. Am J Physiol Lung Cell Mol Physiol 2015;308:L788-96.
8. Gibbs K, Collaco JM, McGrath-Morrow SA. Impact of tobacco smoke and nicotine exposure on lung development. Chest 2016;149:552-61.
9. Spindel ER, McEvoy CT. Reply: Why pregnant women should avoid any form of nicotine during pregnancy: An elastin-based perspective. Am J Respir Crit Care Med 2016;194:247-8.
Takk til Martinus Løvik for hans kommentar til vår artikkel om bruk av snus og røyketobakk blant gravide i Agderfylkene.
Løvik viser til forskning som tyder på at nikotineksponering i fosterlivet kan gi økt risiko for astma via epigenetiske mekanismer. Likeledes skriver Geir W. Jacobsen i lederartikkelen (1) at barn av mødre som røykte i svangerskapet har økt risiko for overvekt senere i livet. Én av de aktuelle hypotesene er også her epigenetisk påvirkning i fosterlivet.
Det er sannsynlig at disse effektene av nikotin gjelder for alle nikotinholdige produkter, som snus, nikotinlegemidler og e-sigaretter. Alt i alt tilsier dette at man bør være meget tilbakeholdende med å anbefale bruk av snus og andre nikotinerstatningsprodukter til gravide. Vi er derfor enig med Løvik i at gravide bør unngå alle former for nikotintilførsel, også snus. Det er bra at Helsedirektoratet har hatt satt søkelys på dette i nylige kampanjer og i opplysningsmateriell rettet mot gravide på sine nettsider. Nyere forskning kan tyde på at nikotin kan gi epigenetiske forandringer også i primordiale germale celler, som da vil ramme genmaterialet til både gutter og jenter, og altså ikke bare påvirkning av fosteret in utero (2). Skal man virkelig være føre var, bør i så fall primærforebygging målrettes mot ungdom av begge kjønn før de får barn.
Litteratur
1. Jacobsen GW. Bør gravide avstå fra enhver bruk av nikotin? Tidsskr Nor Legeforen 2016; 136:1320-1320
2. Leslie, FM. Multigenerational epigenetic effects of nicotine on lung function. BMC Med 2013;11:27