Risk adjustment in measurements of predicted mortality after myocardial infarction
Quality-based funding or pay-for-performance of the Norwegian hospital sector was introduced on 1 January 2014, meaning that a proportion of the budgets of the regional health authorities is made dependent on the quality of the treatment they provide to patients, as measured by selected quality indicators. In 2014, NOK 497 million was earmarked for such funding. The purpose of the scheme is to ensure high quality and patient safety (1, 2).
The set of indicators used in quality-based funding in Norway includes structure, process and outcome indicators, altogether 29 different measures (3). In principle, this provides a broad description of the hospitals’ quality, and the diversity of indicators may in itself help prevent random variations in the budget allocations. The outcome indicators include a number of measures of survival, such as 30-day survival after a myocardial infarction. Survival and mortality are frequently used quality indicators internationally (4, 5). The Norwegian data material does not specify, however, how the survival figures have been adjusted for risk.
If the information on variations in quality is to be used as a criterion in a funding system, the variations in quality observed between different hospitals must be attributable to conditions that are under their control, and not any underlying variables. The objective of this study was to investigate how various forms of risk adjustment had an impact on predicted mortality after myocardial infarctions in the different hospital trusts.
Material and method
Sample, definitions and data
The data set encompassed patients ≥ 18 years, who had been discharged from Norwegian hospitals in 2009 with myocardial infarction (ICD-10 codes I21 and I22) as their main diagnosis. We used 30-day mortality as a quality indicator and included all causes of death.
The methodological approach was developed as part of the Finnish PERFECT project (6, 7) and further refined by EuroHOPE (8) – (10), a comparative project funded by the EU’s 7th framework programme. The unit of analysis was hospital episodes that started at admission and ended 30 days later or with the death of the patient (11).
A single hospital episode would include several hospitalisations if these were sequential and separated by one day or less. Two or more hospitalisations resulting from transfers between hospitals, for example as a result of percutaneous coronary intervention (PCI), were then counted as a single hospital episode. Only the first hospital episode in a year was included in the analysis, meaning that readmission did not generate a new episode. If the hospitals used different diagnoses over a single episode, the diagnostic codes from the highest-ranking hospital were chosen. If the hospital episode encompassed two or more hospitals at the same level of the hierarchy, the diagnostic codes from the first hospital in the episode were used.
To improve the comparability of the patient population across hospitals, we excluded patients who had been admitted to hospital for acute myocardial infarction during the 365 days prior to the index day. Thereafter, the data that described the patients’ risk profiles were linked at the individual level. In addition to gender and age, the following variables were included in the risk adjustment: comorbidity, socioeconomic status, procedures, travel time to the nearest PCI centre and type of myocardial infarction.
Data on hospitalisations, as well as dates of admission and discharge, main and secondary diagnoses, comorbidity and procedures were retrieved from the Norwegian Patient Register. Data on mortality were established on the basis of information from the Causes of Death Registry. Information on medication use was retrieved from the Prescription Registry. «FD-trygd» (Statistics Norway’s database on social assistance payments – «Forløpsdatabasen trygd») provided us with access to data on income, assets, education and disability benefits. The population data are as of 31 December 2009.
The EuroHOPE project has been approved by the Regional Committee on Medical and Health Research Ethics for South-Eastern Norway. Since the project also uses data from the Prescription Registry, a licence was applied for and granted by the Norwegian Data Protection Authority.
Variables
We established variables to describe comorbidity on the basis of hospital data on admissions over the last 365 days prior to the index day and data on medication use from the Norwegian Prescription Registry for the same period (8). For example, patients whose main or secondary diagnosis was hypertension, as well as patients who had been prescribed with anti-hypertension drugs, were registered with hypertension as a comorbidity.
The inclusion of medication use in addition to the registered main and secondary diagnoses caused the proportion of patients with hypertension as a comorbidity in the material to rise by 50 %. The proportion of patients with diabetes, asthma and depression rose by approximately 10 %. With regard to the remaining comorbidities, the inclusion of data from the Prescription Registry caused no more than minor changes.
Socioeconomic conditions were described in terms of variables that have been shown to correlate with mortality from myocardial infarction (10, 12, 13): income, assets, receipt of disability benefit and level of education. Income was defined as the average total personal gross income in the period 2000 – 2008, and assets as average gross personal assets in the same years. We registered whether the patient had received disability benefit in 2008 or earlier. Education was classified as primary/lower secondary, upper secondary and university/university college.
Myocardial-infarction patients primarily receive thrombolytic treatment or percutaneous coronary intervention, while a minority undergo coronary artery bypass graft surgery (CABG). The patients were classified by their reception of thrombolytic or other drug-based treatment, percutaneous coronary intervention or coronary artery bypass graft. Travel time in minutes by car from the centre of the patient’s home municipality to the nearest PCI centre was estimated on the basis of data from Google Maps (14). We made an assumption of non-linearity, since car and boat ambulances are replaced by helicopters when travel distances are extensive and estimated to take more than one hour (15).
To improve the comparability of the patient population across hospitals, the type of myocardial infarction was registered. The hospitals’ classification of patients in the sub-groups of the ICD system is based on discretionary judgement. We therefore estimated the models with as well as without the variables that described the type of myocardial infarction.
Statistical analyses
Descriptive statistics are presented for each hospital trust as averages for continuous variables and as proportions for categorical variables. For reasons of space, we present only the average number of comorbidities for each patient (Table 1). Information on individual comorbidities included in the regression models are grouped by hospital trust and presented in e-Table 2.
Table 1
Description of the patient population discharged with the diagnosis myocardial infarction in Norwegian hospitals in 2009, by the hospital trusts’ catchment areas
| Hospital trust |
Number of hospital episodes |
Incidence per 10 000 inhabitants |
Proportion of deaths, 30 days (%) |
Number of comorbidities (average) |
Proportion men (%) |
Age (years) (average) |
| Akershus University Hospital |
600 |
33.5 |
9.0 |
1.6 |
61.5 |
69.7 |
| Asker og Bærum |
210 |
16.9 |
5.2 |
1.5 |
56.7 |
75.3 |
| Bergen |
864 |
27.6 |
9.3 |
1.5 |
64.7 |
71.2 |
| Buskerud |
616 |
30.8 |
8.6 |
1.5 |
65.7 |
70.2 |
| Finnmark |
222 |
39.8 |
8.1 |
1.4 |
66.7 |
69.7 |
| Fonna |
474 |
36.9 |
6.9 |
1.5 |
61.6 |
72.0 |
| Førde |
254 |
31.2 |
12.6 |
1.6 |
60.6 |
75.4 |
| Helgeland |
175 |
29.3 |
9.1 |
1.4 |
59.4 |
72.6 |
| Innlandet |
1 034 |
33.2 |
9.2 |
1.6 |
62.9 |
72.3 |
| Nord-Trøndelag |
330 |
32.3 |
7.9 |
1.4 |
66.1 |
71.4 |
| Nordland |
346 |
33.6 |
8.1 |
1.6 |
58.4 |
73.4 |
| Nordmøre og Romsdal |
290 |
32.2 |
7.6 |
1.4 |
55.9 |
74.0 |
| Oslo |
1 149 |
20.7 |
8.1 |
1.7 |
56.9 |
73.6 |
| Stavanger |
552 |
22.7 |
8.5 |
1.3 |
65.4 |
69.3 |
| Sunnmøre |
339 |
33.3 |
8.3 |
1.7 |
61.1 |
74.7 |
| Sør-Trøndelag |
631 |
28.0 |
8.6 |
1.5 |
60.4 |
71.6 |
| Sørlandet |
429 |
20.2 |
9.3 |
1.4 |
62.0 |
70.5 |
| University Hospital of North Norway |
466 |
33.0 |
8.6 |
1.4 |
66.5 |
70.7 |
| Vestfold og Telemark |
999 |
32.1 |
8.5 |
1.5 |
61.2 |
71.1 |
| Østfold |
737 |
35.0 |
9.1 |
1.7 |
61.2 |
71.0 |
| Norway as a whole |
10 717 |
28.6 |
8.6 |
1.5 |
61.8 |
71.8 |
Table 2
Prevalence of comorbidities in per cent, by hospital trust
| Hospital trust |
Hypertension |
Coronary heart disease |
Heart fibrillation |
Heart failure |
Diabetes mellitus |
Atherosclerosis |
Cancer |
COPD/asthma |
Dementia |
Depression |
Parkinson’s disease |
Mental disorders |
Renal failure |
Alcoholism |
Stroke |
|
| Akershus University Hospital |
64 |
13 |
7 |
4 |
17 |
2 |
2 |
22 |
4 |
13 |
1 |
4 |
4 |
1 |
4 |
|
| Asker og Bærum |
56 |
12 |
7 |
7 |
19 |
1 |
4 |
15 |
3 |
12 |
0 |
3 |
4 |
0 |
3 |
|
| Bergen |
59 |
14 |
6 |
6 |
16 |
2 |
2 |
14 |
4 |
13 |
2 |
4 |
2 |
0 |
3 |
|
| Buskerud |
62 |
15 |
7 |
6 |
17 |
2 |
2 |
17 |
4 |
10 |
1 |
3 |
3 |
0 |
2 |
|
| Finnmark |
60 |
18 |
5 |
5 |
11 |
3 |
1 |
23 |
3 |
5 |
0 |
4 |
1 |
0 |
5 |
|
| Fonna |
67 |
13 |
6 |
7 |
12 |
1 |
2 |
17 |
4 |
14 |
0 |
3 |
3 |
0 |
3 |
|
| Førde |
66 |
12 |
9 |
8 |
15 |
1 |
2 |
14 |
8 |
11 |
0 |
4 |
5 |
1 |
5 |
|
| Helgeland |
63 |
13 |
5 |
3 |
13 |
0 |
3 |
14 |
3 |
15 |
1 |
3 |
2 |
0 |
3 |
|
| Innlandet |
68 |
16 |
6 |
7 |
17 |
2 |
2 |
18 |
3 |
14 |
1 |
3 |
3 |
1 |
4 |
|
| Nord-Trøndelag |
62 |
13 |
6 |
5 |
13 |
2 |
2 |
11 |
5 |
14 |
2 |
2 |
2 |
1 |
3 |
|
| Nordland |
65 |
14 |
7 |
7 |
14 |
3 |
1 |
19 |
4 |
9 |
2 |
3 |
5 |
1 |
3 |
|
| Nordmøre og Romsdal |
62 |
11 |
7 |
7 |
13 |
2 |
3 |
15 |
4 |
8 |
1 |
2 |
3 |
0 |
3 |
|
| Oslo |
62 |
17 |
8 |
8 |
18 |
2 |
3 |
16 |
7 |
12 |
1 |
4 |
4 |
2 |
5 |
|
| Stavanger |
57 |
12 |
5 |
4 |
12 |
1 |
0 |
14 |
2 |
14 |
1 |
4 |
3 |
1 |
2 |
|
| Sunnmøre |
64 |
18 |
9 |
6 |
15 |
3 |
2 |
17 |
6 |
14 |
0 |
2 |
4 |
1 |
5 |
|
| Sør-Trøndelag |
59 |
13 |
5 |
6 |
15 |
1 |
2 |
16 |
4 |
15 |
2 |
3 |
3 |
0 |
5 |
|
| Sørlandet |
59 |
7 |
5 |
5 |
14 |
2 |
2 |
18 |
3 |
12 |
2 |
2 |
3 |
1 |
2 |
|
| University Hospital of North Norway |
64 |
14 |
6 |
3 |
13 |
2 |
2 |
16 |
4 |
12 |
1 |
2 |
2 |
0 |
3 |
|
| Vestfold |
65 |
14 |
6 |
6 |
14 |
2 |
3 |
16 |
3 |
12 |
1 |
3 |
3 |
0 |
3 |
|
| Østfold |
70 |
13 |
7 |
8 |
20 |
2 |
3 |
18 |
2 |
15 |
1 |
5 |
3 |
1 |
4 |
|
| Norway |
63 |
14 |
7 |
6 |
16 |
2 |
2 |
17 |
4 |
13 |
1 |
3 |
3 |
1 |
4 |
|
We used logistic regression analysis with 30-day mortality as the outcome measure. To avoid non-linear effects on the log scale, all continuous covariates were categorised. The age categories were 18 – 49 years, followed by five-year categories up to 89 years, plus one category that encompassed patients who were 90 years or older. Income and assets were divided into the categories NOK 0 – 150 000, NOK 150 000 – 300 000, NOK 300 000 – 500 000 and NOK ≥ 500 000. Travel time was divided into the categories 0 – 60 minutes, 60 – 120 minutes, 120 – 180 minutes and ≥ 180 minutes.
Three models for risk adjustment were used (9, 10):
Model 1: adjustment for age and gender
Model 2: adjustment for age, gender, comorbidities, socioeconomic variables, travel time and type of myocardial infarction
Model 3: all variables in Model 2, plus adjustment for whether or not percutaneous coronary intervention had been undertaken in the course of 14 days after admission.
The variables were used to estimate risk-adjusted proportions of deaths within a 95 % confidence interval (95 % CI) for each hospital trust. To depict how well the models were able to classify the patients in the data material correctly, i.e. to identify the dead patients as dead and the living as still alive, we provide some AUC values («area under the curve»). An AUC value of 0.5 means that the model classifies no better than the toss of a coin.
Data management was undertaken in SAS version 9.2 (16) and the further analyses were made in Stata version 12.1 (17).
Other methodological issues
The analyses were undertaken at the hospital-trust level on the basis of the enterprise structure such as it was in the first half of 2009. The patients were grouped by hospital trust on the basis of the trusts’ catchment areas. This means that a patient with a residential address in a municipality that fell within the catchment area of a specific hospital trust was classified under this hospital trust, irrespective of where he or she was actually treated.
Results
Description of the patient population
After the exclusion of patients who had been treated for acute myocardial infarction during the last 365 days prior to the index date (n = 1 718), the data material encompassed 10 717 patients. Table 1 presents data on these patients. Supplementary information on comorbidities and sociodemographic factors is presented in e-Tables 2 and 3.
Table 3
Description of the patient population discharged with a diagnosis of myocardial infarction in Norwegian hospitals in 2009, by the hospital trusts’ catchment areas. N = 10 717
| Hospital trust |
Income in NOK 100 000 (average) |
Assets in NOK 100 000 (average) |
Disabled (%) |
Upper secondary school (%) |
University/ university college (%) |
Trans infarction¹ (%) |
Sub infarction² (%) |
Spec. infarction³ (%) |
Unspec. infarction⁴ (%) |
Distance to PCI centre in minutes (average) |
| Akershus University Hospital |
283 |
516 |
16.0 |
41.9 |
12.9 |
27.7 |
53.7 |
4.5 |
14.1 |
24 |
| Asker og Bærum |
342 |
1 004 |
10.0 |
44.8 |
37.4 |
19.5 |
58.6 |
1.4 |
20.5 |
16 |
| Bergen |
279 |
574 |
12.7 |
45.2 |
13.8 |
27.5 |
45.6 |
8.3 |
18.6 |
24 |
| Buskerud |
275 |
590 |
13.3 |
45.8 |
10.0 |
18.6 |
59.6 |
4.2 |
17.6 |
63 |
| Finnmark |
245 |
403 |
21.2 |
36.8 |
9.1 |
17.6 |
54.5 |
3.6 |
24.3 |
476 |
| Fonna |
253 |
576 |
16.0 |
48.3 |
10.0 |
19.8 |
54.6 |
3.2 |
22.4 |
136 |
| Førde |
225 |
562 |
13.4 |
48.8 |
9.6 |
22.4 |
48.8 |
7.1 |
21.7 |
229 |
| Helgeland |
217 |
390 |
22.2 |
34.5 |
8.0 |
26.3 |
57.7 |
7.4 |
8.6 |
370 |
| Innlandet |
238 |
494 |
16.0 |
39.9 |
8.7 |
23.0 |
53.7 |
4.8 |
18.5 |
87 |
| Nord-Trøndelag |
240 |
443 |
19.1 |
47.9 |
7.9 |
26.4 |
51.5 |
6.7 |
15.4 |
120 |
| Nordland |
227 |
433 |
19.1 |
39.4 |
7.3 |
14.7 |
59.5 |
9.2 |
16.6 |
412 |
| Nordmøre og Romsdal |
243 |
640 |
15.5 |
44.7 |
8.2 |
22.4 |
51.4 |
4.8 |
21.4 |
201 |
| Oslo |
297 |
697 |
11.8 |
45.9 |
21.1 |
27.2 |
53.4 |
5.0 |
14.4 |
14 |
| Stavanger |
289 |
548 |
13.2 |
48.2 |
11.5 |
36.3 |
47.2 |
7.4 |
9.1 |
25 |
| Sunnmøre |
235 |
518 |
12.7 |
46.6 |
7.4 |
17.7 |
54.3 |
6.8 |
21.2 |
337 |
| Sør-Trøndelag |
246 |
489 |
17.3 |
42.5 |
12.9 |
30.0 |
45.8 |
5.7 |
18.5 |
38 |
| Sørlandet |
251 |
498 |
22.1 |
50.7 |
14.5 |
26.8 |
57.6 |
6.3 |
9.3 |
54 |
| University Hospital of North Norway |
249 |
396 |
19.3 |
43.2 |
11.3 |
29.4 |
47.4 |
6.2 |
17.0 |
141 |
| Vestfold og Telemark |
260 |
532 |
18.1 |
47.7 |
11.6 |
19.7 |
59.2 |
5.1 |
16.0 |
90 |
| Østfold |
240 |
476 |
19.9 |
45.7 |
7.8 |
23.2 |
54.5 |
3.9 |
18.4 |
65 |
| Norway |
260 |
542 |
16.0 |
44.8 |
12.2 |
24.5 |
53.2 |
5.5 |
16.8 |
102 |
| [i] | ||||||||||
[i] ¹ Trans infarction: First-time infarctions, transmural (ICD-10: I21.0, I21.1, I21.2 and I21.3)
² Sub infarction: First-time infarctions, subendocardial (ICD-10: I21.4 and I21.9)
³ Spec. infarction: Subsequent infarctions, specified localisation (ICD-10: I22.0, I22.1 and I22.8)
⁴ Unspec. infarction: Subsequent infarctions, unspecified localisation (ICD-10: I22.9).
The incidence of myocardial infarction (the number of cases per 10 000 inhabitants) was 28.6 for the country as a whole, and varied from 16.9 in the catchment area of Asker og Bærum Hospital Trust to 39.8 in the catchment area of Finnmark Hospital Trust. The national average of unadjusted 30-day mortality amounted to 8.6 % – highest in Førde Hospital Trust (12.6 %) and lowest in Asker og Bærum (5.2 %). The prevalence of individual comorbidities varied considerably between the hospital trusts (e-Table 2).
Logistic regression analyses
Figure 1 shows the unadjusted proportions of deaths after 30 days, as well as the corresponding adjusted proportions for the three different approaches to risk adjustment. Precise figures and supplementary information on the regression coefficients are found in e-Table 4 – 7. On the whole, there were few confidence intervals for the individual hospital trusts that did not overlap with the national average of 8.6 % for 30-day mortality. Patients in the catchment area for Asker og Bærum Hospital Trust in the unadjusted analysis and in the analysis that was adjusted for gender and age, as well as patients in the catchment areas for Nordmøre og Romsdal and Sunnmøre hospital trusts are the exceptions. The two latter groups had a mortality of 5.2 % after risk adjustment for all covariates.
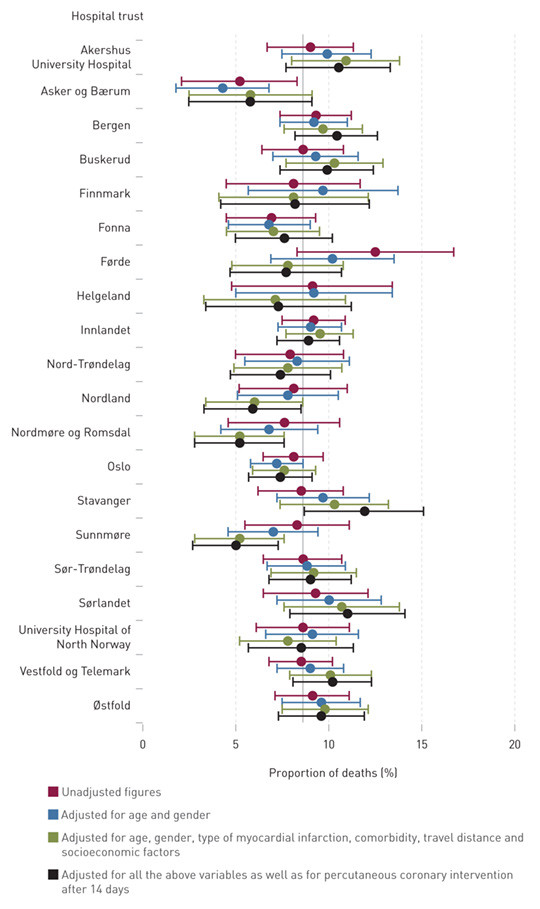
Table 4
Odds ratios with a 95 % confidence interval (95 % CI) from logistic regression analyses with 30-day mortality as outcome: unadjusted and adjusted for age and gender. Ref. = reference category. N = 10 717
| Unadjusted |
95 % CI |
Adjusted for age/gender |
95 % CI |
|
| Man |
1.02 |
0.89 – 1.18 |
||
| 8 – 49 years |
0.05 |
0.03 – 0.09 |
||
| 50 – 54 years |
0.02 |
0.01 – 0.06 |
||
| 55 – 59 years |
0.02 |
0.01 – 0.04 |
||
| 60 – 64 years |
0.06 |
0.04 – 0.09 |
||
| 65 – 69 years |
0.12 |
0.08 – 0.17 |
||
| 70 – 74 years |
0.19 |
0.14 – 0.26 |
||
| 75 – 79 years |
0.26 |
0.20 – 0.34 |
||
| 80 – 84 years |
0.48 |
0.38 – 0.60 |
||
| 85 – 89 years |
0.70 |
0.57 – 0.86 |
||
| > 90 years |
Ref. |
Ref. |
||
| Akershus University Hospital |
Ref. |
Ref. |
||
| Asker og Bærum |
0.56 |
0.29 – 1.09 |
0.39 |
0.20 – 0.78 |
| Bergen |
1.03 |
0.72 – 1.48 |
0.92 |
0.63 – 1.33 |
| Buskerud |
0.95 |
0.64 – 1.41 |
0.93 |
0.62 – 1.41 |
| Finnmark |
0.89 |
0.51 – 1.56 |
0.98 |
0.55 – 1.74 |
| Fonna |
0.76 |
0.48 – 1.19 |
0.65 |
0.41 – 1.03 |
| Førde |
1.46 |
0.92 – 2.32 |
1.04 |
0.64 – 1.69 |
| Helgeland |
1.02 |
0.57 – 1.83 |
0.92 |
0.50 – 1.69 |
| Innlandet |
0.86 |
0.72 – 1.45 |
0.90 |
0.62 – 1.29 |
| Nord-Trøndelag |
0.83 |
0.53 – 1.41 |
0.81 |
0.49 – 1.34 |
| Nordland |
0.89 |
0.55 – 1.43 |
0.75 |
0.46 – 1.23 |
| Nordmøre og Romsdal |
0.83 |
0.50 – 1.39 |
0.64 |
0.38 – 1.09 |
| Oslo |
0.89 |
0.63 – 1.26 |
0.69 |
0.48 – 0.99 |
| Stavanger |
0.84 |
0.62 – 1.41 |
0.98 |
0.64 – 1.49 |
| Sunnmøre |
0.91 |
0.56 – 1.47 |
0.67 |
0.41 – 1.09 |
| Sør-Trøndelag |
0.95 |
0.64 – 1.40 |
0.87 |
0.58 – 1.31 |
| Sørlandet |
1.04 |
0.68 – 1.60 |
1.01 |
0.65 – 1.58 |
| University Hospital of North Norway |
0.95 |
0.62 – 1.45 |
0.90 |
0.58 – 1.41 |
| Vestfold |
0.94 |
0.66 – 1.34 |
0.90 |
0.62 – 1.30 |
| Østfold |
1.01 |
0.69 – 1.47 |
0.96 |
0.65 – 1.43 |
Table 5
Odds ratios with a 95 % confidence interval (95 % CI) from logistic regression analyses with 30-day mortality as outcome: adjusted for all background variables (age, gender, type of myocardial infarction, individual comorbidities for which not having the comorbidity is the reference category, distance and socioeconomic factors), as well as all and percutaneous coronary intervention (PCI) after 14 days. Ref. = reference category. N = 10 379
| Adjusted for all |
95 % CI |
Adjusted for all + PCI |
95 % CI |
|
| Man |
1.06 |
0.90 – 1.24 |
1.12 |
0.95 – 1.31 |
| 18 – 49 years |
0.05 |
0.02 – 0.09 |
0.08 |
0.04 – 0.16 |
| 50 – 54 years |
0.02 |
0.01 – 0.06 |
0.04 |
0.02 – 0.11 |
| 55 – 59 years |
0.02 |
0.01 – 0.05 |
0.03 |
0.01 – 0.08 |
| 60 – 64 years |
0.05 |
0.03 – 0.08 |
0.08 |
0.05 – 0.14 |
| 65 – 69 years |
0.09 |
0.06 – 0.15 |
0.15 |
0.10 – 0.25 |
| 70 – 74 years |
0.17 |
0.12 – 0.24 |
0.25 |
0.18 – 0.37 |
| 75 – 79 years |
0.27 |
0.21 – 0.36 |
0.38 |
0.28 – 0.50 |
| 80 – 84 years |
0.49 |
0.39 – 0.62 |
0.60 |
0.47 – 0.75 |
| 85 – 89 years |
0.69 |
0.56 – 0.86 |
0.75 |
0.61 – 0.93 |
| > 90 years |
Ref. |
Ref. |
||
| Transmural first-time infarctions |
Ref. |
Ref. |
||
| Subendocardial first-time infarctions |
0.52 |
0.43 – 0.63 |
0.40 |
0.33 – 0.49 |
| Specified localised subsequent infarctions |
1.09 |
0.80 – 1.47 |
0.88 |
0.64 – 1.20 |
| Unspecified localised subsequent infarctions |
0.68 |
0.54 – 0.86 |
0.52 |
0.41 – 0.66 |
| Hypertension |
0.82 |
0.69 – 0.98 |
0.82 |
0.68 – 0.98 |
| Coronary heart disease |
0.74 |
0.59 – 0.92 |
0.74 |
0.59 – 0.93 |
| Heart fibrillation |
1.19 |
0.92 – 1.54 |
1.15 |
0.89 – 1.48 |
| Heart failure |
1.54 |
1.18 – 2.00 |
1.48 |
1.13 – 1.92 |
| Diabetes mellitus |
1.22 |
1.01 – 1.48 |
1.19 |
0.98 – 1.45 |
| Atherosclerosis |
1.53 |
0.99 – 2.36 |
1.49 |
0.97 – 2.31 |
| Cancer |
2.08 |
1.41 – 3.06 |
1.88 |
1.28 – 2.77 |
| COPD/asthma |
0.92 |
0.76 – 1.12 |
0.88 |
0.72 – 1.07 |
| Dementia |
1.90 |
1.47 – 2.45 |
1.71 |
1.33 – 2.21 |
| Depression |
1.15 |
0.94 – 1.41 |
1.10 |
0.90 – 1.35 |
| Parkinson’s disease |
1.13 |
0.63 – 2.00 |
1.03 |
0.58 – 1.83 |
| Mental disorders |
1.93 |
1.34 – 2.77 |
1.90 |
1.31 – 2.74 |
| Renal failure |
1.75 |
1.28 – 2.39 |
1.65 |
1.20 – 2.26 |
| Alcoholism |
1.10 |
0.38 – 3.17 |
0.92 |
0.32 – 2.66 |
| Stroke |
1.42 |
1.04 – 1.93 |
1.32 |
0.97 – 1.79 |
| Income NOK 0 – 150 000 |
Ref. |
Ref. |
||
| NOK 150 000 – 300 000 |
0.81 |
0.68 – 0.97 |
0.82 |
0.68 – 0.98 |
| NOK 300 000 – 500 000 |
0.69 |
0.49 – 0.98 |
0.72 |
0.51 – 1.03 |
| More than NOK 500 000 |
0.90 |
0.51 – 1.59 |
0.91 |
0.52 – 1.62 |
| Assets NOK 0 – 150 000 |
Ref. |
Ref. |
||
| NOK 150 000 – 300 000 |
0.89 |
0.71 – 1.11 |
0.90 |
0.71 – 1.13 |
| NOK 300 000 – 500 000 |
0.91 |
0.73 – 1.15 |
0.92 |
0.73 – 1.16 |
| More than NOK 500 000 |
0.93 |
0.74 – 1.18 |
0.93 |
0.74 – 1.18 |
| Education primary/lower secondary |
Ref. |
Ref. |
||
| Upper secondary |
0.91 |
0.77 – 1.07 |
0.90 |
0.77 – 1.06 |
| University/university college |
0.86 |
0.63 – 1.17 |
0.90 |
0.66 – 1.23 |
| Disability benefit before 2008 |
1.73 |
1.19 – 2.49 |
1.64 |
1.13 – 2.37 |
| Travel distance 0 – 60 minutes |
Ref. |
Ref. |
||
| 60 – 120 minutes |
1.07 |
0.85 – 1.35 |
1.05 |
0.83 – 1.33 |
| 120 – 180 minutes |
1.16 |
0.83 – 1.62 |
1.12 |
0.80 – 1.57 |
| More than 180 minutes |
1.50 |
0.97 – 2.31 |
1.40 |
0.90 – 2.17 |
| PCI after 14 days |
0.24 |
0.19 – 0.31 |
||
| Akershus University Hospital |
Ref. |
Ref. |
||
| Asker og Bærum |
0.47 |
0.23 – 0.94 |
0.49 |
0.24 – 0.99 |
| Bergen |
0.86 |
0.58 – 1.28 |
0.98 |
0.66 – 1.46 |
| Buskerud |
0.93 |
0.60 – 1.44 |
0.93 |
0.60 – 1.45 |
| Finnmark |
0.69 |
0.33 – 1.44 |
0.73 |
0.35 – 1.54 |
| Fonna |
0.58 |
0.33 – 1.02 |
0.67 |
0.38 – 1.16 |
| Førde |
0.66 |
0.35 – 1.23 |
0.68 |
0.36 – 1.28 |
| Helgeland |
0.59 |
0.28 – 1.27 |
0.64 |
0.30 – 1.38 |
| Innlandet |
0.84 |
0.56 – 1.27 |
0.81 |
0.54 – 1.22 |
| Nord-Trøndelag |
0.66 |
0.38 – 1.17 |
0.65 |
0.37 – 1.15 |
| Nordland |
0.48 |
0.25 – 0.94 |
0.49 |
0.25 – 0.97 |
| Nordmøre og Romsdal |
0.41 |
0.21 – 0.81 |
0.43 |
0.22 – 0.85 |
| Oslo |
0.64 |
0.43 – 0.94 |
0.65 |
0.44 – 0.95 |
| Stavanger |
0.94 |
0.60 – 1.47 |
1.19 |
0.75 – 1.87 |
| Sunnmøre |
0.42 |
0.22 – 0.81 |
0.41 |
0.21 – 0.81 |
| Sør-Trøndelag |
0.81 |
0.52 – 1.24 |
0.82 |
0.53 – 1.27 |
| Sørlandet |
0.98 |
0.61 – 1.58 |
1.06 |
0.65 – 1.71 |
| University Hospital of North Norway |
0.67 |
0.39 – 1.15 |
0.77 |
0.44 – 1.35 |
| Vestfold |
0.91 |
0.59 – 1.42 |
0.96 |
0.62 – 1.50 |
| Østfold |
0.87 |
0.56 – 1.36 |
0.89 |
0.57 – 1.39 |
Table 6
Proportion of deaths after 30 days with a 95 % confidence interval (95 % CI), unadjusted (N = 10 717), adjusted for age and gender (N = 10 717) and adjusted for all covariates (age, gender, type of myocardial infarction, comorbidity, distance and socioeconomic factors, N = 10 379). All figures are percentages
| Hospital trust |
Unadjusted |
95 % CI |
Adjusted for age/gender |
95 % CI |
Adjusted for all |
95 % CI |
| Akershus University Hospital |
9.0 |
6.7 – 11.3 |
9.9 |
7.5 – 12.3 |
10.9 |
8.0 – 13.8 |
| Asker og Bærum |
5.2 |
2.2 – 8.3 |
4.3 |
1.9 – 6.8 |
5.8 |
2.5 – 9.1 |
| Bergen |
9.3 |
7.3 – 11.2 |
9.2 |
7.3 – 11.0 |
9.7 |
7.5 – 11.8 |
| Buskerud |
8.6 |
6.4 – 10.8 |
9.3 |
7.0 – 11.6 |
10.3 |
7.7 – 12.9 |
| Finnmark |
8.1 |
4.5 – 11.7 |
9.7 |
5.7 – 13.7 |
8.1 |
4.1 – 12.1 |
| Fonna |
6.9 |
4.6 – 9.3 |
6.8 |
4.6 – 9.0 |
7.0 |
4.5 – 9.5 |
| Førde |
12.5 |
8.5 – 16.7 |
10.2 |
7.0 – 13.5 |
7.8 |
4.7 – 10.8 |
| Helgeland |
9.1 |
4.9 – 13.4 |
9.2 |
5.1 – 13.4 |
7.1 |
3.3 – 10.9 |
| Innlandet |
9.2 |
7.4 – 10.9 |
9.0 |
7.4 – 10.7 |
9.5 |
7.7 – 11.3 |
| Nord-Trøndelag |
7.9 |
5.0 – 10.8 |
8.3 |
5.3 – 11.1 |
7.8 |
5.0 – 10.7 |
| Nordland |
8.1 |
5.2 – 11.0 |
7.8 |
5.1 – 10.5 |
6.0 |
3.3 – 8.6 |
| Nordmøre og Romsdal |
7.6 |
4.5 – 10.6 |
6.8 |
4.1 – 9.4 |
5.2 |
2.8 – 7.6 |
| Oslo |
8.1 |
6.5 – 9.7 |
7.2 |
5.8 – 8.6 |
7.6 |
5.8 – 9.3 |
| Stavanger |
8.5 |
6.2 – 10.8 |
9.7 |
7.2 – 12.2 |
10.3 |
7.5 – 13.2 |
| Sunnmøre |
8.3 |
5.3 – 11.1 |
7.0 |
4.6 – 9.4 |
5.2 |
2.9 – 7.6 |
| Sør-Trøndelag |
8.6 |
6.3 – 10.7 |
8.8 |
6.6 – 10.9 |
9.2 |
6.8 – 11.5 |
| Sørlandet |
9.3 |
6.6 – 12.1 |
10.0 |
7.2 – 12.8 |
10.7 |
7.6 – 13.8 |
| University Hospital of North Norway |
8.6 |
6.0 – 11.1 |
9.1 |
6.5 – 11.6 |
7.8 |
5.3 – 10.4 |
| Vestfold og Telemark |
8.5 |
6.8 – 10.2 |
9.0 |
7.3 – 10.8 |
10.1 |
8.0 – 12.3 |
| Østfold |
9.1 |
7.0 – 11.1 |
9.6 |
7.5 – 11.7 |
9.8 |
7.4 – 12.1 |
| Norway |
8.6 |
8.1 – 9.1 |
Table 7
Proportion of deaths after 30 days with a 95 % confidence interval (95 % CI), adjusted for all covariates (age, gender, type of myocardial infarction, comorbidity, distance and socioeconomic factors) and percutaneous coronary intervention (PCI) after 14 days. N = 10 379. All figures are percentages
| Hospital trust |
30-day survival |
95 % CI |
| Akershus University Hospital |
10.5 |
7.7 – 13.3 |
| Asker og Bærum |
5.8 |
2.6 – 9.1 |
| Bergen |
10.4 |
8.1 – 12.6 |
| Buskerud |
9.9 |
7.5 – 12.4 |
| Finnmark |
8.2 |
4.2 – 12.2 |
| Fonna |
7.6 |
4.9 – 10.2 |
| Førde |
7.7 |
4.7 – 10.7 |
| Helgeland |
7.3 |
3.5 – 11.2 |
| Innlandet |
8.9 |
7.2 – 10.6 |
| Nord-Trøndelag |
7.4 |
4.7 – 10.1 |
| Nordland |
5.9 |
3.3 – 8.5 |
| Nordmøre og Romsdal |
5.2 |
2.8 – 7.6 |
| Oslo |
7.4 |
5.7 – 9.1 |
| Stavanger |
11.9 |
8.8 – 15.1 |
| Sunnmøre |
5.0 |
2.8 – 7.3 |
| Sør-Trøndelag |
9.0 |
6.7 – 11.2 |
| Sørlandet |
11.0 |
7.8 – 14.1 |
| University Hospital of North Norway |
8.5 |
5.8 – 11.3 |
| Vestfold og Telemark |
10.2 |
8.0 – 12.3 |
| Østfold |
9.6 |
7.3 – 11.9 |
| Norway |
8.6 |
8.1 – 9.1 |
The prevalence of percutaneous coronary intervention and/or coronary artery bypass surgery after two and fourteen days by age group and hospital trust showed that the former treatment is more common in hospital trusts that have their own PCI centre when compared to the other hospital trusts (e‑Table 8).
Table 8
Description of treatment. Percutaneous coronary intervention (PCI) after 2 and 14 days, PCA = PCI and/or coronary artery bypass surgery after 2 and 14 days by age group (18 – 79 years/> 80 years) and hospital trust. All figures are percentages
| Hospital trust |
PCI 2 d 18 – 79 |
PCI 2 d > 80 |
PCI 14 d 18 – 79 |
PCI 14 d > 80 |
PCA 2 d 18 – 79 |
PCA 2 d > 80 |
PCA14 d 18 – 79 |
PCA 14 d > 80 |
| Akershus University Hospital |
46.1 |
8.7 |
54.3 |
13.8 |
46.1 |
9.2 |
60.7 |
14.9 |
| Asker og Bærum |
45.2 |
11.6 |
48.7 |
20.0 |
46.1 |
11.6 |
59.1 |
20.0 |
| Bergen |
50.4 |
13.1 |
68.5 |
24.5 |
51.6 |
13.1 |
73.3 |
24.8 |
| Buskerud |
43.7 |
8.1 |
52.5 |
10.2 |
45.3 |
8.1 |
59.9 |
12.6 |
| Finnmark |
27.2 |
11.7 |
45.1 |
18.3 |
30.2 |
11.7 |
56.8 |
23.3 |
| Fonna |
37.0 |
12.9 |
54.5 |
19.9 |
38.3 |
12.9 |
60.4 |
20.5 |
| Førde |
33.6 |
8.1 |
55.0 |
10.6 |
34.4 |
8.1 |
60.3 |
10.6 |
| Helgeland |
23.5 |
0.0 |
54.6 |
10.7 |
26.9 |
0.0 |
75.6 |
16.1 |
| Innlandet |
32.6 |
4.4 |
47.8 |
9.7 |
34.3 |
4.6 |
54.0 |
10.8 |
| Nord-Trøndelag |
30.9 |
5.3 |
48.4 |
8.0 |
32.7 |
5.3 |
58.1 |
8.8 |
| Nordland |
16.3 |
2.3 |
44.7 |
9.1 |
18.1 |
2.3 |
57.7 |
11.5 |
| Nordmøre og Romsdal |
30.1 |
3.4 |
53.5 |
7.6 |
32.0 |
3.4 |
55.8 |
9.3 |
| Oslo |
44.4 |
10.7 |
51.8 |
13.2 |
45.3 |
10.7 |
55.7 |
13.4 |
| Stavanger |
71.7 |
32.3 |
73.5 |
32.9 |
72.5 |
32.3 |
75.8 |
32.9 |
| Sunnmøre |
18.9 |
1.9 |
40.0 |
4.5 |
22.7 |
1.9 |
48.6 |
5.8 |
| Sør-Trøndelag |
59.4 |
7.4 |
66.1 |
8.8 |
61.0 |
7.4 |
69.7 |
9.3 |
| Sørlandet |
61.0 |
12.2 |
67.2 |
17.3 |
64.1 |
12.2 |
74.1 |
19.4 |
| University Hospital of North Norway |
49.8 |
15.9 |
64.4 |
23.6 |
55.0 |
16.6 |
76.7 |
28.0 |
| Vestfold og Telemark |
43.3 |
10.8 |
51.6 |
17.6 |
44.4 |
10.8 |
61.2 |
18.5 |
| Østfold |
43.6 |
4.1 |
57.2 |
11.8 |
46.8 |
4.1 |
64.4 |
14.6 |
| Norway |
43.4 |
9.5 |
56.0 |
14.7 |
45.2 |
9.6 |
63.0 |
16.0 |
The unadjusted model had an AUC value of 0.52, i.e. about the same as the toss of a coin. When we added age and gender, the value rose to 0.76. It rose further to 0.80 when the type of myocardial infarction, comorbidities, socioeconomic variables and travel distance were added, climbing to 0.81 when we also included percutaneous coronary intervention after 14 days.
Discussion
Use of quality-based funding, in which data on survival are included in the quality indicators, may encourage the hospitals to treat patients wherever good results may be expected. If no control for underlying variables is made, this may give rise to misallocation of resources. Absence of risk adjustment may thus be a disadvantage, for patients with serious diseases that are hard to treat, as well as for the hospitals that provide care to these patients. For example, it has been shown that the introduction of quality indicators for heart surgery in New York and Pennsylvania gave rise to patient selection among the hospitals (18).
The model used for quality-based funding in Norway does not clarify how the risk adjustment has been undertaken (3). The objective of this study was thus to investigate how various forms of risk adjustment affected the predicted mortality, using patients discharged with a diagnosis of acute myocardial infarction as an example.
The main conclusions from the analysis are that gender, age, comorbidity, disability and travel time are candidate variables that should be considered for inclusion in the adjustment. Other variables to which we have had no access, for example information on genetic factors (19), may also be relevant. The socioeconomic variables made a smaller contribution to the risk adjustment once the former variables had been included.
Even though this analysis has a limited statistical strength and there were few confidence intervals that did not overlap with the national average for 30-day mortality, the changes that occurred as a result of the risk adjustments are important in terms of how resources are allocated in a quality-based funding system. Estimated mortality changed significantly for patients in the catchment areas for the Asker og Bærum, Stavanger, Sunnmøre, and Nordmøre og Romsdal hospital trusts, and also for Førde when further variables were included. Therefore, the main conclusion from the analysis is that controls for a broad range of underlying variables should be made, both when quality information is published and when quality indicators are used as a basis for the funding system.
In the normative debate on how quality-based funding systems should be designed, questions are raised regarding whether the use of procedures should be included as a quality indicator (20). The only variable included in our analysis that can be linked to the treatment provided by the hospital trust was percutaneous coronary intervention.
Two issues render it obvious that rewards for this type of treatment may not be a good solution. It may give rise to overtreatment and result in a geographically skewed distribution of resources due to the current structure of PCI centres, since this method is more common in hospital trusts that have a PCI centre when compared to those that have none. This applies also to percutaneous coronary interventions after 14 days and reflects the opportunities for emergency treatment with the aid of this method as well as the expected effectiveness of such treatment after the acute phase. The list of procedures that could be included in the analysis may be expanded, however. With regard to myocardial-infarction patients, rehabilitation, check-ups and medication use may provide relevant procedure variables.
While the decision to perform percutaneous coronary intervention is made at the clinical level in the hospital, a number of other variables may be influenced at the local or regional level within the health-enterprise system. Travel time to the PCI centre is one example. Seen in isolation, if long distances give rise to higher mortality and a decision is made to adjust for distances in the allocation model, this may entail a premium on centralisation of the activities. The size of the hospital trusts is another example of issues that can be influenced and may have an effect on the results of the type of analyses that we have undertaken. If the analyses are undertaken on the basis of the hospital trusts’ catchment areas, large hospital trusts will, seen in isolation, demonstrate less inter-trust variation when compared to a greater number of small hospital trusts.
Our analysis represents an example of how risk adjustment may be undertaken to provide a basis for quality-based funding. The analysis has its limitations, however. To increase the strength of the analysis we should ideally have used data for more than one year. For some hospital trusts, however, the results reveal confidence intervals that do not overlap with the national average if their mortality rates lie 3 – 4 % above or below this level. One key question that remains unclarified concerns how much the mortality rate for each hospital trust should be permitted to deviate from the national average before this will have an effect on the budget allocations to the regional hospital trusts.
The data need to be as updated as possible, to permit the hospital staff to see the financial effects of quality changes in the course of one or two years. For practical reasons, especially because of the time it takes to process applications for data access and retrieve the data, we have used data for 2009. Improvements to contingency planning have been made in recent years, and the analysis may therefore have yielded different results today. The travel-time variable that we have used could also be improved by including patient-level data from the database that registers information on ambulance call-outs (Akuttmedisinsk informasjonssystem, AMIS).
We have based this study on the responsibility of the hospital trusts to provide care, meaning that the patient’s residential address decides his or her affiliation to a particular hospital trust. The Norwegian Knowledge Centre for the Health Services base their analyses of survival and readmissions to Norwegian hospitals on the actual place of treatment, weighted by hospitalisation time if multiple locations are involved.
These two different perspectives entail consequences in terms of who will be held responsible for the patient’s treatment outcome. While we hold responsible the hospital trust that in practice is charged with providing care to the patient, the Knowledge Centre places this responsibility with the hospital trust that actually provides treatment. In a system of quality-based funding it is essential to have a well-considered opinion regarding the choice of one perspective or the other. We see no reason why the funding in this respect should deviate from the principles that have been chosen for funding of the hospital trusts in general.
We wish to thank our clinical experts Morten Grundtvig, Åsmund Reikvam and Cecilie Risøe for their discussion of operationalisations and patient pathways for myocardial-infarction patients. All assessments are the responsibility of the authors. The analysis was funded by the Research Council of Norway’s project no. 191390 «More for less» and the EU’s 7th framework programme, project no. 241721, «EuroHOPE».
MAIN MESSAGE
Thirty-day survival after hospitalisation for myocardial infarction is a criterion in quality-based funding.
The use of quality indicators in funding presupposes that variations are not caused by underlying variables.
Mortality varies according to the methods used for risk adjustment.
Risk adjustment of quality indicators requires well-documented models.
- 1.
Meld. St. 10 (2012 – 2013). God kvalitet – trygge tjenester — Kvalitet og pasientsikkerhet i helse- og omsorgstjenesten. www.regjeringen.no/no/dokumenter/meld-st-10-20122013/id709025/ (23.1.2016).
- 2.
Prop. 1 S (2013 – 2014). Gul bok. For budsjettåret 2014. www.regjeringen.no/no/dokumenter/prop-1-s-20132014--2/id739677/ (23.1.2016).
- 3.
Kiviluouta L, Arneberg F. Kvalitetsbasert finansiering 2014. Oslo: Helsedirektoratet, 2013.
- 14.
Ozimek A, Miles D. Stata utilities for geocoding and generating travel time and travel distance information. Stata J 2011; 11: 106 – 19.
- 15.
Strømsøe V. Do place and socio economic status matter? Analysis of inequalities in the probability of PCI for AMI in Norway 1999 – 2007 with respect to geographical location, socio economic status and demography. Oslo: Avdeling for helseledelse og helseøkonomi, Institutt for helse og samfunn, Universitetet i Oslo.
- 16.
SAS (R) 9.2 Language Reference. 4. utg. Cary, NC: SAS Institute, 2011.
- 17.
StataCorp. Stata Statistical Software: Release 12. College Station, TX: StataCorp, 2011.
- 18.
Dranove D, Kessler D, McClellan M et al. Is more information better? The effects of «Report cards» on health care providers. J Polit Econ 2003; 111: 555 – 88. [CrossRef]
Vi har med interesse lest Hagen, Iversen og Mogers artikkel der de viser hvorledes risikojusterte verdier for 30 dagers mortalitet etter hjerteinfarkt endres avhengig av hvilke variabler som inngår i regresjonsmodellen for risikojustering (1). Best samsvar mellom predikert og faktisk mortalitet forelå der man justerte for alder, kjønn, grad av sykdom (hjerteinfarkt), komorbiditet, reisetid og PCI innen 14 dager.
Studien illustrerer utstrakt bruk av registerdata og er både forbilledlig og betimelig all den tid våre helsemyndigheter allerede er i gang med å fordele deler av helseforetakenes finansiering basert på kvalitetsindikatorer (KBF: kvalitetsbasert finansiering). 30 dagers mortalitet etter hjerteinfarkt er en av en rekke målte kvalitetsindikatorer som her inngår med uklar risikojustering.
Det er ikke første gang det etterlyses en troverdig risikojustering av kvalitetsdata av typen behandlingsresultater som publiseres på Helsedirektoratets hjemmesider (helsenorge.no) og som nå ligger til grunn for KBF. Vi har tidligere påpekt at dersom man skal sammenligne kvalitetsmål av typen behandlingsresultater, så må adekvate og kontinuerlig oppdaterte modeller for risikojustering være på plass (1).
30 dagers mortalitet etter hjerteinfarkt er 1 av 10 kvalitetsindikatorer av type behandlingsresultater som inngår i KBF. Her har man etter vår mening en stor jobb å gjøre med å etablere gode modeller for risikojustering etter mønster av Hagen og medforfattere.
Ved siden av uklar risikojustering deler vi artikkelforfatternes bekymring for at KBF kan lede til uheldig tilpasninger i form av seleksjon og overbehandling av pasientgrupper. Kodeverket (ICD) åpner også for en viss grad av skjønn når alvorlighet av sykdom skal beskrives. Vi har tidligere sett eksempler på uheldig bruk av diagnoseverktøyet når det får økonomiske konsekvenser.
Et poeng som også nevnes er at kvalitetmåls nærhet i tid og sted er viktig for at det skal oppleves som meningsfullt for de som bidrar. Det kan være en viss fare for at belønningssystemer basert på 30 ulike indikatormål på overordnet foretaksnivå vil drukne den enkeltes innsats og på den måten ikke gi den stimuleringseffekten man er ute etter.
Etter vår mening har artikkelforfatterne pekt på en rekke forhold som det er avgjørende at våre helsemyndigheter tar inn over seg i den bebudede evalueringen av forsøket med KBF.
Litteratur
1. Hagen TP, Iversen T, Moger TA.Risikojustering ved måling av predikert dødelighet etter hjerteinfarkt. Tidsskr Nor Legeforen 2016; 136:423 – 7
2. Asplin M, Fagermoen E. Hvordan sammenlikner vi kvalitet i helsetjenesten?
Tidsskr Nor Legeforen 2015; 135: 1112 - 3.
Artikkelen til Hagen og medarbeidere i Tidsskriftet nr. 5 (1) tar opp et viktig tema: hvordan kan vi bruke harde utfallsmål til å vurdere kvalitet i helsetjenesten. Vi tror det er nyttig at temaet blir behandlet i et norsk faglig forum. Forfatterne diskuterer hvordan man kan justere utfallsmål for forskjeller i pasientsammensetning. I innledningen viser de til at kvalitetsindikatoren 30-dagersoverlevelse etter innleggelse ved sykehus inngår i grunnlaget for kvalitetsbasert finansiering, og skriver at «... det ikke er gjort rede for hvordan overlevelsestallene er risikojustert». Her må vi påpeke at denne indikatoren er meget godt beskrevet i vitenskapelige publikasjoner (2,3) og i en rekke rapporter (4-7) fra Kunnskapssenteret, som nå er en del av Folkehelseinstituttet.
Vi vil også peke på en viktig prinsipiell side ved
risikojustering: den må bare justere for forhold som foreligger ved innleggelsesøyeblikket. Det er helt feil å justere for behandling, f.eks. om pasienten får PCI eller ikke, som Hagen og medarbeidere beskriver. Det er jo nettopp forskjeller i behandling som kan forårsake forskjeller i utfall. Ellers er det mange likhetstrekk mellom metoden i artikkelen og den som Folkehelseinstituttet benytter. Bruk av reseptregisteret er åpenbart nyttig, og viser hvilke muligheter det ligger i å koble de mange registrene som finnes. Men, som forfatterne påpeker, er dette en tung prosess i dagens forskningsregime. Et viktig punkt i måling av kvalitet er attribueringen: hvordan skal utfallene tilordnes sykehus eller foretak? Det vanligste synes å være behandlende sykehus, og dette er etter vårt syn det naturlige valget dersom formålet er sykehusvalg eller lokal kvalitetsforbedring.
Litteratur
1. Hagen TP, Iversen T, Moger TA. Risikojustering ved måling av predikert dødelighet etter hjerteinfarkt. Tidsskr Nor Legeforen 2016; 136:423 – 7
2. Hassani S, Lindman AS, Kristoffersen DT, Tomic O, Helgeland J. 30-Day Survival Probabilities as a Quality Indicator for Norwegian Hospitals: Data Management and Analysis. PLoS One. 2015;10(9):e0136547. Epub 2015/09/10.
3. Kristoffersen DT, Helgeland J, Clench-Aas J, Laake P, Veierod MB. Comparing hospital mortality--how to count does matter for patients hospitalized for acute myocardial infarction (AMI), stroke and hip fracture. BMC health services research. 2012;12:364.
4. Clench-Aas J, Helgeland J, Dimoski T, Gulbrendsen P, Hofoss D, Holmboe O, et al. Methodological development and evaluation of 30-day mortality as quality indicator for Norwegian hospitals. Oslo: Norwegian Knowledge Centre for the Health Services, 2005.
5. Helgeland J, Kristoffersen DT, Hassani S, Lindman AS, Dimoski T, Rygh LH. [30 day survival after admission to Norwegian hospitals in 2010 and 2011]. Oslo: Norwegian Knowledge Centre for the Health Services, 2013.
6. Lindman AS, Hassani S, Kristoffersen DT, Tomic O, Dimoski T, Helgeland J. [30 day survival after admission to Norwegian hospitals for 2013]. Oslo: Norwegian Knowledge Centre for the health Services, 2014.
7. Lindman AS, Kristoffersen DT, Hansen TM, Tomic O, Helgeland J. [The Quality Indicator 30 Day Survival after Admission to Norwegian Hospitals - Results for the Year 2014]. Oslo: Norwegian Knowledge Centre for the Health Services, 2015.
Forfatterne svarer:
Takk til Jon Helgeland og Hanne Narbuvold for kommentarer som vi i hovedsak er enige i. Vi vil likevel legge til to momenter.
Forfatterne gjør for det første et poeng av at en kun skal justere «for forhold som foreligger ved innleggelsesøyeblikket. Det blir helt feil å justere for behandling, for eksempel om pasienten får PCI eller ikke, som Hagen og medarbeidere beskriver». I diskusjonsdelen av vår artikkel konkluderer vi på liknende måte. Vi vil likevel påpeke at belønning av prosedyrebruk er utbredt i kvalitetsbaserte finansieringssystemer i andre land. Ofte er målsettingen da å stimulere til bruk av bestemte prosedyrer.
For det andre mener forfatterne at det er klart dokumentert hvordan risikojusteringen i kvalitetsbasert finansiering i Norge skjer og viser til tidligere og nylige arbeider. Risikojusteringen skjer imidlertid på ulike måter i disse arbeidene og det er fortsatt ikke klart for oss hvilken modell for risikojustering som idag gjelder for kvalitetsbasert finansiering.