A key intention behind the introduction of the GP contract scheme was to promote continuity in the doctor-patient relationship (1). In the context of general practice this is an important quality indicator (2). Establishing continuity in the relationship sets requirements for both parties – the patient must choose to maintain contact with the doctor over time, and the doctor must stay in the same job. The choices made by doctors govern the duration of the GP agreement with the municipality and thus determine whether the RGP scheme will be successful.
On the basis of the Statistics Norway’s living conditions panel, Finnvold and collaborators estimated that an average doctor-patient relationship had a duration of 9.7 years in 2000. In 2003, two years after the introduction of the RGP scheme, the average had fallen to 7.7 years (3). The duration fell because a number of new doctor-patient relationships were established while some long-term relationships were terminated as a result of the reform.
In his summary of the research-based evaluation of the RGP reform, Sandvik (4) ascertained that «in parallel with the RGP scheme, the density of doctors has improved considerably and stability is high among the RGPs. However, some municipalities are still facing problems in terms of scarcity of doctors». Since this evaluation we have found no studies that have investigated whether the objectives related to establishment of continuity in the doctor-patient relationship have been achieved.
This study is based on the population of GP contracts signed in the course of the first 13 years that this scheme has been in effect. We ask:
How is the gender and age composition of the population of RGPs changing?
How long do the GP contracts last, and how does this duration vary in accordance with the doctors’ age and gender, the size of the municipalities and the list size?
How many of the doctors who terminate a GP contract later establish a new one?
Material and method
The investigation included all of the 7 359 GP contracts signed by a municipality and a doctor during the period from 1 May 2001 to 1 May 2014 (the study period). GP contracts signed in the pilot municipalities of Lillehammer, Åsnes, Trondheim and Tromsø before 1 May 2001 were excluded (n = 178).
In addition to these 7 359 GP contracts we analyse lists that have been in effect for a shorter or longer period and are not associated with a named doctor with a GP contract, i.e. lists served by locum doctors hired by the municipality (n = 1 091).
The data material has been retrieved from the RGP registry, which is administered by HELFO. The municipalities are responsible for reporting information on new GP contracts and amendments to existing contracts to HELFO. This material has been supplied by the Directorate of Health upon application.
Each of the GP contracts included in the analysis was registered with the following characteristics: number of inhabitants in the municipality as of 1 January 2014, the doctor’s gender and year of birth, start date and end date of the GP contract (if terminated during the study period) and the last registration of the number of persons on the doctor’s list (list size). Missing data on list size was due to non-registration in HELFO’s database (our data source). We have no information on the reasons for this failure to register some doctors’ list size. With regard to the lists that have been without any doctor during the study period, the analysis is based on the number of inhabitants in the municipality as of 1 January 2014 and on the time that the list has remained vacant.
Statistical analyses
The data material was analysed with the aid of measures for central tendency and dispersion (average, median and confidence interval), frequency tables and cross tabulations. The turnover was measured as the proportion of GP contracts terminated in the course one year as a percentage of all active GP contracts at the end of the year.
The duration of a GP contract is measured as the time that has elapsed between its signature and its termination. This type of data can be analysed with the aid of survival analysis, for which Kaplan-Meier survival curves and Cox’s regression model for proportional hazards are key methods (5).
We have used Kaplan-Meier survival curves to show how the duration of GP contracts changes over time. The curves show the proportion of the GP contracts that remain in effect (have survived) after a specified period of time.
Furthermore, we have implemented a Cox regression model for proportional hazards, in which the duration of the GP contract (i.e. the time elapsing from the signature of the GP contract to its termination or to the end of the study period) is the dependent variable. The analysis includes a dichotomous censoring variable which equals 1 if the GP contract was terminated during the study period and 0 if the GP contract remained in effect at the censoring date (1 May 2014). The analysis included the doctor’s gender, the doctor’s age at the time of signature of the contract, the size of the municipality and the list size as independent variables.
The independent variables are included in the regression analysis as dummy variables. Age at entry into the contracts was grouped into five equally sized groups. List size was similarly grouped into three equally sized groups. As regards the size of the municipalities, we distinguish between small (fewer than 5 000 inhabitants), medium-sized (5 000 – 19 999 inhabitants) and large municipalities (20 000 inhabitants or more), in line with Statistics Norway’s categorisation of municipalities by size (6). A key statistical measure in our analysis is the estimated relative likelihood (hazard ratio) of survival of a GP contract when comparing RGPs who have different values on one of the independent variables.
The data analyses were undertaken with the aid of the IBM SPSS Statistics version 22 software package.
Results
Table 1 summarises characteristics of GP contracts signed during the first 13 years that this scheme has existed (i.e. the period from 1 May 2001 until 1 May 2014). On 1 May 2001, a total of 3 393 GP contracts were entered into: altogether 2 418 by men (71.3 %) and 975 by women (28.7 %). On 1 May 2014, a total of 4 387 contracts were in effect: altogether 2 648 with men (60.5 %) and 1 730 with women (39.5 %). Thus, from 2001 to 2014, the number of active GP contracts rose by 29 % (9.5 % for men and 77 % for women).
Table 1
Characteristics of the RGP and the list of those who signed a GP contract during the period 1 May 2001 – 1 May 2014 (N = 7 359)
| Characteristic |
Number |
(%) |
| Gender |
|
|
| Man |
4 674 |
(63.5) |
| Woman |
2 685 |
(36.5) |
| Total |
7 359 |
(100.0) |
| Age at signature (years) | ||
| ≤ 31 |
1 440 |
(19.6) |
| 32 – 35 |
1 333 |
(18.1) |
| 36 – 42 |
1 599 |
(21.7) |
| 43 – 49 |
1 498 |
(20.4) |
| ≥ 50 years |
1 489 |
(20.2) |
| Total |
7 359 |
(100.0) |
| Contract municipality (number of inhabitants) | ||
| < 2 000 |
426 |
(5.8) |
| 2 000 – 4 999 |
1 072 |
(14.6) |
| 5 000 – 9 999 |
1 028 |
(14.0) |
| 10 000 – 19 999 |
1 259 |
(17.1) |
| 20 000 – 49 999 |
1 499 |
(20.4) |
| ≥ 50 000 |
2 075 |
(28.2) |
| Total |
7 359 |
(100.0) |
| Last recorded list size (number of patients) | ||
| < 900 |
2 422 |
(33.4) |
| 900 – 1 200 |
2 437 |
(33.6) |
| > 1 200 |
2 398 |
(33.0) |
| Total |
7 257 |
(100.0) |
The average age of doctors with a GP contract amounted to 46 years as of 1 May 2001 (men = 47.4 years; women = 42.5 years), compared to 47.7 years on 1 May 2014 (men = 49.7 years; women = 44.7 years).
Figures 1 and 2 show the annual accession and attrition of GP contracts signed by men and women respectively in the period from 1 May 2001 until 31 December 2013. While the difference between accession and attrition has remained nearly constant on the part of the men, it has increased among women.
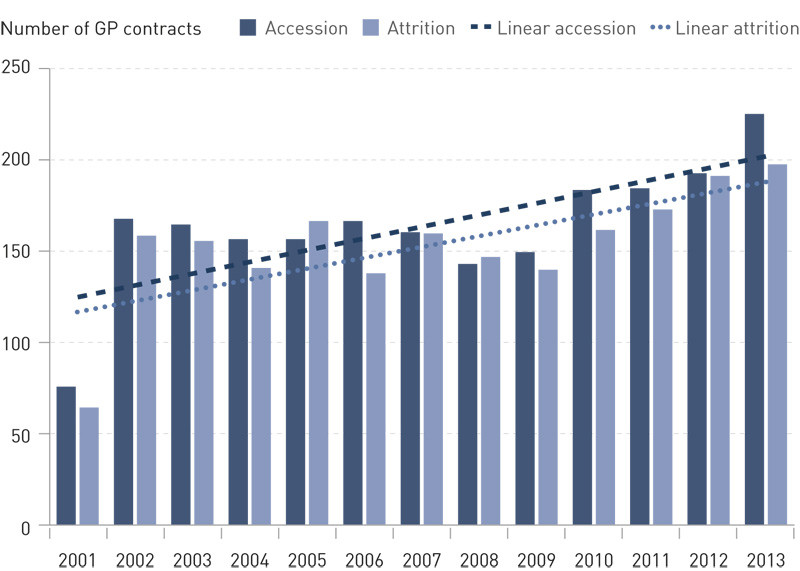
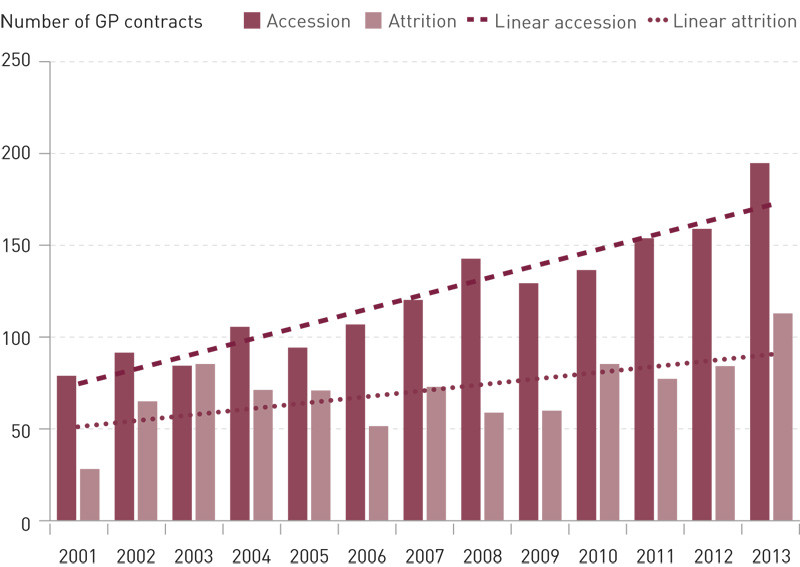
The doctor’s age at the start of a GP contract declined slightly in the period after 1 May 2001 (from 38 years in 2001 to 35.9 years in 2013).
Duration of GP contracts
Figure 3 shows the duration of GP contracts in different groups of municipalities. Median duration nationwide amounted to 5.91 years. The figure shows a clear association between the duration of GP contracts and size of the municipality.
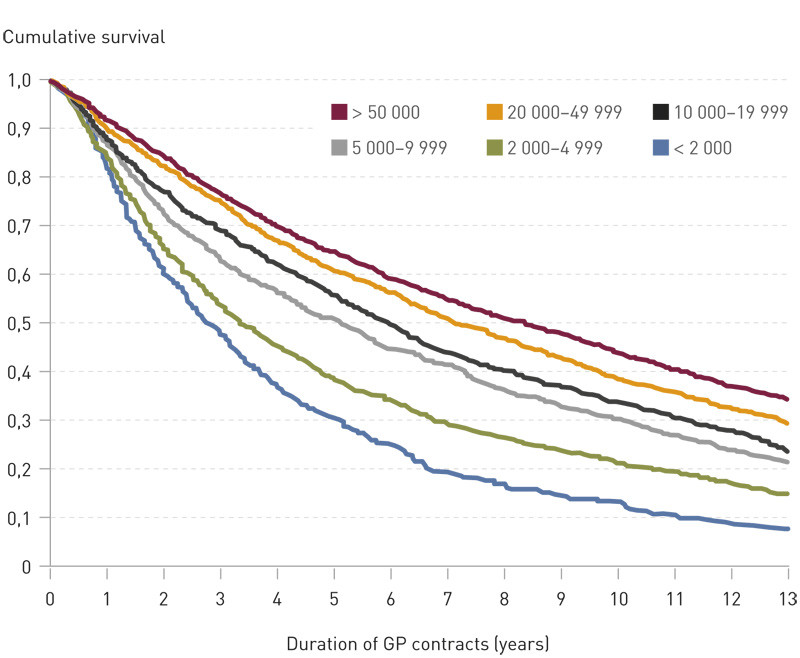
The median duration varied from 2.75 years in municipalities with fewer than 2 000 inhabitants and 8.37 years in municipalities with 50 000 or more inhabitants.
Nationwide, altogether 25 % of all GP contracts signed on 1 May 2001 remained in effect after 13 years. In municipalities with fewer than 2 000 inhabitants the corresponding proportion amounted to 8 %, while in municipalities with 50 000 or more inhabitants it was as high as 34 %.
What affects duration?
Table 2 shows the association between the duration of a GP contract and demographic variables. The table shows that the risk that a GP contract will be terminated (the hazard ratio) is significantly reduced if it has been signed by a woman doctor and also with rising age of the doctor at the time of signing, with increasing size of the municipality and increasing list size.
Table 2
Hazard ratio for termination of GP contracts. Cox’s regression analysis (N = 7 359)
| Independent variable |
Hazard ratio (95 % CI) |
P-value |
| Man |
1.00 |
|
| Woman |
0.83 (0.76 – 0.90) |
< 0.001 |
| ≤ 31 years |
1.00 |
|
| 32 – 35 years |
0.83 (0.73 – 0.94) |
0.003 |
| 36 – 42 years |
0.65 (0.58 – 0.74) |
< 0.001 |
| 43 – 49 years |
0.43 (0.37 – 0.48) |
< 0.001 |
| ≥ 50 years |
0.88 (0.79 – 0.98) |
0.021 |
| Municipality < 5 000 inhabitants |
1.00 |
|
| Municipality 5 000 – 19 999 inhabitants |
0.72 (0.66 – 0.80) |
< 0.001 |
| Municipality ≥ 20 000 inhabitants |
0.58 (0.52 – 0.64) |
< 0.001 |
| List size < 900 patients |
1.00 |
|
| List size 900 – 1 200 patients |
0.64 (0.59 – 0.70) |
< 0.001 |
| List size > 1 200 patients |
0.37 (0.33 – 0.41) |
< 0.001 |
The association between age at the time of signing and duration of the GP contract is non-linear. This is mainly due to the fact that many older doctors signed a GP contract when this scheme was introduced.
Age at termination
Of all the GP contracts that were terminated during the study period, altogether 11.2 % were terminated by doctors who were aged 67 years or older. This proportion varied with the size of the municipality; it was lowest in municipalities with fewer than 5 000 inhabitants (5 %) and highest in municipalities with 20 000 or more inhabitants (16.2 %).
In municipalities with fewer than 5 000 inhabitants, one-half of the GP contracts had been terminated when the doctor was aged 40 years or younger. The equivalent figure from municipalities with 20 000 inhabitants or more was aged 51 years or younger.
Turnover
The turnover rate has increased from 6.4 % in 2002 to 7.3 % in 2013. During the entire period, this rate has been somewhat higher among men than among women, and it has increased for both genders. For men, the proportion amounted to 6.4 % in 2002 and 7.7 % in 2013, for women it amounted to 6.2 % in 2002 and 6.8 % in 2013. In 2002, the number of GP contracts signed per month varied from 6 to 41, and in 2013 the monthly figure ranged from 16 to 79.
Termination of one contract and establishment of a new one
The 7 359 GP contracts encompassed by the study period were signed by a total of 6 476 different doctors, meaning an average of 1.14 GP contracts per doctor. Table 3 shows that 5 704 (88.1 %) of the doctors established only a single GP contract during the study period. The majority (1 985 doctors, 93.3 %) of the 2 098 doctors who no longer had a GP contract as of 1 May 2014 had signed only one contract during the study period. Altogether 333 doctors (15.9 % of those who had no contract as of 1 May 2014) were aged 67 years or older when the contract was terminated.
Table 3
Doctors by the number of GP contracts in the study period and by whether they still remained RGPs as of 1 May 2014
| Number of doctors |
|||||||||
| Number of GP contracts signed per doctor |
Total in the study period |
With a GP contract as of 1 May 2014 |
With no GP contract as of 1 May 2014 |
||||||
| Number |
(%) |
Number |
(%) |
Number |
(%) |
||||
| One |
5 704 |
(88.1) |
3 746 |
(85.5) |
1 958 |
(93.3) |
|||
| Two |
679 |
(10.5) |
553 |
(11.7) |
126 |
(6.0) |
|||
| Three |
80 |
(1.2) |
70 |
(1.6) |
10 |
(0.5) |
|||
| More than three |
13 |
(0.2) |
9 |
(0.2) |
4 |
(0.2) |
|||
| Total |
6 476 |
(100.0) |
4 378 |
(100.0) |
2 098 |
(100.0) |
|||
Among those 11.9 % who terminated a GP contract and established a new one in the course of the study period, a little more than one-half (56.1 %) established a new contract in a larger municipality. Somewhat less than one-third (29.8 %) established a new contract in a smaller municipality. The remaining (14.1 %) signed a new GP contract in the same municipality after an intervening period.
Lists without doctors
As regards those 1 091 lists that for shorter or longer periods had been left with no link to a named doctor with a GP contract, Table 4 shows that such lists could be found in all groups of municipalities during the study period. In 2001, there was a relatively greater proportion of such lists with no doctor in the larger municipalities than in the small ones, which is an indication of problems related to the initial phase of the RGP reform, rather than general recruitment problems.
Table 4
Lists with no doctor in the period 1 May 2001 – 1 May 2014. Total number and median duration without any doctor by different groups of municipalities
| Group of municipalities |
Number of lists with no doctor (%) |
Median number of months with no doctor |
|
| < 2 000 inhabitants |
164 |
(15) |
12.0 |
| 2 000 – 4 999 inhabitants |
292 |
(27) |
11.0 |
| 5 000 – 9 999 inhabitants |
218 |
(20) |
9.0 |
| 10 000 – 19 999 inhabitants |
190 |
(19) |
6.0 |
| 20 000 – 49 999 inhabitants |
146 |
(13) |
4.0 |
| ≥ 50 000 inhabitants |
81 |
(7) |
3.0 |
| Total |
1 091 |
(100) |
7.9 |
A large proportion of the lists with no doctor was found in municipalities with fewer than 5 000 inhabitants (42 %). Table 4 shows that the lists were left without any permanent doctor for significantly longer in small municipalities when compared to larger ones.
Discussion
The analysis reveals major variations in the duration of the GP contracts, showing that the duration depends on the doctor’s gender and age at signature, the list size and the number of inhabitants in the municipality. In the study period, the median duration of a GP contract was more than three times longer in municipalities with 50 000 inhabitants or more, when compared to municipalities with fewer than 2 000 inhabitants. Our data show that lists that have not been linked to a named doctor and thus have been served by one or more locum doctors over a shorter or longer period are mainly found in the small municipalities. This indicates that the challenges associated with instability in the provision of RGP services in the small municipalities are greater than might be assumed from Figure 3.
If we assume that continuity in the doctor-patient relationship makes for better quality of general practice, the results indicate that patients in small municipalities in general are provided with services of a quality that is inferior to the services provided to patients in larger municipalities. When the doctor and the patient meet repeatedly over a long period of time, trust can be established. The same applies to the collaborative relationship between the RGP and other service providers in the municipality.
The RGP can accumulate comprehensive knowledge about the patient’s overall life situation, which may be an advantage for other medical assessments, and also establish a network of other service providers, which may be an advantage for provision of treatment. However, the goal of continuity in the RGP scheme has not been operationalised in terms of a specific duration that a doctor-patient relationship should have in order to be regarded as having continuity.
The assertion of a consistent and significant association between continuity in the doctor-patient relationship on the one hand and patient satisfaction on the other is backed by solid documentation (7). In the DIFI survey in 2015, the average score for satisfaction with RGPs amounted to 75 in the population as a whole (on a scale from 0 to 100). In municipalities with fewer than 5 000 inhabitants the average score amounted to 73, while reaching 74 in municipalities with more than 110 000 inhabitants (8). In other words, those who are least satisfied with the RGP service live in the very smallest and very largest municipalities. The differences are minor, however, leading us to assume that factors other than continuity in the doctor-patient relationship may also have an effect on patient satisfaction.
The average age of doctors with a GP contract was higher in 2014 than in 2001 and had increased for men and women alike. In 2014, the majority of the RGPs were still men, even though the proportion of women had increased during the study period. According to figures from the Norwegian Medical Association (9), the proportion of women among doctors aged younger than 70 years increased by 42 % from 2002 to 2014. In comparison, our figures show that the proportion of women among the RGPs increased by no more than 33 % over the same period. In other words, the job of RGP appears to be fundamentally less attractive to women than to men. However, the risk of termination of a GP contract is significantly lower for women doctors than for men. This indicates that when women have made the choice to become an RGP, they are somewhat more stable in the position than men.
Increased list size is also associated with increased contract duration. The main model in the RGP scheme is based on private enterprise, in which earnings are essentially dependent on the size of the individual doctor’s patient population. Having a large list tends to be a precondition for the ability to establish and operate a financially sound private practice. We know that there is a considerable amount of self-selection of doctors to different business models (10), but there is also reason to assume that the choice of private enterprise is so encompassing that it serves as a stabilising factor in itself. Halvorsen and collaborators (11) as well as Holte and collaborators (12) have shown that the main salary model based on private practice is more compatible with the preferences of RGPs in populous municipalities, while RGPs in smaller municipalities tend to prefer a fixed salary.
Most likely, the duration of the GP contracts is also influenced by factors other than those we have controlled for. There is reason to assume that the burden of on-call duty may play a role. On-call duty is arduous. Even though on-call duty is mandatory for RGPs, their participation, and thus probably also the workload, is greater among RGPs in rural areas (13). Small lists in small municipalities may free up more doctors to share the on-call duty. Moreover, small lists are likely to provide for working conditions that include space for competence development and other tasks in addition to clinical work with patients. Autonomy with regard to the use of time is reflected in high job satisfaction (14). Having time to increase qualifications and provide high-quality treatment to patients are other key factors for the doctors’ well-being (15).
The turnover among RGPs has increased during the study period, which indicates that the challenges that recruitment to the scheme is facing have increased somewhat. In 2013, the turnover rate amounted to 7.3 %. This is lower than among municipal nurses, for example, where this rate amounted to an average of 13 % during the period 2009 – 12 (16).
Most of the doctors who terminate a GP contract while still of working age go to jobs other than that of RGP. This is an indication of a weak identity as RGP among those who leave the profession. Our data indicate that it is difficult to maintain professional satisfaction in the job as RGP over time, and perhaps in the smaller municipalities in particular. However, this issue has not been widely studied. An alternative interpretation could be that the job of RGP in a small municipality is regarded as a good first job while pondering one’s further career path. It tends to be simpler, and not least cheaper, to establish a contract in a rural area than in a city.
Conclusion
If we assume that continuity in the doctor-patient relationship provides for better quality in general practice, the results indicate that patients in small municipalities are generally offered a lower-quality service than patients in large municipalities. In the small municipalities, GP contracts have a significantly shorter duration than in the large ones. In addition, many small municipalities face challenges in terms of long periods of time when a list is left without any permanent doctor. There may be reason to believe that a greater number of women in the RGP population would result in a longer duration for GP contracts.
MAIN MESSAGE
The median duration of a GP contract was more than three times as long in municipalities with 50 000 inhabitants or more than in municipalities having fewer than 2 000 inhabitants.
The duration of the GP contracts varied in proportion to the size of the municipality in question, the doctor’s gender, the doctor’s age at entry into the contract and the size of the list.
Most of the doctors who terminated a contract did not sign a new one.
- 2.
Hjortdahl P. Continuity of care in general practice. A study related to ideology and reality of continuity of care in Norwegian general practice. Oslo: Universitetet i Oslo, 1992.
- 3.
Finnvold JE, Svalund J, Paulsen B. Etter innføring av fastlegeordning – brukervurderinger av allmennlegetjenesten. Rapport nr. 1. Oslo: Statistisk sentralbyrå, 2005.
- 4.
Sandvik H. Evaluering av fastlegereformen 2001 – 2005. Sammenfatning og analyse av evalueringens delprosjekt. Oslo: Norges forskningsråd, 2006.
- 5.
Kleinbaum DG, Klein M. Survival analysis. A Self-Learing Text. 3. utg. New York: Springer, 2012.
- 6.
Langørgen A, Aaberge R. Gruppering av kommuner etter folkemengde og økonomiske rammebetingelser 2008. Rapport nr. 8. Oslo: Statistisk sentralbyrå, 2011.
- 8.
Innbyggerundersøkelsen. (30.6.2015).
- 9.
Den norske legeforening. Medlemsstatistikk. http://legeforeningen.no/Emner/Andre-emner/Legestatistikk/Medlemsstatistikk/Den-norske-legeforening/ (22.12.2014).
- 10.
Grytten J, Skau I, Sørensen R et al. Hva påvirker allmennlegenes kontraktsvalg og flytteplaner? Tidsskr Nor Lægeforen 2000; 120: 3134 – 9. [PubMed]
- 13.
Sandvik H, Hunskår S, Diaz E. Hvilke fastleger deltar i legevakt? Tidsskr Nor Legeforen 2012; 132: 2277 – 80. [PubMed]
- 14.
Nylenna M, Aasland OG. Jobbtilfredshet blant norske leger. Tidsskr Nor Lægeforen 2010; 130: 1028 – 31. [PubMed]
- 15.
Friedberg MW, Chen PG, Van Busum KR et al. Factors Affecting Physician Professional Satisfaction and Their Implications for Patient Care, Health Systems, and Health Policy. RR-439-AMA. Rand Corporation, 2013. www.rand.org/pubs/research_reports/RR439.html (22.10.2015).
- 16.
Rekrutteringsbehov i kommunesektoren fram mot 2022. Oslo: Kommunesektorens organisasjon, 2012.