Weight-loss surgery (bariatric surgery) has become more common, and around 3 000 individuals undergo such surgery in Norway each year (1, 2). Quality of life and obesity-related health problems improve significantly after pronounced weight loss (3), but many patients also experience new physical and psychological impairments due to large amounts of excess skin.
This review considers indications for treatment, choice of post-bariatric plastic surgery procedures, results and complications as well as the treatment options that are available.
Method
A literature search in PubMed on 19 November 2014 using the search string «bariatric surgery» AND «plastic surgery» generated 178 articles. Of these, 141 English and Scandinavian language full-text articles with abstracts were systematically reviewed by the first author. Articles based on case reports or surgical methods were excluded, as were commentary articles.
All abstracts were read thoroughly by the first author, and the most relevant were selected and reviewed by the first and last authors. The final selection comprised 13 articles (4) – (16). Articles from the reference lists and the authors’ own reference libraries, as well as the authors’ clinical experience, also form part of the evidence base.
Excess skin after bariatric surgery
The most common bariatric procedure in Norway today is the gastric bypass. Although average weight loss 1 – 2 years after a gastric bypass is approximately 30 % (35 – 45 kg), most patients will still have a body mass index (BMI) ≥ 30 kg/m² after successful treatment (17, 18).
Skin that has been stretched over long periods shows reduced elasticity (19), and massive weight loss is often accompanied by a corresponding amount of excess skin. Many patients who undergo bariatric surgery develop such severe physical impairments that they require corrective plastic surgery (4, 5, 20). Indeed, most patients (70 – 90 %) express a wish for plastic surgery after weight-loss surgery (5, 6).
Indications and contraindications
Excess skin can cause various complaints, including intertriginous ulcerations and infections of the skin folds and navel, unpleasant odours, back and neck problems, aches and pains associated with work, exercise and intimacy, skin lesions due to chafing, difficulty finding clothes that fit and disparity between appearance and age (5). The abdominal area causes the most problems, followed by the chest and the thighs (5, 6). Excess skin can therefore become a new source of stigma, social isolation and reduced quality of life for these patients (7, 21).
The risk of complications associated with body contouring surgery after pronounced post-bariatric weight loss varies depending on factors such as the size and scope of the procedure, nutritional status, smoking and the degree of overweight. Medical comorbidities are not a contraindication for plastic surgery, but limit the choice of procedures due to a greater risk of complications and suboptimal results (8).
Tobacco smoking is associated with a 2 – 3 times greater risk of post-operative wound complications, infections and delayed healing (22). Preoperative smoking cessation can halve this risk, and the risk is lowest after at least four weeks of abstention from smoking (22). Smoking cessation is therefore an absolute requirement before any type of body contouring surgery (22) – (24).
Prior to plastic surgery, the patient must have good nutritional status, haemoglobin levels > 10 g/100 ml (8, 23) and have a satisfactory level of physical fitness (8, 24). Any gastrointestinal pain after weight-loss surgery should be investigated and treated prior to evaluation for plastic surgery, as it may otherwise be difficult to distinguish sequelae of abdominoplasty from pain in the digestive system. Patients with previous deep vein thrombosis or lymphoedema should be advised about the risk of relapse, and adequate thromboprophylaxis must be ensured (8, 25).
Plastic surgeons often set the upper BMI limit for body contouring surgery at 30 kg/m² due to fear of complications and because removal of skin is easier if there is not much additional fat (9, 26). A number of small retrospective observational studies support this view. Considerable evidence suggests that the incidence of serious and less serious complications is roughly twice as high in those with BMI ≥ 30 kg/m² compared to those with BMI < 30 kg/m² (26) – (28).
Results from two major prospective registry studies failed to confirm preoperative BMI as an independent predictor of surgical complications (24, 29). However, the risk of complications did increase with increasing BMI (OR 1.06; 95 % CI 1.0 – 1.1) (24). Overall, we do not believe there are strong scientific grounds for using BMI alone as a tool to assess indication for surgery. If BMI ≥ 30 kg/m² is used as an exclusion criterion for surgical removal of loose skin after weight loss, more than half of patients in need of such treatment could be excluded (17).
Body contouring surgery or local removal of skin?
In our experience, body contouring surgery is most likely to produce a successful cosmetic outcome and few adverse effects in a «healthy» non-smoking patient with BMI < 28 kg/m². Such patients have a normal body fat distribution, but they have excess skin that hangs in folds, which can be a challenge when contouring (Figure 1, top two images).
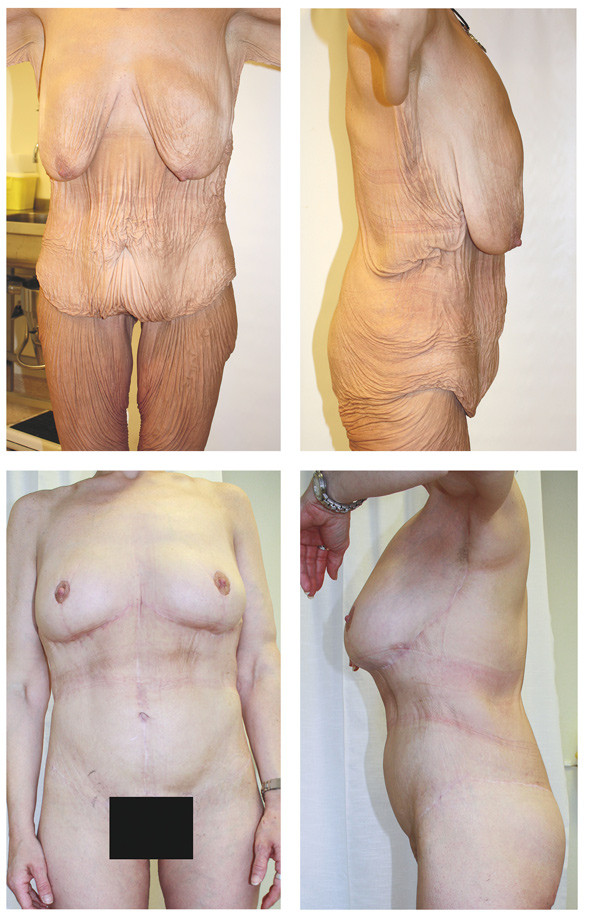
In such cases, treatment usually begins with surgery on the lower body – abdominoplasty, outer thighs, flanks and buttocks. The next session focuses on the upper body – chest, arms and upper back. Lastly, the thighs are treated in a separate operation in which minor corrections can also be made to previous procedures. We recommend up to three months between operations so that patients can recover before the next intervention.
As with any surgery, there is a learning curve – with increased experience the operating time is reduced, there are fewer complications and more procedures can be performed in a single session (26) – (29).
In our experience, local removal of excess skin does not meet patients’ expectations and treatment of one area can quickly lead to further treatment of adjacent areas. Body contouring surgery after significant weight loss involves a series of procedures to reduce or remove excess skin on the abdomen and hips, chest and upper arms as well as the buttocks and thighs. The interventions are based on fundamental plastic surgery techniques, but have a distinctive character due to the extent of the resections, which increases both surgery duration and risk (10, 30).
Time-consuming major surgery in the form of whole-body reshaping increases the risk of blood loss, hypothermia, infection, fat necrosis and wound complications (11, 30, 31). This has resulted in an increasing tendency to split up procedures; several interventions within a single body area might be combined, while surgery on other areas is left to a later date (32, 33). Treatment is tailored to each patient according to his or her needs, health status and expectations.
Common plastic surgery procedures
Table 1 provides an overview of plastic surgery procedures and indications for patients with massive weight loss after bariatric surgery.
Table 1
Overview of plastic surgery procedures and common indications for patients with massive weight loss after bariatric surgery¹
| Localisation |
Procedure |
Indication |
| Lower body |
Abdominoplasty |
Physical strain, intertriginous alterations/abnormalities. Difficulty finding clothes that fit |
| Belt lipectomy/lower body lift |
Problems with several or all of abdomen, mons pubis, hips and buttocks |
|
| Panniculectomy |
Physical strain. Extensive intertriginous abnormalities and/or lipoedema² |
|
| Upper body |
Breast reduction/breast lift |
Back and neck pain. Eczema or intertrigo. Appearance inconsistent with age, highly troublesome excess skin |
| Axilloplasty |
Appearance inconsistent with age, highly troublesome excess skin |
|
| Back lift |
Appearance inconsistent with age, highly troublesome excess skin |
|
| Extremities |
Brachioplasty |
Physical strain, difficulties with clothing. Appearance inconsistent with age, highly troublesome excess skin |
| Thighplasty |
Physical strain. Rubbing and chafing, difficulties with clothing. Appearance inconsistent with age, highly troublesome excess skin |
|
| Gluteal augmentation |
Appearance inconsistent with age, troublesome excess skin and/or pain and difficulties with hygiene |
|
| Face |
Face/neck lift |
Appearance inconsistent with age, highly troublesome excess skin |
| [i] | ||
[i] ¹ Not all interventions are available as part of the current public health provision, and they are considered for each patient on the basis of objective need.
² Lipoedema is the accumulation of fat, mainly in the lower extremities, hips, thighs and mons pubis. It is distinguished from lymphoedema on the basis of fat accumulation and characteristic non-pitting appearance.
Abdominoplasty and lower body lift (belt lipectomy)
The most common post-bariatric surgical procedure is abdominoplasty (4) – (6, 20), but patients who have lost 35 – 45 kg or more will require more extensive surgery. In such cases, we recommend a lower body lift or belt lipectomy, in which the lower body is treated front and back in its entirety. The flanks, sides and backs of the thighs, and the buttocks are treated at the same time as the stomach. A sagging mons veneris (mons pubis) can be reduced and lifted. In some cases, a vertical incision can be made in the centre of the abdomen, or a standard bikini line incision combined with a vertical incision, so that the scar resembles an inverted «T».
Omitting any of these interventions may produce a poor functional and cosmetic outcome (Figure 2). A circumferential lower body lift takes 3 – 5 hours and requires 1 – 4 days of hospitalisation. The recovery period is normally 4 – 6 weeks providing there are no complications (26, 27).
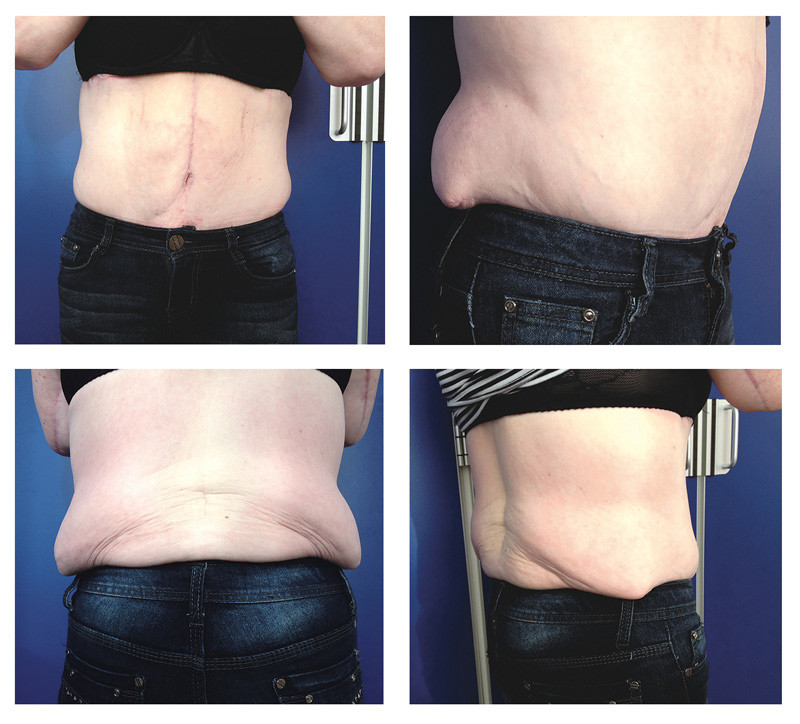
Panniculectomy – removal of abdominal pannus (fat apron)
For patients who are not suitable for body contouring surgery due to significant obesity, panniculectomy can be considered on the basis of medical indication. These patients usually have a large and heavy fat apron, which impedes activity and can result in long-lasting fungal infections (Figure 3, top) or serious soft tissue infections such as cellulitis or necrotising fasciitis.
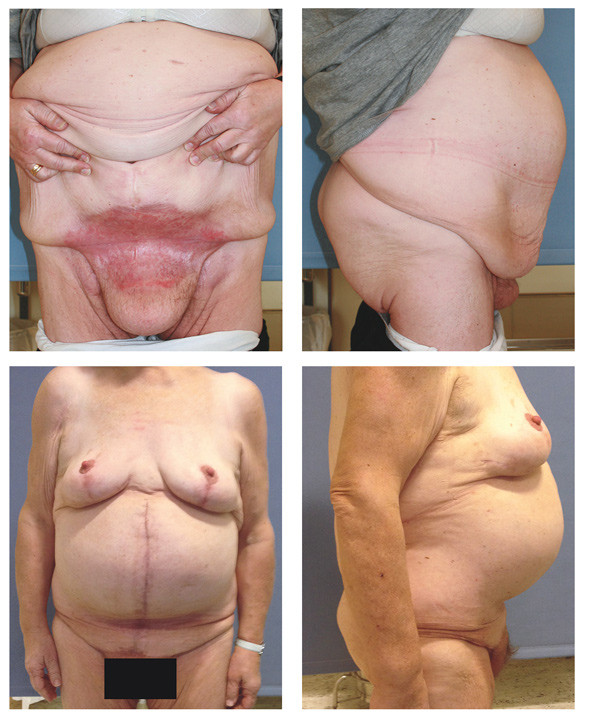
The risks of surgery have been described as very high for these patients, but there is little evidence available regarding outcomes and frequency of complications (12, 22, 34). We have performed panniculectomies with resections of 7 – 20 kg without major complications. However, our patient sample is too small for us to draw any firm conclusions about the frequency of complications in this group, who are among our most grateful patients despite suboptimal cosmetic outcomes (Figure 3, bottom).
Upper body
The upper body is treated after surgery on the lower body. Loose skin on arms, axillae and chest, upper abdomen or back may be isolated to one area or affect the entire upper body.
Treatment consists of breast reduction or breast lift (mastopexy). In women, skin flaps from the surrounding area can be used for breast reconstruction (mammoplasty) (13). The axillae can be treated at the same time as the arms or chest with axilloplasty. Greater emphasis is often placed on treatment of the chest and arms, which can result in the axilla receiving insufficient attention (35). Our experience suggests that best results are achieved when the arms, axillae and chest are treated in the same session.
Thighs
Thighplasty is performed in patients with pronounced physical impairments due to excess medial skin, which can extend all the way down to the knees. Correcting this requires removal of skin and adipose tissue vertically in order to reduce circumferential excess skin (Figure 1). This entails a long and sometimes unsightly vertical scar from the groin to below the knee. The surgery takes 1.5 – 3 hours.
Results and complications
Relatively little is known about the outcomes of plastic surgery after pronounced weight reduction, but several centres report good results in the form of high levels of patient satisfaction, with improved quality of life and functional status (11, 14, 15, 36). Modaressi and co-workers showed that patients who had undergone body contouring surgery after a gastric bypass had significantly better health-related quality of life up to eight years after the bariatric surgery than those who had not undergone plastic surgery (11).
In addition to intraoperative complications, such as bleeding, infection and seroma, complications such as wound dehiscence, fat necrosis and skin necrosis occur more often in those who have undergone weight-loss surgery than in other patients (12, 24). Lymphoedema caused by prolonged obesity can become apparent after weight loss, and thighplasty can accentuate or exacerbate the condition (16). Wound dehiscence occurs frequently and should generally be treated conservatively (24). Seroma formation occurs in 4 – 18 % of patients and correlates with wound surface area and amount of skin removed (37).
To ensure a good working relationship between patient and surgeon, the patient must be thoroughly informed about the procedures and risk of complications, and the surgeon must understand the patient’s expectations. The patient must appreciate that their skin has sustained irreversible damage after being put under great strain and that visible scars will replace the excess skin that is removed. Tightened skin will stretch over time, giving rise to new excess skin. The aim is for there to be an improvement on the starting point, and a reduction in physical ailments.
Treatment provision by the Southern and Eastern Norway Regional Health Authority
Responding to the demand, in 2009 the Southern and Eastern Norway Regional Health Authority supported the establishment of a competency centre for post-bariatric surgery in the Department of Plastic Surgery at Telemark Hospital, in collaboration with the Morbid Obesity Center at Vestfold Hospital Trust.
It was initially estimated that each patient would require an average of two surgical procedures, but experience shows the actual number to be far higher. When several surgeons work together, 4 – 5 interventions can be combined in a single operation. We find that this is both efficient and beneficial for the patient, who thereby avoids unnecessary waiting and repeated periods of convalescence.
The waiting list for post-bariatric plastic surgery at Telemark Hospital as per November 2014 exceeded 300 patients, with a similar number awaiting assessment. Surgical capacity varies from between 100 to 200 operations per year. Most interventions are major and resource-intensive. In our experience, body contouring surgery (abdominoplasty, upper body and thighs) entails a total surgical time of at least nine hours per patient, spread over 3 – 5 operations.
Discussion
In this review, body contouring surgery is described principally from a plastic surgery perspective. This does not necessarily reflect patients’ needs or wishes.
A review of the literature reveals a modest knowledge base with regard to treatment indications, choice of plastic surgery procedures(s) and long-term outcomes. Differences in study designs, surgical methods, endpoints, indications and treatment criteria make it difficult to compare studies. There is a particular need for good quality studies evaluating the outcomes of treating patients with BMI ≥ 30 kg/m² who have achieved their target weight loss after bariatric surgery, but who are nevertheless often refused plastic surgery today.
Postoperative wound complications occur somewhat more frequently after post-bariatric surgery, but our experience to date indicates that customised interventions can give relatively satisfactory results, although little is known about long-term outcomes. High quality information and realistic patient expectations are fundamental to a good treatment course.
This patient group is large and probably increasing in number. Patient registries should therefore provide more objective information on the need for and outcomes of treatment. In this article, we have provided an overview of current knowledge of post-bariatric plastic surgery in general and our clinical experience in the Southern and Eastern Norway Regional Health Authority (Telemark/Vestfold) over five years. We hope this will contribute to an open discussion of future care in Norway.
Conclusion
Massive weight loss after bariatric surgery often creates a need for plastic surgery, and correctly executed procedures (often many) for appropriate indications can improve quality of life (7, 11, 14, 15, 36).
Demand for post-bariatric surgery is high, and in our experience exceeds supply. This patient population deserves a thorough survey (through registry studies, for example) and evaluation of the pros and cons of post-bariatric plastic surgery over the long-term, not least to inform decisions on future prioritisation and treatment provision.
MAIN MESSAGE
The number of patients with serious impairments related to excess skin following bariatric surgery and massive weight loss is increasing
In our experience, plastic surgery can significantly reduce these impairments
However, the evidence base with respect to indications for treatment, methods, results and complications is inadequate
There is a particular need for a thorough survey and evaluation of treatment options for the many patients with BMI ≥ 30 kg/m², who are often denied plastic surgery at present
- 2.
Mala T, Kristinsson J. Akutt inneklemming av tarm etter gastrisk bypass for sykelig fedme. Tidsskr Nor Legeforen 2013; 133: 640 – 4. [PubMed]
- 18.
Aasheim ET, Mala T, Søvik TT et al. Kirurgisk behandling av sykelig fedme. Tidsskr Nor Lægeforen 2007; 127: 38 – 42. [PubMed]
- 24.
Fischer JP, Wes AM, Serletti JM et al. Complications in body contouring procedures: an analysis of 1797 patients from the 2005 to 2010 American College of Surgeons National Surgical Quality Improvement Program databases. Plast Reconstr Surg 2013; 132: 1411 – 20. [PubMed]