Malaria is one of the greatest health problems in the world, with an estimated 207 million cases in 2012 (1). The number of deaths is uncertain owing to inadequate diagnosis and reporting, but has been estimated at between 473 000 and 1.2 million per year. More than 80 % of these occur in sub-Saharan Africa (1, 2).
The European Centre for Disease Control and Prevention (ECDC) registered 5 482 cases of malaria in Europe in 2011 (3). The patients were mainly infected in sub-Saharan Africa and south-east Asia. Imported malaria is most frequently due to the potentially malignant Plasmodium falciparum, and according to figures from the global surveillance system for travel-related infectious diseases (GeoSentinel), falciparum malaria accounted for 5 % of 17 228 cases of travel-related disease in 2009 (4). Infection in Europe is highly unusual in modern times, but 61 cases of vivax malaria contracted in Greece were reported in 2011 (3).
During the period 2004 – 2013, 28 – 88 cases of malaria were reported annually in Norway to the Reporting System for Infectious Diseases (MSIS) (5). The highest number was recorded in 2013, with 88 cases distributed among 18 of Norway’s 19 counties. Nord-Trøndelag was the only county in which no cases of malaria were reported. By way of comparison, 27 – 48 cases of systemic meningococcal disease were reported during the same period (5). As many as 57 – 75 % of the malaria cases diagnosed in Norway are caused by P. falciparum (5).
Atovaquone-proguanil or mefloquine are usually recommended as prophylaxis in connection with travel to malaria areas. According to figures from the Norwegian Prescription Register, 23 787 prescriptions for atovaquone-proguanil and 4 011 for mefloquine were issued in Norway in 2012 (6). There has been a gradual increase in the annual number of prescriptions for atovaquone-proguanil over the past decade, with 8 430 more prescriptions in 2012 than in 2005, while the annual number of prescriptions for mefloquine has remained unchanged.
In Norway, African immigrants are the group who most frequently contract malaria, because they often travel to endemic areas without using prophylaxis (7). Our experience is that people who originate from malaria-endemic areas find the disease troublesome but seldom dangerous, because of immunity, and do not take into account that they have lost their immunity to malaria. Tourists, people on foreign postings and other travellers are also at risk of infection. It is therefore important for all population groups to be aware of the risk of malaria (7).
Malaria symptoms are non-specific in the early phase, and may be misdiagnosed as influenza, gastroenteritis or other acute fevers with general symptoms in the form of nausea, vomiting, diarrhoea, headache, backache, muscular pain or cough (8).
In cases of falciparum malaria or the rare type of malaria that is due to Plasmodium knowlesi, the disease can rapidly develop into serious illness where emergency treatment may save the patient’s life. A malaria patient who is generally affected to the extent of being incapable of swallowing tablets, has signs of vital organ dysfunction or a high parasite count (> 2 – 4 %), has severe malaria (8). Pregnant women and small children are at particular risk of more rapid development of the disease and a more serious course (9).
Malaria is diagnosed by means of Giemsa-stained thin- and thick-film blood film smears that reveal the type of Plasmodium and parasitaemia (percentage of red blood cells infected). Antigen tests constitute a supplement that can rapidly detect whether the patient has malaria and should therefore be available at all hospitals, especially those without malaria microscopy expertise. There are many different malaria rapid diagnostic tests (RDTs) with varying sensitivity and specificity (10). All tests have a generally lower sensitivity to species other than P. falciparum.
Patients with suspected malaria must take a test without delay. If falciparum malaria is detected, the patient must be treated and put under surveillance in hospital where drugs for intravenous treatment must be available in case the disease takes a severe course. Detailed guidelines for malaria treatment in Norway have been published previously in the Journal of the Norwegian Medical Association (11) and in Nasjonal faglig retningslinje for bruk av antibiotika i sykehus [National guidelines for the use of antibiotics in hospitals], published by the Norwegian Directorate of Health in 2013 (12).
The object of the present study was to investigate preparedness and procedures for the diagnosis and treatment of malaria at Norwegian hospitals.
Material and method
We carried out a questionnaire survey in the period October 2012 – August 2014. It was conducted with the aid of the online tool QuestBack Ask & Act (QuestBack Norge, Oslo, Norway). We made telephone contact with heads of department at hospitals with an internal medicine function or heads of sections for infectious diseases at those hospitals that have them. A total of 48 hospitals were contacted. The questions with response alternatives are shown in Box 1.
Questions with response options
-
What is used to diagnose malaria in your department?
Microscopy of thick blood smears
Microscopy of thin blood smears
Microscopy of thick and thin blood smears
Rapid diagnostic test + microscopy of blood smears
Only rapid diagnostic test
Other
-
What first-line drugs do you have in preparedness at your hospital for initial parenteral treatment of severe/complicated falciparum malaria?
Intravenous quinine
Intravenous artesunate
Other
The option «Other» allowed respondents to enter free text in a text box; the other options had a box to set a cross in
The transport time between hospitals was determined using Google Maps.
In cases of doubt regarding the answers reported on the electronic questionnaire, the hospital was contacted by telephone for an explanation. In cases of failure to respond, repeated reminders were sent. The study was submitted to the Regional Ethics Committee, which decided that approval was not necessary.
Results
Of the 48 hospitals contacted, heads of department or sections at 38 hospitals responded to the electronic questionnaire. Responses were subsequently collected from senior consultants at the remaining ten hospitals by telephone, so that we have responses from all hospitals that could potentially encounter malaria patients in Norway. Hospitals that reported that they did not have drugs in preparedness were contacted to ask whether there had been any changes in their malaria preparedness subsequently.
As many as 40 % (19/48) reported that they did not have drugs for severe malaria available. Thirteen hospitals commented that they would have sent malaria patients on to another hospital, two would have had drugs sent from another hospital, while four reported that they did not have drugs for treating severe malaria available – without any further indication of their plan of action should such a case arise.
The results of the reported available means of diagnosing and treating severe malaria at Norwegian hospitals are presented in Table 1.
Table 1
Diagnostic methods and drugs for treating severe malaria available at Norwegian hospitals based on a national questionnaire (n = 48)
| Number |
(%) |
|
| Diagnostic methods |
||
| Rapid diagnostic test and microscopy available |
31 |
(65) |
| Only microscopy available |
13 |
(27) |
| Only rapid diagnostic test available |
1 |
(2) |
| No diagnostic methods available |
3 |
(6) |
| Drugs |
||
| Only artesunate for intravenous use available |
13 |
(27) |
| Only quinine for intravenous use available |
13 |
(27) |
| Both artesunate and quinine for intravenous use available |
3 |
(6) |
| Neither artesunate nor quinine for intravenous use available |
19 |
(40) |
Of hospitals without artesunate or quinine available (n = 19), as many as 11 had more than two hours of travel time to the nearest hospital with preparedness. Three of these did not have diagnostics available either. Table 2 shows available diagnostics and transport time by road to the nearest hospital with preparedness for hospitals without artesunate or quinine available.
Table 2
Diagnostic methods available and transport time by road to reference hospital for hospitals that do not have artesunate or quinine available (n = 19). Figures indicate number of hospitals
| Transport time (min) |
||||
| Hospitals without medical preparedness |
< 60 |
60 – 120 |
121 – 480 |
Total |
| Total number of hospitals |
2 |
6 |
11 |
19 |
| Rapid diagnostic test and microscopy available |
2 |
4 |
2 |
8 |
| Only microscopy available |
0 |
2 |
6 |
8 |
| Only rapid diagnostic test available |
0 |
0 |
0 |
0 |
| No diagnostic methods available |
0 |
0 |
3 |
3 |
Discussion
Malaria is a condition requiring emergency aid for which there has been an increase in the number of cases reported to MSIS in the last few years. Reliable diagnostics and effective drugs should be available at all Norwegian hospitals in order to be able to prevent deaths (5, 13). This survey has revealed deficiencies in emergency preparedness for the diagnostics and treatment of severe malaria in Norway. Three hospitals do not have diagnostics available, and 40 % do not have preparedness for acute treatment of severe malaria.
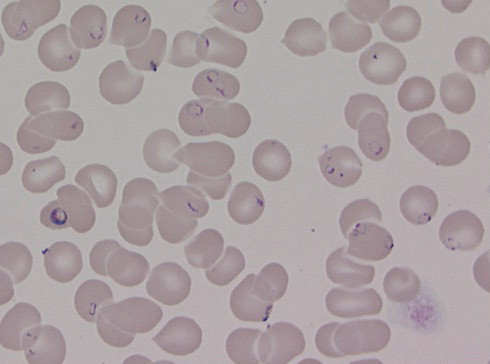
Microscopy requires experience of the method and is necessary for determining the degree of parasitaemia and hence the severity, and for reliable species identification (Fig. 1) (14). At hospitals where microscopy expertise is not available 24 hours a day, a RDT should be available that can be carried out while waiting for a microscopy examination. Twenty-four hour preparedness is necessary for hospitals that have microscopy but no RDT available. It is unlikely that all small local hospitals will have 24-hour preparedness, and these will benefit most from RDTs. These tests are simple to carry out, and are recommended as a minimum for malaria diagnostics at all hospitals in Norway.
Artesunate is an effective malaria drug with few side effects. Randomised studies have shown that it results in higher survival than quinine, and it is recommended as the first choice of treatment for severe falciparum malaria (11, 12, 15) – (17). Quinine is an alternative to artesunate at those hospitals that only have the former available, but in addition to having a slower onset effect than artesunate, it may also cause side effects such as arrhythmia, longer QT interval, cinchonism (tinnitus and dizziness) and hypoglycaemia (17). Both artesunate and quinine must be procured with exemption from registration.
A package of artesunate containing six 60 mg units costs around NOK 670. This means a cost of only about NOK 1 500 for treating an adult. The shelf life is 2 – 3 years from the date of manufacture. The costs of antimicrobial treatment applied on the correct indication will always be justified in cases of serious and life-threatening infectious diseases (18).
In terms of incidence, severity and the need for specialist health services, severe malaria can be compared with acute bacterial meningitis, where intravenous antibiotics are recommended within half an hour of clinical suspicion (12, 19). As with meningitis, treatment delay worsens the prognosis for malaria patients. Malaria deaths in Europe are very largely attributable to delayed diagnosis and treatment (20, 21).
It is cause for concern that all the Norwegian hospitals that reported that they did not have drugs available for treating severe malaria were local hospitals, and only two of 19 had less than an hour’s transport time to hospitals with preparedness. The use of ambulance planes and helicopters must be assumed to reduce the transport time, but geographical and meteorological conditions may restrict the feasibility of this transport at any given time (22).
The increase recorded in the last ten years in the prescription of atovaquone-progruanil is probably due to the fact that Norwegians increasingly travel to malaria-endemic areas, although it may also be partly due to more people protecting themselves against malaria in connection with travel, or increasing use of long-term prophylaxis. In 2013, malaria was diagnosed in 18 counties in Norway, which shows that doctors at any hospital in Norway risk facing a febrile patient who proves to have malaria.
We found that some hospitals that do not have drugs available are well prepared for transferring patients to another hospital, so that the treatment delay is short and compensated for by the benefit of centralising treatment. But the survey reveals that more than a third of Norwegian hospitals cannot provide acute treatment for patients with severe malaria, which increases the risk of a fatal outcome for this disease.
MAIN POINTS
P. falciparum malaria is an acute infection that rapidly becomes life-threatening
There should be a rapid diagnostic test for malaria at all Norwegian hospitals
Artesunate is the first choice for treatment of severe malaria, and should be available at all Norwegian hospitals
- 1.
World malaria report. Genève: WHO, 2013.
- 3.
European Centre for Disease Prevention and Control. www.ecdc.europa.eu/en/publications/Publications/annual-epidemiological-report-2013.pdf (25.9.2014).
- 5.
MSIS. Folkehelseinstituttet. www.msis.no (25.9.2014).
- 6.
Reseptregisteret 2005 – 2012. www.reseptregisteret.no (25.9.2014).
- 7.
Smittevernboka. Oslo: Folkehelseinstituttet, 2013. http://www.fhi.no/eway/default.aspx?pid=239&trg=Content_6493&Main_6157=6287:0:25,5499&MainContent_6287=6493:0:25,6833&Content_6493=6441:82817::0:6446:77:::0:0 (25.9.2014).
- 8.
Severe falciparum malaria. World Health Organization, Communicable Diseases Cluster. Trans R Soc Trop Med Hyg 2000; 94 (suppl 1): S1 – 90. [PubMed]
- 10.
Malaria rapid diagnostic tests performance, round 5. Genève: WHO, 2013.
- 11.
Mørch K, Myrvang B. Medikamentell behandling av malaria i Norge. Tidsskr Nor Legeforen 2012; 132: 664 – 7. [PubMed]
- 12.
Nasjonal faglig retningslinje for bruk av antibiotika i sykehus. Oslo: Helsedirektoratet, 2013.
- 17.
Guidelines for the treatment of malaria. 2 utg. Genève: WHO, 2010.
- 18.
Helsedirektoratet. Kostnadsvurderinger. http://helsedirektoratet.no/sites/antibiotikabruk-i-sykehus/generelle-kapitler/kostnadsvurderinger/Sider/default.aspx (25.9.2014).
- 19.
Skrede S, Sjursen H, Solberg CO. Behandling av akutt bakteriell meningitt. Tidsskr Nor Lægeforen 2001; 121: 3306 – 9. [PubMed]
- 22.
Haug B, Åvall A, Monsen S-A. Luftambulansens pålitelighet – en undersøkelse i tre kommuner på Helgeland. Tidsskr Nor Legeforen 2009; 129: 1089 – 93. [PubMed]