A number of studies have shown that increasing travel distances lead to less use of various health services. Geography may play as large a role as demographic and socioeconomic factors. Examples include the rate of participation in mammography programmes (1), follow-up of patients with dementia (2) and psychiatric treatment of substance addiction (3). Short distances to hospital lead to higher hospitalisation rates for children (4), and long distances are a major barrier to referral to hospital from general practitioners (5).
Distances also have an effect on the use of emergency primary health services. A Belgian study showed that among patients with non-urgent conditions who made use of a paediatric emergency department, children with short travel distances were clearly overrepresented (6). Studies of emergency primary medical services in other countries are not directly transferable to the Norwegian municipal system of out-of-hours (OOH) emergency primary care, since equivalent services are organised differently in other countries.
Previously we have shown that the activity in casualty clinics declines sharply with increasing distances (7, 8). In the period 2007 – 11 in Arendal casualty clinic, an increase in average travel distance of 43 kilometres was associated with a 50 % reduction of face-to-face consultation rates in the participating municipalities. The contact rates declined for all degrees of urgency, and the effect was almost totally independent of several significant demographic and socioeconomic factors. The municipalities in these studies are included in the so-called Watchtower project at the National Centre for Emergency Primary Health Care, in which seven casualty clinics serving a total of 18 municipalities provide detailed but not personally identifiable information on all their patient contacts.
In this study we primarily wanted to investigate whether the correlation between distance and utilisation of OOH services observed in the Watchtower project could be reproduced when analysing activity data based on reimbursement claims (electronic account cards) from all of Norway’s municipalities. We also investigated the distance-adjusted effect on the utilisation of OOH services resulting from two other key issues related to the organisation of such services: Is there any difference in the use of OOH services between municipalities that provide these services only for their own population (single-municipality casualty clinics) and municipalities that participate in an inter-municipal scheme (inter-municipal casualty clinics)? Is the utilisation of casualty clinics affected by a co-location of these services with a hospital?
Material and method
We conducted an ecological cross-sectional study to investigate the correlation between travel distance and utilisation of casualty clinics. Data on travel distances were retrieved from another article in which we calculated the travel times and distances to casualty clinics for 417 of Norway’s 430 municipalities in 2011 (9). The calculations were made using a postcode-based method (8) and data on the organisation of OOH services and addresses of the casualty clinics retrieved from the National Primary Emergency Health Care Registry (10).
In this study we have included municipalities in which the casualty clinic is located in single permanent premises throughout the opening hours. For these municipalities we can calculate the average driving distance to the casualty clinic. We excluded municipalities where the location of the OOH casualty clinic varies with time of day and/or weekday, for example because of cooperation with other municipalities. We also excluded municipalities that have more than one OOH casualty clinic. In a small number of municipalities, boats are used as mobile casualty clinics. These were also excluded.
Information on the activity at the casualty clinics in each municipality in 2011 was retrieved from the website of the Directorate of Health, where management data for the medical services in the municipalities can be downloaded as an Excel document (11). The figures stem from the KUHR registry (Control and Disbursement of Health Reimbursements), which is the information system of the Norwegian Health Economics Administration (HELFO). This includes an overview of reimbursement claims from each individual municipality, grouped by the number of medical consultations (tariff code 2ak), telephone/letter contacts (tariff code 1bk) and home visits (tariff code 11ak). The population-adjusted rates (per 1000 inhabitants per year) are based on the municipalities’ population as of 1 January 2011 (12).
In this study, the measure used for OOH activity is the number of reimbursement claims recorded in the KUHR database for OOH services per 1 000 inhabitants per year in each municipality. Contact rates by travel distance was the main outcome measure, estimated for all reimbursement claims as well as for reimbursement claims with tariff codes for medical consultations, telephones/letter and house calls.
Secondary outcome measures include the activity at casualty clinics adjusted for travel distances in municipalities that are attached to a single-municipality versus an inter-municipal casualty clinic, or where the OOH casualty clinic is co-located with a hospital or have another location.
In addition, we compared hospitalisation rates in the specialist health services based on municipal health data from the Norwegian Institute of Public Health for the period 2010 – 12 (13) in municipalities with an inter-municipal casualty clinic co-located with a hospital and municipalities with an inter-municipal casualty clinic located outside a hospital.
Statistical methods
The statistical analyses were performed in Microsoft Excel 2010 and IBM SPSS Statistics 21. We chose to use exponential regression analysis since this method has previously proven to be best able to describe the correlation between travel distances and utilisation of OOH services (8). No corrections were made for any outliers. The determinant coefficient (r²) with its associated p-value was estimated. The change in the rate (%) following from an increase from 0 to 50 kilometres of average distance was estimated for each outcome.
We also performed exponential regression analysis for sub-groups of casualty clinics independently of distances to investigate the effect on the consultation rates for OOH services from participation in a single-municipality versus an inter-municipal casualty clinic, as well as the effect of whether or not OOH services were co-located with a hospital. We estimated marginal average consultation rates with a 95 % confidence interval (95 % CI) for the average distance involved in all the municipalities included.
Finally, a 95 % confidence interval for differences in hospitalisation rates was estimated.
Results
A total of 101 of Norway’s 430 municipalities in 2011 were excluded because of the alternating location of their OOH casualty clinics, and 13 were excluded because boats were used as casualty clinics. One further municipality was excluded because KUHR data were missing after a municipal merger. This municipality, along with those included, is identical to the 316 municipalities with permanent casualty clinic premises that have been described in another article (9). Altogether 315 municipalities with a total of 3 448 874 inhabitants were available for analysis. These accounted for 73 % of the municipalities and 70 % of Norway’s total population in 2011. The KUHR database provided information on 1 290 630 reimbursement claims from these municipalities, equal to 72 % of all reimbursement claims from OOH services in Norway in 2011.
Results from the regression analysis (exponential) are shown in Table 1. There was a statistically significant association between increasing distances and reduced frequency of contacts, consultations and home visits. The number of telephones/letters was not significantly correlated with the distance to the casualty clinic. Figure 1 shows the consultation rate in casualty clinics by average travel distance. The consultation rate dropped by 1.3 % for each kilometre of added travel distance.
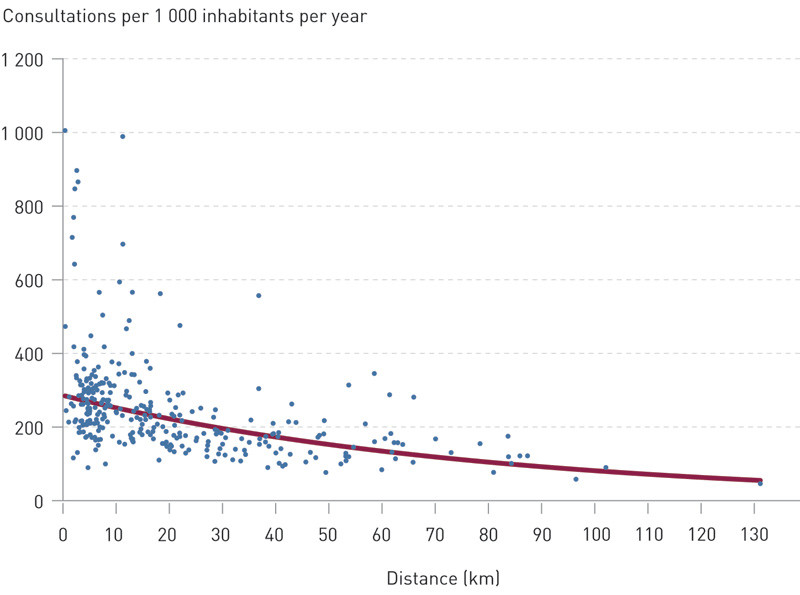
Table 1
Correlation between distances and rates of various types of contact with casualty clinics in Norwegian municipalities that have single permanent casualty clinic premises (N = 315). Exponential regression: Rate = Constant(eCoefficient · distance(km)). Contact rates are estimated for distances of 0 and 50 km from the casualty clinic
| Contact rate (number/1 000 inhabitants/year) |
Reduction from 0 to 50 km (%) |
||||||
| Constant |
Coefficient |
R² |
P-value |
0 km |
50 km |
||
| Consultations |
285 |
–0.013 |
0.3 |
< 0.001 |
285 |
148 |
48 |
| Telephones/letters |
78 |
–0.003 |
0.007 |
0.126 |
78 |
67 |
14 |
| Home visits |
11 |
–0.016 |
0.06 |
0.001 |
11 |
5 |
55 |
| All contacts |
481 |
–0.012 |
0.2 |
< 0.001 |
481 |
263 |
45 |
Table 2 and Figure 2 present the results of exponential regression analysis regarding the correlation between travel distances and consultation rates according to whether the municipalities provided OOH services that were co-located with hospitals or not, and whether they have single-municipality or inter-municipal casualty clinics. There was a statistically significant correlation between distances and consultation rates for all categories of municipalities, except in the ten municipalities that had a single-municipality casualty clinic located outside a hospital (not shown in the figure).
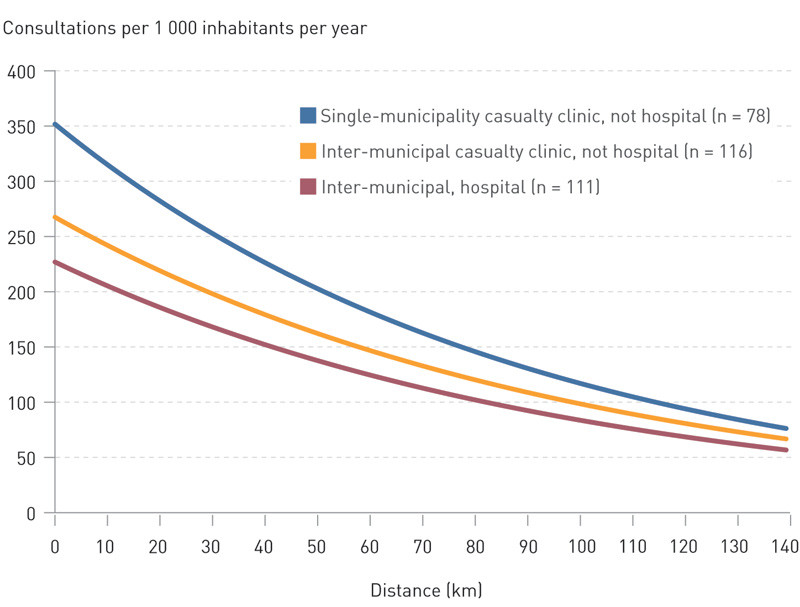
Table 2
Correlation between distances and consultation rates for Norwegian municipalities with a permanent casualty clinic premises by linkage to a single-municipality or an inter-municipal casualty clinic and by linkage to casualty clinics co-located or not co-located with hospitals. Exponential regression: Consultation rate = Constant(eCoefficient · distance (km))
| Number |
Constant |
Coefficient |
R² |
P-value |
|
| Single-municipality casualty clinic |
88 |
339 |
–0.010 |
0.05 |
0.04 |
| Inter-municipal casualty clinic |
227 |
251 |
–0.010 |
0.3 |
< 0.001 |
| Not co-located with a hospital |
194 |
313 |
–0.013 |
0.4 |
< 0.001 |
| Co-located with a hospital |
121 |
233 |
–0.010 |
0.5 |
< 0.001 |
| Single-municipality casualty clinic Not co-located with a hospital |
78 |
354 |
–0.011 |
0.07 |
0.02 |
| Inter-municipal casualty clinic Not co-located with a hospital |
116 |
269 |
–0.010 |
0.2 |
< 0.001 |
| Inter-municipal casualty clinic Co-located with a hospital |
111 |
228 |
–0.010 |
0.5 |
< 0.001 |
| Single-municipality casualty clinic Co-located with a hospital |
10 |
168 |
0.038 |
0.1 |
0.3 |
| All casualty clinics |
315 |
285 |
–0.013 |
0.3 |
< 0,001 |
At a travel distance of 21 kilometres, the single-municipality casualty clinics had a 35 % higher consultation rate than the inter-municipality clinics, and casualty clinics located outside hospitals had a 28 % higher consultation rate than their counterparts that were co-located with a hospital. Figure 2 shows that municipalities participating in inter-municipal casualty clinics that are co-located with hospitals have the lowest consultation rates. In comparison, municipalities participating in inter-municipal casualty clinics located outside hospitals had an 18 % higher estimated consultation rate at 21 kilometres, the average travel distance for all the municipalities included. Similarly, single-municipality casualty clinics outside hospitals had a 53 % higher consultation rate at 21 kilometres (Table 3).
Table 3
Consultation rates (consultation tariff codes per 1000 inhabitants, 2011), non-adjusted and adjusted for distance. Estimated marginal average at 21 kilometres, depending on whether the municipality is linked to a single-municipality or an inter-municipal casualty clinic, and depending on whether the clinic is co-located with a hospital or not
| Number |
Consultation rate, non-adjusted |
Consultation rate at 21 km |
(95 % CI) |
|
| Single-municipality casualty clinic |
88 |
342 |
273 |
(249 – 299) |
| Inter-municipal casualty clinic |
227 |
208 |
202 |
(193 – 211) |
| Not co-located with a hospital |
194 |
282 |
241 |
(227 – 255) |
| Co-located with a hospital |
121 |
189 |
189 |
(180 – 199) |
| Single-municipality casualty clinic Not co-located with a hospital |
78 |
353 |
283 |
(256 – 312) |
| Inter-municipal casualty clinic Not co-located with a hospital |
116 |
234 |
218 |
(205 – 233) |
| Single-municipality casualty clinic Co-located with a hospital |
10 |
257 |
214 |
(174 – 263) |
| Inter-municipal casualty clinic Co-located with a hospital |
111 |
183 |
185 |
(176 – 195) |
Rates for telephones/letters and house calls at 21 kilometres were significantly higher in municipalities with a single-municipality casualty clinic when compared to inter-municipal casualty clinics, as well as in municipalities with casualty clinics located outside hospitals when compared to casualty clinics co-located with hospitals (data not shown).
The analyses of the host municipalities of inter-municipal casualty clinics (n = 71) showed no statistically significant differences in consultation rates, even when adjusted for distance, between municipalities with a casualty clinic at the local hospital (n = 30) and municipalities where the casualty clinic was not located at the hospital (n = 41) (data not shown).
Municipalities that were associated with an inter-municipal casualty clinic co-located with a hospital had a 4 % higher rate of admission to the specialist health services than municipalities that had an inter-municipal casualty clinic outside a hospital: 166 versus 159 admissions per 1 000 inhabitants per year (95 % CI for the difference: 3.0 – 10.5).
Discussion
This study shows that in Norwegian municipalities with casualty clinics in a single permanent location in 2011, increasing average travel distances were strongly associated with reduced activity at the casualty clinic as reflected in reimbursement claims submitted to HELFO. An increase in travel distances from 0 to 50 kilometres led to a 45 % reduction in the frequency of tariff codes for contacts with casualty clinics as a whole. Municipalities linked to casualty clinics located in hospitals had lower consultation rates than municipalities with casualty clinics located outside hospitals when adjusted for distance. Similarly, municipalities linked to single-municipality casualty clinics had higher consultation rates for OOH services than municipalities linked to inter-municipal casualty clinics.
The reduction in the total number of contacts, consultations and house calls was of the same magnitude as in previously reported findings from the casualty clinics included in the Watchtower project (7, 8). The observed drop in the consultation rate of 1.3 % per kilometre was somewhat lower than that in the Watchtower clinics where it amounted to 1.8 % per kilometre (8). We have previously detected a greater use of telephone consultations with an increase in distance. In the present material we cannot observe any such increase, but based on the regression analysis we rather noted a small decrease.
The findings in this study strengthen the hypothesis that travel distance is a crucial factor for utilisation of OOH services. We believe that the results emphasise the necessity of giving priority to measures that can counteract the inequalities in the utilisation of OOH services caused by distance. As in other services, also within health care, the differences can partly be explained by the fact that availability rather than real needs decides the degree of utilisation.
The observation that municipalities having casualty clinics located in an inter-municipal facility or at a hospital have lower face-to-face consultation rates when adjusted for distance can be explained by the fact that these clinics tend to be larger and more professional, and therefore better able to give priority to those patients who are in real need of emergency medical services. The threshold for contacting casualty clinics in hospitals may be higher because the population tends to see them less as part of the primary health services, or because the members of staff who receive the calls may find it easier to turn patients away due to a larger perceived distance to the callers.
Moreover, hospital-based and inter-municipal casualty clinics will often face a greater scarcity of medical resources because of their high patient load, while the lower load at single-municipality casualty clinics may give doctors a greater financial incentive to take in patients who should preferably be treated by a GP during regular office hours. In hospitals, more patients are likely to be directly admitted without first having been examined by a doctor at the casualty clinic.
Figures from the Watchtower project show that three of every four contacts in casualty clinics have a «green» degree of urgency (14), and a considerable proportion of these involve conditions that can often be handled by a GP during the daytime. We may therefore assume that the utilisation of OOH services is somewhat higher than what purely medical conditions would indicate. We believe that the results in this study indicate that the utilisation of OOH services can be reduced by municipalities joining forces in inter-municipal casualty clinics, as suggested in the action plan proposed by the National Centre for Emergency Primary Health Care from 2009 (15).
One may easily take the lower consultation rate detected in hospital-based casualty clinics as an argument for integrating emergency primary and secondary services in hospitals, similar to what is common internationally in the form of «emergency rooms» or «accident and emergency departments». We believe that the findings provide no grounds for such a conclusion. Norwegian casualty clinics are not integrated into the hospitals’ emergency wards as they tend to be in other countries. As a rule, they are co-located in separate premises as an independent organisation. Like other Norwegian casualty clinics, they have a strong basis in general-practice medicine, making them incomparable to emergency wards in other countries.
The advantages of co-location must be weighed against the risk of an increasing number of admissions. The National Centre for Emergency Primary Health Care has been sceptical to the integration of OOH services into emergency wards (so-called joint emergency wards) exactly because of the risk of weakening the casualty clinic’s function as a gatekeeper. This may lead to an increased use of resources in the hospitals and an increased use of easily available technology and diagnostic equipment on the casualty clinic’s patients – with no beneficial health effect (15).
The results from this study show that in 2011 municipalities that were linked to an inter-municipal casualty clinic based in a hospital had a 4 % higher rate of admissions than municipalities in which the casualty clinic was located outside a hospital. This difference was nevertheless far smaller than the difference in consultation rates in casualty clinics (22 %, not adjusted for distance). It is worth noting that these figures are not directly comparable, because a person is counted only once in the admissions statistics if he or she is admitted on repeated occasions with the same condition during a single year. In the KUHR database a person can be registered an unlimited number of times with the same condition.
A key strength of this study is that it retrieves data from the KUHR database, an official and objective source based on all patient contacts for which the doctor has written an electronic invoice to HELFO. The material does not include paper-based reimbursement claims and reimbursements that are paid to the patient if the doctor has no contract for direct settlement; these have been estimated to account for less than 1 % in 2010 (16). The number of reimbursement claims appears to provide a good impression of the activity in the primary health services, and the National Centre for Emergency Primary Health Care publishes annual reports on the activity in casualty clinics on the basis of such figures (16).
A majority of the country’s municipalities and inhabitants are included in the analyses presented in this study. Our data sources cannot tell us anything about the correlation between distances and utilisation of OOH services in the excluded municipalities, but we have no reason to assume that the effect will be any different there. The median population is lower in the excluded municipalities, but according to our previous studies (7, 8) the distance effect is not weaker in small municipalities.
We have previously documented that the method used for estimating average distances is at least as reliable as other standard methods when the exact addresses are unknown (8), although variations in the postcode structure may have given rise to varying levels of precision between municipalities.
Compared to the results from the studies of the municipalities included in the Watchtower project, there is a larger dispersion in the contact rates based on reimbursement claims. Part of the reason is that this study includes a higher number of municipalities, which demonstrates that Norwegian municipalities are more diverse than that indicated by the Watchtower project.
When a patient uses OOH services in another municipality, the reimbursement claim will be registered in his or her home municipality. The effect that this will have on the analysis is uncertain. We have previously shown that the casualty clinics included in the Watchtower project are used to only a small extent by the inhabitants of the neighbouring municipalities (14). Patients from abroad or from municipalities outside the OOH district accounted for 9 % of the contacts at Arendal casualty clinic in the period 2007 – 11 (7), and there is reason to assume that this proportion may be higher in other municipalities where a larger proportion of the inhabitants stay outside the municipality for longer periods of time (weekly commuters, students). Different practices for the use of tariff codes may also have an effect, for example a patient who has contacted the casualty clinic on repeated occasions can account for one or more reimbursement claims, depending on local practices.
Incorrect information in the Norwegian Emergency Primary Health Care Registry may also produce inaccuracies in the results. Even though the information stems from the OOH services themselves, we have identified a number of errors that have been corrected. We cannot exclude that certain errors have been left undiscovered in the information that we have used in our analyses regarding the organisation of OOH services.
Many comparisons have been made, and this increases the risk of false-positive results. We have not corrected for multiple testing. In this study we have only investigated co-location with hospitals and linkages to single-municipality versus inter-municipal casualty clinics. It is possible that the findings can be explained by other factors that we have not investigated. In a previous study we have shown that the utilisation of OOH services is minimally influenced by coverage of medical services, income levels, income differences, the proportion of inhabitants older than 80 and education levels when compared to geographical distance (7).
It is important to point out that the information in the management data from the KUHR database is restricted to the number of different types of contact in each municipality. In contrast to the Watchtower project there is no information on degree of urgency, age, gender or the use of ambulance transport.
Conclusion
This study confirms that the distance to the casualty clinic is crucial for the extent to which the population of a municipality utilises OOH services. Our findings also show that inter-municipal casualty clinics are associated with a reduced utilisation of OOH services. A co-location with hospitals is also associated with a reduced number of consultations in casualty clinics.
MAIN MESSAGE
Statistics based on reimbursement claims from Norwegian municipalities showed a clear correlation between increasing distances to out-of-hours casualty clinics and a lower use of emergency primary health care in 2011.
Municipalities participating in inter-municipal out-of-hours services had lower consultation rates than municipalities with single-municipality out-of-hours services when adjusted for distance.
Municipalities in which the casualty clinic was co-located with a hospital had lower consultation rates, adjusted for distance, than municipalities in which out-of-hours services were provided outside hospitals.
- 4.
Goodman DC, Fisher ES, Gittelsohn A et al. Why are children hospitalized? The role of non-clinical factors in pediatric hospitalizations. Pediatrics 1994; 93: 896 – 902. [PubMed]
- 9.
Raknes G, Morken T, Hunskår S. Reisetid og avstand til norske legevakter. Tidsskr Nor Legeforen 2014; 134: 2145 – 50.
- 10.
Morken T, Zachariassen SM. Legevaktorganisering i Norge. Rapport fra Nasjonalt legevaktregister 2012. Rapport nr. 6 – 2012. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Uni Helse, Uni Research, 2012.
- 11.
Helsedirektoratet. Kommunenes bruk av fastleger og legevakt. www.helsedirektoratet.no/finansiering/okonomiske-virkemidler-i-samhandlingsreformen/styringsdata-for-kommuner/Sider/Kommunenes-bruk-av-fastleger-og-legevakt.aspx (10.2.2014).
- 12.
Statistisk sentralbyrå. Folkemengd og kvartalsvise befolkningsendringar. http://ssb.no/befolkning/statistikker/folkendrkv/kvartal. (10.2.2014).
- 13.
Folkehelseinstituttet. Kommunehelsa statistikkbank. http://khs.fhi.no/webview/ (18.3.2014).
- 14.
Eikeland OJ, Raknes G, Tønsaker S et al. Vakttårnprosjektet. Epidemiologiske data frå legevakt. Samlerapport for 2012. Rapport nr. 4 – 2013. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Uni Helse, Uni Research, 2013.
- 15.
Nasjonalt kompetansesenter for legevaktmedisin. ... er hjelpa nærmast! Forslag til Nasjonal handlingsplan for legevakt. Rapport nr. 1 – 2009. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Unifob helse, 2009.
- 16.
Sandvik H, Hunskår S. Årsstatistikk fra legevakt 2012. Rapport nr. 3 – 2013. Bergen: Nasjonalt kompetansesenter for legevaktmedisin, Uni Helse, Uni Research, 2013.