Patients’ experience of their general practitioner’s follow-up of serious eating disorders
In 2002, a general practitioner (GP) had an average of ten patients with an eating disorder requiring treatment on his/her list – one with anorexia and nine with bulimia (1). More recent epidemiological studies give no reason to believe that eating disorders have increased, but the number of women with anorexia in the age group 15 – 19 years is growing – either because they are being detected sooner, or due to earlier onset of the disorder (2).
An eating disorder may have a fatal outcome. The government’s strategic plan recommends that most patients with an eating disorder be treated in general practice, but that those who are most ill must be dealt with by the specialist health service (2, 3). In the strategic plan and the national guidelines, emphasis is placed on collaboration between the treatment levels (3, 4).
A severe eating disorder arises «when the patient’s relationship to food disrupts and prevents normal functioning, socially, at work or at school for beyond a period of six months» (5). In ICPC-2, bulimia and anorexia have the same diagnostic code: P86 anorexia nervosa/bulimia (6). Conscious weight loss denotes anorexia, while repeated episodes of overeating and vomiting denote bulimia. In ICD-10 a BMI < 17.5 kg/m² is decisive for the diagnosis of anorexia (7). Denial of the illness, feelings of shame and guilt, and ambivalence may prevent the patient from being open about her/his symptoms or from feeling that she/he deserves help (5, 8, 9).
Psychotherapy, which also emphasises symptom reduction, and somatic follow-up/treatment are central elements of the therapy (4). Continuous motivational effort is of crucial importance for recovery (5, 8, 10). A strong alliance with the treatment provider is essential (5, 8) – (12) and cooperation between the patient and the treatment provider, openness, curiosity, patience, focused and systematic follow-up and an individualised approach are crucial (10). Treatment providers who signal acceptance of the person behind the illness, who are involved and show patience and who communicate with professional authority and certainty, are those who most easily achieve the trust of patients with anorexia (11). Drug therapy, beyond any treatment of comorbid mental conditions such as anxiety, depression and/or compulsive behaviours, has a limited role to play (9).
Persons with eating disorders visit their GPs more frequently than their peers in the general population (13) – (15). They present with symptoms that may be attributed to the eating disorder without the illness necessarily being discussed during the consultation. Nothing has been found in the literature about how collaboration between the treatment levels should be implemented. A Norwegian article about patients with eating disorders who are treated in the general medical services emphasises conversations about the situation here and now, functioning and relationships as well as somatic follow-up, supervised self-help and conversations with next of kin (9).
The purpose of our study was to investigate whether patients with a severe eating disorder had spoken with a local GP about their illness during the year preceding the start of treatment at a specialist unit. We wished to ascertain how close the follow-up was, whether the patients were satisfied with their doctor and whether they would visit their GP if the condition worsened. We were also interested in the patients’ experience with collaboration between the treatment levels.
Material and method
The study was conducted at the Outpatient Clinic for Eating Disorders, Department for Personality Psychiatry, Oslo University Hospital, and the Regional Centre for Eating Disorders, Nordland Hospital, Bodø (day unit and outpatient clinic). At both clinics, at least 95 % of patients have one of the following four diagnoses (ICD-10): F.50.0 anorexia nervosa, F.50.1 atypical anorexia nervosa, F.50.2 bulimia nervosa or F.50.3 atypical bulimia nervosa. Fewer than 5 % have the diagnosis F 50.9 unspecified eating disorder.
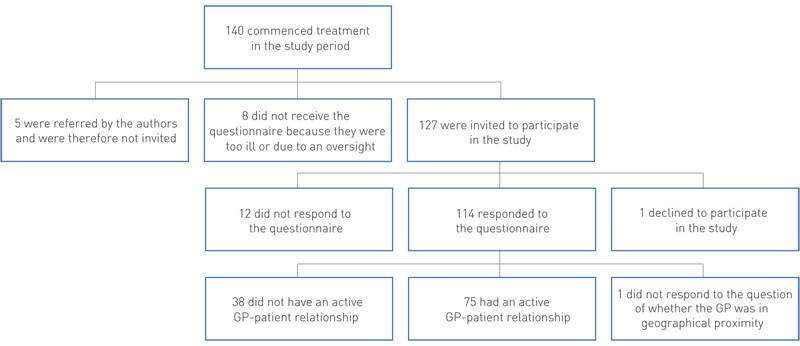
Patients over the age of 18 years at the start of their treatment were requested to respond anonymously to a questionnaire on their use and experience of their GP. The duration of the data collection period for Oslo was from 1 August 2009, and for Bodø from 1 January 2010, to 30 June 2011. Five patients who were referred to specialist units by the authors themselves were not included for reasons of habilitation (Fig. 1).
The questionnaire was developed by the authors based on clinical experience from the GP surgery and the specialist unit. It was tested on 45 patients in a pilot study at the Outpatient Clinic for Eating Disorders in Oslo in 2008 and evaluated and edited in line with the experience gained from this. The questionnaire has been published in full as the Halvorsen appendix (in Norwegian) and is described in e-box 1.
Contents of questionnaire
Section 1. Background information: gender, age, living situation, income
Section 2. Illness data: length of illness, experience of treatment, other somatic illness that could impact on the eating disorder (metabolic syndrome, diabetes, Crohn’s disease, ulcerative colitis, coeliac disease or lactose intolerance), self-reported weight and height, symptoms of eating disorder and relevant afflictions
Section 3. Utilisation of GP: frequency of GP consultations in which the eating disorder was discussed, GP’s gender, allocation of follow-up appointments and call-ins, dropout, use of GP when the condition worsens, experience of collaboration, communication about eating disorder symptoms and afflictions, clinical examinations, satisfaction felt and support by the GP.
Section 4. Conditions related to other health personnel: communication with dentist and accident and emergency doctor
Two definitions were introduced as the results were processed, namely «own GP» and «active GP-patient relationship» (Box 2).
Definitions
«Own GP» was defined based on the patient responding yes to the following question:
«Do you have one GP whom you have seen more than three times and whom you generally use when you need medical services (hereafter referred to as «your doctor»)?»
«Active GP-patient relationship» was defined based on three requirements, all of which had to be fulfilled:
The patient reported having his/her «own GP»
The GP’s practice was in geographical proximity to the patient’s place of residence so that the patient could visit the GP in case of acute exacerbation of the illness
The patient had spoken to the GP about eating disorders during the past year
The data were analysed using a chi-square test and a one-way ANOVA test with SPSS version 20.
Written consent was obtained from the participants, and the study has been approved by the Regional Ethics Committee.
Results
Response rate
Altogether 140 patients commenced treatment in the study period (Fig. 1). Eight of these were not given the questionnaire due to an oversight or because they were too ill to participate. Five were referred by the lead author, and one patient declined to participate. Of the 126 who received the questionnaire, 114 responded (90 %). There were 76 outpatients in Oslo (67 %) and 38 patients (33 %) in Bodø (of whom 20 had been admitted).
We found no significant differences between the patients in Oslo and the patients in Bodø with regard to age, living situation, income, length of illness, somatic comorbidity (thyroid disease, diabetes, Crohn’s disease, ulcerative colitis, coeliac disease or lactose intolerance), proportion of those who were severely underweight, and experience of treatment.
Background data
Three of the patients were men, and 64 patients (56 %) were in the age group 18 – 25 years. Altogether 83 (73 %) had been ill for at least five years. In all, 49 (43 %) of the patients supported themselves with a salary or student loan (Table 1). Every third patient received a work assessment allowance. Half of those who lived alone received this allowance.
Table 1
The patients’ source of income and living situation, given as number of persons (%)
| Salary, student loan, grants and unemployment benefit | Sickness benefit | Work assessment allowance | Financially provided for by others | |||||||||
| Type of living arrangement | Total | Number | (%) | Number | (%) | Number | (%) | Number | (%) | |||
| With partner and/or children | 36 | 19 | (53) | 6 | (17) | 8 | (22) | 3 | (8) | |||
| With parents | 24 | 10 | (42) | 2 | (8) | 5 | (21) | 7 | (29) | |||
| In shared housing | 13 | 8 | (62) | 2 | (15) | 1 | (8) | 2 | (15) | |||
| Alone | 41 | 12 | (29) | 5 | (12) | 23 | (56) | 1 | (2) | |||
| Total | 114 | 49 | (43) | 15 | (13) | 37 | (33) | 13 | (11) | |||
Altogether 24 patients (21 %) had never previously undergone treatment for an eating disorder. Forty (35 %) were only treated as outpatients, whereas 49 (43 %) had had one or more admissions in addition to any outpatient treatment. One patient did not respond to the question regarding whether she had been admitted. Hospital treatment had been provided in the Department for Internal Medicine (n = 26), the Department for General Psychiatry (n = 24) and in the Specialist Unit for Eating Disorders (n = 33).
Average self-reported BMI was 20.2 kg/m² (SD 3.8 kg/m², median 19.8 kg/m²). Altogether 28 patients (26 %) were severely underweight (BMI < 17.5 kg/m²), and 70 (61 %) had been severely underweight in adulthood. The average change in weight in adulthood was 19.5 kg (SD 10.1 kg, median 17.0 kg).
Consultations
In all, 75 patients (66 %) had an active GP-patient relationship according to the study’s definition (Box 2, Fig. 1). Of these, 55 (73 %) had had more than two consultations in the past year during which the eating disorder was discussed (Table 2). In total 49 (65 %) had spoken to their GP about how the illness affected their everyday life (Table 3). Those who were severely underweight and those who had used psychopharmaceuticals/hypnotics visited their GP more frequently than the others (Table 2).
Table 2
Number of GP consultations regarding the eating disorder during the past year for those with an active GP-patient relationship, given as number of patients (%)
| 1 – 2 consultations in past year | 3 – 6 consultations in past year | > 6 consultations | |||||||||
| Number | Number | (%) | Number | (%) | Number | (%) | P-value | ||||
| Total | 75 | 20 | (27) | 30 | (40) | 25 | (33) | ||||
| Current BMI < 17,5 kg/m² | 18 | 2 | (11) | 6 | (33) | 10 | (56) | 0.032 | |||
| Current BMI ≥ 17,5 kg/m² | 54 | 18 | (33) | 23 | (43) | 13 | (24) | ||||
| No previous treatment | 23 | 7 | (47) | 5 | (33) | 3 | (20) | 0.097 | |||
| Previously only outpatient treatment | 40 | 8 | (32) | 11 | (44) | 6 | (24) | ||||
| Previously admitted (and possible outpatient treatment) | 49 | 5 | (14) | 14 | (40) | 16 | (46) | ||||
| Psychopharmaceuticals¹ | 47 | 8 | (17) | 21 | (45) | 18 | (38) | 0.049 | |||
| No psychopharmaceuticals | 28 | 12 | (43) | 9 | (32) | 7 | (25) | ||||
| Sickness benefit | 13 | 2 | (15) | 4 | (31) | 7 | (54) | 0.35 | |||
| Salary, student loan, grant, unemployment benefit | 34 | 11 | (32) | 16 | (47) | 7 | (21) | ||||
| Work assessment allowance | 23 | 6 | (26) | 9 | (39) | 8 | (35) | ||||
| Financially provided for by others | 5 | 1 | (20) | 1 | (20) | 3 | (60) | ||||
| [i] | |||||||||||
[i] ¹ The patients have responded yes to the following question: «Have you taken medication for anxiety, mood swings, psychosis or sleep problems during your period of illness?»
Table 3
Satisfaction with the GP’s manner in encountering the patient and experience of the GP as a mainstay, given as number of patients (%)
| Moderate/high satisfaction | Moderate/strong mainstay | ||||||
| Number | Number | (%) | P-value | Number | (%) | P-value | |
| Total | 75 | 56 | (75) | 35 | (47) | ||
| BMI < 17.5 kg/m² | 18 | 17 | (95) | 0,021 | 11 | (61) | 0.1 |
| BMI ≥ 17.5 kg/m² | 54 | 36 | (67) | 21 | (39) | ||
| Talked about how the illness affects daily life | 49 | 43 | (88) | 0,0003 | 29 | (59) | 0.003 |
| Did not talk about how the illness affects daily life | 26 | 13 | (50) | 6 | (23) | ||
| 1 – 2 consultations in past year | 20 | 9 | (45) | < 0.0001 | 3 | (15) | < 0.0001 |
| 3 – 6 consultations in past-year | 30 | 23 | (77) | 12 | (40) | ||
| > 6 consultations in past year | 25 | 24 | (96) | 20 | (80) | ||
| Check-up appointment allocated | 32 | 29 | (91) | 0,009 | 24 | (75) | < 0.0001 |
| No check-up appointment allocated | 42 | 27 | (64) | 11 | (26) | ||
| Would contact the doctor if condition worsens | 33 | 30 | (91) | 0,004 | 21 | (64) | 0.009 |
| Would not contact the doctor if condition worsens | 42 | 26 | (62) | 14 | (33) | ||
Altogether 32 patients (43 %) who had an active GP-patient relationship were allocated a check-up appointment (Table 3). Those who were severely underweight were allocated the greatest number of check-up appointments (71 % versus 33 %, p = 0.007). Those who had discussed the impact of the illness on their daily lives were more likely to be allocated a check-up appointment than others (57 % versus 16 %, p = 0.001). Ten patients (13 %) had experienced that their GP had contacted them outside normal hours. Altogether 21 patients (28 %) had cancelled their appointments or not attended, without booking a new appointment.
A total of 33 patients with an active GP-patient relationship (44 %) stated that they were accustomed to contacting their GP if their condition worsened. The severely underweight constituted the greatest proportion of these (72 % versus 35 %, p = 0.006). Patients with previous experience of treatment had a greater tendency to contact their GP if their condition worsened (admissions 57 %, outpatient treatment 40 %, no experience of treatment 20 %, p = 0.047). Those who were allocated a check-up appointment were most likely to make contact if their condition worsened (59 % versus 33 %, p = 0.03). Altogether 53 % of those who had spoken about the impact of the illness on their daily lives made contact if their condition worsened, compared to 27 % of the others (p = 0.03).
Patient satisfaction
Fifty-six patients with an active GP-patient relationship (75 %) were moderately/very satisfied with how they were met by their GP (Table 3). Thirty-five (47 %) felt that their GP was an important supporter to a moderate/great degree. Patients who had check-up appointments allocated, and patients who had spoken to their GP about the effect of the illness on their everyday lives, were most satisfied with their GP and were also most likely to experience their GP as an important supporter. The GP’s gender made no significant difference with regard to satisfaction or the support experienced.
The greater the number of consultations, the more patients were satisfied and thought that they had received support. The patients who would contact their GP if their condition worsened were more satisfied and felt that they had more support from their GP than those who stated that they did not contact their GP when their condition worsened.
Collaboration between treatment levels
Altogether 63 (85 %) of the patients with an active GP-patient relationship wanted collaboration between the GP and their treatment providers. Of the 54 patients with previous experience of treatment for which cooperation with their current GP may have been relevant, 21 (39 %) had found that there had been written or spoken communication between the GP and previous treatment provider(s). In total 17 had not experienced this type of communication, and 16 (30 %) did not know whether any collaboration had taken place.
Lack of an active GP-patient relationship
Altogether 38 (34 %) of the patients did not have an active GP-patient relationship. This included 15 patients who did not have their own GP according to the study’s definition, eight who had not spoken to their GP about their eating disorder in the past year (all the GPs were aware of the eating disorder), and 15 who had GPs located in another part of the country. One patient did not state whether the GP surgery was close to their place of residence.
Factors such as age, severe underweight or somatic comorbidity were not decisive in whether the patient had an active GP-patient relationship. Those who were financially provided for were least likely to have an active GP-patient relationship (39 %), whereas those on sick leave most frequently had such a relationship (87 %) (p = 0.045). Altogether 45 % of the patients who lived alone or in shared housing lacked an active GP-patient relationship (p = 0.035).
Discussion
Two out of three patients had an active GP-patient relationship, according to our definition (Box 2). Three out of four of these had spoken to their GP about their illness more than twice in the past year. Overall this means that half of the patients in the study had spoken about their illness to a GP in geographical proximity to them more than twice in the past year (geographical proximity defined as the patient living sufficiently close to the GP surgery that the GP can be consulted in case of acute problems connected to the eating disorder).
Two out of three with an active GP-patient relationship had spoken about how the illness affected their everyday lives. Fewer than half were allocated a check-up appointment and fewer than half were accustomed to contacting their GP if their condition worsened. According to our findings in this study, the GP was therefore not necessarily a part of the treatment apparatus, as the national guidelines indicate (4).
Most of the patients who had used psychopharmaceuticals or were on sick leave had been to see their doctor more than twice in the past year. This may indicate that conversations over several consultations have revealed a need for medication or a medical certificate, or that a wish for a prescription and a medical certificate can function as an entry ticket for contact with the GP.
Two out of four patients with an active GP-patient relationship were satisfied with how the doctor dealt with their illness. Fewer than half thought that the GP was an important supporter. Those who were followed up closely and who spoke about the impact of the illness on their daily lives scored highest on these variables. This indicates that GPs who monitor their patients closely and focus on the patient’s daily life as well as the symptoms of the eating disorder may be most successful in bringing the illness to light in all its aspects. Such an approach may make the patient feel that they are being seen, giving them a feeling of security and thereby a good basis for motivational effort.
This study shows that the patients who lacked an active GP-patient relationship were more often financially provided for, received a work assessment allowance, or lived alone or with persons who were not partners or parents. This group is considered to be particularly exposed to social isolation. This finding supports previous research, in which isolation was a risk factor for deficient follow-up of mental illness in the primary health service (16). It may appear as if the group that completely falls away from the GP follow-up process are those who could have especially benefited from having the GP as their supporter.
Most of those with an active GP-patient relationship wanted collaboration between the treatment levels. However, fewer than half of those who had previously gone for treatment reported these types of experiences. We cannot exclude, for example, that discharge summaries are sent to the GP without the patient having been made aware of this. Researchers emphasise the importance of interdisciplinary cooperation to ensure quality of treatment (17) and to reduce dropout (18). In our opinion, since relatively few have experienced such cooperation, this shows that the national guidelines are not necessarily being followed (4).
Long illness trajectories and several treatment rounds, and the fact that young patients move frequently, make continuity of GP follow-up and collaboration with second-line services especially challenging for patients with eating disorders. The high response rate in the study and the patients’ wish for collaboration between the treatment levels signal that they want greater involvement on the part of the GP.
Strengths and weaknesses of the study
The study’s strength is the relatively large number of patients, which includes both users and non-users of GP services. The findings are nuanced because we have clearly defined «active GP-patient relationship» and because the questions have exclusively dealt with consultations in which the eating disorder is discussed.
The questionnaire was developed based on the authors’ clinical experiences with this patient group from the first as well as the second-line service, and was tested in a pilot study. The high response rate (both in terms of the questionnaire as a whole and each individual question) may indicate that the questions were perceived as relevant by patients. The study thereby provides a picture of some patients’ experiences of the Norwegian health service as it is organised today. These experiences can form the basis for further development of the treatment apparatus for patients with eating disorders.
It is possible that GPs see these patients more seldom when they are treated in the specialist health service. However, the study shows that patients with no experience of treatment did not have more frequent GP follow-up.
The study is based only on the patients’ perceptions, based on a quantitative design. The choice of design limits, for example, the possibility of understanding and describing the patient’s overall behavioural pattern.
It is a weakness of the study that the GPs’ experiences are not presented, and that the questionnaire has not been validated or used in other studies. The fact that the following groups are not represented also constitutes a weakness: patients with a serious eating disorder who do not want or are not offered treatment in a specialist unit, patients with less serious illness and patients with overeating disorders. We therefore do not know whether the findings in the study can be generalised to these groups.
We would like to thank Åse Minde, art psychotherapist and head of unit at the Outpatient Clinic for Eating Disorders, Gaustad, Oslo University Hospital, for her burning commitment, assistance and support in our research project.
MAIN MESSAGE
66 % of those who commenced treatment at a specialist unit for eating disorders had spoken about their illness to a local general practitioner (GP) in the past year
75 % of those who had spoken to a local GP were satisfied with how they were met, but less than half perceived their GP as a main supporter of their treatment
Close follow-up by GPs appears to constitute good support and results in increased satisfaction
Most patients (85 %) with an active GP-patient relationship wanted collaboration between the treatment levels
- 1.
Rosenvinge JH, Götestam KG. Spiseforstyrrelser – hvordan bør behandlingen organiseres? Tidsskr Nor Lægeforen 2002; 122: 285 – 8. [PubMed]
- 3.
Regjeringens strategiplan mot spiseforstyrrelser. I-0984B. Oslo: Sosial- og helsedepartementet, 2000.
- 4.
Statens helsetilsyn. Alvorlige spiseforstyrrelser. Retningslinjer for behandling i spesialisthelsetjenesten. IK–2714. www.helsetilsynet.no/upload/Publikasjoner/utredningsserien/alvorlige_spiseforstyrrelser_ik-2714.pdf (8.9.2014).
- 5.
Røer A. Spiseforstyrrelser – symptomforståelse og behandlingsstrategier. Oslo: Gyldendal, 2006: 33.
- 6.
Helsedirektoratet. Helsefaglige kodeverk. http://helsedirektoratet.no/kvalitet-planlegging/helsefaglige-kodeverk/icpc/Sider/default.aspx (10.2.2014).
- 7.
Helsedirektoratet. ICD-10. http://helsedirektoratet.no/kvalitet-planlegging/helsefaglige-kodeverk/icd-10/Sider/default.aspx (4.2.2014).
- 8.
Skårderud F. Sterk – svak. Håndboken om spiseforstyrrelser. Oslo: Aschehoug, 2000.
- 9.
Bjørnelv S. Spiseforstyrrelser i allmennpraksis. Tidsskr Nor Lægeforen 2004; 124: 2372 – 5. [PubMed]
- 14.
Ogg EC, Millar HR, Pusztai EE et al. General practice consultation patterns preceding diagnosis of eating disorders. Int J Eat Disord 1997; 22: 89 – 93. [PubMed]