The timing and practice for clamping of the umbilical cord in newborns after birth varies internationally. Modern birth monitoring (2) and baby-friendly initiatives (3) may both have an effect on practice related to clamping of the umbilical cord. Early cord clamping is often defined as clamping within 20 – 30 seconds of birth, while late clamping takes place at least 30 – 60 seconds after birth or when pulsation of the umbilical cord has ceased (1, 4) – (6). In Denmark (7, 8) and Sweden (9) guidelines published in recent years emphasise the benefits of late clamping of the umbilical cord. The most recent international guidelines for resuscitation and stabilisation of newborns recommend delaying umbilical cord clamping for at least one minute, unless the infant requires immediate resuscitation after birth (10). The World Health Organization recommends clamping after 1 – 3 minutes (11), and international federations of midwives and obstetricians recommend delaying umbilical cord clamping until pulsation has ceased (12).
The total blood volume in the foetoplacental unit (foetus, placenta and umbilical cord) amounts to approximately 115 ml of blood per kilo foetal bodyweight. Around full-term, more than one-third of the foetoplacental blood volume is concentrated in the placenta and the umbilical cord (13). During and immediately after birth, a placental transfusion passes to the infant through the umbilical vein. In the case of late clamping, the infant can thus receive a considerable blood transfusion (≈ 25 – 35 ml/kg) from the placenta (14). The hydrostatic pressure gradient is essential for the placental transfusion (15, 16). If the infant is held at the level of the introitus, one-half of the transfusion will take place during the first minute and a complete transfusion within three minutes. If the infant is held 20 – 30 cm below the introitus, transfusion speed will accelerate, but if the infant is held 50 – 60 cm above the introitus no transfusion will take place. A placental transfusion helps optimise the transition from foetal circulation to neonate circulation by adding volume to the pulmonary circulation system, which opens with the child’s first breaths (15).
Late clamping of the umbilical cord reduces the prevalence of anaemia in the neonatal period and improves the iron status of the infant during the first six months of life (1, 4, 17). It has been debated whether an increase in the circulating blood volume causes an increased prevalence of jaundice and/or polycythaemia. In term neonates, however, no (4, 17) or only a slightly increased (1) risk of significant jaundice is reported after late clamping, while marginally elevated bilirubin values have been observed in premature infants, although without any need for phototherapy (6). Symptomatic polycythaemia appears not to increase after late clamping of the umbilical cord (1, 4). In premature infants, late clamping (after 30 – 120 seconds) is associated with a lower prevalence of brain haemorrhage and less need for blood transfusions (6). For the mother, there is no evidence of differences in blood loss, the need for manual removal of the placenta or the use of uterotonics in the case of early vs. late clamping of the umbilical cord (1).
A European survey conducted in 2004 reported large variations with regard to the timing of umbilical cord clamping (18). In many countries, early clamping was most common, while approximately two-thirds of all Norwegian maternity units reported to clamp the umbilical cord after pulsation had ceased (18). The Norwegian Guidelines in Obstetrics from 2008 make no reference to the timing of umbilical cord clamping. They recommend, however, to undertake blood-gas analysis of the umbilical cord in the case of a Caesarean section or operative vaginal delivery, when foetal blood gas has been measured, when the birth has been monitored with the aid of cardiotocography or ST-analysis (STAN) of the foetal electrocardiogram, or when the child is ill at birth (19). The STAN manual initially recommended that the umbilical cord be clamped immediately after birth to achieve a «reliable blood-gas analysis», and that «early clamping of the umbilical cord invariably was preferable» (20). This has later been modified to say that the blood-gas analysis should be undertaken immediately after birth, but preferably before the umbilical cord is clamped (7).
On the basis of our interpretation of the literature, we find many arguments in favour of the benefits of late clamping of the umbilical cord, especially in premature infants. We therefore wished to undertake a survey to describe prevailing routines and practices for clamping of the umbilical cord after birth in Norway.
Material and method
In May 2011, we sent a web-based questionnaire to the heads of department in all maternity units in Norway (N = 52). This contained questions with pre-defined response alternatives as well as open-ended questions (see the appendix). Our questions included the maternity institution’s practice with regard to clamping of the umbilical cord of term and premature neonates, and whether the institutions had written routines for this procedure. We asked for routines on taking blood-gas samples from the umbilical cord, the level at which the infant is held relative to the introitus before umbilical cord clamping and whether the umbilical cord was milked. We also asked for their assessment of clinical advantages and disadvantages of early and late clamping of the umbilical cord.
We provided six response alternatives for the timing of umbilical cord clamping (see the appendix). In this article, we have defined response alternatives 1 (immediately after birth) and 2 (within 30 seconds of birth) as early clamping and response alternatives 3 – 6 (commonly around one, two or three minutes after birth or not until pulsation in the umbilical cord has ceased) as late clamping.
Maternity institutions that failed to reply were reminded via email and telephone. Another doctor or midwife in a managerial position at the same unit was contacted if the head of department failed to respond. The last questionnaire was returned in November 2011. Descriptive results are reported as absolute figures and percentages (%).
Results
We received responses from 50 of the 52 maternity units (96 %). One midwife-led unit and one large obstetric department did not respond. Some respondents failed to answer all questions; this applied to small maternity units in particular.
Table 1 shows what the different institutions reported as their usual practice for the timing of umbilical cord clamping. The responses are reported by large obstetric departments (n = 16), small obstetric departments (n = 24) and freestanding midwife-led maternity units (n = 10). Altogether 19 of the 50 maternity units (38 %) had written routines for the timing of umbilical cord clamping of full-term neonates. Eleven of 16 large obstetric departments (69 %) had written routines, compared to seven of 24 small obstetric departments (29 %) and one in ten midwife-led units (10 %). Only 36 units responded to the question on whether they had written routines for clamping of the umbilical cord in premature infants, and 13 of these 36 (36 %) had such routines.
Table 1
Reported timing of umbilical cord clamping in Norwegian maternity institutions in 2011. Early umbilical cord clamping was defined as immediately or within 30 seconds, late clamping as after at least one minute or when pulsation in the umbilical cord had ceased.
| Early clamping | Late clamping | |
| Full-term | ||
| Large obstetric department (n = 16) | 6 | 10 |
| Small obstetric department (n = 24) | 6 | 18 |
| Midwife-led unit (n = 10) | 0 | 10 |
| Premature | ||
| Large obstetric department (n = 16) | 9 | 7 |
| Small obstetric department (n = 24) | 9 | 15 |
Early umbilical cord clamping of term neonates was practised in nine of 19 maternity units with written routines (47 %) and in three of 31 maternity units with no written routines (10 %). A total of 15 of the 50 maternity units (eight large obstetric departments and seven small obstetric departments) reported to routinely undertake blood-gas analysis of the umbilical cord. Twenty-five units undertook blood-gas analysis of the umbilical only in selected cases. None of the midwife-led units undertook blood-gas analysis of the umbilical cord.
Altogether 27 of 48 respondents reported that the infant commonly is placed on the mother’s abdomen prior to clamping of the umbilical cord. This applied, for example, to all the midwife-led units. 14 maternity units reported that the infant is commonly held below the introitus before umbilical cord clamping. The remaining seven followed no consistent practice. Nine of 19 units with written routines reported to hold the infant below the introitus after birth, compared to five of 29 units without written routines. Four large obstetric departments and two small obstetric departments reported that the umbilical cord was milked in the case of births before the 32nd week. Table 2 presents the respondents’ views on what they saw as advantages of early umbilical cord clamping of term neonates. Table 3 presents arguments pertaining to umbilical cord clamping of premature infants.
Table 2
Responses from Norwegian maternity units (n = 50) to statements about early umbilical clamping (within 30 seconds) of full-term neonates. The statements were presented as pre-defined response alternatives in the questionnaire. See the appendix
| Fully/partly agree | Fully/partly disagree | |
| 1. Can quickly obtain correct blood-gas values from the umbilical cord (the STAN protocol) | ||
| Gynaecological ward | 13 | 3 |
| Maternity ward | 12 | 6 |
| 2. Can quickly resuscitate the newborn child if needed | ||
| Large obstetric department | 11 | 5 |
| Small obstetric department | 18 | 3 |
| Midwife-led unit | 4 | 1 |
| 3. Reduces maternal blood loss during birth | ||
| Large obstetric department | 0 | 15 |
| Small obstetric department | 1 | 20 |
| Midwife-led unit | 0 | 5 |
| 4. Reduces jaundice in the child | ||
| Gynaecological ward | 5 | 11 |
| Maternity ward | 5 | 16 |
| Community unit | 1 | 4 |
| 5. Reduces respiratory problems in the child | ||
| Large obstetric department | 1 | 15 |
| Small obstetric department | 0 | 20 |
| Midwife-led unit | 0 | 5 |
Table 3
Responses from Norwegian large and small obstetric departments (n = 36) to statements about late umbilical cord clamping in premature neonates. The statements were presented as pre-defined response alternatives in the questionnaire. See the appendix
| Fully/partly agree | Fully/partly disagree | |
| 1. Increases jaundice in the child | 18 | 18 |
| 2. Increases the haemoglobin concentration in the child | 31 | 5 |
| 3. Causes circulatory instability in the child | 4 | 32 |
| 4. Increases the risk of brain haemorrhage in the child | 1 | 35 |
| 5. Causes a detrimental delay in the start of resuscitation | 25 | 11 |
Discussion
This survey indicates that there is large variation in local routines and guidelines for umbilical cord clamping in Norwegian maternity institutions. We believe that this is a reflection of clinical practice.
Approximately two-thirds of the responding units had no written guidelines. It may appear that units with written guidelines more frequently practice early umbilical cord clamping than units that have no written guidelines. It appears that late umbilical cord clamping is more common in small obstetric departments, while early clamping is practised more frequently in the large obstetric departments. However, ten of 16 large obstetric departments report to practise late umbilical cord clamping of term neonates, while only seven of these units do so for premature infants.
On questions concerning advantages and disadvantages of late vs. early umbilical cord clamping the answers also varied greatly. The majority of the respondents stated that late umbilical cord clamping resulted in higher haemoglobin values in the premature neonate; this is well documented in randomised studies of both premature (6) and term neonates (1, 4, 17). Answers pertaining to jaundice most likely reflect the fact that the effect of the timing of cord clamping on the prevalence of clinically significant jaundice remains somewhat unclear. However, there appear to be only marginal differences in the prevalence of clinically significant jaundice reported by studies that have compared large groups of infants after late vs. early cord clamping (1, 4, 6, 17).
More than two-thirds of the respondents stated that late umbilical cord clamping may cause a detrimental delay in resuscitation (Table 2, Table 3). In the case of acute, serious asphyxia, in term as well as premature neonates, priority will be given to quick clamping of the umbilical cord in order to initiate resuscitation as quickly as possible. Milking of the umbilical cord will thus provide an opportunity for speeding up the placental transfusion in situations where immediate cord clamping is desirable. In premature infants, studies have shown that milking of the umbilical cord causes higher haemoglobin values, higher blood pressure and less need for transfusions when compared to early clamping without milking of the umbilical cord (21, 22). Corresponding findings of higher haemoglobin values and improved iron status have been observed after milking of the umbilical cord of term neonates (23).
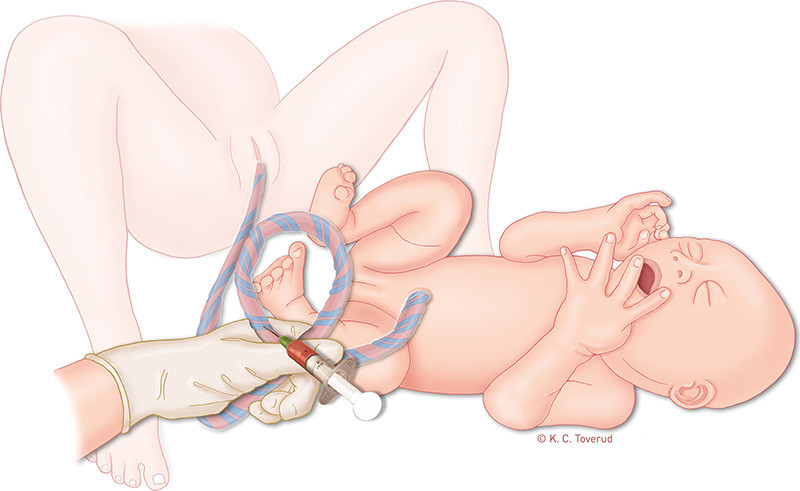
Half of the large obstetric departments and somewhat less than one-third of the midwife-led units reported to undertake blood-gas analysis from the umbilical cord as a matter of routine for all births (Figure 1). Respondents in 13 of the 16 large obstetric departments responded that one advantage of early umbilical cord clamping was the opportunity it provided to obtain «correct blood-gas values» (Table 2). In our experience it has become common, most likely following the introduction of the STAN methodology (2, 20), to immediately clamp a section of the umbilical cord to obtain a «correct» blood-gas sample that reflects the metabolic condition of the foetus (24, 25). The pH value and the base excess will fall slightly if the blood-gas analysis is not undertaken until late cord clamping has been performed, and the changes can be observed after no more than 45 seconds (25, 26). Experience and clinical studies show, however, that it is practically feasible to undertake an early blood-gas analysis from the umbilical cord without having to clamp it first (Figure 1). In this manner, the advantages of obtaining a placental transfusion with late cord clamping (27) can be combined with an early blood-gas analysis (9, 17). Some Norwegian hospitals have already recommended this procedure (Ragnhild Støen, St. Olavs Hospital, personal communication).
The objective of this survey was to identify practice in Norwegian maternity wards. We therefore asked the heads of units to describe the routines and practices in their unit. We cannot exclude, however, that attitudes, professional backgrounds (doctor/midwife) and personal preferences are reflected in the responses. Nor did we collect written routines from the units that stated that they had such. The failure of some units to respond to all the questions is another weakness. This could be because as a main rule, premature births take place in large maternity units, and such questions may therefore be of less relevance for the small units.
There is no generally agreed definition of what should be considered late and early umbilical cord clamping. In our questionnaire we defined early clamping as taking place within 30 seconds and late clamping if it was undertaken after one minute or later. No respondents used the free-text field to report umbilical cord clamping after 30 – 60 seconds, but we cannot exclude the possibility that some follow this routine.
A strength of our study is its high response rate. We therefore believe that the responses represent a real variation in medical practice with regard to a procedure which is undertaken approximately 60 000 times annually in the Norwegian health services.
Conclusion
This survey reveals large variation in reported local routines and guidelines for umbilical cord clamping in Norwegian maternity institutions. We believe that there is a need for establishing national professional guidelines in this area, corresponding to what has already been done in Sweden and Denmark (7, 9).
MAIN MESSAGE
Less than half of all Norwegian maternity units had written routines for clamping of the umbilical cord.
The timing of the clamping and practices for holding the child below the introitus appear to vary greatly.
There is a need for national guidelines for clamping of the umbilical cord in neonates.
- 1.
McDonald SJ, Middleton P. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev 2008; 2: CD004074. [PubMed]
- 2.
Bergsjø P. [Unnecessary umbilical cord blood tests]. Tidsskr Nor Lægeforen 2007; 127: 204. [PubMed]
- 3.
Fugelseth D, Lindemann R. [Perinatal care yesterday, today, tomorrow--which way does the pendulum swing?]. Tidsskr Nor Lægeforen 1994; 114: 57 – 60. [PubMed]
- 6.
Rabe H, Diaz-Rossello JL, Duley L et al. Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database Syst Rev 2012; 8: CD003248. [PubMed]
- 7.
Barfoed A, Christensen AC, Steen Hansen C et al. Afnavling af det meget præmature, det præmature og det mature barn, 2010. Dansk Selskab for Obstetrik og Gynekologi. www.dsog.dk/sandbjerg/ (2.2.2013).
- 8.
Møller NK, Weber T. Tidlig eller sen afnavling af det mature, det præmature og det meget præmature barn. Ugeskr Læger 2008; 170: 1919 – 21. [PubMed]
- 9.
Wiklund I, Nordström L, Norman M. Vårdprogram för avnavling av nyfödda barn. Läkartidningen 2008; 105: 3208 – 10. [PubMed]
- 11.
Abalos E. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes: RHL commentary (last revised: 2 March 2009). The WHO Reproductive Health Library. Genève: World Health Organization, 2009.
- 14.
Moss AJ, Monset-Couchard M. Placental transfusion: early versus late clamping of the umbilical cord. Pediatrics 1967; 40: 109 – 26. [PubMed]
- 19.
Veileder i fødselshjelp. Oslo: Norsk gynekologisk forening, 2008.
- 20.
Sundström AK, Rosén D, Rosen KG. Opplæringsserien «Fosterovervåking». Göteborg: Neoventa Medical AB, 2000.
- 22.
Erickson-Owens DA, Mercer JS, Oh W. Umbilical cord milking in term infants delivered by cesarean section: a randomized controlled trial. J Perinatol 2012; 32: 580 – 4.
- 23.
Upadhyay A, Gothwal S, Parihar R et al. Effect of umbilical cord milking in term and near term infants: randomized control trial. Am J Obstet Gynecol 2013; 208: 120.e1 – 6.
Rutinemessig blodgass fra navlesnorer som fortsatt har forbindelse med barnets blodomkrets (figur 1, side 2371, Tidsskr Nor Legeforen nr. 22, 2013; 133).
Potensielle og uheldige komplikasjoner som ikke nevnes er:
1. Risiko for direkte inokulasjon av barnets blodbane med bakterie som dekker navlnesnoren.
2. Risiko for luftemboli - som har lite konsekvens jo mindre den strømmer gjennom foramen ovale og retter seg mot barnets cerebral cortex 1,2.
3. Risiko for at det dannes ustabile tromber på den intralumenale siden av navlevenen som potesielt kan emboliseres ved, for eksempel, kraftig forandringer i den venøse strømmen i forbindelse med pustebevegelser 3.
Man skal vente lenge for at en slik komplikasjon nevnt over oppstår i en prospektiv randomisert studie. Imidlertid er ett tilfelle av unødvendig og potensiell permanent skade hos et frisk nyfødt ikke verdt teknikken nevnt i artikkelen. At "enkelte norske sykehus allerede har anbefalt" 4 teknikken som metoden for rutinemessig sikring av umbilical syre-base betyr ikke at teknikken aldri kan påføre skade.
De barn helsepersonell trenger å sikre syre-base status er disse som har enten manglende pulsasjon i navlen fordi de har opplevd sirkulatorisk kollaps under fødsel, eller barn hvor det klinisk tilstanden tilsier at å vente i 3 minutter vil drøye nødvendig resucitative tiltak. Enten melker man navlesnoren i disse tilfeller, eller så klemmer man av navlesnoren tidlig etter forløsningen.
Nyfødte som egner seg til teknikken beskrevet i artikkelen har, i de fleste tilfeller, en Apgar score etter ett minutt som tilsier at en acidose med behandlingsmessig betydning er lite sannsynlig. Friske barn er mest utsatt for potensielle skadevirkninger ved anvending av teknikken beskrevet.
Blodgass fra navlesnoren har derimot ingen behandlingsmessige konsekvens men tas med tanke på "kvalitetssikring" av fødselshjelpen (som er viktig), og det tas av rettslige hensyn (å forsvare fødselshjelpen er nødvendig fra tid til annen). Disse hensyn må vurderes opp mot å tillate at barnet forsyner seg med alt det gjenværende blodet i navlesnoren - noe som man vet er helsefremmende. Metoden beskrevet i artikkelen er et bra kompromiss. Imidlertid er ikke sikkerhet ved metoden kritisk vurdert og heller ikke jeg som leser overbevist.
1. European Journal of Pediatrics 25. IV. 1979, Volume 131, Issue 1, pp 71-73
2. Paediatr Child Health. 2009 October; 14(8): 539-541.
3. Am J Perinatol. 2010 Mar;27(3):251-6.
4. Tidsskr Nor Legeforen nr. 22, 2013; 133: s.2369-2372
Takk for kommentar til vår artikkel. Metoden for blodprøvetaking fra intakt navlesnor er beskrevet i det svenske "Vårdprogram för avnavling av nyfödde barn" publisert i 2008 (1). Siden den gang har metoden vært i bruk i Sverige, inkludert i en stor randomisert studie som er publisert på dette temaet (2). Man har fra Sverige over 5 års erfaring med denne metoden og ingen av de komplikasjoner som dr. Alnæs-Katjavivi nevner har vært registrert eller medført en endring av praksis i Sverige (personlig kommunikasjon Magnus Domellöf, Umeå, Sverige). Samme metode anbefales også brukt av Dansk Selskab for Obstetrik og Gynækologi (3).
De to første referansene til dr. Alnæs-Katjavivi omhandler komplikasjoner ved bruk av navlevenekateter. Det er naturligvis en helt annen risiko for komplikasjoner når man setter inn et kateter og infunderer væske enn når man bruker en blodgass-sprøyte til å ta ut blod. Den tredje referansen omhandler føtal placental vaskulopati hos to premature barn der navlesnoren var normal. Det er vanskelig å se at disse tre referansene er gode argumenter mot blodprøvetaking fra intakt navlesnor. Melking av navlesnoren, som Dr. Alnær Katjavivi også nevner, burde teoretisk også medføre risiko for embolisering av "ustabile tromber", men dette er ikke erkjent som en komplikasjon ved denne metoden (4, 5).
Vi er enige i at en blodgass fra navlesnoren sjelden har behandlingsmessig konsekvens, men det er et faktum at den ofte tas allikevel. I vår artikkel argumenterer vi ikke for at man i større grad skal ta blodgass fra navlesnor. Derimot fremhever vi at det er sterke holdepunker for at sen avnavling er gunstig både for premature og fullbårne barn. Ved en asfyksi skriver vi også at rask avnavling prioriteres. Det er fysiologiske holdepunkter for at en føtal asfyksi medfører en intrauterin overføring av blod fra placental til føtal sirkulasjon noe som dermed skulle gi mindre behov for sen avnavling (5). I andre tilfeller der man ønsker å kombinere en tidlig blodgass med sen avnavling mener vi at metoden beskrevet i vår artikkel, og som har vært i bruk i over 5 år i Sverige, er trygg.
Referanser:
1. Wiklund I, Nordstrøm L, Norman, M. Vårdprogram för avnavling av nyfödda barn. Läkartidningen 2008; 105: 3208-10.
2. Andersson O, Hellstrom-Westas L, Andersson D et al. Effect of delayed versus early umbilical cord clamping on neonatal outcomes and iron status at 4 months: a randomised controlled trial. BMJ 2011; 343: d7157.
3. Barfoed A, Christensen AC, Steen Hansen C et al. Afnavling af det meget præmature, det præmature og det mature barn, 2010. Dansk Selskab for Obstetrik og Gynekologi. http://www.dsog.dk/sandbjerg/ (09.12.13).
4. Upadhyay A, Gothwal S, Parihar R, et al. Effect of umbilcal cord milking in term and near term infants: randomized controlled trial. Am J Obstet Gynecol 2013; 208: 120.e 1-6.
5. Niermeyer S, Velaphi S. Promoting physiologic transition at birth: Re-examining resuscitation and the timing of cord clamping. Sem Fetal Neonat Med 2013; 18: 385-392.
Takk for kommentar til vår artikkel. Metoden for blodprøvetaking fra intakt navlesnor er beskrevet i det svenske "Vårdprogram för avnavling av nyfödde barn" publisert i 2008 (1). Siden den gang har metoden vært i bruk i Sverige, inkludert i en stor randomisert studie som er publisert på dette temaet (2). Man har fra Sverige over 5 års erfaring med denne metoden og ingen av de komplikasjoner som dr. Alnæs-Katjavivi nevner har vært registrert eller medført en endring av praksis i Sverige (personlig kommunikasjon Magnus Domellöf, Umeå, Sverige). Samme metode anbefales også brukt av Dansk Selskab for Obstetrik og Gynækologi (3).
De to første referansene til dr. Alnæs-Katjavivi omhandler komplikasjoner ved bruk av navlevenekateter. Det er naturligvis en helt annen risiko for komplikasjoner når man setter inn et kateter og infunderer væske enn når man bruker en blodgasssprøyte til å ta ut blod. Den tredje referansen omhandler føtal placental vaskulopati hos to premature barn der navlesnoren var normal. Det er vanskelig å se at disse tre referansene er gode argumenter mot blodprøvetaking fra intakt navlesnor. Melking av navlesnoren, som Dr. Alnær Katjavivi også nevner, burde teoretisk også medføre risiko for embolisering av "ustabile tromber", men dette er ikke erkjent som en komplikasjon ved denne metoden (4, 5).
Blodgass fra navlesnoren tas først og fremst for kvalitetssikring av fødselshjelpen. Det diskuteres om slike prøver skal tas ved alle fødsler eller selektivt. Denne diskusjon er utenfor rammen for vår artikkel. Derimot fremhever vi at det er sterke holdepunker for at sen avnavling er gunstig både for premature og fullbårne barn. Ved en asfyksi skriver vi også at rask avnavling prioriteres. Det er fysiologiske holdepunkter for at en føtal asfyksi medfører en intrauterin overføring av blod fra placental til føtal sirkulasjon noe som dermed skulle gi mindre behov for sen avnavling (5). I andre tilfeller der man ønsker å kombinere en tidlig blodgass med sen avnavling mener vi at metoden beskrevet i vår artikkel, og som har vært i bruk i over fem år i Sverige, er trygg.
Referanser:
1. Wiklund I, Nordstrøm L, Norman, M. Vårdprogram för avnavling av nyfödda barn. Läkartidningen 2008; 105: 3208-10.
2. Andersson O, Hellstrom-Westas L, Andersson D et al. Effect of delayed versus early umbilical cord clamping on neonatal outcomes and iron status at 4 months: a randomised controlled trial. BMJ 2011; 343: d7157.
3. Barfoed A, Christensen AC, Steen Hansen C et al. Afnavling af det meget præmature, det præmature og det mature barn, 2010. Dansk Selskab for Obstetrik og Gynekologi. http://www.dsog.dk/sandbjerg/ (09.12.13).
4. Upadhyay A, Gothwal S, Parihar R, et al. Effect of umbilcal cord milking in term and near term infants: randomized controlled trial. Am J Obstet Gynecol 2013; 208: 120.e 1-6.
5. Niermeyer S, Velaphi S. Promoting physiologic transition at birth: Re-examining resuscitation and the timing of cord clamping. Sem Fetal Neonat Med 2013; 18: 385-392.
I artikkelen til Lundberg og medarbeidere etterlyses nasjonale retningslinjer om avnavling (1). Det er nettopp utarbeidet en prosedyre om avnavling av nyfødte som er publisert i Kunnskapssenterets prosedyrebank (2).
Prosedyren fyller kvalitetskravene til gode fagprosedyrer og omhandler mange aspekter rundt avnavling, inkludert premature og resuscitering. Den inneholder en fyldig metoderapport og en vurdering av referanser.
Litteratur
1. Lundberg C, Øian P, Klingenberg C. Avnavling ved fødsel – praksis ved norske fødeinstitusjoner. Tidsskr Nor Legeforen 2013; 133: 2369-72.
2. http://helsebiblioteket.no/microsite/fagprosedyrer/fagprosedyrer/avnavling-av-nyfødte (6.3.2014).