Are the Norwegian guidelines for ultrasound in prenatal diagnosis followed?
The Act relating to the application of biotechnology in human medicine (the Biotechnology Act) came into force on 1 January 2004. The Act defines prenatal diagnosis as the examination of fetal cells, a fetus or a pregnant woman to obtain information about the genetic constitution of the fetus or to detect or exclude a disease or abnormality of the fetus (1).
In Norway, five fetal medicine centres are approved to perform ultrasound as part of prenatal diagnosis in the first trimester. The indications are described in the 2004 guidelines for the use of ultrasound during pregnancy, and are specified in the leaflet Information to pregnant women on prenatal diagnosis, issued in 2005 (Box 1 (2, 3).
Indications for prenatal diagnosis
Prenatal diagnosis is regulated by the Biotechnology Act (1). Ultrasound with measurement of nuchal translucency (NT) and a combined ultrasound and blood test (CUB test) are considered as prenatal diagnosis. These are the indications for prenatal diagnosis as described in the leaflet Information to pregnant women on prenatal diagnosis (3).
Pregnant women who are 38 years or older at the expected time of delivery
-
Pregnant women in cases where the woman herself or her partner:
has previously had a child or a fetus with a serious disease or a developmental disorder (e.g. chromosome aberration)
are at an increased risk of serious illness in the fetus and this condition can be ascertained (e.g. certain hereditary diseases)
use medications that can harm the fetus (e.g. for epilepsy in the mother)
Pregnant women in whom suspicion of a developmental disorder have been raised by ultrasound examination
In certain cases, pregnant women who are in a difficult life situation and who are convinced that they will be unable to cope with the extra strain involved in having a sick or disabled child.
Ultrasound during the 11th to13th weeks of gestation with measurement of nuchal translucency (NT) and a combined ultrasound and maternal blood test (CUB test) are considered prenatal diagnostic examinations. Increased NT is caused by an oedema in the fetal neck, and the blood samples taken from the mother measure the concentration of human chorionic gonadotropin (HCG) and pregnancy-associated plasma protein A (PAPP-A). The CUB test predicts the likelihood of an aneuploid fetus and fetal malformations (4) – (6), and the method was introduced to reduce risks associated with invasive procedures (7). Ultrasound as part of prenatal diagnosis can only be performed after prior genetic counselling. Ultrasound performed as part of regular antenatal care, i.e. the routine examination during the second trimester, and examinations due to medical indications are not considered prenatal diagnosis and not regulated by the Biotechnology Act (1, 2).
The Biotechnology Act is currently undergoing revision, and is discussed in public bodies as well as in the media (8) – (10). The Act has been characterised as imprecise, and in 2004 it was predicted that the Act would not be complied with in clinical practice (11). A main problem with this Act is its distinction between ultrasound as part of regular antenatal care and ultrasound as prenatal diagnosis. Other controversial issues include whether «anxiety» constitutes an indication for prenatal diagnosis, how the age criterion should be interpreted, and how vague indications, such as «a difficult life situation», should be dealt with.
The purpose of this study was to investigate whether the doctors complied with the guidelines of the Biotechnology Act when assessing constructed case histories of women who asked for the 11th to 13th week ultrasound examination.
Material and methods
We constructed six case histories of women who wished to have ultrasound examination during the 11th to 13th week (Box 2), and linked three sets of questions to the case histories, which were adapted to the various groups of respondents. The questions had pre-defined response alternatives. The guidelines for use of ultrasound during pregnancy were assumed to be known, and were not presented in association with the questionnaire. The headlines of the case histories (Box 2) were not included in the questionnaire. The data were collected in the period from October to December 2011.
Case histories that were submitted to gynaecologists in private practice, doctors at fetal medicine centres and consultants in the Directorate of Health
Case history no. 1 – Interpretation of the age criterion in the regulations of the Biotechnology Act The woman is pregnant in week 8 of gestation. She will give birth for the third time, is previously healthy and with no particular diseases in her family history. She turned 37 two months ago, and because of her age, she wishes for early ultrasound to exclude chromosome aberration in the fetus.
Case history no. 2 – Will a colleague be treated differently from other pregnant women? The woman is pregnant in week 8 of gestation. She is a trainee doctor in the Department of Gynaecology, pregnant for the first time and has no particular risk factors associated with her pregnancy.
Case history no. 3 – Varying practices in European countries and their significance for Norwegian practice A 35-year-old British woman is pregnant with her third child in gestational week 9. She has lived in Norway for three years. During her two previous, normal pregnancies she underwent screening for trisomy 21 in her home country. She now wishes to have early ultrasound for her current pregnancy. The woman says that she will travel to the UK for an examination if she cannot have it here.
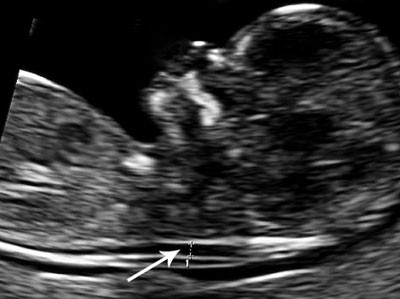
Case history no. 4 – Incidental finding during an examination on the basis of a clinical indication The woman is 35 years old, gravida 7, para 3. She has previously had three uncomplicated pregnancies and deliveries, one induced abortion and two spontaneous abortions. She has undergone early ultrasonography with a private gynaecologist because of vaginal haemorrhaging. During the examination, a vital fetus corresponding to gestational week 11 was observed. The gynaecologists had the impression of a slightly increased nuchal translucency, and reported this. The woman was frightened and requested a referral to a fetal medicine centre. On the basis of the enclosed image, the hospital doctor claimed that the nuchal translucency appeared normal.
Case history no. 5 – Anxiety as an indication of prenatal diagnosis The woman is 24 years old and pregnant for the first time in gestational week 7. She has suffered from musculo-skeletal pains since age 19, and has been diagnosed with fibromyalgia. She works in a 70 % position in a bakery and is on 30 % disability benefit. She uses no regular medications, but takes paracetamol and ibuprofen for her pains as needed. Four years ago, her sister gave birth to a boy with trisomy 21. She is now very worried about having a sick child herself. The doctor has explained that her sister’s child does not increase her risk of having a child with chromosome aberration, and that the drugs she has been using are not harmful. This information has failed to calm her down, and she wishes to have a referral for prenatal diagnosis.
Case history no. 6 – A difficult life situation as an indication for prenatal diagnosis The woman is 31 years and pregnant with her second child in gestational week 6. The couple have a six-year-old daughter. Her husband is unemployed. She works as an assistant nurse in a nursing home, with frequent night shifts. She is overweight and uses Selo-Zok 50 mg × 1 for hypertension. In addition she uses Paralgin forte on a daily basis for tension headache. The couple keenly want another child, but believe that they will be unable to cope with the strains involved in having a sick child, either practically or financially. They are particularly worried about having a disabled child, and are concerned that her use of medications may have caused harm. The couple want an early ultrasonography to exclude abnormalities in the fetus.
The questionnaires were sent to the heads of section in all Norwegian fetal medicine centres (Tromsø, Trondheim, Bergen, Stavanger and Oslo). The section heads distributed the questionnaire to all doctors who assess referrals at their centre. The case histories were presented as referrals, and the doctors were asked to answer the questions as though the referral applied to a real patient. The questionnaires were completed anonymously.
The questionnaire was also distributed to all specialists in obstetrics and gynaecology who were members of the Norwegian Medical Association at the time, and who had reported to be private practitioners of their speciality. The gynaecologists were asked to respond to the questions on the basis of what they would have done if this had been a real patient. The questionnaires were completed anonymously. A questionnaire was also sent to a contact person in the Department of Biotechnology and Health Law in the Directorate of Health. The contact person distributed it further to lawyers and consultants working with legal matters pertaining to health in the same department.
For the first three case histories, the doctors were asked whether they would have offered the woman an ultrasound examination, and if so, of what kind. The respondents in the Directorate of Health were asked whether the woman was entitled to prenatal diagnosis according to the guidelines, and in case history no. 2 they were asked whether in their opinion, doctors who perform prenatal diagnosis on the basis of the problem presented, are violating the provisions of the Act. All respondents were asked to interpret the age criterion, and all the doctors were asked whether they apply the age limit liberally.
For the three final case histories, the gynaecologists in private practice were asked whether they would have referred the woman to a fetal medicine centre. In case history no. 4 we asked whether in that case they would have measured NT, and for case history nos. 5 and 6 they were asked to state the indication for their ultrasound examination. Doctors at the fetal medicine centres were asked to state what kind of examination they would have offered the woman, whether they were of the opinion that she was entitled to prenatal diagnosis according to the guidelines, and if so, on what indication. The respondents in the Directorate of Health were asked whether the women were entitled to prenatal diagnosis according to the guidelines. Irrespective of the case histories, all respondents were asked how they relate to anxiety as an indication for prenatal diagnosis.
Statistics
Any differences in responses from the various centres and groups of professions, as well as gender differences, were investigated by Fisher’s exact test and chi-square testing. The impact of the respondents’ age was investigated with logistic regression, using categorical answers as the dependent variable and age as the explanatory variable. The data were analysed with the statistics application PASW 18.0.
Results
We received responses from 22 (81 %) of 27 doctors who assess referrals to prenatal diagnosis at the approved fetal medicine centres. In Tromsø, Trondheim and Bergen referrals are assessed exclusively by specialists in obstetrics and gynaecology. In Stavanger and Oslo, referrals are also assessed by specialists in medical genetics. Altogether 19 of the respondents were specialists in obstetrics and gynaecology, and three were specialists in medical genetics. Their average age was 51 years, 14 (64 %) were men, and 14 (64 %) also had international approval from the Fetal Medicine Foundation (FMF) to measure NT (12). There were no significant differences in how the referrals were assessed by the various fetal medicine centres, by the gynaecologists or the geneticists, by men or women, or by various age groups.
We received responses from 64 (49 %) of 130 gynaecologists in private practice. Their average age was 56 years, and 33 (52 %) were women. There were no significant differences related to gender or age in how the private gynaecologists assessed the age criterion and measurement of NT, although more women than men would refer the patient to prenatal diagnosis with anxiety as an indication.
Of the 12 possible respondents in the Directorate of Health, we received responses from five (42 %). Four of the respondents were lawyers and one was a consultant.
For the first case history (interpretation of the age criterion), 29 (45 %) of the private gynaecologists would have performed a preliminary ultrasound and made a referral in case of suspicion, and 11 (17 %) would have measured NT themselves. Altogether 14 (64 %) of the doctors at the fetal medicine centres would have performed measurement of nuchal translucency (NT) or a CUB test. All the respondents in the Directorate of Health stated that according to the guidelines, the woman in this case history was not entitled to prenatal diagnosis.
All the doctors at the fetal medicine centres were of the opinion that the age limit of 38 years applies to the expected time of delivery, while four (6 %) of the private gynaecologists believed that the woman should have turned 38 at the time of the examination. Only 29 (34 %) of all the doctors responded that they enforced the age limit of 38 years rigidly.
For the second case history (colleague), 45 (70 %) of the private gynaecologists would have performed a preliminary ultrasound examination and made a referral in case of suspicion, while 12 (19 %) would have measured NT themselves. In the fetal medicine centres, altogether 13 (59 %) would have measured the nuchal translucency NT while one (5 %) would have performed a CUB test. All our respondents in the Directorate of Health stated that this woman was not entitled to prenatal diagnosis, and four (80 %) were of the opinion that doctors who perform prenatal diagnosis in this situation are breaking the law.
For the third case history (foreign woman), altogether 30 (47 %) of the private gynaecologists would have performed a preliminary ultrasound examination and made a referral in case of suspicion, and 13 (20 %) would have measured NT themselves. In the fetal medicine centres, seven (32 %) would have offered prenatal diagnosis. All our respondents in the Directorate of Health stated that the woman was not entitled to prenatal diagnosis.
For the fourth case history (incidental finding), altogether 33 (52 %) of the private gynaecologists responded that they would have referred the woman only if they themselves had measured an increased NT, while 25 (39 %) would have made a referral on the basis of their impression without making any measurement. Altogether 21 (95 %) of the doctors at the fetal medicine centres would have offered measurement of NT or a CUB test), while 18 (80 %) believed that the woman was entitled to prenatal diagnosis according to the guidelines. Four (80 %) of the respondents in the Directorate of Health stated that the woman was entitled to prenatal diagnosis according to the guidelines.
For the fifth case history (anxiety), altogether 43 (67 %) of the private gynaecologists would have referred the woman to a fetal medicine centre. 34 (53 %) would have used anxiety as an indication. 16 (73 %) of the doctors at the fetal medicine centres would have offered measurement of NT or a CUB test. Nine (41 %) claimed that she was entitled to prenatal diagnosis according to the guidelines, and nine (41 %) were of the opinion that anxiety was an indication. All the respondents in the Directorate of Health agreed that she was not entitled to prenatal diagnosis.
Table 1 shows how the respondents relate to anxiety as an indication for prenatal diagnosis. In the group of private gynaecologists there were significantly more women (27/33 vs. 15/27, p = 0.03) who responded that they have made referrals to prenatal diagnosis with anxiety as an indication.
Table 1:
The respondents’ answers to the questions pertaining to anxiety as an indication for prenatal diagnosis
| Have you made referrals to prenatal diagnosis on the indication of anxiety? |
In your opinion, is anxiety an indication for prenatal diagnosis? |
||||||
| Yes |
No |
No response |
Yes |
No |
No response |
||
| Gynaecologists in private practice |
43 |
20 |
1 |
||||
| Doctors at fetal medicine centres |
16 |
5 |
1 |
||||
| Lawyers and consultants in the Directorate of Health |
5 |
||||||
For the sixth case history (difficult life situation), 30 (47 %) of the private gynaecologists would have made a referral to prenatal diagnosis, and seven (11 %) claimed that a difficult life situation was an indication. 13 (59 %) of the doctors at the fetal medicine centres would have offered measurement of NT or a CUB test. Eight (36 %) were of the opinion that a difficult life situation is an indication. Ten (45 %) replied that she was entitled to prenatal diagnosis according to the guidelines. Four (80 %) of the respondents in the Directorate of Health stated that she was entitled to prenatal diagnosis.
Discussion
The results show that the guidelines for the 11th to 13th week ultrasound scan were not uniformly interpreted and followed when the doctors assessed the constructed case histories. The age criterion was not followed, and women were granted prenatal diagnosis without an indication. Many of the private gynaecologists answered that they would have measured the NT themselves, even though they are not allowed to perform prenatal diagnosis. Distinguishing between ultrasound in routine antenatal care and ultrasound as prenatal diagnosis is difficult.
The results indicate attitudes to constructed case histories, and the question of what kind of examinations the women would have been offered in real life remains unanswered. We nevertheless assume that there is a correlation between how case histories are addressed and clinical practice. The questions pertaining to the age limit and to using anxiety as an indication for prenatal diagnosis were also asked independently of the case histories. These results indicate that many doctors do not enforce the age limit rigidly, and that women are offered prenatal diagnosis on the basis of anxiety as an indication in daily practice as well.
The first case history illustrates the problems associated with the interpretation of the age criterion. Women aged 37 and 38 have approximately an equal risk of having a child with a chromosome aberration (5). There is no good reason why only women aged 38 should be offered prenatal diagnosis. In this case history, the woman was 37 years and two months old at the time of the examination. She would have been 37 years and nine months old at the expected time of delivery. The regulations do not specify whether the age criterion applies to the time of the examination or the expected time of delivery (2). The information leaflet on prenatal diagnosis, which is supplied to pregnant women, and also the guidelines issued by the Norwegian Gynaecological Association, specify the age limit as 38 years at the expected time of delivery (3, 13). All the doctors at the fetal medicine centres were aware of this specification. However, only a minority of the doctors responded that they adhere rigidly to the age criterion, and women who are approaching 38 years at the expected time of delivery are often offered prenatal diagnosis.
More than half of the doctors at the fetal medicine centres would have offered their colleague in case history no. 2 an ultrasound examination including prenatal diagnosis. Four of five respondents in the Directorate of Health were of the opinion that these doctors are violating Norwegian law. Only one of the doctors would have offered this colleague a CUB test, the others would have performed ultrasound with measurement of NT. It may appear that the doctors perceive this violation of the regulations to be less serious if the blood tests are omitted.
Women from countries where screening for trisomy 21 is implemented may find it difficult to accept the strict Norwegian regulations. If their request is rejected in Norway, they travel to their home country to be examined, and many of them come back with test results that Norwegian doctors must consider following up. This may be the reason why one-third of the doctors at the fetal medicine centres would grant prenatal diagnosis to the woman in case history no. 3.
The fourth case history highlights the distinction between ultrasound as part of routine antenatal care and ultrasound as an element of prenatal diagnosis. If suspicion of an abnormality is raised by ultrasound in routine antenatal care, the woman should be referred. Increased NT is the most important marker for chromosome aberration, but measurement of NT is defined as prenatal diagnosis. According to the guidelines, a referral should therefore be based on an impression of increased NT, and not on an accurate measurement. Nevertheless 33 (52 %) of the private gynaecologists reported that they would make a referral only if their own measurement had revealed increased NT. The distinction between examinations based on medical indications on the one hand and prenatal diagnosis on the other is not uniformly practised. One reason might be that Norwegian doctors feel insecure about whether or not they are breaking the law by measuring the NT.
A «Perspectives» article published in the Journal of the Norwegian Medical Association in 2009 argues that good, quality-controlled information is a prerequisite for reflective and responsible pregnant women to make informed and autonomous decisions (14). The distinction between ultrasound as part of routine antenatal care and ultrasound as prenatal diagnosis renders this goal difficult. While strict requirements apply to information and guidance prior to a prenatal diagnostic examination, these obligations do not apply to examinations on the basis of a medical indication.
According to the guidelines, anxiety constitutes a medical indication for ultrasound in regular antenatal care, but not for prenatal diagnosis. The respondents in the Directorate of Health were of the opinion that the woman in case history no. 5 was not entitled to prenatal diagnosis. In practice, many doctors at the fetal medicine centres would nevertheless offer this, with anxiety as an indication. Thus, anxiety functions as a back door to prenatal diagnosis. Our results indicate that Norwegian doctors are uncertain as to whether anxiety is an indication for prenatal diagnosis. We can also see that there is a difference between the number of doctors (n = 16) at the fetal medicine centres who granted prenatal diagnosis, and the number of doctors (n = 9) who claimed that the same woman was entitled to prenatal diagnosis according to the guidelines. This indicates that many doctors would choose to grant prenatal diagnosis in spite of their opinion that according to the guidelines the woman has no such entitlement.
Defining what constitutes «a difficult life situation» is complicated. Should the couple themselves and/or the referring doctor assess this, or should the doctor at the fetal medicine centre make the decision? Subjective assessments form the basis, and the case history illustrates the extent to which the outcomes may vary. The respondents in the Directorate of Health fairly unanimously agreed that this woman was entitled to prenatal diagnosis, but fewer than half of the doctors at the fetal medicine centres concurred. Our results indicate that doctors will be more likely than the respondents in the Directorate of Health to accept prenatal ultrasound on the indication of «anxiety», while with regard to «a difficult life situation» the opposite is the case.
It has been claimed that it is easier to have prenatal diagnosis performed in Central and Eastern Norway than in other regions of the country. A report from the Directorate of Health published in 2011 showed an unbalanced distribution between the counties, and the number of prenatal diagnostic examinations seen in relation to the number of pregnant women older than 38 in the various counties confirms this. In 2009, this ratio was 2.4 in Sør-Trøndelag, 1.8 in Oslo, 1.1 in Rogaland and 0.6 in Aust-Agder (8). Our study did not reveal any differences in the assessments made by the various fetal medicine centres.
We conclude that many doctors failed to comply with the regulations of the Biotechnology Act when assessing the constructed case histories. There was also disagreement regarding the interpretation of the guidelines between the doctors on the one hand and the respondents in the Directorate of Health on the other.
Tabell
| Main message |
|
- 1.
Lov om humanmedisinsk bruk av bioteknologi (bioteknologiloven). www.lovdata.no/all/hl-20031205-100.html (23.3.2012).
- 2.
Veiledende retningslinjer for bruk av ultralyd i svangerskapet. Bruk av ultralyd i den alminnelige svangerskapsomsorgen og i forbindelse med fosterdiagnostikk. IS-23/2004. Oslo: Helsedirektoratet, 2004. www.helsedirektoratet.no/publikasjoner/veiledende-retningslinjer-for-bruk-av-ultralyd-i-svangerskapet/Sider/default.aspx (23.3.2012).
- 3.
Informasjon til gravide om fosterdiagnostikk. IS-1313. Oslo: Helsedirektoratet, 2005. http://helsedirektoratet.no/publikasjoner/informasjon-til-gravide-om-fosterdiagnostikk/Sider/default.aspx (23.3.2012).
- 5.
Nicolaides KH, Sebire NJ, Snijders RJM. The 11 – 14 week scan: the diagnosis of fetal abnormalities. New York, NY: Parthenon, 1999.
- 6.
Snijders RJ, Sebire NJ, Nayar R et al. Increased nuchal translucency in trisomy 13 fetuses at 10 – 14 weeks of gestation. Am J Med Genet 1999; 86: 205 – 7. [PubMed]
- 8.
Evaluering av bioteknologiloven – status og utvikling på fagområdene som reguleres av loven. IS-1897. Oslo: Helsedirektoratet, 2011. www.helsedirektoratet.no/publikasjoner/evaluering-av-bioteknologiloven-status-og-utvikling-pa-fagomradene-som-reguleres-av-loven/Sider/evaluering-av-bioteknologiloven-status-og-utvikling-pa-fagomradene-som-reguleres-av-loven.aspx (23.3.2012).
- 9.
Lauvrak V, Norderhaug IN, Hagen G et al. Tidlig ultralyd i svangerskapsomsorgen. Oslo: Kunnskapssenteret, 2012. www.kunnskapssenteret.no/Nyheter/Ingen+dokumentasjon+for+en+helsemessig+gevinst+av+tidlig+ultralyd.14398.cms (23.3.2012).
- 10.
Fredrikstad A. Tom har Downs: – Alle har rett til å leve. TV2-nyhetene 14.1. 2012. www.tv2.no/nyheter/innenriks/tom-har-downs-alle-har-rett-til-aa-leve-3682994.html (23.3.2012).
- 11.
Salvesen KÅ. Ultrauklar bioteknologilov. Tidsskr Nor Lægeforen 2004; 124: 819 – 21. [PubMed]
- 12.
Fetal Medicine Foundation. www.fetalmedicine.com/fmf/ (23.3.2012).
- 13.
Norsk gynekologisk forening. Veileder i fødselshjelp 2008. www.legeforeningen.no/id/131701.0 (23.3.2012).
- 14.
Solberg B. Informerte valg - viktig også for norske gravide. Tidsskr Nor Lægeforen 2009; 129: 1346-8. [PubMed]