The main goal of the Norwegian hospital reform of 2002 was to improve accessibility and quality, but it should also contribute to cost control. Merging hospitals into health enterprises was a key instrument and an international trend (1, 2). After a review of literature on the effects of hospital mergers in terms of health economics, we concluded that a cost reduction of ten per cent could be achieved if the process led to a common organisational culture and more appropriate dimensioning of the services (3). Cooperation between the top management and the organisational core, especially the doctors, is a known precondition for success (4, 5).
The University Hospital of North Norway was established as a health enterprise in 2002, and took over the care of substance abusers in 2004, pre-hospital services in 2006, and the local hospitals in Narvik and Harstad in January 2007. After the merger, the enterprise had 6 000 employees and a challenging financial position with a deficit of NOK 470 million (10 per cent of the annual budget) in 2006.
In August 2007, the board launched a project for long-term development and restructuring. Its goals were to strengthen the function as a university hospital and regional hospital, improve the function as a local hospital, financially balance the operations, reduce the discrepancy between the hospital’s remit and resources, and develop a common organisational culture. This observational study describes the hospital operations through the process of merging and restructuring. Findings are discussed in light of published research on change processes in hospitals.
Material and method
Project organisation
The process of change was implemented using project methodology and led by the Chief Executive Officer (a doctor) and an internal project manager (a nurse) assisted by a management group consisting of experts with experience of change management in hospitals, as well as representatives of the users and employees. A focus group of 25 experts with various professional backgrounds provided advice. The process was based on involvement through board seminars, plenary meetings, discussion forums on the intranet and hearings.
It was planned for the process to be implemented with the aid of a knowledge-based approach grounded in the principles described in the reviewed literature, described above (3). Concentrating the activities on fewer and larger units, more efficient use of premises and a reorientation from in-patient to day treatment was expected to reduce costs. We assembled 64 operational units into ten divisions, two operational centres and four administrative units. In the divisions, it was planned to merge departments and wards across medical specialties, to reduce the number of beds and to transform wards into out-patient units and patient hotel units, as well as to relocate satellite units and concentrate the activities on a smaller area in the largest premises.
We based our approach on a notion of hospitals as complex organisations, in which the top management act as coordinators and providers of direction (4). Having medically trained management at all levels was seen as necessary to achieve a full merger of the professional groups and a common organisational culture. The divisions and departments were established with unified responsibilities across geographical locations. The administrative units and the works centres were given a stronger supportive role.
The staffing of the management positions was seen as decisive to ensure cooperation between the top management and the operational core. A total of six doctors, four nurses and a bioengineer were recruited as division heads. The project organisation was completed after ten months through the establishment of the director’s management group (the division heads, the administrative units and the centres), and the further development work was delegated to the line management.
The electronic patient records and the administrative system for patients (EPR/PAS) were merged into a single system. A programme for improvement of clinical pathways with lean-type methodology was established (6, 7). The goal of the programme was to ensure coordination across the divisions, quality improvement, enhanced employee satisfaction and better efficiency. The projects were assumed to be employee-initiated and employee-based, but management-led. Success criteria and measurable result indicators were established.
Enterprise data
We present prospective enterprise data from the first four-month period of 2006 through the first four-month period of 2011. Data from the Norwegian Patient Registry (NPR) describe the activity related to the treatment of patients, waiting times and national quality indicators. The number of surgical interventions, DRG points and employee-months are taken from the data warehouse of Analysesenteret AS, the management system of Northern Norway Regional Health Authority, and our own data bases (HR and wage systems, as well as EPR/PAS). The clinical-pathway projects are described with the aid of quantitative data for this activity in the project programme. Statistics from the Nordic Institute for Studies in Innovation, Research and Education document the number of scientific publications. Figures for financial performance were retrieved from the accounting system.
Employee satisfaction was measured in a cross-sectional survey undertaken in each division from the third four-month period of 2009 to the first four-month period of 2011. The questions were sent by e-mail to all permanent employees (n = 5 004), and altogether 3 119 (62 per cent) responded. We present results from the main question: «On the whole, how satisfied are you with the job that you currently have?«
The accounts contain registrations of revenues and costs, but cost reductions achieved through the merger and development process cannot be identified. Therefore, we undertook shadow accounting for the degree of implementation of the budgeted restructuring efforts, and these registrations are presented as an estimate of the cost reductions associated with the change process.
Results
Project implementation
The organisational changes were mainly implemented as planned within the specified time frame. One division could not continue operations after a management change occurring 12 months after its establishment, because the span of control and complexity were deemed excessive, and the division was split into two units.
Therapy and research activities
Somatic disorders
The therapeutic activity related to patients with somatic disorders remained stable, at an average of 280 977 patient contacts per year through 2008. In 2009, the level of activity declined by approximately seven per cent to 260 796, before it gradually rose to 276 837 in 2010. In the first four-month period of 2011, the activity (99 983 patient contacts) was 0.5 per cent higher than in the years prior to the restructuring (average for the first four-month period of each year from 2006 to 2008 was 99 480).
The number of outpatient contacts followed the same trend, and reduced outpatient activity was the main cause of the decline in 2009. The number of overnight stays gradually declined from 38 980 in 2006 to 35 647 in 2010 (9 per cent), while the number of outpatient surgical interventions gradually increased from 9 161 to 11 045 (21 per cent) over the same period. The number of surgical interventions was registered in EPR/PAS from 2008, and remained stable at approximately 20 000 per year.
The average number of DRG points per year amounted to 53 125 for the period 2006 – 2008, but the number declined by five per cent to 50 725 in 2009, before increasing to 56 710 in 2010. The number of DRG points in the first four-month period of 2011 (20 210 points) was 12 per cent higher than the average for the first four-month period (18 111 points) of each year in the period from 2006 to 2008.
Mental healthcare and inter-disciplinary specialised addiction therapy (TSB)
Figure 1 shows the development of activity related to mental healthcare for adults (VOP), mental healthcare for children and adolescents (BUP) and interdisciplinary specialised addiction therapy (TSB). The level of activity in mental healthcare for adults increased continuously from 40 757 patient contacts in 2006 to 58 108 patient contacts in 2010 (43 per cent). There was a growth in overnight stays (13 per cent) as well as outpatient contacts (45 per cent). As a whole, the level of activity in healthcare for children and adolescents increased from 20 884 patient contacts in 2006 to 25 418 in 2010 (22 per cent). There was an increase in the number of overnight stays (35 per cent) as well as outpatient contacts (22 per cent).
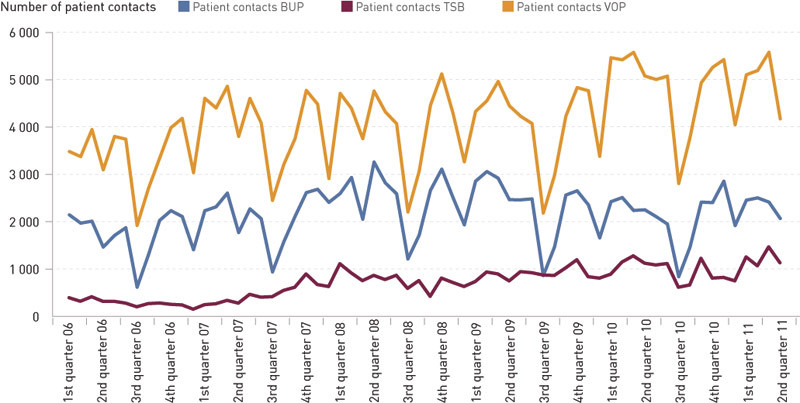
The level of activity related to specialised addiction therapy more than tripled from 3 635 patient contacts in 2006 to 11 753 in 2010. The number of overnight stays increased from 377 to 645 (71 per cent) and the number of outpatient contacts increased from 3 258 to 11 753 (261 per cent).
Research
The number of published articles increased by 62 per cent from 137 in 2006 to 222 in 2010, and the number of PhDs rose by 130 per cent, from ten in 2006 to 23 in 2010.
Treatment quality
Waiting times – somatic disorders
Figure 2 shows the waiting times. Average waiting time increased from somewhat less than 80 days in 2006 to 108 days in the third four-month period of 2010, but subsequently declined to 85 days in the first four-month period of 2011. For patients without entitlement to prioritised health assistance, the waiting time increased from 91 days in 2006 to 136 days in the third four-month period of 2010, although with a subsequent reduction to 104 days in the first four-month period of 2011. For patients who had an entitlement to prioritised health assistance there were minor fluctuations around an average of 65 days (data not shown).
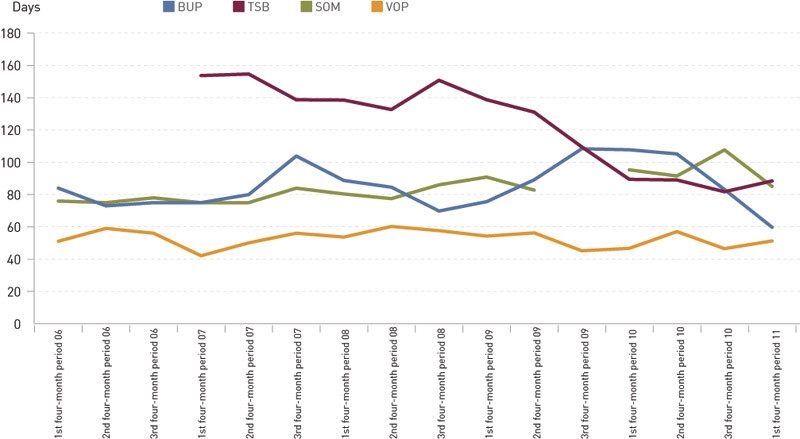
Waiting time – mental healthcare and addiction therapy
In healthcare for adults, the waiting time remained largely unchanged at approximately 50 days, with minor differences between patients with and without entitlement to prioritised health assistance. Average waiting times in healthcare for children and adolescents increased temporarily from 84 days in the first four-month period of 2006 to an average of 97 days in 2010, and declined to 60 days in the first four-month period of 2011. For specialised addiction therapy, waiting times declined from an average of 154 days in the first four-month period of 2007 to 88 days in the first four-month period of 2011. There was an unstable and inconsistent differentiation between patients with and without entitlement in mental healthcare services for children and adolescents as well as in cross-disciplinary specialised addiction therapy.
Quality indicators – somatic disorders
The proportion of case histories dispatched within seven days remained stable at 50 – 60 per cent from 2006 to 2010, but increased to 76 per cent in the first four-month period of 2011. The number of cancellations of planned surgery declined from 14 per cent in the first four-month period of 2006 to five per cent in the first four-month period of 2011. The proportion of patients with fracture of the femoral neck who were operated on within 48 hours varied from 89 per cent to 97 per cent and the proportion of emergency Caesarean sections varied from two per cent to 17 per cent, both without any clear trend over time. The proportion of corridor patients remained stable at approximately two per cent. The proportion of patients with an individual plan within the child rehabilitation programme fluctuated within a range from 11 per cent to 100 per cent during the period from 2006 to 2008, but stabilised at more than 80 per cent from the second four-month period of 2009.
Clinical pathway projects
A total of 29 lean-type projects were established throughout all divisions. Several of them included complex pathways across divisions and departments. Altogether 57 staff members received training in the methodology, and more than 400 have participated actively in the projects. A total of 14 improved pathways have been implemented in the routine operations, and another 15 are under implementation.
Staffing, productivity, financial development and employee satisfaction
The number of man-months increased from 5 682 in January 2006 to 6 422 in July 2007. This volume was reduced by ten per cent to 5 783 in January 2010, and later stabilised at approximately 6 000. Figure 3 shows that productivity (the number of DRG points per man-month) increased from an average of 0.73 in the period 2006 – 2008, to 0.79 in 2010, that the deficit of NOK 470 million in 2006 gradually declined to NOK 43 million in 2009, and that 2010 returned a surplus of NOK 67 million. At the end of the first four-month period of 2011 operations were close to balancing, with a deficit of NOK 4 million. Through 2009, cost-saving measures amounting to NOK 170 million had been registered. Some of these were modified in 2010, so that they amounted to NOK 106 million (20 per cent of the increase) for the five-year period.
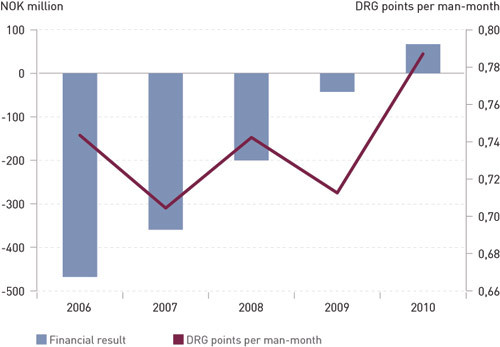
In the survey on employee satisfaction, altogether 81 per cent were satisfied with their job (33 per cent were very satisfied and 48 per cent were fairly satisfied), while 13 were neither satisfied nor dissatisfied and six per cent were dissatisfied.
Discussion
We describe a complex merger and development process that was implemented mainly as planned. We have observed a shift from in-patient to day treatment, an increase in productivity and an improved financial situation, while employee satisfaction remained at a high level at the end of the restructuring period. A temporary decline in activity occurred and waiting times for patients with somatic disorders increased, but in other respects the quality indicators pointed to unchanged or improved quality.
Our review of the literature on hospital mergers showed that cost reductions of ten per cent can be achieved (3). The restructuring process in the University Hospital of North Norway was implemented without supplementary funding. The gradual improvement in the financial situation indicates that the cost reductions outweighed the costs incurred by the restructuring process at all times. We estimated that the measures for cost reductions directly accounted for NOK 106 million (20 per cent of the improvement). In addition, the process is assumed to have had effects in the form of increased cost awareness, improved financial management and economies of scale. If we assume that 50 per cent of the improvement in financial performance can be ascribed to the merger and development process, this will amount to NOK 265 million, or six per cent. This is less than the possible effect foreseen, but still sufficient to allow the hospital to undertake large investments, such as a PET centre, new construction to increase capacity in the functions as a regional and university hospital, a new patient hotel and – in the somewhat longer term – a new local hospital.
We observed a temporary increase in waiting times, but the quality of treatment of patients remained stable or improved. One could imagine that lower costs would result in reduced quality. Chen at al. (8) studied 800 000 patients treated in 3 000 hospitals in the US, but found no correlation between costs and treatment outcomes. This concurs with our experience, as well as with a comprehensive body of literature indicating that cost reductions and quality improvements can be achieved when organisational changes are accompanied by improvements in clinical pathways (6, 9) – (11). We cannot exclude, however, that the quality standard of the University Hospital of North Norway has declined in areas that are not covered by our enterprise data.
There is scant research on change processes in hospitals, but a consistent finding is that problems are quite common, and in a transitional phase these may reduce the capacity and the quality of treatment provided to patients (12, 13). The main cause is a shift of attention from professional development to organisational development (14). Change processes can be subdivided into a rationalisation phase involving requirements for financial balance, a consolidation phase during which the organisation is redesigned, and a renewal phase when focus is returned to the core activities (15). If a long period of time elapses before the renewal phase starts, the risk of problems increases. We describe a change process that followed this pattern, proceeding at a rapid pace and with overlap between the phases. We combined the organisational changes with an improvement in clinical pathways, and we believe that this was crucial to maintain a focus on patient care (7).
Our observational study cannot identify any possible causal correlations between the organisational changes on the one hand and the level and quality of the core activities on the other. The authors are not independent observers, and this may have coloured our interpretation of possible correlations. Several methodological weaknesses can be pointed out. Changes in the database structure after the merging of EPR/PAS, the method for data extraction to the Norwegian Patient Registry and the activity-based funding (ISF) may have had an impact on figures for activities, waiting times and DRG points. The number of publications may be a flawed measure of research activity. Changes have been made to the registration routines and the definitions used by the quality indicators, and no indicators were available for mental healthcare and inter-disciplinary specialised addiction therapy. The number of man-months is influenced by sickness absence and new job tasks. Real growth in the budgets as well as changes in the activity-based funding, the regional revenue model, pension costs and rules for capital depreciation have contributed to the improvement in financial performance, but these effects cannot be isolated in the accounts. We have considered adjusting for these factors, but this would require an exclusion of large parts of the data base and entail a loss of the overall impression.
West (16) has summarised the challenges involved in research on change processes in hospitals. She emphasises the need for longitudinal studies with variables that can control for composition of the patient population as well as organisational and socio-economic aspects associated with the organisation, and the need for standardised measurements of the quality of patient care. The Norwegian Patient Registry and the national clinical quality registers are currently introducing person-specific registrations. Such data ought to be used for studies of the correlations between forms of organisation and restructuring in hospitals and treatment outcomes.
Conclusion
Experience from the University Hospital of North Norway shows that the level of activity and the quality of the core activities can be maintained throughout a complex merger and development process. The financial sustainability of the hospital has been improved such as to allow for investments in new treatment options and construction activities. There is no methodological basis for drawing conclusions on causal correlations between the changes and development of the core activities. Future research on correlations between change processes in hospitals and the results in terms of treatment outcomes ought to be based on person-specific data from the Norwegian Patient Registry and the national quality registers.
Tabell
| Main message |
|
- 1.
Kjekshus LE, Harsvik T. Organisasjonsutvikling ved norske sykehus. Tidsskr Nor Legeforen 2007; 127: 288-90. [PubMed]
- 3.
Ingebrigtsen T. Helseøkonomiske effekter av sykehussammenslåinger. Tidsskr Nor Legeforen 2010; 130: 940-2. [PubMed]
- 4.
Mintzberg H. Structure in 5’s: a synthesis of the research on organization design. Manage Sci 1980; 26: 322 – 41. [CrossRef]
- 7.
Aasebø U, Strøm HH, Postmyr M. The Lean method as a clinical pathway facilitator in patients with lung cancer. Clin Respir J 2011; e-publisert 26.9.2011.
- 9.
Porter ME, Teisberg EO. Redefining health care. Creating value-based competition on results. Boston: Harvard Business School Press, 2006.
- 12.
Brousselle A, Denis J-L, Langley A. What do we know about hospital mergers? A selected annotated bibliography. Ottawa: Canadian Health Services Research Foundation, 1999.
- 15.
Ghoshal S, Bartlett CA. Rebuilding behavioral context: a blueprint for corporate renewal. I: Beer M, Nohria N, red. Breaking the code of change. Boston: Harvard Business School Press, 2000: 195 – 222.