Mortality statistics are essential for monitoring public health. To ensure that these statistics are of good quality, the doctors need to emphasise correct completion of the death certificate and they must understand the true cause of death (1).
An autopsy is a medical investigation which is undertaken to determine the underlying cause of death and as a quality assurance of the medical treatment that has been provided to the patient. The importance of autopsies for mortality statistics has been referred to and debated at regular intervals on the pages of this journal (2) – (4). Previous studies from the US and Europe have shown that in close to half of all cases there is no correspondence between the information on the death certificate and the result of the autopsy (5, 6). We wished to investigate whether this situation has changed. Thus, the purpose of this study is to examine the importance of the findings from the autopsies for the determination (ICD-10 coding) of the underlying cause of death, and to see whether any differences are correlated with age or gender. Such studies have not previously been undertaken in Norway.
Material and method
The data for the study are based on information from death certificates. In column I, the reporting doctor should note the sequence of pathological conditions, injuries or functional impairments that caused the death to occur. I.a. contains the immediate cause of death, for example pulmonary embolism, I.b. states the intermediate cause of death, for example thrombosis of the fibular vein, and I.c. contains the underlying cause of death, for example pancreatic cancer. Usually, the lowermost diagnosis in column I will be registered as the underlying cause of death. Often it will not be necessary to complete all three fields. In column II, the doctor can note any other significant conditions that may have contributed to the fatal outcome, but have no direct causal relationship to the sequence of pathologies in column I.
To correct any obvious errors made and illogical conclusions drawn by the doctor during the completion of the death certificate, The World Health Organization (WHO) has elaborated a set of rules that govern the manner in which the Cause of Death Registry will determine the underlying cause of death on the basis of the death certificate. Until 2005 the underlying cause of death was determined manually by the coding personnel at the Cause of Death Registry, but since 2005 it has been determined electronically by a software application (Automated Classification of Medical Entities, ACME) developed by the National Center for Health Statistics in the US (7). The application requires the cause of death to be «translated» into ICD-10 codes (International Classification of Diseases, version 10) (8). This translation is performed by the coding personnel. The ACME application subsequently «reads» the coded death certificate and determines the underlying cause of death.
In addition to the death certificates, the Cause of Death Registry receives the results of all autopsies. The autopsy diagnoses will usually be listed in the same manner as the diagnoses on the death certificate, although the diagnoses will tend to be based on the morphological changes caused by the disease or the injury.
When a death certificate and an autopsy result are both available, the set of ICD-10 codes to be analysed by the ACME application must be selected manually. In light of the additional findings from the autopsy, the Cause of Death Registry thereby constructs a «combined» death certificate, which may contain diagnoses from the death certificate as well as from the autopsy. In most cases, the autopsy results will be given priority, but in many cases several of the diagnoses on the death certificate will be included, even if they are not referred to in the autopsy report.
For all those who underwent a medical autopsy in 2005, we were granted access to ICD-10 codes for the underlying cause of death determined on the basis of the original death certificates as well as the «combined» death certificates, which included autopsy diagnoses and the gender and age of the patient. Since the registration of the causes of perinatal deaths also uses information from the Medical Birth Registry, we did not examine deaths of persons younger than two years.
Information on underlying causes of death, gender distribution and age at death for the entire population was retrieved from official records in Statistics Norway. All statistical analyses of discrepancies between the original and the «combined» death certificates were undertaken with the aid of PASW Statistics 18. Chi-square tests were used to assess age and gender differences and variations in ICD-10 codes. The material was subdivided into five age groups: 2 – 30 years, 31 – 50 years, 51 – 70 years, 71 – 90 years and > 90 years. P values < 0.05 were regarded as statistically significant. All data had been anonymised, and the study was thus exempt from submission to the Regional Committee for Medical and Health Research Ethics.
Results
The 1,773 medical autopsies performed on persons aged two and over included 989 men and 784 women. Median age at death was 71 years and 76 years respectively. In comparison, the median age at death in the population as a whole was 80.5 years for men and 85.5 years for women (9).
Causes of death in the population as a whole in 2005 and the underlying causes of death for the 1,773 cases examined, based on the death certificate alone and after adjustment by the autopsy, are shown in Table 1 (10). The autopsy results led to a change in the underlying cause of death for 1,077 (61 %) of the 1,773 deaths. In 567 cases (32 %) the adjustments involved a change of ICD-10 chapter for cause of death. For 510 cases (29 %) the adjustment involved a change of cause of death within the same ICD-10 chapter. For the remaining 696 cases (39 %) the cause of death remained unchanged. There were considerable changes with regard to the two largest groups of diseases, cardiovascular diseases and cancer. The shifts in codes between these two groups and the other ICD-10 chapters are shown in Figure 1. Of a total of 778 deaths coded as cardiovascular disease after autopsy, a total of 238 (31 %) had been transferred to this chapter from other chapters. In the chapter for malign neoplasms, the number of deaths transferred from other chapters amounted to 83 of 450 (18 %).
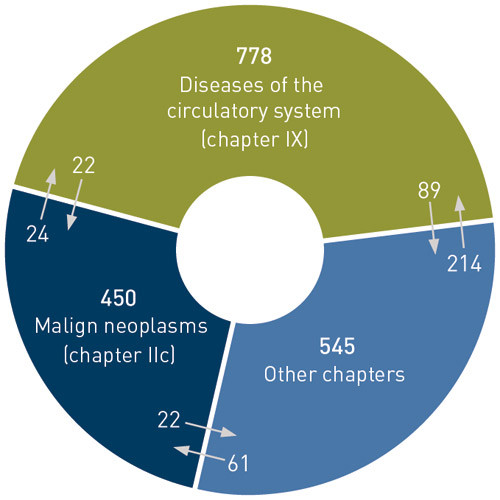
Table 1:
Underlying causes of death in 2005, for all deaths, and for deaths examined by a hospital autopsy. The overview of all deaths (column 2) is based on figures from Statistics Norway (10).
| All deaths¹ n = 41,152 |
Autopsies (underlying cause of death based on the death certificate) n = 1,773 |
Autopsies (underlying cause of death based on the autopsy) n = 1,773 |
|
| ICD-10 chapter |
Percentage |
Percentage |
Percentage |
| I A 00-B99: Certain infectious and parasitic diseases |
1.9 |
4.9 |
3.2 |
| II C00-C99: Neoplasms² |
25.7 |
23.3 |
25.4 |
| III D50-D89: Diseases of the blood and blood-forming organs and certain disorders involving the immune system |
0.6 |
0.7 |
0.4 |
| IV E00-E90: Endocrine, nutritional and metabolic diseases |
0.8 |
2.3 |
1.4 |
| V F00-F99: Mental and behavioural disorders |
3.8 |
1.4 |
0.3 |
| VI G00-G99: Diseases of the nervous system |
3.2 |
2.4 |
2.0 |
| VII-VIII H00-H95: Diseases of the eye and adnexa |
< 0.01 |
0.1 |
0.1 |
| IX I00-I99: Diseases of the circulatory system |
35.3 |
36.6 |
43.9 |
| X J00-J99: Diseases of the respiratory system |
9.9 |
10.1 |
8.9 |
| XI K00-K93: Diseases of the digestive system |
0.3 |
8.0 |
7.7 |
| XII L00-L99: Diseases of the skin and subcutaneous tissue |
0.2 |
0.1 |
0.1 |
| XIII M00-M99: Diseases of the musculoskeletal system and connective tissue |
0.6 |
1.1 |
0.7 |
| XIV N00-N99: Diseases of the genitourinary system |
2.1 |
1.0 |
0.8 |
| XV O00-O99: Pregnancy, childbirth and the puerperium |
< 0.01 |
0 |
0.1 |
| XVI P00-P96: Certain conditions originating in the perinatal period |
0.2 |
0.1 |
0.1 |
| XVII Q00-Q99: Congenital malformations, deformations and chromosomal abnormalities |
0.3 |
1.1 |
0.6 |
| XVIII R00-R99: Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified |
4.3 |
3.2 |
0.3 |
| XIX-XX S-Y: External causes, total |
5.9 |
3.2 |
3.4 |
| [i] | |||
[i] ¹ Also includes deaths of persons younger than two years. This group is small, and with few exceptions coded in ICD chapter XVI and XVII.
² Not included D00-D48: in situ, benign and unknown or uncertain behaviour. The total of the column for all deaths does not therefore add up to 100 per cent.
The autopsy result led to the greatest change in ICD-10 chapter for underlying cause of death among the youngest and oldest age groups. The proportion of women who had their disease chapter changed was higher than that of men in all age groups, except the age group > 90 years: Women versus men > 30 years: 38 % versus 35 %; 31 – 50 years: 30 % versus 23 %; 51 – 70 years: 28 % versus 26 %; 71 – 90 years: 39 % versus 32 %; > 90 years: 40 % versus 43 %.
Diseases of the circulatory system
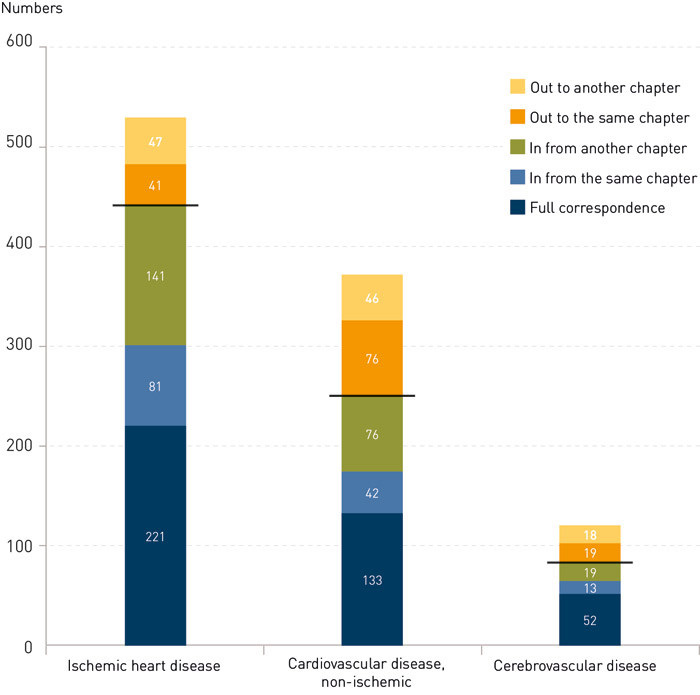
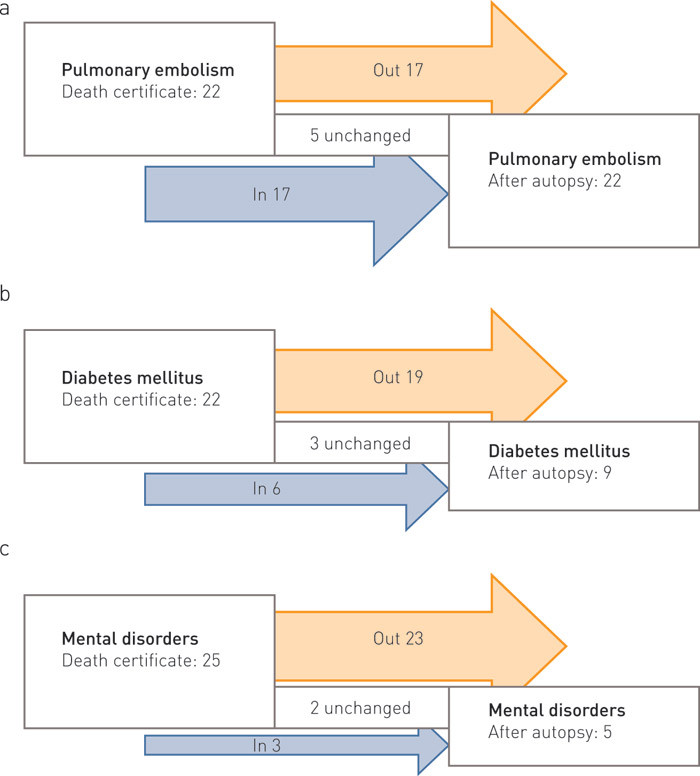
There was a considerable shift in causes of death within this chapter. Changes following the autopsy within the three main groups of ischemic heart disease, cardiovascular diseases of non-ischemic origin and cerebrovascular disease within Chapter IX are shown in Figure 2. The number of cases with ischemic heart disease as an underlying cause of death increased from 309 to 443, or from 17 % to 25 % of all causes of death. The number of deaths caused by pulmonary embolism or deep-vein thrombosis (in the group of cardiovascular diseases of non-ischemic origin) was not changed after the autopsy, but there was a considerable exchange of cases. A correspondence was detected for only five out of 22 deaths (Figure 3a).
Malignant diseases
Autopsy findings caused cancer to be introduced as a new underlying cause of death in 83 cases, whereas cancer was excluded as an underlying cause of death in 46 cases (Figure 1). In 48 of the 83 new cases there was no information on cancerous disease on the original death certificate. The changes within Chapter IIc, malign neoplasms, were mostly concerned with a change in primary location or type of cancer (55 cases).
Other causes of death
The autopsy results caused a drop in the proportion of deaths from other causes from the remaining ICD-10 chapters (Table 1).
Diabetes mellitus was reported as the underlying cause of death on the death certificate of 22 individuals (Figure 3b). Following the autopsy, the underlying cause of death was changed for 19 of them (Figure 3c). A major part of this reduction was caused by a change of the diagnosis to alcohol addiction syndrome, which is coded as a mental disorder. When alcohol-related pathology is detected by autopsy, the mental diagnosis is changed to alcohol-induced injuries to the organs. Of the ten cases that had alcohol addiction syndrome on the death certificate only one case was left unchanged as mental illness. Three were coded as alcohol-induced organ injury (liver cirrhosis and cardiomyopathy) and six were given diagnoses unrelated to alcohol abuse. The autopsies also revealed new alcohol-related deaths, but only in the form of organ injuries. Even though only one death was coded as alcohol addiction syndrome after autopsy, the number of alcohol-related deaths still increased from 17 to 23.
The other large group of psychiatric diagnoses that were changed following autopsy were all in the «dementia» category. Only two out of a total of eight cases of unspecified dementia were given an organically defined dementia code (Alzheimer’s disease) following autopsy, the remaining were coded as cardiovascular disease, pulmonary disease or infection.
For all the six cases where epilepsy had been reported as the underlying cause of death on the death certificate, another cause was determined by the autopsy: cancer, subarachnoidal haemorrhage, Alzheimer’s disease, Sjögren’s syndrome, myopathy and ischemic heart disease.
In all the nine cases for which the underlying cause of death had been reported to be side effects of drugs or complications of medical treatment, the code was changed to a disease code following autopsy (heart disease, thromboembolic disease, chronic obstructive pulmonary disease (COPD), cancer or fracture). Autopsy findings also reduced the number of cases of pneumonia and chronic obstructive pulmonary disease as causes of death. Only 17 of 70 reported deaths from pneumonia and 13 of 71 cases of death from COPD were confirmed by the autopsy.
The number of deaths caused by diseases of the urinary tract and the genitals was also greatly reduced following autopsy. All 11 cases with the symptom diagnosis of «renal failure» on the death certificate were given a specific diagnosis after an autopsy.
Hospital autopsies produced a drop in the number of deaths by unknown causes, Chapter XVII, from 56 to 6 (Table 1). Altogether 34 of these (61 %) were diagnosed with ischemic heart disease or other cardiovascular disease as the cause of death.
In 18 of 37 deaths for which the underlying cause after autopsy was reported to be fracture caused by a fall, the accident was reported on the death certificate. An equal number (n = 18) had fracture caused by a fall excluded as the cause of death after autopsy, and were transferred to chapters for other diseases.
Discussion
Death certificates and autopsy reports serve as the basis for public mortality statistics, which are published annually by Statistics Norway. These statistics are used as the basis for assessment of public health, and it is therefore essential that the registry is of good quality.
Since medical autopsy findings produced a change in the underlying cause of death for a full 61 % of the deaths, as well as a cause of death from another ICD-10 chapter for 32 %, this study demonstrates that there is a large margin of uncertainty associated with determination of the cause of death. Even though a medical autopsy was performed on a relatively limited number of deaths (n = 1,773) when compared to the total number of deaths (n = 41,152) and the sample is highly selective, in our opinion the results would warrant a debate on the quality of mortality statistics.
One weakness of most autopsy studies, including our own, is that the patients are not representative of the population as a whole. In our material, the proportion of deaths caused by infections, mental disorders and diseases of the digestive system differs from what is found in the population as a whole. The higher occurrence of infections and diseases of the digestive system reflects the fact that patients suffering from such diseases more often die following admission to hospital, while the low proportion of mental disorders can mainly be explained by the fact that patients with unspecific dementia, which is coded as a mental disorder, more often die in nursing homes. In addition, autopsy studies tend to be biased with regard to gender and age, as they include a preponderance of men and people in younger age groups (11, 12). The lower frequency of autopsies performed on women can be explained by women’s higher age at death, and their concurrently higher likelihood of dying not in a hospital, but in a nursing home.
We are not familiar with any similar studies undertaken on the basis of the ACME system, but several previous comparisons of death certificates and autopsy results have yielded similar findings. A study undertaken in Connecticut in 1980 showed that the autopsy findings produced a change in the underlying cause of death with a transfer to another ICD chapter in 29 % of the cases (5). The autopsy frequency for the population of Connecticut was not reported. An East German study from 1987 with an autopsy frequency of approximately 100 % showed that the autopsy findings produced a change in the underlying cause of death and a change of ICD chapter in 30 % of the cases (6).
The fact that our findings from 2005 are similar to findings in older studies may indicate that the progress of diagnostic methodology in recent decades has not produced a better conformity between the clinician and the medical examiner with regard to the reporting of causes of death. There is a possibility that falling autopsy rates have caused autopsies to be reserved for especially complicated courses of illness, for which the cause of death is difficult to determine. Most of the patients in our material, however, have been examined in regional hospitals, and the doctors have had access to all medical records. The fact that the patients autopsied were on average close to ten years younger than the median age at death of the population as a whole also implies that age-related multi-morbidity has only to a lesser extent complicated the determination of the underlying causes of death in our material.
As in the previous studies, we found a marked increase in causes of death from diseases of the circulatory system (ICD-10 chapter IX) after having taken the autopsy results into account. During the last forty years, a consistent decrease in mortality rates from cardiovascular diseases has been reported (13). An overview study from 1998 on the role of autopsies for epidemiological studies of cardiovascular diseases concluded that the death certificate, the clinical records or an interview could replace autopsies (14). Most of the decrease in mortality from cardiovascular diseases is undoubtedly real, but a Finnish study on causes of death among middle-aged men has pointed out that a high autopsy rate is important (especially for those who die outside hospitals) to monitor the further development of mortality from cardiovascular diseases (15). In Norway, the declining rate of mortality from cardiovascular diseases has occurred simultaneously with a strong decrease in the number of autopsies undertaken after sudden and unexpected deaths (16).
The correspondence between the death certificate and the autopsy result was best for deaths caused by cancer. This notwithstanding, as a result of the autopsy findings approximately ten per cent of the cases for which the death certificate had given cancer as the cause of death were reclassified to other causes. However, the shift in the opposite direction was even greater, so that the proportion of deaths caused by cancer increased from 23.3 % to 25.4 %. One in ten of these cases of cancer was not referred to on the death certificate. These findings tally with a Swedish study from 1997, which reported that a decreasing autopsy rate may be the cause of the declining rate of several forms of cancer (11). The Swedish researchers therefore warned against drawing conclusions on the development of the incidence of cancer without taking differences in autopsy rates into account.
We cannot exclude the possibility that some of the death certificates have been completed following the availability of preliminary autopsy findings. If so, we may underestimate the importance of autopsies for the determination of the underlying cause of death.
The poor quality of death certificates and the validity of mortality statistics are frequently being discussed (1). Articles questioning the quality of autopsy results are published less frequently. It is appropriate to note that autopsy results may not always provide the ultimate answer. A study from 2006 on the quality of autopsy reports from the British system of coroners who investigate deaths showed that 25 % of the reports were of poor or unacceptable quality (17). In addition to recommending quality controls at regular intervals, including a second opinion, the study concluded that there was a need to define a national standard for identification of causes of death in the autopsy reports.
Even though the examinations undertaken by the British coroners are not directly comparable to Norwegian medical autopsies, there is reason to note that Norway has no standard for the performance of autopsies and assessment of their results either. For forensic post mortems in Norway, the Forensic Commission undertakes a systematic quality control (16). An introduction of a national standard and a systematic quality review could help strengthen the role of medical autopsies in the assessment of the cause of death.
The changes in recorded cause of death after autopsy may indicate that the clinician and the pathologist differ in their understanding of the listing of causes of death. The absence of deaths from epilepsy and a reduction in diabetes-related deaths by half indicate that pathologists to some extent fail to diagnose causes of death from certain groups of diseases. Insufficient use of clinical-chemical supplementary examinations may also cause some diseases without a morphological correlate to be left out of the autopsy diagnoses. Differences in understanding may also be caused by insufficient knowledge. Most likely, a major proportion of the autopsy reports are completed without any knowledge of the diagnosis given in the death certificate, which is often completed by other doctors than those who submit the autopsy request. If a discussion of the clinically provided cause of death on the death certificate were made into a regular procedure in the autopsy report, this would make the interpretation of the various diagnoses easier for the Cause of Death Registry.
A new, electronic death certificate is currently being planned. In this context it will be possible to introduce changes that could improve the quality of the registration of causes of death, including the registration of autopsy findings. For example, one should consider whether the coding personnel at the Cause of Death Registry should be charged with the assessment of the list of diagnoses in the autopsy report against the list of diagnoses on the death certificates. In Finland, this responsibility lies with the doctor who completes the death certificate and requests the autopsy (15).
Conclusion
Following medical autopsy findings, the underlying cause of death was changed for 61 % of those who were subject to an autopsy in 2005. In 32 % of the cases, the changes involved transfer to another chapter of ICD-10. The high rate of change and the in some cases considerable transfer between various groups of diseases indicate that autopsies remain considerably important for the mortality statistics.
Tabell
| Main message |
|
- 1.
Alfsen GC, Lyckander LG, Lindboe AW et al. Kvalitetssikring ved dødsfall i sykehus. Tidsskr Nor Legeforen 2010; 130: 476–9. [PubMed]
- 2.
Rogde S. Hvor pålitelig er dødsårsaksstatistikken? Tidsskr Nor Legeforen 2009; 129: 980. [PubMed]
- 3.
Svare A. Trenger vi virkelig flere obduksjoner? Tidsskr Nor Legeforen 2010; 130: 756–8. [PubMed]
- 4.
Ellingsen CL, Mæhlen J. Heller flere enn færre obduksjoner. Tidsskr Nor Legeforen 2010; 130: 1121. [PubMed]
- 7.
Om statistikken. Oslo: Statistisk sentralbyrå, 2010. www.ssb.no/vis/emner/03/01/10/dodsarsak/om.html (20.12.2010).
- 8.
International statistical classification of diseases and health related problems ICD. 10th revision, version for 2007. Genève: World Health Organization, 2007. http://apps.who.int/classifications/apps/icd/icd10online/ (20.12.2010).
- 9.
Dødelighetstabeller. Oslo: Statistisk sentralbyrå, 2005. www.ssb.no/dode/arkiv/tab-2006-04-27-05.html (22.1.2011).
- 10.
Dødsfall etter kjønn, alder og underliggende dødsårsak. Hele landet. 2005. Oslo: Statistisk sentralbyrå, 2007. www.ssb.no/dodsarsak/arkiv/tab-2007-10-19-11.html (30.1.2011).
- 13.
Dødelighet av hjerte- og karsykdommer og svulster. 2000–2009. Oslo: Statistisk sentralbyrå, 2010. www.ssb.no/dodsarsak/fig-2010-12-03-01.html (25.1.2011).
- 15.
Lahti RA, Sarna S, Penttilä A. Exploitation of autopsy in determining natural cause of death: trends in Finland with special reference to the diagnostics of ischemic heart diseases and cerebrovascular diseases in middle-aged males, 1974 – 1993. Forensic Sci Int 1998; 91: 109 – 21. [PubMed] [CrossRef]
- 16.
Den rettsmedisinske kommisjon. Årsrapport 2009 www.justissekretariatene.no/nb/Innhold/DRK/Arsmeldinger-og-veiledere/ (28.1.2011).
- 17.
The coroner’s autopsy. Do we deserve better? A report of the National Confidential Enquiry into Patient Outcome and Death NCEPOD (2006). www.ncepod.org.uk/2006.htm (28.1.2011).