Attitudes to seeking medical assistance – variations depending on social background?
Recent research indicates that socio-economic differences in health are increasing, even in an egalitarian society such as Norway, and one of the key objectives of Norwegian health policies is to reduce these differences (1) – (2). To succeed in this endeavour, we need to understand the mechanisms that give rise to these differences. Many alternative theories have been put forward, and there is little consensus among professionals regarding which theory best explains these differences.
In this article we will focus on features of the population, restricted to factors associated with attitudes to seeking medical attention. By attitudes, we refer to a relatively permanent normative point of view that indicates how we ought to think and act – not how we act in reality (3). Are there any systematic differences in the way in which people from various social strata relate to seeking medical attention when experiencing various physical problems? This question is discussed on the basis of a statistical analysis of interview data from the Norwegian part of the «European Social Survey 2004/2005», in which attitudes to the use of health services was a key topic (4, 5).
Material and method
The European Social Survey (ESS) is a European cross-sectional survey which has been undertaken every two years in more than 20 countries. The population comprises all individuals aged 15 or older who are resident in private households in each participating country. The samples are selected according to procedures for random sampling. The data collection is undertaken in personal face-to-face interviews lasting approximately one hour, and all the interviewers are trained according to the guidelines for ESS – additional information is available online (4, 5). In Norway, the study is undertaken by Statistics Norway on commission from the Research Council of Norway. All data are freely available on the Internet (6). The data used in this study are taken from a module on health and health services which was included only in round 2 (2004/2005).
Sample
The Norwegian sample was drawn as a random sample from the national registry in one step. A response rate of 66 per cent yielded a net sample of 1,760 respondents aged 15 – 94 (5, 7). In the analyses described here, the sample has been restricted to respondents aged 25 – 75. Respondents younger than 25 years (235 persons) were excluded, because we are using level of education as an indicator of socio-economic position, and the youngest age group is likely to include many who have not yet completed their education (8). The upper age restriction of 75 years (90 persons excluded) was introduced because the method of selection prevented us from excluding people who, whilst living in private households, have such extensive contact with the health services that they no longer have a fully independent responsibility for assessing their own need for medical attention. Following these restrictions, the final sample comprised 1,435 respondents, whereof 694 were women and 741 were men.
Independent variables
We used education as an indicator for socio-economic position. This was because of the practical advantages that this variable offers – such as an inherent ranking, stability over the life course and few missing values – as well as the assumption that education constitutes one of the key mechanisms for social differentiation in our society (8). The education variable is self-reported and measures formal competence through the question «What is your highest level of education?» The respondents were provided with nine response alternatives, ranging from 0 – no education, to 8 – research competence, PhD. The variable was recoded into three categories according to the Norwegian Standard Classification of Education (NUS 2000), which recommends this three-level categorisation for analytical purposes (9) (e-tab 1).
Table 1:
Overview of response alternatives for the education variable – original and recoded
| Self-reported education; «What is your highest level of education?» |
Level of education, recoded |
||
| 0 |
No education |
1 |
Mandatory education |
| 1 |
Primary school |
||
| 2 |
Lower secondary, one or two years of schooling after primary level |
||
| 3 |
Basic upper secondary, one year of vocational training |
2 |
Intermediate education |
| 4 |
Completed upper secondary, two or three years of vocational training, former gymnasium |
||
| 5 |
Extension of upper secondary level, technical college |
||
| 6 |
University/university college, four years or less with graduation, teacher training college, nursing college, cand. mag. degree, engineer |
3 |
University and university college education |
| 7 |
University/university college, more than four years with graduation, Master’s degree, civil engineer, chartered economist |
||
| 8 |
Research level, PhD |
||
Furthermore, we used information on age, gender and self-reported health. Age was included in the analysis as a continuous variable with 25 years as a reference value. The health variable was included to adjust for educational differences in health, but also because poor health in itself may be assumed to have an impact on attitudes to the use of medical services – some may for example have extensive need for help, which in turn may produce a broader experience with the system and colour the experience of the system’s ability to provide help. Using the question «How is your health in general?» the respondents were asked to report the state of their health in one of five categories: 1 – very good, 2 – good, 3 – fair, 4 – bad, and 5 – very bad. In accordance with common practice, this variable was dichotomised so that fair, poor and very poor health were collapsed into the category «poor health» (10).
Initially we also considered including two variables for social networks: the first based on the question of whether the respondent had somebody he or she could confide in, the second on the frequency of social interaction. The former was excluded because the proportion reporting to have nobody to confide in was very small, and because the p value was > 0.25 for several of the attitude-related variables in the univariate analyses. The challenge related to small numbers of units in certain categories was also noticeable for the variable of frequency of social interaction. In combination with the fact that the design of this variable made it difficult to recode it without a significant loss of information, this caused us to exclude this variable also from the multivariate analyses.
Dependent variables
The data set comprises four variables on attitudes, in which the respondents were asked to identify their assumed strategy for seeking help in the event of four hypothetical symptoms: Sore throat, serious headache, serious sleeping problems and serious backache. «If you experienced (...), whom would you turn to first for advice or treatment?» Response alternatives included: 1 – nobody, 2 – friends or family, 3 – pharmacy or dispensary, 4 – doctor, 5 – nurse, 6 – the Internet, 7 – a medical helpline, and 8 – other practitioner. We were primarily interested in the difference between those who chose «doctor» versus those who chose any of the other alternatives, and the four variables were dichotomised accordingly. Since both social position and personal variations in medical history and experiences may affect the choice of response for an individual symptom, the four dichotomous variables were also collapsed into one collective variable that separates those respondents who gave «doctor» as their primary strategy for seeking help for all four symptoms from the others.
Analysis
The purpose of the analyses was to investigate whether attitudes to seeking medical attention, operationalised as the reported primary strategy for seeking help in case of various symptom scenarios, co-varies systematically with socio-economic position, measured in terms of level of education. Bivariate cross-tabulations and Pearson’s chi-square test were used to establish an impression of how the respondents’ attitudes vary according to the chosen socio-demographic characteristics. Possible associations between education and health on the one hand, and the reported intention to seek medical attention in case of hypothetical symptoms on the other, were later tested with the aid of univariate and multivariate logistic regression for each gender. In the multivariate analyses, the independent variables were added in a stepwise fashion: first age, then level of education and finally state of health. This was to see whether the importance of the explanatory variables changed when more variables were included in the model. The statistics software package SPSS (Version 16.0) was used for the computations.
Ethical concerns
All data were anonymised after the study, which was undertaken in accordance with the provisions in the Personal Data Act.
Results
E-table 2 shows how the sample was distributed according to the independent variables.
Table 2:
Distribution of the sample with regard to the independent variables used in the analyses
| Personal characteristics |
Total (N = 1435) |
Men (n = 741) |
Women (n = 694) |
|||||
| Age in years. average (SD) |
47.4 |
(13.1) |
47.4 |
(13.3) |
47.4 |
(12.9) |
||
| Self-reported level of education. N (%) |
||||||||
| Mandatory education |
278 |
(19.4) |
139 |
(18.8) |
139 |
(20.0) |
||
| Intermediate education |
577 |
(40.2) |
300 |
(40.5) |
277 |
(39.9) |
||
| University and university college education |
578 |
(40.3) |
300 |
(40.5) |
278 |
(40.1) |
||
| Not reported |
2 |
(0.1) |
2 |
(0.3) |
||||
| Self-reported state of health. N (%) |
||||||||
| Poor health |
364 |
(25.4) |
179 |
(24.2) |
185 |
(26.7) |
||
| Good health |
1 071 |
(74.6) |
562 |
(75.8) |
509 |
(73.3) |
||
Gender
Among the women, the proportion who would choose a doctor in the event of any of the different symptoms varied within a range from 32.9 to 75.6 per cent, and among the men within a range from 34.3 to 77.6 per cent (e-tab 3).
Table 3:
Distribution of the sample with regard to the dependent variables, real figures and proportions (%)
| Attitude variables |
Total (N = 1 435) |
Men (n = 741) |
Women (n = 694) |
|||||
| Chooses to see a doctor for a very sore throat |
482 |
(33.6) |
254 |
(34.3) |
228 |
(32.9) |
||
| Other strategy for seeking help |
953 |
(66.4) |
487 |
(65.7) |
466 |
(67.1) |
||
| Chooses to see a doctor for a serious headache |
510 |
(35.5) |
257 |
(34.7) |
253 |
(36.5) |
||
| Other strategy for seeking help |
924 |
(64.4) |
483 |
(65.2) |
441 |
(63.5) |
||
| Not reported |
1 |
(0.1) |
1 |
(0.1) |
||||
| Chooses to see a doctor for serious sleeping problems |
943 |
(65.7) |
500 |
(67.5) |
443 |
(63.8) |
||
| Other strategy for seeking help |
487 |
(33.9) |
238 |
(32.1) |
249 |
(35.9) |
||
| Not reported |
5 |
(0.3) |
3 |
(0.4) |
2 |
(0.3) |
||
| Chooses to see a doctor for serious backache |
1 100 |
(76.7) |
575 |
(77.6) |
525 |
(75.6) |
||
| Other strategy for seeking help |
333 |
(23.2) |
164 |
(22.1) |
169 |
(24.4) |
||
| Not reported |
2 |
(0.1) |
2 |
(0.3) |
||||
| Chooses to see a doctor for all four symptoms |
226 |
(15.7) |
128 |
(17.3) |
98 |
(14.1) |
||
| Other choice |
1 204 |
(83.9) |
610 |
(82.3) |
594 |
(85.6) |
||
| Not reported |
5 |
(0.3) |
3 |
(0.4) |
2 |
(0.3) |
||
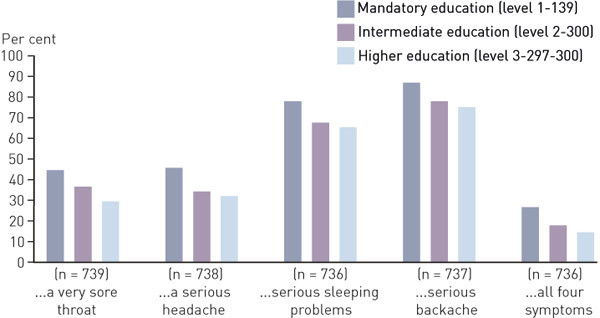
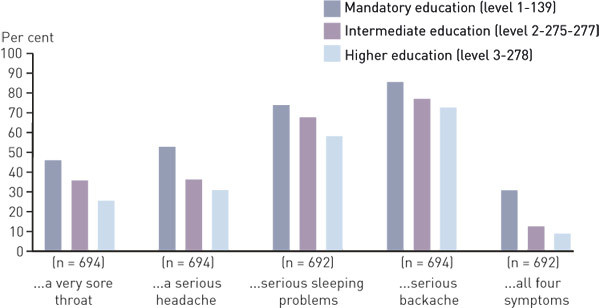
Chi-square testing of the gender difference within each level of education showed that the difference in the proclivity to seek medical attention was statistically significant only for men and women at the highest level of education on the collective variable: 13.8 per cent of the men, compared to 8.3 per cent of the women would choose to see a doctor in case of all four symptoms (p = 0.035; Figures 1 and 2).
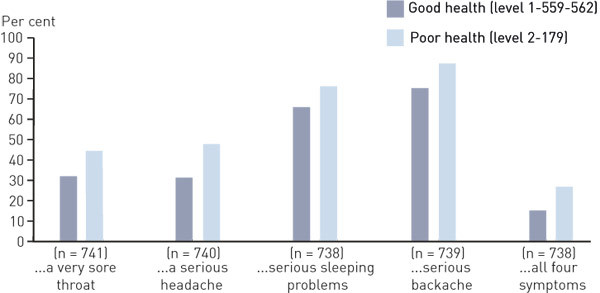
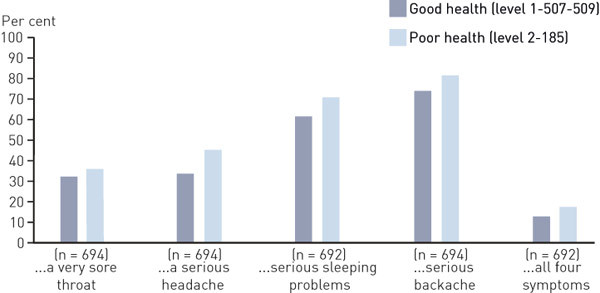
In corresponding tests among respondents with good versus poor health, the gender difference was statistically significant only for the collective variable, according to which 26.3 per cent of the men and 17.3 per cent of the women with poor health would choose to see a doctor (p = 0.038; e-figure 3 and e-figure 4).
Education
The proportion reporting that they would see a doctor was highest among respondents with only the mandatory level of education, and diminished for every step up the educational ladder. This pattern emerged for all attitude variables for both genders. However, the difference between the lowest and the highest levels of education was on the whole more prominent for women (figures 1 and 2).
The univariate logistic regression analyses showed that the odds rates for choosing to see a doctor were higher to a statistically significant extent among respondents at the lowest level of education when compared to those at the highest level of education, among men and women alike (tables 4 and 5).
Table 4:
Logistic regression analyses, men: Would have gone to see a doctor first for advice or treatment if they suffered from (…)
| Dependent variables (attitude variables) |
|||||||||||||||
| …a very sore throat (n = 739 – 741) |
…a serious headache (n = 738 – 740) |
…serious sleeping problems (n = 736 – 738) |
…serious backache (n = 737 – 739) |
…all four symptoms (n = 736 – 738) |
|||||||||||
| Independent variables |
OR |
95 % CI |
OR |
95 % CI |
OR |
95 % CI |
OR |
95 % CI |
OR |
95 % CI |
|||||
| 1. |
Age in years |
1.03 |
1.02 – 1.05 |
1.03 |
1.02 – 1.04 |
1.03 |
1.02 – 1.04 |
1.02 |
1.01 – 1.04 |
1.04 |
1.03 – 1.06 |
||||
| 25 years |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Level of education |
|||||||||||||||
| Mandatory |
1.95 |
1.28 – 2.96 |
1.76 |
1.16 – 2.66 |
1.83 |
1.15 – 2.90 |
2.16 |
1.25 – 3.75 |
2.18 |
1.32 – 3.61 |
|||||
| Intermediate |
1.38 |
0.98 – 1.95 |
1.09 |
0.77 – 1.54 |
1.09 |
0.78 – 1.53 |
1.15 |
0.79 – 1.67 |
1.28 |
0.82 – 2.00 |
|||||
| University/university college |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Self-reported health |
|||||||||||||||
| Poor health |
1.69 |
1.20 – 2.39 |
1.98 |
1.41 – 2.80 |
1.63 |
1.11 – 2.39 |
2.42 |
1.49 – 3.94 |
2.10 |
1.40 – 3.16 |
|||||
| Good health |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| 2a. |
Age in years |
1.03 |
1.02 – 1.04 |
1.03 |
1.02 – 1.04 |
1.03 |
1.01 – 1.04 |
1.02 |
1.00 – 1.03 |
1.04 |
1.02 – 1.06 |
||||
| 25 years |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Level of education |
|||||||||||||||
| Mandatory |
1.51 |
0.98 – 2.34 |
1.40 |
0.91 – 2.15 |
1.47 |
0.91 – 2.36 |
1.87 |
1.06 – 3.28 |
1.60 |
0.95 – 2.69 |
|||||
| Intermediate |
1.37 |
0.96 – 1.94 |
1.07 |
0.76 – 1.52 |
1.08 |
0.77 – 1.52 |
1.14 |
0.78 – 1.66 |
1.23 |
0.78 – 1.94 |
|||||
| University/university college |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| 2b. |
Age in years |
1.03 |
1.02 – 1.04 |
1.02 |
1.01 – 1.04 |
1.02 |
1.01 – 1.04 |
1.01 |
1.00 – 1.03 |
1.04 |
1.02 – 1.05 |
||||
| 25 years |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Level of education |
|||||||||||||||
| Mandatory |
1.45 |
0.94 – 2.25 |
1.30 |
0.84 – 2.01 |
1.40 |
0.87 – 2.27 |
1.71 |
0.97 – 3.02 |
1.50 |
0.88 – 2.54 |
|||||
| Intermediate |
1.35 |
0.95 – 1.92 |
1.05 |
0.74 – 1.49 |
1.07 |
0.76 – 1.50 |
1.11 |
0.76 – 1.62 |
1.22 |
0.77 – 1.93 |
|||||
| University/university college |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Self-reported health |
|||||||||||||||
| Poor health |
1.36 |
0.95 – 1.96 |
1.68 |
1.17 – 2.40 |
1.38 |
0.93 – 2.06 |
2.08 |
1.27 – 3.42 |
1.61 |
1.05 – 2.47 |
|||||
| Good health |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| 1. Univariate (unadjusted) analyses for choice of a doctor as a strategy for seeking help 2a. Multivariate analyses, model 1: Estimates for the choice of a doctor adjusted for age and level of education 2b. Multivariate analyses, model 2: Estimates for the choice of a doctor adjusted for age, level of education and self-reported health | |||||||||||||||
In the multivariate analyses, when adjusted for age, only the symptom «serious backache» would return a statistically significant higher odds rate for men with the mandatory level of education to choose to see a doctor, and when state of health was included in the model even this correlation disappeared (table 4). For women, on the other hand, all the education-related differences in terms of reported proclivity to see a doctor were statistically significant, even when controlled for age as well as state of health (table 5).
Table 5:
Logistic regression analyses, women: Would have gone to see a doctor first for advice or treatment if they suffered from (…)
| Dependent variables (attitude variables) |
|||||||||||||||
| … a very sore throat (n = 694) |
… a serious headache (n = 694) |
… serious sleeping problems (n = 692) |
… serious backache (n = 694) |
… all four symptoms (n = 692) |
|||||||||||
| Independent variables |
OR |
95 % CI |
OR |
95 % CI |
OR |
95 % CI |
OR |
95 % CI |
OR |
95 % CI |
|||||
| 1. |
Age in years |
1.02 |
1.01 – 1.03 |
1.04 |
1.03 – 1.05 |
1.02 |
1.01 – 1.03 |
1.01 |
1.00 – 1.02 |
1.05 |
1.03 – 1.06 |
||||
| 25 years |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Level of education |
|||||||||||||||
| Mandatory |
2.56 |
1.66 – 3.94 |
2.53 |
1.66 – 3.84 |
1.99 |
1.28 – 3.10 |
2.15 |
1.27 – 3.63 |
4.80 |
2.74 – 8.40 |
|||||
| Intermediate |
1.66 |
1.15 – 2.41 |
1.29 |
0.90 – 1.84 |
1.49 |
1.05 – 2.10 |
1.27 |
0.87 – 1.85 |
1.51 |
0.86 – 2.65 |
|||||
| University/university college |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Self-reported health |
|||||||||||||||
| Poor health |
1.19 |
0.83 – 1.69 |
1.62 |
1.15 – 2.29 |
1.52 |
1.05 – 2.18 |
1.60 |
1.05 – 2.44 |
1.40 |
0.88 – 2.22 |
|||||
| Good health |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| 2a. |
Age in years |
1.01 |
1.00 – 1.03 |
1.04 |
1.02 – 1.05 |
1.01 |
1.00 – 1.03 |
1.00 |
0.99 – 1.02 |
1.03 |
1.01 – 1.05 |
||||
| 25 years |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Level of education |
|||||||||||||||
| Mandatory |
2.21 |
1.39 – 3.52 |
1.66 |
1.05 – 2.61 |
1.71 |
1.07 – 2.75 |
2.07 |
1.19 – 3.62 |
3.30 |
1.81 – 6.02 |
|||||
| Intermediate |
1.58 |
1.09 – 2.30 |
1.11 |
0.77 – 1.60 |
1.42 |
1.00 – 2.01 |
1.25 |
0.85 – 1.84 |
1.32 |
0.75 – 2.33 |
|||||
| University/university college |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| 2b. |
Age in years |
1.01 |
1.00 – 1.03 |
1.03 |
1.02 – 1.05 |
1.01 |
1.00 – 1.02 |
1.00 |
0.99 – 1.02 |
1.03 |
1.01 – 1.05 |
||||
| 25 years |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Level of education |
|||||||||||||||
| Mandatory |
2.24 |
1.40 – 3.58 |
1.62 |
1.02 – 2.56 |
1.65 |
1.02 – 2.66 |
1.96 |
1.12 – 3.45 |
3.37 |
1.84 – 6.19 |
|||||
| Intermediate |
1.60 |
1.10 – 2.33 |
1.09 |
0.75 – 1.58 |
1.38 |
0.97 – 1.97 |
1.21 |
0.82 – 1.78 |
1.34 |
0.75 – 2.37 |
|||||
| University/university college |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| Self-reported health |
|||||||||||||||
| Poor health |
0.92 |
0.63 – 1.35 |
1.17 |
0.81 – 1.69 |
1.27 |
0.87 – 1.86 |
1.43 |
0.92 – 2.23 |
0.88 |
0.53 – 1.45 |
|||||
| Good health |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
1 |
– |
|||||
| 1. Univariate (unadjusted) analyses for choice of a doctor as a strategy for seeking help 2a. Multivariate analyses, model 1: Estimates for the choice of a doctor adjusted for age and level of education 2b. Multivariate analyses, model 2: Estimates for the choice of a doctor adjusted for age, level of education and self-reported health | |||||||||||||||
Health status
A cross-tabulation of self-reported state of health and the attitude variables showed that the proportion choosing a doctor tended to be higher among respondents with poor health, when compared to those with good health. The pattern was identical for both genders, even though the differences were more pronounced among the men (e-figure 3 and e-figure 4).
In the univariate analyses, poor state of health gave a statistically significant higher odds rate for choosing a doctor for all the attitude variables for men (table 4) and for three of the attitude variables – serious headache, serious sleeping problems and serious backache – for women (Table 5).
In the multivariate analyses, where the estimates for state of health were controlled for age and level of education, the correlation remained statistically significant for three of the attitude variables for the men (serious headache, serious backache and the collective variable), while no statistically significant correlation could be detected for the women.
Discussion
An analysis of Norwegian interview data indicates that there are statistically significant differences between educational groups with regard to attitudes to seeking medical attention in case of less serious afflictions, even when controlling for age and state of health. The proportion claiming that they would see a doctor is generally higher among women with lower levels of education for all of the hypothetical symptom scenarios in the study.
What causes the differences in attitude among the educational groups?
At this point, it is essential to emphasise that we have only investigated hypothetical behaviour with regard to seeking medical attention, and these data can therefore not reveal whether the observed patterns correspond to actual patterns of use of medical services by these groups. There is a possibility that the respondents report help-seeking strategies that they perceive to be more socially acceptable (7). Similarly, a stated intention to seek medical attention is no guarantee that a doctor will be contacted when the need arises, since a number of factors may restrict the individual’s freedom of action in the given situation, irrespective of whether he or she may or may not be in control of these circumstances (3, 11). These circumstances may include issues pertaining to place of residence (such as local availability of medical services), financial situation, family situation and social networks, as well as state of health, prior experience of the health services and health-related norms and values. If we restrict the discussion to this latter issue, we may interpret the responses as expressions of individual and cultural variations related to:
Expectations of bodily function and health, including the interpretation of bodily symptoms, tolerance of physical afflictions and opinions as to the meaning of good health.
Confidence in personal abilities to cope and in professional medical expertise.
Norms pertaining to seeking medical attention; what individuals believe one ought to hold to be an acceptable use of medical services.
These three factors – the degree of acceptance of afflictions, beliefs regarding the best source of help and norms about what we ought to do – are likely to interact in a complex and unsystematic manner. The conviction that we should not see a doctor before this is absolutely imperative is not necessarily accompanied by a pronounced confidence in personal capabilities and a high degree of tolerance; for example, we may be of the opinion that seeking medical attention should be avoided as far as possible, but still have a high confidence in professional medical assistance and a low degree of tolerance. This complexity makes it difficult to draw any conclusions regarding the implications of the results of the analysis.
Since the threshold for hypothetical seeking of medical assistance is composed of a number of different factors, while the pattern in the responses is relatively consistent, it is unlikely that the threshold hypothesis alone may explain our findings. An alternative hypothesis, therefore, is that the systematic patterns indicate that the informants should be perceived as carriers of culture, and that their individually espoused attitudes should be interpreted as expressions of cultural norms and values within the educational group to which they belong. In this case, the results of the analyses are expressions of cultural variations between educational groups, since cultural norms and values associated with seeking medical attention are systematically correlated with levels of education among women. One example: What norms and values will apply when the question concerns whether it is good or bad to see a doctor in order to address minor physical conditions? The results indicate that the norm «one should seek to rely on oneself» has a stronger position among women with higher levels of education than among those with less education. In other words, it may be less socially and culturally acceptable for a highly educated woman to report that she goes to see a doctor for a headache or a sore throat – and thereby possibly admit that she has little confidence in her own abilities or is unable to cope with this on her own – than for a woman with a lower level of education.
Does education affect the seeking of medical assistance differently among men and women?
The results showed modest differences between the genders in terms of hypothetical seeking of medical attention. Thus, we can not assert that men have a significantly lower threshold for seeking of medical attention than women, or vice versa. This is in accordance with findings from previous studies (12, 13). At the same time, there seems to be a difference between men and women with regard to the impact of education and health respectively on the likelihood of choosing to see a doctor, since the co-variation between education and hypothetical seeking of medical attention is stronger for women than for men, while the co-variation between health and hypothetical seeking of medical attention is stronger for men than for women.
Our analyses indicate that the threshold for hypothetical seeking of medical attention varies according to socio-economic position for women in particular. Previous studies of the correlation between education and hypothetical seeking of medical help (12, 14, 15) have found similar patterns related to education, although the apparently different impact of education on the attitudes of men and women respectively have not been previously reported.
Limitations of the study
Since all the data were collected at the same time, we are unable to determine the direction of significant associations within the data set. Furthermore, the specific symptoms on which the study is based constitute a limited selection of what can be described as minor afflictions. The results are therefore not amenable to generalisation to other and more serious conditions. A further limitation of our study is that it refers only to norms and attitudes; whether these norms will be reflected in actual behaviour remains an open question.
The selection of explanatory variables is also rather modest, and the results may well be swayed in other directions if controls for the effects of other confounding factors are introduced. An interesting observation, however, is that the effect of education in analyses of men is non-significant when adjusted for age and state of health. The observed differences in the results of the multivariate analyses of men and women respectively may indicate that the effect of education on hypothetical seeking of medical attention is weaker for men than for women (figures 1 and 2), that education does not have any significant effect on hypothetical seeking of medical attention for men, or that our study does not have the strength to determine any such effect.
Characteristics of the education variable may also have influenced the results. The Norwegian study suffered from a selective attrition related to level of education, meaning that respondents with low levels of education are underrepresented in relation to respondents with the highest level of education (7, 16). Furthermore, education is self-reported in the ESS, and the self-reported levels of education differ from registry-based data on education for the sample. The discrepancy is higher for men, and overreporting of levels is a greater problem than underreporting. However, the scope of this problem is reduced when analyses are based on a three-level variable similar to the one we have been using (16).
Conclusion
Attitudes to hypothetical seeking of medical attention in the Norwegian population, and among women in particular, appear to be socially structured according to levels of education. Our interpretation of the education-related differences in hypothetical seeking of medical attention among women is that these patterns do not reflect individual attitudes, but are expressions of cultural norms and values. In other words, the results elucidate how various social strata in the population perceive that they ought to think and act, reflecting what is recognised as socially acceptable in given situations. Since the education-related patterns for women are fairly systematically distributed between different educational groups, this may indicate that levels of education have an impact on norms for seeking of medical attention.
Tabell
| Main message |
|
- 1.
St.meld nr. 20 (2006 – 2007). Nasjonal strategi for å utjevne sosiale helseforskjeller. Oslo: Helse- og omsorgsdepartementet, 2007.
- 2.
Strand BH, Grøholt E-K, Steingrímsdóttir ÓA et al. Educational inequalities in mortality over four decades in Norway: prospective study of middle aged men and women followed for cause-specific mortality, 1960 – 2000. BMJ 2010; 340: c654. doi; 10.1136/bmj.c654.
- 3.
Korsnes O. red. Sosiologisk leksikon. Oslo: Universitetsforlaget, 2008: 113 – 14.
- 4.
Den europeiske samfunnsundersøkelsen. ESS Round 2: European Social Survey Round 2 Data (2004). Data file edition 3.1. Norwegian Social Science Data Services, Norway – Data Archive and distributor of ESS data. Bergen: Norsk samfunnsvitenskapelige datatjeneste, 2004. http://ess.nsd.uib.no/ (18.11.2011).
- 5.
Den europeiske samfunnsundersøkelsen. ESS Round 2: European Social Survey (2008): ESS-2 2004 Documentation Report. Edition 3.2. European Social Survey Data Archive, Norwegian Social Science Data Services. Bergen: Norsk samfunnsvitenskapelige datatjeneste, 2008. http://ess.nsd.uib.no/ (18.11.2011).
- 6.
Norsk samfunnsvitenskapelig datatjeneste. ESS Data – European Social Survey Data archive. http://ess.nsd.uib.no/ (18.11.2011).
- 7.
Stoop I, Billiet J, Koch A et al. Improving survey response: Lessons learned from the European Social Survey. Chichester: John Wiley, 2010.
- 8.
Elstad JI. Utdanning og helseulikheter: Problemstillinger og forskningsfunn. IS-1573. Oslo: Helsedirektoratet, 2008.
- 9.
SSB. Norsk standard for utdanningsgruppering, Revidert 2000. Oslo: Statistisk sentralbyrå, 2001.
- 10.
Eikemo TA. Social inequalities in self-assessed health between European welfare regimes: evidence from the European Social Survey. Doktoravhandling. Trondheim: Norges teknisk-naturvitenskapelige universitet, 2008: 147.
- 16.
Kleven Ø, Ringdal K. A comparison of two ways of measuring level of education in Norway: Questions in survey interviews versus register data. http://ess.nsd.uib.no/bibliography/details/publication/181 (7.12.2011).