Poisonings by substances of abuse at the Oslo Accident and Emergency Outpatient Clinic 2014–18
Main findings
The incidence of poisonings related to substances of abuse at the Oslo Accident and Emergency Outpatient Clinic (OAEOC) remained stable from 2014 to 2017, with a transient decline in 2016 followed by an increase in 2018.
In 2018, OAEOC treated 4 021 poisonings related to substances of abuse, of which 2 022 were lone ethanol poisonings.
From 2014 to 2018, the incidence increased for most substances, but fell for heroin and benzodiazepines. The prevalence of unspecified opioids, probably more long-acting, increased in 2017 and 2018.
Poisoning by a substance of abuse is dangerous in itself as well as a marker for risky substance use behaviour. Cohort studies in Oslo found that mortality was 5–10 times higher than expected 5–20 years after a poisoning by a substance of abuse, and up to 30 times higher after an opioid poisoning (1–3).
The panorama of substances that appear in poisonings varies over time and from one place to another (4–6). In recent years we have seen an epidemic of opioid overdoses and deaths, especially in the United States (6), and an increasing use of fentanyl derivates (5, 7). Furthermore, a large number of new intoxicants have appeared, frequently referred to as novel psychoactive substances (NPS), more than 600 different types of which have been reported in Europe in the last decade (5, 8).
Currently, 250–300 deaths from drug overdoses occur in Norway each year, and another 350–400 deaths are alcohol-related (9, 10). Ethanol is by far the most common intoxicant in Norway and accounted for a little more than one-half of all poisonings from substances of abuse treated at the Oslo Accident and Emergency Outpatient Clinic (OAEOC) in 2012 (11, 12). Cannabis, heroin, amphetamine, cocaine and benzodiazepines have been in use in Norway since the 1960s and 1970s (10). Methylenedioxymethamphetamine (MDMA) appeared in the 1980s, and gamma-hydroxybutyrate (GHB) in the 1990s (10). Novel psychoactive substances are now also found here. Paramethoxymethamphetamine (PMMA) took many lives in Norway during an outbreak in 2010–11 (13), and novel psychoactive substances were detected in 8 % of all poisonings by substances of abuse in Oslo in 2014 (14).
Monitoring of trends in poisonings by substances of abuse provides knowledge on what we can expect to encounter and thereby makes us better prepared to deal with patients. Updated studies are constantly needed, and monitoring of poisonings by substances of abuse in Oslo contributes to an overview of the situation in Europe. In Oslo, most poisonings by substances of abuse are treated at OAEOC, and the prevalence has previously been identified in studies, most recently in 2008 and 2012 (15, 16).
We describe trends over time in poisonings by substances of abuse treated at the OAEOC from 2014 to 2018, and focus on the substances taken, simple data on the course of illness, and the patients' sex and age.
Material and method
The study was observational, with retrospective data registration from patient records at the general emergency department at OAEOC for the period 1 January 2014 to 31 December 2018. The study was based on the inclusion criteria and variable set developed by the European Drug Emergencies Network (Euro-DEN) (4, 17).
Setting
OAEOC, located in the city centre at no. 40 Storgata, is open 24 hours and has approximately 200 000 consultations per year, divided between its general emergency and trauma departments. The general emergency department treats most of the poisonings by substances of abuse in Oslo in accordance with a locally developed systematic procedure (12).
Inclusion
The patients were identified by a review of the registration lists in the electronic records system of the OAEOC's general emergency department. We included all patients who had been treated for poisoning by a substance of abuse, defined as a toxic effect of a psychoactive substance that the patient had ingested to achieve a state of intoxication. Patients were not included if the drug had been taken with a suicidal intent or inflicted involuntarily. In accordance with the Euro-DEN inclusion criteria, which we applied for the first four years, we did not include patients with lone alcohol poisoning. To improve comparability with previous local studies, in which ethanol poisonings accounted for one-half of all poisonings by substances of abuse (15, 16), we expanded the inclusion criteria from 2018 onwards to also encompass intoxication-related ethanol poisonings.
The inclusion and data registration were undertaken sequentially by the last author and medical students under the supervision of the last author.
Data registration
We registered the patient's sex and age, the substances taken, time of arrival, observation time at the clinic and any further measures taken. The diagnosis of toxic agents was based on the recorded assessment made by the doctor responsible for treatment, which in turn was based on information from the patient, companions, ambulance personnel and/or the police, as well as clinical symptoms and signs. No toxicological laboratory diagnostics were undertaken. Amphetamine and methamphetamine were categorised as a single substance.
Statistics
To describe trends in the occurrence of the various substances we estimated incidences per 1 000 inhabitants per year, based on the number of poisonings at the OAEOC and the number of inhabitants in the City of Oslo aged ≥ 12 years (18).
The analyses were performed in IBM SPSS version 25. We described categorical variables as numbers and percentages, and continuous variables as median values and interquartile ranges.
Ethics
The study was undertaken as a quality assurance project and the data protection officer at Oslo University Hospital assessed it as not subject to submission to the Regional Committee for Medical and Health Research Ethics.
Results
A total of 8 116 cases of poisoning by substances of abuse were treated at the OAEOC in the period 2014–18, lone alcohol poisonings not included. The median age of the patients was 34 years (interquartile range 27–43, age range 13–85), 6 236 (77 %) were men. The most frequent substances were heroin with 3 237 (40 %) cases, benzodiazepines with 2 196 (27 %) and amphetamine/methamphetamine with 1 827 (23 %) (Table 1).
Table 1
Substances of abuse taken in substance use-related poisonings treated at the OAEOC 2014–18. The diagnosis of toxic agents was based on the clinical assessment made by the doctor responsible. Some patients had taken multiple toxic agents. Results are given as number (n) (%).
|
| 2014 | 2015 | 2016 | 2017 | 2018 | Total (n = 8 116) |
|---|---|---|---|---|---|---|
| Heroin | 715 (45) | 703 (44) | 620 (47) | 527 (33) | 672 (34) | 3 237 (40) |
| Benzodiazepines | 496 (31) | 495 (31) | 387 (29) | 397 (25) | 421 (21) | 2 196 (27) |
| Amphetamine/methamphetamine | 313 (20) | 368 (23) | 312 (24) | 394 (24) | 440 (22) | 1 827 (23) |
| Cannabis | 181 (12) | 225 (14) | 165 (12) | 228 (14) | 282 (14) | 1 081 (13) |
| Gamma-hydroxybutyrate (GHB) | 152 (10) | 169 (11) | 140 (11) | 200 (12) | 243 (12) | 904 (11) |
| Cocaine | 99 (6) | 111 (7) | 74 (6) | 103 (6) | 182 (9) | 569 (7) |
| Methylenedioxymethamphetamine (MDMA) | 38 (2) | 47 (3) | 62 (5) | 68 (4) | 76 (4) | 291 (4) |
| Methadone | 42 (3) | 52 (3) | 48 (4) | 71 (4) | 44 (2) | 257 (3) |
| Buprenorphine | 40 (3) | 24 (1) | 17 (1) | 22 (1) | 18 (1) | 121 (1) |
| Lysergic acid diethylamide (LSD) | 16 (1) | 18 (1) | 18 (1) | 16 (1) | 47 (2) | 115 (1) |
| Z-hypnotics | 16 (1) | 16 (1) | 15 (1) | 13 (1) | 8 (< 0,5) | 68 (1) |
| Other/unspecified opioids1 | 110 (7) | 126 (8) | 40 (3) | 169 (11) | 268 (13) | 713 (9) |
| Other | 58 (4) | 53 (3) | 71 (5) | 80 (5) | 63 (3) | 325 (4) |
| Unknown | 38 (2) | 40 (2) | 62 (5) | 192 (12) | 145 (7) | 477 (6) |
| Ethanol2 | 418 (27) | 455 (28) | 351 (26) | 428 (27) | 573 (29) | 2 225 (27) |
1Unspecified opioids accounted for a total of 546 (77 % of other/unspecified opioids), with 69, 93, 15, 135 and 234 for the years 2014–18 respectively
2Ethanol taken in addition to other toxic agents. Does not include lone alcohol poisonings
Trends
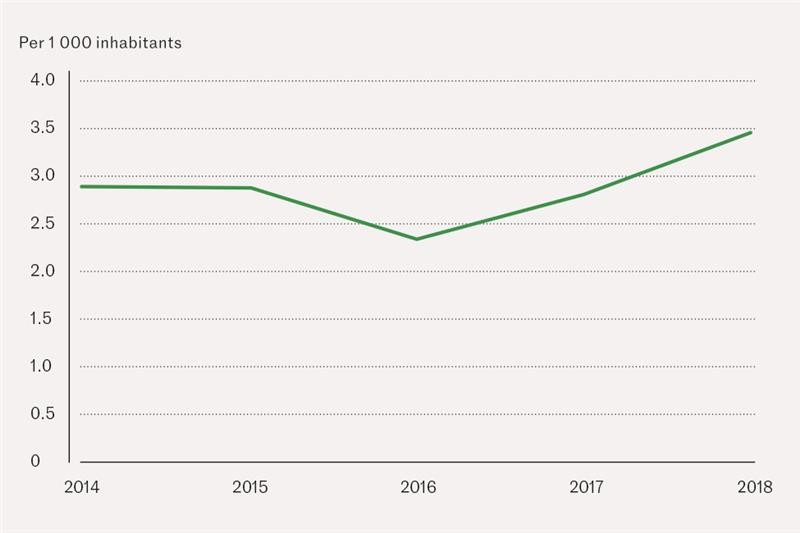
The incidence of poisonings by substances of abuse was 2.90 per 1 000 inhabitants in 2014 and remained stable at that level, followed by a dip to 2.35 in 2016 and an increase to 3.45 in 2018 (Figure 1). The decline in 2016 applied to all substances with the exception of MDMA.
From 2014 to 2018, the incidence of poisonings by heroin fell from 1.32 per 1 000 inhabitants to 1.16, accompanied by an increase in other/unspecified opioids from 0.20 to 0.46 (Table 2). The incidence for central stimulants increased: amphetamine/methamphetamine from 0.58 to 0.76, cocaine from 0.18 to 0.31 and MDMA from 0.07 to 0.13. The incidence also increased for cannabis (from 0.33 to 0.49) and GHB (from 0.28 to 0.42), but decreased for benzodiazepines (from 0.91 to 0.73).
Table 2
Number of poisonings by substances of abuse treated at OAEOC 2014–18 per 1 000 inhabitants per year. The diagnosis of toxic agents was based on the clinical assessment made by the doctor responsible. Some patients had taken multiple toxic agents.
|
| 20141 | 20151 | 20161 | 20171 | 20181 |
|---|---|---|---|---|---|
| Heroin | 1.32 | 1.27 | 1.10 | 0.92 | 1.16 |
| Amphetamine/methamphetamine | 0.58 | 0.66 | 0.55 | 0.69 | 0.76 |
| Benzodiazepines | 0.91 | 0.89 | 0.69 | 0.69 | 0.73 |
| Cannabis | 0.33 | 0.41 | 0.29 | 0.40 | 0.49 |
| Other/unspecified opioids2 | 0.20 | 0.23 | 0.07 | 0.30 | 0.46 |
| Gamma-hydroxybutyrate (GHB) | 0.28 | 0.30 | 0.25 | 0.35 | 0.42 |
| Cocaine | 0.18 | 0.20 | 0.13 | 0.18 | 0.31 |
| Methylenedioxymethamphetamine (MDMA) | 0.07 | 0.08 | 0.11 | 0.12 | 0.13 |
| Methadone | 0.08 | 0.09 | 0.09 | 0.12 | 0.08 |
| Lysergic acid diethylamide (LSD) | 0.03 | 0.03 | 0.03 | 0.02 | 0.08 |
| Buprenorphine | 0.07 | 0.04 | 0.03 | 0.04 | 0.03 |
1The estimated incidences are based on the number of inhabitants in the City of Oslo aged ≥ 12 years; 2014: 543 154; 2015: 554 618; 2016: 564 351; 2017: 571 946; 2018: 578 635 (18)
2Unspecified opioids accounted for 77 % of the cases of other/unspecified opioids
The gender distribution remained unchanged through the period with around 77 % men, and the median age remained stable at approximately 34 years (Table 3). The proportion of patients who were brought in by ambulance increased from 56 % to 66 %. In the same period, the proportion of patients admitted to a somatic hospital fell from 18 % to 11 %. No patients died at OAEOC.
Table 3
Demography and trajectory for patients treated for poisoning by substances of abuse at the OAEOC 2014–18. Lone ethanol poisonings are not included. Results are given as n (%).
|
| 2014 | 2015 | 2016 | 2017 | 2018 | Total | |
|---|---|---|---|---|---|---|---|
| Sex |
|
|
|
|
|
| |
|
| Men | 1 234 (78) | 1 236 (77) | 1 014 (76) | 1 214 (75) | 1 538 (77) | 6 236 (77) |
|
| Women | 342 (22) | 369 (23) | 313 (24) | 395 (25) | 461 (23) | 1 880 (23) |
| Age, median (interquartile range)1 | 34 (26–45) | 34 (27–44) | 34 (26–43) | 33 (27–42) | 35 (27–44) | 34 (27–43) | |
| Brought by ambulance | 887 (56) | 922 (57) | 801 (60) | 992 (62) | 1323 (66) | 4 925 (61) | |
| Observation time, median (interquartile range) | 3:57 | 3:31 | 3:41 | 4:02 | 3:45 | 3:47 | |
| Further measures2 |
|
|
|
|
|
| |
|
| Transferred to somatic hospital | 287 (18) | 285 (18) | 247 (19) | 257 (16) | 211 (11) | 1 287 (16) |
|
| Transferred to psychiatric hospital | 63 (4) | 65 (4) | 58 (4) | 39 (2) | 98 (5) | 323 (4) |
|
| Treatment completed at OAEOC | 937 (59) | 1026 (64) | 779 (59) | 1047 (65) | 1391 (70) | 5 180 (64) |
|
| Left OAEOC during treatment | 288 (18) | 229 (14) | 243 (18) | 266 (17) | 298 (15) | 1 324 (16) |
| Total | 1 576 (100) | 1 605 (100) | 1 327 (100) | 1 609 (100) | 1 999 (100) | 8 116 (100) | |
1Data missing for 162 cases
2Data missing for two cases
Ethanol in 2018
In 2018, there were 2 022 lone ethanol poisonings. The median age was 38 years (interquartile range 24–53, age range 13–85), 1 329 (66 %) were men. The median observation time at OAEOC was 3 h 32 min (interquartile range 1 h 56 min – 5 h 10 min), after which 73 (4 %) were admitted to a somatic hospital, 10 (0.5 %) to a psychiatric hospital, 1 592 completed their treatment at OAEOC and 347 (17 %) left the clinic during treatment. No patients died at OAEOC.
Including the poisonings in which ethanol had been taken in addition to other substances, there was a total of 2 595 ethanol poisonings in 2018, an incidence of 4.48 per 1 000 inhabitants.
There was a total of 4 021 poisonings by substances of abuse in 2018, an incidence of 6.95 per 1 000 inhabitants.
Discussion
When lone alcohol poisonings are excluded, the total incidence of poisonings by substances of abuse treated at the OAEOC remained stable from 2014 to 2017, with a transient decline in 2016, followed by an increase to 3.45 per 1 000 inhabitants in 2018. Over the five-year period, the incidence increased for most of the substances, but declined for heroin and benzodiazepines. More patients were brought in by ambulance, but fewer were admitted to a somatic hospital. When lone ethanol poisonings are included, altogether 4 021 patients were treated for poisoning by substances of abuse at the OAEOC in 2018, an incidence of 6.95 per 1 000 inhabitants.
Trends
Compared to previous studies, the number of poisonings by substances of abuse treated at the OAEOC has increased markedly, from 1 714 in 2008 via 2 328 in 2012 to 4 021 in 2018 (15, 16). Estimated in the same way as in our study, the incidence was 3.57 per 1 000 inhabitants in 2008 and 4.44 in 2012 (inhabitants in the City of Oslo aged ≥ 12 years: 480 782 in 2008; 524 704 in 2012 (18)), compared to 6.95 in 2018.
Numerically, the greatest increase was for ethanol, from 1 236 in 2008 via 1 684 in 2012 to 2 595 in 2018 (15, 16). The total alcohol consumption in Norway has remained stable since 2012, while alcohol use is declining among young people (11). Seeing that the number of alcohol poisonings is nevertheless increasing, a possible explanation is that those who drink a lot drink more than before, a pattern which has been observed both in Sweden and the UK (19, 20). Another possibility is that alcohol consumption has moved out of people's homes and into pubs and bars, which increases the likelihood of being in a public space when the alcohol poisoning occurs.
Among the opioids, there was a clear decline in the incidence of heroin poisonings. One possible explanation is that more heroin overdoses take place in the supervised injection site (municipal premises for injection of substances) and are treated there (21). However, over this five-year period there was also a decline in the amount of heroin seized by the police, which may indicate that there is less heroin on the streets (22).
Towards the end of the period, the incidence of poisonings by unspecified opioids increased. The doctors at the general emergency department of OAEOC often record 'unspecified opioid' as the toxic agent when no specific information is available and the patient continues to appear clinically under the influence of opioids after the intoxicant effect of heroin should have passed. This may indicate that long-acting opioids are appearing more frequently than before, which is clear from the development in overdose deaths (9). The increase in unspecified opioids may conceal an increase in the number of poisonings by methadone and buprenorphine, which in our material were stable and declining respectively. In a study from 2014 with toxicological laboratory testing we detected methadone in many patients in which this was not clinically suspected (14).
Illegal fentanyl derivates and/or long-acting formulations of opioid analgesics are also possible agents. Poisonings with these are increasing in other European countries and the United States (5, 7), and police seizures of these drugs also increased in Norway in 2017 and 2018 (22). The prescribing of oxycodone medications in Norway increased by 27 % from 2014 to 2018 (23). The increasing occurrence of poisonings by long-acting opioids gives grounds for concern, especially in light of the American opioid overdose epidemic (6).
The increase in the number of poisonings by central stimulants from 2014 to 2018 is a trend that has been observed since 2008 (15, 16). The number of poisonings by GHB increased by 150 % from 2008 to 2012, before stabilising until a new increase occurred in 2017 and 2018. This reflects the curve for police seizures (22).
The incidence of cannabis poisoning was increasing. This tendency has been clear from as far back as 2008 (15, 16). Since 2012, the use and number of seizures have remained stable, but the cannabis has become more potent (9, 22). In most cases and as previously, cannabis was most likely taken in addition to the drug that was the main reason for the patient being brought to OAEOC (16).
The fact that more patients were brought in by ambulance and fewer were sent to hospital from OAEOC may indicate that some of the OAEOC patients suffered less serious poisonings than before. A possible explanation is that the public has a lower threshold for calling an ambulance. Another possibility is that more people are taking drugs in public spaces and therefore are found when they take an overdose.
Strengths and limitations
The data collection was retrospective, and inclusion depended on the patient having been registered with a presentation that gave rise to suspicion of poisoning by a substance of abuse. Some cases are therefore likely to have eluded inclusion.
The majority of poisonings by substances of abuse in Oslo are treated at OAEOC. However, the most serious cases are brought directly to hospital by the ambulance service, approximately 300 per year, and some patients remain on site after having been treated by the ambulance personnel, including approximately 350 per year who have received naloxone to counteract opioid poisoning (12, 21). Additional to these are approximately 100 overdose deaths per year (9, 10) and an unknown number of people who survive their poisoning without any contact with the healthcare system. Our figures therefore do not provide a complete picture of the poisonings by substances of abuse in the city, but give a good indication for the Oslo region.
The incidences that we have estimated are not exact measurements of the incidences of poisonings by substances of abuse among the inhabitants of Oslo, but a suitable indication of trends over time. Although one-third of the OAEOC's patients with poisoning by a substance of abuse came from outside the city (24), we chose to use the population of Oslo as the basis for estimating incidences. To have a representative risk population, we set the lower age limit at 12 years, since poisonings by substances of abuse are extremely rare among persons younger than this.
The diagnostics of the substances involved were not based on toxicological analyses, but on the clinical judgement of the doctor responsible for treatment. This makes the diagnosis of the toxic agents imprecise. However, studies that compare clinical judgement with laboratory diagnostics tend to find that the patients have generally taken the substances that were clinically suspected, in addition to some others (14).
Although the last author instructed and supervised the medical students who collected the data, there may have been systematic variations in the way in which the inclusion criteria and the classification of toxic agents were applied. This could be an explanation for the fall in incidence in 2016. The police seizures were not particularly large or small that year (22). However, the incidence of MDMA increased while the incidence of heroin fell even further in the following year, which may indicate that the findings for 2016 are genuine.
We categorised amphetamine and methamphetamine together, since their clinical pictures are similar and the users in Oslo rarely distinguish between them. In the study period, methamphetamine accounted for a little under one-third of the police's total seizures of amphetamine and methamphetamine combined (22).
Conclusion
The incidence of poisonings by substances of abuse in OAEOC remained stable from 2014 to 2017, with a transient decline in 2016 and an increase in 2018. In the period 2014–18, the incidence of most of the substances increased, with the exception of heroin and benzodiazepines. This is worrisome, since the unspecified opioids may represent more potent and/or long-acting opioids.
The article has been peer reviewed.
- 1.
Bjornaas MA, Jacobsen D, Haldorsen T et al. Mortality and causes of death after hospital-treated self-poisoning in Oslo: a 20-year follow-up. Clin Toxicol (Phila) 2009; 47: 116–23. [PubMed][CrossRef]
- 2.
Bjornaas MA, Bekken AS, Ojlert A et al. A 20-year prospective study of mortality and causes of death among hospitalized opioid addicts in Oslo. BMC Psychiatry 2008; 8: 8. [PubMed][CrossRef]
- 3.
Lund C, Bjornaas MA, Sandvik L et al. Five-year mortality after acute poisoning treated in ambulances, an emergency outpatient clinic and hospitals in Oslo. Scand J Trauma Resusc Emerg Med 2013; 21: 65. [PubMed][CrossRef]
- 4.
Dines AM, Wood DM, Yates C et al. Acute recreational drug and new psychoactive substance toxicity in Europe: 12 months data collection from the European Drug Emergencies Network (Euro-DEN). Clin Toxicol (Phila) 2015; 53: 893–900. [PubMed][CrossRef]
- 5.
European drug report 2019: trends and developments. Lisbon, Portugal: European monitoring centre for drugs and drug addiction (EMCDDA), 2019. https://www.emcdda.europa.eu/edr2019_en Accessed 4.4.2020.
- 6.
Kolodny A, Courtwright DT, Hwang CS et al. The prescription opioid and heroin crisis: a public health approach to an epidemic of addiction. Annu Rev Public Health 2015; 36: 559–74. [PubMed][CrossRef]
- 7.
Wilson N, Kariisa M, Seth P et al. Drug and opioid-involved overdose deaths: United States, 2017–2018. MMWR Morb Mortal Wkly Rep 2020; 69: 290–7. [PubMed][CrossRef]
- 8.
Krabseth HM, Tuv SS, Strand MC et al. Nye psykoaktive stoffer. Tidsskr Nor Legeforen 2016; 136: 714–7. [PubMed][CrossRef]
- 9.
Folkehelseinstituttet. Narkotika i Norge. https://www.fhi.no/nettpub/narkotikainorge/ Accessed 4.4.2020.
- 10.
Skretting A, Bye EK, Vedøy TF et al. Rusmidler i Norge 2016. Oslo: Folkehelseinstituttet; 2016. https://www.fhi.no/publ/2017/rusmidler-i-norge-2016/ Accessed 4.4.2020.
- 11.
Folkehelseinstituttet. Alkohol i Norge. https://www.fhi.no/nettpub/alkoholinorge/ Accessed 4.4.2020.
- 12.
Vallersnes OM, Jacobsen D, Ekeberg Ø et al. Outpatient treatment of acute poisoning by substances of abuse: a prospective observational cohort study. Scand J Trauma Resusc Emerg Med 2016; 24: 76. [PubMed][CrossRef]
- 13.
Vevelstad M, Øiestad EL, Middelkoop G et al. The PMMA epidemic in Norway: comparison of fatal and non-fatal intoxications. Forensic Sci Int 2012; 219: 151–7. [PubMed][CrossRef]
- 14.
Vallersnes OM, Persett PS, Øiestad EL et al. Underestimated impact of novel psychoactive substances: laboratory confirmation of recreational drug toxicity in Oslo, Norway. Clin Toxicol (Phila) 2017; 55: 636–44. [PubMed][CrossRef]
- 15.
Lund C, Vallersnes OM, Jacobsen D et al. Outpatient treatment of acute poisonings in Oslo: poisoning pattern, factors associated with hospitalization, and mortality. Scand J Trauma Resusc Emerg Med 2012; 20: 1. [PubMed][CrossRef]
- 16.
Vallersnes OM, Jacobsen D, Ekeberg Ø et al. Patients presenting with acute poisoning to an outpatient emergency clinic: a one-year observational study in Oslo, Norway. BMC Emerg Med 2015; 15: 18. [PubMed][CrossRef]
- 17.
Wood DM, Heyerdahl F, Yates CB et al. The European Drug Emergencies Network (Euro-DEN). Clin Toxicol (Phila) 2014; 52: 239–41. [PubMed][CrossRef]
- 18.
Oslo kommune. Statistikkbanken. https://statistikkbanken.oslo.kommune.no Accessed 1.7.2019.
- 19.
Hallgren M, Leifman H, Andréasson S. Drinking less but greater harm: could polarized drinking habits explain the divergence between alcohol consumption and harms among youth? Alcohol Alcohol 2012; 47: 581–90. [PubMed][CrossRef]
- 20.
Holmes J, Ally AK, Meier PS et al. The collectivity of British alcohol consumption trends across different temporal processes: a quantile age-period-cohort analysis. Addiction 2019; 114: 1970–80. [PubMed][CrossRef]
- 21.
Madah-Amiri D, Skulberg AK, Braarud AC et al. Ambulance-attended opioid overdoses: An examination into overdose locations and the role of a safe injection facility. Subst Abus 2019; 40: 383–8. [PubMed][CrossRef]
- 22.
Narkotika- og dopingstatistikk 2019. Oslo: KRIPOS, 2019. https://www.politiet.no/globalassets/04-aktuelt-tall-og-fakta/narkotika/narkotika-og-dopingstatistikk-kripos-2019.pdf Accessed 4.4.2020.
- 23.
Folkehelseinstituttet. Reseptregisteret. http://www.reseptregisteret.no Lest 24.4.2020.
- 24.
Akopian M, Vallersnes OM, Jacobsen D et al. Levekår i Oslos bydeler og legevaktbehandlet rusmiddelforgiftning. Tidsskr Nor Legeforen 2015; 135: 1943–8. [PubMed][CrossRef]