Adherence to the Scandinavian guidelines for initial management of minimal, mild and moderate head injuries in adults
Main findings
The Scandinavian guidelines for initial management of minimal, mild and moderate head injuries in adults were followed for 96 out of 150 (64 %) patients treated at the University Hospital of North Norway, Tromsø.
Overtesting in the form of a (non-recommended) CT scan was performed for 30 of 150 (20 %) patients, and was the most common reason for non-compliance.
The majority of patients with a head injury are conscious during the initial assessment. The aim of the initial management is to identify those patients at risk of developing traumatic intracranial haematoma, while also avoiding unnecessary computed tomography (CT) scans and hospital admissions.
In 2013, the Scandinavian Neurotrauma Committee (SNC) published guidelines for the initial management of adults with minimal, mild or moderate head injuries (1). A literature review that used the Appraisal of Guidelines for Research and Evaluation (AGREE) II criteria to assess the quality of ten guidelines, found the Scandinavian guidelines to be among the top three in terms of meeting these criteria (2). A validation study of five guidelines found that the Scandinavian guidelines had a good balance between sensitivity and specificity, and that their adoption led to the greatest reduction in the use of CT scans, without intracranial haematomas being missed (3).
There is growing concern that ionising radiation, even in moderate doses, may be oncogenic (4), and in Norway the radiation protection authorities have expressed concern about the increasing use of CT scans. The aim of this study was therefore to examine compliance with the Scandinavian guidelines at the University Hospital of North Norway, Tromsø.
Material and method
The University Hospital of North Norway, Tromsø is a local hospital for 167 202 inhabitants in Troms county (2018). The majority of head injuries are assessed by general practitioners on call at a local emergency room, with patients referred to hospital if the severity of their injury – as assessed using the Scandinavian guidelines – is greater than minimal (1). The emergency medical dispatch centre can also arrange direct transport to the hospital if a serious head injury is suspected.
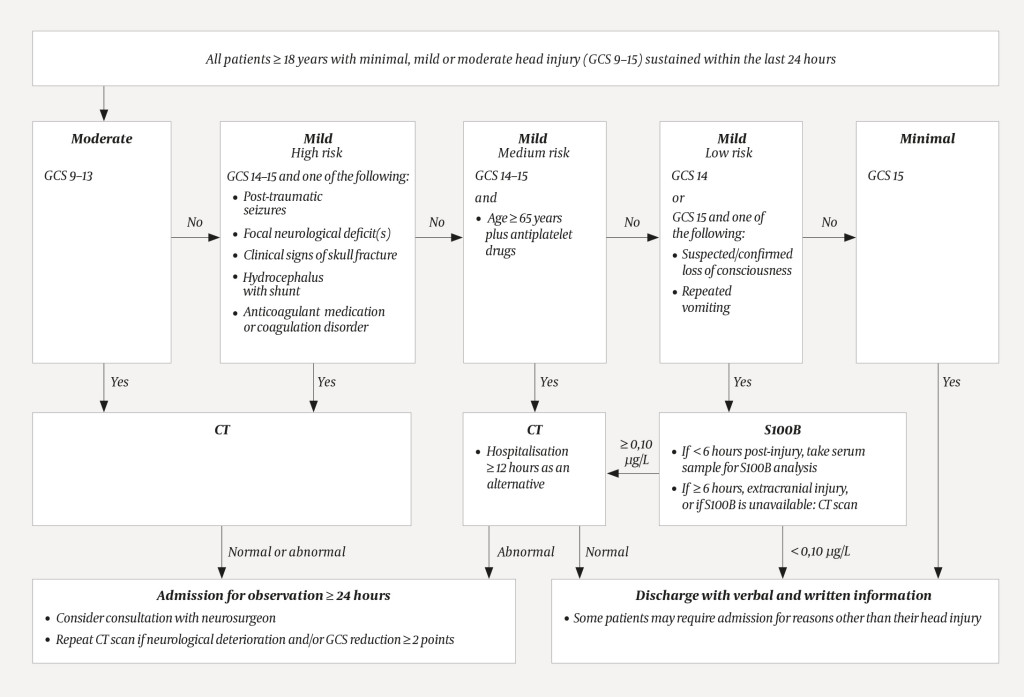
Triage in the Accident and Emergency department is performed by a nurse. Patients with a score > 13 on the Glasgow Coma Scale (GCS) without focal neurological deficits are examined by a specialty registrar in general surgery, while patients with a GCS score ≤ 13 and/or focal neurological deficits are examined by a specialty registrar in neurosurgery. The hospital performs CT scans as well as analysis of the brain injury marker S100B, which is released into the bloodstream upon damage to glial cells. The Scandinavian Neurotrauma Committee guidelines recommends the test as an alternative to a CT scan for mild, low-risk head injuries (Figure 1).
We conducted a study of all adult patients with minimal, mild or moderate head injuries assessed in Acute Admissions in the period 1 September 2018–31 August 2019. A search in the patient administration system identified 448 patients with an ICD-10 diagnosis code for head injury. We included 150 patients aged ≥ 18 years who were assessed within 24 hours of injury. A total of 298 patients were excluded because they either had a serious head injury (GCS score < 9), had inadequate medical records such that their GCS score could not be calculated (n = 8), did not have a head injury (miscoded), or because they arrived at the hospital following a trauma alert in accordance with the national trauma system criteria (such cases are managed using other guidelines).
A retrospective review of the medical records was performed and the following information recorded: age and sex, relevant previous illnesses, use of anticoagulants and antiplatelet agents, history of the injury (loss of consciousness, nausea/vomiting and seizures after the injury) and findings upon clinical examination (GCS score, focal neurological deficits and clinical signs of skull fracture).
In 42 patients for whom GCS scores were not recorded, we were able to calculate the scores using information in the medical records on eye opening as well as motor and verbal responses. We also recorded whether a CT scan and/or S100B analysis had been performed, plus any results, and whether the patient had been admitted for observation. Management was categorised as either compliant or non-compliant with the Scandinavian guidelines (Figure 1). We defined non-compliance as overtesting (unnecessary CT scan and/or hospital admission) or undertesting (omission of necessary CT scan and/or hospital admission).
The study was approved by the Data Protection Officer as a quality assurance project (no. 02344).
Results
The 150 patients included had a mean age of 50 years (range 18–94), and 97 (65 %) were male. The head injury was minimal in 12/150 (8 %) patients, minor in 119/150 (79 %) and moderate in 19/150 (13 %). A CT scan was performed in 120/150 (80 %) patients, 93/150 (62 %) were admitted for observation, and analysis of S100B was performed in 50/150 (33 %).
Management was in accordance with the Scandinavian guidelines for 96/150 (64 %) patients. This proportion increased with the severity of the injury (minimal 4/12 (33 %), minor 76/119 (64 %) and moderate 16/19 (84 %)). The reasons for non-compliance with the guidelines are shown in Table 1.
Table 1
Over- and undertesting in 54/150 (36 %) patients who were not treated in accordance with the Scandinavian guidelines for acute management of adult patients with minimal, mild or moderate head injuries (1). Overtesting = unnecessary CT scan and/or hospital admission. Undertesting = omission of necessary CT scan and/or hospital admission. CT = computed tomography.
| Diagnostics | N (%) | |
|---|---|---|
| Overtesting | ||
| CT scan | 24 (44) | |
| Admission | 9 (17) | |
| CT scan and admission | 6 (11) | |
| Undertesting | ||
| CT scan | 4 (7) | |
| Admission | 9 (17) | |
| CT scan and admission | 2 (4) | |
| Total | 54 (100) | |
Among patients with low-risk mild head injuries, 35/57 (61 %) underwent analysis of S100B as per the recommendations. Serum S100B levels were ≥ 0.10 μg/L in 20/35 (57 %) patients, and 17 of these 20 (85 %) underwent a CT scan. Among 15/35 (43 %) patients with S100B < 0.10 μg/L, one patient underwent a CT scan. S100B analysis was performed without a specific recommendation in 15/150 (10 %) patients, of whom 6/15 (40 %) had minimal injuries, 7/15 (47 %) had minor injuries with medium or high risk, and 2/15 (13 %) had moderate injuries.
Discussion
The results of this study show that management of minimal, mild and moderate head injuries was in accordance with the guidelines for about two-thirds of patients. Overtesting in the form of a (non-recommended) CT scan occurred for 30 of 150 (20 %) patients, and was the most common form of non-compliance. Such scans pose a small but non-negligible risk in association with exposure to ionising radiation. At the same time, recommended CT scans and/or admission for observation did not occur for 15 of 150 (10 %) patients. This in turn entails a small risk that a serious intracranial injury will be missed.
S100B analysis was performed as recommended in almost two-thirds of patients when the head injury was categorised as mild and low risk. The results were negative in 15 of 35 (43 %) patients, sparing these individuals a CT scan that would otherwise have been performed. Increased use of S100B analysis could contribute to a further reduction in CT scans.
Our study was conducted in routine hospital clinical practice several years after the Scandinavian guidelines were implemented. It is likely to be representative of routine practice both at the University Hospital of North Norway, Tromsø and at other Norwegian hospitals. One weakness of the study is that we excluded 298 patients without documenting the distribution of reasons for exclusion. This means there is a small risk of selection bias. We identified patients using a broad search that included all diagnosis codes for head injuries. The most common reasons for exclusion were age below 18 years, more than 24 hours between injury and assessment, and multiple trauma.
Heskestad et al. examined patients treated at Stavanger University Hospital in 2003–04 and 2005–09 and found that 259/508 (51 %) and 738/1180 (63 %) patients, respectively, were treated in accordance with the guidelines (5, 6). This is consistent with our findings. Systematic reviews show the reasons for non-compliance to be numerous and highly variable (7). Personal factors related to doctors' knowledge and attitudes, the characteristics of the guidelines (accessibility and practicality), as well as external factors such as collaboration within the hospital and access to resources, all affect compliance (8).
Interventions to improve compliance will probably need to build on the findings of qualitative studies into the reasons for non-compliance at individual hospitals. Adoption and promotion of the guidelines by management, training new employees, incorporating checklists into the workflow in the electronic patient records, and adapting protocols so that they are in accordance with the recommendations in the guidelines, are likely to be crucial (8).
This article has been peer-reviewed.
- 1.
Sundstrøm T, Wester K, Enger M et al. Skandinaviske retningslinjer for akutt håndtering av voksne pasienter med minimal, lett eller moderat hodeskade. Tidsskr Nor Legeforen 2013; 133: E1–6. [PubMed][CrossRef]
- 2.
Di BS, Wei M, Ma WJ et al. A critical review to traumatic brain injury clinical practice guidelines. Medicine (Baltimore) 2019; 98: e14592. [PubMed][CrossRef]
- 3.
Svensson S, Vedin T, Clausen L et al. Application of NICE or SNC guidelines may reduce the need for computerized tomographies in patients with mild traumatic brain injury: a retrospective chart review and theoretical application of five guidelines. Scand J Trauma Resusc Emerg Med 2019; 27: 99. [PubMed][CrossRef]
- 4.
Davis F, Il'yasova D, Rankin K et al. Medical diagnostic radiation exposures and risk of gliomas. Radiat Res 2011; 175: 790–6. [PubMed][CrossRef]
- 5.
Heskestad B, Baardsen R, Helseth E et al. Guideline compliance in management of minimal, mild, and moderate head injury: high frequency of noncompliance among individual physicians despite strong guideline support from clinical leaders. J Trauma 2008; 65: 1309–13. [PubMed][CrossRef]
- 6.
Heskestad B, Waterloo K, Ingebrigtsen T et al. An observational study of compliance with the Scandinavian guidelines for management of minimal, mild and moderate head injury. Scand J Trauma Resusc Emerg Med 2012; 20: 32. [PubMed][CrossRef]
- 7.
Arts DL, Voncken AG, Medlock S et al. Reasons for intentional guideline non-adherence: A systematic review. Int J Med Inform 2016; 89: 55–62. [PubMed][CrossRef]
- 8.
Fischer F, Lange K, Klose K et al. Barriers and strategies in guideline implementation – a scoping review. Healthcare (Basel) 2016; 4: 36. [PubMed][CrossRef]