Main findings
In 2020, the incidence of confirmed SARS-CoV-2 among health service staff in Norway was 1.48 %, varying from 0.80 % (psychologists) to 1.83 % (ambulance personnel).
The incidence among staff in nursing homes and acute hospitals was higher than in other parts of the health service. Testing activity varied between the occupational groups; with the highest proportion of positive tests among nursing associates, healthcare assistants, ambulance personnel, and cleaners.
The proportion of imported infections was highest for dentists, psychologists, and doctors.
The SARS-CoV-2 virus and COVID-19 disease have put a great strain on health services around the world. The first confirmed case of SARS-CoV-2 in Norway was reported on 26 February 2020, and by the end of week 53, a total of 51 322 cases had been reported (1). In the working-age population (20–69 years), the incidence was 1.11 % (38 454/3 452 287) in 2020 (2).
Employees in the health and care service (herein referred to as the health service) are vital to the care of all patients and service users during the pandemic, both those with and without COVID-19. Infection among employees can have major consequences both for their own health and for the provision of necessary health services. When staff are self-isolating or in quarantine, the capacity in the health service is compromised, individual workloads increase and the risk of outbreaks grows. The disease can be transmitted through occupational exposure, but non-work-related factors can also play a role, such as transmission by close contacts in social settings or on foreign holidays. Socio-economic aspects can also be a contributory factor.
In a non-peer-reviewed study using data from the emergency preparedness register, Beredt C19, Magnusson et al. found that in the early stages of the pandemic in Norway, a higher proportion of doctors, nurses, dentists and physiotherapists were diagnosed with SARS-CoV-2 compared to other occupational groups, but in the second period (July–December), the risk was not higher in these occupational groups than for the general population (3). A study conducted in Bergen found a low incidence rate among healthcare personnel, which coincided with a low prevalence in the local community (4). However, the study also implied a possible increased incidence among healthcare personnel with direct contact with COVID-19 patients. The data in the study are limited and must be interpreted with caution. Basso et al. studied the healthcare personnel caring for one symptomatic COVID-19 patient and found that no one became infected when following the recommended infection control measures (5).
International studies have described how the risk of health service staff being infected with SARS-CoV-2 varies across the different settings (6). While some studies have found an increased risk (7–11), other studies have not found any evidence of this, even where there is close patient contact (12–17). International studies are not directly transferrable to the situation in Norway due to Norway's relatively low infection rate, low hospital admission rates, health service structure, infection control measures, and access to personal protective equipment (PPE) (1).
The purpose of this register study is to describe confirmed cases of SARS-CoV-2 among various occupational groups in the health service and across different parts of the health service in Norway in 2020. This knowledge can be used when assessing the risk of transmission to and within the health service. In this study, we have not been able to determine whether health service employees tend to be infected in the workplace or elsewhere.
Material and method
We used data from Beredt C19, in which several different data sources are collated into one accessible database. We used four of the data sources – the National Population Register, the Aa Register (register of employers and employees), MSIS (Norwegian Surveillance System for Communicable Diseases) and the National Microbiology Laboratory Database. With the exception of freelancers and the self-employed (e.g. some general practitioners, dentists, physiotherapists and chiropractors), all employment is reported in the Aa Register. Under the MSIS regulations, MSIS must be notified of confirmed cases of SARS-CoV-2. The National Microbiology Laboratory Database is a new database where, inter alia, all SARS-CoV-2 test results, including negative ones, are reported.
Using Beredt C19, we identified 750 892 employees that were registered with an industrial classification (Standard Industrial Classification, SIC2007) that we defined as part of the health service (Figure 1, Appendix 1). From these, we selected employees (n = 653 975) that were registered with certain STYRK-98 codes (Norwegian Standard Classification of Occupations), either because we assumed that they were healthcare personnel, or had a background in healthcare, or had contact with patients in the health service. The quality of detailed data in STYRK-98 is poor, and we therefore converted our selection to ISCO-08 codes using the conversion table in Appendix 2. The employees we excluded (n = 96 917) mainly consisted of administrative staff, managers, kitchen staff and other support staff.
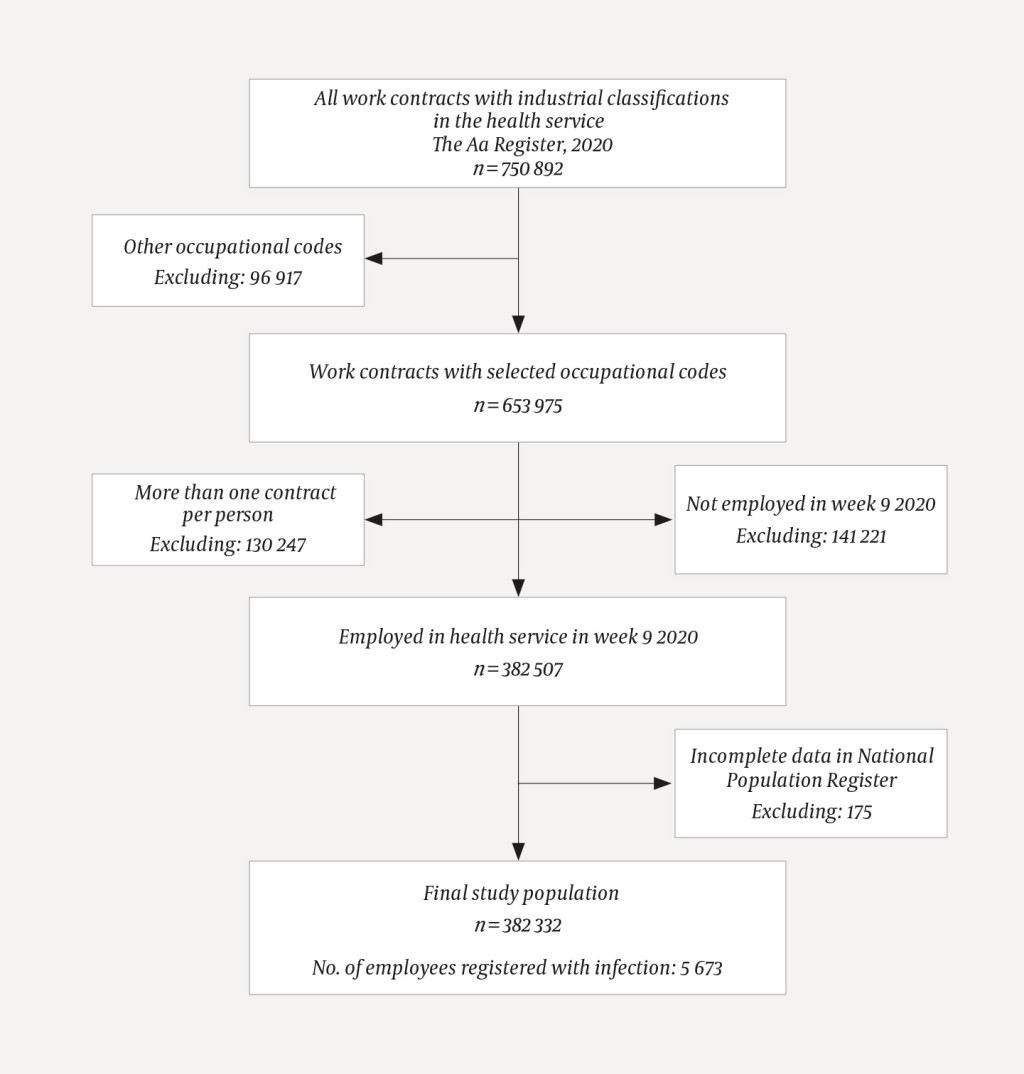
All employment contracts that were active in week 9 in 2020 are included, and each employee is included only once. Where an employee was registered with more than one occupation, we selected the occupation with the highest qualification requirement, as we assumed that someone who is registered as both a healthcare assistant and a doctor, for example, is likely to be working as a doctor. Where an employee held more than one position in the same occupation, we selected one at random. After removing employees that we were unable to find using a personal identification number or D-number (a unique identification number provided to certain groups of non-residents in Norway) in the National Population Register (n = 175), the final study population totalled 382 332.
We looked at all polymerase chain reaction tests (PCR tests) in the National Microbiology Laboratory Database and confirmed infections in MSIS in 2020. Each person may have been tested several times. Individual data on testing activity before 1 April 2020 are incomplete in the laboratory database.
We divided the study population into age categories (≤ 29 years, 30–39 years, 40–49 years, 50–59 years and ≥ 60 years), sex (male or female), country of birth (Norway, high-income and low- and middle-income countries (World Bank definitions)), place of residence (municipality with more than or fewer than 100 000 inhabitants), and type of health service (acute hospital, specialist health service, primary health service excluding nursing homes, home care services, nursing homes and other health services). Dental services were included in the primary health service.
For each of the categories above, we described the incidence (cumulative incidence as a proportion) in two different periods (March–July and August–December). In addition, we described the number of tests per person, the proportion of positive tests and the incidence both including and excluding employees who were registered with an imported infection, as these were unlikely to have been infected at work. We also drew up a timeline for the incidence rate (new cases per week per 100 000 people), the proportion tested per week and the proportion whose test was positive. The proportion whose test was positive was calculated by dividing the number of positive tests by the total number of employees tested in the given period. Stata/SE 16.0 (College Station, Texas, USA) was used for all data management and analysis.
Ethical considerations
Beredt C19 was established under Section 2–4 of the Health Preparedness Act. The Norwegian Institute of Public Health has conducted a data protection impact assessment of the register. This study has been assessed and approved by the Regional Committee for Medical and Health Research Ethics (case no. 2020/187735).
Results
The incidence among health service staff for the entire period was 1.48 % (5673/382 332) (Table 1). The incidence was highest in the second period, at 1.00 % (3813/382 332), and lowest in the first period, at 0.49 % (1860/382 332). With an incidence of 1.83 % (95/5203), ambulance personnel were the occupational group with the highest incidence, while psychologists had the lowest: 0.80 % (39/4900). Among doctors and nurses, the incidence was 1.56 % (379/24 290) and 1.66 % (999/60 337), respectively.
Table 1
Number of persons and incidence of confirmed cases of SARS-CoV-2 in two periods in 2020 among employees in selected occupational groups in the health service in Norway 2020, employed in week 9
| n | Year as a whole | March– July | August– December | ||
|---|---|---|---|---|---|
| Total | 382 332 | 1.48 | 0.49 | 1.00 | |
| Occupational groups | |||||
| Ambulance personnel | 5 203 | 1.83 | 0.56 | 1.27 | |
| Cleaners | 7 647 | 1.74 | 0.69 | 1.05 | |
| Registered nurses | 60 337 | 1.66 | 0.69 | 0.97 | |
| Nursing associates | 99 222 | 1.58 | 0.49 | 1.08 | |
| Doctors | 24 290 | 1.56 | 0.64 | 0.92 | |
| Radiographers etc. | 2 971 | 1.51 | 0.74 | 0.77 | |
| Healthcare assistants | 101 703 | 1.50 | 0.35 | 1.15 | |
| Bioengineers | 5 258 | 1.39 | 0.38 | 1.01 | |
| Social educators | 15 993 | 1.29 | 0.41 | 0.88 | |
| Midwives | 2 827 | 1.20 | 0.53 | 0.67 | |
| Dentists | 2 941 | 1.19 | 0.61 | 0.58 | |
| Specialist nurses | 30 146 | 1.08 | 0.45 | 0.63 | |
| Occupational therapists | 2 580 | 1.01 | 0.39 | 0.62 | |
| Physiotherapists | 5 709 | 0.95 | 0.37 | 0.58 | |
| Psychologists | 4 900 | 0.80 | 0.35 | 0.45 | |
| Other health workers | 10 605 | 1.30 | 0.36 | 0.94 | |
| Age | |||||
| ≤ 29 years | 94 655 | 1.97 | 0.56 | 1.41 | |
| 30–39 years | 84 493 | 1.58 | 0.53 | 1.05 | |
| 40–49 years | 76 293 | 1.46 | 0.47 | 0.99 | |
| 50–59 years | 73 338 | 1.27 | 0.47 | 0.80 | |
| ≥ 60 years | 53 553 | 0.81 | 0.35 | 0.46 | |
| Sex | |||||
| Female | 310 946 | 1.38 | 0.45 | 0.93 | |
| Male | 71 386 | 1.96 | 0.65 | 1.30 | |
| Country of birth | |||||
| Norway | 295 152 | 1.20 | 0.40 | 0.80 | |
| High-income country | 26 213 | 1.49 | 0.51 | 0.98 | |
| Low- and middle-income countries | 43 095 | 3.72 | 1.16 | 2.56 | |
| Data incomplete | 17 872 | ||||
| Place of residence | |||||
| < 100 000 inhabitants1 | 273 702 | 1.03 | 0.30 | 0.73 | |
| > 100 000 inhabitants | 108 630 | 2.62 | 0.96 | 1.66 | |
| Health service | |||||
| Nursing home | 82 776 | 1.86 | 0.63 | 1.22 | |
| Acute hospital | 72 913 | 1.67 | 0.70 | 0.97 | |
| Home care service | 62 673 | 1.33 | 0.33 | 1.00 | |
| Primary health service (excl. nursing homes) | 24 279 | 1.24 | 0.42 | 0.83 | |
| Other specialist health service | 34 634 | 1.16 | 0.44 | 0.72 | |
| Other health service | 105 057 | 1.32 | 0.35 | 0.97 | |
1Includes 6168 records without a known place of residence
The incidences were highest for the youngest group (1.97 %, 1860/94 655), men (1.96 %, 1396/71 386), persons born in low- and middle-income countries (3.72 %, 1605/43 095) and residents of large municipalities (2.62 %, 2845/108 630) (Table 1). Among the different services, we found the highest incidences among employees in acute hospitals (1.67 %, 1218/72 913) and in nursing homes (1.86 %, 1536/82 776). Appendix 3 provides more comprehensive data distributed by occupational group.
Doctors were tested most frequently, with 1.45 tests per person for the entire period (Table 2). Cleaners had the lowest testing rate (0.59 tests per person), and also the highest proportion of positive tests (2.78 %). When we excluded employees who were registered with an imported infection, the incidence for the period as a whole decreased from 1.56 % to 1.39 % for doctors, and from 1.19 % to 1.02 % for dentists (Table 2). The highest proportions of imported infection were found among dentists (14.3 %), psychologists (12.8 %) and doctors (10.8 %).
Table 2
Testing activity, proportion of positive tests, incidence and incidence excluding imported cases of SARS-CoV-2 among employees in selected occupational groups in the health service in Norway 2020, employed in week 9
| Occupational group | No. of tests per person | Proportion of positive tests | Incidence | Incidence excluding imported cases | Proportion of cases imported |
|---|---|---|---|---|---|
| Cleaners | 0.59 | 2.78 | 1.74 | 1.66 | 4.5 |
| Ambulance personnel | 0.99 | 1.57 | 1.83 | 1.71 | 6.3 |
| Healthcare assistants | 0.94 | 1.52 | 1.50 | 1.43 | 4.9 |
| Nursing associates | 1.01 | 1.48 | 1.58 | 1.50 | 4.7 |
| Radiographers etc. | 1.15 | 1.23 | 1.51 | 1.48 | 2.2 |
| Dentists | 0.86 | 1.19 | 1.19 | 1.02 | 14.3 |
| Other health workers | 1.06 | 1.16 | 1.30 | 1.25 | 3.6 |
| Registered nurses | 1.34 | 1.15 | 1.66 | 1.55 | 6.2 |
| Social educators | 1.07 | 1.14 | 1.29 | 1.23 | 5.3 |
| Bioengineers | 1.17 | 1.10 | 1.39 | 1.37 | 1.4 |
| Doctors | 1.45 | 0.94 | 1.56 | 1.39 | 10.8 |
| Occupational therapists | 1.23 | 0.82 | 1.01 | 1.01 | 0.00 |
| Midwives | 1.31 | 0.81 | 1.20 | 1.10 | 8.8 |
| Specialist nurses | 1.21 | 0.78 | 1.08 | 1.00 | 8.0 |
| Physiotherapists | 1.22 | 0.67 | 0.95 | 0.89 | 5.6 |
| Psychologists | 1.38 | 0.47 | 0.80 | 0.69 | 12.8 |
We observed an infection peak in our study population in week 14 (incidence rate of 84.7 per 100 000) and in week 46 (105.4 per 100 000), and the rate was rising as we entered 2021 (Figure 2). In the first period, most staff testing was carried out in week 12 (3.3 %, 12 617/382 332), and in the last period, most tests were performed in week 51 (5.7 %, 21 793/382 332). The proportion of positive tests was highest in week 15, at 5.2 % (209/4022) (Figure 3).
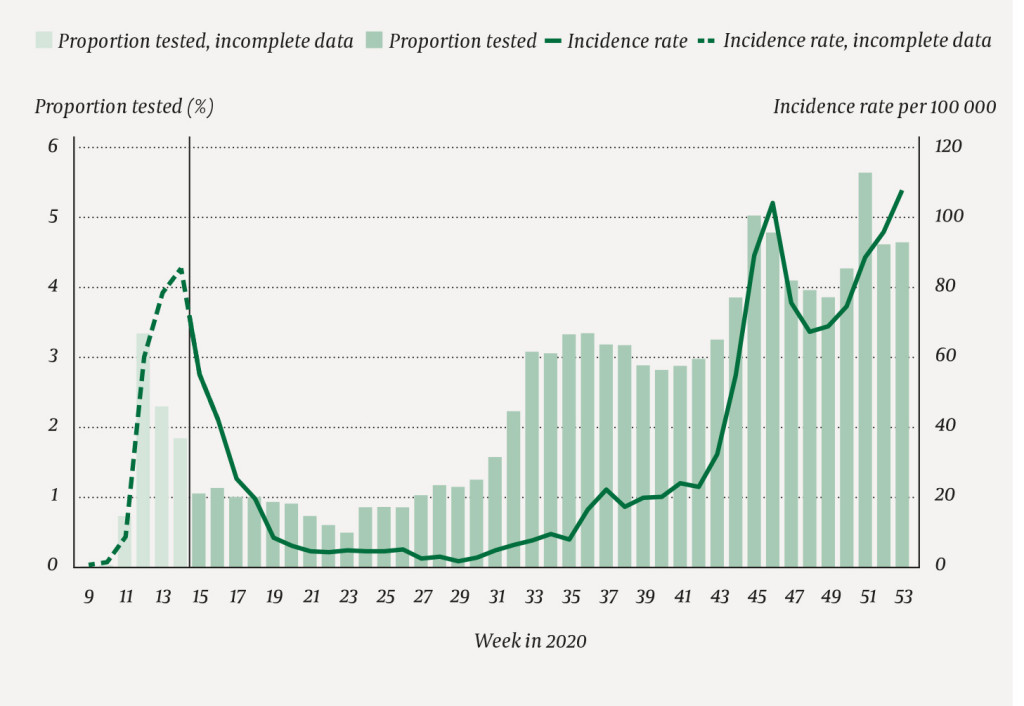
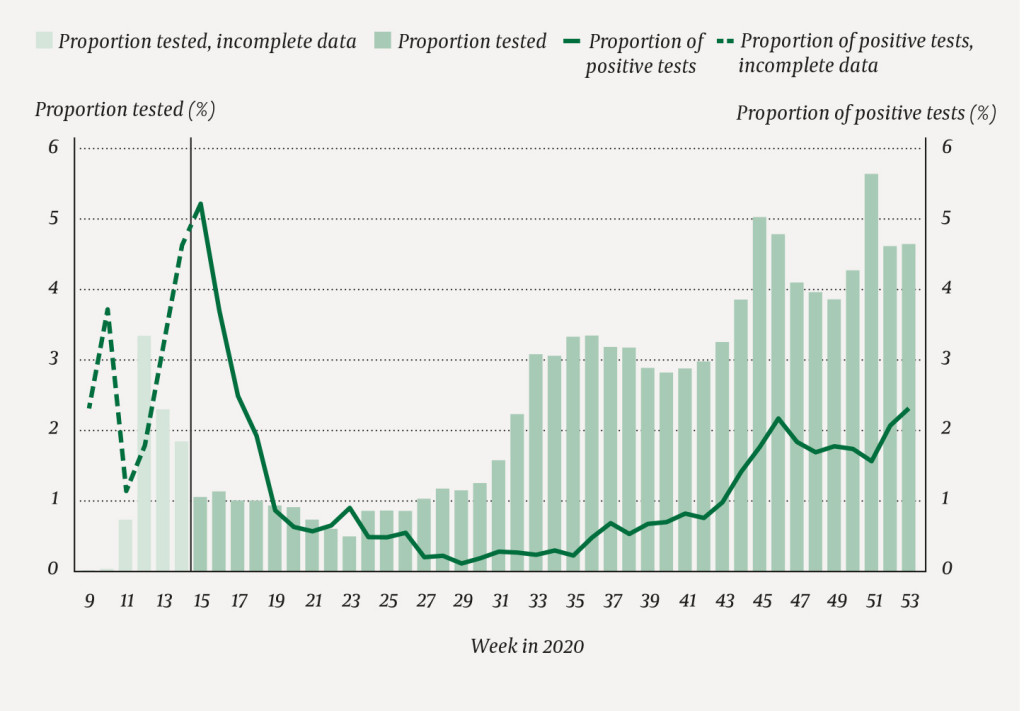
Discussion
In this register study, we found an incidence rate of 1.48 % for confirmed SARS-CoV-2 among health service staff in Norway in 2020. The incidence varied between sex, age, country of birth and place of residence, but also between different occupational groups and within different parts of the health service. As with the general population, the number of positive cases among health service staff rose in the post-summer period, but a peak was also seen for this group in the early stages of the pandemic.
Health service employees are a heterogeneous group with differing characteristics that can impact on their level of non-work-related risk of being diagnosed with SARS-CoV-2. This can include infection transmission from close contacts outside work, which has also been shown to be a key factor in the incidence among healthcare personnel (8). The majority of positive cases in Norway relate to people who were infected by household members, and only about one-sixth are transmitted at work or university (1). Structural and social inequalities have been shown to be associated with increased transmission rates and severity of disease (18–20). The transmission rate and hospital admission rates are higher among people born outside Norway (8, 21). In the early stages of the pandemic, the higher proportions of infections that were imported among dentists, psychologists and doctors may indicate that transmission has a positive correlation with socio-economic status and mobility. The high incidence among the youngest age group and people born in low- and middle-income countries suggests that transmission is more likely to take place outside the workplace and should be compared with similar patterns in the rest of the population (1).
Possible work-related risks of infection may be associated with particular types of work, such as patient-centred tasks that entail exposure to SARS-CoV-2, either from COVID-19 patients or patients with an unknown infection status, or with other variations in working practices in the different parts of the health service. Differences in physical working conditions and opportunities for social distancing can impact on the work-related risk, since it is known that those who are pre- and asymptomatic are contagious. Evidence has been found of nosocomial transmission to and between employees during SARS-CoV-2 outbreaks in Norway (22–24). Access to PPE and training in correct use can also impact on the risk level. Lack of PPE is associated with an increased risk of COVID-19 in healthcare personnel (7). In Norway, shortfalls in local supplies of PPE were reported at the start of the pandemic (25), but the national supply gradually reached an adequate level (26). Any potential work-related risk is impacted by the community transmission risk.
Magnusson et al. found that the proportion of doctors, nurses, dentists and physiotherapists with confirmed SARS-CoV-2 was higher than in other occupational groups in the early stages of the pandemic, but no such disparity was found for the second period (July–December) (3). During the first six weeks, approximately 2 % of the population in Norway was tested for SARS-CoV-2 (approximately 120 000 tests), and 5 % of these tests were positive (27). Health service staff accounted for about a quarter of all tests during this period (about 30 000), and about 3 % of these were positive (Figure 3). In order not to exceed the test capacity, health service staff who have close contact with patients were prioritised for testing early in the pandemic (28). This prioritisation may have contributed to more confirmed infections for this group.
Our data show that doctors were tested more frequently than the other occupational groups. Ambulance personnel, nursing associates, healthcare assistants and cleaners are groups that were tested less. However, these groups have a relatively high proportion of positive tests, which may imply higher undiagnosed infection among these groups. We know that staff can transmit the infection to patients and residents. Escalating the testing activity for these large occupational groups could potentially prevent infection transmission in the health service. The high incidence among ambulance personnel is concerning, as it appears to be high irrespective of various other characteristics. However, it may also be coincidental, as the study population for this group is small.
We found a higher incidence of confirmed infections among staff in acute hospitals and nursing homes than other parts of the health service. Infection rates among acute hospital staff may be related to the fact that the majority of such hospitals are located in cities with widespread community transmission. In nursing homes, the incidence should be considered in conjunction with the numerous major outbreaks of nosocomial transmission to and between staff (23, 24), but also with the composition of occupational groups, age distribution and socio-economic factors. We find higher confirmed infection among cleaners and staff born in low- and middle-income countries. It has also been previously reported that cleaners are an overrepresented group (8).
In this large register study, we have shown the prevalence of confirmed SARS-CoV-2 among health service staff in Norway at an overarching level. The number of confirmed cases has been relatively low in Norway, which in turn means incidences are low in many occupational groups and must therefore be interpreted with caution. We have not performed analyses that compare groups, and the data material in Beredt C19 is not suited to further breakdowns by occupational groups or industrial classifications for examining different specialties or departments that could be assumed to be particularly at risk of infection. This study can thus not provide an answer to whether occupational practice is associated with an increased risk of SARS-CoV-2 infection.
A weakness of our study is that data for testing activity before 1 April are incomplete and of a relatively low quality, which means that we have underestimated the incidence and testing rates in the first four weeks. The data sources in the study also have some weaknesses. For example, the Aa Register does not include self-employed persons. If these had been included, it may have changed the number of confirmed infections among staff in parts of the primary health service, but we do not know in which direction. We included health service employees even where this was not their main job, which may have been outside the health service. This means that our population is somewhat larger than that used in other statistics. We did not have data on income, and some of the employees may have been inactive.
This study has shown that the incidence of confirmed infections differs among health service staff. It is important to shed light on this in order to be able to evaluate infection control measures and target efforts to prevent transmission in the health service. However, more research is needed to establish whether, and to what extent, infection among staff is linked to exposure from occupational practice in the health service in Norway.
Thank you to all the clinicians and laboratory personnel who have reported and continue to report infection cases and testing figures during this pandemic. This study would not have been possible without their help. We would also like to thank Anja Schou Lindmann, project manager for Beredt C19, and Gutorm Høgåsen, who was responsible for developing the register. Thanks also go to those responsible for MSIS for their tireless work throughout the pandemic. Special thanks are extended to Kirsten Gravningen for her valuable input.
- 1.
Folkehelseinstituttet. COVID-19 Ukerapport – uke 53. https://www.fhi.no/contentassets/8a971e7b0a3c4a06bdbf381ab52e6157/vedlegg/andre-halvar--2020/2021.01.06-ukerapport-uke-53-covid-19.pdf Accessed 12.1.2021.
- 2.
Folkehelseinstituttet. Statistikk om koronavirus og covid-19. https://www.fhi.no/sv/smittsomme-sykdommer/corona/dags--og-ukerapporter/dags--og-ukerapporter-om-koronavirus/ Accessed 12.1.2021
- 3.
Magnusson K, Nygard KM, Vold L et al. Occupational risk of COVID-19 in the 1st vs 2nd wave of infection medRxiv 2020 doi: 10.1101/2020.10.29.20220426. [CrossRef]
- 4.
Trieu MC, Bansal A, Madsen A et al. SARS-CoV-2-specific neutralizing antibody responses in Norwegian healthcare workers after the first wave of COVID-19 pandemic: a prospective cohort study. J Infect Dis 2020; 223: jiaa737. [PubMed][CrossRef]
- 5.
Basso T, Nordbø SA, Sundqvist E et al. Transmission of infection from non-isolated patients with COVID-19 to healthcare workers. J Hosp Infect 2020; 106: 639–42. [PubMed][CrossRef]
- 6.
Chou R, Dana T, Buckley DI et al. Update alert 5: epidemiology of and risk factors for coronavirus infection in health care workers. Ann Intern Med 2020; 173: W154–5. [PubMed][CrossRef]
- 7.
Nguyen LH, Drew DA, Graham MS et al. Risk of COVID-19 among front-line health-care workers and the general community: a prospective cohort study. Lancet Public Health 2020; 5: e475–83. [PubMed][CrossRef]
- 8.
Eyre DW, Lumley SF, O'Donnell D et al. Differential occupational risks to healthcare workers from SARS-CoV-2 observed during a prospective observational study. eLife 2020; 9: 60675. [PubMed][CrossRef]
- 9.
Porru S, Carta A, Monaco MGL et al. Health surveillance and response to SARS-CoV-2 mass testing in health workers of a large Italian hospital in Verona, Veneto. Int J Environ Res Public Health 2020; 17: 15. [PubMed][CrossRef]
- 10.
Shah ASV, Wood R, Gribben C et al. Risk of hospital admission with coronavirus disease 2019 in healthcare workers and their households: nationwide linkage cohort study. BMJ 2020; 371: m3582. [PubMed][CrossRef]
- 11.
Iversen K, Bundgaard H, Hasselbalch RB et al. Risk of COVID-19 in health-care workers in Denmark: an observational cohort study. Lancet Infect Dis 2020; 20: 1401–8. [PubMed][CrossRef]
- 12.
Hunter E, Price DA, Murphy E et al. First experience of COVID-19 screening of health-care workers in England. Lancet 2020; 395: e77–8. [PubMed][CrossRef]
- 13.
Folgueira MD, Munoz-Ruiperez C, Alonso-Lopez MA et al. SARS-CoV-2 infection in Health Care Workers in a large public hospital in Madrid, Spain, druing March 2020. medRxiv 2020 doi: 10.1101/2020.04.07.20055723. [CrossRef]
- 14.
Steensels D, Oris E, Coninx L et al. Hospital-wide SARS-CoV-2 antibody screening in 3056 staff in a tertiary center in Belgium. JAMA 2020; 324: 195–7. [PubMed][CrossRef]
- 15.
Korth J, Wilde B, Dolff S et al. SARS-CoV-2-specific antibody detection in healthcare workers in Germany with direct contact to COVID-19 patients. J Clin Virol 2020; 128: 104437. [PubMed][CrossRef]
- 16.
Jeremias A, Nguyen J, Levine J et al. Prevalence of SARS-CoV-2 Infection Among Health Care Workers in a Tertiary Community Hospital. JAMA Intern Med 2020; 180: 1707–9. [PubMed][CrossRef]
- 17.
Sahu AK, Amrithanand VT, Mathew R et al. COVID-19 in health care workers - A systematic review and meta-analysis. Am J Emerg Med 2020; 38: 1727–31. [PubMed][CrossRef]
- 18.
Bhala N, Curry G, Martineau AR et al. Sharpening the global focus on ethnicity and race in the time of COVID-19. Lancet 2020; 395: 1673–6. [PubMed][CrossRef]
- 19.
Drefahl S, Wallace M, Mussino E et al. Socio-demographic risk factors of COVID-19 deaths in Sweden: A nationwide register study. Stockholm Research Reports in Demography 2020:23. https://su.figshare.com/articles/preprint/Socio-demographic_risk_factors_of_COVID-19_deaths_in_Sweden_A_nationwide_register_study/12420347 Accessed 21.12.2020.
- 20.
Lauvrak V, Juvet L. Social and economic vulnerable groups during the COVID-19 pandemic. Rapid review. Oslo: Folkehelseinstittutet, 2020. https://www.fhi.no/globalassets/dokumenterfiler/rapporter/2020/social-and-economic-vulnerable-groups-during-the-covid-19-pandemic-report-2020-v3.pdf Accessed 21.12.2020.
- 21.
Indseth T, Godøy A, Kjøllesdal M et al. Covid-19 etter fødeland: Personer testet, bekreftet smittet og relaterte innleggelser og dødsfall. Rapport 2020. Oslo: Folkehelseinstituttet, 2020. https://www.fhi.no/globalassets/dokumenterfiler/rapporter/2020/covid-19-etter-fodeland-personer-testet-bekreftet-smittet-og-relaterte-innleggelser-og-dodsfall-rapport-2020-v2.pdf Accessed 21.12.2020.
- 22.
Folkehelseinstituttet. Covid-19, Hammerfest sykehus – statusrapport 03.11.2020. https://finnmarkssykehuset.no/Documents/Beredskap/Hammerfest%20utbruddsrapport%20-%20FHI.pdf Accessed 21.12.2020.
- 23.
Kittang BR, Hofacker SV, Solheim SP et al. Outbreak of COVID-19 at three nursing homes in Bergen. Tidsskr Nor Legeforen 2020; 140. doi: 10.4045/tidsskr.20.0405. [PubMed][CrossRef]
- 24.
Folkehelseinstituttet. Covid-19, Sykehjem i Eidsvoll kommune – statusrapport 27.11.2020. https://www.eidsvoll.kommune.no/siteassets/20-pdf-dokumenter/beredskap/eidsvoll-kommune-fhi-rapport._.pdf Accessed 15.1.2021.
- 25.
KS. NSF og Fagforbundet ber om strakstiltak for å øke tilgangen til nødvendig smittevernsutstyr i kommunene. https://www.ks.no/informasjon-om-koronaviruset/helse-og-omsorg/ks-nsf-og-fagforbundet-ber-om-strakstiltak-for-a-oke-tilgangen-til-nodvendig-smittevernsutstyr-i-kommunene/ Accessed 8.1.2021.
- 26.
Helsedirektoratet. Ingen mangel på smittevernutstyr. https://www.helsedirektoratet.no/nyheter/ingen-mangel-pa-smittevernutstyr Accessed 8.1.2021.
- 27.
Seppälä E, Tønnessen R, Veneti L et al. COVID-19 cases reported to the Norwegian Institute of Public Health in the first six weeks of the epidemic. Tidsskr Nor Legeforen 2020; 140. doi: 10.4045/tidsskr.20.0525. [PubMed][CrossRef]
- 28.
Folkehelseinstituttet. Testkriterier for koronavirus. https://www.fhi.no/nettpub/coronavirus/testing-og-oppfolging-av-smittede/testkriterier/?term=&h=1 Accessed 20.12.2020.