Main findings
Total sales of antibiotics increased in March 2020.
The prescribing of antibiotics to persons outside institutions was at a normal level in March 2020.
Since March 2020, the use of antibiotics outside institutions has been significantly lower than in the preceding years.
Compared to other countries, the consumption of antibiotics in Norway is low, and the proportion of narrow-spectrum antibiotics is high (1, 2). Dispensing on prescription outside institutions accounts for 80 % of total sales (1). Since 2012, the use declined year on year until 2018, followed by a small increase of 2 % in 2019. This decline is in line with the intentions in the National Plan Against Antibiotic Resistance of a 30 % reduction from 2012 to 2020 (3). In persons outside institutions, antibiotics are most frequently prescribed against respiratory infections. As a result, the use of antibiotics is at its highest during the winter months.
Since antibiotics have been suggested as a treatment for COVID-19, it is interesting to see how the COVID-19 pandemic has affected the use of antibiotics. In this article, we describe the consumption of antibiotics in Norway during the COVID-19 pandemic, compared to the preceding period.
Material and method
We retrieved data on sales of systemic antibiotics, defined as all drugs included in the Anatomic Therapeutic Chemical (ATC) classification group J01 (Antibacterials for systemic use) (4) in the two databases that provide information on the use of medicinal drugs in Norway. These are the Norwegian Prescription Database (NorPD), which includes all drugs prescribed and dispensed to patients outside institutions, and the wholesaler-based drug statistics, which encompass all sales of drugs in Norway, including sales to hospitals and nursing homes (5, 6). Methenamine was excluded, since this drug is used exclusively for prophylaxis.
Total sales in the wholesaler-based drug statistics are measured in defined daily doses (DDD). From the Prescription Database we retrieved information on patient age, defined daily doses and the number of prescriptions. Use is measured in DDD/1 000 inhabitants/day, percentage of users in the population (prevalence) and the number of prescriptions/1 000 inhabitants in the period studied. The monthly consumption in 2019 was compared to the use in the same month in 2020.
The Prescription Database provides no information on the diagnoses for which the prescriptions were issued. We have therefore grouped the antibiotics by their assumed area of use. Antibiotics for treatment of respiratory infections contain amoxicillin, phenoxymethylpenicillin, macrolides and doxycycline.
We have divided the population into the age groups 0–4 years, 5–12 years, 13–29 years, 30–64 years and > 65 years. The data were retrieved from the Norwegian Institute of Public Health's internal retrieval solution for health analysis, where individual data cannot be identified. This type of anonymous data retrieval does not require approval by the Regional Committee for Medical and Health Research Ethics (REK) or the data protection officer. Data from the wholesaler-based drug statistics was available for the period through December 2020 and from the Prescription Database through September 2020.
Results
Total sales of antibiotics
In March 2020, total sales increased by 15.9 % compared to February 2020 and by 20.3 % compared to March 2019 (Figure 1, Table 1). Most notably, the sales of azithromycin increased by 86 % (measured in DDD/1 000 inhabitants/day) from February to March 2020 and by 93 % from March 2019. In the following months sales fell when compared to 2019, most notably in May, by 27.2 % (Table 1). Total sales in 2020 amounted to 11.5 DDD/1 000 inhabitants/day (J01, exclusive of methenamine).
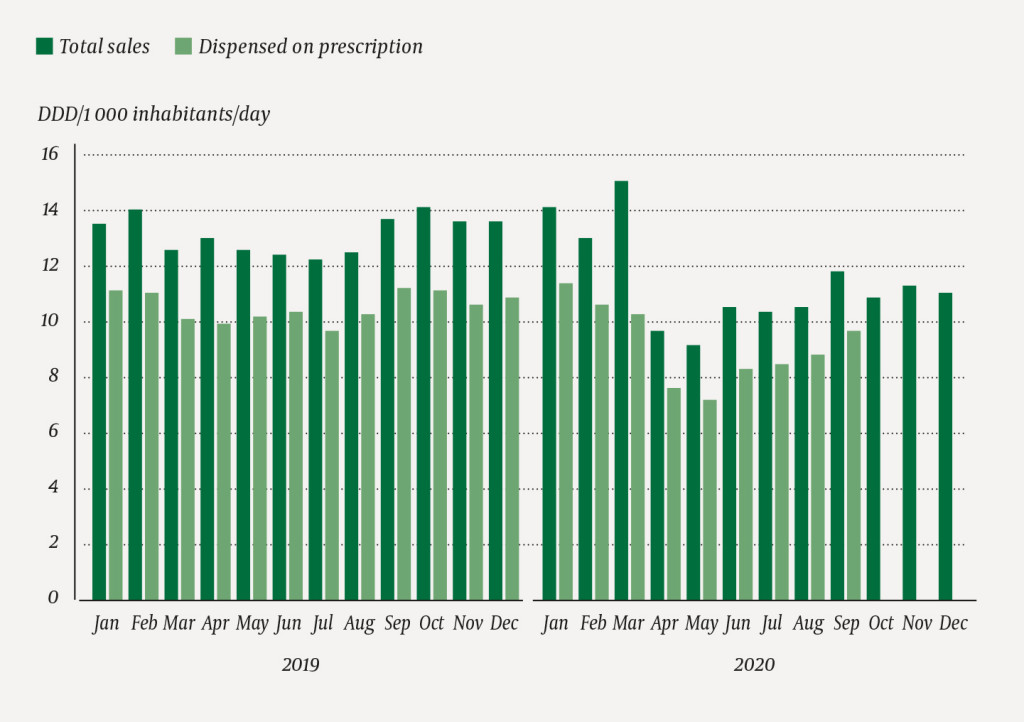
Table 1
Sales of antibiotics, J01, exclusive of methenamine, per month in 2020. Total sales are measured in DDD/1 000 inhabitants/day and change from 2019. Sales outside institutions are measured in DDD/1 000 inhabitants/day and change from 2019, in prevalence (proportion (%) of the population that took out prescriptions for antibiotics at least once during the month), in the number of prescriptions per 1 000 inhabitants and the proportion of all antibiotics prescriptions in the period.
| Total sales |
Sales outside institutions |
|||
|---|---|---|---|---|
| DDD/1000 inhabitants/day in 2020 (% change from 2019) |
DDD/1000 inhabitants/ day in 2020 (% change from 2019) |
Prevalence % 2020 (2019) |
Respiratory antibiotics 2020. |
|
| January |
14.2 (4.8) |
11.4 (2.7) |
2.6 (2.6) |
16.7 (54) |
| February |
13.1 (−7.3) |
10.6 (−4.1) |
2.3 (2.4) |
14.6 (54) |
| March |
15.1 (20.3) |
10.3 (2.5) |
2.3 (2.4) |
14.2 (52) |
| April |
9.7 (−25.8) |
7.6 (−23.2) |
1.7 (2.3) |
8 (41) |
| May |
9.2 (−27.2) |
7.2 (−28.7) |
1.6 (2.4) |
7.4 (39) |
| June |
10.6 (−14.8) |
8.3 (−19.8) |
1.8 (2.3) |
8.6 (40) |
| July |
10.4 (−15.1) |
8.5 (−12.5) |
1.9 (2.2) |
9.2 (41) |
| August |
10.6 (−15.6) |
8.8 (−14.4) |
1.9 (2.3) |
9.5 (41) |
| September |
11.9 (−13.7) |
9.7 (−13.1) |
2.1 (2.4) |
10.1 (42) |
| October |
10.9 (−23.0) |
|||
| November |
11.3 (−17.4) |
|||
| December |
11.1 (−18.7) |
|||
Prescriptions outside institutions
In March 2020, prescription sales accounted for only 68 % of the total wholesale volume (Figure 1), but were nevertheless at a normal level when compared to March of the preceding year. From March to April 2020, sales measured in prescriptions/1 000 inhabitants fell by 28 %. The prescription sales measured in DDD/1 000 inhabitants/day for the months April–September were lower than expected (Table 1).
In 2019, antibiotics against respiratory infections accounted for 47 % (August) to 55 % (January) of all prescriptions for antibiotics. During the pandemic, the proportion of antibiotics for treatment of respiratory infections declined (Table 1). In May, the number of prescriptions for treatment of respiratory infections per 1 000 inhabitants was nearly halved when compared to May 2019.
The greatest reduction in use occurred in children. In April 2019, the proportion of 0–4-year-olds who were prescribed antibiotics was nearly three times higher than in April 2020 (prevalence ratio (PR) 2.8, figures not stated in the table). The reduction in the prescribing of antibiotics for treatment of respiratory infections was even higher (PR 3.9). The number of prescriptions for antibiotics for treatment of respiratory infections in this age group fell by 73 % when compared to 2019. For children aged 5–12 years, the antibiotics prevalence was nearly twice as high in 2019 when compared to April 2020 (PR 1.8). The prevalence ratio for prescriptions for antibiotics to treat respiratory infections was 2.4, and the number of prescriptions was reduced by 55 %. Compared to 2019, in the period April–September there were 63 % fewer prescriptions for treatment of respiratory infections per 1 000 inhabitants among 0–4-year-olds, followed by the 5–12-year-olds (–44 %), the 13–29-year-olds (–36 %), the 30–64-year-olds (–32 %) and the over-65-year-olds (–32 %).
Discussion
The total sales of antibiotics increased greatly in March 2020, while the sales of antibiotics on prescription did not increase. This can be interpreted as reflecting high procurement by hospitals/institutions in the first weeks of the pandemic in an attempt to step up their preparedness in a situation of uncertainty. In the following months, the use of antibiotics fell steeply. Similar changes have been found also in Sweden and Denmark (7, 8). Internationally, an increased use of broad-spectrum antibiotics has been reported in hospitals during the pandemic (9), but we were unable to find any studies from the primary health service. At an early stage of the pandemic it was suggested to treat COVID-19 patients with azithromycin in combination with hydroxychloroquine. In Norway, such use was advised against. On 3 April, the Norwegian Directorate of Health recommended that the national guidelines be followed (10).
The significant reduction may have two main causes. First, it seems as though the powerful infection control measures have also reduced the number of infections that otherwise would have been treated with antibiotics. This is consistent with the observation that the number of hospitalisations for infections has also fallen during the pandemic (11). Second, the threshold to visit a prescribing doctor has been raised during the pandemic. In practice, many GPs' surgeries have been closed to patients with fever and/or symptoms of a respiratory infection, who instead have been referred to separate respiratory clinics or dealt with by way of e-consultations as needed. In April 2020, the number of consultations resulting in respiratory infection diagnoses (except COVID-19) in the primary health service was 34 % lower than in April 2019, and the figure has remained low (12). It appears as though patients have tended to wait out the infection at home – or alternatively had themselves tested for COVID-19 – instead of seeking out their GP. It is reasonable to imagine that whereas prior to the pandemic, people would have been more concerned whether a respiratory infection should be treated with antibiotics, during the pandemic this has been replaced by a need to check whether the infection is due to SARS-CoV-2.
In recent years, a number of measures have been taken to achieve more correct and less frequent use of antibiotics, both in the primary and the specialist health services. In 2019, it did not appear that we would achieve the target of a 30 % reduction from 2012 to 2020. With the COVID-19 pandemic, however, the target seems to have been achieved: from 2012 to 2020, the use has been reduced by 32 %. Strict infection control measures and a ban on visiting your GP for a respiratory infection cannot be justified by a possible reduction in the use of antibiotics. Nevertheless we can draw a lesson from this – an already limited use of antibiotics can be further reduced.
The article has been peer reviewed.
- 1.
NORM/NORM-vet. 2019. Usage of antimicrobial agents and occurrence of antimicrobial resistance in Norway. Tromsø/Oslo: Norsk overvåkingssystem for antibiotikaresistens hos mikrober/Veterinærinstituttet/Folkehelseinstituttet, 2019. https://www.vetinst.no/en/surveillance-programmes/norm-norm-vet-report/_/attachment/download/df4ceec7-f93c-435d-85ba-4376819bc1db:b912eb920994ba60f90889595a43d4e5e63c9ea1/NORM%20NORM-VET%202019.pdf Accessed 7.2.2021.
- 2.
WHO Report on Surveillance of Antibiotic Consumption 2016–2018. Early implementation. Geneve: World Health Organization, 2018. https://www.who.int/medicines/areas/rational_use/oms-amr-amc-report-2016-2018/en/ Accessed 7.2.2021.
- 3.
Regjeringen. Nasjonal Strategi mot Antibiotikaresistens 2015–2020. https://www.regjeringen.no/no/dokumenter/nasjonal-strategi-mot-antibiotikaresistens-2015-2020/id2424598/ Accessed 7.2.2021.
- 4.
ATC index with DDDs 2020. Oslo: WHO Collaborating Centre, 2019.
- 5.
Grossistbasert legemiddelstatistikk. Legemiddelforbruk i Norge 1988–2020. Oslo: Folkehelseinstituttet, 2020.
- 6.
Reseptregisteret 2004–20. http://www.reseptregisteret.no/ Accessed 7.2.2021.
- 7.
Folkehelsemyndighetene i Sverige. Kraftigt minskad försäljning av antibiotika under covid-19-pandemin. https://www.folkhalsomyndigheten.se/nyheter-och-press/nyhetsarkiv/2020/juni/kraftigt-minskad-forsaljning-av-antibiotika-under-covid-19-pandemin/ Accessed 3.11.2020.
- 8.
Sundhedsdatastyrelsen i Danmark. Småbørn har fået mindre antibiotika under nedlukningen. https://sundhedsdatastyrelsen.dk/da/nyheder/2020/antibiotika_under_covid19_060720 Accessed 3.11.2020.
- 9.
Dieringer TD, Furukawa D, Graber CJ et al. Inpatient antibiotic utilization in the Veterans' Health Administration during the coronavirus disease 2019 (COVID-19) pandemic. Infect Control Hosp Epidemiol 2020; 1–3. [PubMed][CrossRef]
- 10.
Helsedirektoratet. Antibiotika. https://www.helsedirektoratet.no/tema/antibiotika Accessed 30.11.2020.
- 11.
Interregionalt pandemiprosjekt. Sørge-for-ansvaret under koronapandemien. https://helse-nord.no/Documents/SKDE/SKDE%20Publikasjoner/S%c3%b8rge-for-ansvaret%20under%20koronapandemien%20%28SKDE%202020%29.pdf Accessed 7.2.2021.
- 12.
Helsedirektoratet. Statistikk fra Kommunalt pasient- og brukerregister (KPR). https://www.helsedirektoratet.no/statistikk/statistikk-fra-kommunalt-pasient-og-brukerregister-kpr Accessed 30.1.2020.