Main findings
All patients with severe injuries received opioids and paracetamol during their hospital stay.
Thirty-one of 40 patients were discharged with opioids to treat pain without any plan for tapering or cessation.
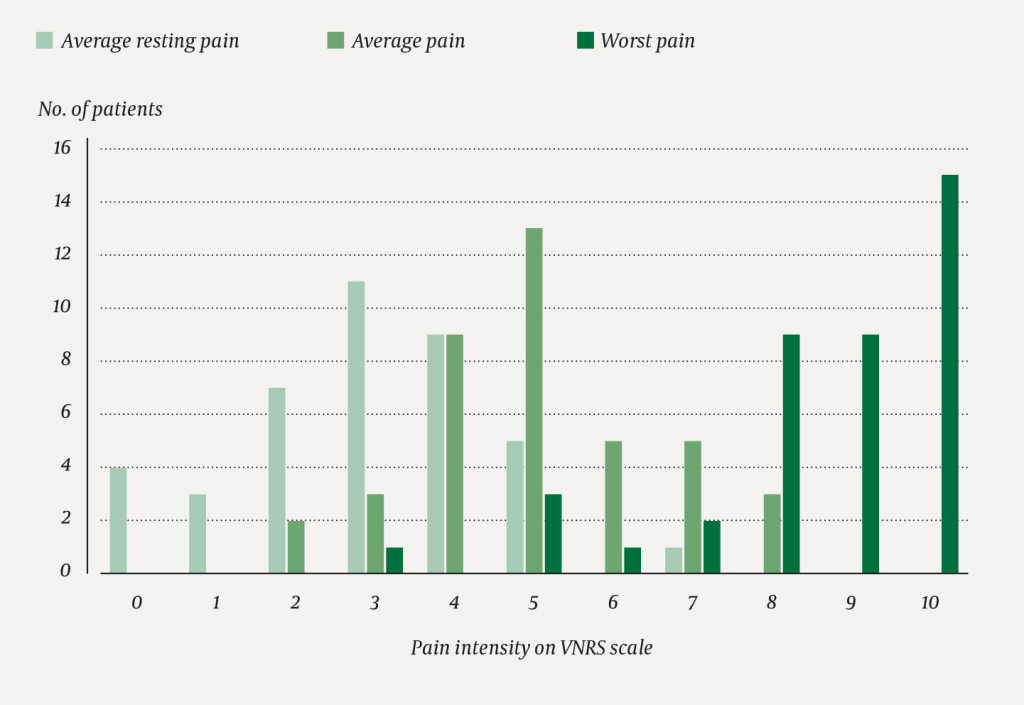
In the first two weeks, 15 patients had an average resting pain higher than 3 on a verbal numeric rating scale from 0 to 10.
When severe injuries have been incurred, the initial focus is on surgical treatment and life-saving measures. In studies of this early phase, severe pain has been reported in more than 50 % of conscious patients (1, 2). A high incidence of chronic pain has also been reported in severely injured patients (3). In a study from Oslo University Hospital in 2007, 62 % of severely injured patients experienced severe or very severe pain during their hospital stay, and 24 % had severe chronic pain after six years (3). Early-stage pain management was mostly limited to opioids.
In our study, we wanted to investigate the intensity of pain in the first two weeks after severe injuries had been incurred, which pain-relieving methods and medications were used, as well as the planned use of pain relief after discharge from hospital.
Material and method
The study was conducted at the Emergency Department, Oslo University Hospital, Ullevål, in the period June 2018–March 2019. The Regional Committee for Medical and Health Research Ethics classified the study as a quality assurance study, and as such it was outside their mandate. The study was approved by the Data Protection Officer at Oslo University Hospital (case number 17/1740) and registered at clinicaltrials.gov (registration number NCT 03730272).
Patients were assessed for possible inclusion in a daily review of the trauma register at Oslo University Hospital. The inclusion criteria were as follows: aged 18 and over, sent directly to our trauma team from the site where the injury was incurred, an ISS score higher than 8, competent to give consent and ability to communicate well in Norwegian or English. The Injury Severity Score (ISS) has a scale from 0 to 75, and the score is calculated by grading the severity of the injury from 1 to 6 in each of six body regions. The scores from the three most severely injured body regions are then squared and added together. An ISS score of 9 can indicate a moderate injury in two different regions or one moderate to severe injury in one region.
We excluded patients who were intubated, or had isolated head injuries, a Glasgow Coma Scale score below 9, a high spinal cord transection, a diagnosed substance abuse disorder, or were discharged within six hours.
Written informed consent was obtained, and data were collected from patient records, the trauma register and patient interviews. The interviews were conducted an average of two weeks (95 % within 11–17 days) after the injury was incurred. Patients were asked about the pain they experienced after the injury. For pain intensity, they were asked about the average pain, average resting pain and worst pain that they experienced during the two-week period, indicated by a verbal numeric rating scale (VNRS) from 0 to 10 (0 = no pain, 10 = worst pain imaginable). In order to establish the timing of pain, the patients were asked about the total duration of pain with a score higher than 3.
They were also asked about the administration of analgesics in the period up to the point of interview, and the answers were checked against patient records and discharge reports. Hospital-prescribed analgesics for the period after discharge were registered. All patients' discharge reports were read to obtain information on opioid prescribing and any plans for tapering or cessation.
Results
After checking the patient lists, a total of 64 were considered to be relevant candidates for the study. Of these, 22 were excluded, and two of the remaining 42 declined to participate.
Of the 40 patients included, 30 were men. The mean age was 46 years (range 25–82 years), and the mean ISS score was 17 (9–30). Overall, 19/40 (48 %) patients had been injured in traffic accidents, and 33/40 (83 %) had experienced blunt trauma.
At the time of interview, 33/40 (83 %) had been discharged. During the two-week period, 35/40 (88 %) reported an average pain higher than 3 on the VNRS scale, and of these, 13/40 (33 %) scored more than 5. In 15/40 (38 %), the average resting pain had been higher than 3. 19/40 (48 %) reported having a pain score higher than 3 for more than half of the period after the injury.
All patients were treated with opioids and paracetamol while in hospital, and 31 of 40 (78 %) received epidural analgesics or nerve blockers, 14/40 (35 %) received ketamine, 11/40 (28 %) NSAIDs, 9/40 (23 %) alpha-2 agonists and 4/40 (10 %) gabapentinoids. Upon discharge, the following analgesics were prescribed for further use: paracetamol to 31/40 (78 %), opioids to 31/40 (78 %), NSAIDs to 3/40 (8 %), gabapentinoids to 2/40 (5 %) and alpha-2 agonists to 4/40 (10 %). At the time of the interview, 29/40 (73 %) were using opioids. None of the discharge reports included a plan for tapering or cessation of the opioid treatment.
Discussion
In this study of conscious, severely injured patients, we found that 88 % had an average pain score higher than 3 on the VNRS scale during the first two weeks after the injury was incurred. At rest, 38 % had an average score of more than 3, which corresponds to moderate to severe pain. This was despite the fact that everyone had received paracetamol and opioids to treat the pain, and 78 % had received epidural analgesics or nerve blockers in addition.
Although nerve blockers are very effective for pain relief, they are normally only used for a short period immediately after the injury was incurred and will not prevent pain in the subsequent period (4). Opioids were prescribed for use after discharge for 78 % of the patients, but none of the patient records indicated that they had been given advice about opioid tapering or cessation. We do not know what kind of oral information the patients received, but in light of the current discourse about opioid abuse, this situation is in need of urgent improvement. A Swedish study showed that the risk of opioid abuse was more than three times greater in patients who had incurred an injury than in the control population (5). Particularly prolonged use after discharge following trauma or surgery is associated with an increased risk of misuse (6).
A weakness of our study is that patients were only asked to assess pain retrospectively after a two-week period in which most experienced varying and decreasing pain intensity. We were able to note what treatment was actually given at the time of admission and at the interview, but we do not know to what extent the medications prescribed upon discharge were actually used beyond the two-week period. Mixed datasets on trauma, such as ours, tend to have a predominance of young men and people with psychosocial problems (3). Our findings about pain and pain reactions are therefore not directly transferable to the general population.
Our conclusion is that many trauma patients suffer severe pain after incurring a serious injury and that there is potential to improve this by increasing the use of non-opioid analgesic drugs. This is important both to lessen unnecessary suffering and to reduce opioid use. Patients and general practitioners should be given information about the tapering and cessation of opioids after discharge from hospital.
The article has been peer-reviewed.
- 1.
Berben SA, Schoonhoven L, Meijs TH et al. Prevalence and relief of pain in trauma patients in emergency medical services. Clin J Pain 2011; 27: 587–92. [PubMed][CrossRef]
- 2.
Farčić N, Barać I, Pačarić S et al. Acute postoperative pain in trauma patients – The fifth vital sign. Open Access Maced J Med Sci 2017; 5: 310–5. [PubMed][CrossRef]
- 3.
Kolstadbraaten KM, Spreng UJ, Wisloeff-Aase K et al. Incidence of chronic pain 6 y after major trauma. Acta Anaesthesiol Scand 2019; 63: 1074–8. [PubMed][CrossRef]
- 4.
Holmberg A, Sauter AR, Klaastad Ø et al. Pre-operative brachial plexus block compared with an identical block performed at the end of surgery: a prospective, double-blind, randomised clinical trial. Anaesthesia 2017; 72: 967–77. [PubMed][CrossRef]
- 5.
von Oelreich E, Eriksson M, Brattström O et al. Risk factors and outcomes of chronic opioid use following trauma. Br J Surg 2020; 107: 413–21. [PubMed][CrossRef]
- 6.
Brat GA, Agniel D, Beam A et al. Postsurgical prescriptions for opioid naive patients and association with overdose and misuse: retrospective cohort study. BMJ 2018; 360: j5790. [PubMed][CrossRef]