This case report illustrates the challenges of diagnosing pulmonary embolism and sheds light on an association between thromboembolism and Klinefelter's syndrome.
A man in his forties was admitted to the Department of Medicine with functional dyspnoea. Three weeks earlier, he had noticed swelling in his lower right leg and transient chest pain. He had had functional dyspnoea for two days and had fainted while climbing the stairs.
Upon arrival at hospital, the patient was breathing normally, with blood pressure 124/84 mm Hg, heart rate 84 beats per minute, respiratory rate 16 per minute and temperature 36.5 °C measured with an infrared forehead thermometer. Oxygen saturation was 97 % with pulse oximetry on room air. Breath sounds were diminished over the basal region of the left lung. The patient's right calf was tense and tender to palpation with pitting oedema extending halfway up the calf but with no redness or warmth.
Scoring tools revealed a moderate pre-test probability of pulmonary embolism, with a Geneva score of 10 points, and a modified Wells score of 6 points. The patient had Klinefelter's syndrome and was taking testosterone supplements. He had polycythaemia, probably secondary to the testosterone replacement therapy, and was therefore taking acetylsalicylic acid (Albyl-E) 75 mg × 1 and undergoing regular therapeutic venesection. He had no other known risk factors for pulmonary embolism.
The ECG showed non-significant ST elevations (II, aVF and V6) and T-wave inversions (V1 and V2). Arterial blood gases (room air) showed pH 7.45 (reference range 7.36–7.44), pCO2 4.5 kPa (4.7–5.9) and pO2 9.7 kPa (11.0–14.4). A chest X-ray showed sparse laminar basilar atelectases, and blood tests revealed CRP 24 mg/L (< 5), troponin T 22–25 ng/L in two sets (< 15) and D-dimer > 4.00 mg/L (< 0.5).
Enoxaparin (Clexane) 1 mg/kg was administered subcutaneously × 2. The patient was placed on telemetry monitoring, and a CT pulmonary angiogram was ordered for the next day. This revealed an extensive saddle thrombus as well as bilateral segmental pulmonary emboli (Figure 1). The patient was therefore transferred to the intermediate care ward for close monitoring of his circulatory status. Echocardiography revealed a thrombus in the pulmonary artery, a slightly dilated right ventricle, and flattening of the interventricular septum. Estimated pulmonary artery systolic pressure was 55 mm Hg (< 36).
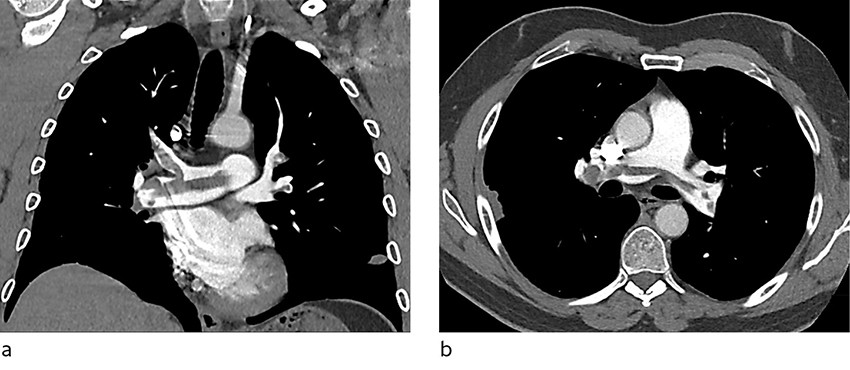
The patient scored 59 points on the Pulmonary Embolism Severity Index (PESI), corresponding to class I (≤ 65 points), with a good prognosis. No signs of circulatory shock were observed over the course of the next four days, and therefore thrombolytic therapy was not administered. The patient's troponin levels normalised after four days. Echocardiography prior to departure showed normalised septal motion and almost normal pressure readings.
The patient was discharged in good general condition after one week, with instructions to take direct-acting oral anticoagulants (DOACs), specifically rivaroxaban (15 mg twice daily for three weeks, then 20 mg once daily for life). Albyl-E was discontinued. Two years later, his dyspnoea has not recurred.
Discussion
Pulmonary embolism with circulatory shock is a clear indication for thrombolytic therapy. In the absence of circulatory shock, a decision on whether to monitor patients for the development of shock should be based on PESI scores, troponin levels and signs of right ventricular dysfunction; if a patient does develop shock, thrombolytic therapy should be considered. Patients with evidence of both right ventricular dysfunction and increased troponin levels should initially be monitored closely. A common dilemma when on call is whether to perform a CT pulmonary angiogram immediately or wait until the next day. Here, it was decided to wait, but if CT had been used to determine the right ventricular (RV)/left ventricular (LV) diameter ratio, the patient's right ventricular dysfunction might have been detected earlier (1). Syncope in the medical history of a patient with pulmonary embolism is a clinical indicator of increased risk of massive embolisation and death (2). Such patients require rapid assessment and close monitoring.
Our patient had Klinefelter's syndrome, a chromosome abnormality seen in males, usually in the form of an additional X chromosome. The condition affects 1: 500–1: 1 000 men, but it is estimated that 75 % of men with Klinefelter's syndrome are undiagnosed. Typical physical traits are above-average height, reduced body hair, and gynaecomastia that persists after puberty. All adults with Klinefelter's syndrome have small testicles, and many will have decreased libido and hypergonadotropic hypogonadism (3).
Several studies have shown an increased incidence of venous thromboembolism in patients with Klinefelter's syndrome. A Swedish study from 2016 followed 1 085 men with Klinefelter's syndrome for 41 years, and reported a standardised incidence ratio for venous thromboembolism of 6.43 (95 % CI 5.15–7.93) compared with the general population. The incidence of venous thromboembolism was 8.6 % at 50 years of age and as much as 20.8 % at 70 (4). Based on these findings, patients with Klinefelter's syndrome have a persistently elevated thrombosis risk, similar to that of patients with hypercoagulability syndromes (4, 5); we therefore recommended lifelong anticoagulant therapy, as is standard practice for patients with persistent risk factors for thrombosis. We are not aware of any studies on the optimal duration of anticoagulant therapy in patients with Klinefelter's syndrome (5). In a young man with a low risk of bleeding, anticoagulant therapy would probably be recommended indefinitely also in cases of unexplained pulmonary embolism.
No single factor has been identified that can explain why patients with Klinefelter's syndrome are at increased risk of venous thromboembolism, but the genes for factor VIII and factor IX are located on the X chromosome, and increased levels of coagulation factors have been observed in Klinefelter's syndrome (6). Testosterone-replacement therapy could potentially increase the risk of thromboembolism. Thrombosis risk should therefore be considered prior to the initiation of testosterone-replacement therapy in patients with Klinefelter's syndrome.
The patient has consented to the publication of this article.
The article has been peer-reviewed.
- 1.
Konstantinides SV, Meyer G, Becattini C et al. 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS): The Task Force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC). Eur Respir J 2019; 54: 1901647. [PubMed][CrossRef]
- 2.
Omar HR, Mirsaeidi M, Weinstock MB et al. Syncope on presentation is a surrogate for submassive and massive acute pulmonary embolism. Am J Emerg Med 2018; 36: 297–300. [PubMed][CrossRef]
- 3.
Lanfranco F, Kamischke A, Zitzmann M et al. Klinefelter's syndrome. Lancet 2004; 364: 273–83. [PubMed][CrossRef]
- 4.
Zöller B, Ji J, Sundquist J et al. High risk of venous thromboembolism in Klinefelter syndrome. J Am Heart Assoc 2016; 5: e003567. [PubMed][CrossRef]
- 5.
Anderson FA, Spencer FA. Risk factors for venous thromboembolism. Circulation 2003; 107: I9–16. [PubMed][CrossRef]
- 6.
Dissemond J, Knab J, Lehnen M et al. Increased activity of factor VIII coagulant associated with venous ulcer in a patient with Klinefelter's syndrome. J Eur Acad Dermatol Venereol 2005; 19: 240–2. [PubMed][CrossRef]