Treatment rates for lumbar spine surgery in Norway and Northern Norway Regional Health Authority 2014–18
Main findings
The average rate of surgical treatment for degenerative lumbar spine disease in Norway remained stable at approximately 120 surgical procedures per 100 000 inhabitants per year during the period 2014–18.
The treatment rate was lower for inhabitants within the Northern Norway Regional Health Authority area (91% of the national average), mainly because of a considerably lower rate of complex spine surgery (57% of the national average).
Service provision coverage within the Northern Norway Regional Health Authority area was low in the local hospital functions for simple spine surgery at Nordland Hospital and Helgeland Hospital (approximately 30%) and in the regional function for complex spine surgery at the University Hospital of North Norway (55%).
Lumbar spine conditions are the most common cause of non-fatal health loss and short-term sickness absence, and the second most frequent reason for disability (1, 2). Diagnostic imaging is recommended if symptoms persist for more than four to six weeks without any improvement (3). More than 50 % of those examined are diagnosed with a herniated disc, spinal stenosis or other degenerative changes. Many are therefore referred for assessment with a view to surgical treatment, which could be relevant for patients with persistent discomfort and neurological symptoms caused by a lumbar disc herniation or lumbar spinal stenosis.
In the United States, decompression or spinal fusion for degenerative lumbar spine disease were the third and fifth most frequent surgical interventions respectively to be carried out in the period 2003–2014 (4). Many have reported increasing treatment rates (5–8), but few have studied the total consumption of lumbar spine surgery (9). In Norway, the treatment rate increased by 54 % from 78 to 120 procedures per 100 000 inhabitants per year from 1999 to 2013 (10).
In board agenda item 55–2004, Northern Norway Regional Health Authority decided that complex spine surgery should be undertaken as a regional function at the University Hospital of North Norway in Tromsø and simple spine surgery as a local hospital function at Helgeland Hospital Mo i Rana and Nordland Hospital Bodø. University Hospital of North Norway covers the local hospital function within its own catchment area as well as that of Finnmark Hospital.
The objective of this study was to investigate whether the provision of spine surgery within the area of Northern Norway Regional Health Authority complies with the distribution of functions that have been decided, and whether there are any geographical variations in service provision. We therefore studied the treatment rates in Norway as whole and within the Northern Norway Regional Health Authority area and assessed the activity in the region.
Material and method
Study design and data source
We used data on hospitalisations for lumbar spine surgery from the Norwegian Patient Registry in the period 2014–18. The registry encompasses all lumbar spine surgery in Norway, with the exception of procedures that have been performed in private hospitals and paid for by the patients themselves or by private health insurance.
The data extraction was based on an algorithm validated by the National Quality Registry for Spine Surgery (11, 12). We modified the algorithm by excluding removal of osteosynthesis material and including surgical treatment of fractures. The algorithm included patients with ICD-10 diagnostic codes for degenerative lumbar spine disease or thoracolumbar spinal fracture combined with NSCP procedure codes for decompression surgery, spinal fusion surgery or treatment of fracture. The procedures were categorised as simple spine surgery (discectomy and/or other decompression for lumbar disc herniation or spinal stenosis), complex spine surgery (spinal fusion and/or disc prosthetics surgery and/or other instrumentation) or surgical treatment of fractures. These categorisations accord with the definitions in the National Quality Registry for Spine Surgery and with the use of the terms 'simple' and 'complex' spine surgery in the decision regarding distribution of functions by Northern Norway Regional Health Authority. The algorithm excluded patients who underwent cervical spine surgery for cancer or other neoplastic disease, scoliosis and infections, as well as those who underwent repeat surgery for removal of osteosynthesis material.
Treatment rates
Treatment rates were estimated as the number of procedures per 100 000 inhabitants per area of residence per year. Areas of residence were defined at three levels, as in the Norwegian Health Atlas: the catchment areas of the regional health authorities, the health enterprises and the local hospitals respectively (13). The rates include all those who have undergone surgery per year, divided by the population (0–105 years) in the area of residence registered by Statistics Norway as of 1 January in the same year, standardised by sex and age, with 2015 as the reference year. The analysis encompassed all of Norway, but we focused on residents in the area of Northern Norway Regional Health Authority, i.e. the catchment areas for Finnmark Hospital (Finnmark county), University Hospital of North Norway (Troms county and the Ofoten district), Nordland Hospital (Nordland district) and Helgeland Hospital (the Helgeland district).
Local coverage
Local coverage was defined as the proportion of patients who underwent surgery at a hospital within their own area of residence (14). We categorised the treatment locations as the University Hospital of North Norway, Nordland Hospital Bodø, Helgeland Hospital Mo i Rana, public hospitals in other health regions or private hospitals under contract with a regional health authority. For residents in Finnmark county, surgery at the University Hospital of North Norway was registered as treatment within the area of residence, since this hospital provides local hospital functions for Finnmark county.
Ethics
The Centre for Clinical Documentation and Evaluation is authorised to analyse data pursuant to the Data Protection Regulation and exempted from the duty of confidentiality by the Regional Committee for Medical and Health Research Ethics (REK North). As a consequence, the study was not subject to notification. For reasons of privacy, the data source hides the exact figures for registrations that occur with a frequency of less than five per year, but this has no effect on the total figures.
Results
Activity and treatment rates
The number of inhabitants and the number of surgical procedures in Norway increased by the same proportion, leaving the treatment rate for simple and complex spine surgery stable at an average of 120 procedures per 100 000 inhabitants per year over the period (Table 1). In the area encompassed by Northern Norway Regional Health Authority, the number of inhabitants grew at a slower rate, and the number of surgical procedures showed little variation with no clear trend over time. The average rate amounted to 109 surgical procedures per 100 000 inhabitants per year (91 % of the national average).
Table 1
Number of inhabitants, number of surgical procedures for degenerative lumbar spine disease (simple and complex surgery) and treatment rates standardised by sex and age (number of procedures per 100 000 inhabitants per area of residence per year) for people resident in Norway as a whole and in the area of Northern Norway Regional Health Authority, 2014–2018.
| Area of residence | 2014 | 2015 | 2016 | 2017 | 2018 | Average | |
|---|---|---|---|---|---|---|---|
| Norway | |||||||
| Inhabitants, n | 5 165 802 | 5 213 985 | 5 258 317 | 5 295 619 | 5 328 212 | 5 252 387 | |
| Surgical procedures, n | 5 995 | 6 342 | 6 417 | 6 492 | 6 494 | 6 348 | |
| Treatment rate | 116.5 | 121.6 | 121.6 | 121.5 | 120.2 | 120.3 | |
| Northern Norway Regional Health Authority | |||||||
| Inhabitants, n | 480 740 | 481 994 | 484 647 | 486 001 | 486 452 | 483 967 | |
| Surgical procedures, n | 552 | 566 | 544 | 562 | 518 | 548 | |
| Treatment rate | 111.1 | 113.8 | 108.0 | 110.6 | 101.8 | 109.1 | |
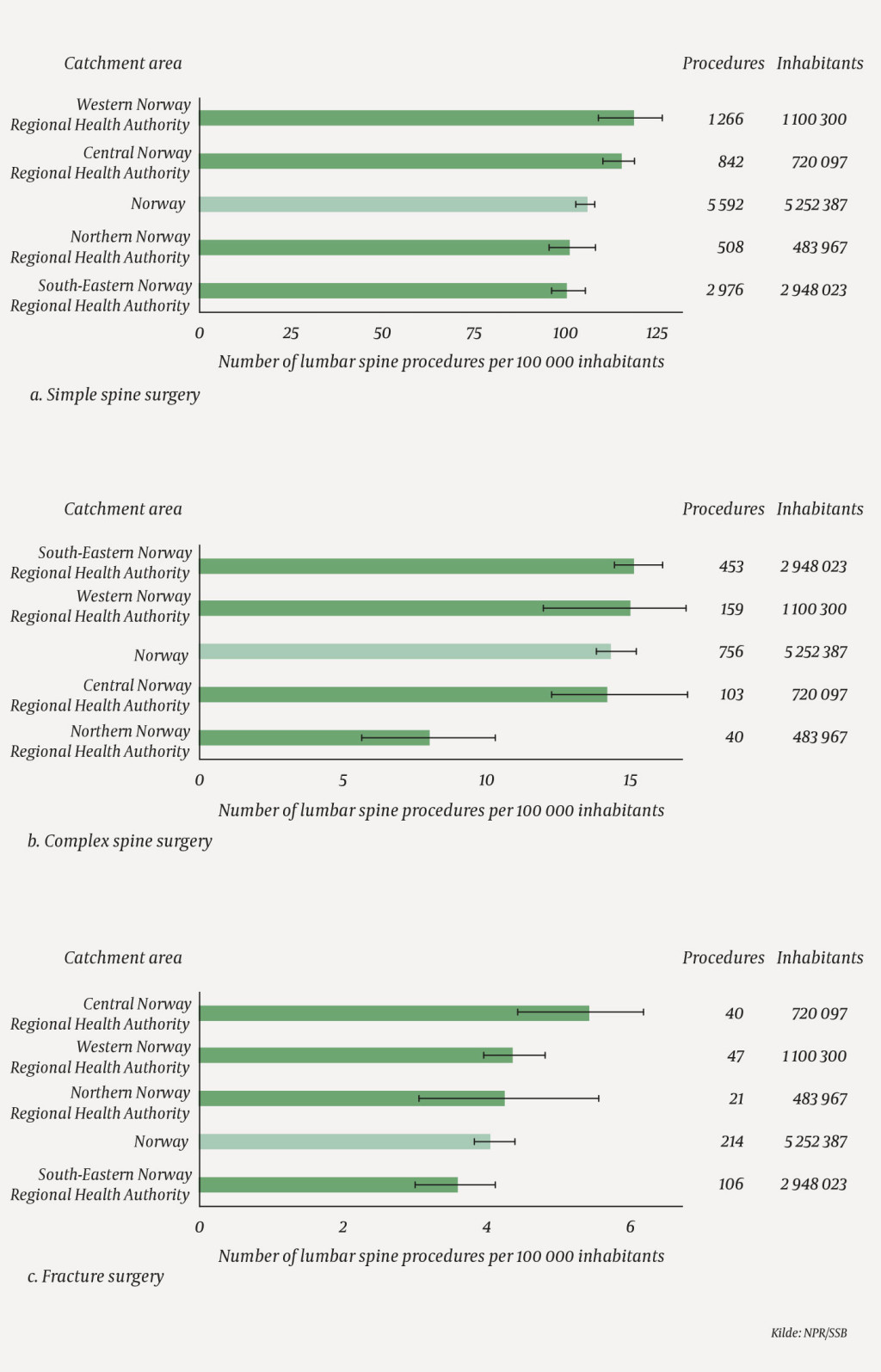
There were minor variations in the treatment rates for simple spine procedures and treatment of fractures in Norway during this period (Figures 1a and 1c). For those resident in the area of Northern Norway Regional Health Authority, the average treatment rates for simple and complex spine surgery were 101 (95 % of the national average) and 8 (57 % of the national average) lumbar spine procedures per 100 000 inhabitants per year respectively (Figures 1a and 1b).
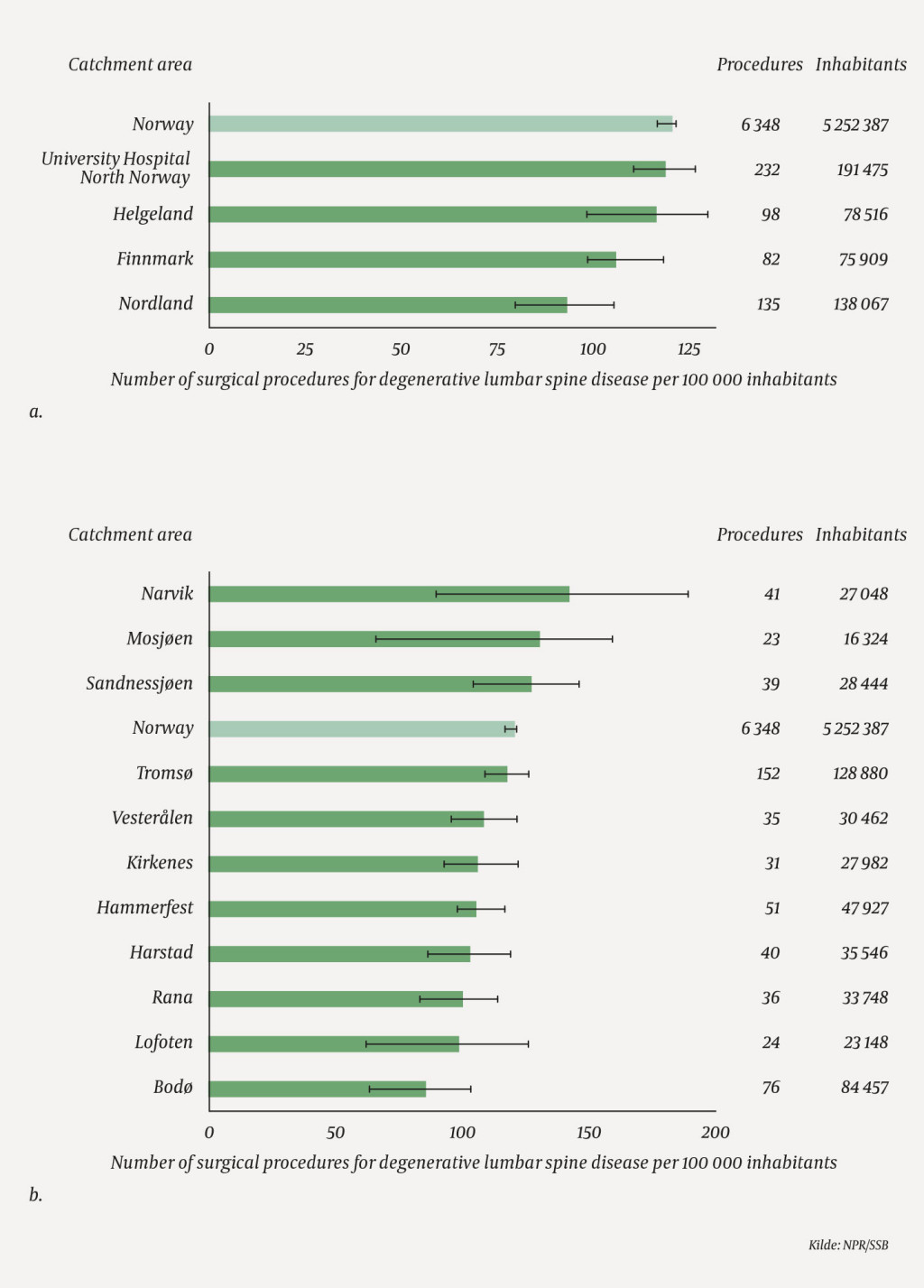
The differences in treatment rates between the areas of residence in the catchment area of Northern Norway Regional Health Authority were moderate, but there were large annual variations in some areas of residence (Figure 2). Starting from 2015, residents in the local hospital area of Bodø had a consistently lower rate than the national average, with an average of 86 surgical procedures per 100 000 inhabitants per year (72 % of the national average).
Local coverage
The number of surgical procedures for degenerative lumbar spine disease among people resident in the Northern Norway Regional Health Authority area included 2 541 (93 %) simple and 201 (7 %) complex procedures. The local coverage (simple and complex spine surgery) increased from 60 % to 84 % over the period (Table 2). Local coverage remained stable at more than 90 % for emergency surgery over the entire period (data not shown).
Table 2
Place of treatment for patients who were resident in the Northern Norway Regional Health Authority area and who underwent surgery for degenerative lumbar spine disease (simple and complex surgery), 2014–2018. Number (%). UNN = University Hospital of North Norway.
| Place of treatment | 2014 | 2015 | 2016 | 2017 | 2018 | Average | |
|---|---|---|---|---|---|---|---|
| Northern Norway Regional Health Authority | 334 (60) | 432 (76) | 439 (81) | 453 (81) | 436 (84) | 419 (77) | |
| UNN Tromsø | 265 (48) | 359 (63) | 363 (67) | 367 (65) | 352 (68) | 341 (62) | |
| Central Norway Regional Health Authority | 78 (14) | 50 (9) | 20 (4) | 27 (5) | 33 (6) | 41 (7) | |
| Western Norway Regional Health Authority | 45 (8) | 19 (3) | 7 (1) | 11 (2) | 6 (1) | 17 (3) | |
| South-Eastern Norway Regional Health Authority | 20 (4) | 22 (4) | 28 (5) | 29 (5) | 35 (7) | 27 (5) | |
| Private hospital under contract | 75 (14) | 43 (8) | 50 (9) | 42 (7) | 8 (2) | 44 (8) | |
| Total | 552 (100) | 566 (100) | 544 (100) | 562 (100) | 518 (100) | 548 (100) | |
In 2014, approximately 65 % of all patients resident in Finnmark and Troms counties and the Ofoten district underwent surgery at the University Hospital of North Norway in Tromsø, 25 % in state-owned hospitals in other regions and 10 % in private hospitals under contract with a regional health trust (Table 3). This situation changed during the period: in 2018, more than 90 % underwent surgery at the University Hospital of North Norway and less than 5 patients were treated in private hospitals. For those resident in the Nordland and Helgeland districts, the only clear trend over time was that the proportion of nearly 20 % who underwent surgery in private hospitals at the start of the period gradually fell to less than 5 patients in 2018.The degree of local coverage varied by around 30 % for both regions of residence. In the period overall, a larger proportion of the residents of the Nordland district (42 %) underwent surgery at the University Hospital of North Norway, compared to residents of the Helgeland district (24 %). The proportion of patients treated in state-owned hospitals in another health region was higher for residents of the Helgeland (28 %) than for Nordland district (17 %).
Table 3
Place of treatment for patients resident in the area of Northern Norway Regional Health Authority who underwent surgery for degenerative lumbar spine disease (simple and complex surgery), 2014–2018, by the regions of residence covered by the health trusts.1 Number of procedures (%). UNN = University Hospital of North Norway.
| Region of residence | Treatment location | 2014 | 2015 | 2016 | 2017 | 2018 |
|---|---|---|---|---|---|---|
| Finnmark Hospital | UNN Tromsø | 51 (66) | 64 (81) | 82 (88) | 71 (83) | 70 (92) |
| Nordland Hospital Bodø | 0 | 0 | 0 | / | / | |
| Public hospital in another health region | 18 (23) | 12 (15) | 8 (9) | 10 (12) | 6 (8) | |
| Private hospital | 8 (10) | / | / | / | 0 | |
| UNN | UNN Tromsø | 139 (64) | 206 (84) | 205 (88) | 218 (88) | 200 (91) |
| Public hospital in another health region | 55 (26) | 27 (11) | 14 (69 | 17 (7) | 15 (7) | |
| Private hospital | 22 (10) | 12 (5) | 14 (6) | 14 (6) | / | |
| Nordland Hospital | UNN Tromsø | 52 (35) | 61 (45) | 55 (47) | 61 (45) | 55 (40) |
| Nordland Hospital Bodø | 35 (23) | 38 (28) | 29 (25) | 43 (32) | 54 (39) | |
| Helgeland Hospital Mo i Rana | 0 | 0 | 0 | 0 | / | |
| Public hospital in another health region | 36 (24) | 22 (16) | 14 (12) | 17 (13) | 26 (19) | |
| Private hospital | 27 (18) | 15 (11) | 18 (16) | 15 (11) | / | |
| Helgeland Hospital | UNN Tromsø | 23 (21) | 28 (26) | 21 (21) | 17 (19) | 27 (32) |
| Nordland Hospital Bodø | 5 (5) | / | 9 (9) | 6 (7) | 6 (7) | |
| Helgeland Hospital Mo i Rana | 29 (27) | 31 (29) | 38 (37) | 36 (40) | 23 (27) | |
| Public hospital in another health region | 34 (31) | 30 (28) | 19 (19) | 23 (25) | 27 (32) | |
| Private hospital | 18 (17) | 13 (12) | 15 (15) | 9 (10) | / |
1For reasons of data protection, the data source hides the exact figures for registrations that occur with a frequency of less than 5 per health enterprise area per year, but this has no effect on the totals at the aggregated level. Frequencies < 5 are marked with a slash.
A component analysis of simple spine surgery alone (data not shown) shows nearly the same distribution and trend over time as the analysis of all surgical procedures for degenerative lumbar spine disease.
The distribution of complex spine surgery by treatment location remained stable, and the local coverage within the area of Northern Norway Regional Health Authority was low, with an average of 22 (55 %) procedures per year undertaken at the University Hospital of North Norway Tromsø and 16 (40 %) in public hospitals other regions. The proportion of patients treated outside the region was the same among residents of the four areas covered by the four health enterprises. Altogether 50 % of the procedures were undertaken in hospitals under South-Eastern Norway Regional Health Authority. Treatment of fractures occurred only in exceptional cases (0–3 patients per year) outside the region (data not shown).
Discussion
The treatment rate for lumbar spine surgery in Norway remained stable, and there were only minor variations between the regions in terms of the rates for treatment of fractures and simple spine surgery during the study period. There was greater variation in the treatment rate for complex spine surgery, with a rate for residents in the area of Northern Norway Regional Health Authority of 57 % of the national average. Local coverage was low in the area of Northern Norway Regional Health Authority, especially in the local hospital functions for simple spine surgery at Nordland Hospital Bodø and Helgeland Hospital Mo i Rana (approximately 30 %) and in the regional function for complex spine surgery at the University Hospital of North Norway Tromsø (55 %).
Treatment rates
Similarly with our study, Grotle and colleagues also analysed figures from the Norwegian Patient Registry and found that the treatment rate for lumbar spine surgery in Norway increased from 78 to 120 procedures per 100 000 inhabitants per year from 1999 to 2013 (10). We found that the rate has remained consistently at the same level in the following years. However, the number of procedures nevertheless increased by nearly 500 from 2014 to 2018. The studies indicate that this trend is mainly caused by demographic change in the form of an increasing population and a growing proportion of older people. The increasing population and the growing proportion of older people will help generate a continued increase in the number of procedures per year, especially for lumbar stenosis that affects the elderly, even if the rates remain stable.
The treatment rate remained stable also for those who were resident in the area of Northern Norway Regional Health Authority, but at a lower level (91 %) than the national average. Similar differences between the regions were observed also in the period 1999–2013 (M. Grotle, personal communication). The large annual variations in some districts of residence are likely to be random in areas with few inhabitants. The differences in average rates were small, with the exception of residents in the Bodø district, who had a rate of 72 % of the national average in the period 2015–2018. This is equivalent to 20 procedures less than the national average per year.
The treatment rates in Norway are far lower than those for equivalent spine surgery in the United States, where 149 simple and 144 complex procedures were undertaken per 100 000 inhabitants in 2012 (4). In the UK, the rate for all lumbar spine procedures amounted to 49 per 100 000 inhabitants in 2013, while in Ireland, the rate remained stable at approximately 26 per 100 000 inhabitants per year in the period 2012–2016 (9, 15). The British study did not state whether procedures undertaken in private hospitals were included, while the Irish study only analysed data from public hospitals. It is nevertheless likely that these rates are lower than in Norway.
The Norwegian Patient Registry does not include surgical procedures that have been undertaken in private hospitals and that have been paid for by the patients themselves or by private health insurance. However, these hospitals report data to the National Quality Registry for Spine Surgery, which in 2018 recorded 862 procedures undertaken by seven private hospitals. More than 10 % of all spine surgery procedures are undertaken without any public funding. The total Norwegian treatment rate may thus be close to 140 procedures per 100 000 inhabitants per year. Patients who undergo surgery in private hospitals in Norway are on average younger and have a higher level of education, better health and fewer risk factors for an adverse outcome when compared to patients in public hospitals (16). Private health insurance most likely contributes to geographical variation and less equality in service provision.
Local coverage
Local coverage in the area of Northern Norway Regional Health Authority was low in 2014, but increased to 84 % in 2018 as a result of approximately 100 additional lumbar spine procedures per year at the University Hospital of North Norway in Tromsø. The local coverage in the local hospital function for simple spine surgery remained stably low (approximately 30 %) at Nordland and Helgeland hospitals. The University Hospital of North Norway to some extent and increasingly compensated for this by performing 30–40 % of this function. In the same period, the local coverage of the regional function for complex spine surgery at the University Hospital of North Norway remained persistently low (55 %).
Treatment in private hospitals under contract with a regional health authority virtually ceased in 2018, because South-Eastern Norway Regional Health Authority did not renew its contracts for purchase of lumbar spine procedures after April 2018 (O. Tjomsland, personal communication). The other regional health authorities have no such contracts, and patients from the Northern Norway Regional Health Authority area (and the rest of the country) therefore lost the possibility to choose treatment in private institutions through the Free Hospital Choice scheme. Until 2017, the scheme was used by an average of 55 patients from Northern Norway each year. This shortfall has not been compensated for by an equivalent capacity increase in the region, and this tallies well with the observation that the number of lumbar spine procedures fell by close to 50 in 2018. This raises the question of whether the regional health authorities might cooperate better in their capacity planning.
Assessment of the activity
Wennberg categorised health services as effective, preference-sensitive or supply-sensitive (17). Effective services have a well documented effect and there is a high degree of consensus regarding their utility. Little variation is expected in the use of such services. Consistent with this, we found little variation in surgical treatment of spinal fractures. Preference-sensitive services are characterised by the availability of treatment options, each with various advantages and disadvantages. Here, differences of opinion between clinicians, differences in patient preferences and differences in capacities between hospitals may give rise to greater variation. Wennberg assessed lumbar spine procedures, for which conservative treatment can be an alternative, as preference-sensitive (18). Better capacity at the University Hospital of North Norway for simple spine procedures that can be performed as day surgery than for complex procedures than require hospitalisation may have contributed to the lower treatment rate for complex spine surgery in the area of Northern Norway Regional Health Authority.
No generally recognised method is available for estimating the need for lumbar spine surgery in a population. A comparison of estimates for eight countries, including Norway, indicated a need for 100 procedures per 100 000 inhabitants per year (5). Equality in service provision with little geographic variation is a Norwegian policy objective. We therefore estimated what the activity level in the Northern Norway Regional Health Authority area would have been if the treatment rate for residents in this region had been equal to the national average, even if this is high. In this case, the average number of procedures would have been 585. This is equivalent to approximately 40 (whereof 30 complex) additional lumbar spine procedures per year. We did not investigate the associations between treatment rates, degrees of local coverage and waiting times, but the University Hospital of North Norway has the country's longest waiting time (12 months) for spine surgery (19). Studies indicate that the risk of an adverse outcome increases when the waiting time exceeds six months (20). Furthermore, it is assumed that implementation of evidence-based guidelines for conservative treatment can prevent unnecessary spine procedures (21).
It is uncertain whether, and if so how, the somewhat low treatment rate for simple spine procedures (95 % of the national average) should be emphasised in the assessment of activity, while the considerably lower rate for complex procedures (57 % of the national average) indicates non-equal service provision for residents of the area covered by Northern Norway Regional Health Authority. We therefore assume that the number of complex spine procedures should be increased by approximately 30 per year, to bring these to the same level as the national average. Irrespective of treatment rates, Northern Norway Regional Health Authority has as its goal that patients should prefer treatment within the region (22). The consumption in public hospitals in other regions amounted to an average of 85 lumbar spine procedures per year. In order to compensate for the cessation of service provision by private hospitals from 2018 onwards (53 procedures per year on average in the period 2014–2017), the activity in the region needs to increase by a total of approximately 170 procedures per year.
Conclusion
The treatment rate for complex spine surgery and the local coverage for all surgical treatment of degenerative lumbar spine disease were low in the catchment area of Northern Norway Regional Health Authority. In order to compensate for this within the region, the activity needs to increase by a total of approximately 170 interventions per year.
The article has been peer reviewed.
- 1.
Tollånes MC, Knudsen AK, Vollset SE et al. Sykdomsbyrden i Norge i 2016. Tidsskr Nor Legeforen 2018; 138: 1439–45.
- 2.
NAV. Mottakere av uføretrygd etter hoveddiagnose (primærdiagnose), alder og kjønn. https://www.nav.no/no/nav-og-samfunn/statistikk/aap-nedsatt-arbeidsevne-og-uforetrygd-statistikk/uforetrygd/diagnoser-uforetrygd Accessed 31.3.2020.
- 3.
Formidlingsenheten for muskel- og skjelettlidelser og Sosial- og helsedirektoratet. Nasjonale kliniske retningslinjer. Korsryggsmerter – med og uten nerverotaffeksjon. https://www.helsebiblioteket.no/retningslinjer/fysio-og-ergoterapi/ korsryggsmerter-med-og-uten-nerverotaffeksjon?lenkedetaljer=vis Accessed 8.7.2020.
- 4.
Fingar KR, Stocks C, Weiss AJ et al. Most frequent operating room procedures performed in U.S. hospitals, 2003–2012. HCUP statistical brief #186. Rockville, MD: Agency for healthcare research and quality, 2014.
- 5.
Kim P, Kurokawa R, Itoki K. Technical advancements and utilization of spine surgery–international disparities in trend-dynamics between Japan, Korea, and the USA. Neurol Med Chir (Tokyo) 2010; 50: 853–8. [PubMed][CrossRef]
- 6.
Steiger HJ, Krämer M, Reulen HJ. Development of neurosurgery in Germany: comparison of data collected by polls for 1997, 2003, and 2008 among providers of neurosurgical care. World Neurosurg 2012; 77: 18–27. [PubMed][CrossRef]
- 7.
Yoshihara H, Yoneoka D. National trends in the surgical treatment for lumbar degenerative disc disease: United States, 2000 to 2009. Spine J 2015; 15: 265–71. [PubMed][CrossRef]
- 8.
Martin BI, Mirza SK, Spina N et al. Trends in lumbar fusion procedure rates and associated hospital costs for degenerative spinal diseases in the United States, 2004 to 2015. Spine 2019; 44: 369–76. [PubMed][CrossRef]
- 9.
Sivasubramaniam V, Patel HC, Ozdemir BA et al. Trends in hospital admissions and surgical procedures for degenerative lumbar spine disease in England: a 15-year time-series study. BMJ Open 2015; 5: e009011. [PubMed][CrossRef]
- 10.
Grotle M, Småstuen MC, Fjeld O et al. Lumbar spine surgery across 15 years: trends, complications and reoperations in a longitudinal observational study from Norway. BMJ Open 2019; 9: e028743. [PubMed][CrossRef]
- 11.
Solberg TK, Olsen LR. Årsrapport 2013. Tromsø: Nasjonalt kvalitetsregister for ryggkirurgi, 2014. https://unn.no/Documents/Kvalitetsregistre/Nasjonalt%20kvalitetsregister%20for%20ryggkirurgi/Årsrapporter/Årsrapport_NRK_2013_.pdf Accessed 8.7.2020.
- 12.
Uleberg B, Balteskard L. Ortopedi i Helse Nord 2012–2016. Tjenestebruk og pasientstrømmer. Tromsø: Senter for klinisk dokumentasjon og evaluering, 2018. https://helse-nord.no/Documents/SKDE/SKDE%20Notater/Ortopedi%20i%20Helse%20Nord%202012-2016%20%28SKDE%202018%29.pdf Accessed 8.7.2020.
- 13.
Senter for klinisk dokumentasjon og evaluering. Helseatlas. https://helseatlas.no Accessed 8.7.2020.
- 14.
NOU 2016:25. Organisering og styring av spesialisthelsetjenesten – Hvordan bør statens eierskap innrettes framover? https://www.regjeringen.no/no/dokumenter/nou-2016-25/id2522062/ Accessed 17.9.2020.
- 15.
Walsh ME, Boland F, O'Byrne JM et al. Geographical variation in musculoskeletal surgical care in public hospitals in Ireland: a repeated cross-sectional study. BMJ Open 2019; 9: e028037. [PubMed][CrossRef]
- 16.
Madsbu MA, Salvesen Ø, Carlsen SM et al. Surgery for herniated lumbar disc in private vs public hospitals: A pragmatic comparative effectiveness study. Acta Neurochir (Wien) 2020; 162: 703–11. [PubMed][CrossRef]
- 17.
Wennberg JE. Unwarranted variations in healthcare delivery: implications for academic medical centres. BMJ 2002; 325: 961–4. [PubMed][CrossRef]
- 18.
Wennberg JE, Freeman JL, Culp WJ. Are hospital services rationed in New Haven or over-utilised in Boston? Lancet 1987; 1: 1185–9. [PubMed][CrossRef]
- 19.
Helse Norge. Velg behandlingssted. https://helsenorge.no/velg-behandlingssted/ventetider-for-behandling?bid=51 Accessed 1.4.2020.
- 20.
Siccoli A, Staartjes VE, de Wispelaere MP et al. Association of time to surgery with leg pain after lumbar discectomy: is delayed surgery detrimental? J Neurosurg Spine 2019; 32: 160–7. [PubMed][CrossRef]
- 21.
Foster NE, Anema JR, Cherkin D et al. Prevention and treatment of low back pain: evidence, challenges, and promising directions. Lancet 2018; 391: 2368–83. [PubMed][CrossRef]
- 22.
Helse Nord RHF. Visjon og verdier. https://helse-nord.no/om-oss/hva-gjor-helse-nord-rhf#visjon-og-verdier Accessed 31.3.2020.