Main findings
Of all individuals who tested positive for COVID-19, altogether 7 632 (94 %) were 20 years of age or older, and of these, 1 025 (13.4 %) had been hospitalised.
Among those hospitalised for COVID-19, there were a larger proportion of individuals with underlying conditions than in the general population after adjusting for age.
There were few differences between persons who had tested positive and the general population in terms of underlying conditions.
COVID-19 is caused by infection with SARS-CoV-2 (severe acute respiratory syndrome coronavirus 2), a coronavirus which rapidly spread to become a global pandemic after the first case was reported in Wuhan in December 2019. At an early stage, the most common conditions among persons who were hospitalised for COVID-19 were non-communicable diseases such as cardiovascular disease, cancer, diabetes and chronic respiratory diseases (1). At the start of the outbreak, advanced age was also identified as an important risk factor for a severe disease progression (2, 3). The clinical picture of COVID-19 is wide-ranging. Some will not notice any symptoms, while a minority will develop serious illness with pneumonia and a need for hospitalisation, possibly intensive care.
Younger people tend to have a milder disease course than older persons, and are less often hospitalised for COVID-19 (4). It has been debated whether chronic diseases independently increase the risk of severe illness or whether the presence of such diseases reflects the fact that those who develop a severe disease tend to be older (4). Norway has had limited testing capacity, and authorities have been particularly alert to persons with underlying diseases. These may thus be overrepresented among persons who are tested for COVID-19. We still have little knowledge about the degree to which various conditions, age and sex may account for a severe disease course with COVID-19 infection. The objective of this study is to describe the distribution of various conditions among persons with a confirmed COVID-19 infection and among patients hospitalised for COVID-19 compared to the general population.
Material and method
In this study we have used data from the Norwegian Patient Registry (NPR), the Norwegian Registry for Primary Health Care (KPR) (5), the Norwegian Surveillance System for Communicable Diseases (MSIS) in the Norwegian Institute of Public Health, and the Person Registry (the Norwegian Health Network's version of the National Population Registry).
The Norwegian Patient Registry is an administrative database that contains activity data from all government-funded hospitals and outpatient clinics from 2008 onwards. Reporting to the registry is mandatory and provides the basis for specialist health care reimbursements. The registry contains identities and ICD-10 codes (International Classification of Diseases, 10th revision). The Norwegian Registry for Primary Health Care, established in 2016, holds reimbursement claims sent to the government administration from therapists in the primary health service. The ICPC-2 coding system (International Classification for Primary Care, 2nd edition) is used in reimbursement claims. The Norwegian Surveillance System for Communicable Diseases receives notifications about confirmed SARS-CoV-2 infections from microbiological laboratories. The Person Registry was used to identify the study population to persons who were resident in Norway as of 1 March 2020.
The Norwegian Directorate of Health was provided with data on all individuals who had tested positive for SARS-CoV-2 in a polymerase chain reaction test (PCR) in the period 1 March 2020–13 May 2020. These data were linked to data from the Norwegian Patient Registry and the Norwegian Registry for Primary Health Care with the aid of a project-specific serial number shared by the three registries. Retrievals and linking of data and facilitation of statistics were undertaken with the aid of the database tool SQL Server Management Studio (SSMS, Microsoft) and the R statistics tool (6).
Population data were retrieved from Statistics Norway's website (population statistics per 1 January 2020, persons aged 20 years or older).
Ethics
The facilitation of statistics complies with the regulations for the registries in question, since the objectives of this study were monitoring and health security. Staff of the Norwegian Directorate of Health had no access to personal registration numbers or any other characteristics that could identify individuals. Staff of the Norwegian Institute of Public Health only had access to aggregated data in a tabular format.
Definitions
Diseases and conditions that could lead to an increased risk of a severe disease course COVID-19 were defined on the basis of knowledge about COVID-19 trajectories from other countries, the infection risk for influenza and the course of illnesses, as well as treatments and possible effects on the immune system (2). For some chronic diseases we used all available past data, while for others we went seven or five years back in time, depending on knowledge about the course of the disease (Tables 1 and 2). We included a large number of diseases, because monitoring and emergency preparedness were the main objective of this study, and there was little knowledge about COVID-19. Cancer patients in active treatment were included as a separate group, because many patients still go for regular follow-ups after primary cancer treatment and therefore remain registered in the Norwegian Patient Registry with a diagnostic code for cancer.
Table 1
Definitions of diseases and conditions used in the study
| Disease/condition | ICD-10 | ICPC-2 | |
|---|---|---|---|
| Diabetes1 | E10, E11 | T89, T90 | |
| Diabetes type 11 | E10 | T89 | |
| Diabetes type 21 | E11 | T90 | |
| Asthma1 | J45, J46 | R96 | |
| Chronic obstructive pulmonary disease from 40 years1 | J43, J44 | R95 | |
| Other chronic pulmonary disease1 | J41, J42, J47, J84, J98 | ||
| Cancer2 | C00–C97, D32–33, D35.2–35.4, D42–43, D44.3–44.5, D45–47 | ||
| Cardiovascular diseases3 | I00–I99, G45, H34 | K74–80, K82–83, K85–87, K89–92 | |
| Stroke3 | G45, I60–I61, I63–I64 (except I63.6), I69 | K89, K90–K91 | |
| Ischaemic heart disease3 | I20–I25 | K76 | |
| Atrial fibrillation3 | I48 | K78 | |
| Cardiac failure3 | I50, I11.0, I13.0, I13.2, I42 | K77 | |
| Hypertension2 | I10 | K86 | |
| Complications of hypertension 2 | I11–I13, I15 | K87 | |
| Obesity2 | E66 | T82 | |
| Overweight2 | T83 | ||
| Hypercholesterolaemia2 | E78 | T96 | |
| Dementia1 | F00–F03, G30, G31.0, G31.8, G31.2 | ||
| Hip fracture1 | S72.0, S72.1, S72.2 | ||
| Renal failure1 | N18.3–N18.5 | ||
| Gastric ulcer and diseases of the biliary tract2 | K80, K81, K83, K25, K26, K27 | ||
| Neurological disorders1 | G12, G20–21, G30–32, G35, G40–41, G70–73 | ||
| Cerebral palsy1 | G80–G83 | ||
| Transplantation1 | Z94.0–Z94.4, Z94.8 | ||
| Immunological failure1 | D80–D84 | ||
| Rheumatological diseases1 | M05–M09 | L88 | |
| Inflammatory bowel disease1 | K50, K51, K52 | D94 | |
| Biological drugs4 | 4AA23, 4AA24, 4AA26, 4AA33, 4AA34, 4AB02, 4AB06, 4AC07 | ||
| Alcohol-related illness1 | F10, G62.1, G72.1, I42.6, K29.2, K70.0–K70.4, K70.9, K86.0, O35.4, P04.3, Q86.0 | P15–P16 | |
| Other diagnosis related to psychoactive substance use1 | F11–F19 | P18–P19 | |
| Serious mental disorder1 | F20–29, F30–31, F32.3, F33.3 | P72–P73, P98 | |
| Other mental disorder1 | F32 (except F32.3), F33 (except F33.3), F34–F39, F40–F48 | P01–P06, P74–85 | |
1All available historic data for the period 2008–19 in the Norwegian Patient Registry (ICD10 codes) and July 2016–March 2020 in the Norwegian Registry for Primary Health Care (ICPC2 codes) as far back in time as possible.
2Last five years.
3Last seven years.
4Biological drugs administered in hospital, identified from procedure codes in the Norwegian Patient Registry (used e.g. for multiple sclerosis, rheumatological diseases, ulcerative colitis, Crohn's disease, psoriasis and spondylitis).
Table 2
Definitions of diseases and conditions and proportion in the population aged 20 years and older, among those who tested positive for COVID-19 and among those hospitalised for COVID-19. Number and proportion in per cent. For the COVID-19 groups, the proportions are age-adjusted and shown with a 95 % confidence interval.
| Disease/condition | Population | COVID-19 test positives | COVID-19 hospitalised | |
|---|---|---|---|---|
| Diabetes1 | 242 592 (5.9) | 468 (6.3 [5.8–6.9]) | 157 (9.4 [8.0–11.0]) | |
| Type 1 diabetes1 | 30 007 (0.7) | 44 (0.6 [0.4–0.8]) | 7 (0,6 [0,3–1,3]) | |
| Type 2 diabetes1 | 212 585 (5.2) | 424 (5.7 [5.2–6.3]) | 150 (8,6 [7,3–10,1]) | |
| Asthma1 | 225 169 (5.5) | 515 (6.8 [6.3–7.5]) | 127 (11.5 [9.7–13.7]) | |
| Chronic obstructive pulmonary disease (COPD) from 40 years1 | 111 493 (2.7) | 161 (2.3 [2.0–2.7]) | 67 (3.8 [3.0–4.8]) | |
| Other chronic pulmonary disease1 | 13 554 (0.3) | 34 (0.5 [0.3–0.7]) | 13 (0.8 [0.5–1.4]) | |
| Cancer2 | 224 018 (5.4) | 421 (5.8 [5.2–6.3]) | 127 (6.9 [5.8–8.3]) | |
| treated during the last 6 months | 23 277 (0.6) | 40 (0.6 [0.4–0.8]) | 16 (1,0 [0,6–1,6]) | |
| treated during the last 3 months | 10 599 (0.3) | 20 (0.3 [0.2–0.4]) | 11 (0,7 [0,4–1,3]) | |
| Cardiovascular disease3 | 644 443 (15.6) | 1 233 (16.4 [15.5–17.4]) | 333 (18.3 [16.4–20.3]) | |
| Stroke3 | 94 766 (2.3) | 190 (2.5 [2.2–2.9]) | 49 (2,4 [1,8–3,2]) | |
| Ischaemic heart disease3 | 159 355 (3.9) | 278 (3.7 [3.3–4.2]) | 94 (4,5 [3,7–5,5]) | |
| Atrial fibrillation3 | 132 491 (3.2) | 270 (3.5 [3.1–3.9]) | 91 (3,9 [3,2–4,8]) | |
| Cardiac failure3 | 63 552 (1.5) | 136 (1.7 [1.4–2.0]) | 60 (2,6 [2,0–3,3]) | |
| Hypertension2 | 578 867 (14.1) | 977 (13.4 [12.5–14.2]) | 251 (14,4 [12,7–16,3]) | |
| Complications of hypertension2 | 43 419 (1.1) | 88 (1.2 [1.0–1.5]) | 32 (1,6 [1,2–2,3]) | |
| Obesity2 | 68 047 (1.7) | 120 (1.5 [1.3–1.8]) | 26 (2.8 [1.9–4.2]) | |
| Overweight2 | 56 781 (1.4) | 105 (1.3 [1.1–1.6]) | 24 (2.6 [1.8–3.9]) | |
| Hypercholesterolaemia2 | 28 756 (0.7) | 64 (0.9 [0.7–1.1]) | 11 (0.7 [0.4–1.3]) | |
| Dementia1 | 15 190 (0.4) | 107 (1.3 [1.1–1.6]) | 9 (0.4 [0.2–0.7]) | |
| Hip fracture1 | 7 659 (0.2) | 19 (0.2 [0.1–0.4]) | 6 (0.2 [0.1–0.6]) | |
| Renal failure1 | 23 196 (0.6) | 67 (0.9 [0.7–1.1]) | 37 (1.7 [1.3–2.4]) | |
| Gastric ulcer and diseases of the biliary tract 2 | 41 846 (1.0) | 88 (1.1 [0.9–1.4]) | 21 (1.5 [1.0–2.4]) | |
| Neurological disorders1 | 73 178 (1.8) | 197 (2.6 [2.3–3.0]) | 42 (3.0 [2.2–4.0]) | |
| Cerebral palsy1 | 10 204 (0.2) | 13 (0.2 [0.1–0.3]) | 5 (0.5 [0.2–1.1]) | |
| Transplantation1 | 6 921 (0.2) | 22 (0.3 [0.2–0.4]) | 12 (0.9 [0.5–1.6]) | |
| Immunological failure1 | 3 054 (0.1) | 17 (0.2 [0.1–0.4]) | 8 (0.7 [0.4–1.5]) | |
| Rheumatological diseases1 | 86 720 (2.1) | 157 (2.1 [1.8–2.5]) | 35 (2.5 [1.8–3.5]) | |
| Inflammatory bowel disease1 | 56 206 (1.4) | 95 (1.3 [1.0–1.5]) | 22 (2.0 [1.3–3.0]) | |
| Biological drugs4 | 17 849 (0.4) | 24 (0.3 [0.2–0.5]) | 6 (0.6 [0.3–1.4]) | |
| Alcohol-related illness1 | 71 592 (1.7) | 79 (1.0 [0.8–1.3]) | 11 (1.0 [0.6–1.9]) | |
| Other diagnosis related to psychoactive substance use1 | 69 574 (1.7) | 72 (0.9 [0.8–1.2]) | 15 (2.0 [1.2–3.4]) | |
| Serious mental disorder1 | 79 363 (1.9) | 91 (1.2 [1.0–1.4]) | 17 (1.8 [1.1–2.9]) | |
| Other mental disorder1 | 1 070 244 (26.0) | 1 827 (23.6 [22.5–24.7]) | 259 (27.0 [23.9–30.5]) | |
1All available historic data for the period 2008–19 in the Norwegian Patient Registry (ICD10 codes) and July 2016–March 2020 in the Norwegian Registry for Primary Health Care (ICPC2 codes) as far back in time as possible.
2Last five years.
3Last seven years.
4Biological drugs administered in hospital, identified from procedure codes in the Norwegian Patient Registry (used e.g. for multiple sclerosis, rheumatological diseases, ulcerative colitis, Crohn's disease, psoriasis and spondylitis).
To define diseases we used data from the Norwegian Patient Registry for the period 2008–19 (ICD-10 codes; principal and secondary diagnoses) and from the Norwegian Registry for Primary Health Care (ICPC-2 codes) for the period July 2016–March 2020 (Table 1). For all persons registered with at least one contact with one or more of these conditions as a principal or secondary diagnosis and who had not died or emigrated as of 1 March 2020, dummy variables (yes/no) were created for each of these conditions.
The information on hospitalisations for COVID-19 is based on data on completed hospital care episodes that are reported monthly to the Norwegian Patient Registry (the period January–April 2020). The periods vary somewhat, because of the national procedures for reporting hospitalisations to the Norwegian Patient Registry and the availability of data in the project. We defined hospitalisation for COVID-19 as a positive test for COVID-19 and a hospitalisation with the diagnostic code U07.1 (COVID-19, virus identified), B34.2 (coronavirus infection, unspecified) or B97.2 (coronavirus as cause of diseases classified elsewhere).
Statistical analyses
The analyses included all persons aged 20 or older in the total population, among all those who have tested positive for COVID-19 and among all those who have been hospitalised for COVID-19.
The proportion of persons who have been registered with each condition in the three populations is reported in percentages. We present results for all conditions for men and women combined and in 20-year age groups (20–39 years, 40–59 years, 60–79 years and 80 years and older). For the largest groups of diseases (cardiovascular diseases, cancer, type 2 diabetes and COPD) we also present results for men and women separately and in 20-year age groups among persons aged 40 years and older, because the proportion with these diseases is low in the age group 20–39 years.
The proportion with each condition among those who had tested positive or had been hospitalised for COVID-19 is adjusted for sex and age and presented with a 95 % confidence interval. The age adjustment was made with the aid of the ageadjust.indirect function in the R package Epitools, with the population divided into five-year age groups as reference (6). This function also estimates the confidence interval.
Results
The population aged 20 years and older encompassed 4 118 831 persons, of whom 65 % were 40 years or older. Furthermore, 8 125 persons were registered as having tested positive for COVID-19 in the period 1 March–13 May 2020 according to the Norwegian Surveillance System for Communicable Diseases. Of these, 7 632 (94 %) were 20 years or older, and 5 046 (66 %) were 40 years or older. In the period from January through April 2020, altogether 1 025 (13.4 %) of those who were registered as having tested positive for COVID-19 and aged 20 years and older had been hospitalised for COVID-19, and of these, 905 (88 %) were 40 years or older. They had been hospitalised for eight days on average, the median hospitalisation time was six days, and the longest hospitalisation time was 50 days.
Among all those hospitalised, a total of 333 (18.3 %) were registered with a cardiovascular disease, 127 (6.9 %) with cancer, 150 (8.6 %) with type 2 diabetes and 67 (3.8 %) with COPD (these percentages are adjusted for sex and age). The proportions were higher than in the population as a whole (Table 2).
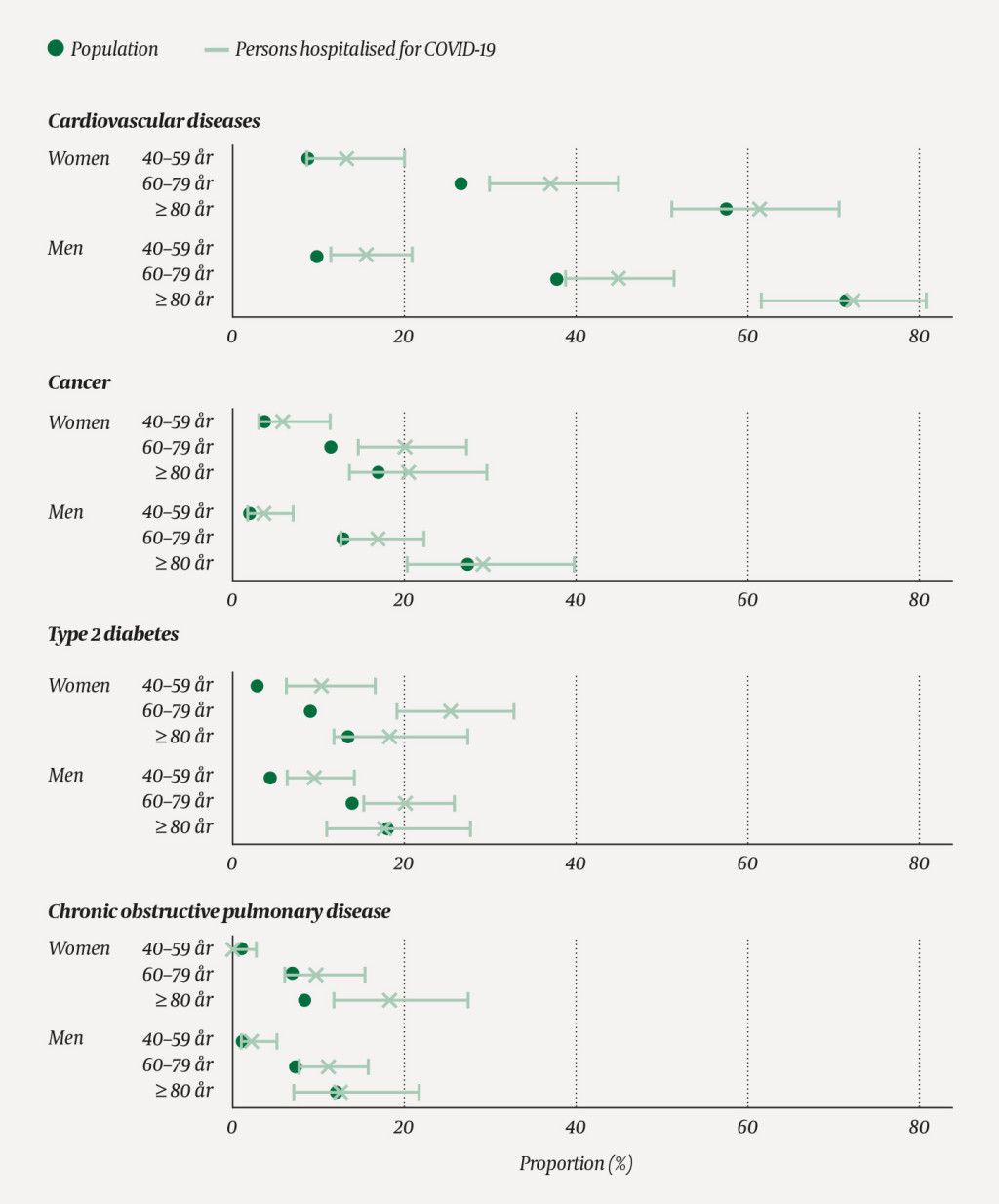
When looking in detail at the largest disease groups distributed by sex and age among those aged 40 years and older, we observed that the proportion of patients hospitalised for cardiovascular diseases, cancer, type 2 diabetes and COPD increased with age (Figure 1). The same tendency can be seen in the general population (Figure 1) and in the group who tested positive for COVID-19 (data not shown). Among those hospitalised for COVID-19, several age groups had a higher proportion of these four diseases than the population as a whole, among women and men alike (Figure 1). However, the figures are small with wide confidence intervals. The proportion of individuals hospitalised with one of these diseases in the age group 40 years and older was 31.3 %, while the proportion with two was 16.9 %, with three 2.8 % and four 0.4 % (not adjusted for age). There were only minor differences between women and men, and the proportion of patients hospitalised with multiple diseases increased with age (data not shown).
The proportion with underlying diseases and conditions, for both sexes combined in the age group 20 years and older, shows that individuals hospitalised with COVID-19 are distributed over a number of conditions (Table 2). That is also the case for the total group of individuals with a positive test (COVID-19 test positives). Among those hospitalised, there are a larger proportion of individuals with active cancer treatment in the last six and three month, asthma, other chronic pulmonary disease, cardiovascular diseases, cardiac failure, complications of hypertension, obesity, overweight, renal failure and neurological disorders than in the general population as a whole (Table 2).
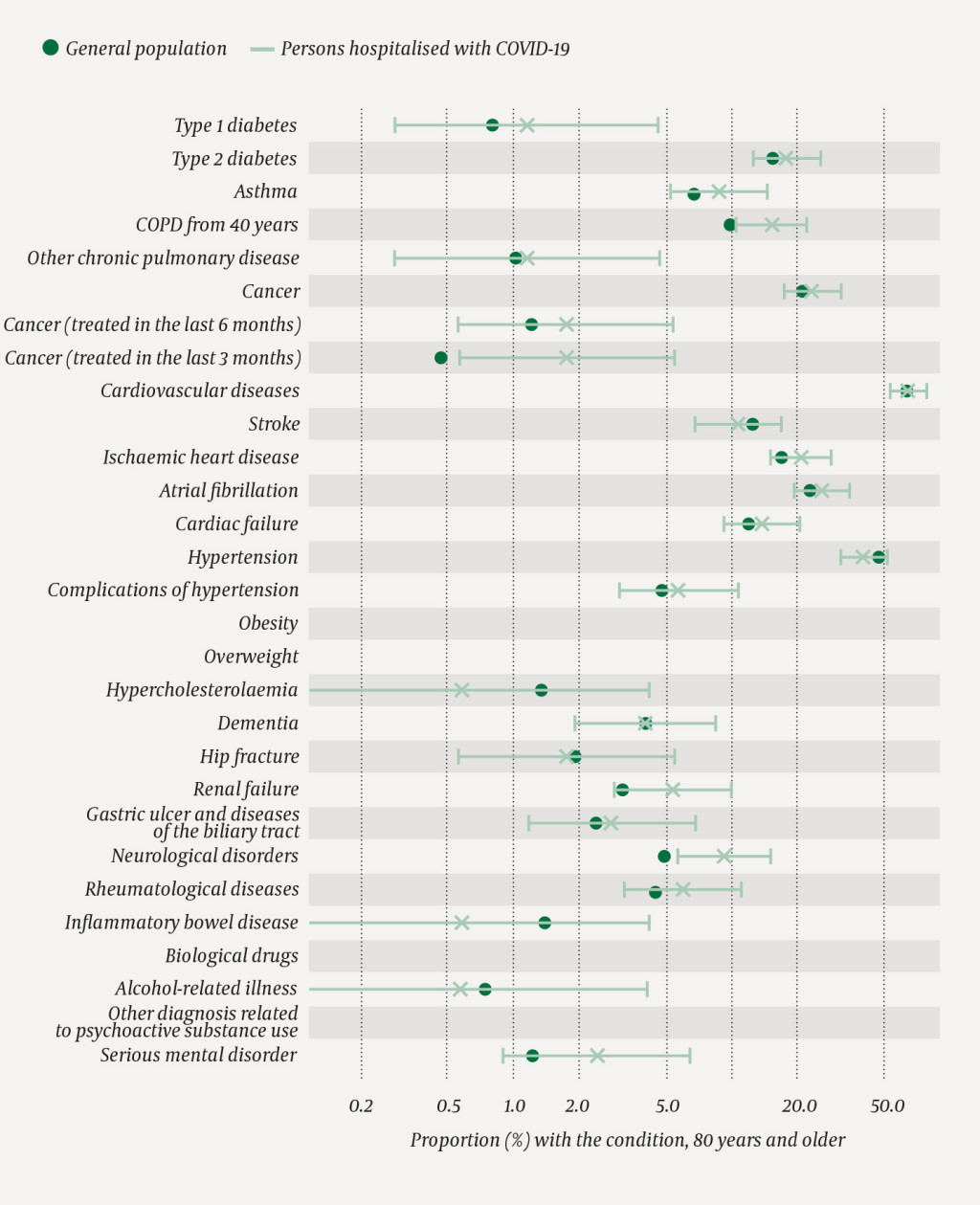
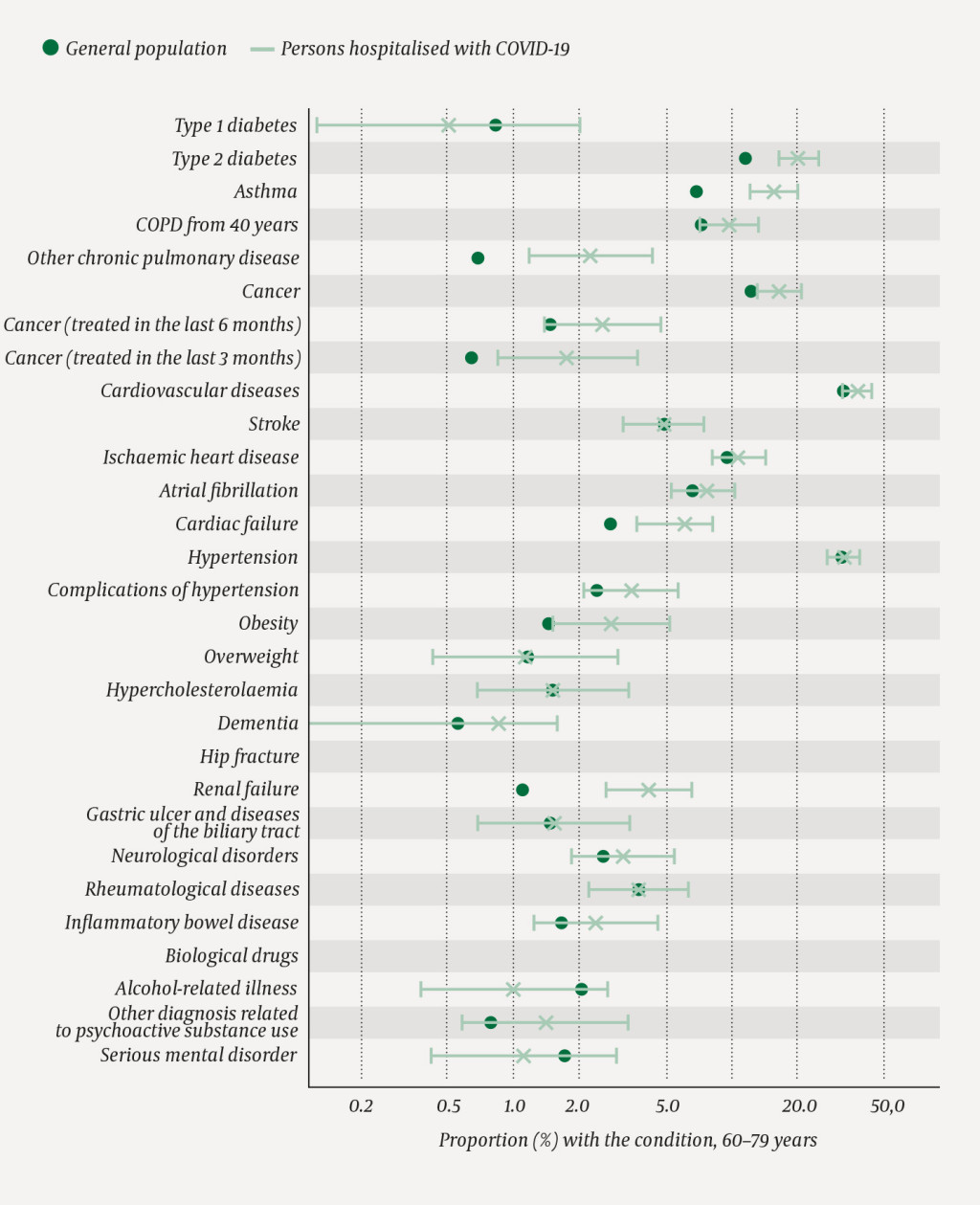
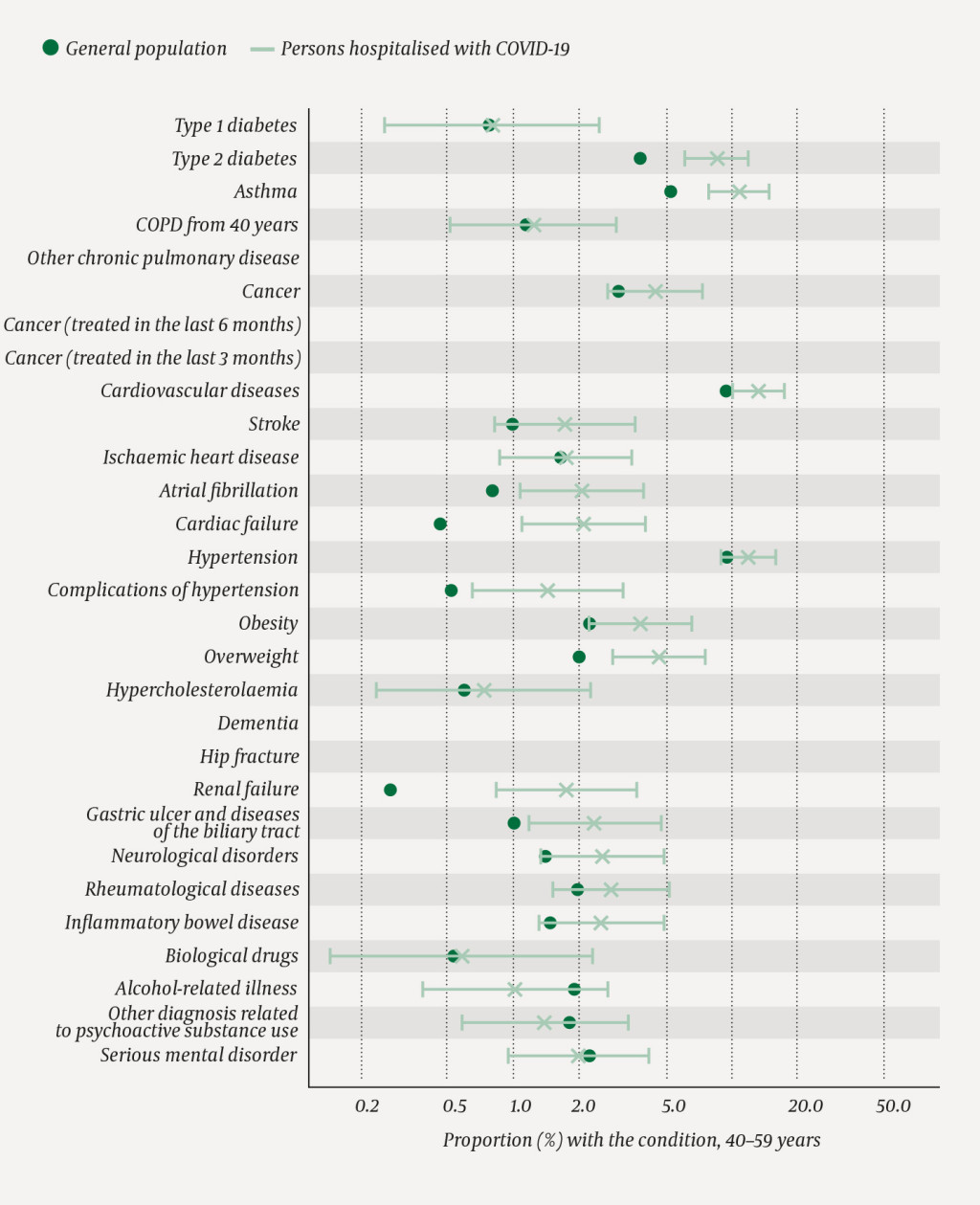
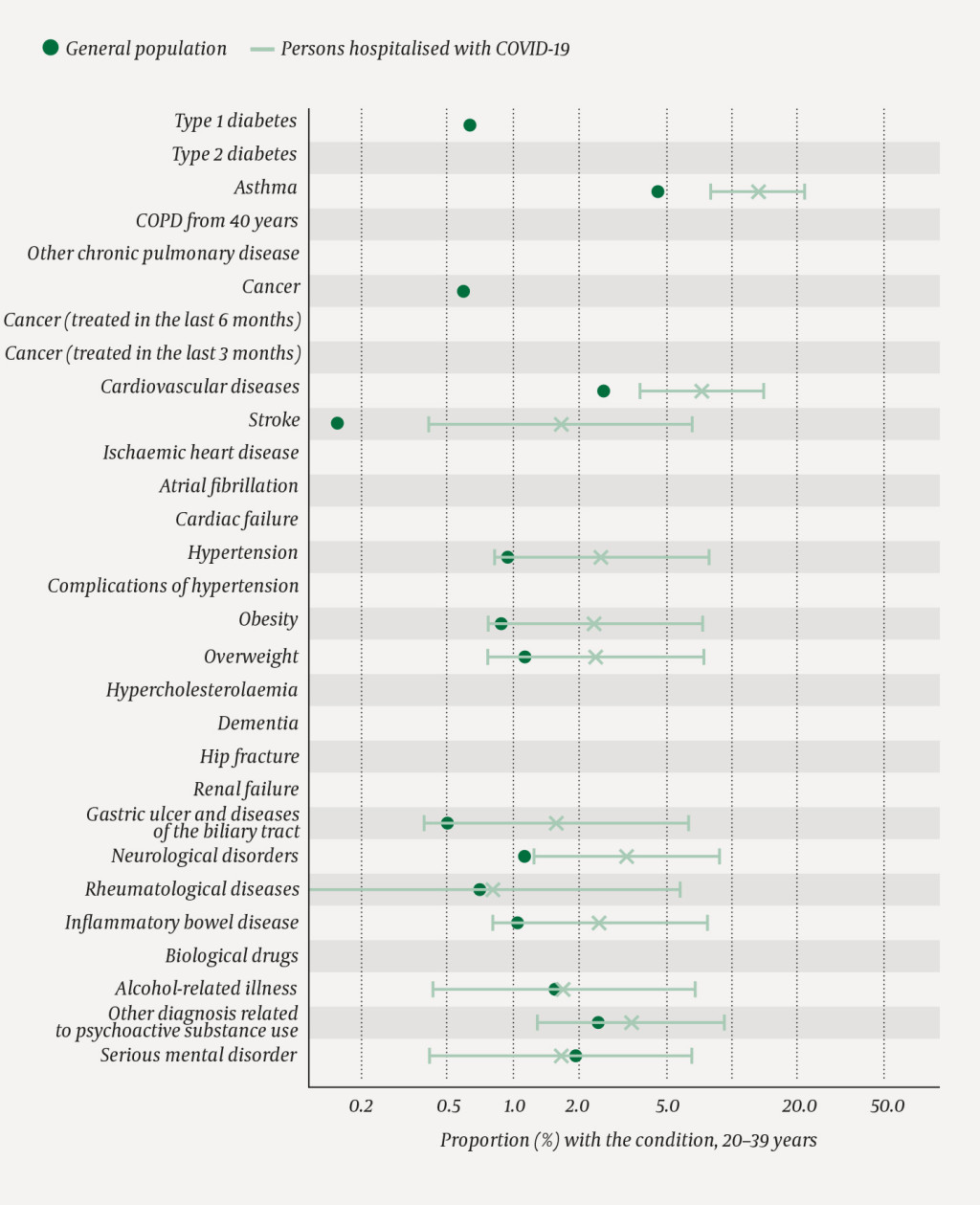
The distribution by age groups among those hospitalised for COVID-19 is shown in Figures 2–5. Among the oldest patients, there are more people with cancer in active treatment in the last three months than in the general population as a whole (Figure 2). In this age group, the proportion with dementia who tested positive to COVID-19 is higher than in the general population (data not shown), but not among the group of hospitalised patients (Figure 2). Moreover, we can see that the proportion with type 1 diabetes, asthma, other pulmonary diseases, cancer, cardiac failure, obesity and renal failure is higher than in the general population in the age group 60–79 years (Figure 3). In the age group 40–59 years, the proportion with type 2 diabetes, asthma, atrial fibrillation, cardiac and renal failure, complications of hypertension, overweight, gastric ulcer and diseases of the biliary tract is higher than in the general population (Figure 4), while the proportion with asthma, cardiovascular diseases, stroke and neurological disorders is higher in the age group 20–39 years than in the general population (Figure 5). It should be noted that the figures are small, and this is reflected in their confidence intervals.
Discussion
Among hospitalised adults registered with COVID-19 there was a higher proportion of patients with various underlying conditions than in the population as a whole. The clinical picture changes with age. We found a tendency towards a higher proportion registered with non-communicable diseases such as cardiovascular diseases, cancer, type 2 diabetes and COPD than in the general population in many age groups, among both women and men. There was little difference in the prevalence of registered conditions between persons who had tested positive for COVID-19 and the general population.
Currently there is little research evidence as to whether persons with specific underlying diseases and conditions are at a higher risk of a serious course of COVID-19 (7). In most previous studies, the analyses are based on population groups where there might be a selection to be tested for SARS-CoV-2 and to be hospitalised with COVID-19 (8, 9). This might influence the results (7, 10).
Advanced age alone, or the presence of multiple diseases, is associated with a severe course of COVID-19 (7). However, it is difficult to determine whether the increased risk of developing severe disease after COVID-19 is due to the presence of multiple diseases or whether it is a reflection of the fact that older persons with these diseases are often hospitalised as a precautionary measure.
It is difficult to distinguish between these factors in our project as well. Being hospitalised for COVID-19 may in itself be an expression of the disease severity. We did, however, observe that even though the length of the hospitalisation period may reflect the severity of the COVID-19 infection, some patients also died during or shortly after a short stay in hospital. It will thus be difficult to rate the illness severity among hospitalised patients exclusively based on the length of their stay or use of intensive care.
Analyses of individual diseases have pointed out that cardiovascular diseases, cancer, diabetes and COPD are overrepresented among persons who developed severe disease after COVID-19, although the findings are not entirely unambiguous across the studies (4). For example, in a study by Petrilli et al., chronic pulmonary diseases are not overrepresented among hospitalised patients (11). For other diseases, such as diabetes, the findings are more consistent across studies and well as with our own findings. A Danish non-peer reviewed study by Riley et al. shows that the proportion with diabetes is higher among adults with a serious course of COVID-19 (10). We have little knowledge of how the diseases are distributed by age and sex among hospitalised patients when compared to the general population. Our data therefore have value despite the small and non-random nature of the data material, which needs to be interpreted with caution.
The proportion of hospitalised persons with multiple diseases such as cardiovascular diseases, cancer, type 2 diabetes and COPD increases with age and can explain part of the difference between age groups. It is interesting to note that among the oldest – 80 years and older – we find that compared to the general population, a higher proportion of those who tested positive to COVID-19 are registered with dementia, while the proportion with dementia among patients hospitalised with COVID-19 is not higher than in the general population. This may partly be due to the Norwegian testing procedures, whereby people who are at higher risk, including elderly nursing home residents with dementia, may have been tested more frequently, but perhaps not hospitalised to the same extent.
The strength of this registry study lies in its inclusion of the entire Norwegian population aged 20 years and older. This means that we have shown how the proportion of the population with the large disease groups of cardiovascular diseases, cancer, type 2 diabetes and COPD are distributed by sex and age among persons who have tested positive or been hospitalised for COVID-19. This is important when assessing the potential effects of pandemics that can affect persons in these large disease groups. We included separate analyses for cancer patients who were undergoing active treatment, since we can assume that they will be more vulnerable than other cancer patients. The proportion of patients undergoing treatment for cancer was also higher among those hospitalised for COVID-19 than in the general population.
A registry study will include non-validated data. Here, this does not apply to the definition of the patient group, since one of the strengths of our study is the high degree of correspondence between the Norwegian Surveillance System for Communicable Diseases and the coding in the Norwegian Patient Registry for hospitalised patients. As regards all the listed diseases, on the other hand, non-validated data will be included. Validation of data from the Norwegian Patient Registry may, for example, show that 'suspicion of a disease' has been coded as 'the disease'. Furthermore, we have insufficient knowledge about the quality of the Norwegian Registry for Primary Health Care, since it was established relatively recently. Overestimation of disease prevalence is generally likely in registry studies without validation, and this is a weakness. Unfortunately, the project had no data on multimorbidity for all the diseases. This means that an individual can be affected by more than one disease, in the same way as the general population with which the hospitalised patients are compared.
Follow-up times vary between the different registries. The Norwegian Patient Registry contains information on completed hospital care episodes, and consequently we have no data on those who were hospitalised in late April/early May. Access to data on currently hospitalised patients could have further strengthened the study. This group is likely to have encompassed a proportion with long hospitalisation periods and a more serious disease course may assume, however, that this weakness of the study will have little effect on the results, since this group is small. The regulations stipulate that the code for COVID-19 infection should not be used as a main diagnosis. In the hospital data, it is thus impossible to distinguish between patients who have been admitted for COVID-19 and patients who have been diagnosed with COVID-19 during hospitalisation for other conditions.
Because of the Norwegian testing strategies in the spring of 2020, the likelihood of being tested was higher for a person with an underlying disease than for an otherwise healthy person with the same symptoms. If many people have had COVID-19 without being tested, this could weaken the findings in our study. The majority of these would then most likely be in the group of 'otherwise healthy' persons, and we would have expected an overrepresentation of chronically ill patients among those who had tested positive. This seems however not to be the case.
With access to data about those who tested negative for COVID-19 we could have estimated the degree of selection caused by the testing strategies. Many of those who were first confirmed to have COVID-19 were fit and healthy ski tourists, and this may also have served to reduce the proportion of chronically ill persons among those who tested positive. A person with an underlying disease will also tend to be hospitalised with milder symptoms than an otherwise healthy person. We know that during the influenza pandemic caused by the A(H1 N1) virus in 2009–2010, the likelihood of hospitalisation was higher among persons with type 2 diabetes than among the general population, while the disease severity and complications was not any higher (12). The weaknesses of observation studies that use non-random material, as in parts of this study, and how this affects the results have been described in a number of recently published articles (8, 9, 13).
The objective of this study was to describe how different diseases were distributed among persons with confirmed COVID-19 and among patients hospitalised for COVID-19 when compared to equivalent figures for the general population. The main purpose has been to contribute to monitoring and emergency preparedness. Having such an overview is important in order to follow the development in Norway further. Linking registry data with personal data that include all persons tested for COVID-19 and where the group that tested positive to COVID-19 is not selected, could have helped answer questions about the risk of being infected with or hospitalised for COVID-19, and thus provided more evidence about the underlying causes of the development of severe disease.
The article has been peer reviewed.
- 1.
Emami A, Javanmardi F, Pirbonyeh N et al. Prevalence of underlying diseases in hospitalized patients with COVID-19: A systematic review and meta-analysis. Arch Acad Emerg Med 2020; 8: e35. [PubMed]
- 2.
Folkehelseinstituttet. Råd og informasjon til risikogrupper og pårørende. https://www.fhi.no/nettpub/coronavirus/fakta/risikogrupper/ Accessed 5.6.2020.
- 3.
The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team. The epidemiological characteristics of an outbreak of 2019 novel coronavirus diseases (COVID-19) — China, 2020. China CDC Weekly 2020; 2: 113–22. [CrossRef]
- 4.
Brurberg K. COVID-19: The relationship between age, comorbidity and disease severity – a rapid review, 1st update. Oslo: Folkehelseinstituttet, 2020. https://www.fhi.no/globalassets/dokumenterfiler/rapporter/2020/covid-19-the-relationship-betweenage-comorbidity-and-disease-severity-1st-update-report-2020-v2-.pdf Accessed 1.9.2020.
- 5.
Bakken IJ, Ariansen AMS, Knudsen GP et al. The Norwegian Patient Registry and the Norwegian Registry for Primary Health Care: Research potential of two nationwide health-care registries. Scand J Public Health 2020; 48: 49–55. [PubMed][CrossRef]
- 6.
The R Project for Statistical Computing. https://www.R-project.org/ Accessed 1.9.2020.
- 7.
Flodgren G, Vestrheim D, Brurberg K. COVID-19 and risk factors for severe disease – a rapid review, 2nd update. Oslo: Folkehelseinstituttet, 2020. https://www.fhi.no/en/publ/2020/COVID19-and-risk-factors-for-severe-disease-2nd-update/ Accessed 28.5.2020.
- 8.
Griffith G, Morris TT, Tudball M et al. Collider bias undermines out understanding of COVID-19 disease risk and undermines our understandingo f COVID-19 disease risk and severity medRxiv 2020.
- 9.
Westreich D, van Smeden M, Edwards J. Response to Goldacre et al. (OpenSAFELY Collaborative). https://zenodo.org/record/3855586#.X1CtQXkzaJM Accessed 1.9.2020.
- 10.
Reilev M, Kristensen KB, Pottegaard A et al. Characteristics and predictors of hospitalization and death in the first 9,519 cases with a positive RT-PCR test for SARS-CoV-2 in Denmark: A natiowide cohort. medRxiv 2020.
- 11.
Petrilli CM, Jones SA, Yang J et al. Factors associated with hospital admission and critical illness among 5279 people with coronavirus disease 2019 in New York City: prospective cohort study. BMJ 2020; 369: m1966. [PubMed][CrossRef]
- 12.
Ruiz PLD, Bakken IJ, Håberg SE et al. Higher frequency of hospitalization but lower relative mortality for pandemic influenza in people with type 2 diabetes. J Intern Med 2020; 287: 78–86. [PubMed][CrossRef]
- 13.
Wynants L, Van Calster B, Collins GS et al. Prediction models for diagnosis and prognosis of covid-19 infection: systematic review and critical appraisal. BMJ 2020; 369: m1328. [PubMed][CrossRef]