Main findings
The period 1995–2019 saw an increase in the total number of patients and the proportion of patients referred from other health regions to Haukeland University Hospital for treatment of gynaecological fistulae.
Gynaecological fistulae after surgery most frequently affected the urinary tract, and the most common causes were hysterectomies and stress incontinence procedures.
Gynaecological fistulae after radiotherapy occurred most frequently after treatment for rectal or cervical cancer, and most often affected the bowel.
As a general rule, post-surgical fistulae were operable by means of vaginal fistuloplasty and the prognosis was very good (94 % healing), while post-radiotherapy fistulae healed more rarely (26 %) and patients were often left with a permanent urostomy or enterostomy (72 %).
Gynaecological fistulae with communication between genitalia (uterus, vagina or perineum) and urinary tract (urogenital fistula) or the bowel (enterogenital fistula) give rise to leakage of urine or of faeces/gas resulting in considerably reduced quality of life (1). At global level, fistulae as complications of childbirth (obstetric fistulae) predominate. These occur after up to 124/100 000 births in developing countries (2) and 16/100 000 in countries with good obstetric care (3). In industrialised countries, gynaecological fistulae have an annual incidence of 6/10 000 (4), mainly as a complication of pelvic surgery or radiotherapy (5).
Gynaecological fistulae are frequently described in organ-specific cohort studies, for example urogenital fistula treated in urological departments (6) or enterogenital fistula in gastrointestinal surgery departments (7). Studies from gynaecological departments have described obstetric fistulae (3), while few publications deal with gynaecological treatment of fistulae with other causes.
At the Department of Gynaecology and Obstetrics, Haukeland University Hospital, treatment of gynaecological fistulae has been systematically recorded and followed up since 1995 (8), and in 2012 the department was appointed the National Unit for Gynaecological Fistulae. The centre has previously reported on fistulae treated in the period 1995–2005, i.e. prior to it formally becoming the national service (8).
Abdominal and pelvic surgery have changed substantially over the past few decades, with an increasing proportion of laparoscopy (including robotic surgery) replacing laparotomy (9, 10) and the use of vaginal mesh and slings for urinary incontinence and genital prolapse (11, 12), which may influence the risk and pattern of fistula development. Radiotherapy continues to be a relevant form of treatment, particularly for anorectal and cervical cancer (13).
In Norway, more than 1 600 women (0.6 ‰ of the female population) have been hospitalised three or more times with a fistula diagnosis, according to the Norwegian Patient Register (NPR) (4). Data from this register reflect the number of women who receive surgical treatment for gynaecological fistulae, but cannot provide information about the cause or outcome of treatment. In the present study, we wish to describe clinical characteristics of and treatment outcomes for gynaecological fistulae due to surgery or radiotherapy by reviewing a 25-year cohort from a department which has been a national treatment unit since 2012.
Material and method
This study covered a hospital cohort of women who were treated at the Department of Gynaecology and Obstetrics, Haukeland University Hospital, in the period 1995–2019 for gynaecological fistula due to radiotherapy and/or surgery. Data were extracted from patient records, and from 2014 onwards from the Register of Gynaecological Fistulae (Norwegian Data Inspectorate approval 14/00215–2/CGN). All women have given broad, written consent to inclusion in the register. The study has been approved by the Regional Committee for Medical and Health Research Ethics (REK 2015/326). The committee granted exemption from the obtaining of consent from women who were already dead prior to the start of the study. Some of the material (1995–2005) has been discussed earlier (8) and has been included to show developments over a long period.
Fistulae were classified as urogenital (from the ureter, bladder or urethra to the uterus or vagina) or enterogenital (from the bowel to uterus, vagina or perineum). Fistulae that affected both the urinary tract and the bowel were classified separately. If the woman had received radiotherapy, the fistula was classified as radiation-induced, irrespective of whether there had been previous or concomitant surgery.
The level of a fistula was defined as the distance from hymenal level to the aperture of the fistula in the uterus, vagina or perineum, and the size given as the largest cross-sectional diameter of the fistula.
Diagnostic and surgical procedures
Gynaecological examination under general anaesthesia was supplemented with cystoscopy for urogenital fistulae and direct probing or methylene blue solution or gel via the rectum for enterogenital fistulae. Diagnostic imaging (urography/magnetic tomography with contrast enhancement) was used for supplementary tests in cases of uncertain findings or suspected affection of the ureter or bowel segment above the rectum.
A catheter with drainage based on the siphon principle (urogenital fistulae) or temporary enterostomy (enterogenital fistulae) was used as primary treatment if the injury was detected less than 21 days after its presumed occurrence.
The department's current standard treatment is vaginal fistuloplasty. An excision is made from the vaginal side with layerwise closure of bladder/bowel wall, vesicovaginal/rectovaginal space and vaginal mucosa/perineal skin. Fistulae from the ureter or a higher bowel segment than the rectum are most often operated upon via abdominal access in collaboration with a urologist or gastrosurgeon.
In the case of a urogenital fistula, the woman had catheter drainage until post-operative follow-up after 14 days, while enterogenital fistulae were followed up 2–3 months after the initial treatment. For post-radiotherapy fistulae, an enterostomy was always established before any fistula surgery, and was then reversed if the follow-up consultation confirmed healing (14). The women were followed up with consultations until it was confirmed that the fistula was closed or it was concluded that there was no further fistula treatment to offer.
Statistical analysis
All individual data were anonymised prior to registration. Statistical analyses were performed using SPSS version 21 (IBM Corporation, Armonk, NY, USA). Continuous data were not normally distributed, and are presented as medians. Dispersion is reported as interquartile range (IQR) and compared by means of a non-parametric test (the Mann-Whitney U test). Categorical variables were compared by means of Pearson's chi-squared test or Fisher's exact test if assumed to be < 5 in individual cells. Statistical significance was reported as a two-tailed p-value < 0.05.
Results
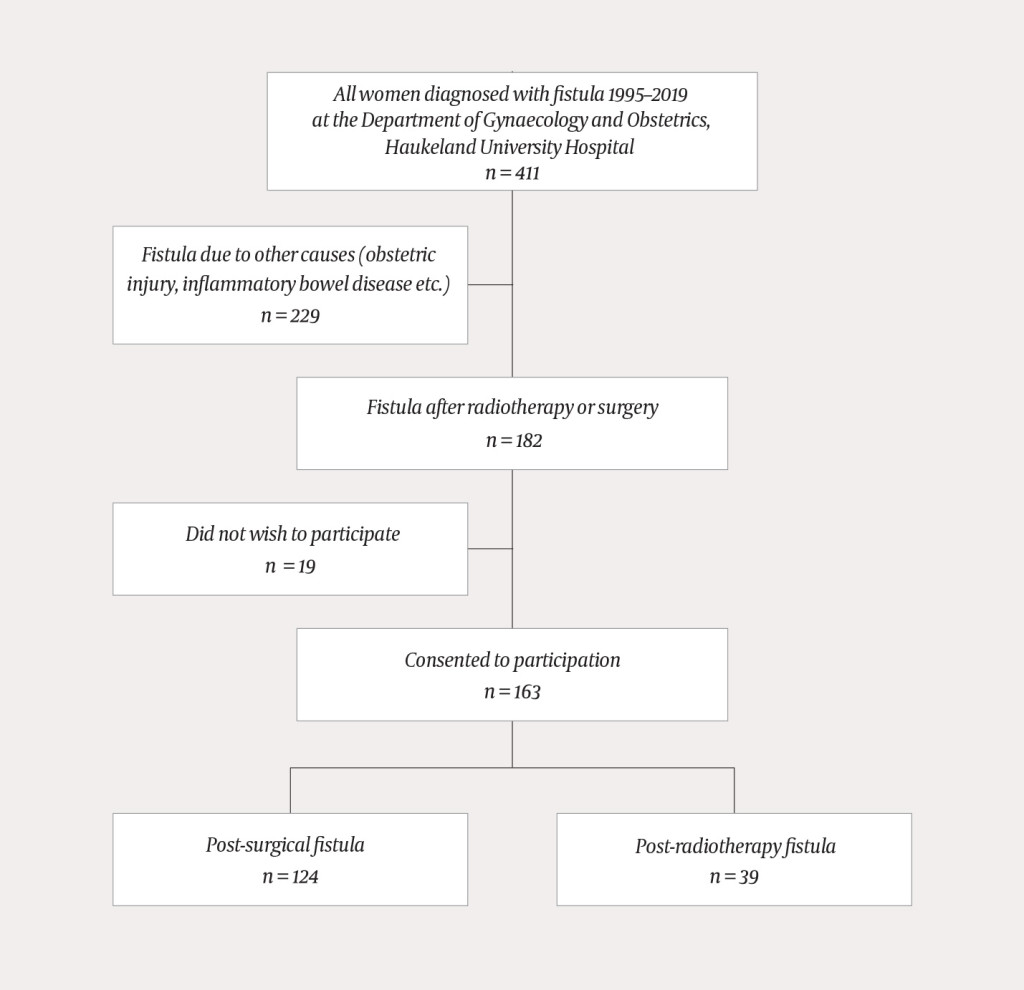
Of a total of 411 women diagnosed with gynaecological fistulae in the period 1995–2019, 182 had a fistula caused by radiotherapy or surgery. Altogether163/182 (90 %) of them consented to take part in the study (Figure 1). A total of 80/163 women (49 %) had undergone treatment for cancer. In all, 94 women had urogenital fistula, 62 enterogenital fistula and 7 had fistula involving both urinary tract and bowel.
Developments over time
The number of women treated in the department increased in each five-year period in the course of the 25 years surveyed (Table 1). The percentage referred from health regions other than those under the Western Norway Regional Health Authority increased significantly, from 1/12 patients (8 %) in the period 1995–1999 to 89/154 (58 %) in the period 2015–2019. This percentage was largest for women with fistula attributable to surgery. A total of 35/46 (76 %) of the patients with post-surgical fistulae were referred from other regions in the last five-year period.
Table 1
Women diagnosed with gynaecological fistula (n = 411) in the period 1995–2019 at the Department of Gynaecology and Obstetrics, Haukeland University Hospital (from 2012: Norwegian National Unit for Gynaecological Fistulae). The percentage of women per five-year period who came within the Western Norway Regional Health Authority is compared with women referred from other regions.
| Health region, n (%) |
1995–99 |
2000–04 |
2005–09 |
2010–14 |
2015–19 |
P-value1 |
|---|---|---|---|---|---|---|
| Western Norway Regional Health Authority |
11 (92) |
46 (90) |
68 (75) |
70 (68) |
65 (42) |
< 0.001 |
| Other regions |
1 (8) |
5 (10) |
23 (25) |
33 (32) |
89 (58) |
1Chi-squared test
Post-surgical fistula
Surgery was the cause of fistula in 124/163 women (76 %) (Table 2). Post-surgical fistulae were urogenital in 91/124 (73 %) and caused by hysterectomy in 71/124 (57 %) (of which 6 vaginal and 12 laparoscopic), or by urinary incontinence procedures employing tension-free vaginal tape (TVT) in 11/124 (9 %). In 24/33 (72 %) of women with enterogenital fistula, the cause was a procedure involving the bowel. Of the women with post-surgical fistula, 41/124 (33 %) had undergone surgery owing to cancer, with colorectal cancer accounting for 20 patients. Women with post-surgical fistula were significantly younger than women with post-radiotherapy fistula, and developed symptoms after a significantly shorter interval than those with post-radiotherapy fistula (Table 2).
Table 2
Clinical characteristics of 163 women with gynaecological fistulae after surgery or radiotherapy treated at the Department of Gynaecology and Obstetrics, Haukeland University Hospital, in the period 1995–2019. All values are medians (interquartile range).
| Variable |
Post-surgical fistula n = 124 |
Post-radiotherapy fistula n = 39 |
P-value1 |
|---|---|---|---|
| Age at the time of diagnosis (years) |
52.5 (17) |
60.0 (23) |
0.017 |
| Time from injury to symptom (weeks) |
1 (4) |
39 (206) |
< 0.001 |
| Time from symptom to diagnosis (weeks) |
17 (57) |
14 (21) |
0.470 |
| Fistula level (mm above hymen level) |
85 (30) |
60 (40) |
0.002 |
| Max. fistula diameter (mm) |
3 (3) |
10 (16) |
< 0.001 |
1Mann-Whitney test
Post-radiotherapy fistula
Of 39 women with post-radiotherapy fistula, 29 had also had surgery for cancer. Post-radiotherapy fistulae were enterogenital in 34/39 (87 %).
Rectal cancer (22/39: 56 %) and cervical cancer (11/39: 28 %) were the most frequently occurring forms of cancer. In all 5/39 (13 %) had fistulae that involved both bowel and urinary tract. Post-radiotherapy fistulae had a significantly larger median diameter and were located significantly lower in the vagina than post-surgical fistulae (Table 2).
Results of fistula treatment
Vaginal fistuloplasty was performed on 107/163 (66 %) of the women. This resulted in healing in 96/100 (96 %) of patients with post-surgical fistula, compared with 4/7 (57 %) with post-radiotherapy fistula. An abdominal procedure was performed on 16/163 (9 %) of all patients, in the form of reimplantation of the ureter in eight cases of ureterovaginal fistula. Catheter drainage or a temporary stomy without further fistula treatment resulted in healing in a total of 14/163 (9 %), ten of them with post-surgical fistula. The median follow-up time for post-surgical fistula was eight weeks, compared with 39 weeks for post-radiotherapy fistula. Table 3 shows differences in the type of treatment and outcome between the two patient groups. There was a substantially higher healing rate for post-surgical fistula, 117/124 (94 %), compared with 10/39 (26 %) for post-radiotherapy fistula.
Table 3
Gynaecological fistula after surgery or radiotherapy (n = 163) treated in the period 1995–2019 at the Department of Gynaecology and Obstetrics, Haukeland University Hospital. Choice of treatment and outcomes are compared. Median fistula follow-up time (interquartile range) was 8 (18) weeks after surgery and 39 (102) weeks after radiotherapy. All values are numbers (percentages).
| Post-surgical fistula n = 124 |
Post-radiotherapy fistula n = 39 |
P-value |
||
|---|---|---|---|---|
| Treatment category |
<0.0011 |
|||
| Vaginal fistuloplasty |
100 (80) |
7 (18) |
||
| Abdominal fistula surgery |
12 (10) |
4 (10) |
||
| Catheter/pyelostomy/enterostomy2 |
12 (10) |
23 (59) |
||
| Other3/No treatment |
0 (0) |
5 (13) |
||
| Post-treatment outcome |
< 0.0014 |
|||
| Healed fistula |
117 (94) |
10 (26) |
||
| Persistent fistula |
7 (6) |
29 (74) |
||
| Permanent pyelostomy/enterostomy |
9 (7) |
28 (72) |
< 0.0014 |
|
1Fisher's exact test
2No other specific fistula surgery
3Includes any hyperbaric treatment
4Chi-squared test
Discussion
In this hospital cohort, large differences were found in characteristics of and the prognosis for gynaecological fistulae caused by surgery as opposed to radiotherapy. Post-radiotherapy fistulae caused later symptoms, were larger in diameter, more often enterogenital and healed more seldom (26 %). Conversely, post-surgical fistulae had a very good healing rate (94 %).
At Haukeland University Hospital, where a national treatment centre was established in 2012, there has been a steady increase in both the total number of patients with gynaecological fistulae and the percentage of patients referred from other health regions. A review of the Norwegian Patient Register 2008–2014 revealed that a significantly larger proportion of fistula procedures, 31 %, had been performed under the Western Norway Regional Health Authority compared with the rest of Norway (4). In the last five-year period (2015–2019) a full 76 % of women with post-surgical fistula had been referred from other health regions (the Western Norway Regional Health Authority covers 21 % of Norway's population). This indicates that the centre's services have become more widely known and are now used for the whole of the patient group in question.
In our dataset, hysterectomy was the cause of 57 % of the post-surgical fistulae, and was the predominant cause of urogenital fistula. This is consistent with a British cohort from a urology department, where hysterectomy had caused 159/238 (67 %) of urogenital fistulae (6). Hospital registry data from the UK indicate the risk of urinary tract injury in connection with hysterectomy at 1/788 (0.13 %), and higher for radical cancer surgery (15). The fact that as many as 41/124 (33 %) of our post-surgical fistulae occurred in connection with cancer treatment supports these findings.
An increasing incidence of urinary tract injuries has been described in connection with the transition to use of laparoscopic technique for hysterectomies (10). In Norway laparoscopy is now the main method used for hysterectomies for patients with benign conditions (9) and its use in cancer treatment is increasing. Our dataset with 6 vaginal and 12 laparoscopic interventions in a total of 71 hysterectomies is too small for a conclusion to be drawn about the risk associated with the different surgical approaches.
Tension-free vaginal tape is the most common procedure for stress incontinence (11). A total of 9 % of post-surgical fistulae in our dataset were caused by tension-free vaginal tape. In Norway, 9 286 procedures involving tension-free vaginal tape were performed in the period 2004–08 (16). Extrapolated to the end of 2019, this number would be 31 443. This is equivalent to 3.5 per 10 000 women who underwent procedures involving tension-free vaginal tape being treated for fistula at our centre in this period.
The time from injury to onset of symptoms was significantly shorter for post-surgical fistula: a median of 1 week compared with 39 weeks in the group with post-radiotherapy fistula. This reflects the fact that a surgical procedure often results in an immediate fistula, while radiotherapy induces tissue changes over time. In both groups, however, a relatively long period elapsed between symptom and diagnosis: 17 and 14 weeks, respectively. This underlines the fact that health personnel should be more aware of the risk of fistula development as a possible cause of new-onset urine or faecal leakage following a surgical procedure or radiotherapy in the pelvic region. In our cohort, 9 % of the women healed purely as a result of temporary relief with a catheter or enterostomy. This is consistent with earlier studies (17), which show that it is beneficial to insert a catheter with good siphonage as soon as a fistula is suspected. The patient will then be able to avoid a fistula procedure.
The healing rate of 94 % (117/124) for post-surgical fistula is very good and equal to the healing rate for obstetric fistula in Norway (93 %) (5). Vaginoplasty has long been the centre's primary method, and a healing rate of 97 % is good, also when compared with data from the UK, where 86 % healing was found with transvesical fistuloplasty at a urological department (6).
Post-radiotherapy fistulae healed in only 26 % of our dataset, and 72 % of them remained with a permanent urostomy or enterostomy. A British study of urogenital post-radiotherapy fistulae found 53 % healing (6), and an American study of post-radiotherapy bowel complications found that 63 % of those with enterogenital fistulae needed a permanent stomy (18). Women with post-radiotherapy fistula often had problematic symptoms of radiation damage other than urinary/faecal leakage as a consequence of a fistula, such as bladder pain, dysuria and diarrhoea (13). Hyperbaric oxygenation is often used in attempts to treat these patients. Few patients in our cohort received this treatment, and we cannot assess the extent to which this contributes to fistula healing.
Participation in a study by 90 % of a patient cohort is high, and must be regarded as representative for our treatment cohort. Although patients were registered consecutively at the centre, information regarding specific clinical details and therapeutic outcomes was added retrospectively. The study therefore has the general limitations associated with a retrospective cohort study.
The primary goal of the study was to demonstrate the outcome of the treatment. As in several other studies (19), the lack of patient-reported data on quality of life can be regarded as a weakness. We are therefore currently reviewing possible relevant measures of quality to include in the service's register, to make provision for this aspect in future patient therapy.
Conclusion
On the basis of our figures we can conclude that the National Unit for Gynaecological Fistulae is used increasingly by patients from all health regions, and that the treatment of gynaecological fistulae caused by surgery is successful and far better than for fistulae due to radiation. Post-radiotherapy fistulae will mainly be permanent. A systematic review of the results from a national treatment unit is important for making the service known and assuring equal provision of treatment.
The article has been peer-reviewed.
- 1.
Wilson SM, Sikkema KJ, Watt MH et al. Psychological symptoms among obstetric fistula patients compared to gynecology outpatients in Tanzania. Int J Behav Med 2015; 22: 605–13. [PubMed][CrossRef]
- 2.
Vangeenderhuysen C, Prual A, Ould el Joud D. Obstetric fistulae: incidence estimates for sub-Saharan Africa. Int J Gynaecol Obstet 2001; 73: 65–6. [PubMed][CrossRef]
- 3.
Trovik J, Thornhill HF, Kiserud T. Incidence of obstetric fistula in Norway: a population-based prospective cohort study. Acta Obstet Gynecol Scand 2016; 95: 405–10. [PubMed][CrossRef]
- 4.
Børseth KF, Acharya G, Kiserud T et al. Incidence of gynecological fistula and its surgical treatment: A national registry-based study. Acta Obstet Gynecol Scand 2019; 98: 1120–6. [PubMed][CrossRef]
- 5.
Brown HW, Wang L, Bunker CH et al. Lower reproductive tract fistula repairs in inpatient US women, 1979-2006. Int Urogynecol J Pelvic Floor Dysfunct 2012; 23: 403–10. [PubMed][CrossRef]
- 6.
Hilton P. Urogenital fistula in the UK: a personal case series managed over 25 years. BJU Int 2012; 110: 102–10. [PubMed][CrossRef]
- 7.
Ozuner G, Hull TL, Cartmill J et al. Long-term analysis of the use of transanal rectal advancement flaps for complicated anorectal/vaginal fistulas. Dis Colon Rectum 1996; 39: 10–4. [PubMed][CrossRef]
- 8.
Egeland P, Gjøen JE, Trovik J et al. Gynekologiske fistler til urinveier og tarm. Tidsskr Nor Laegeforen 2007; 127: 417–20. [PubMed]
- 9.
Goderstad JM, Lieng M, Busund B. Kirurgisk behandling av benigne gynekologiske lidelser. Tidsskr Nor Legeforen 2009; 129: 1460–3. [PubMed][CrossRef]
- 10.
Aarts JW, Nieboer TE, Johnson N et al. Surgical approach to hysterectomy for benign gynaecological disease. Cochrane Database Syst Rev 2015; 8: CD003677. [PubMed][CrossRef]
- 11.
Holdø B, Verelst M, Svenningsen R et al. Long-term clinical outcomes with the retropubic tension-free vaginal tape (TVT) procedure compared to Burch colposuspension for correcting stress urinary incontinence (SUI). Int Urogynecol J Pelvic Floor Dysfunct 2017; 28: 1739–46. [PubMed][CrossRef]
- 12.
Cohen AM, Kahn MA, Brown S. Comments to: surgical management of pelvic organ prolapse in women. Tech Coloproctol 2016; 20: 327–30. [PubMed][CrossRef]
- 13.
Viswanathan AN, Lee LJ, Eswara JR et al. Complications of pelvic radiation in patients treated for gynecologic malignancies. Cancer 2014; 120: 3870–83. [PubMed][CrossRef]
- 14.
Trovik J, Kiserud T, Reimers C et al. Gynekologiske fistler. I: Veileder i gynekologi 2015. Oslo: Den norske legeforening, 2015. https://www.legeforeningen.no/contentassets/a5d7370e547a4198900ada248f77a6cb/gynekologiske-fistler.pdf Accessed 26.5.2020.
- 15.
- 16.
Dyrkorn OA, Kulseng-Hanssen S, Sandvik L. TVT compared with TVT-O and TOT: results from the Norwegian National Incontinence Registry. Int Urogynecol J Pelvic Floor Dysfunct 2010; 21: 1321–6. [PubMed][CrossRef]
- 17.
Margolin DJ, Gonzalez RP. Retrospective analysis of traumatic bladder injury: does suprapubic catheterization alter outcome of healing? Am Surg 2004; 70: 1057–60. [PubMed]
- 18.
Turina M, Mulhall AM, Mahid SS et al. Frequency and surgical management of chronic complications related to pelvic radiation. Arch Surg 2008; 143: 46–52, discussion 52. [PubMed][CrossRef]
- 19.
Göttgens KW, Smeets RR, Stassen LP et al. The disappointing quality of published studies on operative techniques for rectovaginal fistulas: a blueprint for a prospective multi-institutional study. Dis Colon Rectum 2014; 57: 888–98. [PubMed][CrossRef]