Main findings
More than half of the respondents had considered general practice but decided against it, or quit working as a general practitioner.
The administrative burden and small professional community were key reasons why doctors opted out of general practice, in addition to a number of other factors.
There has been a prolonged focus on under-recruitment to general practice (1–7). In an evaluation undertaken in 2016 (8, 9), one in every four foundation doctors reported wanting to enter general practice. The need for new general practitioners (GPs), however, far exceeds this supply (2). Previous studies have identified the factors that GPs believe are important to recruit and retain doctors in this specialty. By asking doctors who have opted out of or quit general practice, we may also gain further insight into issues that have an impact on this choice.
Recruitment and stability have been shown to be important to ensure a sufficient number of doctors in this specialty and to persuade GPs to work in rural areas (4, 10). The need for economic security, as well as income and working conditions, including the size of the workload, are assumed to be factors that cause doctors to opt out of general practice (1). Norwegian studies have shown that professional development and autonomy, control over working hours and a subjectively manageable size of the practice are keys to a continuing career in general practice (3, 11). Studies from other countries show that economic incentives may have a positive effect on recruitment to non-central regions, although professional content and opportunities for development appear to play a greater role (12, 13). The introduction of the Coordination Reform in 2012 entailed a greater workload and a transfer of responsibilities from the specialist to the primary healthcare service (14, 15). Despite a reduction in average list length of 6 % in the period 2010–17, data from Statistics Norway show that the workload of the GPs has grown more than available medical resources (16).
A report from Denmark shows that the proportion of GPs who were dissatisfied with their job situation increased from 6 % in 2012 to 22 % in 2016 (17). This was due to longer working hours, poorer incomes, lack of recognition for a job well done and little freedom to choose working methods. In Sweden, estimates made in 2014 showed that assuming a coverage of 1500 patients per doctor in 2017, twice the existing number of GPs would be needed (18). In addition to this, a qualitative study revealed that the experience of a high workload and low staffing made medical practice less meaningful and gave rise to numerous challenges. Having control over one's own working day and the ability to plan working hours, including the possibility of part-time work, were highlighted as key criteria for the choice of specialty (18).
A study in the UK showed that increased workloads and longer working weeks for GPs were the main causes of them taking early retirement (19). Moreover, most GPs felt that they benefited little from the national measures initiated to counteract the shortfall in recruitment.
Previous studies have primarily investigated the GPs' own viewpoints with regard to factors that affect recruitment to general practice and decisions to remain in the specialty. To gain insight into the reasons that have been important for doctors who have opted out of general practice, we will therefore examine these doctors and their reasons for doing so.
Material and method
The Institute for Studies of the Medical Profession (LEFO) used the Medical Panel, which consists of 2 195 members. This is a sample of working doctors who have been followed up with postal questionnaires since 1994. Representativeness in terms of age, sex and position is maintained by including young doctors when their older colleagues retire, die or leave the sample for other reasons. The relevant data were collected from the panel from November 2016 – March 2017, including two reminders. The survey was approved by the Norwegian Centre for Research Data (NSD), and was not subject to mandatory submission to the Regional Committee for Medical and Health Research Ethics (IRB 0000 1870).
Doctors who were not working in general practice at the time were asked: 'Did you ever consider becoming a general practitioner?' Response alternatives were 'no', 'yes' and 'yes, I have been a general practitioner, but have quit'. Those who had considered general practice, but did not choose it, and those who had quit general practice were routed to questions asking which of 17 different factors had caused them to quit as GPs. Each factor had three response alternatives (yes/no/not relevant). Those who answered 'other reasons' had the opportunity to specify this in more detail in a free-text field. The questions were developed by LEFO researchers in collaboration with elected representatives of the Norwegian College of General Practitioners.
We present descriptive data on doctors who considered becoming GPs, but chose not to, and doctors who have been GPs, but have quit the specialty. Respondents with missing data were excluded from the analyses. Data were registered and analysed with the aid of SPSS Version 25.
Results
In total, 1 604 out of 2 195 doctors (73.1 %) responded to the survey. Altogether 44 of these were older than 70 years and therefore excluded. Of the remaining 1 560 there were 287 (18.4 %) GPs, who were thus not relevant to the further analysis. Of the remaining 1 273 doctors, altogether 1 153 had answered 'no' to the question of whether they were GPs and had answered the question of whether they had ever considered becoming GPs. This means that we have no data for 120 of the 1 273 (9.4 %).
Of those 1 153 who answered the question of ever having considered becoming a GP, 508 (44.1 %) answered 'no', 460 answered 'yes' and 185 reported that they had been GPs, but had quit.
A larger proportion of the women (294/641; 45.9 %) than of the men (166/512; 32.4 %) had considered general practice, but made another choice. On the other hand, a larger proportion of the men (104/512; 20.3 %) than of the women (81/641; 12.6 %) had been GPs, but quit. A total of 287/471 (60.9 %) of the doctors in the age group 25–35 years had considered, but did not choose general practice, compared to 94/254 (37.0 %) of those in the age group 36–45 years and 43/184 (23.4 %) in the age group 46–55 years (Table 1).
Table 1
Percentage distribution of answers to the question 'Did you ever consider becoming a GP?' The question was put in 2016–17 to doctors in the Medical Panel of the Institute for Studies of the Medical Profession who at that time were not GPs (N = 1 153).
| No | Yes | Yes, and I have been a GP, but have quit | ||
|---|---|---|---|---|
| Sex | ||||
| Men (n = 512) | 47.3 | 32.4 | 20.3 | |
| Women (n = 641) | 41.5 | 45.9 | 12.6 | |
| Age categories (years)1 | ||||
| 25–35 (n = 471) | 31.2 | 60.9 | 7.9 | |
| 36–45 (n = 254) | 53.1 | 37.0 | 9.9 | |
| 46–55 (n = 184) | 56.0 | 23.4 | 20.6 | |
| 56–69 (n = 224) | 51.3 | 14.3 | 34.4 | |
| Specialty in the main position2 | ||||
| General practice (n = 82) | 15.8 | 62.2 | 22.0 | |
| Laboratory disciplines (n = 89) | 56.2 | 32.6 | 11.2 | |
| Internal-medicine disciplines (n = 415) | 48.9 | 39.5 | 11.6 | |
| Surgical disciplines (n = 275) | 55.3 | 35.6 | 9.1 | |
| Psychiatry (n = 161) | 28.6 | 38.5 | 32.9 | |
| Community medicine (n = 27) | 22.2 | 11.1 | 66.7 | |
| Other (n = 61) | 27.9 | 59.0 | 13.1 | |
1Age not stated by 20 doctors
2Specialty not stated by 43 doctors
Among those who had quit general practice there was a larger proportion of women (33/80; 41.3 %) than men (20/100; 20.0 %) who had chosen psychiatry. The other main specialty where former GPs could be found in particular was internal medicine (women 17/80; 21.3 % and men 31/100; 31.0 %).
Of those doctors in the sample who reported not to be GPs, altogether 82 stated that their main position was within general practice. A total of 38 of these were foundation doctors, 5 were hospital doctors, 13 worked in the municipal health service, 4 were engaged in research, 12 answered 'other' and 10 reported to work in general practice.
Figure 1 shows 16 reasons for opting out of and quitting general practice, ranked by declining proportion in per cent for those who decided not to choose general practice compared to proportion in per cent of those who have quit.
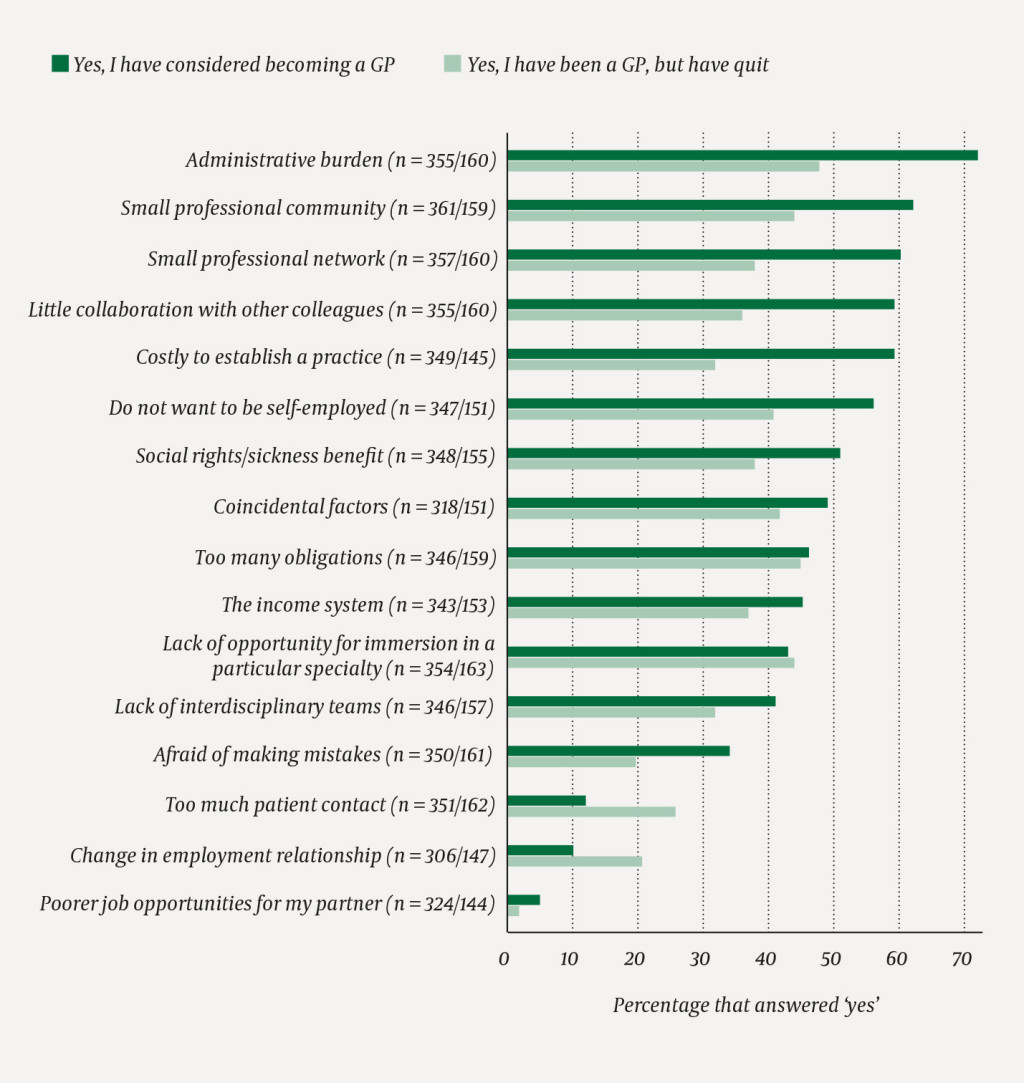
In addition to the proposed reasons, comments in the free-text field stated these reasons for opting out of general practice: 57 reported other plans/interests, 30 said that they were foundation doctors/had not yet chosen, 19 stated on-call/work burden, 13 reported negative experiences from work placement/internship and 8 gave family-related reasons (such as relocation, age, illness and small municipality), while 13 answered 'other'. The remaining 42 comments referred to factors that have already been referred to in Figure 1.
Discussion
More than one-half of those respondents who were not working as GPs had either considered general practice but decided against it, or they had been a GP and quit the profession.
More women (than men) and more young doctors had considered taking up general practice. The most important reasons for doctors not to choose general practice were the administrative burden and the small professional community. The fact that so many of the proposed reasons are highly ranked indicates that the reasons are complex. It is worth noting that 'too many obligations' appears to be a prominent cause for opting out.
Studies have repeatedly shown that GPs have a longer working week than most other doctors (20, 21). In 2018, the average working week for GPs was measured at 56 hours (22). The same study also showed that GPs have more tasks to perform than previously, for example e-consultations, certificates/declarations and dialogue meetings. A report from the Norwegian Directorate of Health shows that each patient has more consultations than was the case before (2). This indicates that the disease pathways to be dealt with in general practice have become more complicated than previously, and that the threshold to attending GPs has been lowered.
Doctors included in this study believe that too many obligations and an excessive administrative burden have contributed to their choice of leaving general practice. Studies from other countries show that the administrative burden imposed on has increased, and that this is perceived as taking time away from patient treatment (19). Tasks that entail longer working hours can be hard to reconcile with the doctors' increasing wish for a better work-life balance (23),(24). A Norwegian study points out the importance of a good work-life balance, with an opportunity to work part-time – especially for women – in order to reduce the risk of work-life stress that may lead to burn-out (24).
The need for more knowledge about the disease pathways and responsibility for standardised patient pathways and follow up from the specialist health service that have been transferred to the primary healthcare service may have been underestimated in the introduction of health service reforms (5). The health enterprise reform and the Coordination Reform, which included expedited transfer of patients from hospitals to the primary healthcare service and expectations for more decentralised treatment (such as standardised pathways for cancer treatment), may have increased the need for professional knowledge and thereby also for good professional communities and networks for GPs (5, 15). Reduced hospitalisation time, higher patient expectations and patients' access to knowledge about medical issues connected to their own health demand an expansion of GPs' knowledge (5, 15). This development highlights the need for a professional community.
In recent years, job satisfaction has declined among the GPs. The main reasons are lack of recognition for a job well done, less freedom to choose methods, heavy responsibility, long working hours and insufficient financial compensation (25). Doctors who opt out of general practice report that the most important factors are the difficulty of being self-employed and the cost of establishing a private practice, while having little access to social rights and benefits. To recruit specialists in general practice, regions in Western Norway have been granted government support for a pilot project for the years 2017–2020, in which doctors are employed in permanent traineeships (specialty registrars in general practice, ALIS). GPs who participate in this project believe that a fixed salary, social security, shorter patient lists and good supervision in this type of position will help increase the recruitment to general practice (26). In our data, we find that 'coincidental factors' are frequently reported as a reason for opting out of general practice by doctors who had considered this possibility, but made another choice. This may reflect a situation where the choice of specialty is governed to a large extent by the opportunities that present themselves during the training period, as well as when and where they appear (27). An opportunity for an ALIS position may thus have a major bearing. While many municipalities struggle to recruit applicants to GP positions (4), the ALIS positions are attracting numerous applicants.
Some studies suggest that more systematic effort should be devoted to improvement measures aiming to cater to the doctors' own health and generate enthusiasm for the profession (28, 29). The suggestions include changes to the distribution of tasks, such as delegating some of the administrative duties to others. Nurses and other auxiliary medical personnel could be given an expanded role in planning and responsibility for prevention, at the doctor's recommendation. To avoid fragmentation and non-transparent distribution of responsibilities this would require careful impact assessments and require considerable coordination (30, 31).
Measures that may help achieve a better work-life balance provide stability in everyday life and are important for a good career in general practice. These issues have been widely discussed in the GPs' own forums and the media in general in recent years (30, 31, 32). Findings in this study provide further knowledge on issues that affect doctors' choice of general practice and their decision to remain in this specialty.
Strengths and limitations
Since previous studies have focused on the opinions of the GPs themselves as to the key factors for choosing this specialty, it is a strength of this study that we have studied those who have opted out of general practice. The high response rate (73.1 %) provides for good representativeness.
A limitation of this study, on the other hand, is that the causal factors included in the questionnaire do not necessarily encompass all the work-related burdens of the GPs, for example on-call duty. Since the on-call duty burdens in the cities are very unlike those in rural areas, we chose instead to ask about workloads in general. Missing data account for 9.4 % of our data material, which is unlikely to have a major impact on the validity of the results.
Conclusion
The administrative burden and small professional community were the main reasons why doctors opt out of general practice. The findings indicate, however, that the picture is complex. It is therefore crucial to assess a multiplicity of conditions, both to persuade more young doctors to choose general practice and to retain doctors in this specialty. The discussion of why it is difficult to recruit and retain doctors in general practice may until now have focused narrowly on single causes. This study indicates that evaluation of projects involving permanent positions and structured supervision for GP specialty registrars may be measures that are important to implement, and their recommendations should be followed. Furthermore, it points to the importance of better professional networks and updating of skills, as well as a reduction in workloads and working hours. This combination of different measures may have an impact on the recruitment and retention of doctors in general practice.
The article has been peer reviewed.
- 1.
Øren TO. Flere unge må velge allmennmedisin. Dagens Medisin 1.4.2017. https://www.dagensmedisin.no/artikler/2017/04/01/flere-unge-ma-velge-allmennmedisin/ Accessed 20.12.2019.
- 2.
Utvikling i bruk av fastlege og legevakt 2010–2016. Analysenotat i Samdata kommune. Oslo: Helsedirektoratet, 2018. https://www.helsedirektoratet.no/rapporter/utvikling-i-bruk-av-fastlege-og-legevakt-2010-2016/ Accessed 10.12.2019.
- 3.
Holte JH. Remuneration and organization in general practice: Three essays on doctors'preferences. Doktoravhandling. Tromsø: UiT – Norges Arktiske Universitet, 2015. https://munin.uit.no/handle/10037/8259 Accessed 20.12.2019.
- 4.
Sæther AS, Nærø AF. Kampen om fastlegene. VG 2018. https://www.vg.no/spesial/2017/fastleger/ Accessed 10.12.2019.
- 5.
Fastlegeordningen 2.0.Trønderopprørets fastlegeundersøkelse og helsemedarbeiderundersøkelse. Trondheim: Trønderopprøret, 2018. http://www.flo20.no/wp-content/uploads/2018/06/TOundersøkelse-2.pdf Accessed 10.12.2019.
- 6.
Westnes SL, Kristoffersen EA, Burman RA. Fastlegeordningen trenger flere leger. Tidsskr Nor Legeforen 2012; 132: 674–6. [CrossRef]
- 7.
Sollien K. Fastlegene flykter fra distriktene. Dagens Medisin 1.2.2016. https://www.dagensmedisin.no/artikler/2016/02/01/fastlegene-flykter-fra-distriktene/ Accessed 10.12.2019.
- 8.
Birkeli CN. Nasjonal evaluering av turnustjenesten for leger. Rapport. Oslo: LEFO – Legeforskningsinstituttet, 2015. https://www.legeforeningen.no/contentassets/ea5f46eb1dc7453d91502248df658427/turnusrapporten-nasjonal-evaluering-avturnustjenesten-2010.pdf Accessed 20.12.2019.
- 9.
Birkeli C. Motiverte turnusleger starter i allmennpraksis, men blir de værende? Tidsskr Nor Legeforen 2016; 136: 1261. [PubMed][CrossRef]
- 10.
Legeforeningen. Fastlegesituasjonen forverret, viser ny kartlegging. https://www.legeforeningen.no/nyheter/2019/fastlegesituasjonen-forverret-viser-ny-kartlegging/ Accessed 10.12.2019.
- 11.
Holte JH, Kjaer T, Abelsen B et al. The impact of pecuniary and non-pecuniary incentives for attracting young doctors to rural general practice. Soc Sci Med 2015; 128: 1–9. [PubMed][CrossRef]
- 12.
Li J, Scott A, McGrail M et al. Retaining rural doctors: doctors' preferences for rural medical workforce incentives. Soc Sci Med 2014; 121: 56–64. [PubMed][CrossRef]
- 13.
Matsumoto M, Inoue K, Kajii E. Policy implications of a financial incentive programme to retain a physician workforce in underserved Japanese rural areas. Soc Sci Med 2010; 71: 667–71. [PubMed][CrossRef]
- 14.
Christiansen TW, Sandvik H. Fastlegeordningen forvitrer – hva nå? Tidsskr Nor Legeforen 2017; 137. doi: 10.4045/tidsskr.17.0856. [PubMed][CrossRef]
- 15.
St.meld. nr. 47 (2008–2009). Samhandlingsreformen: rett behandling – på rett sted – til rett tid. https://www.regjeringen.no/no/dokumenter/stmeld-nr-47-2008-2009-/id567201/ Accessed 20.12.2019.
- 16.
Statistisk sentralbyrå. Kortere pasientlister, lengre arbeidsdager? Rapport: Analyse SSB. 2018/14: Fastlegeordningen. https://www.ssb.no/helse/artikler-og-publikasjoner/kortere-pasientlister-lengre-arbeidsdager Accessed 10.12.2019.
- 17.
Pedersen AF, Nørøxe KB, Bro F et al. Alment praktiserende lægers psykiske arbeidsmiljø og jobbtilfredshet 2016. Aarhus: Forskningsenheden for Almen Praksis, Aarhus Universitet, 2016. https://feap.au.dk/fileadmin/feap/Rapport_Praktiserende_laegers_arbejdsmiljoe_30.10.2016.pdf Accessed 20.12.2019.
- 18.
System och strategier för att öka antalet ST-läkare i allmänmedicin. Kunnskapsgrunnlag om hur vi kan nå balans i primärvårdens läkarförsörjing. Rapport. Stockholm: Sveriges läkarforbund, 2014. https://slf.se/app/uploads/2018/05/rapport-om-st-lakare-iallmanmedicin.pdf Accessed 10.12.2019.
- 19.
Owen K, Hopkins T, Shortland T et al. GP retention in the UK: a worsening crisis. Findings from a cross-sectional survey. BMJ Open 2019; 9: e026048. [PubMed][CrossRef]
- 20.
Aasland OG, Rosta J. Fastlegenes arbeidstid 2000–08. Tidsskr Nor Legeforen 2011; 131: 1076–9. [PubMed][CrossRef]
- 21.
Rosta J, Aasland OG. Legers arbeidstid og tid til pasientarbeid i perioden 1994 - 2014. Tidsskr Nor Legeforen 2016; 136: 1355–9. [PubMed][CrossRef]
- 22.
Hundskår S, red. Fastlegers tidsbruk. Rapport til Helsedirektoratet. Bergen: Uni Research Nasjonalt kompetansesenter for legevaktmedisin, 2018.
- 23.
Kjosavik SR. Ongoing recruitment crisis In Norwegian general practice. Scand J Prim Health Care 2018; 36: 107–8. [PubMed][CrossRef]
- 24.
Hertzberg TK, Tyssen R, Skirbekk H et al. Jobb–hjem-balanse i to kohorter av norske leger. Tidsskr Nor Legeforen 2019; 139. doi: 10.4045/tidsskr.18.0339. [CrossRef]
- 25.
Rosta J, Aasland OG, Nylenna M. Changes in job satisfaction among doctors in Norway from 2010 to 2017: a study based on repeated surveys. BMJ Open 2019; 9: e027891. [PubMed][CrossRef]
- 26.
Bårdvik M. Unge fastleger og kommuner hyller fastlønn-prosjekt. Dagens Medisin 31.8.2018. https://www.dagensmedisin.no/artikler/2018/08/31/unge-fastleger-og-kommuner-hyller-fastlonn-prosjekt/ Accessed 10.12.2019.
- 27.
Dommerud T. Åpner for 200 flere stillinger for nyutdannede leger. Aftenposten 29.1.2019. https://www.aftenposten.no/norge/i/QleoMQ/Apner-for-200-flere-stillinger-for-nyutdannede-leger Accessed 10.12.2019.
- 28.
Sinsky CA, Willard-Grace R, Schutzbank AM et al. In search of joy in practice: a report of 23 high-functioning primary care practices. Ann Fam Med 2013; 11: 272–8. [PubMed][CrossRef]
- 29.
Bodenheimer T, Sinsky C. From triple to quadruple aim: care of the patient requires care of the provider. Ann Fam Med 2014; 12: 573–6. [PubMed][CrossRef]
- 30.
Brandstorp H. Rekruttering til fastlegeordningen. Aftenposten 27.5.2017. https://www.aftenposten.no/meninger/debatt/i/x6BnQ/rekruttering-til-fastlegeordningen-helen-brandstorp Accessed 20.12.2019.
- 31.
Allmennleger i spesialisering (ALIS). Rapport del 2 av 2. Oslo: Helsedirektoratet, 2018. https://www.nsdm.no/wp-content/uploads/2019/02/Allmennleger-i-spesialisering-ALIS-Del-2-av-2-endelig-23645184_4_1.pdf Accessed 20.12.2019.
- 32.
Nilsen L. Dette kan bidra til en bedre rekruttering til allmennmedisin. Dagens Medisin 20.2.2018. https://www.dagensmedisin.no/artikler/2018/02/20/-dette-kan-bidra-til-en-bedre-rekruttering-til-allmennmedisin/ Accessed 20.12.2019.
Manger allmennleger trives godt i sitt arbeid og føler for å fortsette etter at de har passert aldersgrensen på 70 år. Vi har et enestående yrke, med rik anledning til å bruke erfaring og menneskekontakt. En deltidsstilling på 40/50 % kan lette inngangen til ny allmennlege og lette overgangen for de allmennleger som ønsker å trappe ned, samtidig som de fortsatt trives svært godt i sitt arbeid. Nå som det er stor mangel på almenpraktikere, kan en slik gradvis nedtrapping over 3 til 4 år tilføre nye ressurser til allmennhelsetjenesten.