Main findings
Twelve of 1 999 women with perineal rupture underwent surgery within two years of childbirth.
Two of 41 maternity departments routinely referred patients for endoanal ultrasound scan and used validated anal incontinence scoring systems.
It should be possible to improve follow-up of this patient group, for example by routinely assessing the degree of anal incontinence with the aid of St. Mark's scoring six months after the injury occurred. Those with moderate to severe anal incontinence should have an ultrasound scan and be assessed for sphincteroplasty or sacral neuromodulation.
Vaginal birth is often the best option for both mother and child, and as a rule proceeds without serious complications. However some women incur tears in the perineum during a vaginal birth. The extent of the injury is graded from 1 to 4 (1, 2) (Box 1).
First degree: Superficial injury of perineum or vaginal mucosa
Second degree: Deep perineal injury with affection of perineal musculature, without affection of external anal sphincters
Third degree: Injuries involving anal sphincters
Fourth degree: Perineal injury involving anal sphincters and rectal mucosa
Around 900 women incur third or fourth degree perineal ruptures each year in Norway (3). The injury is repaired immediately after the birth by the obstetrician suturing the anal sphincters. However, several studies show that at least one third of women with such injuries experience leakage of gas or of both gas and faecal matter despite receiving treatment (4, 5). Some only experience problems many years later, others immediately after the injury has occurred. A Norwegian study from 2011 showed that 6 % of women with third or fourth degree perineal ruptures experienced faecal incontinence ten months postpartum and 21 % experienced gas incontinence (6). Other studies have shown that these problems are strongly related to permanent damage to the anal sphincters (7–10).
All patients with perineal rupture are recommended to go to a physiotherapist for pelvic floor exercises (2), and some of those who develop anal incontinence experience an improvement in their symptoms during the first few months (11, 12). As a result, 4–5 months usually elapse before it is possible to say whether the symptoms are persistent, and sometimes up to a year before physiotherapy has been attempted to an adequate extent. Patients with persistent problems should undergo a surgical procedure, either sphincteroplasty or sacral neuromodulation. Around 35–45 sphincteroplasty procedures are performed in Norway each year, and 45–55 sacral neuromodulations (13).
The main purpose of this study was to investigate what proportions of patients with third or fourth degree perineal rupture undergo either sphincteroplasty or sacral neuromodulation within two years of childbirth. We also wanted to survey how women with this type of injury are followed up by maternity departments in Norway.
Material and method
De-identified data on all women who have undergone vaginal birth and received the diagnosis perineal rupture third or fourth degree in Norway in the period 1.1.2012–31.12.2013 were obtained from the Medical Birth Registry of Norway. The dataset was linked to the Norwegian Patient Registry to find out how many of these patients have undergone either sphincteroplasty or sacral neuromodulation within two years of incurring the injury. The de-identified dataset was received by the authors after the link had been made by executive officers at the Medical Birth Registry and the Norwegian Patient Registry (with the aid of encrypted files and linkage keys). We did not at any time have access to identifiable information about the patients in this study.
The dataset from the Medical Registry of Births included variables such as the mother's age, parity, height and weight. The child's month and year of birth were also listed. The dataset from the Patient Registry included information on place of treatment, surgical method used and procedure date.
The procedures for follow-up of women with third and fourth degree perineal rupture were surveyed by means of a questionnaire sent to all maternity departments in Norway (see appendix on tidsskriftet.no). Questions asked included what information, written and/or verbal, the women received before discharge, who they were told to contact in the event of symptoms of anal incontinence, how many follow-up appointments the women were called in to as a matter of routine, and how many months after the birth. The maternity departments were asked to send us any written information they issued to the women, and were asked where they referred women who developed anal incontinence.
The study received advance approval from the Regional Committee for Medical and Health Research Ethics (reference no. 344/16) and from the Research Committee at Innlandet Hospital Trust. The Ethics Committee granted exemption from the need to obtain the participants' consent because the datasets were retrieved in de-identified form.
Results
There were a total of 98 000 vaginal births in Norway in the course of the inclusion period (2012–2013), and the incidence of third and fourth degree perineal rupture was 2 % (1 999 women) (3). The average age of these women at the time of the birth was 29.8 years, and over two thirds were primipara. Twelve (0.6 %) of the women had sphincteroplasty, 14 months on average into the follow-up period, while none underwent sacral neuromodulation.
Almost all (41 of 45) maternity departments responded to the questionnaire on their procedures for follow-up of women with third and fourth degree postnatal perineal rupture. All the maternity departments that responded informed patients verbally that they might experience gas or faecal leakage after the injury. Most also informed patients that they might experience dyspareunia. The same information, including advice on training with a physiotherapist, was provided in writing at 37 of the 41 maternity departments.
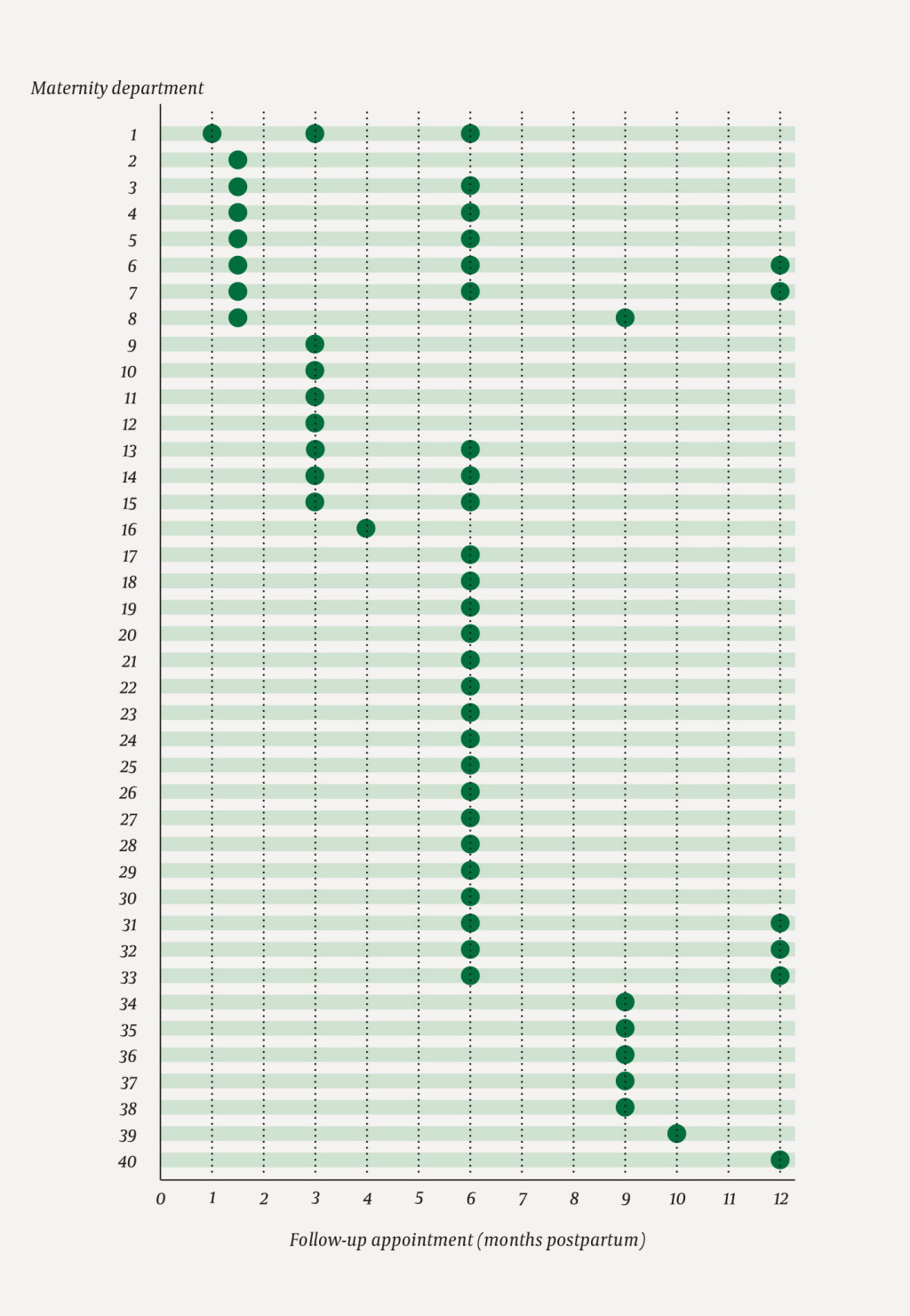
All departments called the women in for an outpatients check-up after the birth, but the number of follow-up appointments they received varied, as did the number of months after childbirth that the follow-up took place (Fig. 1). Five maternity departments offered gynaecological follow-up for three months, while eight offered the same follow-up for up to twelve months postpartum. Only two maternity departments referred all patients for a routine endoanal ultrasound scan six months postpartum and used a validated anal incontinence scoring system.
Discussion
A surprisingly small proportion (0.6 %) of women with third or fourth degree perineal rupture were treated for severe anal incontinence in the course of the first two years postpartum, despite the fact that international and Norwegian studies have shown that 6–23 % of these patients develop anal incontinence with faecal leakage (6, 10, 14, 15). Twelve women underwent sphincteroplasty, but none had sacral neuromodulation. Most women should have conservative treatment with physiotherapy as well as assessment and surgery in the event of persistent problems up to two years after giving birth. Patients who underwent sphincteroplasty were treated 14 months postpartum on average. We see no obvious reason why assessment and sacral neuromodulation therapy should take more than two years.
Norwegian maternity departments have sound procedures for informing women with third or fourth degree perineal rupture that they may experience gas or faecal leakage, and who they should contact if that happens, but not all provide patients with written information, although this is recommended in the national Veileder i fødselshjelp [Obstetrics guidelines] (2)
Conservative treatment with physiotherapy is offered at all maternity departments. At the same time, few departments offer more than one gynaecological outpatients follow-up appointment, and the offer is seldom extended for more than six months. According to several studies, six months is the optimal follow-up time, because spontaneous resolution of anal incontinence cannot be expected once 4–5 months have passed since childbirth (12, 13). Norway also offers longer parental leave than other countries, and some women may experience considerable distress due to anal incontinence when their parental leave is over and they resume work or studies. The optimal solution would probably be to offer follow-up for all women six months after childbirth and after twelve months for those with persistent problems.
Very few women raise the subject of anal incontinence with medical personnel of their own accord (7, 14, 16, 17). It is therefore conceivable that using an objective scoring system in connection with follow-up would lead to more women being referred in time for further assessment and treatment. Only three maternity departments reported using a validated anal incontinence scoring system, while only two of these routinely performed endoanal ultrasound scans.
We recommend using St Mark's scoring system for assessing anal incontinence, as it provides a clear picture of severity, and can be used to monitor symptom development over time. This is one of the most widely used anal incontinence scoring systems in Norway. Scores are based on the patient's symptoms over the previous four weeks, and have proved to be in agreement with how the patients themselves experience the severity of their symptoms (18, 19). The highest possible score is 24, which equates with complete anal incontinence Box 2). The severity increases with the patient's degree of faecal leakage. Most studies classify anal incontinence without faecal leakage as low-grade. If there is faecal leakage, the degree is assessed as moderate or severe, depending on the frequency of the leakage episodes and the impact on quality of life ((8, 16, 20)(20–25). A St Mark's score of over 8 implies moderate or severe anal incontinence (19).
Questions where the patient responds with a score of 0–4 (never–daily):
Liquid stool leakage
Solid stool leakage
Gas leakage
How often have leakage problems restricted your everyday activities?
Questions to which the patient answers yes or no:
Use of continence medication
Inability to postpone defecation for 15 minutes
Inability to postpone defecation for 15 minutes
An ultrasound scan is an important part of the assessment to detect the cause of anal incontinence problems (16, 26, 27). Damage to the anal sphincters during vaginal childbirth is usually the cause, but conditions such as rectal prolapse, anal fistula, malabsorption, inflammatory bowel disease and irritable bowel can also cause anal incontinence. In order for the correct treatment to be given, the cause of the problem must be known (28). Endoanal ultrasound is regarded as the most reliable method of detecting damage to the anal sphincters, but transperineal ultrasound has also proved suitable for excluding injury (29). However, transperineal ultrasound findings should always be confirmed with endoanal ultrasound, as the former have a low positive predictive value compared with the latter (30–32). The advantage of transperineal ultrasound is that the equipment is more readily available than that used for endoanal ultrasound. The examiner's experience is important in both modalities for avoiding misinterpretation (33).
A key strength of the study is that we have used health registers of high quality as the source of our study population. On the other hand, we did not receive information about the problems the women had, which must be regarded as the greatest weakness of the study.
The findings of this study indicate that the follow-up of women who incur a third or fourth degree perineal rupture can be improved. All maternity departments should provide written information about the symptoms that may develop and where women can turn for help. Routine follow-up should also be conducted six months after the injury occurred, and St. Mark's scoring should be used. Those who are found to have moderate or severe anal incontinence should have an ultrasound scan of the anal sphincters and be considered for treatment in the form of either sphincteroplasty or sacral neuromodulation.
The study is part of a PhD project at Innlandet Hospital Trust, which is the hospital in Norway at which most sphincteroplasty procedures are performed. Other hospitals prefer to treat patients with sacral neuromodulation. There are differing views as to preferred treatment form and which patients should receive the treatment.
The article has been peer-reviewed.
- 1.
Andrews V, Sultan AH, Thakar R et al. Occult anal sphincter injuries–myth or reality? BJOG 2006; 113: 195–200. [PubMed][CrossRef]
- 2.
Spydslaug A, Baghestan E, Laine K et al. Veileder i fødselshjelp. Oslo: Den norske legeforening, 2014. https://beta.legeforeningen.no/contentassets/9c5011955cc644a595cec42c01934c92/veileder-i-fodselshjelp-2014.pdf Accessed 31.8.2019.
- 3.
Folkehelseinstituttet. Medisinsk fødselsregister. http://statistikkbank.fhi.no/mfr/ Accessed 15.5.2019.
- 4.
Dudding TC, Vaizey CJ, Kamm MA. Obstetric anal sphincter injury: incidence, risk factors, and management. Ann Surg 2008; 247: 224–37. [PubMed][CrossRef]
- 5.
Huebner M, Gramlich NK, Rothmund R et al. Fecal incontinence after obstetric anal sphincter injuries. Int J Gynaecol Obstet 2013; 121: 74–7. [PubMed][CrossRef]
- 6.
Laine K, Skjeldestad FE, Sanda B et al. Prevalence and risk factors for anal incontinence after obstetric anal sphincter rupture. Acta Obstet Gynecol Scand 2011; 90: 319–24. [PubMed][CrossRef]
- 7.
Evers EC, Blomquist JL, McDermott KC et al. Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth. Am J Obstet Gynecol 2012; 207: 425.e1–6. [PubMed][CrossRef]
- 8.
Fornell EU, Matthiesen L, Sjödahl R et al. Obstetric anal sphincter injury ten years after: subjective and objective long term effects. BJOG 2005; 112: 312–6. [PubMed][CrossRef]
- 9.
Oberwalder M, Dinnewitzer A, Baig MK et al. The association between late-onset fecal incontinence and obstetric anal sphincter defects. Arch Surg 2004; 139: 429–32. [PubMed][CrossRef]
- 10.
Wagenius J, Laurin J. Clinical symptoms after anal sphincter rupture: a retrospective study. Acta Obstet Gynecol Scand 2003; 82: 246–50. [PubMed][CrossRef]
- 11.
Dietz HP. Exoanal imaging of the anal sphincters. J Ultrasound Med 2018; 37: 263–80. [PubMed][CrossRef]
- 12.
Shek KL, Zazzera VD, Atan IK et al. The evolution of transperineal ultrasound findings of the external anal sphincter during the first years after childbirth. Int Urogynecol J Pelvic Floor Dysfunct 2016; 27: 1899–903. [PubMed][CrossRef]
- 13.
Prøsch-Bilden T, Berglund ML, Norderval S et al. Norsk register for analinkontinens, Årsrapport 2017 med plan for forbedringstiltak. Tromsø: Norsk register for analinkontinens, 2018. https://www.kvalitetsregistre.no/sites/default/files/32_arsrapport_2017_nra.pdf Accessed 31.8.2019.
- 14.
Norderval S, Nsubuga D, Bjelke C et al. Anal incontinence after obstetric sphincter tears: incidence in a Norwegian county. Acta Obstet Gynecol Scand 2004; 83: 989–94. [PubMed][CrossRef]
- 15.
Sundquist JC. Long-term outcome after obstetric injury: a retrospective study. Acta Obstet Gynecol Scand 2012; 91: 715–8. [PubMed][CrossRef]
- 16.
Gjessing H, Backe B, Sahlin Y. Third degree obstetric tears; outcome after primary repair. Acta Obstet Gynecol Scand 1998; 77: 736–40. [PubMed][CrossRef]
- 17.
Lo J, Osterweil P, Li H et al. Quality of life in women with postpartum anal incontinence. Obstet Gynecol 2010; 115: 809–14. [PubMed][CrossRef]
- 18.
Maeda Y, Parés D, Norton C et al. Does the St. Mark's incontinence score reflect patients' perceptions? A review of 390 patients. Dis Colon Rectum 2008; 51: 436–42. [PubMed][CrossRef]
- 19.
Roos AM, Sultan AH, Thakar R. St. Mark's incontinence score for assessment of anal incontinence following obstetric anal sphincter injuries (OASIS). Int Urogynecol J Pelvic Floor Dysfunct 2009; 20: 407–10. [PubMed][CrossRef]
- 20.
Barisic GI, Krivokapic ZV, Markovic VA et al. Outcome of overlapping anal sphincter repair after 3 months and after a mean of 80 months. Int J Colorectal Dis 2006; 21: 52–6. [PubMed][CrossRef]
- 21.
Bravo Gutierrez A, Madoff RD, Lowry AC et al. Long-term results of anterior sphincteroplasty. Dis Colon Rectum 2004; 47: 727–31. [PubMed][CrossRef]
- 22.
Glasgow SC, Lowry AC. Long-term outcomes of anal sphincter repair for fecal incontinence: a systematic review. Dis Colon Rectum 2012; 55: 482–90. [PubMed][CrossRef]
- 23.
Goetz LH, Lowry AC. Overlapping sphincteroplasty: is it the standard of care? Clin Colon Rectal Surg 2005; 18: 22–31. [PubMed][CrossRef]
- 24.
Maslekar S, Gardiner AB, Duthie GS. Anterior anal sphincter repair for fecal incontinence: Good longterm results are possible. J Am Coll Surg 2007; 204: 40–6. [PubMed][CrossRef]
- 25.
Mevik K, Norderval S, Kileng H et al. Long-term results after anterior sphincteroplasty for anal incontinence. Scand J Surg 2009; 98: 234–8. [PubMed][CrossRef]
- 26.
Norderval S, Oian P, Revhaug A et al. Anal incontinence after obstetric sphincter tears: outcome of anatomic primary repairs. Dis Colon Rectum 2005; 48: 1055–61. [PubMed][CrossRef]
- 27.
Sultan AH, Kamm MA, Talbot IC et al. Anal endosonography for identifying external sphincter defects confirmed histologically. Br J Surg 1994; 81: 463–5. [PubMed][CrossRef]
- 28.
Dehli T, Norderval S, Lindsetmo RO et al. Utredning av anal inkontinens hos voksne. Tidsskr Nor Laegeforen 2008; 128: 1670–2. [PubMed]
- 29.
Thakar R, Sultan AH. Anal endosonography and its role in assessing the incontinent patient. Best Pract Res Clin Obstet Gynaecol 2004; 18: 157–73. [PubMed][CrossRef]
- 30.
Oom DM, West RL, Schouten WR et al. Detection of anal sphincter defects in female patients with fecal incontinence: a comparison of 3-dimensional transperineal ultrasound and 2-dimensional endoanal ultrasound. Dis Colon Rectum 2012; 55: 646–52. [PubMed][CrossRef]
- 31.
Ros C, Martínez-Franco E, Wozniak MM et al. Postpartum two- and three-dimensional ultrasound evaluation of anal sphincter complex in women with obstetric anal sphincter injury. Ultrasound Obstet Gynecol 2017; 49: 508–14. [PubMed][CrossRef]
- 32.
Taithongchai A, van Gruting IMA, Volløyhaug I et al. Comparing the diagnostic accuracy of 3 ultrasound modalities for diagnosing obstetric anal sphincter injuries. Am J Obstet Gynecol 2019; 221: 134.e1–9. [PubMed][CrossRef]
- 33.
Turel Fatakia F, Subramaniam N, Bienkiewicz J et al. How repeatable is assessment of external anal sphincter trauma by exoanal 4D ultrasound? Ultrasound Obstet Gynecol 2019; 53: 836–40. [PubMed][CrossRef]