Main findings
We estimated that 0.43 % of Norwegian children born during the period 2002–10 receive a diagnosis of Tourette syndrome by the age of 12.
The percentages varied considerably between the counties.
The majority had other psychiatric or neurological diagnoses in addition.
16 % were prescribed antipsychotic drugs in the year after receiving the diagnosis, probably for the treatment of tics.
Tourette syndrome (TS) is a neurological condition that first appears in childhood and is characterised by motor and vocal tics (1). Tics are involuntary, rapid, repetitive, intermittent motor movements or sudden, uncontrolled vocal sounds. Tics often occur in children and are normally transient. The TS diagnosis is often employed when at least two motor tics and one or more vocal tics have been present, not necessarily at the same time, for more than a year. In the case of TS, tics usually first appear at age 5–6 and are most intense at age 10–12 (1). Most population-based studies of TS are small, and estimates of its prevalence vary considerably (2). In a meta-analysis of prevalence studies, a mean prevalence of 0.77 % was found (2). The studies were mainly conducted in Europe and North America and comprised children aged 6–15 years. The prevalence was higher for boys than girls, with an average boy-girl ratio of 4.2 (2).
Studies based on health registry data have demonstrated a lower prevalence of Tourette syndrome than studies based on a representative sample of the population. In Denmark, 0.4–0.5 % of all children receive the diagnosis before the age of 15, whilst the corresponding prevalence in Finland is 0.1–0.2 % and less than 0.1 % in Sweden (3). The diagnostic practice in Norway has never been examined.
Genetic predisposition is the most important known risk factor for Tourette syndrome (4). In studies of twins and families, the heritability is calculated at 77 %. The pathogenesis has not been clarified but MR studies indicate that people with TS have functional disturbances in the neural pathways between the cerebral cortex and the basal ganglia (1). The majority of people with TS also have other neurological or psychiatric conditions (1). In childhood and adolescence, hyperkinetic disorder (ADHD) and obsessive-compulsive disorder (OCD) are the most common comorbidities (1, 4). Behavioural problems and anger issues are common, and emotional distress often occurs in adolescence. More than one-third are assumed to have outgrown TS by adulthood, while the other conditions often persist (1).
The best-documented non-medication form of therapy is tics management training (5), which is also the first-choice therapy. This is cognitive behavioural therapy where you learn to resist the tic urge. In addition, it incorporates relaxation techniques and psychosocial interventions. If the tics cause pain, social and emotional problems or make it difficult to function normally at school and in daily life, drugs therapy may be an option (6). However, there are only small studies of drugs therapy and only a few have been conducted as randomised, double-blind and placebo-controlled trials.
The European clinical guidelines for treating Tourette syndrome recommend risperidone, an atypical antipsychotic drug, as the first choice of treatment (7). Aripiprazole, a newer atypical antipsychotic drug, is also reported as promising. Clonidine, an antiadrenergic drug, is recommended for combined treatment of TS and ADHD. In Norway, regional guidelines have been drawn up for the Southern and Eastern Norway Regional Health Authority, and the recommendations are in line with the European guidelines (6). Aripiprazole and clonidine can be reimbursed on individual application, but this only applies to children, not adults. Risperidone is not reimbursed.
In this study, we used data from the Norwegian Patient Registry in order to calculate the percentage of children and adolescents receiving the TS diagnosis for the country as a whole, and by county. We also examined any other psychiatric and neurological diagnoses these children and adolescents receive. By combining data from the Norwegian Patient Registry and the Norwegian Prescription Database, we examined the use of psychopharmaca and other medications that affect the central nervous system. The analyses were initiated by the Autism and Tourette's committee, a government-appointed body that was established in 2018 to assess the range of services to people with autism spectrum disorders and Tourette syndrome.
Material and method
The Norwegian Patient Registry holds personally identifiable information from 2008 onwards. In this study, we used data relating to children and adolescents who have been in contact with mental health care institutions for children and adolescents, somatic hospitals and specialists in private practice in the period 2008−16. TS was defined as one or several registrations of the ICD-10 diagnosis code F95.2: Combined vocal and multiple motor tic disorder (de la Tourette) – Tourette syndrome.
TS is normally diagnosed from the age of six and upwards in Norway. We included all children born in the period 2002−10 in Norway, i.e. everyone who would be registered in the Norwegian Patient Registry from the calendar year they turned six years of age. Then we estimated the percentage who had received the diagnosis in the age group 6–14 years using Kaplan-Meier analyses, both for the country as a whole and by county. We also examined any other psychiatric and neurological diagnoses registered for those who had received the diagnosis in the years 2008–16.
At the end of the follow-up period, the population was aged 6–14 years, but we chose to terminate the Kaplan-Meier curves at the age of 12 because the county estimates for 13 and 14-year-olds were uncertain. The comparisons by county therefore apply to 12-year-olds. For the county estimates, we calculated the confidence intervals in order to compare the county average with the national average. Because we were conducting multiple comparisons (19 counties), we used strict confidence intervals (99.7 % based on the Bonferroni correction). The analyses were conducted in Stata 15 (Stata Statistical Software, StataCorp. 2017).
We also examined how many children and adolescents in the population were registered with the F95.1 diagnosis code: Chronic motor or vocal tic disorder. This code should be used for those who have had either motor or vocal tics for one year or more, but not a combination of both motor and vocal tics as in the case of TS.
We also wanted to study any changes in TS diagnostic practice over time. Therefore, we calculated the percentage of children registered with the diagnosis in each calendar year from 2008 to 2016, distributed by age and gender. These calculations included everyone in the age group 6–17 years in the calendar year in question. The population data were retrieved from the National Registry.
In the analyses of medication use, we linked data from the Norwegian Patient Registry and data from the Norwegian Prescription Database. The linkage encompassed data for the period 2008−15. We assessed medication use for everyone in the 6–17 age group first registered with Tourette syndrome in 2013 and 2014. The assessment included medications that had been prescribed in the course of the 365 days following the first registration of the diagnosis. We limited our assessment to recently registered diagnoses because we wanted to examine the treatment given in comparable periods after the diagnosis had been made.
The Norwegian Data Protection Authority (DPA) approved the use of data from the Norwegian Patient Registry (ref. 15/01648). The DPA (ref. 10/00447) and the Regional Committee for Medical and Health Research Ethics (ref. 2010/131) approved the linkage of data from the Patient Registry and the Norwegian Prescription Database for analyses of medication use.
Results
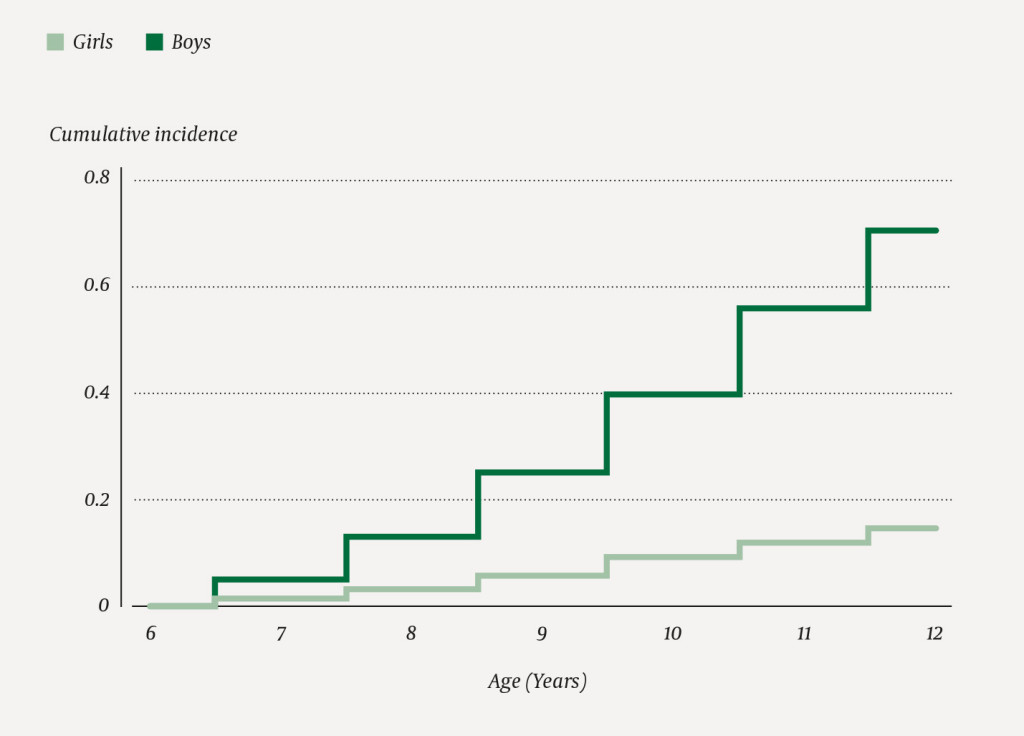
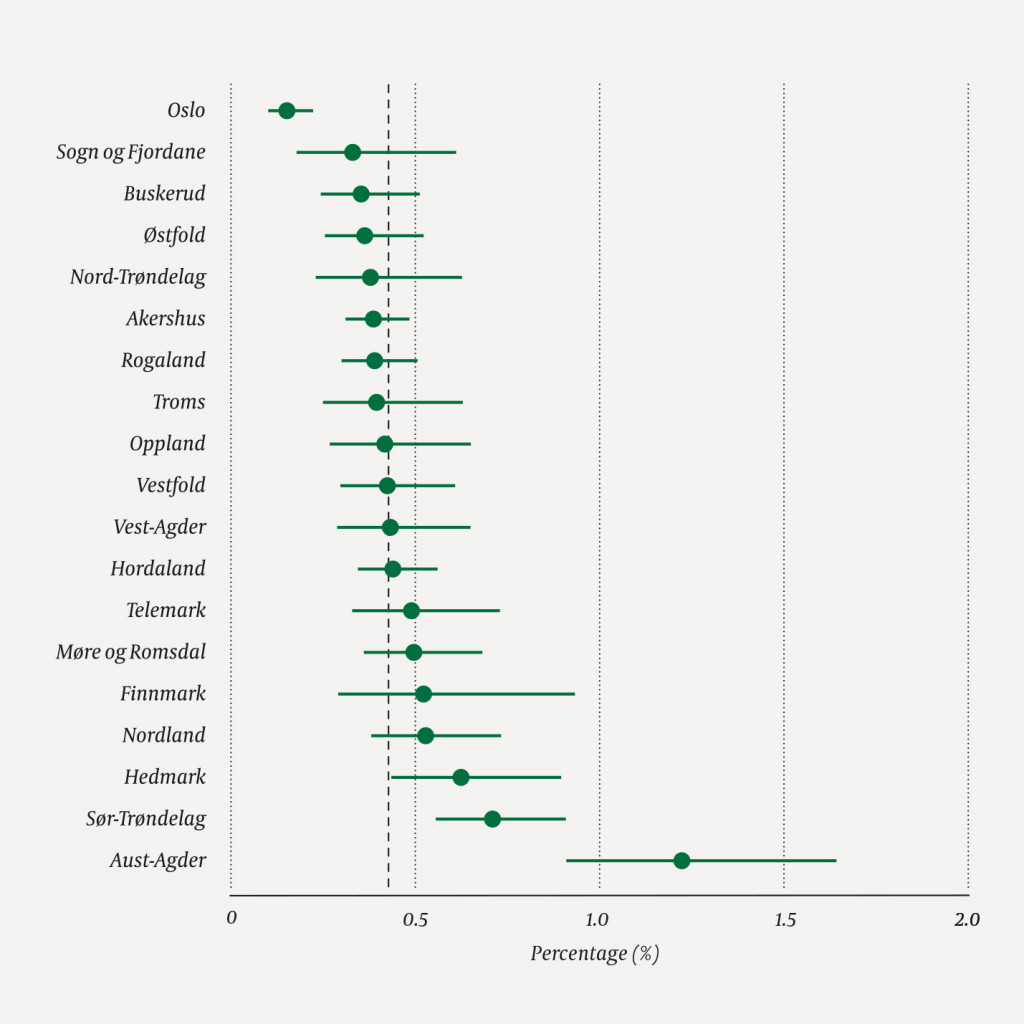
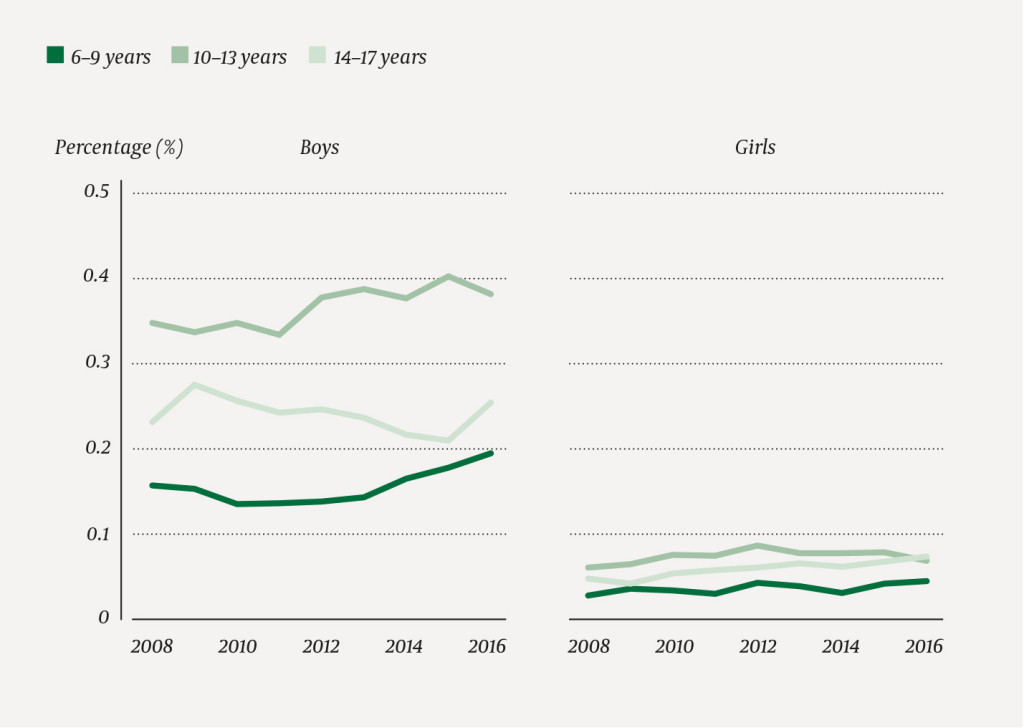
A total of 556 917 children were born between 2002 and 2010 and were resident in Norway at the age of six. Of these, 1814 were registered once or more with Tourette syndrome as the main or secondary diagnosis in the age group 6–14 years. On average, the children received the first diagnosis in the year they turned nine. In the year they turned twelve, the percentage was 0.43 %, broken down into 0.71 % for boys and 0.15 % for girls (Figure 1). The majority of counties were close to the national average (Figure 2) with the exception of Oslo where there was a lower average of 0.15 %, and Hedmark, Sør-Trøndelag and Aust-Agder where the average was higher at 0.63 %, 0.71 % and 1.23 % respectively. The percentage with the diagnosis was stable for both genders in all age groups in the years 2008–16 (Figure 3). The percentage share was highest for both boys and girls in the age group 10–13 years.
Of the 1814 children with TS, 1277 (70 %) were also registered with other psychiatric and neurological diagnoses (Table 1). The most common comorbid diagnosis was ADHD, which was registered in the case of 50 %. Autism spectrum disorders were registered in the case of 11 %. Many also had specific developmental disorders, i.e. language disorders (9 %), learning difficulties (6 %), mixed developmental disorders (4 %) and coordination disorders (2 %). Intellectual disability was registered in 3 %. Common psychiatric diagnoses were obsessive-compulsive disorder (7 %), anxiety disorders (7 %), reactions to stress, and adjustment disorders (7 %), behavioural disorders (6 %) and non-organic enuresis (7 %). Of neurological diagnoses, epilepsy (6 %) and sleep disorders (4 %) were the most common.
Table 1
Psychiatric and neurological supplementary diagnoses among children and adolescents registered with Tourette syndrome in the age group 6–17 years (N = 1 814). Applies to diagnosis groups registered in more than 1 % of children and adolescents with Tourette syndrome.
| Diagnosis group |
ICD-10 codes |
Number |
|---|---|---|
| Depressive episode/depression |
F32, F33, F92.0 |
23 (1) |
| Anxiety disorders |
F40, F41, F92.8, F93.0, F93.1, F93.2 |
129 (7) |
| Obsessive-compulsive disorder |
F42 |
128 (7) |
| Reactions to stress, and adjustment disorders |
F43 |
66 (4) |
| Non-organic sleeping disorder |
F51 |
23 (1) |
| Intellectual disability |
F70–F79 |
48 (3) |
| Language disorder |
F80 |
158 (9) |
| Learning disorders |
F81 |
117 (6) |
| Coordination disorder |
F82 |
34 (2) |
| Mixed developmental disorders |
F83 |
66 (4) |
| Autism spectrum disorder |
F84 |
200 (11) |
| Hyperkinetic disorder (ADHD) |
F90 |
909 (50) |
| Behavioural disorder |
F91 |
102 (6) |
| Non-organic enuresis |
F98.0 |
131 (7) |
| Non-organic encopresis |
F98.1 |
27 (1) |
| Other specified behavioural disorders |
F98.8 |
31 (2) |
| Epilepsy |
G40 |
106 (6) |
| Migraine |
G43 |
28 (2) |
| Sleeping disorders |
G47 |
65 (4) |
In the population, 878 (0.16 %) were registered with the F95.1 diagnosis code: Chronic motor or vocal tics. Of these, 140 (16 %) were also registered with the diagnosis code for TS (F95.2).
Altogether 754 children and adolescents in the age group 6–17 years received the TS diagnosis for the first time in 2013 and 2014. Many of these used pyschopharmaca or other drugs that affected the central nervous system (Table 2). The two most common medication categories were ADHD medications (37 %) and sleeping pills (23 % in total). The use of antipsychotics was registered in 16 %. Of the 122 who had received antipsychotics, 105 (86 %) had been prescribed risperidone. The reimbursement code most often used for risperidone was behavioural problems. No psychotic disorders were registered in any of the children. Clonidine (for combined treatment of TS and ADHD) was prescribed for 1 %.
Table 2
Prescription of psychopharmaca, antiepilectic and hypnotic drugs in the year following diagnosis of Tourette syndrome in children and adolescents (N = 754).
| Medication group (ATC code) |
Number (%) |
|---|---|
| Antipsychotic drugs (N05A) |
120 (16) |
| Clonidine (N02CX02) |
11 (1) |
| Antidepressant drugs (N06A) |
38 (5) |
| Anxiolytic drugs (N05B) |
6 (1) |
| Psychostimulants (Agents used for ADHD) (N06B) |
279 (37) |
| Antiepilectics (N03A) |
24 (3) |
| Melatonine (N05CH01) |
154 (20) |
| Alimemazine (R06AD01) |
24 (3) |
Discussion
Among Norwegian children born between 2002 and 2010, we estimate that 0.43 % will have received a TS diagnosis by the age of 12. The percentage share is lower than the mean prevalence of 0.77 % found in studies of the age group 6–15 years in other countries (2). The difference may indicate that a number of children in Norway who satisfy the diagnostic criteria for Tourette syndrome, do not receive the diagnosis. The average age at the time of diagnosis (9 years) is also somewhat high in view of the fact that the symptoms often make their first appearance at the age of 5–6.
A number of children with the diagnosis code for Tourette syndrome (F95.2) are also registered with the diagnosis code for chronic motor or vocal tics (diagnosis code F95.1). If code F95.1 is used for children who actually satisfy the criteria for TS, this will partly explain why the percentage share with the diagnosis is lower than in population studies. The registration of both codes for the same child can also have a natural explanation in that a child first presents one type of tic (motor or vocal) and then goes on to manifest both motor or vocal tics. Our data do not support any definite conclusions about this.
In Oslo, the percentage of children with Tourette syndrome is surprisingly low, while it is high in Aust-Agder. Hedmark and Sør-Trøndelag are above the national average and are more in line with the international prevalence estimate (2). We do not know why the percentages vary between the counties. This is probably due to variations in referral and diagnostic practices, or differences in the ability to recognise the condition. We have no knowledge of epidemiological studies that have demonstrated that the risk factor for TS varies geographically.
The majority of children and adolescents with TS have one or more other psychiatric or neurological diagnoses, and sleeping disorders are common. We already know that ADHD, learning difficulties, behavioural disorders and emotional problems are common in children and adolescents with TS (1, 4). The high percentage of those with autism spectrum disorders (11 %) was more unexpected. This had not been reported previously. The percentage share of obsessive-compulsive disorder (7 %) was surprisingly low, since other studies have shown that 40–60 % of those with Tourette syndrome present with this (4). The prevalence of OCD may be lower in our population, but it may also be the case that many have symptoms consistent with OCD without having received a diagnosis. Obsessive-compulsive thoughts and actions can be extensive and troublesome. It is important to assess and diagnose obsessive-compulsive disorders because children's access to cognitive therapy or other treatment is reliant on this.
Altogether 16 % had been prescribed antipsychotic drugs in the year following their diagnosis, and the majority had received risperidone. The reimbursement code was normally behavioural problems but the risperidone was most probably prescribed for the treatment of tics or combined tics and behavioural problems. This is in line with the recommendations of both the Norwegian and European guidelines (6, 7). Limiting the study to medication prescribed in the first 365 days after the diagnosis meant that we did not capture all treatment that commenced later in the patient pathway. Thus, the percentage share of those trying out drugs therapy at some point may be higher than 16 %.
It is unsatisfactory that Tourette syndrome is not approved as an indication or reimbursement basis for risperidone, since international professional guidelines recommend its use to counteract tics. It is also unreasonable that children can receive individual reimbursement for aripiprazole, but not adults.
The use of other medications for children and adolescents with TS corresponded with the other psychiatric and neurological diagnoses registered. The exception was that the percentage of those using sleeping pills was much higher than the percentage of those who had been diagnosed with sleeping disorders.
Our study is based on health registry data. We have not reviewed patient records or quality assured the diagnostic data. We have data on drugs dispensed but we do not know with certainty that these have been ingested, and we have no data on non-medication therapy.
Conclusion
The percentage of children diagnosed with Tourette syndrome in Norway is below the mean prevalence in population studies. Diagnostic practice varies considerably from county to county. More knowledge is needed about the prevalence of TS, the quality of assessment and diagnostics, the impact of drugs therapy and non-medication therapy as well as the long-term prognosis. By long-term prognosis, we mean not only the course of the condition itself but also supplementary disorders and how the children function at school and in working life. By combining data from health registries, health surveys and reviews of patient records, we are well positioned in Norway to conduct population-based studies of Tourette syndrome, thereby helping to remedy the lack of knowledge in the field.
The article has been peer reviewed.
- 1.
Grøholt B, Garløv I, Weidle B et al. Lærebok i barnepsykiatri. 5. utgave. Oslo: Universitetsforlaget, 2015.
- 2.
Knight T, Steeves T, Day L et al. Prevalence of tic disorders: a systematic review and meta-analysis. Pediatr Neurol 2012; 47: 77–90. [PubMed][CrossRef]
- 3.
Atladottir HO, Gyllenberg D, Langridge A et al. The increasing prevalence of reported diagnoses of childhood psychiatric disorders: a descriptive multinational comparison. Eur Child Adolesc Psychiatry 2015; 24: 173–83. [PubMed][CrossRef]
- 4.
Robertson MM, Eapen V, Singer HS et al. Gilles de la Tourette syndrome. Nat Rev Dis Primers 2017; 3: 16097. [PubMed][CrossRef]
- 5.
Verdellen C, van de Griendt J, Hartmann A et al. European clinical guidelines for Tourette syndrome and other tic disorders. Part III: behavioural and psychosocial interventions. Eur Child Adolesc Psychiatry 2011; 20: 197–207. [PubMed][CrossRef]
- 6.
Regional retningslinje for utredning og behandling av Tourettes syndrom. Oslo: Helse Sør–Øst, 2013. https://oslouniversitetssykehus.no/seksjon/regional-kompetansetjeneste-for-autisme-adhd-tourettes-syndrom-og-narkolepsi-helse-sor-ost/Documents/RR-TSOslo%20Universitetssykehus.pdf Lest 8.8.2019.
- 7.
Roessner V, Plessen KJ, Rothenberger A et al. European clinical guidelines for Tourette syndrome and other tic disorders. Part II: pharmacological treatment. Eur Child Adolesc Psychiatry 2011; 20: 173–96. [PubMed][CrossRef]