Screening for symptoms of depression and anxiety in a cardiology department
Main findings
Symptoms of depression and anxiety were reported by one-quarter of all patients with cardiac disease.
The screening tools for symptoms of depression and anxiety were easy to use in a cardiology department.
Time constraints, uncertainty about benefits and procedures for follow-up of the patient can be barriers to implementation of screening.
Symptoms of depression and anxiety are common in patients with cardiac disease (1, 2). Depressive symptoms are associated with increased mortality (3), reduced quality of life (4), increased use and increased cost of health services (5) and reduced opportunities for returning to work (6). According to the American Heart Association (7), depression is a negative prognostic factor at all stages of the disease (8). Depressive symptoms are also associated with other cardiac risk factors, such as smoking, poor diet and overweight, and predict reduced physical activity and poorer compliance with drug-based treatment regimens (9).
Depression is often a recurring disorder with onset during adolescence or early adulthood, and only a minority of the patients experience their first depressive episode in connection with the cardiac disease (10). Depression is therefore both a risk factor in a life-course perspective, in common with smoking, and a factor that may help trigger and exacerbate acute cardiac disease and reduce the patient's ability to cope with the illness. Anxiety disorders are associated with reduced quality of life after myocardial infarction, an unhealthy lifestyle and weakened compliance with treatment regimens (11). The risk may increase additively when depression and anxiety disorder coincide (12).
The American Heart Association (7) and European guidelines (13), including the National Institute for Health and Care Excellence (NICE) (14) and the Norwegian Directorate of Health (15), recommend procedures for screening for depression in cases of cardiac disease. There is sound evidence that treatment may improve mental health, functioning and quality of life (16, 17). A Cochrane review similarly concluded that a reduction in mortality from cardiac disease was possible, while pointing out that the evidence base here is uncertain (17). The American Heart Association (7) and the Norwegian Directorate of Health (15) recommend two screening questions for symptoms of depression, the Patient Health Questionnaire-2 (PHQ-2). These questions have been shown to be an independent predictor of mortality from heart failure up to four years after hospitalisation (18). NICE recommends screening with the use of two questions on symptoms of anxiety, the Generalized Anxiety Disorder Scale-2 (GAD-2) (19).
Although screening for symptoms of depression and anxiety is recommended in patients with cardiac disease, it is rarely done in practice. Experience from a study at the cardiology ward, Diakonhjemmet Hospital, where the nurses used the Patient Health Questionnaire-9 (PHQ-9) as a screening tool, indicated that screening is time-consuming in a busy hospital ward, and that the methods need to be simple (20). We wished to try out a simple procedure that involved oral questions, mainly asked by cardiologists. Moreover, we wished to screen outpatients, the largest group of patients in a cardiology department. Admitted patients were included a minimum of one month after discharge, not during hospitalisation as in the study referred to above (20). This was done to ensure that the reported symptoms of anxiety and depression were not overly influenced by ongoing stress during hospitalisation. The main objective was to assess a simple method for screening for symptoms of depression and anxiety among patients with cardiac disease.
Material and method
Sample
The study was carried out at the Department of Cardiology, Diakonhjemmet Hospital, in Oslo during the period 1 January–28 June 2017. The inclusion criteria were patients older than 18 years with a main diagnosis of valvular heart disease (I34–I37), tachyarrhythmia (I47–I49), myocardial infarction (I21, I22) or heart failure (I50). The patients were recruited on an ongoing basis until there were a minimum of 50 patients in each diagnostic group. The exclusion criteria were severe mental disorder, substance abuse, lack of capacity to provide informed consent or lack of ability to read and/or understand Norwegian.
Study design and screening tools
The study consisted of a screening component and subsequent follow-up identification and assessment by a clinical psychologist where this was indicated (Figure 1). PHQ-2 (21) and GAD-2 (22) were used as screening tools for symptoms of depression and anxiety respectively. In addition, the patient answered a yes/no question on panic attacks from the Patient Health Questionnaire – Somatic, Anxiety, and Depressive Symptom Scales (PHQ-SADS) (21) (Table 1). Patients from the outpatient clinic were screened by oral questioning during an appointment at the clinic – mainly by a cardiologist, but in some cases by a nurse. Admitted patients signed a consent form during hospitalisation and were screened over the telephone by a clinical psychologist one month after discharge. A score of ≥ 2 points on the PHQ-2 and/or the GAD-2, and/or an affirmative answer to the question on panic attacks were cut-off values values, aiming to achieve a high sensitivity to symptoms (23).
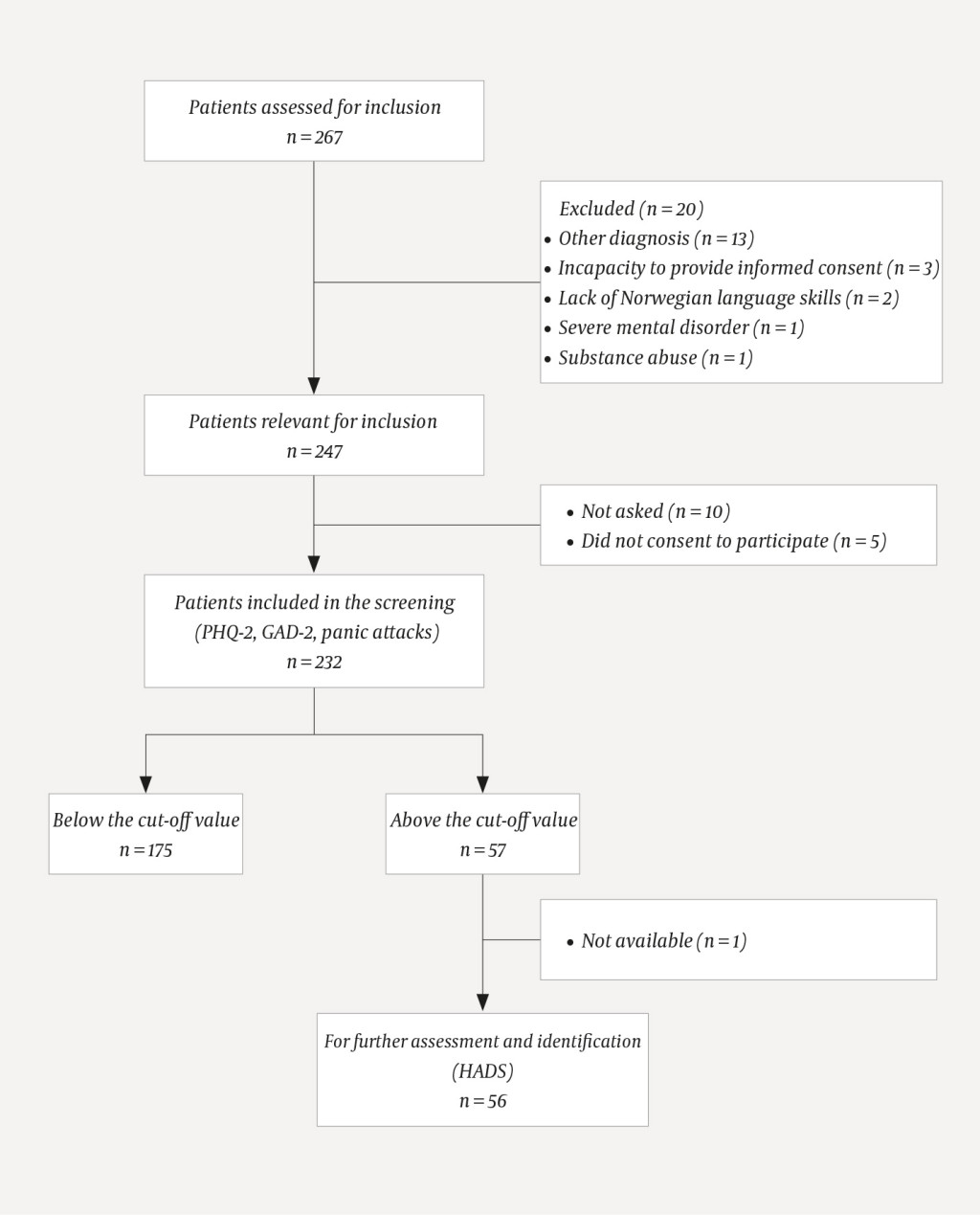
Table 1
Screening for symptoms of depression, anxiety and panic attacks at the Department of Cardiology, Diakonhjemmet Hospital (n = 232). PHQ-2 = Patient Health Questionnaire-2. PHQ-SADS = Patient Health Questionnaire – Somatic, Anxiety, and Depressive Symptom Scales. GAD-2 = Generalized Anxiety Disorder Scale-2.
| Not at all |
Several days |
More than half the days |
Nearly every day |
No |
Yes |
|
|---|---|---|---|---|---|---|
| Little interest or pleasure in doing things? (PHQ-2, n = 232) |
172 |
39 |
10 |
11 |
- |
- |
| Feeling down, depressed or hopeless? (PHQ-2, n = 232) |
163 |
46 |
7 |
16 |
- |
- |
| Feeling nervous, anxious or on edge? |
171 |
42 |
7 |
12 |
- |
- |
| Not being able to stop or control worrying? (GAD-2, n = 231) |
193 |
19 |
6 |
13 |
- |
- |
| In the last four weeks, have you had an anxiety attack (suddenly feeling fear or panic)? |
- |
- |
- |
- |
218 |
12 |
To obtain more information on the severity of the reported symptoms, patients who scored above the cut-off value were also assessed with the Hospital Anxiety and Depression Scale (HADS). If they were screened by a clinical psychologist one month after discharge, they were immediately followed up with the HADS. If they were screened by a cardiologist or a nurse at the outpatient clinic, HADS was completed a few days later by a clinical psychologist over the telephone. HADS omits questions about somatic symptoms of depression and anxiety that may be confused with symptoms of cardiac disease. Two sub-scales target symptoms of depression (HADS-D) and anxiety (HADS-A) respectively. A cut-off value of ≥ 4 for HADS-D and/or HADS-A has been used in studies of different patient groups (24). Patients who scored above this cut-off value were asked supplementary questions about the impact of their symptoms on functioning (Table 2).
Table 2
Supplementary questions for further identification of patients with symptoms of depression and anxiety (n = 41). n corresponds to the patients who scored above the cut-off value on the initial screening and the Hospital Anxiety and Depression Scale (HADS).
| Not difficult at all |
A little difficult |
Very difficult |
Extremely difficult |
No |
Yes |
|
|---|---|---|---|---|---|---|
| In case of heart disease, it is normal to receive health advice on physical activity, dietary changes, cutting down on smoking and taking medicines as recommended. Do you feel that the mental symptoms that you have described here have made it more difficult to follow such advice in practice? (n = 36) |
19 |
13 |
2 |
2 |
- |
- |
| To what extent do you feel that the mental symptoms that you have described here have made it difficult for you to perform your work, deal with things at home or get along with others? |
9 |
22 |
3 |
2 |
- |
- |
| Have your next of kin expressed concern about the mental symptoms that you have described here? (n = 34) |
- |
- |
- |
- |
17 |
17 |
| Accompanied by someone close to you if relevant, would you like a session with a clinical psychologist on preventing and coping with mental symptoms associated with cardiac disease? (n = 41) |
- |
- |
- |
- |
21 |
20 |
Ethics
The Regional Committee for Medical and Health Research Ethics (REC South-Eastern Norway, ref. no. 2016/1137) considered the study to be outside their mandate, but it was approved by the Data Protection Officer at Oslo University Hospital (ref. no. 2016/16558) and registered in ClinicalTrials.gov (ID: NCT03203395). Written informed consent was collected from all patients.
Statistical analyses
The data were analysed using SPSS Statistics 21.0 and are reported descriptively.
Results
A total of 267 patients were assessed for inclusion, whereof 20 were excluded and 15 did not consent to participation or were excluded for reasons of time constraints (Figure 1). The final sample consisted of 232 patients, of whom 58 had valvular heart disease, 73 had tachyarrhythmia, 52 had myocardial infarction and 49 had heart failure. Altogether 161 (69 %) of the patients who participated in the screening were men, and the average age was 72 years (SD 11.3). A total of 173 (75 %) of the patients were recruited from the outpatient clinic and 59 (25 %) from the hospital ward. Altogether 57 (25 %) patients scored above the cut-off value when screened. Of these, 12 patients answered 'yes' to the question on panic attacks, and all of these simultaneously scored above the cut-off value in PHQ-2 and/or GAD-2 (Table 1).
Of the 57 patients who scored above the cut-off value in the screening, altogether 56 continued to further identification and assessment by a clinical psychologist (Figure 1). A total of 41 (73 %) of these also scored ≥ 4 on HADS-A and/or HADS-D. For 17 (47 %) patients, the mental symptoms had made it more difficult to comply with health advice in practice. For 27 (75 %) patients, the mental symptoms had made it more difficult for them to perform their work, deal with things at home or get along with others, and a total of 17 (50 %) of those asked had experienced that their next of kin had expressed concern for their mental state (Table 2).
Altogether 20 (49 %) of those 41 patients who scored above the cut-off value on the initial screening and HADS wanted counselling sessions with a clinical psychologist, and 9 (43 %) of those who did not want counselling sessions reported that they would like an opportunity for counselling at a later time (Table 2).
Discussion
The main conclusion is that we have suitable screening tools for symptoms of depression and anxiety in patients with cardiac disease. The gap between the recommendations for routine screening on the one hand and what actually happens in clinical practice on the other is likely to have other causes. One such cause could be uncertainty as to whether the treatment of symptoms of depression and anxiety also contributes to increased survival for patients with cardiac disease (17).
Altogether 73 % of those who scored above the cut-off value on the screening questions also scored above the cut-off value on HADS. Other studies have found that a score of ≥ 2 points on PHQ-2 and/or GAD-2 is a suitable cut-off value for further assessment (25). Raising the cut-off value to ≥ 3 points may increase the risk of failing to identify patients in need of follow-up. No more than twelve patients answered 'yes' to the question on panic attacks, and all of them scored above the cut-off value in PHQ-2 and/or GAD-2, which may be an argument in favour of omitting this question (Table 1).
One limitation of this study is that we could not ascertain the number of patients who were not assessed for screening. Not all of the doctors in the department participated, and during periods of high workload screenings could sometimes not be performed. Measures to increase the proportion might be to include all relevant health personnel and ensure that patients who are not screened can be included at a later time. The proportion will increase even further if GPs also perform screening of those patients who receive such follow-up.
One advantage of having the specialist health services perform the screening is that it helps direct attention to the barriers to compliance that symptoms of depression and anxiety entail. Many of the patients in the study reported difficulties in complying with health advice (47 %) or performing work, dealing with things at home or getting along with others (75 %) (Table 2). A Norwegian study showed that few patients achieve an adequate reduction in their cardiovascular risk factors after a myocardial infarction (26). In case of a positive screening, health personnel can follow up with questions about the extent to which the symptoms hinder compliance.
It is important to ascertain when in the disease course screening should be performed, if at all, and whether it should be done by the specialist and/or primary health services. Attempting to perform screening at both levels would increase the likelihood of identifying relevant patients, and for coordinated treatment between service levels and between different primary health agencies ('collaborative care') (27). Screening can be performed on a routine basis while taking patient history and can also be carried out by nurses. Moreover, many cardiologists find it natural to ask questions about the mental burden associated with cardiac disease, and to view the person in a holistic way.
By asking questions about mental symptoms one opens up a topic that may require further follow-up. It is thus essential to have a strategy for what to do if the patient answers in the affirmative. Internal referral in the hospital or communicating this information to the patient's GP may represent such strategies. In addition, the patient may be asked the same questions again in a later consultation, especially in case of problems with compliance. Here, one might provide information that measures recommended for heart disease also can prevent mental symptoms. These include regular physical exercise, avoiding isolation and passivity, freeing oneself from depressing thoughts and establishing a daily routine of meaningful activities. Systematic screening may thus provide a good basis for beneficial support measures.
The article has been peer reviewed.
- 1.
Thombs BD, Bass EB, Ford DE et al. Prevalence of depression in survivors of acute myocardial infarction. J Gen Intern Med 2006; 21: 30–8. [PubMed][CrossRef]
- 2.
Tully PJ, Cosh SM, Baumeister H. The anxious heart in whose mind? A systematic review and meta-regression of factors associated with anxiety disorder diagnosis, treatment and morbidity risk in coronary heart disease. J Psychosom Res 2014; 77: 439–48. [PubMed][CrossRef]
- 3.
Nicholson A, Kuper H, Hemingway H. Depression as an aetiologic and prognostic factor in coronary heart disease: a meta-analysis of 6362 events among 146 538 participants in 54 observational studies. Eur Heart J 2006; 27: 2763–74. [PubMed][CrossRef]
- 4.
Ruo B, Rumsfeld JS, Hlatky MA et al. Depressive symptoms and health-related quality of life: the Heart and Soul Study. JAMA 2003; 290: 215–21. [PubMed][CrossRef]
- 5.
Rodwin BA, Spruill TM, Ladapo JA. Economics of psychosocial factors in patients with cardiovascular disease. Prog Cardiovasc Dis 2013; 55: 563–73. [PubMed][CrossRef]
- 6.
Henderson M, Harvey SB, Overland S et al. Work and common psychiatric disorders. J R Soc Med 2011; 104: 198–207. [PubMed][CrossRef]
- 7.
Lichtman JH, Froelicher ES, Blumenthal JA et al. Depression as a risk factor for poor prognosis among patients with acute coronary syndrome: systematic review and recommendations: a scientific statement from the American Heart Association. Circulation 2014; 129: 1350–69. [PubMed][CrossRef]
- 8.
May HT, Horne BD, Knight S et al. The association of depression at any time to the risk of death following coronary artery disease diagnosis. Eur Heart J Qual Care Clin Outcomes 2017; 3: 296–302. [PubMed][CrossRef]
- 9.
Sin NL, Kumar AD, Gehi AK et al. Direction of association between depressive symptoms and lifestyle behaviors in patients with coronary heart disease: the Heart and Soul Study. Ann Behav Med 2016; 50: 523–32. [PubMed][CrossRef]
- 10.
Carney RM, Freedland KE. Treatment-resistant depression and mortality after acute coronary syndrome. Am J Psychiatry 2009; 166: 410–7. [PubMed][CrossRef]
- 11.
Kuhl EA, Fauerbach JA, Bush DE et al. Relation of anxiety and adherence to risk-reducing recommendations following myocardial infarction. Am J Cardiol 2009; 103: 1629–34. [PubMed][CrossRef]
- 12.
Watkins LL, Koch GG, Sherwood A et al. Association of anxiety and depression with all-cause mortality in individuals with coronary heart disease. J Am Heart Assoc 2013; 2: e000068. [PubMed][CrossRef]
- 13.
Piepoli MF, Hoes AW, Agewall S et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice: The Sixth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of 10 societies and by invited experts): Developed with the special contribution of the European Association for Cardiovascular Prevention & Rehabilitation (EACPR). Eur J Prev Cardiol 2016; 23: NP1–96. [PubMed][CrossRef]
- 14.
Depression in adults with a chronic physical health problem: recognition and management. NICE guideline (CG91). London: National Institute for Health and Clinical Excellence, 2009. https://www.nice.org.uk/guidance/cg91/resources/depression-inadults-with-a-chronic-physical-health-problem-recognition-and-management-pdf-975744316357
- 15.
Nasjonale retningslinjer for diagnostisering og behandling av voksne med depresjon i primær- og spesialisthelsetjenesten. IS-1561. Oslo: Helsedirektoratet, 2009. https://www.helsedirektoratet.no/retningslinjer/voksne-med-depresjon/Voksne%20med%20depresjon%20%E2%80%93%20Nasjonal%20retningslinje%20for%20diagnostisering%20og%20behandling%20%20i%20prim%C3%A6r-%20og%20spesialisthelsetjenesten.pdf/_/attachment/inline/ed0d2ef2-da11-4c4e-9423-58e1b6ddc4d9:961cda6577d48345aa0d6fe9642b6b6acc2a6506/Voksne%20med%20depresjon%20%E2%80%93%20Nasjonal%20retningslinje%20for%20diagnostisering%20og%20behandling%20%20i%20prim%C3%A6r%20og%20spesialisthelsetjenesten.pdf Lest 16.9.2019.
- 16.
Huffman JC, Mastromauro CA, Beach SR et al. Collaborative care for depression and anxiety disorders in patients with recent cardiac events: the Management of Sadness and Anxiety in Cardiology (MOSAIC) randomized clinical trial. JAMA Intern Med 2014; 174: 927–35. [PubMed][CrossRef]
- 17.
Richards SH, Anderson L, Jenkinson CE et al. Psychological interventions for coronary heart disease: Cochrane systematic review and meta-analysis. Eur J Prev Cardiol 2018; 25: 247–59. [PubMed][CrossRef]
- 18.
Deveney TK, Belnap BH, Mazumdar S et al. The prognostic impact and optimal timing of the Patient Health Questionnaire depression screen on 4-year mortality among hospitalized patients with systolic heart failure. Gen Hosp Psychiatry 2016; 42: 9–14. [PubMed][CrossRef]
- 19.
Common mental health problems: identification and pathways to care. NICE guideline (CG123). London: National Institute for Health and Clinical Excellence, 2011. https://www.nice.org.uk/guidance/cg123/resources/common-mental-health-problemsidentification-and-pathways-to-care-pdf-35109448223173
- 20.
Berge T, Finset A, Fjerstad E et al. Kartlegging av depressive symptomer ved hjertesykdom. Sykepleien Forsk 2017; 12: 60372.
- 21.
Kroenke K, Spitzer RL, Williams JB et al. The Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales: a systematic review. Gen Hosp Psychiatry 2010; 32: 345–59. [PubMed][CrossRef]
- 22.
Plummer F, Manea L, Trepel D et al. Screening for anxiety disorders with the GAD-7 and GAD-2: a systematic review and diagnostic metaanalysis. Gen Hosp Psychiatry 2016; 39: 24–31. [PubMed][CrossRef]
- 23.
Arroll B, Goodyear-Smith F, Crengle S et al. Validation of PHQ-2 and PHQ-9 to screen for major depression in the primary care population. Ann Fam Med 2010; 8: 348–53. [PubMed][CrossRef]
- 24.
Sagen U, Vik TG, Moum T et al. Screening for anxiety and depression after stroke: comparison of the hospital anxiety and depression scale and the Montgomery and Asberg depression rating scale. J Psychosom Res 2009; 67: 325–32. [PubMed][CrossRef]
- 25.
Manea L, Gilbody S, Hewitt C et al. Identifying depression with the PHQ-2: A diagnostic meta-analysis. J Affect Disord 2016; 203: 382–95. [PubMed][CrossRef]
- 26.
Sverre E, Peersen K, Husebye E et al. Unfavourable risk factor control after coronary events in routine clinical practice. BMC Cardiovasc Disord 2017; 17: 40. [PubMed][CrossRef]
- 27.
Celano CM, Healy B, Suarez L et al. Cost-Effectiveness of a Collaborative Care Depression and Anxiety Treatment Program in Patients with Acute Cardiac Illness. Value Health 2016; 19: 185–91. [PubMed][CrossRef]