Main findings
The use of nitrous oxide during selected paediatric procedures was judged by the nurse in charge of care to be highly effective in 81 % of cases
Adverse effects led to stoppage of the procedure in 2 % of cases
For 43 % of procedures, it was felt that general anaesthesia would have been necessary had nitrous oxide not been available
Painful procedures are often necessary in association with medical assessment, diagnosis and some forms of treatment. Painful experiences in childhood may influence pain perception in adulthood (1, 2), and anxiety and pain during procedures may adversely affect responses to subsequent procedures (3). Paediatric healthcare professionals have therefore become increasingly focused on reducing pain, alleviating anxiety and avoiding psychological trauma in association with medical procedures.
An ideal sedative agent relieves anxiety and pain, and provides effective sedation. It has a short half-life, rapid onset of action and few adverse effects. In addition, it should be easy to administer and cost-effective (4). Good communication and age-appropriate preparation of the child are also highly important for optimising drug efficacy. A successful procedure takes place under calm conditions and without the need for repeated attempts.
In Norway, midazolam has long been the first-line anxiolytic for paediatric medical procedures, often in combination with local anaesthesia (5). However, the efficacy and duration of action of midazolam can vary and a lengthy observation period may be required after its administration (6, 7). Dexmedetomidine is also increasingly used, despite not being approved for use in a paediatric setting. Nitrous oxide has rarely been used in children in Norway, but is more frequently used in Sweden and Denmark (8).
At the request of several paediatric departments in Norway, a national health technology assessment was recently conducted on the use of nitrous oxide in children. It was concluded that nitrous oxide is safe for use by trained nurses in departments with standard monitoring procedures without the need for anaesthesia personnel to be present (8).
We wished to investigate the safety and adverse effect profile of nitrous oxide when used on wards or during outpatient procedures, and to record how effective children and nurses perceived it to be, whether its effectiveness was age-dependent and whether introduction of nitrous oxide could reduce the use of general anaesthesia.
Material and method
In July 2013, the Department of Paediatric and Adolescent Medicine at Østfold Hospital Trust began the use of nitrous oxide (N2O). In 2015, the Orthopaedics and Trauma Clinic adopted the technique following training by nurses from the Department of Paediatric and Adolescent Medicine. A list of procedures for which N2O could be used was prepared by nurses and doctors from the Department of Paediatric and Adolescent Medicine, with the aid of the Department of Anaesthesia, and was based on previous studies (4, 9, 10) and the experiences of paediatric departments in Hammerfest and Copenhagen. The nurses received group training on educational days, practical one-to-one guidance, and annual refresher training on administration, observation and recording techniques.
We offered nitrous oxide to children aged 4–17 years as an alternative to general anaesthesia for procedures that are easier to perform with the patient lightly sedated and where the expected procedure duration is less than 20 minutes. For scenarios in which midazolam would previously have been used, nitrous oxide was considered as an option depending on the child's capacity to cooperate.
All procedures with nitrous oxide were performed by two nurses, with a paediatrician present in the department. The child and his or her parents were provided with information, and children were allowed to play with the mask, try it on and choose a scent (strawberry, cola, chocolate or vanilla) to rub inside the mask. Oxygen and a suitable bag valve mask were present in the immediate vicinity during the procedures. Children were monitored throughout the entire procedure with a pulse oximeter. A doctor was present during the procedure if nitrous oxide was used in combination with other sedatives or opioids.
A mixture of 50 % oxygen and 50 % nitrous oxide (Livopan) was used. The gas was administered through a demand valve, which delivers nitrous oxide upon inspiration. Expired air was extracted through the ventilation system (11). Inhalation was initiated at least 3–4 minutes prior to the start of the procedure (9, 10). The parents or one of the nurses reassured and distracted the patient. The duration of inhalation did not exceed 30 minutes. Upon completion of the procedure, the child received 100 % oxygen for 3–5 minutes to prevent diffusion hypoxia.
We applied exclusion criteria in line with international recommendations (12) (Box 1). All patients who received nitrous oxide are included in the study.
Absolute
Decreased consciousness
Respiratory depression
Pneumothorax
Ileus
Acute sinusitis or otitis
Head injuries
Severe heart failure
Pregnancy in 1st–2nd trimester
Relative
Reduced ability to cooperate (children aged < 4 years)
Expected procedure duration > 20 minutes
Known vitamin B12- or folic acid deficiency
As part of quality assurance work, we collected data systematically and anonymously during the period 13 July 2013–25 August 2017 using an observation form. Data were recorded during the procedure and immediately after it ended. The nurse with primary responsibility for the procedure recorded age, sex, type and duration of procedure, adverse effects and any supplementary medication. Further comments were made as free text on the effectiveness of nitrous oxide, the parents' impressions, and any unexpected incidents such as the stoppage of a procedure and the reasons why.
Children rated the effectiveness of nitrous oxide on a pain scale, where 0 represents no pain and 10 the worst pain imaginable. The choice of pain scale was adjusted for age: the FPS-R scale (Faces Pain Scale – revised) was used for children aged 4–7 years (13) and the NRS (Numerical Rating Scale) for children over 7 years (7). Scoring was performed following completion of the procedure and inhalation of oxygen, when the children were no longer sedated.
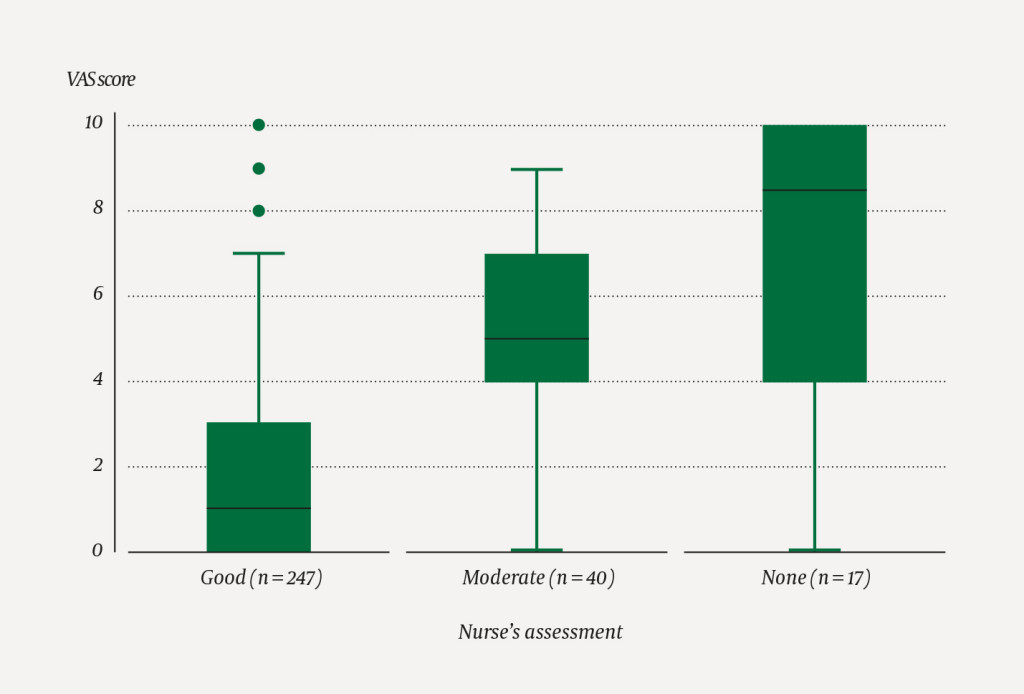
The nurse who performed the procedure rated its overall effectiveness as 'good', 'moderate' or 'none' based on their observations of how well the child coped with the procedure, pain before and afterwards, crying, facial expressions, fear and anxiety. Effectiveness was considered good if the patient reported feeling calm and comfortable during the procedure, the procedure was performed in full, and the patient and his or her guardians regarded the overall experience as positive.
A nurse and/or doctor retrospectively assessed whether the procedure would have been performed under general anaesthesia had nitrous oxide not been an option.
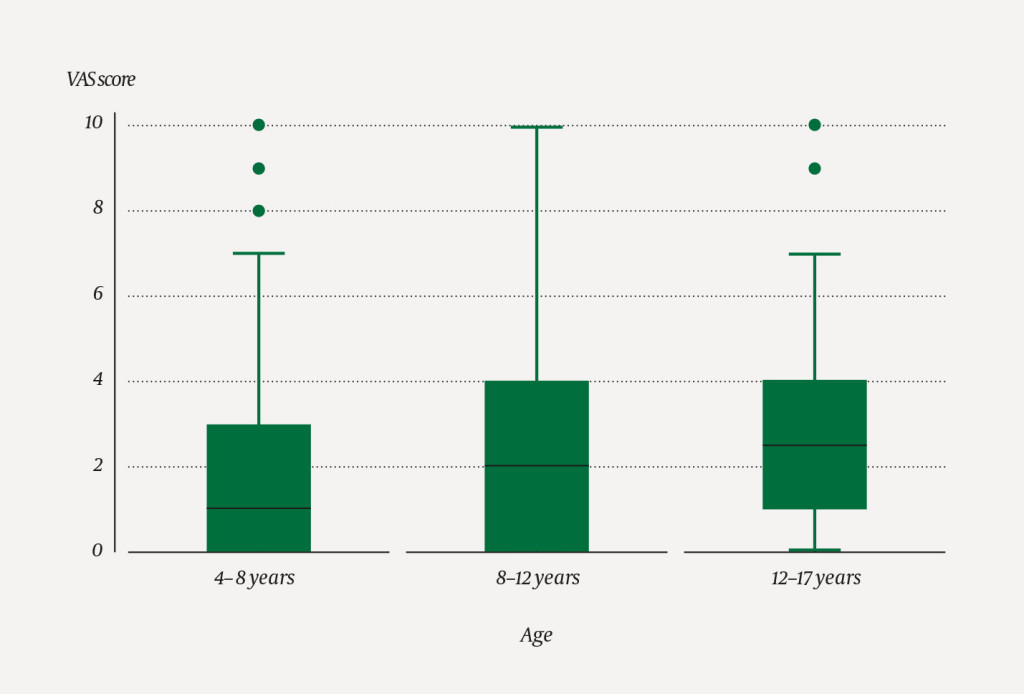
Data were recorded and summarised in Microsoft Excel 2013. Numerical data are given as medians, and categorical data are summarised as numbers and percentages. The relationship between the child's pain rating and the nurse's assessment is presented as a box plot for each age group.
The storage of anonymised data was approved by the Norwegian Centre for Research Data as part of an internal quality assurance study, and the study fell outside the scope of the Health Research Act. As a quality assurance study, the study was exempt from the requirement to seek approval from the Regional Committee for Medical and Health Research Ethics.
Results
A total of 311 procedures were performed on 238 patients. The median age was eight years (interquartile range 6–12), and 163 of 311 procedures (52 %) were on boys. The median procedure duration was ten minutes (interquartile range 6–15). Table 1 shows the distribution of procedure types, with orthopaedic interventions the most common, followed by lumbar puncture.
Table 1
Number and percentage of different procedures performed at the Department of Paediatric and Adolescent Medicine, Østfold Hospital Trust, in the period 13 July 2013–25 August 2017 with use of nitrous oxide for sedation. PEG = percutaneous endoscopic gastrostomy, CVC = central venous catheter.
| Procedure type |
No. (N = 311) |
Percentage (%) |
|
|---|---|---|---|
| Medical procedures |
|||
| Lumbar puncture |
47 |
15 |
|
| Enema/PEG replacement/CVC care/probe insertion |
28 |
9 |
|
| Injection of botulinum toxin |
31 |
10 |
|
| Venepuncture |
19 |
6 |
|
| Peripheral venous catheter insertion |
4 |
1 |
|
| Total |
129 |
41 |
|
| Orthopaedic procedures |
|||
| Setting of fractures and dislocations |
59 |
19 |
|
| Removal of osteosynthetic material |
53 |
17 |
|
| Suturing |
20 |
6 |
|
| Changing wound dressing |
20 |
6 |
|
| Removal of drain/foreign body/sutures |
13 |
4 |
|
| Other |
17 |
5 |
|
| Total |
182 |
59 |
|
Table 2 shows the drugs that were administered together with nitrous oxide. In 148 of 311 procedures (48 %), nitrous oxide was the only medication. In 91 of 311 procedures (31 %), nitrous oxide was used in combination with local anaesthesia. Longer procedures more often required opioid-based analgesia. The median duration of procedures in which opioids were used was 18 minutes (interquartile range 11–24) compared to 10 minutes for procedures without opioids (interquartile range 6–15).
Table 2
Supplementary medication in paediatric procedures involving use of nitrous oxide at Østfold Hospital Trust from 13 July 2013 to 25 August 2017. Number and percentage of all procedures.
| Type of supplementary medication |
Number of procedures |
Percentage (%) |
|---|---|---|
| None |
151 |
48 |
| Local anaesthesia |
97 |
31 |
| Local anaesthesia and non-opioid in combination |
24 |
8 |
| Paracetamol/NSAID |
17 |
5 |
| Opioid-based combinations |
14 |
4 |
| Benzodiazepines |
8 |
3 |
| Total |
311 |
100 |
The nurses rated the effectiveness of nitrous oxide as good in 247 of 304 (81 %) procedures (Figure 1). The median pain score reported by the child on a 10-point scale was 2 (interquartile range 0–4), and there was concordance between these two ratings, as shown in Figure 1. Effectiveness did not differ between age groups (<8, 8–12, and >12 years) (Figure 2).
Adverse effects were reported in 110 of 311 procedures (35 %). Minor adverse effects were dizziness in 66 of 311 procedures (21 %), nausea/vomiting in 12 of 311 procedures (4 %), and anxiety/euphoria/other in 25 of 311 procedures (8 %). In 7 of 311 procedures (2 %), serious adverse effects were recorded such as respiratory distress, bradycardia, deep sedation, decreased oxygen saturation, and seizures. These adverse effects led to stoppage of the procedure and halting of nitrous oxide inhalation, with a switch to 100 % oxygen.
In total, 286 of 311 procedures (92 %) were performed in full. Reasons for stoppage were inadequate cooperation with use of the mask, inhalation errors, mask leakage, anxiety, adverse effects, pain and because the procedure took longer than expected.
In all, it was felt that 134 of the 311 (43 %) procedures would have required general anaesthesia had nitrous oxide not been available. Of these procedures, 132 were surgical. Spread over 4.1 years, this represents an average of 33 fewer cases of general anaesthesia per year.
Discussion
This quality assurance study has shown that, on the whole, nitrous oxide was rated as highly effective by both nurses and children. However, certain adverse effects led to the delivery of nitrous oxide being halted.
Serious adverse effects were defined in this study as adverse effects that led to the delivery of nitrous oxide being halted. These adverse effects were managed by the nurse and doctor present, without it being necessary to summon anaesthesia personnel. As with all forms of sedation, careful monitoring of the use of nitrous oxide is important. We routinely administered oxygen for 3–5 minutes following the procedure to prevent diffusion hypoxia. Falling oxygen saturation during the procedure was observed in one case in our dataset, and in 0.1 % of procedures in the largest safety study conducted (10). In the Norwegian Institute of Public Health's technology assessment, none of the 525 adverse effects observed was considered serious according to standard definitions (8).
Dizziness, anxiety and euphoria were recorded as adverse effects in our study. These adverse effects are to be expected to some degree with sedation of this type. The incidence of nausea/vomiting in our dataset was comparable to that in the studies summarised in a health technology assessment by the Norwegian Institute of Public Health (8), although the incidence was higher in individual studies (14). Both the Norwegian Institute of Public Health's assessment and a review published in 2013 conclude that use of nitrous oxide in children is effective, safe and has few adverse effects (4).
In a safety study of 7 802 procedures on 5 779 children aged 1 month–18 years, adverse effects were reported in 4 % of cases, despite some use of nitrous oxide of a higher concentration (70 %) than in our study (50 %) (10). In our study, the risk of adverse effects increased with the length of the procedure.
The safety of employees who are regularly exposed to nitrous oxide is an important factor to consider when deciding whether nitrous oxide can be used in hospitals (15). Such safety concerns may be one reason why Norwegian hospitals use nitrous oxide to only a limited degree. Because nitrous oxide is released from the mask only upon inspiration, in theory there should be no leakage of nitrous oxide into the room from a securely-fitting mask. In addition, the procedures are short, in most cases less than 15 minutes, and a limited number of procedures are performed per day, often by different nurses. The safety of nitrous oxide for personnel is also supported by the previous health technology assessment (8), which found no evidence for an increased miscarriage rate in midwives/dental nurses. A risk of infertility was seen with high, but not low, levels of exposure, and congenital malformations were no more frequent among children born to exposed personnel.
Our quality assurance study, with a large number of procedures performed over a little more than four years, provides experience relevant to clinical practice. Data were collected prospectively and systematically. This results in better quality data than retrospective review of medical records, because it allows complete data to be obtained and is not dependent on making assumptions and interpreting information in medical records. Prospective recording also allows for subjective assessment of effectiveness.
We did not administer nitrous oxide to children younger than four years. We could therefore ensure that the child understood and was able to cooperate with the procedure and that the gas was administered through a securely-fitting mask. Studies have shown that nitrous oxide is safe for use in infants as young as one month, but the average age in these studies was 4–6 years (9, 10, 16, 17). We used nitrous oxide in children aged 4–17 years, and found that effectiveness varied little with age. The median age in our dataset was also higher than in the aforementioned studies. Nitrous oxide was tried when there was reason to believe that it would work well, thus all of our patients were pre-selected. In our experience, cooperation and acceptance of the mask are greater when the child understands the procedure well, and we have no plans to significantly change the lower age limit in our clinic.
In our study, nitrous oxide was administered and evaluated by well-trained nurses with expertise in monitoring sick children. The nurses' assessments may be influenced to some degree by prior expectations of a beneficial effect. Nevertheless, the children's experiences were highly consistent with the nurses' assessments, and both were mainly positive. One of the effects of nitrous oxide on children may be mild euphoria and indifference, which can affect pain scoring. However, concordance between the nurses' and the children's assessments helps increase confidence in the ratings.
We did not compare different methods of sedation in our study. However, nitrous oxide was compared with other sedation methods and with placebo in the recently published health technology assessment (8), which included a total of 22 randomised studies. Nitrous oxide was deemed to be as effective as other methods of sedation and more effective than placebo; shorter duration of sedation was also highlighted as an advantage of nitrous oxide (8). Nitrous oxide is a good alternative to agents such as midazolam, not least because a rapid onset of action and faster elimination time are advantageous both for children and for busy hospital personnel (2, 18).
Many of the procedures in our study are relatively simple and do not require general anaesthesia. Nevertheless, our results show that a number of surgical and orthopaedic procedures in which general anaesthesia would normally be used, could in fact be performed with nitrous oxide. As nitrous oxide is considered to be effective, there is an argument for using it in combination with effective pain relief for shorter procedures, instead of general anaesthesia. However, nitrous oxide often has an insufficient analgesic effect, and supplementary medication such as local anaesthesia, non-opioid analgesics or opioids may be required. Our usual practice is therefore to offer nitrous oxide as an alternative to midazolam. Effective pain relief during the procedure is important with both types of sedative.
Conclusion
This study has thus shown that nitrous oxide works well as a sedative on the ward and in the outpatient clinic. It was easy to administer, most adverse effects were mild, and it was highly effective in all age groups examined. Nitrous oxide can be administered by existing personnel with proper training.
We wish to thank the nurses and doctors at the Orthopaedics and Trauma Clinic for data collection and for helpful comments regarding data interpretation, and the doctors and nurses at the Department of Paediatric and Adolescent Medicine for data collection.
This article has been peer-reviewed.
- 1.
von Baeyer CL, Marche TA, Rocha EM et al. Children's memory for pain: overview and implications for practice. J Pain 2004; 5: 241–9. [PubMed][CrossRef]
- 2.
Noel M, Chambers CT, McGrath PJ et al. The influence of children's pain memories on subsequent pain experience. Pain 2012; 153: 1563–72. [PubMed][CrossRef]
- 3.
Taddio A, Katz J, Ilersich AL et al. Effect of neonatal circumcision on pain response during subsequent routine vaccination. Lancet 1997; 349: 599–603. [PubMed][CrossRef]
- 4.
Pedersen RS, Bayat A, Steen NP et al. Nitrous oxide provides safe and effective analgesia for minor paediatric procedures–a systematic review. Dan Med J 2013; 60: A4627. [PubMed]
- 5.
Peters U, Schneeweiss S, Trautwein EA et al. A case-control study of the effect of infant feeding on celiac disease. Ann Nutr Metab 2001; 45: 135–42. [PubMed][CrossRef]
- 6.
Blumer JL. Clinical pharmacology of midazolam in infants and children. Clin Pharmacokinet 1998; 35: 37–47. [PubMed][CrossRef]
- 7.
von Baeyer CL, Spagrud LJ, McCormick JC et al. Three new datasets supporting use of the Numerical Rating Scale (NRS-11) for children's self-reports of pain intensity. Pain 2009; 143: 223–7. [PubMed][CrossRef]
- 8.
Tjelle TE, Pike E, Hafstad E et al. Health technology assessments – effectiveness and safety of nitrous oxide as sedation regiment in children. Oslo: Folkehelseinstittutet, 2018. https://www.fhi.no/publ/2018/metodevurdering-av-sikkerhet-og-effekt-ved-bruk-av-lystgass-for-barn/ Lest 15.2.2019.
- 9.
Zier JL, Rivard PF, Krach LE et al. Effectiveness of sedation using nitrous oxide compared with enteral midazolam for botulinum toxin A injections in children. Dev Med Child Neurol 2008; 50: 854–8. [PubMed][CrossRef]
- 10.
Zier JL, Liu M. Safety of high-concentration nitrous oxide by nasal mask for pediatric procedural sedation: experience with 7802 cases. Pediatr Emerg Care 2011; 27: 1107–12. [PubMed][CrossRef]
- 11.
Messeri A, Amore E, Dugheri S et al. Occupational exposure to nitrous oxide during procedural pain control in children: a comparison of different inhalation techniques and scavenging systems. Paediatr Anaesth 2016; 26: 919–25. [PubMed][CrossRef]
- 12.
Medscape. Nitrous Oxide Administration – contraindication. https://emedicine.medscape.com/article/1413427-overview Lest 15.2.2019.
- 13.
Hicks CL, von Baeyer CL, Spafford PA et al. The Faces Pain Scale-Revised: toward a common metric in pediatric pain measurement. Pain 2001; 93: 173–83. [PubMed][CrossRef]
- 14.
Bar-Meir E, Zaslansky R, Regev E et al. Nitrous oxide administered by the plastic surgeon for repair of facial lacerations in children in the emergency room. Plast Reconstr Surg 2006; 117: 1571–5. [PubMed][CrossRef]
- 15.
Eftimova B, Sholjakova M, Mirakovski D et al. Health effects associated with exposure to anesthetic gas nitrous oxide-n2o in clinical hospital – Shtip personel. Open Access Maced J Med Sci 2017; 5: 800–4. [PubMed][CrossRef]
- 16.
Luhmann JD, Kennedy RM, Porter FL et al. A randomized clinical trial of continuous-flow nitrous oxide and midazolam for sedation of young children during laceration repair. Ann Emerg Med 2001; 37: 20–7. [PubMed][CrossRef]
- 17.
Rao J, Kennedy SE, Cohen S et al. A systematic review of interventions for reducing pain and distress in children undergoing voiding cystourethrography. Acta Paediatr 2012; 101: 224–9. [PubMed][CrossRef]
- 18.
Norsk legemiddelhåndbok. L22.2.1.1 Dinitrogenoksid. https://www.legemiddelhandboka.no/L22.2.1.1/Dinitrogenoksid Lest 15.2.2019.