Main message
The prevalence of unwanted sexual attention among doctors in Norway increased from 1993 to 2014/15
Female gender and young age increased the likelihood of experiencing unwanted sexual attention
Future studies should identify those responsible for unwanted sexual attention, its degree of seriousness and consequences for the individuals concerned and the working environment
In the wake of the #MeToo online campaign, media reports about sexual harassment and unwanted sexual attention have shaken organisations and workplaces across the world (1). In December 2017, more than 3 600 women doctors and medical students signed a petition against unwanted sexual attention in the Aftenposten daily. They referred to how one in every five women doctors in a Facebook group reported personal experience of work-related abuse or sexual harassment (2).
Statistics Norway's (SSB) living conditions surveys show that the proportion of gainfully employed persons who had experienced unwanted sexual attention at least a couple of times every month increased during the period 1989–2016, from 4 % to 7 % among women and from 1 % to 2 % among men. The highest rates of occurrence were found among young employees and among employees on shift or rota work, and in the culture, sports, nursing and care sectors (3).
Harassment and bullying in the workplace cause a higher incidence of mental afflictions, stress reactions, sickness absence and reduced job satisfaction (4–6). A meta-analysis of 41 studies of the consequences of unwanted sexual attention found associations with reduced satisfaction, less organisational participation, higher rates of sickness absence and mental ill-health (7).
Norwegian legislation regulates workplace behaviour, including unwanted sexual attention. The Equality and Anti-Discrimination Act prohibits sexual harassment, defined as 'any form of unwanted sexual attention that has the purpose or effect of being offensive, frightening, hostile, degrading, humiliating or troublesome' (8). The Working Environment Act states that the employer shall 'secure a working environment that provides a basis for a healthy and meaningful working situation' (9), and the Norwegian Medical Association's Code of Ethics states that doctors should show their colleagues and co-workers respect and help, advise and guide them (10).
The #MeToo campaign has cast necessary light on unwanted sexual attention. There is a major commitment behind the statements made about this in the media, but the figures are not reliably representative for the occupational groups described. We therefore wished to investigate the perception and development of unwanted sexual attention in representative samples of doctors – from prior to the #MeToo campaign.
Material and method
The data are drawn from surveys in two independent and approximately representative samples of working doctors: a study of the working conditions of doctors conducted by the Institute for Studies of the Medical Profession in 1993 and the Doctors Panel in 2014/15, both described in detail in previous studies (11, 12). In their identification of experiences of violence, bullying and harassment in the workplace, both surveys included a question about unwanted sexual attention. In 1993, the question was phrased: 'Does it happen that you are exposed to unwanted sexual attention, comments or similar?' The 2014/15 survey used the same question, but added 'in the workplace setting'. The response alternatives ranged from 'no' to 'yes, on a daily or near-daily basis' (Table 1). Gender and age were registered.
Table 1
Proportion of doctors who had experienced unwanted sexual attention in 1993 and 2014/15, percentages
| 1993 |
2014/15 |
|||||
|---|---|---|---|---|---|---|
| Does it happen that you are exposed to unwanted sexual attention, comments or similar? |
Does it happen that you are exposed to unwanted sexual attention, comments or similar in the workplace setting? |
|||||
| Women |
Men |
Total |
Women |
Men |
Total |
|
| No |
94.8 |
98.3 |
97.3 |
92.2 |
97.8 |
95.4 |
| Yes, up to a couple of times per month |
5.0 |
1.5 |
2.6 |
6.8 |
1.7 |
3.9 |
| Yes, approximately once per week |
0.1 |
0.1 |
0.1 |
1.0 |
0.5 |
0.7 |
| Yes, a couple of times per week |
0.0 |
0.1 |
0.0 |
0.0 |
0.0 |
0.0 |
| Yes, on a daily or near-daily basis |
0.1 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
We used proportions to describe the central tendency and to compare gender and age groups. Statistical significance was assessed in light of overlapping 95 % confidence intervals. A concurrent effect of gender and age on experience of unwanted sexual attention was assessed by logistic regression models. Returned questionnaires that had no information on gender, age or experience of unwanted sexual attention were excluded from the analyses. We used Predictive Analytics statistics software, version 23.
Results
The respondents
The samples encompassed 2 628 (72.8 %) respondents in 1993 and 1 261 (78.2 %) in 2014/15, whereof 41 and 153 respectively had not answered questions about unwanted sexual attention, gender and age, and were excluded from the analyses.
The proportion of women increased from 28.9 % (95 % CI 27.2–30.7; n = 748) in 1993 to 42.6 % (95 % CI 39.7–45.5; n = 472) in 2014/15. Average age was 42.2 years (95 % CI 41.8–42.6) in 1993 and 48.5 years (95 % CI 47.9–49.2) in 2014/15, range 25–69. The majority were working full-time in hospitals (data not shown).
Experience of unwanted sexual attention
Table 1 shows the frequencies of unwanted sexual attention experienced by female and male doctors in 1993 and 2014/15. There was a slight increase in the responses 'yes, up to a couple of times per week' and 'yes, approximately once per week', while 'yes, a couple of times per week' and 'yes, on a daily or near-daily basis' were reported by two doctors in 1993 and none in 2014/15.
There was a significant increase in the proportion that had experienced unwanted sexual attention at least a couple of times per month, from 2.7 % (95 % CI 2.1–3.3) in 1993 to 4.6 % (95 % CI 3.4–5.8) in 2014/15. Among women, there was an increase from 5.2 % (95 % CI 3.6–6.8) to 7.8 % (95 % CI 5.4–10.2) and among men from 1.7 % (95 % CI 1.1–2.3) to 2.2 % (95 % CI 1.1–3.3), but these were not statistically significant (Figure 1).
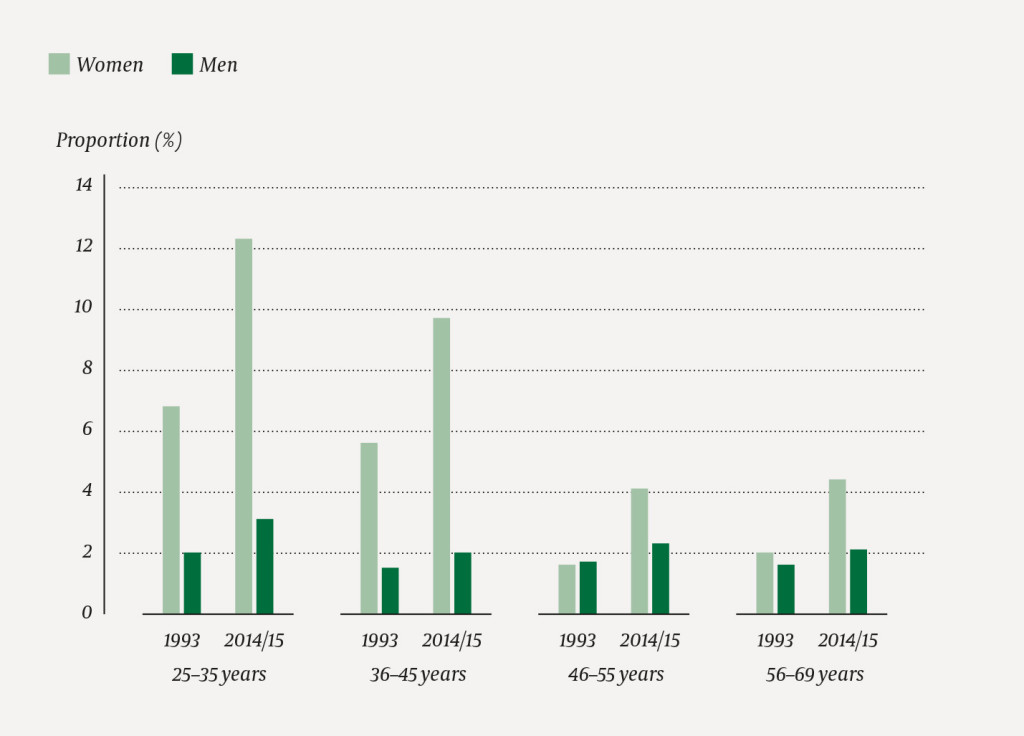
Age and gender
The logistic regression analyses in Table 2 show that female gender, both in 1993 and 2014/15, and young age in 2014/15, were statistically significant predictors of unwanted sexual attention.
Table 2
Effect of gender and age on unwanted sexual attention experienced up to at least a couple of times per month or more often among doctors in Norway in 1993 and 2014/15
| 1993 |
2014/15 |
|||
|---|---|---|---|---|
| OR (95 % CI) |
P-value |
OR (95 % CI) |
P-value |
|
| Gender |
||||
| Male |
1 |
1 |
||
| Female |
2.88 (1.75–4.73) |
< 0.001 |
3.03 (1.59–5.78) |
< 0.001 |
| Age (years) |
0.98 (0.95–1.01) |
0.11 |
0.96 (0.94–0.99) |
0.01 |
Discussion
The study shows that the proportion of doctors reporting to have been exposed to unwanted sexual attention increased from 1993 to 2014/15. Over the period, there was a tendency towards an increase in all age groups and both genders, but the figures were too small to permit any firm conclusions. Women were more exposed than men, and younger women were more exposed than older women.
Comparisons
In November 2017, 40 per cent of a random sample of Swedish female doctors reported to have been exposed to sexual harassment or abuse by patients, colleagues or superiors (13), and in an article in the Aftenposten daily in December 2017, 20 per cent of the members of a Facebook group of female doctors reported to have been exposed to sexual abuse or harassment from healthcare service employees (2). The difference in incidence, both between these two studies and in relation to our figures, may be due to a number of issues.
Increasing awareness of this topic in the wake of the #MeToo campaign and a lowered reporting threshold may probably help explain the higher incidence in these two studies when compared to data from 2015.
The differences may also be due to the fact that unwanted sexual attention was measured differently in these studies. Previous studies show, for example, that a direct question of exposure to unwanted sexual attention (with or without a definition of what this implies) returns a lower incidence rate than a concrete question that refers to exposure to a range of specifically defined comments and actions (14, 15).
Nor are the two reports from 2017 necessarily representative of doctors as a group in Norway or Sweden. Previous studies have shown that research on unwanted sexual attention is especially vulnerable to reporting bias, both because of the difficulty involved in defining the concepts and the dearth of representative samples (14).
Most likely, the differences between the Norwegian and Swedish figures from 2017 are also related to whether this harassment or abuse was committed by colleagues, vs. by colleagues and patients/clients. The Living Conditions Survey 2016 reported that 79 per cent of the unwanted sexual attention stemmed from customers, clients, students or other non-employees, 20 per cent from colleagues and 6 per cent from superiors.
Measures against unwanted sexual attention must be adapted to whether it is committed by employees or non-employees. In future studies, it will be crucial to distinguish between these groups in order to provide employers, trade union representatives and the medical profession as a whole with a better basis for choosing necessary measures to reduce unwanted sexual attention.
Since our question about experience of unwanted sexual attention is directly comparable to the one posed in Statistics Norway's living conditions survey regarding the working environment ('Exposed to unwanted sexual attention, comments or similar, a couple of times per month or more often') (3), we can see that the incidence among doctors was fairly similar to the incidence in the population in general in 2014, for women (7.8 % vs. 7.0 %) as well as for men (2.2 % vs. 2.0 %) (3).
Over the last 20 years, including before the #MeToo campaign, we can see an increase in the occurrence of unwanted sexual attention, especially among women (doctors from 5.2 % to 7.8 % and in the general population from 4.0 % to 7.0 %). This could be due to a gradual change in attitudes and attention to this, and may thus be an expression of changes in the understanding of the phenomenon. On the other hand, in the same period we can find no corresponding change in the incidence of bullying or violence, which we identified in parallel (12, 16).
According to Statistics Norway, nurses constitute the group which is most frequently exposed to unwanted sexual attention (3). The major difference between the proportion of nurses (17 %) and female doctors (7.8 %) may be related to differences in the rate of contact with patients, clients or their next of kin. As described above, studies indicate that the occurrence of unwanted sexual attention is higher in occupations with extensive contact with customers or users (4).
Workplace culture
In similarity to other types of violence and harassment (4–6), studies show that unwanted sexual attention and sexual harassment are related to mental health problems and low job satisfaction (7, 14). It might thus be relevant to consider unwanted sexual attention in the context of wider issues pertaining to a negative culture in which bullying, exclusion and violence may occur (4). A Swedish study from 2017 showed that the choice of specialty by young doctors, especially female doctors, could be affected by a perception of the working environment in the department in question as exclusionary and characterised by a macho culture, in combination with unwanted sexual attention (17). In Norway as well, there are studies indicating that a negative workplace culture might have an effect on the choice of specialty (18), and we should investigate whether unwanted sexual attention might be an element of this picture.
Gender differences
Like many studies, the #MeToo campaign has mainly focused on sexual harassment of women by men. Our study shows that men also report unwanted sexual attention, and the topic is therefore salient for both genders.
In a representative sample of the Norwegian population and with questions similar to those in our study, a ratio of 3:1 was found between the rates of occurrence among women and men (14). This is equivalent to what was found in our study. In the same sample, however, no gender differences were found in the number of perceived comments and actions (later defined by the authors as unwanted sexual attention). The study discusses a number of possible reasons for this observation. A key question is whether exposure to specifically defined comments and actions is harmful if these are not perceived as unwanted by those concerned (14). Men might feel it as more threatening for their self-esteem to define themselves as victims of unwanted sexual attention, and thus deliberately or unconsciously underreport incidents. On the other hand, identical comments may be perceived as more threatening or offensive by a woman than by a man (14). The degree of offense or threat may also be influenced by age and position, and may be a key explanation why women perceive more unwanted sexual attention than men, even though the number of experiences of comments and actions may be the same.
In our samples, the proportion of female doctors increased from 29 % to 43 % from 1993 to 2014/15, and now exceeds 50 % in Norway (19). It is essential to monitor further developments in unwanted sexual attention among female and male doctors alike, in light of the changed gender balance.
Strengths and weaknesses
The strengths of this study consist in its representative sample of doctors and relatively high response rate, which result in reliable data. In addition, use of the same questions as those of Statistics Norway (3) provides an opportunity for comparisons with the population in general and between different occupational groups.
A crucial limitation lies in the lack of a definition of what unwanted sexual attention means in the questionnaire, as well as the absence of information on those responsible for the unwanted sexual attention (superiors, colleagues, patients, others) and the degree of seriousness of their actions. As discussed above, the phrasing of the question has a major impact on the incidence of unwanted sexual attention detected (14, 15).
Despite this uncertainty with regard to the point prevalence, use of the same question at different times and in different groups will be able to show any changes that occur over time, as well as differences between genders and occupational groups.
A more detailed analysis of data by specialty and job category was impossible because of the relatively low proportion that reported unwanted sexual attention.
In 2014/15, we used the same question as in 1993, but added 'in a workplace setting'. This potential narrowing down of the question in 2014/15 may have resulted in lower reporting. On the other hand, in both studies the question was placed in a section comprising issues related to violence and bullying in the workplace. Most likely, the question has thus been interpreted identically on both occasions. Moreover, the question was not specified in terms of a reference period. Since the immediately preceding question referred to occurrence of bullying over the last year, it is likely that the question about unwanted sexual attention was also interpreted as referring to experiences over the last year.
Conclusion
We found an increase in the rates of reported unwanted sexual attention among Norwegian doctors from 1993 to 2014/15. The higher risk of exposure to unwanted sexual attention among women and the increasing proportion of women in the medical profession highlights the need to enact measures to reduce this occurrence. The phenomenon should be regularly monitored, precisely specifying those responsible for this unwanted sexual attention, its degree of seriousness and consequences of the incidents. In the healthcare sector as a whole, where there are groups of professions that report even higher rates of occurrence of unwanted sexual attention than doctors, it is essential to obtain a better understanding of this phenomenon, improve the accuracy of measures enacted and enhance the follow-up of those who have been exposed to such incidents.
- 1.
Lønning KJ. Ringer i vannet etter #Metoo. Dagens Medisin 11.1.2018. https://www.dagensmedisin.no/artikler/2018/01/11/ringeri-vannet-etter-metoo/ (28.2.2018).
- 2.
#utentaushetsplikt: 3600 norske leger og medisinstudenter bryter tausheten. Vil stoppe trakassering og maktmisbruk. Aftenposten 7.12.2017. https://www.aftenposten.no/article/ap-VRbQm6.html (28.2.2018).
- 3.
Statistisk sentralbyrå. Levekårsundersøkelsen: Arbeidsmiljø. Statistikkbanken. https://www.ssb.no/statbank/list/arbmiljo?rxid=3a56e123-4959-4de1-891d-d3c7e242d660 (28.2.2018).
- 4.
Normann TM, Rønning E. Konflikter, mobbing, trakassering og vold i arbeidslivet. Få utsatte, noen yrker mer utsatt enn andre. Samfunnsspeilet 2007; nr. 4: 62–71.
- 5.
Taniguchi T, Takaki J, Hirokawa K et al. Associations of workplace bullying and harassment with stress reactions: a two-year follow-up study. Ind Health 2016; 54: 131 - 8. [PubMed][CrossRef]
- 6.
Niedhammer I, Chastang JF, Sultan-Taïeb H et al. Psychosocial work factors and sickness absence in 31 countries in Europe. Eur J Public Health 2013; 23: 622 - 9. [PubMed][CrossRef]
- 7.
Willness CR, Steel P, Lee K. A meta-analysis of the antecedents and consequences of workplace sexual harassment. Person Psychol 2007; 60: 127 - 62. [CrossRef]
- 8.
LOV-2017-06-16-51. Lov om likestilling og forbud mot diskriminering (likestillings- og diskrimineringsloven): § 13.
- 9.
LOV-2005-06-17-62. Lov om arbeidsmiljø, arbeidstid og stillingsvern mv. (arbeidsmiljøloven).
- 10.
Den norske legeforening. Etiske regler for leger: kapittel II §1. https://legeforeningen.no/Om-Legeforeningen/Organisasjonen/Rad-og-utvalg/Organisasjonspolitiske-utvalg/etikk/etiske-regler-for-leger/ (23.7.2018).
- 11.
Aasland OG, Olff M, Falkum E et al. Health complaints and job stress in Norwegian physicians: the use of an overlapping questionnaire design. Soc Sci Med 1997; 45: 1615 - 29. [PubMed][CrossRef]
- 12.
Rosta J, Aasland OG. Perceived bullying among Norwegian doctors in 1993, 2004 and 2014-2015: a study based on cross-sectional and repeated surveys. BMJ Open 2018; 8: e018161. [PubMed][CrossRef]
- 13.
Wihlborg A. 40% av kvinnliga läkare utsatta för sexuella trakasserier. Framtidens karriär – Läkare. http://karriarlakare.se/artikel/40-av-kvinnliga-lakare-utsatta-for-sexuella-trakasserier/ (28.2.2018).
- 14.
Nielsen MB, Bjørkelo B, Notelaers G et al. Sexual harassment: Prevalence, outcomes, and gender differences assessed by three different estimation methods. J Aggress Maltreat Trauma 2010; 19: 252 - 74. [CrossRef]
- 15.
Stark S, Chernychenko OS, Lancaster AR et al. Toward standardized measurement of sexual harassment: Shortening the SEQDoD using Item Response Theory. Mil Psychol 2002; 14: 49 - 72. [CrossRef]
- 16.
Johansen IH, Baste V, Rosta J et al. Changes in prevalence of workplace violence against doctors in all medical specialties in Norway between 1993 and 2014: a repeated cross-sectional survey. BMJ Open 2017; 7: e017757. [PubMed][CrossRef]
- 17.
Diderichsen S. It's just a job. A new generation of physicians dealing with career and work ideals. Doktoravhandling. Umeå: Institutionen för folkhälsa och klinisk medicin, Universitetet i Umeå, 2017. http://umu.diva-portal.org/smash/get/diva2:1145048/FULLTEXT01.pdf (28.02.18).
- 18.
Gjerberg E. Gender similarities in doctors' preferences–and gender differences in final specialisation. Soc Sci Med 2002; 54: 591 - 605. [PubMed][CrossRef]
- 19.
Den norske legeforening. Alle yrkesforeninger samlet – medlemstall. http://legeforeningen.no/Emner/Andre-emner/Legestatistikk/Medlemsstatistikk/Yrkesforeninger/Alle-yrkesforeninger-samlet-medlemstall/ (11.2.2018).