Main message
We found that many sustained frostbite during military service
One in five persons with frostbite reported to suffer from chronic health problems that affected their quality of life and ability to work
A follow-up prospective study might provide further knowledge about the incidence of frostbite
More research, especially on injuries in young conscripts, would provide an important basis for further preventive efforts in the Armed Forces
Historically, hypothermia, cold injuries and frostbite have claimed many human lives and inflicted debilitating injuries on a considerable number of military personnel. In the Great Northern War in the 18th century, cold weather was probably the greatest challenge during General Armfeld's retreat, later known as the 'Death March', where half of his army succumbed to the cold (1). In 1982, a considerable number of British special forces personnel sustained frostbite during the Falklands War (2).
Today, the Norwegian Armed Forces act as a centre of excellence in relation to frostbite within NATO, Center of Excellence – Cold Weather Operations (3), and a large number of foreign troops undertake winter training in Norway, including in the Armed Forces School of Winter Operations. Army personnel and conscripts nevertheless sustain frostbite during exercises and other service. Although the quality of equipment and clothing is excellent, the Armed Forces' annual reports confirm that a considerable number of injuries and health problems occur as a result of military activity, especially winter exercises (4).
Published literature on the diagnosis of cold injuries and frostbite has a varying level of precision. The confusion around terminology has a number of reasons. For example, cold injuries and frostbite are divided among several specialties, little research has been undertaken in this area and there is little correspondence between the terminology used in different countries. The distinction between different types of injuries, the degree of severity, treatment and prognosis is made even more challenging since the term 'cold weather injury' (CWI) is commonly used in international medical literature.
The term 'cold weather injury' is imprecise and sometimes encompasses three quite different injuries (5):
-
frostbite (tissue temperature below -0.55 °C)
-
cold injury (hypothermic peripheral tissue, but with temperatures above the freezing point of the tissue: -0.55 °C)
-
general hypothermia (the core temperature of the body falls below 35.0 °C).
In principle, frostbite occurs in temperatures below the freezing point of the tissue, which is -0.55 °C (6, 7). Below this temperature cell damage occurs with a subsequent inflammation process and disruption of the local microcirculation. Local frostbite with a specific 'frostbite pathophysiology' does not occur in temperatures above the freezing point of the tissue. International medical literature uses the term 'frostbite' and 'freezing cold injuries' (FCI) to denote such injuries. In the Norwegian nomenclature, we should use 'frostskade' (frostbite) consistently wherever symptoms and findings indicate that the tissue temperature has dropped below -0.55 °C.
Cold injuries develop when the peripheral skin on the extremities is exposed to high levels of moisture in combination with cooling, commonly approaching but not falling below the freezing point of the tissue (8). Cold injuries commonly occur at temperatures down to 0 °C. However, lengthy exposure to moisture in combination with ambient temperatures as high as 20 °C may also result in 'cold-injury pathophysiology', especially neuropathy. Cold injuries may in principle affect any part of the body, but occurs most frequently on the feet, hence the historical names of 'trench foot' or 'lifeboat foot'. International medical literature tends to use the term 'non-freezing cold injuries' (NFCI) to refer to cold injuries. In the Norwegian nomenclature we should be specific and use the term 'kuldeskade' (cold injury) where symptoms and findings indicate that the tissue temperature has been lowered, but not below the freezing point of tissue.
Hypothermia is defined as a lowering of the body's core temperature to below 35 °C. Traditionally, hypothermia has been divided into mild, moderate and severe forms (9). A lowering of the body's core temperature by 1–2 degrees may cause drowsiness and disruption of bodily functions, while a lowering by 4–5 degrees may be fatal (10). Severe hypothermia may frequently be life-threatening (arrhythmia) in otherwise healthy patients. In case of trauma or other co-morbidity, mild hypothermia will often be life-threatening, for example as a result of bleeding. New clinical recommendations for treatment of patients with lowered core temperature emphasise reporting of consciousness, shivering, respiration and pulse rate for selection of an appropriate level of treatment (11). The new clinical recommendations are divided into four levels (mild, moderate, severe, deep) and comply with international standards (12).
When tissue is exposed to temperatures below the freezing point of the skin (-0.55 °C), ice crystals may form within the cells. The ice crystals rupture the cells and blood vessels and cause cell death. When only the skin surface is frozen, a white patch ('chilblain') is observed, which normally will be a Grade 1 frostbite (13). If the frostbite continues, deeper layers of the skin can become affected and oedemas and blisters may appear, possibly indicating a Grade 2 frostbite. If the injury develops further, a deeper frostbite will occur in tissue below the level of the skin (14).
A considerable proportion of patients with peripheral frostbite suffer permanent changes in their microcirculation and disruption of neurological functions. Depending on the extent of injury, general functioning and ability to work may be impaired by vasospasm, hypersensitivity to cold, pain and hyperhidrosis (15). Permanent paraesthesia involving sensations of electric shock (16), growth-plate disruptions and osteoarthritis may exacerbate the course of illness (13, 17).
A possible challenge in diagnosing mild frostbite (Grade 1) could be that the symptoms fluctuate, making an exact diagnosis difficult. For severe frostbite (Grades 2–4), somewhat clearer clinical criteria are provided (16) (Table 1).
Table 1
Clinical criteria and levels of frostbite (7, 14, 16)
| Symptoms and findings | Morphology/level | ||
|---|---|---|---|
| Superficial frostbite | Grade 1 | Reddish skin, swelling, numbness, stinging discomfort ('frostnip'), white patches ('chilblains') | Partial intradermal frostbite |
| Grade 2 | Pronounced hyperaemia, blisters filled with clear fluid, superficial erosions, severe pain (gradually reduced sense of pain) | Complete dermal frostbite | |
| Deep frostbite | Grade 3 | Blisters filled with bloody fluid, bluish-white discoloration of the skin, necrosis, significantly reduced sensation of pain | Injury down to the subcutaneous tissue |
| Grade 4 | Deep red/bluish-black discoloration of the skin, skin is firm and immobile, full- thickness oedema, tissue necrosis, no sensation of pain | Injury to muscles and bone | |
In addition to preventive measures, the literature also describes initial emergency treatment and recommendations for further clinical follow-up and therapy. However, the prognosis and long-term course of severe frostbite has not previously been investigated in larger cohorts.
The Armed Forces Health Registry is a central health registry (18) that contains data from Armed Forces personnel (9), including conscripts as well as civilian and military staff employed by the Armed Forces. The objective of the registry is to identify risks linked to the different services and provide a basis for research and statistics on the health of Armed Forces personnel. The types of personal data that can be processed are defined by Section 1–8 of the Regulations concerning the collection and processing of information in the Armed Forces Health Registry (19).
Pursuant to the regulations, the registry may contain personal information, administrative information, medical information and workplace information. The information in the Armed Forces Health Registry is drawn from Armed Forces medical records and HR systems, as well as internal health surveys. The Ministry of Defence is the data controller and the Armed Forces Medical Services is the data processor. Medical and operational responsibility lies with the Institute of Military Medicine and Epidemiology, Norwegian Armed Forces Joint Medical Service, at Sessvollmoen camp.
Data from the health registry contribute increasingly to research seeking to identify health injuries during, or as a consequence of, military service (20–22). A separate module of the SANDOK patient records system has been developed to collect data on illness, injury and death.
In this study, we will investigate how many of those who are registered in the Armed Forces Health Registry with frostbite that occurred during military service can confirm that they sustained this injury. Furthermore, we will investigate the degree of frostbite, the location of the injury, activities at the time of injury and the long-term course of illness.
Material and method
The study is based on self-reported data from those who are identified in the Armed Forces Health Registry with the ICD codes T33, T34, T35, T68 and T69 having occurred during military service in the period 1 January 2010–31 December 2014. Experience indicates that diagnostic code T68/T69 (hypothermia/other condition caused by reduced temperature) has been wrongly entered for patients with frostbite. Persons coded with T68 and T69 in the Armed Forces Health Registry during the study period are included in the survey sample. Data were collected as part of quality assurance of data in the Armed Forces Health Registry and follow-up of personnel that had sustained frostbite during military service.
In the period 1 January 2010–31 December 2014, a total of 810 people were registered with cold injuries and frostbite in the Armed Forces Health Registry. Individuals suffering from cold injuries and frostbite in the Armed Forces Health Registry come from all service branches and include officers and enlisted personnel in regular service, military winter exercises and military operations.
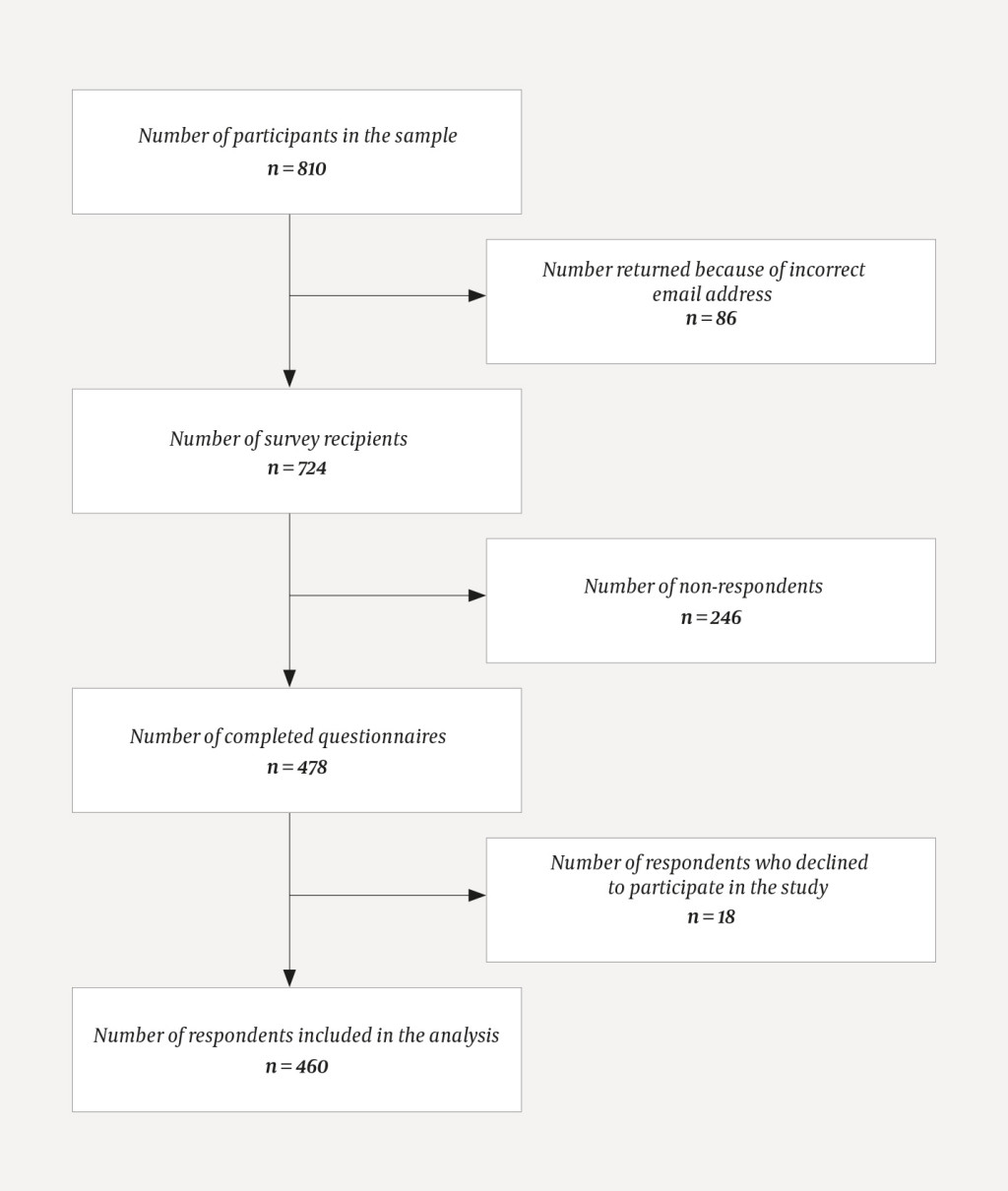
In March 2017, a questionnaire developed by the authors was sent to these persons using email addresses in the Armed Forces Health Registry. The questionnaire was designed on the basis of experience gained from treating frostbite during national service in the winter of 2014/2015 (23). The questionnaire was distributed and completed with the aid of the Confirmit online tool (24). Reminders were sent out one and three weeks after distribution. The number of questionnaires sent out and returned as well as the final response rate are shown in the flowchart (Figure 1).
The participants in the study were asked whether they had sustained frostbite during military service, what they were doing at the time of injury, what part of their body was affected, whether they had sustained frostbite with blisters, how the frostbite had developed and whether they had received any medical treatment for their frostbite (see appendix).
The study is primarily of a descriptive nature, with few presentations of statistical estimates. To compare categorical data we use chi-square analysis with a significance level of 0.05. To estimate the risk of frostbite among conscripts we use figures for the number of soldiers who completed national military service.
Results
A total of 478 of the 724 people who received the questionnaire returned a completed response, equal to a response rate of 66 %. Eighteen respondents did not wish to participate in the study. Of those 460 persons who answered the questions in the questionnaire, 397 persons (86.3 %) confirmed that they had sustained frostbite during military service in the five-year period of the study. Thirty persons (6.5 %) reported having not sustained any frostbite during service, while 33 persons (7.1 %) did not know whether they had sustained frostbite during their national service.
Most of those who confirmed that they had been injured were men (80.4 %), and the majority (90.9 %) of these were 22 years old or younger at the time of injury. Approximately two-thirds of all those injured (67.3 %) were conscripts (Table 2).
Table 2
Background variables for 397 persons who confirmed that they had sustained frostbite during military service in the period 1 January 2010–31 December 2014
| N = 397 | (%) | |||
|---|---|---|---|---|
| Gender | Woman | 78 | (19.6) | |
| Man | 319 | (80.4) | ||
| Age at the time of injury | Mean | 20 years, 11 months | ||
| Median | 20 years | |||
| (min–max) | (19–41) | |||
| Type of service | National service | 267 | (67.2) | |
| Officer candidate school | 69 | (17.4) | ||
| Officer | 32 | (8.1) | ||
| Other service | 29 | (7.3) | ||
| Year of injury | 2010 | 95 | (24.0) | |
| 2011 | 62 | (15.6) | ||
| 2012 | 77 | (19.4) | ||
| 2013 | 91 | (22.9) | ||
| 2014 | 72 | (18.1) |
Among those 397 persons who confirmed that they had sustained frostbite, a total of 123 (31.0 %) reported to have had blisters, which may give rise to suspicion of second-degree frostbite. The majority (56.8 %) reported to have sustained frostbite, but without blisters, most likely an indication of first-degree frostbite. A smaller proportion (12.1 %) did not know whether they had had any blisters or not. It seems reasonable to assume that the latter group most likely had not sustained any such injury.
Blisters occurred with equal frequency in men and women, 31.3 % and 29.9 % respectively. Blisters were equally common in conscripts (32.0 %) and officers (34.4 %), but twice as many conscripts as officers did not know whether they had suffered from blisters or not (14.3 % versus 6.3 %). The vast majority (n = 322) sustained their frostbite during field/winter exercises (81.1 %).
By far the majority had sustained injuries to their fingers/hands or toes/feet (96 %), and 12.3 % had injuries on their fingers/hands and their toes/feet.
Our estimation of the annual incidence of frostbite among conscripts who have completed their national service (≥ 320 days of service) is based on the number of persons who are registered with frostbite, ICD codes T33, T34 and T35, in the Armed Forces Health Registry. In the period 2010–2014, a total of 40 653 Norwegian men and women completed their national service (18). Altogether 572 of these were diagnosed with frostbite during the same period. This results in an annual incidence of frostbite of 1.4 % among all conscripted personnel in national service in Norway.
Of those persons who were diagnosed with frostbite, altogether 287 (50.2 %) served in five garrisons in Troms and Finnmark counties (Setermoen, Skjold, Bardufoss, Kirkenes, Lakselv). A total of 13 707 persons did their national service in these garrisons in the years 2010–2014 (18). The annual incidence of frostbite for conscripts who served in these exposed geographical areas amounts to 2.1 %. The annual incidence of frostbite in other regions in Norway is 1.1 %. This difference in incidence of frostbite between Northern Norway and the remaining parts of the country is statistically significant (p < 0.01).
More than two out of three (69.8 %) reported to have sustained permanent health afflictions as a result of their frostbite. One in five (20.7 %) reported that health ailments caused by their frostbite affected their ability to work and their leisure activities more than two years after the injury. Permanent serious health afflictions were more common among service personnel who had suffered from blisters (27.6 %) than among those who had not suffered from blisters (15.1 %) (p = 0.03). Only ten persons (2.5 %) had attempted any medical treatment for their frostbite (Table 3).
Table 3
Injury situation and outcome/treatment of frostbite during military service in the period 1 January 2010–31 December 2014
| N = 397 | (%) | |||
|---|---|---|---|---|
| Place of injury1 | Winter exercise | 321 | 81.1 | |
| Inside military camp | 81 | 15.9 | ||
| During military training | 49 | 12.4 | ||
| Other | 11 | 2.8 | ||
| Body part1 | Fingers/hands | 191 | 48.0 | |
| Toes/feet | 190 | 47.9 | ||
| Face/ears/cheeks | 81 | 20.4 | ||
| Other | 6 | 1.5 | ||
| Outcome/development2 | No symptoms | 93 | 23.5 | |
| (n = 395) | Moderate symptoms | 195 | 49.2 | |
| Symptoms during work/leisure | 82 | 20.7 | ||
| Don't know | 25 | 6.6 | ||
| Treatment2 | No treatment | 377 | 95.2 | |
| (n = 396) | Attempted treatment | 10 | 2.5 | |
| Don't know | 9 | 2.3 |
1Multiple responses were possible.
2Percentage of those who answered the question
Discussion
In the survey, more than 80 % of the group of military personnel who were diagnosed with a cold injury or frostbite during military service in the period 1 January 2010–31 December 2014 confirm having sustained frostbite. Most of them suffered peripheral frostbite on their fingers and/or toes during a winter exercise. More than one-fifth of those who confirm having sustained frostbite during their service period report that this has resulted in chronic health ailments that affect them at work and during leisure time.
Strengths and weaknesses of the study
The study has a relatively high response rate (66 %), which strengthens its validity. In this study, the Armed Forces Health Registry has retrieved data from the medical records system used by army medical officers. The study population has been diagnosed with frostbite during the period, but diagnosing frostbite is challenging, even for experienced clinicians. Many of the doctors in the sick quarters are recently graduated, conscripted doctors. They have limited experience in diagnosing frostbite, and the doctor may have diagnosed frostbite erroneously. This is corroborated by the observation that one-fifth of those who had been registered with frostbite did not acknowledge having sustained one.
The Armed Forces' efforts to prevent frostbite are complicated by the fact that military personnel do not always consult the military health services for treatment of cold injuries or frostbite. Experience indicates that some may be apprehensive that such episodes will have an effect on further military advancement (in the authors' personal experience and reports from colleagues). Based on many years of work in the military health services it is reasonable to assume some underreporting in this study.
In our study, there is uncertainty related to self-reporting of the severity of the frostbite. Even the appearance of blisters, which ought to be easily detectable and are characteristic of second-degree frostbite, was not recalled by more than one in ten respondents. There was no significant difference in the proportion that failed to recall any frostbite (with or without blisters), irrespective of the year in which it had occurred. As regards any possible shortcomings or errors in the doctor's diagnosis, we should bear in mind that blisters and scarring may occur many hours after the onset of the injury. This may change the appearance of the injury that was initially assessed by the army medical officer. Questionnaire-based health information may also be subject to information bias.
Incidence of frostbite
As seen also in previous studies, most of those who become injured are young people, primarily conscripted personnel. They have least military and field-related experience, and because they are in a training situation they are also most exposed to injuries. This is consistent with comparable studies among military personnel in the United Kingdom and the United States, for example (25, 26). Among British military servicemen who sustained frostbite over a 13-year period, two-thirds of the cases had occurred during winter training/exercises in Norway (25). In comparison, approximately 80 % of the cases of frostbite in our study had occurred during winter exercises.
The incidence of frostbite for the Norwegian Armed Forces as a whole is lower than among Finnish soldiers, where the incidence amounts to approximately 2 % (27, 28). In military garrisons in Troms and Finnmark counties, however, the incidence is equal to that in Finland. Significantly higher incidence rates have been reported in predisposed groups such as whalers/sealers (22 %) and mountaineers (37 %) (29).
The study indicates a higher incidence of frostbite in geographically exposed garrisons in Northern Norway, but the figures are not suitable for statistical analysis. Nor can our figures highlight a possible correlation between degree of severity and geographical location. The fact that the majority of the cases of frostbite in our study have occurred in Northern Norway may be due to the lower temperatures prevailing during exercises, longer winters with lower mean annual temperatures, and that the exposure is greater through a large number of days in the field for young and inexperienced conscripts.
The Armed Forces have previously undertaken a study to identify reduced ability to generate heat after a peripheral cooling as a risk factor for frostbite (23). A total of 196 soldiers in inner Troms county were monitored throughout their conscription period with the aid of repeated clinical and questionnaire-based assessments. Of these, 17 soldiers (8.7 %) reported to have sustained frostbite. However, only four of them were registered with a diagnosis of frostbite in the Armed Forces Health Registry (authors' non-published data).
A number of international studies among military personnel describe frostbite as one aspect of 'cold weather injuries'. Since this term also encompasses peripheral cold injuries and hypothermia, the incidence figures are somewhat imprecise, even though the majority of cold weather injuries are in fact frostbite. A review of these studies indicates an annual incidence of local frostbite in predisposed groups of 7–11 % (30, 31), which is also higher than our estimates, including tentative underreporting. In a study of Dutch elite soldiers, the cases of frostbite occurred during winter exercises in Norway (31), consistent with the occurrence of frostbite in our study.
A large American study conducted over 20 years showed a considerable decline in the number of hospital admissions for military personnel with cold injuries and frostbite during the period 1980–99, from 38.2/100 000 in 1985 to 0.2/100 000 in 1999. This study will soon be 20 years old and includes all types of 'cold weather injuries' (32), but more recent figures also indicate that the incidence of 'cold weather injuries' among American soldiers is declining (33). This trend towards falling incidence rates cannot be seen in our material because of its short five-year observation period.
Severity and outcomes of frostbite
Scientifically based knowledge on pathophysiology (34) and advanced diagnostic procedures can predict outcomes and improve the follow-up of frostbite (6). Although experimental forms of treatment appear promising (35), no evidence-based causal treatment is available on a routine basis (36). This is corroborated by the observation that 95.2 % of the injured people in our study have received no medical treatment for their chronic ailments after frostbite.
The outcome of frostbite is hard to predict (30). The majority of the patients suffer symptoms long after the time of injury, but even less pronounced frostbite can result in permanent ailments (34). This is corroborated by our study, in which 69.8 % suffer from symptoms more than two years after the time of injury. A Finnish study found a similar level, where 63 % of the patients suffered subjective symptoms 4–11 years after the injury (15).
In line with previous research (15), complications occurred more frequently in cases of severe frostbite with blisters. However, 15 % of the soldiers who did not have any blisters also reported sequelae that caused them discomfort in daily life. This indicates that limited frostbite that initially is perceived as mild also may result in chronic health ailments.
The authors wish to thank the Armed Forces Health Registry and the Armed Forces HR and Conscription Centre for contributing figures to the study.
- 1.
Wikipedia. Carl Gustav Armfeld. https://no.wikipedia.org/wiki/Carl_Gustaf_Armfeldt (14.5.2018).
- 2.
Golden FS, Francis TJ, Gallimore D et al. Lessons from history: morbidity of cold injury in the Royal Marines during the Falklands Conflict of 1982. Extrem Physiol Med 2013; 2: 23. [PubMed][CrossRef]
- 3.
Forsvaret. Center of Excellence – Cold Weather Operations. https://forsvaret.no/en/education-and-training/coe-cwo (14.5.2018).
- 4.
Forsvaret. Helse for stridsevne 2016. https://forsvaret.no/aktuelt/helse-for-stridsevne1 (14.5.2018).
- 5.
Ikäheimo TM, Hassi J. Frostbites in circumpolar areas. Glob Health Action 2011; 4: 8456. [PubMed][CrossRef]
- 6.
Heil K, Thomas R, Robertson G et al. Freezing and non-freezing cold weather injuries: a systematic review. Br Med Bull 2016; 117: 79 - 93. [PubMed][CrossRef]
- 7.
Handford C, Buxton P, Russell K et al. Frostbite: a practical approach to hospital management. Extrem Physiol Med 2014; 3: 7. [PubMed][CrossRef]
- 8.
Imray CH, Richards P, Greeves J et al. Nonfreezing cold-induced injuries. J R Army Med Corps 2011; 157: 79 - 84. [PubMed][CrossRef]
- 9.
Oslo universitetssykuhus. Metodebok for indremedisinere. Hypotermi. www.helsebiblioteket.no/retningslinjer/metodebok/akuttmedisin/hypotermi (14.5.2018).
- 10.
Brown DJ, Brugger H, Boyd J et al. Accidental hypothermia. N Engl J Med 2012; 367: 1930 - 8. [PubMed][CrossRef]
- 11.
Thomassen Ø. Nasjonale retningslinjer for aksidentell hypotermi. Nasjonal kompetansetjeneste for traumatologi. traumatologi.no/2017/10/17/faglig-retningslinje-for-handtering-av-aksidentell-hypotermi/ (14.5.2018).
- 12.
Deslarzes T, Rousson V, Yersin B et al. An evaluation of the Swiss staging model for hypothermia using case reports from the literature. Scand J Trauma Resusc Emerg Med 2016; 24: 16. [PubMed][CrossRef]
- 13.
Arvesen A, Rosén L, Eltvik LP et al. Skin microcirculation in patients with sequelae from local cold injuries. Int J Microcirc Clin Exp 1994; 14: 335 - 42. [PubMed][CrossRef]
- 14.
Imray C, Grieve A, Dhillon S et al. Cold damage to the extremities: frostbite and non-freezing cold injuries. Postgrad Med J 2009; 85: 481 - 8. [PubMed][CrossRef]
- 15.
Ervasti O, Hassi J, Rintamäki H et al. Sequelae of moderate finger frostbite as assessed by subjective sensations, clinical signs, and thermophysiological responses. Int J Circumpolar Health 2000; 59: 137 - 45. [PubMed]
- 16.
Sachs C, Lehnhardt M, Daigeler A et al. The triaging and treatment of cold-induced injuries. Dtsch Arztebl Int 2015; 112: 741 - 7. [PubMed]
- 17.
Hutchison RL. Frostbite of the hand. J Hand Surg Am 2014; 39: 1863 - 8. [PubMed][CrossRef]
- 18.
Forsvaret. Forsvarets helsregister. https://forsvaret.no/helseregister (14.5.2018).
- 19.
FOR-2005-09-02-1010. Forskrift om innsamling og behandling av opplysninger i Forsvarets helseregister. https://lovdata.no/dokument/SF/forskrift/2005-09-02-1010 (14.5.2018).
- 20.
Fadum EA, Fønnebø V, Borud EK. Presence of minor and major mental health impairment in adolescence and death from suicide and unintentional injuries/accidents in men: a national longitudinal cohort study. J Epidemiol Community Health 2017; 71: 19 - 24. [PubMed][CrossRef]
- 21.
Strand LA, Martinsen JI, Fadum EA et al. External-cause mortality among 21 609 Norwegian male military peacekeepers deployed to Lebanon between 1978 and 1998. Occup Environ Med 2017; 74: 573 - 7. [PubMed][CrossRef]
- 22.
Strand LA, Martinsen JI, Borud EK. Cancer risk and all-cause mortality among Norwegian military United Nations peacekeepers deployed to Kosovo between 1999 and 2011. Cancer Epidemiol 2014; 38: 364 - 8. [PubMed][CrossRef]
- 23.
Norheim AJ, Mercer J, de Weerd L et al. Termografi ved frostskader i Forsvaret. Tidsskr Nor Legeforen 2014; 134: 1645. [PubMed][CrossRef]
- 24.
Confirmit. https://www.confirmit.com (14.5.2018).
- 25.
Heil KM, Oakley EH, Wood AM. British Military freezing cold injuries: a 13-year review. J R Army Med Corps 2016; 162: 413 - 8. [PubMed][CrossRef]
- 26.
Armed Forces Health Surveillance Center (AFHSC) Cold weather injuries, active and reserve components, U.S. Armed Forces, July 2008-June 2013. MSMR 2013; 20: 12 - 7, discussion 16 - 7.
- 27.
Lehmuskallio E, Lindholm H, Koskenvuo K et al. Frostbite of the face and ears: epidemiological study of risk factors in Finnish conscripts. BMJ 1995; 311: 1661 - 3. [PubMed][CrossRef]
- 28.
Ervasti O, Juopperi K, Kettunen P et al. The occurrence of frostbite and its risk factors in young men. Int J Circumpolar Health 2004; 63: 71 - 80. [PubMed][CrossRef]
- 29.
Harirchi I, Arvin A, Vash JH et al. Frostbite: incidence and predisposing factors in mountaineers. Br J Sports Med 2005; 39: 898 - 901. [PubMed][CrossRef]
- 30.
Cattermole TJ. The epidemiology of cold injury in Antarctica. Aviat Space Environ Med 1999; 70: 135 - 40. [PubMed]
- 31.
Daanen HA, van der Struijs NR. Resistance Index of Frostbite as a predictor of cold injury in arctic operations. Aviat Space Environ Med 2005; 76: 1119 - 22. [PubMed]
- 32.
DeGroot DW, Castellani JW, Williams JO et al. Epidemiology of U.S. Army cold weather injuries, 1980-1999. Aviat Space Environ Med 2003; 74: 564 - 70. [PubMed]
- 33.
O'Donnell FL, Taubman SB. Update: Cold weather injuries, active and reserve components, U.S. Armed Forces, July 2011-June 2016. MSMR 2016; 23: 12 - 20. [PubMed]
- 34.
Hallam MJ, Cubison T, Dheansa B et al. Managing frostbite. BMJ 2010; 341: c5864. [PubMed][CrossRef]
- 35.
Norheim AJ, Mercer J, Musial F et al. A new treatment for frostbite sequelae; Botulinum toxin. Int J Circumpolar Health 2017; 76: 1273677. [PubMed][CrossRef]
- 36.
Su CW, Lohman R, Gottlieb LJ. Frostbite of the upper extremity. Hand Clin 2000; 16: 235 - 47. [PubMed]