MAIN MESSAGE
94 % of the women who had an abortion performed by a specialist in private practice felt that the procedure was absolutely safe
42 % of the women perceived the abortion as easier than expected
Nearly all the women included in the study would have a medical abortion performed by a specialist in private practice should they choose to have an abortion later in life
Induced abortion is one of the most commonly performed procedures in reproductive health. Globally, the number of abortions is declining, while the number of unsafe abortions is on the increase (1). In Norway, the number of abortions has remained relatively stable, with 13 977 pregnancy terminations in 1998 and 13 169 in 2016, although there has been a significant decrease in induced abortions among young women since 2006 (2). Until 1998, all abortions in Norway were undertaken surgically, but in that year an option for medical abortions was introduced (3). Since 1998, a near-total change in abortion procedures from surgical to medical treatment has occurred. In 2006, the proportion of abortions that were undertaken medically was 45 %; in 2016 this proportion amounted to 88 % (2). Most abortions are undertaken at an early stage of pregnancy. In 2016, altogether 81 % of all abortions were performed before the 9th week of gestation, and of these, 92 % were undertaken medically.
Abortion is regulated by the Abortion Act (4), which says that the treatment should be undergone in a public hospital where a doctor holds medical responsibility for the abortion, the dispensing of the drugs and the check-up. In Norway, medical abortions are undertaken with a combination of the antiprogesterone mifepristone and the prostoglandin misoprostol (5). It is recommended that women with a gestational period of less than nine weeks (63 days) take the mifepristone in hospital (as outpatients) and be admitted 24–48 hours later as day patients to take the misoprostol, or complete the treatment at home. If the pregnancy is between the 9th and 12th week of gestation, the woman will complete the procedure in hospital.
Many countries practice abortion treatment outside of public hospitals. In 2005, Denmark introduced a legal amendment that permitted abortions outside hospitals to be performed by specialists in private practice (6). Sweden and the Netherlands also provide medical abortions outside of public hospitals. The World Health Organization recommends that abortion be made easily available, meaning that this option should be available at the level of primary health services and with established routines for referral to specialist services (7). This corresponds to national principles (the lowest effective level of care) and is stipulated by a number of public studies and plans.
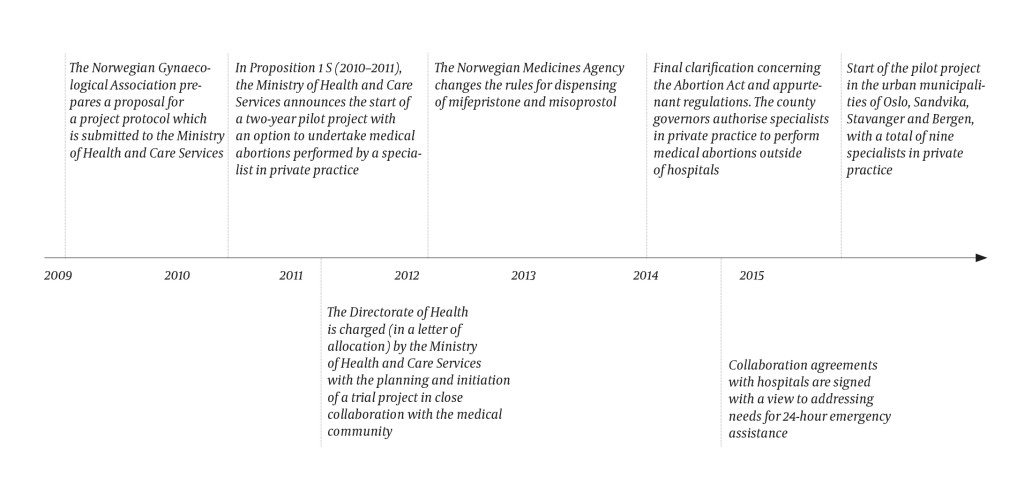
Following an initiative by the Norwegian Gynaecological Association, the Ministry of Health and Care Services indicated in the state budget for 2011 (8) that 'a two-year pilot project will be initiated, whereby gynaecologists/obstetricians (specialists) in private practice who have a contract with a regional health authority will be permitted to provide medically induced pregnancy terminations (abortion pill) as a home-based procedure before the end of the 9th week of gestation'. In 2010, the Directorate of Health was charged with the planning, initiation and evaluation of the project, in close collaboration with the medical community.
The Ministry of Health and Care Services and the Directorate of Health have been in a dialogue concerning the medical assessments that form the basis for the practice of medical abortions and the necessary clarifications with regard to legislation, regulations, dispensing of drugs and reporting (Figure 1). In March 2015, the project was established in Oslo, Sandvika, Stavanger and Bergen, with a total of nine specialists in private practice and a duration of two years. The main objective of the pilot project was to identify working methods that can provide a wider range of options to pregnant women who want an abortion, as well as to test out the medical and organisational aspects of providing medical abortions performed by specialists in private practice.

In this article we describe how this treatment option was received by a series of 476 women with a gestation period of < 63 days who chose to have a medical abortion performed by a specialist in private practice.
Material and method
Nine specialists in private practice with a particular interest in this patient group were permitted to provide medical abortions for the duration of the project period. In the selection of specialists in private practice to be included in the pilot project, emphasis was placed on the specialist's own desire to participate. Some professional requirements were also set. Information about the project was distributed to all health enterprises, GPs and mother and child clinics in Oslo, Akershus, Hordaland and Rogaland counties. Furthermore, information about the project has been posted on the website helsenorge.no/gravid and the Directorate of Health's web pages on pregnancy.
All pregnant women who had a documented gestation period of 62 days or less and who underwent a medical abortion performed by a specialist in private practice were included in the study on an ongoing basis. Determination of the gestation period was based on ultrasonography with a measurement of crown-rump length. Written and oral information was provided with regard to the nature and medical effects of the intervention, as well as optional information and advice about available benefit schemes (cf. Section 2 of the Abortion Act). All the women voluntarily chose to have this procedure performed by a specialist in private practice, by informed consent.
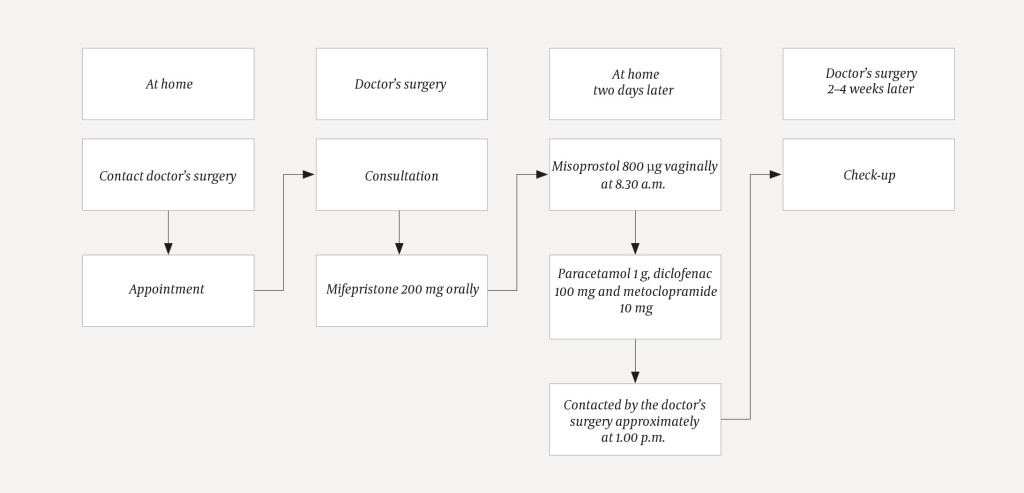
Two consultations were planned for each woman (Figure 2). In the first consultation, the women would take 200 mg mifepristone orally while being monitored. The women were instructed to insert 800 µg misoprostol vaginally and simultaneously take 1 000 mg paracetamol, 100 mg diclofenac and 10 mg metoclopramide orally two days later. Information on expected bleeding volume was given, including that the woman should contact the specialist in private practice or a hospital if the bleeding exceeded normal levels, defined as more than six large sanitary pads (night pads) over two hours. Healthcare personnel from the doctor's surgery contacted the women by telephone after the insertion of the misoprostol to check on pain, bleeding and safety concerns. All project participants were provided with optional check-ups that included advice on contraception two to four weeks after the abortion procedure.
Information on volume of bleeding, pain, safety and satisfaction was collected with the aid of a questionnaire during the abortion and at the check-up. By telephone, the women were asked to assess the bleeding as none, light, moderate, heavy or very heavy, and their pain as none, slight, moderate or severe. They were asked to report their perception of safety during the abortion procedure by answering questions such as: 'Does it feel safe to be at home during the procedure?' The degree of safety was reported on a ten-point Likert scale, where 1 was least safe and 10 most safe. At the check-up, the women were again asked about their perception of safety during the abortion procedure. In addition, they were asked about their personal satisfaction, including whether they would choose to have an abortion performed by a specialist in private practice also for later pregnancy terminations, should the need arise, and whether they would recommend this option to others in the same situation, with yes/no as response alternatives. The specialists in private practice were also asked to report the time spent for the first consultation and the check-up, and whether the woman had needed additional consultations between the planned ones and/or contact with other groups of healthcare personnel (general practitioner, hospital).
The descriptive analyses are presented in the form of the median and range for continuous data and as frequencies and percentages for categorical data. The distribution of scores for safety is visualised in a histogram. Only anonymous data were registered and analysed. No linkage keys were used, and no personal ID numbers or names were recorded. The project was processed by the South-Eastern Regional Committee for Medical and Health Research Ethics on 17 September 2014 (ref.no. 2014/1427) and was considered not subject to mandatory submission.
Results
A total of 476 women were included in the project on an ongoing basis during the study period. Their median age was 30 years (range 17–47), and 193 women (41 %) were nulliparous. Approximately one-half of the women (235/476, 49 %) had never previously undergone an induced abortion. Characteristics of the included women are given in Table 1. Their median gestation period was 43 days (range 28–63). Altogether 415 women attended for the check-up two to four weeks after the abortion, while 61 women (13 %) did not attend.
Table 1
Characteristics of the women included in the project
| Variables |
n = 476 |
|---|---|
| Gestation period in days, median (range) |
43 (28–63) |
| Age, median (range) |
30 (17–47) |
| Previous births, n (%) |
|
| 0 |
193 (41) |
| 1 |
83 (17) |
| 2 |
135 (28) |
| ≥ 3 |
65 (14) |
| Previous abortions, n (%) |
|
| 0 |
235 (49) |
| 1 |
179 (38) |
| ≥ 2 |
62 (13) |
The degree of bleeding was registered for 451 (95 %) of the women during the abortion procedure and for 408 (86 %) at the check-up. During the abortion procedure, nine women (2 %) reported very heavy bleeding, 162 (36 %) heavy bleeding, 196 (44 %) moderate bleeding, 69 (15 %) light bleeding and 15 (3 %) no bleeding (Table 2). During the first days after the abortion procedure, 26 women (6 %) reported very heavy bleeding, 160 (39 %) heavy bleeding, 178 (44 %) moderate bleeding and 44 (11 %) light bleeding. The median duration of the bleeding was 13 days (range 3–35).
Table 2
Degree of pain and bleeding registered 4–6 hours after intake of misoprostol and degree of bleeding during the first days after the abortion procedure. The data were collected in a questionnaire during the abortion procedure and at the check-up 2–4 weeks after the abortion
| 4–6 hours after misoprostol, n (%) |
The first days after the abortion procedure, n (%) |
|
|---|---|---|
| Pain |
n = 450 |
|
| None |
28 (6) |
|
| Slight |
126 (28) |
|
| Moderate |
191 (42) |
|
| Severe |
105 (23) |
|
| Bleeding |
n = 451 |
n = 408 |
| None |
15 (3) |
0 (0) |
| Light |
69 (15) |
44 (11) |
| Moderate |
196 (44) |
178 (44) |
| Heavy |
162 (36) |
160 (39) |
| Very heavy |
9 (2) |
26 (6) |
Information on pain was recorded for 450 of the women during the abortion procedure. During the procedure, 28 women (6 %) had no pain, 126 (28 %) slight pain, 191 (42 %) moderate pain and 105 (23 %) severe pain (Table 2).
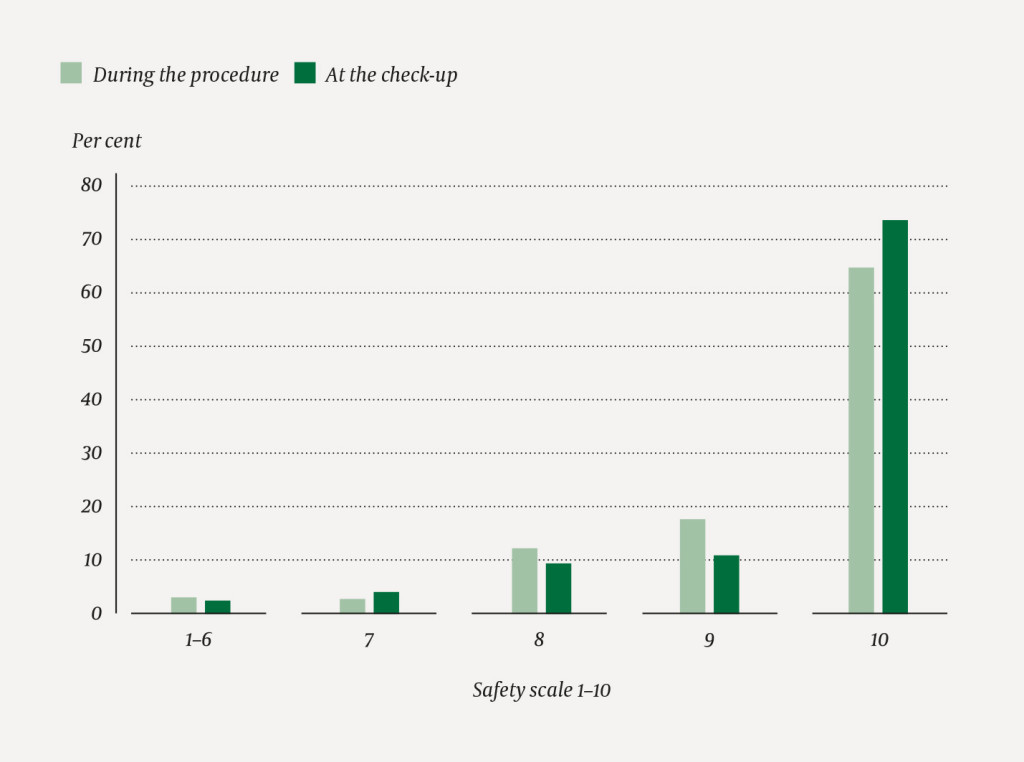
The degree of safety in undertaking the abortion procedure at home was registered for 426 women during the procedure and for 394 women at the check-up. The perception of safety in undertaking the abortion procedure at home is illustrated in Figure 3. During the abortion procedure, 379 women (94 %) reported a safety score of 8, 9 or 10. Altogether 368 women reported a safety score of 8, 9 or 10 at the check-up. The median perception of safety reported during the abortion procedure was 10 (range 4–10). At the check-up, the median perception of safety was also 10 (range 1–10). During the abortion procedure, five women (1 %) reported a safety score of 1,2, 3 or 4. At the check-up, five women reported a safety score of 1, 2, 3 or 4.
Satisfaction with the procedure, including questions on the woman's experience of the abortion procedure, whether she would choose the same option for a possible later abortion, and whether she would recommend medical abortion performed by a specialist in private practice to others in the same situation, are described in Table 3. Altogether 42 % (173/409) of the women found the abortion procedure easier than expected, and 96 % (390/406) would have a medical abortion performed by a specialist in private practice should they need another abortion. A total of 97 % (392/405) of the women would recommend having a medical abortion with a specialist in private practice to others in the same situation.
Table 3
Satisfaction with the abortion procedure. The data were collected with the aid of a questionnaire at the check-up 2–4 weeks after the abortion
| Variables |
n (%) |
|---|---|
| How did you perceive the abortion procedure? |
n = 409 |
| Easier than expected |
173 (42) |
| As expected |
153 (37) |
| Harder than expected |
83 (20) |
| Should you need to do it again, what would you choose? |
n = 406 |
| Home abortion under the auspices of a specialist in private practice |
390 (96) |
| Home abortion under the auspices of a hospital |
0 (0) |
| Having the abortion performed in a hospital |
16 (4) |
| Would you recommend having a home abortion with a specialist in private practice to others? |
n = 405 |
| Yes |
392 (97) |
| No |
13 (3) |
Information on whether the woman had been in contact with other groups of healthcare personnel (including hospitals) during the abortion procedure was registered for 403 women. Altogether 36 women (9 %) had been in contact with other healthcare personnel. Information on whether the woman had any additional consultations with the specialist in private practice was registered for 377 women. A total of 68 women (18 %) had attended one or more additional consultations with the specialist in private practice in connection with the abortion (Table 4).
Table 4
Contact with other healthcare personnel, need for additional consultations and time spent by the specialist in private practice. The data were collected in a questionnaire at the check-up 2–4 weeks after the abortion
| Variables |
n (%) |
|---|---|
| Contact with other healthcare personnel (including hospitals)? |
n = 403 |
| Yes |
36 (9) |
| No |
367 (91) |
| Additional consultation with the specialist in private practice? |
n = 377 |
| Yes |
68 (18) |
| No |
309 (82) |
| Time spent per patient at the first consultation |
n = 427 |
| < 20 minutes |
110 (26) |
| 20–40 minutes |
266 (62) |
| Variables |
n (%) |
| > 40 minutes |
51 (12) |
| Time spent per patient at the second consultation |
n = 384 |
| < 20 minutes |
200 (52) |
| 20–40 minutes |
179 (47) |
| > 40 minutes |
5 (1) |
Altogether 62 % of the first consultations (266/427) lasted from 20 to 40 minutes, 26 % (110/427) less than 20 minutes and 12 % (51/327) more than 40 minutes. Less time was set aside for the check-ups: 52 % (200/384) lasted less than 20 minutes, 47 % (179/384) from 20 to 40 minutes and 1 % (5/384) more than 40 minutes (Table 1).
Discussion
This study of a patient series of 476 women represents the first experience gained from permitting specialists in private practice to provide medically induced abortions before the end of the ninth week of gestation. The vast majority of the women were satisfied with their abortion procedure and would recommend it to others in the same situation. A small proportion of the women were less satisfied with the procedure and would not choose medical abortion performed by a specialist in private practice again, should the need arise.
The results show that many women endured moderate or severe pain during their abortion. Pain is a frequently reported adverse effect of medical abortion and must be regarded as a natural consequence of the procedure (9–12). Since the method is expected to be painful, sufficient analgesic treatment is of great importance. The project provided written and oral information about pain, and analgesic drugs for use at home were dispensed to all the women concerned.
Vaginal bleeding is also a necessary consequence of the procedure (9–11). Four to six hours after the administering of misoprostol most of the women (79 %) reported moderate or heavy bleeding. At the check-up, 83 % reported to have bled moderately or heavily during the first days after the abortion procedure. Few women (2 %) reported very heavy bleeding four to six hours after the administration of misoprostol, nor did many (6 %) experience very heavy bleeding during the days after the abortion procedure. A median bleeding period of 13 days is consistent with what has been reported by other studies (9–11).
During the abortion procedure, nearly all of the women (94 %) reported a score between 8 and 10 for perceived safety. At the check-up as well, the majority of the women (93 %) reported high scores for perceived safety. Good information may help increase the patient's sense of safety and ability to cope with what will happen, and form the basis for more realistic expectations (13). Often, it will be easier to cope with discomfort when this is known beforehand and accords with the woman's expectations. We believe that because of the good written and oral information provided in advance, the women had a realistic notion of pain and bleeding as natural consequences of the procedure, and therefore perceived a high degree of safety during the abortion procedure.
The patients were highly satisfied with having a medical abortion performed by a specialist in private practice, reflected in the fact that the vast majority would choose the same option should they need another elective abortion. They would also recommend the option provided by a specialist in private practice to others in the same situation. This concurs with the results from other studies that have assessed patient satisfaction with medical abortions that were initiated in hospital and completed at home (11, 14, 15). In the pilot project, the women themselves had chosen to have a medical abortion performed by a specialist in private practice.
Women who want an abortion are concerned with choosing the abortion method themselves (10, 16), and it is possible that the opportunity to choose the location for undergoing the abortion may have an effect on the woman's perception of safety and satisfaction with the procedure.
Few of the women included in the pilot project (9 %) had any contact with other healthcare personnel and/or hospital during the abortion procedure, while one in every five women who underwent the procedure needed additional consultation with the specialist in private practice. Abortion is an issue that requires comprehensive information and a thorough clinical assessment. We have no information on resource use (time spent) associated with medical abortions performed in hospitals, and we can thus not compare our results to equivalent results from hospitals.
Weaknesses of the study
A weakness of the study is the absence of a comparable group of women who have undergone a medical abortion in hospital. If we had compared the women who had the procedure performed by a specialist in private practice with 'all other' women who had undergone a medical abortion in hospital, we would most likely have seen a good result for those women who had a medical abortion performed by a specialist in private practice, without this being attributable to the procedure in the specialist in private practice's surgery. The reason is that those patients who turned to a specialist in private practice to have the procedure did so voluntarily and can thus be assumed to favour this option.
A randomised controlled study would be preferable in research terms, but would be difficult to implement and have a low rate of inclusion. A Norwegian study investigated the extent to which women would be willing to let themselves be randomly assigned to an abortion method (medical or surgical abortion) (10). The study showed that 70 % would be unwilling to be randomised with regard to method.
Conclusion
The pilot project has shown that a large majority of the women who participated in the project were satisfied with having the abortion procedure performed by a specialist in private practice and would recommend it to others. Few women had contact with a hospital or other healthcare personnel during the abortion procedure.
- 2.
Folkehelseinstituttet. Medisinsk fødselsregister og abortregisteret – Statistikkbanker. https://www.fhi.no/hn/statistikk/statistikkalenderen/statistikkbanker/ (3.3.2018).
- 3.
Løkeland M, Bjørge T, Iversen OE et al. Implementing medical abortion with mifepristone and misoprostol in Norway 1998-2013. Int J Epidemiol 2017; 46: 643 - 51. [PubMed]
- 4.
LOV-1975-06-13-50. Lov om svangerskapsavbrudd (abortloven). https://lovdata.no/dokument/NL/lov/1975-06-13-50 (3.3.2018).
- 5.
Bjørge L, Løkeland M, Oppegaard K. Provosert abort. Veileder i generell gynekologi. Oslo: Norsk gynekologisk forening, 2017. https://legeforeningen.no/Fagmed/Norsk-gynekologisk-forening/Veileder-arkiv--utgatte-versjoner/veileder-i-generellgynekologi-2009/provosert-abort/ (3.3.2018).
- 7.
World Health Organization. Safe abortion: technical and policy guidance for health systems. 2012. http://www.who.int/reproductivehealth/publications/unsafe_abortion/9789241548434/en/ (3.3.2018).
- 8.
Helse- og omsorgsdepartementet. Prop. 1 S (2010-2011) for budsjettåret 2011; 126. https://www.regjeringen.no/no/dokumenter/prop-1-s-20102011/id617556/ (3.3.2018).
- 10.
Iversen OE, Midbøe G, Johnsen SL et al. Medikamentell abort – de første norske erfaringene. Tidsskr Nor Lægeforen 2003; 123: 2422 - 4. [PubMed]
- 13.
Grønnestad BK, Blystad A. Pasienters opplevelse av informasjon i forbindelse med en operasjon – en kvalitativ studie. Nordic Journal of Nursing Research 2004; 24: 4 - 8. [CrossRef]