MAIN MESSAGE
Individuals who died at the age of 56–95 had on average 3.8 admissions to somatic hospitals during their final three years
Those who died at the age of 56–65 had on average 5.2 admissions during their final three years of life, compared to 2.8 admissions among those who died at the age of 86–95
Average admission frequency rose from 0.3 admissions in the period 31–36 months prior to death to 1.6 admissions during the last six months prior to death
The demand for health services will be affected by increasing life expectancy and a growing number of elderly people in the population. However, the need for health services will not only reflect the number of people in each age group (1–3). Serious and fatal disorders give rise to intensive use of health services, irrespective of the patient's age. As life expectancy increases, the average age at death will also increase, and the particularly heavy use of health services will shift to a higher age. Some researchers have claimed that not only age, but the remaining lifetime of individuals can best explain the need for health services (4, 5).
Most studies (1–3), (3, 6, 7), including two Norwegian ones (8, 9), indicate, however, that both age and remaining lifespan affect the use of hospital services independently of each other. The estimation of the need for hospital services in an ageing population is further complicated by the fact that the older the dying person the less they are used during the final months of life (8–12). Melberg and collaborators (8) showed, for example, that a 65-year-old who died in 2010 would on average generate hospital costs that were twice as high as those incurred by a dying 85-year-old. It is therefore possible that the use of hospital services at the final stage of life will decrease as the typical age at death rises in pace with the increase in life expectancy.
Studies of the use of health services in the period preceding the death of individuals may help us understand the implications of increasing life expectancy for the future need for health services. This topic is also of interest because a considerable proportion of the health services' resources is devoted to patients who are approaching the end of life. In Norway, it has been estimated that approximately 10 % of hospital resources are spent on patients who die within the same year (8, 9). Studies from other countries have shown similar results (11, 13).
Previous Norwegian studies have analysed hospital costs in specific calendar years for those who died during the calendar year, and compared to those who lived through the entire year (8, 9). Godager and Gregersen (9) showed, for example, that among individuals aged 85–89, altogether 26 % (men) and 19 % (women) of the hospital costs could be associated with patients who died in the same year. Melberg and collaborators (8) estimated that the hospital costs for a 70-year-old woman who died in 2010 were approximately ten times higher than for a woman of the same age who did not die, and the use of hospital services was especially intensive during the last two months of life.
The objective of this study was to obtain more detailed knowledge about admissions to somatic hospitals during the final stage of life. We analysed individuals who died at the age of 56–95 years, with particular emphasis on variations by age at death, since these could give indications of possible changes generated by higher life expectancy. Previous Norwegian studies have had access to data for specific calendar years. We used a longer observation period and analysed the number of admissions to somatic hospitals during the last three years of life. We examined individual variations in the use of hospital services and analysed variations by cause of death, place of death, gender, education, immigration status and health region.
Material and method
This study is part of a research project on the use of specialist health services, funded by the Research Council of Norway (project no. 222100) and approved by the South-Eastern Regional Committee for Medical and Health Research Ethics (REC) (ref. 2013/821) and the Norwegian Data Protection Authority (ref. 13/00484). Statistics Norway has provided access to data files with individual information on all persons who were resident in Norway as of 1 January 2008. The data files contain information from the vital statistics registry (gender, home municipality and immigration status), the Causes of Death Registry (year and month of death, age at death, place of death and underlying cause of death) and the Education Registry (highest completed level of education). Furthermore, the project has been granted access to individual information from the Norwegian Patient Registry on admissions to somatic hospitals in the years 2008–11. The information on individuals from Statistics Norway and the Norwegian Patient Registry was linked with the aid of encrypted personal ID numbers.
From the data material we retrieved individuals who had died in 2011 at the age of 56–95. Information on time (month and year) of death and time (month and year) of admission to somatic hospitals was used to estimate the total number of admissions during the last three years of life, as well as the total number of admissions during six six-month periods (0–6 months prior to death, 7–12 months prior to death etc.). An admission normally involves at least one hospitalisation day, but we also included admissions registered with zero hospitalisation days, when the patient had been sent home on the same day.
Statistics Norway provided information on the underlying cause of death coded according to the International Classification of Diseases (ICD, 10th edition) (14) and classified according to the European Shortlist for Causes of Death (15). Information in the Causes of Death Registry on place of death was grouped into three categories: care and nursing institution, hospital and home/other. Information in the Education Registry was used to group the individuals into three educational categories (primary/lower secondary, upper secondary and tertiary). Individuals born outside Norway to two foreign-born parents were classified as immigrants. Information on home municipality was used to link the individuals to a specific health region.
First we estimated how the admission frequency (average number of admissions per person in the periods of time studied) varied by age at death (four ten-year intervals), gender, place of death and group of cause of death. Multivariate Poisson regression analyses of the number of admissions during the last three years of life were then made to ascertain whether the observed correlations with age at death persisted after control for gender, education, immigration status and health region. The results are reported in adjusted incidence rate ratios (IRR) and 95 % confidence intervals.
Results
The studied sample included 35 954 individuals who died in 2011 at the age of 56–95 (Table 1). These individuals had a total of 136 484 admissions to somatic hospitals during their final three years of life. Women accounted for 39.4 % of those who died at the age of 56–65, compared to 64.4 % of those who died at the age of 86–95. 14.1 % had no admissions during their final three years of life, while 13.3 % had eight or more admissions, and this latter group accounted for 41.2 % of all admissions in the analytical sample during the observation period. The proportion of deaths that occurred in care and nursing institutions rose in pace with higher age of death, from 19.6 % of those who died at the age of 56–65, to 66.1 % for age of death 86–95 years.
Table 1
Sample used in the analysis: 35 954 persons aged 56–95 who died in 2011, by age at death, gender, number of hospital admissions during the final three years of life (grouped), place of death and group of causes of death
| Age at death |
|||||
|---|---|---|---|---|---|
| All 56–95 years |
56–65 years |
66–75 years |
76–85 years |
86–95 years |
|
| Number (= 100 %) |
35 954 (100) |
3 806 (100) |
6 115 (100) |
12 080 (100) |
13 953 (100) |
| Number of women (proportion in %) |
18 600 (51.7) |
1 500 (39.4) |
2 349 (38.4) |
5 771 (47.8) |
8 980 (64.4) |
| Number of admissions during the final three years of life (prop. in %) |
|||||
| 0 admissions |
5 055 (14.0) |
599 (15.7) |
707 (11.6) |
1 348 (11.2) |
2 401 (17.2) |
| 1–7 admissions |
26 130 (72.7) |
2 285 (60.0) |
4 077 (66.7) |
9 066 (75.0) |
10 702 (76.7) |
| 8+ admissions |
4 769 (13.3) |
922 (24.2) |
1 331 (21.8) |
1 666 (13.8) |
850 (6.1) |
| Place of death, number (prop. in %) |
|||||
| Care and nursing institution |
17 540 (48.8) |
745 (19.6) |
1 769 (28.9) |
5 806 (48.1) |
9 220 (66.1) |
| Hospital |
12 803 (35.6) |
1 758 (46.2) |
2 869 (46.9) |
4 618 (38.2) |
3 558 (25.5) |
| At home, other |
5 611 (15.6) |
1 303 (34.2) |
1 477 (24.2) |
1 656 (13.7) |
1 175 (8.4) |
| Cause of death (ICD-10 codes), number (prop. in %) |
|||||
| Diseases of the circulatory system (I00-I99) |
11 779 (32.8) |
730 (19.2) |
1 489 (24.3) |
3 886 (32.2) |
5 674 (40.7) |
| Malignant neoplasms (C00-D48) |
9 930 (27.6) |
1 796 (47.2) |
2 633 (43.1) |
3 468 (28.7) |
2 033 (14.6) |
| Diseases of the respiratory system (J00-J99) |
3 702 (10.3) |
243 (6.4) |
583 (9.5) |
1 389 (11.5) |
1 487 (10.7) |
| External causes (S00-Y98) |
1 452 (4.0) |
252 (6.6) |
179 (2.9) |
423 (3.5) |
598 (4.3) |
| All other causes |
9 091 (25.3) |
785 (20.6) |
1 231 (20.1) |
2 914 (24.1) |
4 161 (29.8) |
The composition of the causes of death varied by age (Table 1). Diseases in the circulatory system accounted for 19.2 % of the deaths in the age group 56–65 years, compared to 40.7 % of the deaths in the age group 86–95 years. Malignant neoplasms caused 47.2 % of the deaths in the age group 56–65 years, compared to 14.6 % in the age group 86–95 years.
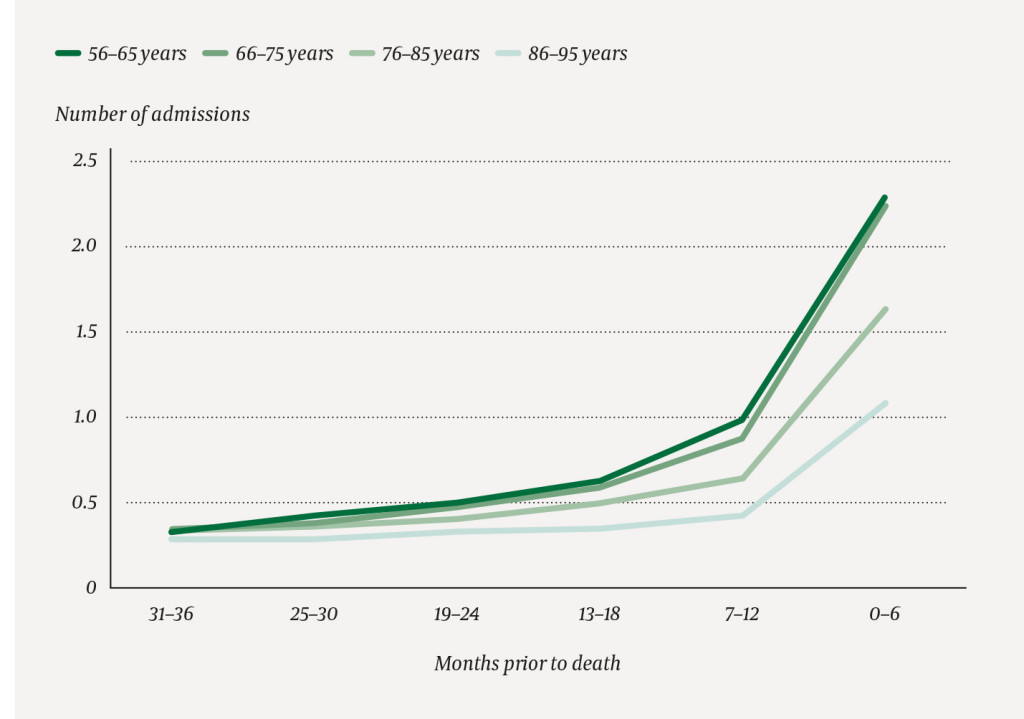
The average number of admissions per person was 0.3 in the period 31–36 months prior to death, with insignificant variations by age at death (Figure 1). The frequency of admission rose with decreasing time of life remaining and increased sharply during the final year of life, especially during the last six months, but in different ways in the age categories analysed. Those who died at the age of 56–65 had 1.0 admission on average in the period 7–12 months before death, increasing to 2.3 admissions on average during their final six months of life. Those who died at the age of 86–95 had on average 0.4 admissions 7–12 prior to death and 1.1 admissions of average during their final six months of life.
In the course of the final three years of life, the sample analysed had on average 3.8 admissions to somatic hospitals (Table 2) – men somewhat more frequently (4.1 admissions/3 years) than women (3.5 admissions/3 years). The number of admissions during the final three years of life declined with increasing age of the deceased, from 5.2 for age at death 56–65 years to 2.8 for age at death 86–95 years. The frequency of admissions during the final three years of life also varied by place of death – highest (4.9 admissions) among those who died in hospital, compared to 3.4 admissions when death occurred in a care and nursing institutions and 2.7 admissions among those who died in their own home (Table 2).
Table 2
Average number of admissions to somatic hospitals during the final three years of life for 35 954 persons aged 56–95 who died in 2011, by age at death, gender, place of death and group of causes of death
| Age at death |
All 56– |
56–65 years |
66–75 years |
76–85 years |
86–95 years |
|---|---|---|---|---|---|
| All |
3.8 |
5.2 |
5.0 |
3.9 |
2.8 |
| Men |
4.1 |
4.6 |
5.1 |
4.2 |
3.2 |
| Women |
3.5 |
6.1 |
4.9 |
3.7 |
2.5 |
| Place of death |
|||||
| Care and nursing institution |
3.4 |
6.5 |
5.3 |
3.7 |
2.5 |
| Hospital |
4.9 |
6.3 |
5.9 |
4.7 |
3.6 |
| At home, other |
2.7 |
2.9 |
3.0 |
2.6 |
2.2 |
| Cause of death (ICD-10 codes) |
|||||
| Circulatory disease (I00-I99) |
3.1 |
2.7 |
3.7 |
3.4 |
2.7 |
| Malignant neoplasm (C00-D48) |
5.6 |
7.1 |
6.3 |
5.2 |
3.9 |
| Respiratory disease (J00-J99) |
4.2 |
6.4 |
6.0 |
4.4 |
3.0 |
| External causes (S00-Y98) |
2.9 |
1.9 |
2.8 |
3.6 |
2.8 |
| All other causes |
2.8 |
3.7 |
3.7 |
3.0 |
2.1 |
For all places of death, the frequency of admission declined with increasing age at death. Furthermore, the average number of admissions varied with the groups of causes of death: 3.1 admissions/3 years among those who died from circulatory diseases, compared to 5.6 admissions/3 years among those who died from malignant neoplasms and 4.2 admissions/3 years among those who died from respiratory diseases. The variations by age at death were unsystematic when death was caused by a circulatory disease or external causes, but when death was caused by a malignant neoplasm, respiratory disease or other disease, the number of admissions over the three-year period clearly declined with increasing age at death.
The results from the multivariate analysis (Table 3) concurred with the findings in the bivariate analyses with regard to variations by gender, age at death, place of death and groups of causes of death. Individuals with education at university college or university level had a statistically significant (p-value < 0.05) higher likelihood of hospitalisation during their last three years of life than those who had only primary/lower secondary education (IRR = 1.02). There was also a significantly higher frequency of admissions in the Western Norway Health Authority (IRR = 1.07) and the Northern Norway Health Authority (IRR = 1.04) when compared to the South-Eastern Norway Health Authority. Immigration status had no significant effect on the frequency of admission.
Table 3
Multivariate Poisson regression analysis of the number of admissions to somatic hospitals during the final three years of life: incidence rate ratios (IRR) and 95 % confidence intervals (95 % CI), significant coefficients in bold type
| IRR |
(95 % CI) |
|
|---|---|---|
| Men (reference) |
1 |
|
| Women |
0.94 |
(0.93–0.95) |
| Age at death 56–65 years (reference) |
1 |
|
| Age at death 66–75 years |
0.96 |
(0.94–0.97) |
| Age at death 76–85 years |
0.80 |
(0.79–0.82) |
| Age at death 86–95 years |
0.62 |
(0.61–0.64) |
| Place of death |
||
| Care and nursing institution (reference) |
1 |
|
| Hospital |
1.25 |
(1.24–1.27) |
| At home, other |
0.71 |
(0.70–0.72) |
| Group of causes of death (ICD-10 main chapters) |
||
| Circulatory disease (I00-I99) (reference) |
1 |
|
| Malignant neoplasm (C00-D48) |
1.53 |
(1.51–1.55) |
| Respiratory disease (J00-J99) |
1.30 |
(1.28–1.33) |
| External causes (S00-Y98) |
0.93 |
(0.90–0.96) |
| All other causes/diseases |
0.91 |
(0.89–0.92) |
| Primary/lower secondary school (reference) |
1 |
|
| Upper secondary school |
1.00 |
(0.99–1.01) |
| University college/university |
1.02 |
(1.01–1.03) |
| Non-immigrant (reference) |
1 |
|
| Immigrant |
0.99 |
(0.96–1.02) |
| South-Eastern Norway Health authority (reference) |
1 |
|
| Western Norway Health Authority |
1.07 |
(1.05–1.08) |
| Central Norway Health Authority |
0.99 |
(0.97–1.00) |
| Northern Norway Health Authority |
1.04 |
(1.03–1.06) |
Discussion
While previous Norwegian studies have investigated the number of hospital admissions before death in a one-year perspective (8, 9), this study has focused on the final three years of life. In the earliest period (31–36 months before death), the sample had 0.3 admissions on average. The admission frequency rose slightly in the subsequent six-month periods. One likely reason why the frequency of admissions starts increasing as early as two years before death is that many fatal disorders develop slowly over several years, as has been shown by international studies (6, 16). In the final year of life, the frequency of admissions increased to an average of 1.6 in the final six-month period that preceded death. The impact of proximity to the time of death on the use of hospital services was shown by the fact that 42.1 % of the 136 484 admissions analysed by this study occurred during the included persons' last six months of life.
As in previous studies, we also found that the number of hospital admissions in the final period of life declined with higher age of death. Those who died at the age of 56–65 had 5.2 admissions on average during their final three years of life and 2.3 admissions during their last six months, compared to 2.8 and 1.1 respectively among those who died at the age of 86–95.
However, the oldest group (age at death 86–95 years) accounted for 28.3 % of all admissions, compared to 14.4 % for the youngest group (age at death 56–65), since the oldest group was more than three times more numerous than the youngest.
Those who died because of a malignant neoplasm had 5.6 admissions on average during their final three years of life, compared to 3.1 among those who died from a disease of the circulatory system. International studies have also shown similar variations between groups of causes of death in terms of their use of hospital services before death (10–12).
The composition of the causes of death cannot explain the declining frequency of admission as age at death increases. There was, however, an unsystematic age pattern for deaths caused by circulatory diseases, but otherwise there were fewer admissions the higher the age at death, if the death was caused by a malignant neoplasm, respiratory disease or another disease.
Most likely, there are a number of reasons why the oldest patients have fewer hospitalisations in their final stage of life. Patients and their next of kin may be sceptical of the strain that further treatment would involve and prefer death with dignity with no unnecessary life-prolonging treatment. Previous research has also raised the question of whether a kind of 'age rationing' is taking place (8, 10), either in the form of informal age discrimination or as a result of resource use being adapted to what is expected to be of benefit to the patient.
The average figures conceal major individual differences. 14.1 % of the persons in the sample had no hospital admissions during their final three years of life. Previous studies have shown that relatively large amounts of hospital resources are devoted to a minority of the patients (13, 17). This is clear also in our data, since more than 40 % of the admissions occurred among those relatively few (13.3 %) who had eight or more admissions.
Since the frequency of admissions to somatic hospitals declines with increasing age at death, it is conceivable that the use of hospital services in the final period of life will be reduced per patient on average as the typical age at death increases. However, the level of use will be affected by multiple factors, such as new medical technology and changes in the composition of causes of death. An increasing level of education might perhaps give rise to increasing expectations for treatment at the final stage of life. In addition, increasing life expectancy and more elderly people in the population will most likely give rise to an increased use of both home-based services and care institutions.
In our material, the use of hospital services among the oldest (age at death 86–95 years) was relatively modest, but two-thirds of the deaths among them occurred in nursing homes. A Finnish study found that even though the use of hospital services immediately before death declined among the very oldest patients, the use of nursing homes would increase to such an extent that the total cost of institutionalisation in the final stage of life would increase in pace with rising life expectancies (3). Should a greater proportion of the deaths be caused by dementia-related diseases, the consequence could be fewer hospitalisations in the period prior to death, but longer periods of stay in nursing homes.
A strength of this study is its basis in nationwide registry data of high quality. Attrition and measurement error with regard to such key variables as age at death or hospitalisation will not be a major source of error, but erroneous classifications of causes of death may occur (18).
One key limitation is that this study only focused on the number of admissions, while types of treatment or other aspects of the hospitalisation were not analysed. A key challenge to the interpretation is that these analyses could not distinguish between admissions that were directly related to diseases that finally caused the person's death on the one hand and admission caused by conditions that were unrelated to the death of the person.
- 7.
OECD. Public spending on health and long-term care: a new set of projections. OECD Economic Policy Papers No 6. Paris: Organisation for Economic Co-operation and Development, 2013.
- 9.
Godager G, Gregersen FA. The association between age and mortality related hospital expenditures. Nordic Journal of Health Economics 2014; 2: 203 - 18.
- 13.
Christensen BJ, Gortz M, Kallestrup-Lamb M. Medical spending in Denmark. Fisc Stud 2016; 37: 461 - 97 . [CrossRef].. [CrossRef]
- 14.
Helsedirektoratet. ICD-10: Den internasjonale statistiske klassifikasjonen av sykdommer og beslektede helseproblemer. Oslo: Helsedirektoratet, 2015. https://helsedirektoratet.no/Lists/Publikasjoner/Attachments/743/Lcd-10-den-internasjonale-statistiske-klassifikasjonen-av-sykdommer-og-beslektede-helseproblemer-2015IS-2277.pdf (26.2.2018).
- 15.
Eurostat. European Shortlist for Causes of Death, 1998 (COD SL-1998). http://ec.europa.eu/eurostat/ramon/nomenclatures/index.cfm?TargetUrl=LST_CLS_DLD&StrNom=COD_1998&StrLanguageCode=EN&StrLayoutCode=HIERARCHIC (10.7.2017).
- 17.
Karlsson M, Klein TJ, Ziebarth NR. Skewed, persistent and high before death: Medical spending in Germany. Fisc Stud 2016; 37: 527 - 59 . [CrossRef].. [CrossRef]