MAIN MESSAGE
The prescribing of asthma drugs to children varied substantially between counties.
Few children used asthma drugs continuously over long periods of time
The results may indicate variations in treatment practices that are not in line with the guidelines
Recurrent episodes of airway obstruction or coughing are very common during the first years of life. In most children younger than 4–5 years, these symptoms will be transient, but such episodes may also be the first indication of asthma (1). Because few objective diagnostic tests of children younger than 4–5 years are available, the guidelines for treatment of asthma in these children are largely based on assessment and interpretation of various aspects of their history and a clinical examination (1–3). This may lead to differences in treatment. From the age of 5–6 years, the children can more easily perform pulmonary function tests, providing a higher degree of diagnostic accuracy (3).
Inhaled steroids are the main controller drug for asthma. In previous studies, we have shown that the prescribing of inhaled steroids for children aged 0–5 in Norway increased until 2010 (4) before declining (5). The prescribing rate was highest for the youngest children (4), in contrast to what is observed in the UK, where the rate of children who are prescribed inhaled steroids increases with age (6). It also contrasts with what might be expected in light of asthma prevalence (7).
We and others have also shown that few children use inhaled steroids continuously over long periods of time (5, 8, 9). This may indicate that asthma drugs are prescribed for transient symptoms of obstructive airway diseases other than chronic asthma (10), and not invariably in compliance with Norwegian and international guidelines (3, 11).
Figures from the Norwegian 'Barnehelseatlas' ('Child Health Atlas') shows that the number of consultations in the specialist health service for children diagnosed with asthma varies considerably from one region to another (12). With some exceptions, these regions coincide geographically with the counties. The 'Child Health Atlas' underscores that this variation is unlikely to have been caused by geographic variations in morbidity or general framework conditions such as inequality in education or income (12). Whether or not the prescribing of asthma drugs also varies between different Norwegian regions is unknown.
The objective of this study was therefore to investigate whether the prescribing of asthma drugs for pre-school children (0–4 years) and early school age (5–9 years) varied between Norwegian counties and to study whether these variations had changed during the period 2004–15.
Material and method
In this descriptive study, asthma drugs prescribed by a doctor and dispensed from a pharmacy in the years 2004–15 to children in the age groups 0–4 years and 5–9 years were studied for Norway as a whole and for each county separately. Data were retrieved from the Norwegian Prescription Database, which contains records of all prescribed drugs dispensed from Norwegian pharmacies since 1 January 2004 (13).
The drugs are classified by an ATC code (Anatomic-Therapeutic-Chemical code) (14). The following variables were used: the patient's national identification number (encrypted), age, place of residence (county), date of dispensing of the drug, ATC code and the specialty of the prescribing doctor. The following drugs (ATC code) were included: selective beta-2-adrenoreceptor agonists for inhalation (R03AC), glucocorticoids for inhalation (R03BA), adrenergics in combination with corticosteroids for inhalation (R03AK) and leukotriene receptor antagonists (R03DC).
The analyses were performed with Stata, version 14.
Definitions
A 'prescribing' was defined as a single dispensing of a drug from a pharmacy. The 'prescribing rate' was defined as the number of individuals per 1 000 inhabitants who had at least one prescribing within a calendar year. The denominator was the mean population figure per age and county, retrieved from Statistics Norway.
Drug groups
We divided the most common combinations of asthma drugs dispensed to patients over a single year into four groups – Group 1: Only short-acting beta-2-adrenoreceptor agonist; Group 2: leukotriene receptor antagonist with or without short-acting or long-acting beta-2-adrenoreceptor agonist; Group 3: long-acting beta-2-adrenoreceptor agonist with or without short-acting beta-2-adrenoreceptor agonist; Group 4: inhaled steroid with or without short-acting/long-acting beta-2-adrenoreceptor agonist or leukotriene receptor antagonist.
The prescribing rates for these combinations per year are presented as averages for the years 2012–14.
Categories of users of inhaled steroids
The children who were dispensed inhaled steroids on at least one occasion in 2012 were followed for three years and divided into three mutually exclusive user categories based on the frequency and time between the dispensings.
A 'single user' received only one dispensing. A 'sporadic user' received at least two dispensings, but did not use the drug continuously and was defined by having an interval of at least 182 days between the dispensings. A 'continuous user' had a maximum interval of 182 days between each dispensing.
Specialty of the prescribing doctor
The prescribing rate for inhaled steroids was further subdivided into mutually exclusive groups according to the type of specialist that had written the prescription for each child and estimated as an average of the prescribing rate for the years 2012–14.
'Paediatrician' also included specialty registrars in hospitals, and 'general practitioner' (GP) also included specialty registrars outside hospitals. The third group consisted of other specialties.
Results
Proportions and types of drugs prescribed
There were major variations between the counties in terms of their prescribing rates for asthma drugs averaged over the period 2012–14 (the 0–4 age group: median 104 children with prescriptions per 1 000 children in the population, range 64–147; the 5–9 age group: 68/1 000, 46–86) (Figure 1). In both age groups, the lowest proportions of children to whom asthma drugs were prescribed were found in Rogaland and Sør-Trøndelag counties and the highest in Aust-Agder county.
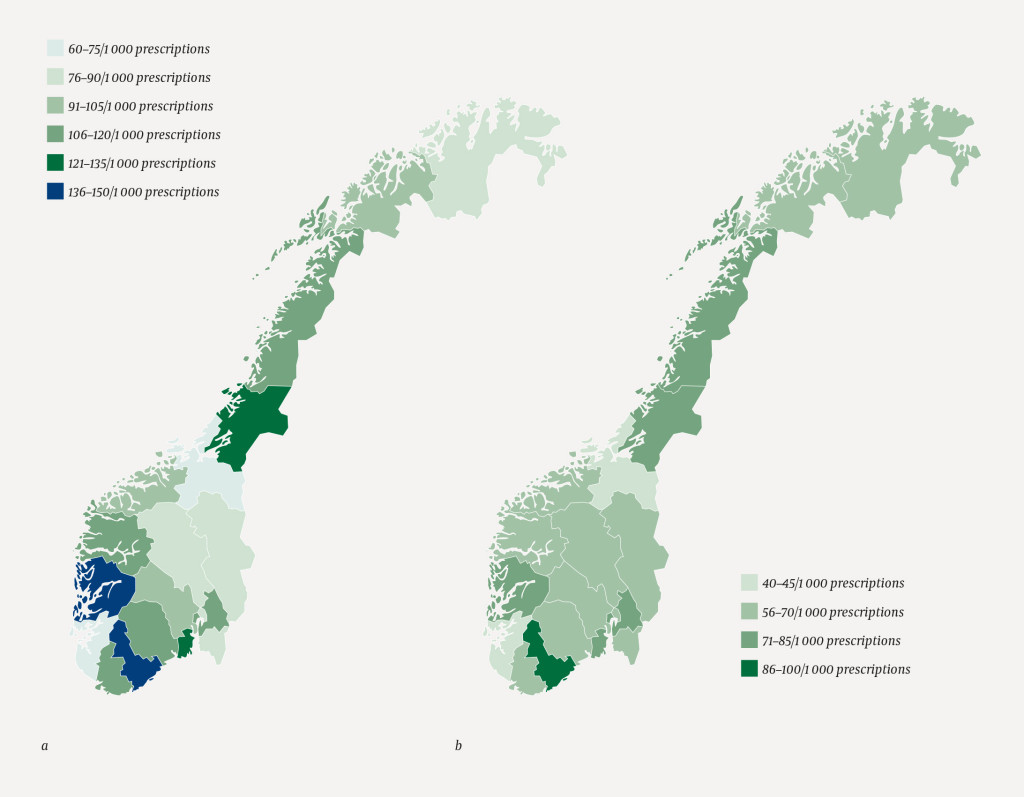
In all counties and both age groups, inhaled steroids alone or in combination with other asthma drugs were the most frequently prescribed drug types. The variations between the counties were highest for this group of drugs (the 0–4 age group: 85/1 000, 42–116; the 5–9 age group: 51/1 000, 31–70) (Figure 2). There were considerable differences in dispensings between some neighbouring counties (Rogaland versus Hordaland counties and Sør-Trøndelag versus Nord-Trøndelag counties).
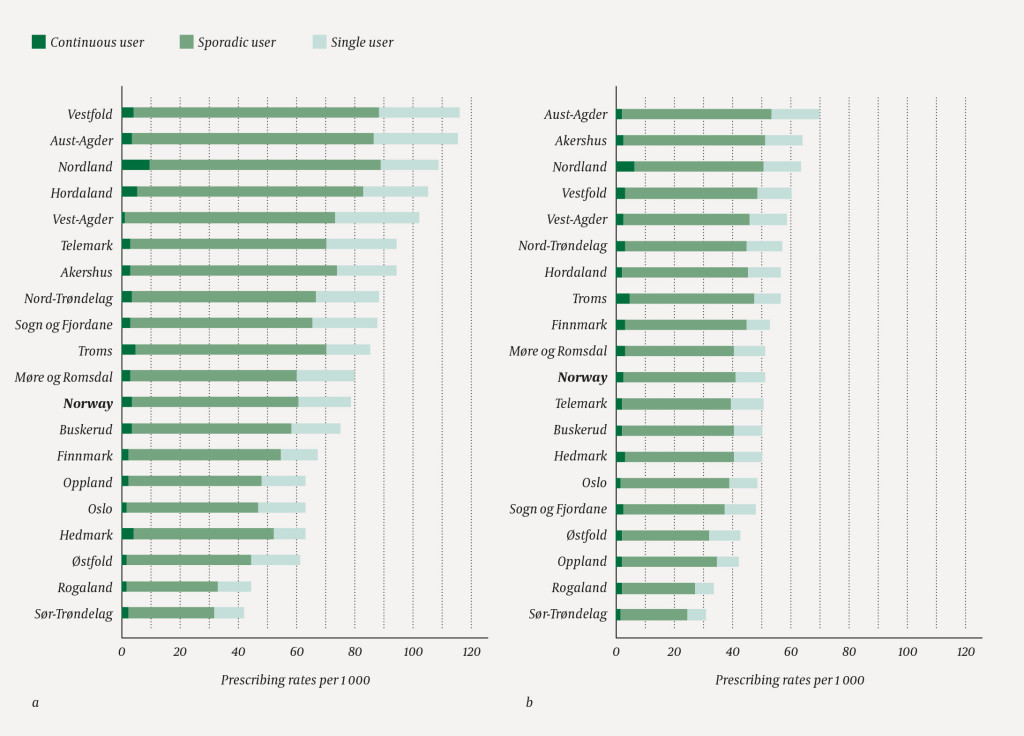
There were few prescriptions of leukotriene receptor antagonist alone or in combination with other asthma drugs (the 0–4 age group: 1/1 000, 0–4; the 5–9 age group: 1/1 000, 1–4). The prescribing of short-acting beta-2-adrenoreceptor agonists alone also varied between the counties, but less so than for inhaled steroids (the 0–4 age group: 17/1 000, 11–38; the 5–9 age group: 12/1 000, 9–18). There were < 1/1 000 prescriptions of long-acting beta-2-adrenoreceptor agonists with or without short-acting beta-2-adrenoreceptor agonist in both age groups.
For the most frequently used drugs, there were more prescriptions to children in the 0–4 age group than in the 5–9 age group in all counties. In all counties and both age groups, there were few children who were continuous users of inhaled steroids (age group 0–4: median 3/1 000, range 1–10; age group 5–9: 2/1 000, 1–6) and many who were sporadic users (age group 0––4: 62/1 000, 30–84; age group 5–9: 38/1 000, 23–52) (Figure 2). This was observed both in counties with a high prescribing level and in counties with a low total prescribing level.
Changes in the use of inhaled steroids in the counties over time
Nationwide, the prescribing of inhaled steroids for the age group 0–4 years increased from 2004 (60/1 000) to 2010 (85/1 000) before declining again until 2015 (71/1 000) (age group 0–4 years, Figure 3). In the entire period, the prescribing rate was higher for the age group 0–4 years than for the age group 5–9 years. In the age group 5–9 years, the prescribing rate increased from 2004 (44/1 000) to 2007 (56/1 000) when it stabilised before declining slightly from 2010 (55/1 000) to 2015 (49/1 000) (no figure shown).
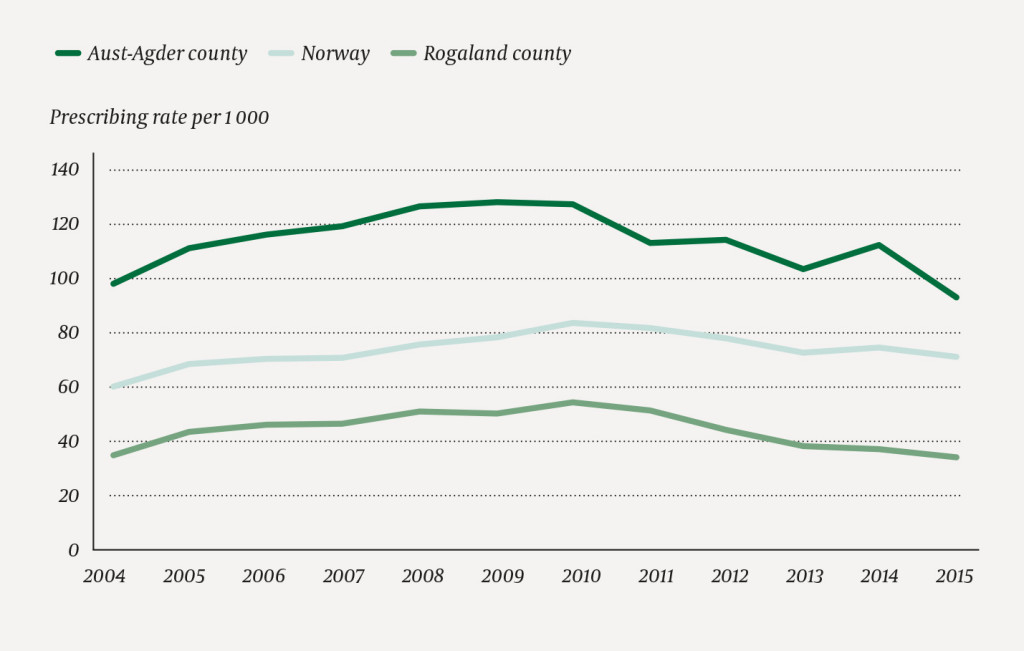
The changes in prescribing practices over time varied considerably between the counties, and for the age group 0–4 years in particular. Some counties had a low prescribing rate with minor changes over time, other counties had a high prescribing rate with minor changes over time, whereas in other counties there were major variations during the period.
Specialties of the prescribing doctors
GPs prescribed more than paediatricians to both age groups (0–4 years and 5–9 years: GPs – 46/1 000 and 32/1 000; paediatricians – 28/1 000 and 17/1 000) (age group 0–4 years, Figure 4). The GPs prescribed more to both age groups in most counties, with the exception of Akershus, Oslo and Sør-Trøndelag counties, where paediatricians prescribed more.
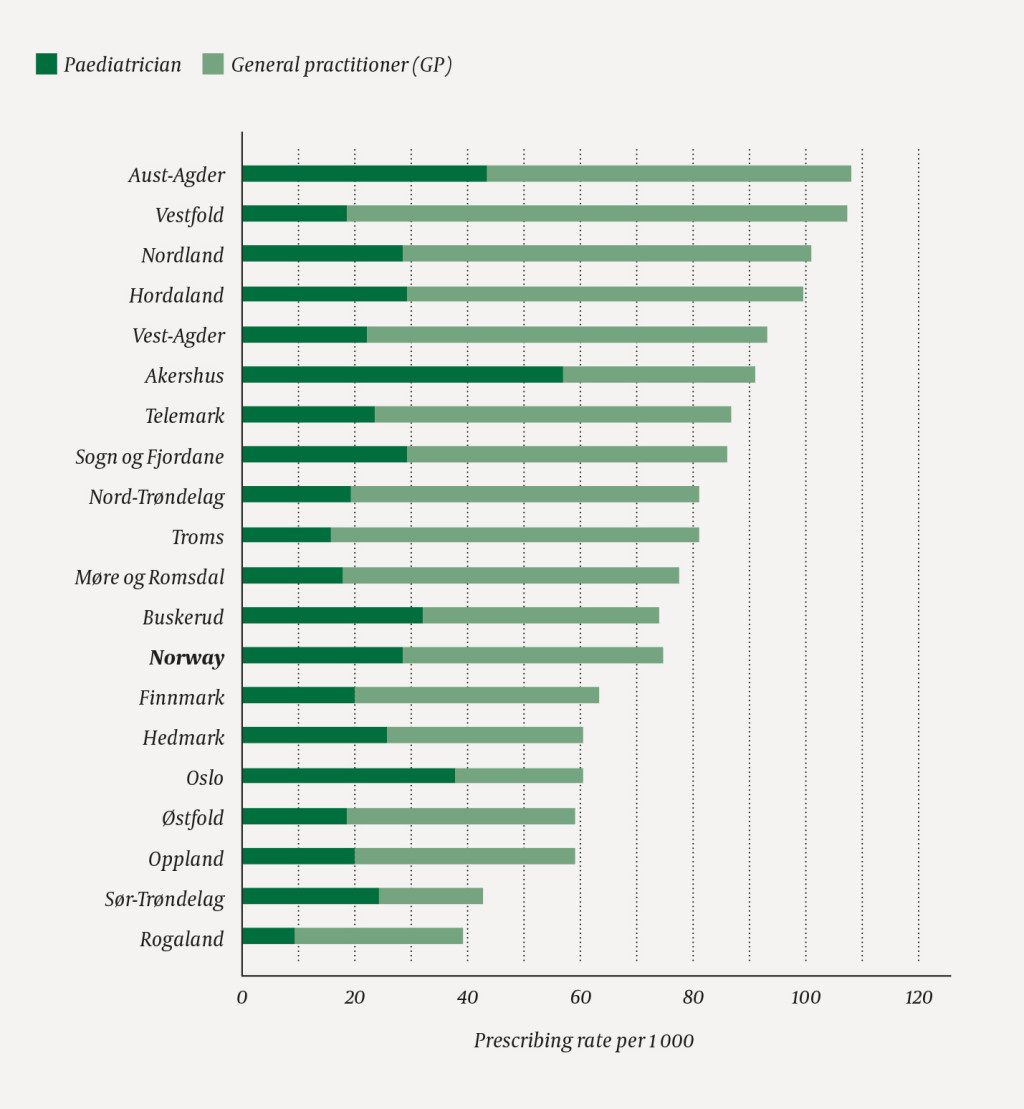
The proportion of children aged 0–4 who were prescribed inhaled steroids by a paediatrician was six times higher in Akershus county than in Rogaland county. A similar pattern was found for the age group 5–9 years. In none of the counties did other specialists write more than 5/1 000 prescriptions (no figure shown).
Discussion
There were considerable variations between Norwegian counties in the prescribing of asthma drugs for children. This included inhaled steroids, which are the most important drugs for treatment of asthma.
The proportion of children who were prescribed with asthma drugs was higher in the age group 0–4 years than in the age group 5–9 years, and the county-wise variations were largest in the youngest group. Most of the children in both age groups were prescribed inhaled steroids only once or a few times during a three-year period.
Differences in prescribing practices between the counties
There is little reason to assume that these substantial differences in prescribing practices between the counties are caused by differences in asthma prevalence. One study shows some variations in asthma prevalence in children living in different regions in Norway, but no variation between urban and rural districts (15). Two recent studies show approximately identical prevalence of asthma in Oslo and Northern Norway in children aged 10–11 (16, 17).
This descriptive study cannot accurately explain the causes of the variations that we have found. It is difficult to determine how much of the variation between the counties in the use of health services and prescribing of drugs is due to natural variation, and how much is due to systematic inequalities in the provision of medical services or medical practice (12, 18).
Wennberg describes three different groups of health services where different preconditions may give rise to variations (18). The first group includes health services that have clear diagnostic criteria. In this group, large variations may be caused by differences in prevalence or actual undertreatment in some locations. We believe that chronic obstructive airway symptoms in children do not fall into this group.
The second group encompasses variations in supply-sensitive health services. The 'Child Health Atlas' shows that in Akershus county and the Vestre Viken health region there is a high number of specialist consultations for asthma, but these regions do not belong to the counties with the highest prescribing rates for asthma drugs. The number of consultations for asthma is lowest in Vestfold county, although this county has a high prescribing rate for asthma drugs. In Rogaland county there are few consultations as well as a low prescribing rate. The figures are not directly comparable, but they may indicate that consumption of, and access to, health services offers limited explanation for the considerable differences between the counties in the prescribing of asthma drugs to children.
The third group encompasses variations caused by preference-sensitive health services and includes diagnoses with unclear treatment criteria, causing preferences, local practice and subjective opinions to influence the choice of treatment, occasionally even in conflict with good, evidence-based practice (18). This may be an important reason for the variations that we found between the counties, because a diagnosis of asthma in pre-school children in particular is based on an assessment of the history and a clinical examination, and to a lesser extent with the aid of objective diagnostic tests.
There are various Norwegian guidelines for treatment of asthma in children, such as the Generell veileder i pediatri ('General manual of paediatrics') from the Norwegian Paediatric Association (11) and the Norsk legemiddelhåndbok ('Norwegian Medicines Guide') (19). In addition, international guidelines from the Global Initiative for Asthma (3) are used; these are updated more frequently than the guidelines from the Norwegian Paediatric Association.
No studies have yet assessed whether these guidelines are precise and operational, nor what status they have among doctors. Nevertheless, our results indicate a need for clearer Norwegian guidelines for diagnosis and treatment of asthma in children, equivalent to the guidelines in the UK, which contain detailed diagnostic criteria as well as a specific review of examination and treatment (20).
Continuous versus sporadic use of inhaled steroids
In this study, a continuous user needed to be dispensed with an inhaled steroid only once every six months. However, there was a very low proportion of this user category in both age groups, including in the counties with a low total prescribing rate. This finding is in line with results from previous Norwegian (5, 21) and international studies (8, 9). In Australia, approximately 40 % of children and adults were provided with a single prescription for inhaled steroids combined with oral antibiotics, which may indicate that inhaled steroids are prescribed for transient obstructive airway symptoms (10).
Many preschool children have recurrent episodes of obstructive airway disease that later turns out not to be asthma (1, 3). It can be difficult to determine which of these children have asthma and will respond to treatment. This may open the way for a therapeutic trial of inhaled steroids as suggested by guidelines (3, 11), and this may be the reason why some receive only one prescription.
On the other hand, this cannot explain why the prescribing rate in the youngest age group is significantly higher in Norway than in a number of other countries (5), nor the high level of sporadic use observed in the age group 5–9 years, where asthma is easier to diagnose.
The age group 0–4 years versus the age group 5–9 years
For the most important asthma drugs, the prescribing rate and the variations over time were higher in the age group 0–4 years than in the age group 5–9 years. More than half of all children with asthma-like symptoms triggered by viral infections of the respiratory tract do not have asthma and should thus not be treated with inhaled steroids (3, 11, 20).
Atopic sensitisation is a key factor in order to assess whether children with chronic obstructive lower airway symptoms in fact have asthma and should start treatment with inhaled steroids (7). The prevalence of atopic asthma is higher in older children than in younger children (2), and we would thus expect that the proportion of children treated with inhaled steroids would increase with age, as found for example in the UK (6). Asthma drugs are free of charge to children in both Norway and the UK, so different reimbursement schemes cannot explain this difference.
Specialty of the prescribing doctor
In all counties except Sør-Trøndelag, Oslo and Akershus, GPs prescribed more inhaled steroids than paediatricians and other specialists. In Oslo and Akershus counties this may be due to better access to specialists in private practice than in other parts of the country, and that more children with asthma are consequently followed up by private specialists, as shown in the 'Child Health Atlas' (12).
Our data cannot identify whether specialists issue more correct prescriptions than GPs. On the other hand, the considerable variation among paediatricians may also indicate that diagnosis and treatment of asthma largely depend on the treatment practices of the individual doctor, irrespective of specialty.
Strengths and weaknesses
Data from the Norwegian Prescription Database provide accurate information on all dispensed asthma drugs, and more reliable results than we might have obtained from a sample of the population of children in Norway. However, the figures do not show whether the drugs were used as prescribed, nor the diagnosis on which each prescription is based.
We have chosen to study differences in prescribing practices between counties and not between major population concentrations, as the 'Child Health Atlas' does (12). Some of the differences between the counties that are observed in this study would have evened out if we had grouped them in larger regions. GPs in the same county belong to, refer to and normally consult with the specialist health service in the same region, and it is thus natural to regard each county as an entity.
Data from Statistics Norway show that the proportion of children in the different age groups and their gender ratio vary little between the counties (22). In our analyses we have therefore used prescribing per 1 000 children in two age groups, rather than age and gender standards. Using the average annual proportion over three years also helps reduce the effect of random variations.
Conclusion
There is considerable variation between Norwegian counties in terms of prescribing of asthma drugs to children. The results may indicate that major differences in treatment practices have evolved, and that the treatment is not always in line with applicable guidelines.
A low number of continuous users and major variations in treatment over time may indicate that asthma drugs are frequently prescribed for obstructive airway symptoms other than asthma. There is a need for uniform guidelines for the treatment of asthma in children in Norway, and they ought to be implemented in the specialist health services as well as in general practice.
- 3.
From the Global Strategy for Asthma Management and Prevention, Global Initiative for Asthma (GINA). 2016. www.ginasthma.org (22.9.2016).
- 9.
Ingemansson M, Wettermark B, Jonsson EW et al. Adherence to guidelines for drug treatment of asthma in children: potential for improvement in Swedish primary care. Qual Prim Care 2012; 20: 131 - 9. [PubMed]
- 11.
Norsk barnelegeforening. Generell veileder i pediatri. www.helsebiblioteket.no/retningslinjer/pediatri/%C3%B8vreog-nedre-luftveier/astma-bronkiale (14.7.2016).
- 12.
Helse Nord. Barnehelseatlas. www.helseatlas.no/mer-om-barnehelseatlas (14.7.2016).
- 14.
WHO Collaborating Centre for Drug Statistics Methodology. Guidelines for ATC Classification and DDD Assignment 2016. www.whocc.no (14.7.2016).
- 19.
Norsk legemiddelhåndbok. www.legemiddelhandboka.no/Terapi/søker/+%2Bastma/14403 (1. 3.2017).
- 20.
British Thoracic Society. BTS SIGN Asthma Guidelines. www.brit-thoracic.org.uk/guidelines-and-quality-standards/ asthma-guideline (14.7.2016).
- 22.
Statistics Norway Statistics Norway. 2017. Statistics Norway Statistics Norway. http://www.ssb.no/natur-og-miljo/statistikker/agassn/aarforelopige/2014-05-14?fane=tabell&sort=nummer&tabell=177124 (15.1.2017).