MAIN MESSAGE
Interns in Finnmark experienced professional growth and a sense of mastery through the general practice internship.
The doctors wanted better skills in leadership and communication.
An efficient emergency primary health care service chain in the first phase of serious illness or injury is critical to ensuring that the population receive prompt and competent assistance in acute situations. The municipal out-of-hours service and local emergency medical communication centres are important elements in the initial stages of the chain, together with non-medical personnel, the medical emergency number 113 and the ambulance service.
In pre-hospital emergency medicine, the local emergency medical communication centre and the Emergency Medical Communication Centre operators decide whether or not the on-call doctor should be notified along with the ambulance service (1). The regulations concerning requirements for emergency primary health care services (Forskrift om krav til akuttmedisinske tjenester utenfor sykehus) require the municipal out-of-hours scheme to cover the need for emergency assistance, in addition to duty doctors being available via the Nødnett Helse 'health radio' station (2). It is also a requirement that the parties involved facilitate training in teamwork (2).
It has previously been shown that duty doctors in the municipal health service do not always take part in call-outs where the level of urgency is acute. There may be several reasons why this is the case (3, 4). Factors such as the establishment of ever-increasing inter-municipal out-of-hours districts, greater distances, fear of simultaneity conflicts, more independent and better trained ambulance personnel, geographic conditions and lack of warning can all influence the doctor's decision.
The aim of this study was to investigate newly qualified doctors' expectations and attitudes with regard to participation in call-outs and their experiences with acute situations and call-outs after completing their general practice internship in a large county with large distances to the hospitals.
Material and method
The informants were made up of all 23 interns in the general practice internship arrangement in Finnmark county during the period September 2015 to February 2016. Everyone took part in the first interview, and 21 took part in the second interview, with two unable to attend. They were divided into three groups based on the location of their workplace. Recruitment to the study took place via the interns' supervisors in the general practice internship.
The interviews were conducted at planned meetings at the start of the internship at three locations in the county, outside the hospitals. Two of the groups' second interview round was conducted at the final internship meeting, while the third group was interviewed in a video conference.
Questionnaire
The interns answered a questionnaire before starting the general practice internship. The questionnaire was devised following a literature search and based on the authors' collective experiences. In the questionnaire, the interns described their confidence levels in relation to their own skills and future participation in call-outs (Figure 1).

We used a Likert scale based on the values 1 (no command of skills) and 10 (very good command) to describe how confident they felt about their own skills in emergency medicine and how confident they felt when they had to attend a call-out with ambulance personnel (1 = not confident, 10 = confident) (5). The interns described in a free text field what emergency medicine skills they wished they had practised more before having to attend call-outs.
The questionnaires were distributed immediately prior to the start of the general practice internship.
Focus group interview
The focus group interviews were conducted at the start and at the end of the general practice internship in the municipal health service with the same group of interns (6). They were divided into three groups based on their geographical location in the county. The group size varied between five and eight.
Two interviews were held per group; a total of six interviews, at the start and at the end of the general practice internship. The groups were located in Eastern, Central and Western Finnmark. The interviews took between 34 minutes to one hour. All were conducted by one of the authors (KHH). The interview guide is shown in Boxes 1 and 2.
Box 1 Questions discussed during the focus group interview with interns before the general practice internship
The following questions were used to guide the informants during the interview at the start of the general practice internship:
-
How do you feel about/what are your thoughts on being called out by the doctor-ambulance alarm?
-
What do you think will influence your decision on whether to attend a call-out or not?
-
What do you think the greatest challenges will be when taking part in a call-out?
-
How do you think you could have been better prepared for this task?
Box 2 Questions discussed during the focus group interview with interns after the general practice internship
The following questions were used to guide the informants during the interview after completion of the general practice internship:
-
What challenges have you faced in connection with emergency ambulance call-outs?
-
Did you ever decide not to take part in a call-out? If yes, why?
-
What has influenced your decision about whether to attend?
-
How could you have been better equipped for the task?
The interviews were recorded in audio files and transcribed verbatim immediately after completion (KHH). Further coding and analysis were conducted by KHH and TW using the grounded theory method (7).
We identified words and phrases of meaning in the transcribed text (indicators), and these were sorted into categories describing common qualities. These in turn were divided into main categories, and finally into one core category. The quotes and categories were reviewed in conjunction with the transcribed data in several rounds in order to ensure that the analysis reflected the actual content of the interns' statements.
Ethics
The Regional Committee for Medical and Health Research Ethics (REC) for the Northern Norway Regional Health Authority did not consider it necessary to submit the study for approval (12.5.2015 2015/827/REC North), and the Norwegian Centre for Research Data (NSD, formerly Norwegian Social Science Data Services) confirmed that registration was not necessary (conveyed by telephone in May 2015). All informants agreed to participation after receiving written information and signed the consent form before the interviews. All data was anonymised.
Results
Questionnaire
The results of the questionnaire before the general practice internship showed that the interns had most confidence in their ability to safeguard clear airways and in chest compression, but felt they had not mastered intraosseous infusion or pleural aspiration (Figure 2, Table 1).
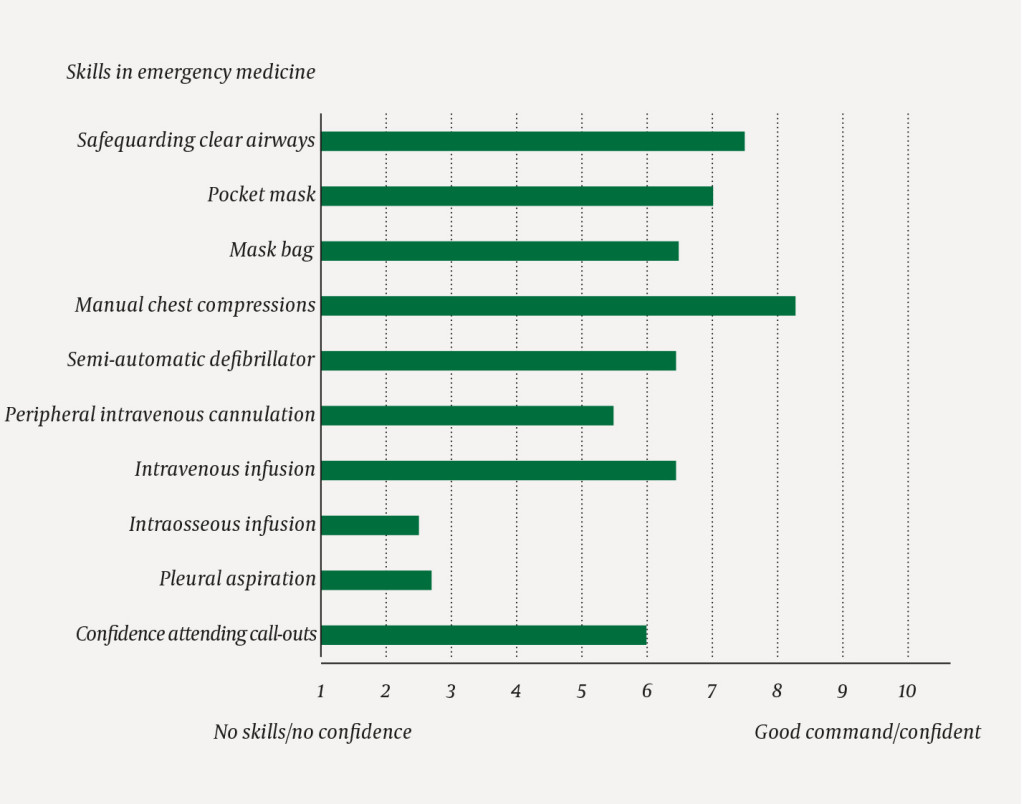
Table 1
Interns' wishes for further training before starting the general practice internship, specified in the free text field in the questionnaire. 23 respondents. No. of times mentioned = number of times the wish is stated in the free text fields
| Skill | No. of times mentioned |
|---|---|
| Teamwork training | 5 |
| Paediatric cases | 3 |
| Primary investigation | 2 |
| Endotracheal intubation | 2 |
| Administering thrombolytic treatment | 1 |
| Dealing with visible bleeding | 1 |
| Vacuum splint and mattress | 1 |
| Dealing with epilepsy | 1 |
| Administering medication | 1 |
Focus group interview
Interview before general practice internship. The first focus group interviews with the interns resulted in the core category 'Can I do anything useful?'. This core category was further classified into the subcategories 'Experience', 'Skills', 'Logistics', 'Confidence in other occupational groups' and 'Own considerations'. These categories are described in more detail below.
'Experience'. The interns had a general belief that experience and knowledge of the patients could contribute to doctors deciding not to take part in call-outs. They drew parallels to hospital internship, where they were uncertain at first, but became more experienced during the period. The doctors were tense and nervous before heading into the new work situation, and their thoughts were filled with the responsibility they would be faced with and a fear of being superfluous.
Participation in call-outs has no doubt something to do with how much experience you have. So, I will not dare to say no. Doctors who are more experienced are, however, more likely to say, 'no, I've come across this one before, I see them when they come to my practice for consultations.' (Woman 1, Group 2)
'Skills'. There was general agreement among the participants that they had received adequate training in most practical skills. Working with experienced ambulance personnel was considered to create a good sense of security. Nevertheless, they would like to have spent more time practising medication management, peripheral intravenous cannulation, intubation, advanced cardiopulmonary resuscitation and dealing with critically ill children prior to the general practice internship.
I think it's fair to say that we have generally been trained well in most aspects of internship work. (Man 2, Group 2)
Before the hospital internship, we had one review of AHLR when we started the clinical internship. If we were not involved in cardiac arrest during the six-month internship, then there were no further opportunities to practise. So, in order to be better prepared, it may be beneficial to include more frequent AHLR exercises. (Woman 3, Group 1)
'Logistics'. In Finnmark, there are major geographic and weather-related challenges. Fear of simultaneity conflicts was a key factor in decisions not to take part in call-outs. The interns believed that they had little to contribute when there was only a short distance to the accident and emergency department or hospital, and felt that the response time may be longer if they had to be collected first.
If I am notified about a patient who seems stable, I may have to assess whether the situation is serious or important enough for me to warrant letting the rest of the municipality's population go without a doctor for two hours. (Woman 2, Group 1)
'Confidence in other occupational groups'. Due to the ambulance personnel's local knowledge and medical expertise, the interns had particular confidence in this group and felt a sense of security when attending call-outs with them. Several mentioned that they had little training in teamwork and team leadership. This could be a contributing factor to the uncertainty.
The little time I've spent working with ambulance personnel ... They've seen everything! ... Often more than once. So you really lean on them. At least when you're out on a call. So, the medical side is not what worries me the most, because I know that they're very good to have around! (Man 3, Group 3)
'Own considerations'. The interns had the idea that duty doctors down-prioritise ambulance call-outs out of consideration for their own working conditions. Most hospital doctors in general practice in Finnmark have to go to work the next day and have a full list the day after their shift at the accident and emergency department. The doctors envisaged that the strain of this could make them refrain from taking part in call-outs. In addition, they had experienced episodes and heard stories about a drug and psychiatric community in the county that could be difficult to handle pre-hospital.
If I was to ask for any training, I could see myself taking a psychiatry/substance abuse course. Because that's what I think is most uncomfortable, and we haven't had much about that ... although I covered it a bit at the hospital. But how to handle it up here and how to assess suicidality and so on is really difficult. (Woman 4, Group 3)
Interview after general practice internship. By analysing the focus group interviews conducted after the internship, 'It all went well in the end' emerged as a core category. This was further explained by the subcategories 'Experience', 'Skills', 'Logistics' and 'Confidence in other occupational groups'.
'Experience'. The interns described that experience had helped them to feel more confident in their clinical work, in the new role and in teamwork. The fear that the doctors held before starting the general practice internship diminished in most cases, and they felt better equipped to assess the need to participate in call-outs.
Much of it is like an algorithm, so once you've been exposed to it you're slightly more relaxed the next time. (Woman 1, Group 3)
I used to think, if someone takes ill on the plane, what would I do? But now I'm more inclined to think that it will be okay. So I feel that I have learned something ... (Woman 2, Group 3)
Some of the local authorities in Finnmark have local guidelines stipulating that duty doctors must take part in call-outs when the doctor-ambulance alarm is raised. The interns in these municipalities therefore participated on all call-outs where the level of urgency was acute. This applied to a few of the interns. Others received requests from the Emergency Medical Communication Centre to attend and had to make an independent decision.
Some of the interns reported that they had occasionally refrained from taking part in call-outs, but nevertheless thought they had a lower threshold for attending than the more experienced doctors, who have more knowledge about the patients.
We notice that we have a much lower threshold for going on call-outs than the other doctors who are in permanent positions. Some of these others never participate in call-outs. (Man 1, Group 2)
I have opted not to take part, and prefer for the patients to be brought to the acute admissions ward for examination. But these are often patients that you have in ten times with the same symptoms, and each time it's been shown that there is no somatic illness. (Woman 1, Group 1)
'Skills'. The doctors learned that the role of a medical officer outside hospitals was very time-consuming. They also found that participation in specific treatment was less of a requirement. This meant a reduced need for practical skills.
Good training was needed in skills in connection with abuse and rape, and how to handle patients in the most vulnerable situations was something that they lacked.
Often, if there is a situation where a lot of things need to be done at once; a catheter needs to be fitted, and blood tests taken ... If you had to do all the practical things, it would take a very long time. And there are other things that you need to do first, like taking the patient's anamnesis, taking written notes, making some phone calls ... (Man 1, Group 3)
'Logistics'. Challenging weather and geographic conditions combined with a lack of resources meant that it was difficult to solve logistical problems. The doctors therefore had to work with several different services in the area. On short call-outs, several of the doctors chose instead to examine the patients at the accident and emergency department rather than taking part in the call-out, with a view to shortening the call-out time and because they felt that they had nothing more to contribute before and during transportation to the accident and emergency department.
Administration and logistics ... It's hard ... It's perhaps the most difficult thing about the whole job. It takes such a long time. If the patient is severely ill and you have to wait, that's stressful. That's the worst thing about being a duty doctor I think. (Woman 3, Group 3)
Where I work, I have had to request a snow plough to get us to a call-out. (Man 2, Group 2)
Several of the interns found that their main job on call-outs was to talk on the phone. Nevertheless, some of them considered logistics to be part of the clinical assessment, where one is dependent on the other.
You need to explain the background to their condition at least three times; first to the Emergency Medical Communication Centre in Kirkenes, then the one in Tromsø, and then a duty doctor in Kirkenes, maybe the University Hospital of North Norway, and then maybe you need to tell a duty medical officer as well as a surgeon. That's how the story can start to change ... You spend a lot of time on the phone. (Woman 2, Group 3)
'Confidence in other occupational groups'. The interns reported that they were surprised at how well the cooperation with the ambulance personnel went. They felt they had the competence to contribute beyond the level of the ambulance personnel and that they were respected for this.
I was really surprised how well it went and how well they accepted a younger doctor, an inexperienced doctor. I expected to be a bit railroaded, but once I showed that I was getting a handle on things and I started giving a few orders, it went really well! (Man 2, Group 2)
The cooperation with the Emergency Medical Communication Centre was a challenge – both cases of communication failures and cases where the operators railroaded the interns on issues regarding transport and call-outs.
I have had to argue once with the Emergency Medical Communication Centre. But ultimately, you need to establish who is in charge. I don't remember exactly what was wrong with the patient, but I wanted air transport. Then there was another operator who became very argumentative. So I said I cannot force them to send a helicopter, but I said I would enter in the medical record that they had responsibility for the patient in that case. No, I couldn't do that. So I got a helicopter in the end. (Man 1, Group 2)
In some places in Finnmark, the police are not available in the community around the clock. Long call-out times led to difficult situations in connection with the work of the interns. Having to wait for the police in situations that involve people with substance abuse and psychiatric issues represented a challenge to the personal safety of the doctors and other parties involved.
We had to wait for the police from somewhere else. A man was threatening to shoot himself, and said that if we approached him he would shoot everyone in sight. So we sat there and waited for the police. Not very cool. (Woman 2, Group 1)
Discussion
This study shows that interns on general practice internships in Finnmark during the period September 2015 to February 2016 felt that they became more confident in their abilities and in the clinical work through attending call-outs as part of their general practice internship. They felt better equipped to assess the need to participate in call-outs and found that they had an important – and manageable – role as a doctor during call-outs. It seems that the decision about whether to participate in a call-out or not may have been founded on a more solid basis during the general practice internship. Before starting the internship, the interns generally felt they had a good enough command of most practical skills. Throughout the internship, they found that this indeed was the case, but that practical tasks outside hospitals, and particularly on call-outs, were often not their primary focus (8).
The questionnaires showed that the interns felt confident in their skills, such as manual heart compressions and safeguarding clear airways, but were not as confident with regard to intraosseous infusion and pleural aspiration in cases of pneumothorax. The interns felt remarkably little confidence in their skills in peripheral intravenous cannulation, which is a relatively common procedure. They were generally moderately confident in relation to emergency ambulance call-outs. The free text responses showed that teamwork training in particular was a skill they would have liked to have mastered better. The role of the doctor in the team, communication and cooperation, particularly with ambulance personnel, were mentioned specifically.
It is thought-provoking that the doctors felt they had an inadequate command of practical skills, such as intravenous cannulation, and of non-technical skills. Mastering how to work in a team and being a good communicator are core management skills in emergency medicine and something that interns should feel confident about before starting their general practice internship.
This small study cannot be used to compare medical schools or hospital internships, and the participants in the general practice internship undertook their earlier hospital internship in different health trusts. In this context, it is strange that the general training in teamwork that is imposed on local authorities and health trusts pursuant to the regulations concerning requirements for emergency medical services outside hospitals is rarely carried out (2).
The purpose of the study was to try to obtain a better understanding of why duty doctors in the municipal health service do not always participate in emergency call-outs (9, 10). Because the study is qualitative and not intended for generalisation, the findings cannot simply be transferred to other accident and emergency doctors. The study only includes newly qualified doctors and therefore does not describe the other more experienced doctors. We believe, however, that our findings may be of importance to the training and preparation of doctors in hospital internships and may raise their awareness of their role in the general practice internship.
This qualitative analysis is based on the grounded theory method (7). Due to the design of the study, with the need to attend initial and final meetings for the interns, it was not possible to meet the requirement for a successive analysis of each data collection before the next, and the number of informants was limited to all interns in a particular year. We believe, however, that the analysis was robust and that we achieved saturation, whereby the views in the group are represented in our description.
Conclusion
The participating interns were generally satisfied with their own practical skills before the general practice internship. Skills such as intravenous cannulation, leadership and communication were areas they required more training in. During the internship, the fear of being superfluous or useless in an emergency call-out turned into a sense of being able to master the situation, particularly with regard to logistics and patient assessment.
The interns found that they benefitted considerably from a close cooperation with the ambulance personnel and felt they were respected and valued on call-outs. They found themselves better able to make an assessment when it was appropriate to participate in a call-out.
- 1.
Den norske legeforening. Norsk indeks for medisinsk nødhjelp. 3. utg. Stavanger: Laerdal Medical, 2009.
- 2.
Forskrift om krav til og organisering av kommunal legevaktordning, ambulansetjeneste, medisinsk nødmeldetjeneste mv. (Akuttmedisinforskriften). 2015. Kapittel 2, § 6; kommunens ansvar for kommunal legevaktordning. https://lovdata.no/dokument/LTI/forskrift/2015-03-20-231 (8.11.2017).
- 3.
Momyr M, Kindt PG. Akuttmedisinske hendelser utenfor sykehus. Hovedoppgave. Trondheim: Institutt for sirkulasjon og bildediagnostikk, Det medisinske fakultet, Norges teknisk-naturvitenskapelige universitet, 2011.
- 5.
Pell G. Use and misuse of Likert scales. Med Educ 2005; 39: 970 –, author reply 971. [PubMed] [CrossRef]
- 6.
Malterud K. Fokusgrupper som forskningsmetode for medisin og helsefag. Oslo, Universitetsforlaget, 2012.
- 7.
Hartman J. Grundat teori, teorigenerering på empirisk grund. Lund: Studentlitteratur, 2001.