Suicides, mental health care and interdisciplinary specialised addiction services in the Agder counties 2004–13
MAIN MESSAGE
64 % of those who committed suicide had previously been in contact with mental health care or interdisciplinary specialised addiction services
46 % of them had had such contact during the year preceding their suicide, and 29 % had contact at the time of the suicide
We found that a large proportion of those who had no such contact were younger than 20 years
The group that had completed their treatment included a larger proportion of patients with adjustment disorders, while there was a larger proportion of patients with psychotic disorders in the group that remained in treatment
Each year, more than 500 Norwegians take their own life. This figure is four times higher than the number of road traffic fatalities in 2015 (1). The causes of suicide are complex, difficult to investigate and only partly understood (2, 3). Each suicide has its own history, and each suicide has a major impact on those affected (4).
Approximately 90 % of those who take their own life suffer from one or more mental disorders at the time of their suicide (5–8). Most mental disorders are associated with an elevated risk of suicide (9–11).
Treatment is available for many disorders, for example severe depression, a condition which is associated with a high risk of suicide. However, many of those who take their own life have never been in contact with mental health care or interdisciplinary specialised addiction services. A meta-analysis from 2002 reviewed 40 studies of people who had died from suicide (12). It showed that three-quarters of them had been in contact with a GP over the previous year, while only one-third had been in contact with mental health care.
In the UK, suicides and homicides associated with mental health care have been registered through The National Confidential Inquiry into Suicide and Homicide by People with Mental Illness (NCISH) (13). More than 10 000 suicides were investigated over the period 1996–98. Approximately 24 % of those affected had been in contact with mental health care during the year prior to their suicide (14). The proportion with contact has since increased from 27 % in 2003 to 30 % in 2013 (15).
In Norway, collation of data from the Cause of Death Registry and the Patient Registry for the period 2009–11 showed that 42 % had been in contact with mental health care during the year prior to their suicide (16). However, this study reported only contacts in general, with no specification of the type or time of the last contact. Moreover, there is a considerable overlap between patient groups in interdisciplinary specialised addiction services and mental health care, and a study of suicides in these groups thus ought to include both of these parts of the specialist health service.
Measuring the extent to which suicides are prevented inside and outside the health services is no easy task. On the other hand, preventive work is a general goal for health policy, and obtaining information about those who commit suicide is thus important for our ability to undertake targeted interventions. To be able to assess the potential effect of any measures to prevent suicides and evaluate them after implementation, it is also crucial to ascertain whether the suicide victims have had any contact with the health services.
The objective of this study was to identify the proportion of people who had taken their own life while being in treatment or had been in contact with mental health care or interdisciplinary specialised addiction services at any time during their life or in the last year prior to their death. We also wished to describe demographic and diagnostic characteristics of the group that had had such contact.
Material and method
The study population
Information on all persons who were registered as resident in Aust-Agder or Vest-Agder counties and died from suicide in the period 2014–13 was retrieved from the Cause of Death Registry. Altogether 330 such deaths had been recorded over this period.
In this period, the suicide rate in Norway amounted to 11.6/100 000/year. The equivalent rate amounted to 11.8/100 000/year for Vest-Agder county and 12.3/100 000/year for Aust-Agder county (17). The average population in this period was 167 506 in Vest-Agder and 107 211 in Aust-Agder county.
Data collection
Items in the information from the Cause of Death Registry included personal identification numbers, place and date of death, marital status and ICD-10 codes for the underlying cause of death. The personal identification number was used to clarify whether the deceased had an electronic patient record at Sørlandet Hospital. These records contain information on all contacts with somatic health services, mental health care and interdisciplinary specialised addiction services. All parts of the records were included in the data collection. If no notes were found in the electronic records, a search was undertaken to retrieve the paper-based records based on the personal identification number in the electronic archive of paper-based records and in the physical archive.
The data collection consisted of a review of the patient records accompanied by completion of a form retrieved from The National Confidential Inquiry (18), adapted and translated into Norwegian at the National Centre for Suicide Research and Prevention. The form included questions about social situation, diagnosis, treatment history and type of care at the time of death, previous self-harm or attempted suicide, drug abuse and suicide method. The English version of the form is available online (17); the Norwegian translation can be obtained from the authors on request.
The data collection was undertaken by two psychiatrists and a specialist in psychology. If multiple diagnoses were found in the patient record, the most recent main diagnosis was chosen. The length of the illness period was based on the time of the first referral to mental health care or interdisciplinary specialised addiction services at Sørlandet Hospital. In cases where it was discovered that the patient had received previous treatment in another health institution, this information was used in the calculation.
Ethics
The study was approved by the Regional Committee on Medical and Health Research Ethics (REK South -East, ref. no. 2014/417). The committee granted exemption from the duty of confidentiality for access to personal information on the cause of death from the national registry, as well as for access to records at Sørlandet Hospital with no requirement for consent from the next of kin. Sørlandet Hospital is the institution responsible for the research project.
Statistics
The data analysis was performed with the aid of SPSS Statistics 22.0 for Mac (IBM Corp.). The results are presented descriptively in the form of numbers and percentages, with standard deviations as the measure of dispersion. Chi-square and t-tests were used to compare groups on the basis of demographic variables. Linear regression analysis was used to investigate changes in the proportion with contact during the period. The significance level was set to 0.05.
Results
Altogether 330 suicides were registered in Aust-Agder and Vest-Agder counties in the period 1 January 2004–31 December 2013. Of these, 198 (60 %) were resident in Vest-Agder county, and 230 of them (69.7 %) were men. Their average age was 42.3 years (SD 18.5), 22.1 % were married, 51.5 % were unmarried, while 26.3 % were divorced, separated or widowed. We had access to 329 patient records, and the remaining results are based on these.
A total of 219 of the 329 suicide victims (66.6 %) had been in contact with mental health care and/or interdisciplinary specialised addiction services at least once during their lifetime. This also includes contact in the form of psychiatric liaison consultation in somatic wards. For 56.6 %, the last contact took place in mental health care, while 10.0 % had their last contact with interdisciplinary specialised addiction services.
Table 1 provides an overview of the proportions that had any contact with mental health care or interdisciplinary specialised addiction services during their lifetime or in the year immediately prior to their suicide. Altogether 46.2 % had such contact during their final year, 28.6 % had contact with treatment institutions on an ongoing basis, while 17.6 % had discontinued their contact during their last year. The latter group includes those who had completed a regular course of treatment as well as those who had contact only in the form of psychiatric liaison consultations in a somatic ward.
Table 1
Overview of contacts with mental health care or interdisciplinary specialised addiction services at any time in life and in the last year prior to suicide in the period 2004–2013 in the Agder counties. The table also shows the gender distribution in the various groups
| Number (%) |
Women |
Men |
Age in years |
||
|---|---|---|---|---|---|
| Suicides included in the study |
329 (100) |
100 (30.4) |
229 (69.6) |
42.3 (18.5) |
|
| Contact with mental health care or interdisciplinary specialised addiction services at any time in life |
219 (66.6) |
72 (32.9) |
147 (67.1) |
43.5 (17.0) |
|
| Contact with mental health care or interdisciplinary specialised addiction services during the last year |
152 (46.2) |
49 (32.2) |
103 (67.8) |
44.2 (16.9) |
|
| Ongoing treatment |
94 (28.6) |
31 (33.0) |
63 (67.0) |
40,6 (14,9) |
|
| Contact discontinued during the last year |
58 (17.6) |
18 (31.0) |
40 (69.0) |
50,2 (18,3) |
|
| No contact with mental health care or interdisciplinary specialised addiction services during the last year |
177 (53.8) |
51 (28.8) |
126 (71.2) |
40.8 (19.8) |
|
Altogether 41.0 % of those who had any contact during their last year had contact with mental health care, while 5.2 % had their last contact with interdisciplinary specialised addiction services. The table also shows the average age of the groups. There was a significant difference between the groups: the group that remained in treatment was significantly younger than the group that had discontinued their contact (p = 0.001).
The proportion that had contact with mental health care or interdisciplinary specialised addiction services per year in the period in question ranged from 33 % to 73 %. Linear regression analysis showed a tendency towards an increase in the proportion of people who had been in contact over the period (R2 = 0.35; p = 0.071).
Of those who had any contact over their final year, 67.8 % (n = 103) were men, while the proportion of men who had not had any contact amounted to 71.2 % (n = 126). This difference was not significant (p = 0.501). There was a slight tendency towards a lower average age in the group that did not have any contact in their final year (= 40.8) compared to the group that had been in contact (= 44.2), p = 0.089).
Figure 1 shows the proportion that had been in contact with mental health care or interdisciplinary specialised addiction services during the last year prior to their suicide, in different age groups. There was a tendency towards age differentiation (p = 0.052) – among those who did not have any contact, a larger proportion was younger than 20 years.
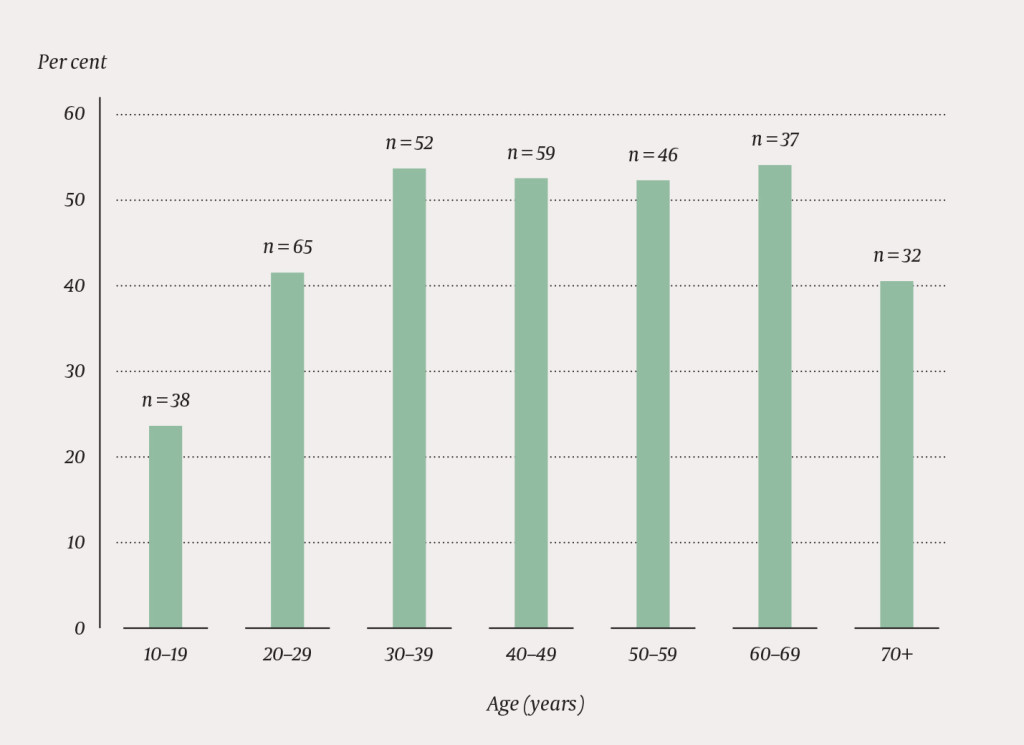
The further analyses are based on data from patient records for those 152 people (46.2 %) who had been in contact with mental health care or interdisciplinary specialised addiction services over the last year prior to their suicide.
Of these 152 patients, altogether 63 (41.4 %) had been in contact during the last seven days, while 98 people (64.5 %) had been in contact over the last 30 days, and 120 (78.9 %) had been in contact over the last three months. This corresponds to 19.1 %, 29.8 % and 36.5 % respectively of all those who died from suicide in the general population.
More than half of the patients who had been in contact during the last year prior to their suicide (n = 78; 51.3 %) had a history of illness going back more than five years, while for 32 (21.1 %) this amounted to 1–5 years and 32 (21.1 %) had a history of illness with a duration of less than 12 months. For ten patients (6.6 %) we had insufficient information to determine the length of their histories of illness.
Altogether 124 people (81.6 %) had been admitted to an inpatient unit one or more times during their lifetime. Of these, 106 (69.7 %) had been admitted during the last year, 14 (9.2 %) took their own life within seven days after discharge, 33 (21.7 %) did so within 30 days after discharge and 13 (39.4 %) had discontinued their treatment at discharge.
For 58 of those 152 patients (38.2 %) who had been in contact during the last year prior to their suicide, the treatment had been discontinued before the suicide occurred or had involved only a single consultation, for example in the form of a psychiatric liaison consultation. For ten (6.6 %) of these, the last contact occurred during the last week prior to the suicide, for 20 (13.2 %), the last contact occurred within the final 30 days, and for 31 (53.4 %) within the final three months.
Altogether 94 patients (61.8 %) were in ongoing contact with mental health care or interdisciplinary specialised addiction services at the time of their suicide. Of these, 24 (25.5 %) were hospitalised or on leave, equivalent to 15.8 % of all those who had been in contact for purposes of treatment. A total of 55 patients (58.6 %) were under outpatient follow-up. 15 patients (16 %) were receiving ambulatory or outpatient treatment, or were waiting for their treatment to start at a new institution.
Figure 2 shows the distribution of main diagnoses for all those who had been in contact with mental health care or interdisciplinary specialised addiction services during the year prior to their suicide. Depression was the most frequent diagnostic group, in the group that was undergoing treatment as well as in the group that had discontinued their treatment. In the group that was undergoing treatment, psychotic disorders and substance use disorders were among the three most frequently occurring, while adjustment disorders and substance use disorders were among the most frequent in the group that had discontinued their treatment.
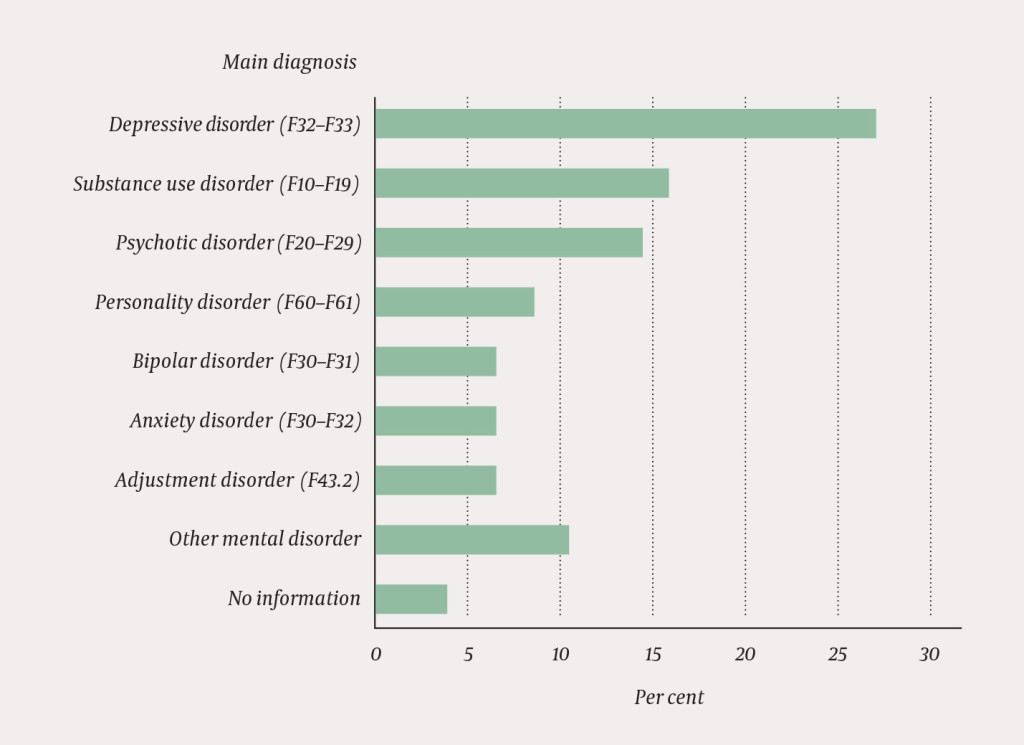
There was a significant difference in the distribution of main diagnoses (p = 0.036) between the group that was attending treatment and the group that had discontinued theirs. The material did not permit any further analyses to specify the diagnostic groups within which there were significant differences in occurrence.
Discussion
This study shows that two-thirds of those who died from suicide in Aust-Agder and Vest-Agder counties in the period 2004–2013 had been in contact with mental health care or interdisciplinary specialised addiction services at any point during their lifetime. Slightly less than half had been in such contact during the last year prior to their suicide. Approximately one-third of all those who committed suicide had been in contact with mental health care or interdisciplinary specialised addiction services during the last 30 days before the suicide took place.
The proportion with contact represents a minimum estimate, since some may have lived and received treatment in other counties without having received any treatment after relocating to the Agder region. Nor do we have any overview of the contacts that these patients may have had with psychiatrists or psychologists in private practice, but the number is likely to be low, since there are very few professionals in private practice in the Agder counties.
The proportion that had been in contact during the last year prior to their suicide is higher than what has been found in the UK (14) and other countries (12), while the proportion in this study corresponds to findings made in a previous Norwegian study (16). We found a tendency towards an increasing proportion with contact through the period 2004–2013. For such a small catchment area, this is an uncertain finding, although it corresponds to the trend that was observed in the UK over the same period (19).
The observation that a greater proportion had contact with the specialist health service in Norway compared to the UK can be interpreted in different ways. This may be due to differences in the forms of organisation, design and consumption of health services. Moreover, it can be an indication that the health services in Norway are more dispersed and more easily available, for example as a result of the escalation plan for mental health care (20).
Data from The National Confidential Inquiry in the UK shows that the suicide rate declines in areas where the national recommendations for expansion of the services are followed, according to a study that compared suicide rates in 1998 and 2006 in light of the measures that had been implemented in various regions. The measures that had the greatest impact were a 24-hour, easily accessible health service for people in crisis, measures for persons with dual diagnoses and an interdisciplinary review in the aftermath of each suicide incident with a view to learning (21).
In Norway as well, the health authorities have initiated national initiatives for suicide prevention in the health services, such as the National guidelines for suicide prevention in mental health care (22) and a national campaign for patient safety directed at acute wards (23). These measures came into force much later than their UK equivalents, and their effects have not yet been systematically evaluated.
There were no significant differences in terms of gender distribution between the group that had been in contact in the final year and the group that had had no contact with mental health care or interdisciplinary specialised addiction services. There was a slight tendency towards a lower average age in the group with no contact; the age distribution shows that there was a larger proportion of people younger than 30 years in this group. Special measures should therefore be considered for this group in particular, to ensure increased contact with the health services.
More than half of the patients had a history of illness dating back more than five years. This must be deemed a conservative estimate, since the estimation of the duration is fraught with some uncertainty because some may have attended treatment in other health enterprises. Four of every five had been admitted to an inpatient mental healthcare unit or interdisciplinary specialised addiction services at least once during their lifetime. In combination with the distribution of diagnoses, this indicates that a major proportion of the patients suffered from serious and to some extent long-term mental health problems.
Approximately one in every six patients who had undergone treatment during the last year took their life during hospitalisation, while one in every five took their life within one month after discharge from an inpatient unit. The proportion of suicides during hospitalisation is higher than what was found in the UK (19). The reason could be that patients in Norway are more frequently admitted to inpatient facilities in general. Another reason could be that in recent years, special emphasis has been placed on suicide prevention during hospitalisation in the UK. This has resulted in a 60 % reduction in this group (19). National guidelines exist also in Norway in this area (22), but their impact is as yet unknown.
Approximately one-third of the patients who had been in contact with treatment institutions over their final year were no longer in treatment in the specialist health service at the time of their suicide. On average, this group was older than the group that remained in treatment. The proportion suffering from psychotic disorders was greater in the group that remained in treatment and the proportion with adjustment disorders was greater in the group that had discontinued their treatment. As regards the psychotic disorders, the explanation could be that these patients frequently receive long-term follow-up by the specialist health service.
The large proportion of persons with adjustment disorders in the group that had discontinued their treatment may stem from a number of issues. Adjustment disorders are by definition time-limited, so it should come as no surprise to find more patients with completed therapies in this diagnostic group. Another explanation could be that insufficient diagnostic assessment was made to detect other mental disorders, such as depression, addiction or personality disorders.
One area for further studies could be to validate the use of adjustment disorders in this context, especially in delimiting personality disorders, post-traumatic stress disorder and depression, and study specific risk factors for suicide in this population.
A strength of this study is that it was based on the entire population of two counties. Sørlandet Hospital has a high coverage rate in mental health care and interdisciplinary specialised addiction services, and all treatment provided by the health trust is documented in a shared electronic records system. For people who did not have an electronic patient record, searches were undertaken in the paper-based records. Old records archives are exposed to a somewhat higher risk of archive misplacement, meaning that we cannot know for certain that all relevant records were identified. The Cause of Death Registry provides a good overview of suicides in Norway, and we regard the identification procedure at Sørlandet Hospital as reliable.
The weaknesses of the study are primarily associated with our basing the data collection on records whose main purpose is not research. Some variables, such as the main diagnosis, therefore have uncertain validity. The study's design is primarily descriptive, and the methods of inferential statistics that have been used in the analyses must be assessed in this context. For this reason, the study's findings ought to be validated, for example through an approach based on hypothesis testing.
In the period studied, the suicide rate in the Agder region did not differ significantly from the national rate. However, for many years Sørlandet Hospital has had a somewhat higher proportion of the population as patients in mental health care and interdisciplinary specialised addiction services (24), meaning that the contact estimates for persons who commit suicide may be somewhat elevated. With this reservation, it is reasonable to assume that the results from this study can be generalised to Norway as whole.
- 1.
Veitrafikkulykker med personskade, 2015. https://www.ssb.no/transport-og-reiseliv/statistikker/vtu/aar/2016-05-31 (23.5 2017).
- 15.
The National Confidential Inquiry into Suicide and Homicide by People with Mental Illness. Annual Report. England, Northern Ireland, Scotland and Wales. Manchester: University of Manchester, 2015.
- 17.
Folkehelseinstituttet - Dødsårsaksregisteret Folkehelseinstituttet - Dødsårsaksregisteret. 2016. Folkehelseinstituttet - Dødsårsaksregisteret Folkehelseinstituttet - Dødsårsaksregisteret. http://statistikkbank.fhi.no/dar/ (2.5 2016).
- 18.
The University of Manchester - Centre for Mental Health and Safety. 2016. The University of Manchester - Centre for Mental Health and Safety. http://research.bmh.manchester.ac.uk/cmhs/research/centreforsuicideprevention/nci/sample_questionnaires (10.5 2016).
- 19.
The National Confidential Inquiry into Suicide and Homicide by People with Mental Illness. Making Mental Health Care Safer: Annual Report and 20-year Review. Manchester: University of Manchester, 2016.
- 20.
St.prp. nr. 63 (1997–1998). Om opptrappingsplan for psykisk helse 1999–2006. https://www.regjeringen.no/no/dokumenter/stprp-nr-63-1997-98-/id201915/sec1 (25.7.2017).
- 22.
Nasjonale retningslinjer for forebygging av selvmord i psykisk helsevern. IS–1511. Oslo: Helsedirektoratet, 2008. https://helsedirektoratet.no/Lists/Publikasjoner/Attachments/3/Nasjonal-faglig-retningslinje-for-forebygging-avselvmord-i-psykisk-helsevern-IS-1511.pdf (25.7.2017).
- 23.
Brudvik M, Ness E, Walby F. Selvmordsforebygging i akuttpsykiatriske døgnavdelinger - erfaringer fra nasjonalt læringsnettverk. Suicidologi 2014; 19: 7 - 12.
- 24.
Helsedirektoratet - Samdata - Spesialisthelsetjenesten. 2015. https://helsedirektoratet.no/statistikk-og-analyse/ samdata (28.10.2016).