MAIN MESSAGE
Of 41 hospitals, 17 reported having a diabetic foot ulcer team
Only one in three foot ulcer teams used the Norwegian Quality Improvement of Laboratory Examinations' (Noklus) diabetes patient records
Few used written routines for assessment and/or an ulcer classification system
More than half of the foot ulcer teams had planned to undertake interdisciplinary collaboration
Only one in four foot ulcer teams had planned interdisciplinary collaboration with both medical and surgical competence
The prevalence of diabetes mellitus in Norway has risen from 2.5 % in 2005 to 3.2 % in 2011 (1). Foot ulcers are not uncommon in persons with diabetes; two Norwegian studies show that 7 – 10 % of these have had diabetic foot ulcers (2, 3). Diabetic foot ulcers are defined as ulcers below the ankle due to reduced capillary and/or arterial circulation, neuropathy and foot deformities (4). A number of studies show that persons with diabetic foot ulcers report reduced quality of life, that the ulcers contribute to increased morbidity, and are a marker for excess mortality (5, 6). In Norway, 400 – 500 below-the-knee amputations are performed each year as a result of diabetic foot ulcers (7).
According to national and international recommendations, diabetic foot ulcers should be treated by specialised interdisciplinary diabetic foot ulcer teams (8–11). However, these teams are not statutory. Interdisciplinary foot ulcer teams consist of persons with different clinical competencies who collaborate to treat these foot ulcers (12, 13).
The main responsibility of the foot ulcer team is to undertake ulcer treatment through ulcer revision, pressure relief, initiation of antibiotic treatment, measures associated with re-establishment of arterial circulation, and optimisation of blood glucose (8). This is deemed to enable a more systematic treatment of diabetic foot ulcers, a shorter period of healing, and fewer amputations resulting from foot ulcers (14–16).
The teams are assumed to be effective in terms of cost-benefit (17). It is recommended that the foot ulcer teams have both medical and surgical competence, and that clear routines for referral to the teams are in place (8–11). Use of the Noklus diabetes patient records and a structured ulcer classification system, for example the Site, Ischaemia, Neuropathy, Bacterial Infection, Area and Depth (SINBAD) system, are recommended to ensure prevention, follow-up and treatment of diabetic foot ulcers (8). Information stored in the Noklus diabetes patient records is also important for reporting to the national quality register, the Norwegian diabetes register for adults, in order to provide an overview of the quality of diabetes treatment in Norway.
No overview exists of diabetic foot ulcer teams in Norway, the clinical competence that they possess, or the treatment options they provide to patients with diabetic foot ulcers. This renders it difficult to ensure that this patient group receives optimal health care. The purpose of this study was therefore to identify diabetic foot ulcer teams in the specialist health service in Norway, and survey the clinical competence, organisation and work routines of these teams.
Material and method
The study is cross-sectional. Data were collected by means of a questionnaire from October 2015 to February 2016. The criteria for participation were somatic hospitals with 24-hour operations and a specialist function for diabetes mellitus. Of 66 hospitals identified, 51 fulfilled the inclusion criteria and received a questionnaire. Of 51 hospitals invited, we received responses from 41 (80 %).
Based on international and national recommendations for diabetic foot care (9, 13), two questionnaires were developed, A and B. Representatives from the Nordic Diabetic Foot Task Force, the Norwegian Nurses Organisation's Group for Diabetes Specialist Nurses, and the Norwegian Diabetes Association contributed to the design of the questionnaires.
Questionnaire A
Questionnaire A consisted of eight questions that mapped which hospitals have diabetic foot ulcer teams, and how the treatment options for patients with diabetic foot ulcers were organised in hospitals that did not have such teams (iversenengappendiks1).
Questionnaire B
Questionnaire B was answered by hospitals that had diabetic foot ulcer teams. The questionnaire consisted of 40 questions divided into five sections: 1) background information, 2) organisation, 3) resources and treatment options, 4) specialist groups and collaboration, 5) internal work routines and treatment of diabetic foot ulcers in locations other than the hospital (iversenengappendiks2).
The head of the division or department was contacted by telephone or email to obtain permission to conduct the study and to identify the correct contact person to answer questionnaire A. In order to map the teams' competence, collaboration, work routines and treatment options, it was desirable for the respondents to questionnaire B to be permanently assigned to the foot ulcer team and regularly perform ulcer care. The head of the foot ulcer team was therefore responsible for recruitment and authorisation to answer questionnaire B. The completed form was returned by email/mail. To enable reminders to be sent to those who had not responded to the questionnaire, each form was marked with an ID code. The Statistical Package for Social Sciences (SPSS, version 21) was used to analyse the data. The study was approved by the Norwegian Social Science Data Services (2015/44409).
Results
Of the 41 hospitals that answered questionnaire A, altogether 17 hospitals reported having diabetic foot ulcer teams, while 24 hospitals did not have such teams. The 17 hospitals that had diabetic foot ulcer teams were requested to answer questionnaire B.
All the university hospitals reported having diabetic foot ulcer teams, South-Eastern Norway Regional Health Authority had nine foot ulcer teams, Western Norway and Central Norway Regional Health Authorities each had three, and Northern Norway Regional Health Authority had two (Fig. 1). The hospitals had had foot ulcer teams for an average of 13 years.
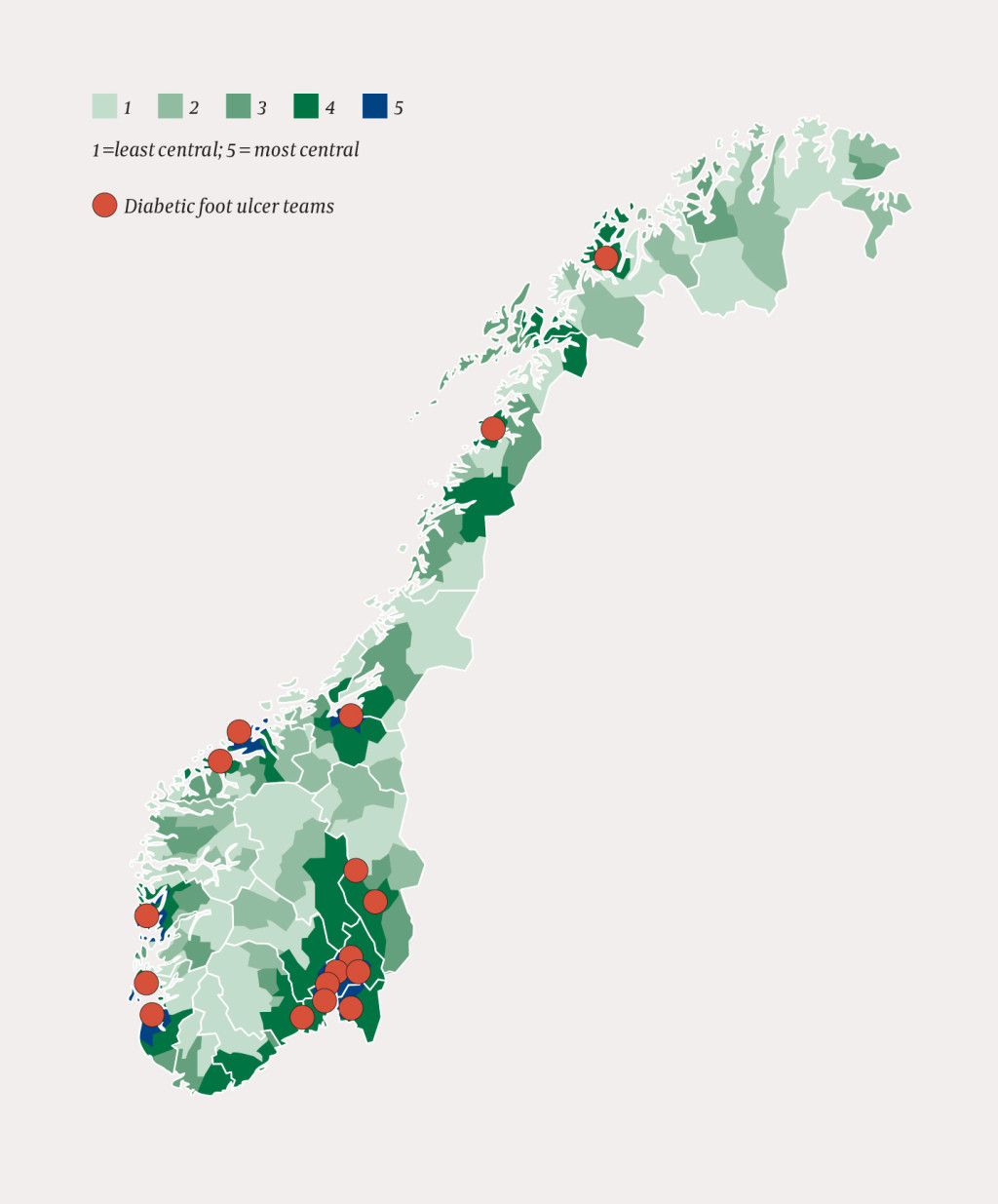
At 15 of the hospitals that did not have diabetic foot ulcer teams, the surgical department was responsible for the outpatient follow-up of patients with these foot ulcers. Twelve of the hospitals that did not have foot ulcer teams also reported that patients were admitted to the surgical ward when they were hospitalised for diabetic foot ulcers.
Organisation and competence
Ten foot ulcer teams were based in the medical department, five in the surgical department, and two were associated with both the medical and surgical departments. The ten foot ulcer teams that were organised in the medical department were led by a specialist in endocrinology, while the remaining seven were led by orthopaedic surgeons (n = 3), ulcer specialist nurses (n = 2), vascular surgeons (n = 1) and specialists in internal medicine (n = 1).
The specialist groups that comprised the foot ulcer teams were an endocrinologist, specialist in internal medicine, orthopaedic surgeon, vascular surgeon, diabetes specialist nurse, ulcer specialist nurse, non-specialist nurse, chiropodist and orthopaedic engineer. The specialist groups that the teams wanted to add were a chiropodist (n = 8), vascular surgeon (n = 6), orthopaedic surgeon (n = 4), diabetes specialist nurse (n = 2), specialist in infectious diseases (n = 1) and orthopaedic engineer (n = 1).
Waiting time and treatment
Six foot ulcer teams had one consulting day per week, while three had one consulting day every second or third week. The waiting time for an initial consultation was one week or less for eight teams, whereas 14 teams reported a waiting time of 2 – 3 weeks or less. The duration of an initial consultation was estimated to be 30 minutes or less for three of the teams, while ten teams estimated from 31 to 60 minutes. There were always two or more clinical specialists (median 4) present during all or part of the initial consultation. At the initial consultation, all the foot ulcer teams always or usually checked for type of diabetes and use of medication, monofilament testing, palpation of foot pulses, size and depth of ulcer, and pressure relief by means of footwear/insoles.
One foot ulcer team only had a diagnostic function, and the patients were followed up by another ulcer outpatient department at the hospital. Regarding follow-up of patients with diabetic foot ulcers, altogether 11 teams followed up patients until the ulcer had healed, and 12 teams had between one and three follow-up consultations with the patients per month. Nine teams also offered preventive ulcer treatment to patients with a high risk of developing diabetic foot ulcers.
Collaboration
Ten foot ulcer teams had interdisciplinary discussions before, during and after the consultation; six of these had meetings that only included specialist groups from their own outpatient department. A total of 11 teams also reported that the patients, in addition to receiving treatment from the foot ulcer team, also received treatment at other outpatient departments. The teams were most satisfied with the collaboration and competence within their own teams (n = 13) and least satisfied with the collaboration and competence outside the teams (n = 12).
In terms of collaboration with the municipal health service, nine foot ulcer teams had written contact with the GP after each consultation, six had written contact with the homecare nurse and five with the nursing homes. None of the foot ulcer teams held consultations in the municipal health service.
Guidelines and documentation
Nine foot ulcer teams had written guidelines for the assessment of diabetic foot ulcers. Five used the Noklus diabetes patient records to document follow-up and treatment of diabetic foot ulcers, none of which were university hospitals. Five foot ulcer teams used the ulcer classification system, whereof none used the SINBAD system.
Discussion
At the initial consultation, all the foot ulcer teams checked neuropathy, circulation, use of pressure-relieving footwear and the degree of severity of the ulcer. This indicates that national and international recommendations are being followed (8–11). With regard to documentation of ulcer treatment, less than one-third used the Noklus diabetes patient records, which implies a lack of structured follow-up data at the individual level, as well as a lack of data on diabetic foot ulcers in the Norwegian diabetes register for adults. This impedes quality improvement efforts and research on diabetic foot ulcers in Norway (18, 19).
Altogether 60 % of the foot ulcer teams had an arena for interdisciplinary collaboration but less than half of these teams had both medical and surgical competence, which is recommended and is deemed to be cost-effective (8–11), (17). This indicates that some foot ulcer teams do not fulfil the requirements for interdisciplinary collaboration. Interdisciplinary collaboration, evidence-based guidelines and standardised treatment pathways are the best method of diagnosing and treating diabetic foot ulcers (8–11), (17), (20–22). The teams are also expected to provide better clinical coordination and use of resources in the treatment and follow-up of diabetic foot ulcers (8). It is thus essential to make provision for more foot ulcer teams to be given an arena for interdisciplinary collaboration.
None of the foot ulcer teams held consultations or monitoring in the municipal health service. As patients with diabetic foot ulcers are often older and have multimorbidity (5), they are often dependent on assistance to attend a consultation in the specialist health service. According to the national clinical guidelines, this can be resolved through the use of telemedicine (8) or by using ambulant foot ulcer teams in combination with telemedicine (21).
Altogether 59 % of Norwegian hospitals that responded to the survey had no diabetic foot ulcer teams. This implies that the service for patients with diabetic foot ulcers is vulnerable. Previous research (14, 17) underlines the cost-benefit effect and the importance of diabetic foot ulcer teams for healing time and the rates of amputation and mortality. It is also pointed out in national professional guidelines for diabetes (8) that diabetic foot ulcer teams can provide better use of resources since a large number of new/alternative treatment methods require experience and competence. It is thus essential to focus on organisation of services for patients with diabetic foot ulcers.
Strengths and weaknesses
A strength of the study is that 80 % of the hospitals participated, which represents a significantly higher participation rate than a study conducted in Denmark (37 %) (22).
A weakness of the study is that one representative from each foot ulcer team answered the questionnaire, which may have affected the study's reliability.
Conclusion
Less than half of Norwegian hospitals that treat diabetes have foot ulcer teams. Norwegian diabetic foot ulcer teams are composed of a broad range of disciplines and have a short waiting time for initial consultations. They follow national and international recommendations in surveying risk factors and treatment of foot ulcers. Half of the foot ulcer teams have planned interdisciplinary collaboration, but few include both medical and surgical competence. The foot ulcer teams do not have structured documentation of the results that they achieve, which may impede quality improvement efforts and research.
We wish to thank the Norwegian Diabetes Association and the Group for Diabetes Specialist Nurses for their participation in the reference group for the study.
- 3.
Iversen MM, Midthjell K, Østbye T et al. History of and factors associated with diabetic foot ulcers in Norway: the Nord-Trøndelag Health Study. Scand J Public Health 2008; 36: 62 - 8. [PubMed]
- 4.
LeMaster JW, Reiber GE. Epidemiology and economic impact of foot ulcers. I: Boulton AJM, Cavanagh PT, Rayman G, red. The foot in diabetes. Chichester, John Wiley & Sons Ltd, 2008: 1-13.
- 7.
Helsenorge.no. Amputasjoner blant personer med diabetes. https://helsenorge.no/kvalitet-seksjon/Sider/Kvalitetsindikatorer-rapporter.aspx?kiid=Amputasjoner_blant_diabetespasienter (22.5.2017).
- 8.
Helsedirektoratet. Nasjonal faglig retningslinje for diabetes. https://helsedirektoratet.no/retningslinjer/diabetes (22.5.2017).
- 9.
International Working Group on the Diabetic Foot. Summary guidance for the daily practice 2015.http://iwgdf.org/guidelines/summary-guidance-for-the-daily-practice-2015/ (22.5.2017).
- 10.
National Institute for Health and Care Excellence. Foot care for people with diabetes overview.https://pathways.nice.org.uk/pathways/foot-care-for-people-with-diabetes/foot-care-for-people-with-diabetesoverview#content=view-node%3Anodes-principles-of-care (22.5.2017).
- 11.
Sundhedsstyrelsen. National klinisk retningslinje for udredning og behandling af diabetiske fodsår. https://sundhedsstyrelsen.dk/da/udgivelser/2013/~/media/54AAA6F78D8B4BF89929A4AFB8B68B0F.ashx (22.5.2017).
- 17.
Kerr M. Foot care for people with diabetes: The economic case for change. NHS Diabetes and Kidney Care 2012
- 18.
Cooper JG, Thue G, Claudi T et al. The Norwegian diabetes register for adults – an overview of the first years. Nor Epidemiol 2013; 23: 29 - 34. [CrossRef]
- 22.
Kirketerp-Møller K, Svendsen OL, Jansen RB. The management of diabetic foot ulcers in Danish hospitals is not optimal. Dan Med J 2015; 62: A5097. [PubMed]