Are stipulated requirements for the quality of maternity care complied with?
MAIN POINTS
All maternity institutions in Norway have introduced selection criteria for determining where pregnant women can give birth
Several maternity institutions lacked written procedures describing the responsibilities of the midwife and attending doctor during births
Only half the doctors' posts at the maternity departments (level 2 birth units) were filled, and some departments had difficulty in meeting the requirement of four-shift rotation of duty, whereby four obstetricians are on duty during the day and one of the four covers the night as well.
There was limited interdisciplinary, mandatory instruction and practical training in the maternity institutions
In 1996, the Norwegian Board of Health Supervision published the report Faglige krav til fødeinstitusjoner [Functional requirements for maternity institutions] (1). The aim was to provide an overview of the functional requirements that should apply to maternity institutions. The report recommended that births should take place at institutions at three levels: level 1 birth units (university hospitals/central hospitals), level 2 birth units (small and medium-sized departments of obstetrics and gynaecology) and level 3 birth units (midwife-managed birth units including modified midwife-managed birth units with preparedness for acute caesarean sections). Minimum requirements were made with respect to the number of births at each level, and emphasis was placed on sound risk assessment and on placing the woman at the right level.
The report formed the basis for the report to the Storting (Norwegian parliament)En gledelig begivenhet [A joyous occasion] (2). Maternity care should be differentiated and decentralised. The division of maternity institutions into three levels should be maintained. Modified midwife-managed birth units should be converted into midwife-managed birth units. The use of birth rates as a criterion for selecting an institutional level should be replaced by quality requirements for maternity institutions.
In 2010, the Directorate of Health published the guide Et trygt fødetilbud – kvalitetskrav til fødselsomsorgen [A safe maternity service – quality requirements for maternity care] (3). The guide followed up the intentions of the report to the Storting, with "quality" applying to requirements regarding organisation, distribution of tasks and functions and competencies, systems for following up the requirements, and requirements regarding information and communication.
The guidelines provide specific selection criteria for births – who can give birth at level 1, level 2 and level 3 birth units. Guidelines are provided for monitoring and treatment of low-risk and high-risk deliveries, including the importance of having clear guidelines for when a doctor must be summoned in connection with complicated births.
It is recommended that the bulk of the permanent staff of level 1 and 2 units should consist of specialists. A succession of locums should be avoided, and the competencies of locums should be checked. The obstetricians should not have more than four-shift rotation, to ensure a minimum number of obstetricians in the department. There is a requirement for level 1 units that the senior on-call doctor must be on duty. There are requirements relating to the use of different types of fetal monitoring, including competencies and instruction for both doctors and midwives. Instruction and practical training in acute situations form part of the requirements.
In 2011, the Journal of the Norwegian Medical Association published a three-year summary by the Norwegian Board of Health Supervision of cases brought before the Board in which the baby died or was severely harmed during delivery (4). The cases showed that there were often mistakes in fetal monitoring, in the summoning of qualified personnel, in rapid delivery of the baby when necessary, and in the duty of the health enterprise to report serious incidents in accordance with the statutory reporting arrangement. A study by the Norwegian System of Compensation to Patients (NPE) revealed similar findings (5).
The Directorate of Health's national guide are intended to be advisory and designed to achieve a professionally acceptable service and a means of ensuring high quality and correct priorities. The regional health authorities and the health enterprises are responsible for ensuring that the service is properly executed and that national guides and guidelines are used and applied in practice. The purpose of this study was to obtain information on the implementation of the guide Et trygt fødetilbud [A safe maternity service] (3) in maternity institutions. The survey was not conducted as a supervisory activity.
Material and method
Information was obtained with the aid of an electronic questionnaire (Questback). The form was based on the Directorate of Health's national guide Et trygt fødetilbud [A safe maternity service] and on input from medical personnel.
The questions are divided into six sections – Part 1: Background information, Part 2: Selection and differentiation, Part 3: Staffing and preparedness, Part 4: Fetal monitoring, workup and fetal medicine, Part 5: Competency development, Part 6: Preparing the way and cooperation. The questionnaire mainly contains dichotomous questions of the yes/no type or a six-part Likert scale.
The exception is questions concerning comments on staffing (Part 3) and revision of the guide (Part 6), where the respondents had the opportunity to reply freely. There are a total of 40 questions in the questionnaire (johansenengappendiks).
The invitation to respond to the form was sent by e-mail on 3 January 2015, with a deadline of 13 February 2015 for responses. Information about the survey was provided, and a link to the questionnaire. The form was sent to all of Norway's 47 maternity institutions as at 1 January 2015. When the deadline expired, all but six had responded, and after two reminders all of them had responded. The last response arrived on 16 May 2015.
The medical officer in charge of the maternity section responded on behalf of level 1 birth units and level 2 units. The head midwife responded on behalf of the midwife-managed units (level 3), and a clinic director and senior consultant responded on behalf of the modified midwife-managed units (level 3).
Results
A total of 47 respondents completed the form (100 %). They represented 17 level 1 units, 22 level 2 units and eight midwife-managed birth units (including two modified midwife-managed birth units). Table 1 shows the number of maternity institutions at enterprise level and the distribution in each health region.
Information about the maternity institution was provided by the medical officer in charge of the maternity section.
Table 1
Number of maternity institutions in Norway in 2014, by institutional level and health region.
|
| University hospitals/Central hospitals (level 1 birth units) | Department of Obstetrics and Gynaecology (level 2 birth units) | Midwife-managed birth units (level 3 birth units) | Modified midwife-managed birth units (level 3 birth units) | Total |
|---|---|---|---|---|---|
| South-Eastern Norway Regional Health Authority | 9 | 8 | 1 |
| 18 |
| Western Norway Regional Health Authority | 4 | 2 |
| 1 | 7 |
| Central Norway Health Authority | 2 | 5 |
|
| 7 |
| Northern Norway Regional Health Authority | 2 | 7 | 5 | 1 | 15 |
| Total | 17 | 221 | 6 | 2 | 47 |
1Four of which had neonatal departments
Selection and differentiation
All the institutions responded that they had defined which patients belonged in the category "normal birth". Two level 1 birth units (4.3 %) had not defined which patients were in the category "high-risk births". The selection criteria of all the respondents were in line with the quality requirements, and apart from three (6.4 %) they had adapted the selection criteria to local conditions.
Two of the 39 maternity institutions (excluding midwife-managed birth units) responded that they did not have written procedures for how normal births should be monitored and treated, and one out of 39 did not have these procedures for high-risk births. Six of 39 maternity institutions (15.4 %) had not drawn up written procedures for the midwife's area of responsibility during births, and 15 of 39 maternity institutions (38.5 %) had no procedures defining the responsibilities of the duty doctor. Four of 39 maternity institutions (10.3 %) reported that they had no procedures for when a doctor should be summoned in cases of complicated deliveries. Seven of 39 maternity institutions (17.9 %) had no procedures describing the responsibilities of the midwife in charge.
Organisation and staffing
Eleven of 21 level 2 birth units (one department did not respond) (52.4 %) and eleven of 15 level 1 birth units (73.3 %) had a full complement of doctors (two did not respond). Seventeen of 21 level 2 birth units (81.0 %) and eleven of 15 level 1 birth units (73.3 %) had a full complement of midwives. In total, then, the level 1 and 2 birth units had 77.8 % of their midwife posts and 61.1 % of their doctor posts filled. One level 1 and two level 2 birth units responded that the requirement of four-shift rotation for doctors was not met.
The maternity institutions responded to the question of how dependent they were on using locum midwives and/or doctors. Ten level 1 birth units (58.8 %) reported an extensive or moderate need to use locum midwives. Nineteen level 2 birth units (86.4 %) reported that they had little or moderate need for locum doctors.
All level 1 and 2 birth units had a specialist in obstetric and gynaecology on duty twenty-four hours a day, with the exception of one level 2 birth unit which responded that they only had a specialist during the day. The level 2 birth units usually have an arrangement whereby the duty doctor is on call during the evening and night. All the level 1 birth units and seven of the 22 level 2 birth units (31.8 %) had a paediatric specialist on twenty-four hour emergency preparedness duty.
Twenty-two of 47 maternity institutions (46.8 %) responded that they had no written criteria for when a midwife must be present during active labour. Twenty-four maternity institutions (51.1 %) responded that they offered a midwife's presence during active labour to a large or moderate extent. Nine of them (37.5 %) had an overview of the number of deliveries where a midwife actually was present during active labour.
Fetal monitoring
Maternity institutions were asked about their fetal monitoring methods (Table 2). All the level 1 birth units had fetal monitoring in the form of ST analysis (STAN), scalp pH or lactate measurement. Four level 2 birth units (18.2 %) did not have access to this type of monitoring. All the level 1 birth units had drawn up criteria for when various fetal monitoring methods should be used, while five of the level 2 birth units (22.7 %) had no such criteria.
Table 2
Different fetal monitoring methods used at departments of gynaecology and obstetrics and maternity departments in Norway in 2014 (number of maternity institutions in per cent) reported by the medical officer in charge of the maternity section
|
| University hospitals/central hospitals (level 1 birth units) | Departments of obstetrics and gynaecology (level 2 birth units) |
|---|---|---|
| Hand-held Doppler | 100 | 86.4 |
| CTG recording | 100 | 95.5 |
| ST analysis (STAN) | 88.2 | 36.4 |
| CTG recording with analysis of short-term variability | 82.4 | 27.3 |
| Pinard stethoscope | 76.5 | 54.5 |
| Measurement of fetal scalp blood pH or lactate | 52.9 | 59.1 |
Two level 1 birth units (11.8 %) and one level 2 birth unit (4.5 %) had not drawn up written criteria for when a doctor should be contacted in the event of cardiotocographic changes (CTG changes). Ten of 46 maternity institutions (21.7 %) had no facility for electronic storage of charts showing fetal heart rate during labour.
Instruction and training
The maternity institutions were asked how often they had instruction on the subject of fetal monitoring. Seven level 1 birth units (41.2 %) and six level 2 birth units (27.3 %) reported that they held weekly instruction for their midwives. Eight level 1 birth units (47.1 %) and six level 2 birth units (27.3 %) reported that they held weekly instruction in fetal monitoring for doctors.
A certification scheme in fetal monitoring for doctors and midwives (STAN or CTG recording) was established at ten of 19 level 2 birth units (three departments did not respond) (63.2 %) and 16 of 16 level 1 birth units (one did not respond) (100 %). An instruction programme that includes certification accompanies the acquisition of a STAN machine.
Thirty-nine of 47 maternity institutions (83.0 %) had instituted professional development officers for midwives, and 18 of 47 (38.3 %) had professional development officers for their doctors. Internal instruction for midwives and obstetricians together was established at 24 of 47 maternity institutions (51.0 %) and joint review of case histories was established at 31 of 47 institutions (66.0 %). Joint practical training for midwives, obstetricians, paediatricians and paediatric nurses was established at 37 of the 47 maternity institutions (78.7 %), and practical training was mandatory at 19 maternity institutions (40.4 %).
Training programmes for new employees and locums were available at 29 of 47 maternity institutions (61.7 %). Systematic observation was established at one of 17 level 1 birth units (5.9 %), six of 22 level 2 birth units (27.3 %) and six of eight level 3 birth units (75.0 %).
Have the quality requirements led to change?
Twelve level 2 birth units (54.5 %) and eight level 1 birth units (47.1 %) reported that the quality requirements had led to extensive changes with respect to the presence of doctors at high-risk births. The interdisciplinary cooperation between doctors and midwives had improved considerably at five level 1 birth units (29.4 %) and 11 level 2 birth units (50.0 %). Six level 1 birth units (35.3 %) and 13 level 2 birth units (59.1 %) believed that the quality requirements had led to extensive changes in competency requirements.
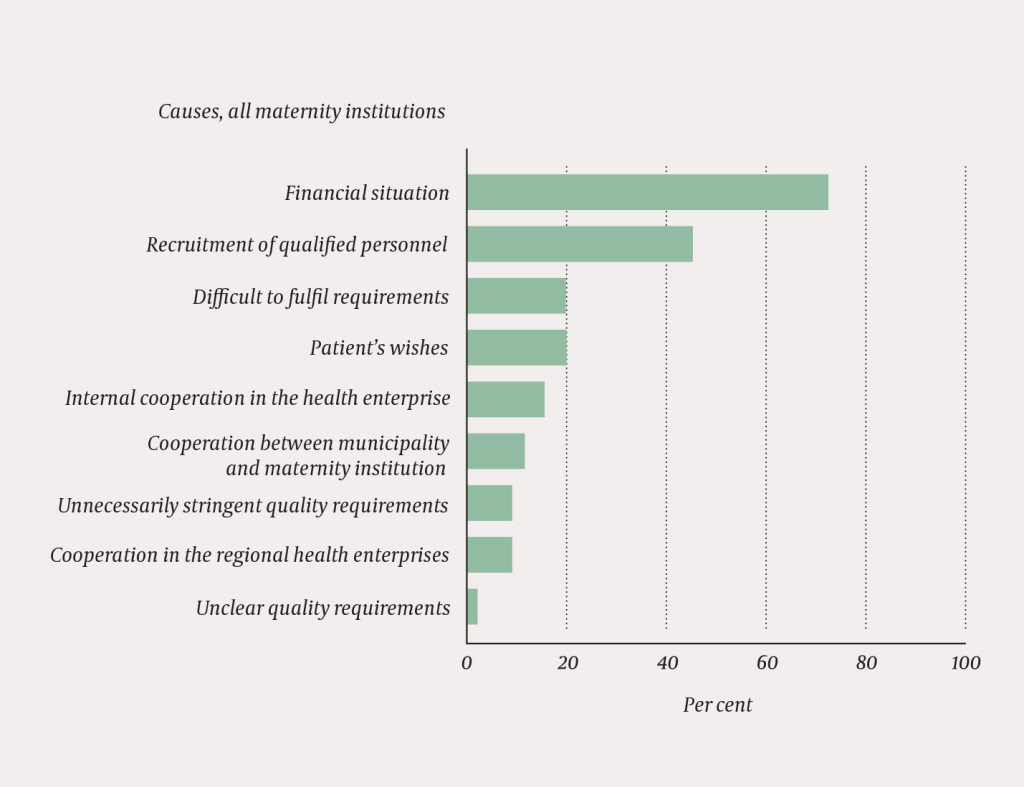
Figure 1 shows what the respondents considered to be the greatest obstacles to meeting the quality requirements. Financial constraints were stated by 73 % to be the cause, and 52 % responded that a shortage of qualified personnel played a significant part.
Discussion
The study shows that the Norwegian Directorate of Health's guide Et trygt fødetilbud [A safe maternity service] (3) has contributed to reported changes in Norwegian obstetrics, but that considerable challenges are presented by the procedures that describe the areas of responsibility of doctor and midwife, availability of personnel resources and staff training.
Selection criteria have been introduced, and high-risk pregnancies defined
Criteria for determining which women are recommended to give birth at institutions at the different levels have been introduced in all maternity institutions. The majority of the institutions have defined criteria that classify normal births and high-risk births. This is a prerequisite for providing differentiated maternity care.
Cases brought before the Board of Health Supervsion have revealed that maternity care is often inadequate when the course of the labour changes from normal to abnormal, because birthing assistants with the necessary expertise are not summoned (4–6). The explanation may be lack of procedures for summoning a doctor, but may also be due to failure to define responsibilities in connection with the midwives' and obstetricians' tasks. Some maternity institutions had no written procedures for when a doctor should be summoned, and a large number had nothing in writing about the responsibilities of the birthing assistants. The quality requirements state clearly that these responsibilities must be defined.
Limited availability of personnel resources
About half of the level 2 birth units reported unfilled doctors' posts. It is a known fact that small maternity institutions have had staffing challenges for many years (2, 3, 7), and the survey shows that the problem still exists. The quality requirements specify that doctors must have at least four-shift rotation. Nevertheless, there were two level 2 birth units that did not meet this requirement. There may be more – the survey did not provide answers as to how the duty rota is implemented in practice. A maternity institution may employ four doctors, but in reality only from one to three doctors may be present at any given time. In that case, the requirement of four-shift rotation is not met.
Just under half of the level 2 birth units had unfilled doctors' posts, and over a quarter of level 1 birth units had unfilled midwife posts. However, most level 2 birth units reported that they had little or moderate need for locum doctors. This may mean that the level 2 birth units more frequently use doctors on permanent staff to cover unfilled posts, holidays, illness etc.
Over half of the level 1 birth units reported a moderate or extensive need to use midwife locums. This may mean less use of permanent staff to cover the unfilled shifts and that the hospitals have to use hired locums to a greater extent. Extensive use of locums gives rise to risk of adverse incidents in the specialist health service, because many locums are not familiar enough with the patient group, equipment, routines, procedures and other members of staff (2, 3, 7, 8). The survey does not indicate whether the maternity institutions mainly use regular locums or not.
The quality requirements recommend that a midwife be with the patient during the active stage of labour, in one-to-one follow-up. This gives the patient a sense of security, and leads to more spontaneous births and shorter labour and less need for pain relief (9). Fewer caesarean sections and operative vaginal deliveries are also reported.
Only half of the respondents answered the question about one-to-one follow-up. Almost all of those who responded stated that they provided this service, but very few actually recorded whether a midwife was continuously present during active labour. The health enterprises should use the presence of a midwife during active labour as a quality indicator, and therefore also record whether patients are offered this service. This is also mentioned in Assignment Document 2017 to the regional health authorities.
Access to advanced fetal monitoring and training
The quality requirements state that those maternity institutions that accept high-risk pregnancies must have access to advanced fetal monitoring (STAN monitoring, analysis of lactate or pH from fetal scalp blood) in addition to CTG recording. Four level 2 birth units did not fulfil this requirement.
New systematic reviews and meta-analyses have demonstrated that STAN technology does not yield better results than CTG recording alone (10, 11). However, the STAN concept can take the credit for making CTG recording more systematic, for example through a certification scheme.
Maternity institutions must have clear guidelines for differentiated maternity care, and this includes choice of monitoring method. Review and analysis of serious adverse events in obstetrics have shown that the fault often lies in the use and interpretation of fetal monitoring (4, 5, 12).
The enterprises must provide regular instruction and set qualification requirements regarding the interpretation and use of fetal monitoring for midwives and doctors. The survey showed that the level 1 birth units more often hold courses in fetal monitoring, and that they make more use of certification schemes to secure expertise. These schemes may be one means of ensuring that all personnel have the necessary expertise in fetal monitoring. A third of the level 2 birth units do not have these certification schemes.
The quality requirements specify that the instruction and practical training should be interdisciplinary and mandatory. The survey has shown that joint internal instruction for midwives and doctors is only carried out at half the maternity institutions. Interdisciplinary instruction is important, because birthing assistants gain a shared understanding of obstetrics issues and how to deal with them.
Moreover, less than half of the maternity institutions had mandatory shared instruction for obstetricians, paediatricians and midwives. It is conceivable that the institutions have separate instruction for each category of health personnel. Health enterprises have a duty to ensure that all personnel have the necessary competencies, and one possible means of achieving this is to conduct mandatory interdisciplinary instruction. This could help to ensure that all personnel have necessary competencies and mandatory skills.
Strengths and weaknesses of the study
One strength of the study is that all the maternity institutions in Norway responded to the questionnaire. The medical officer in charge was responsible for the response, so the response may reflect a subjective perception rather than the general view of the department.
Implementation of quality requirements also involves an assessment of whether all birthing assistants in the department are familiar with the guidelines, and whether they are actually followed. Our survey provides no information on these points.
Some questions allow latitude for a certain amount of discretion. Some questions were not answered, which may be due to the person who completed the form lacking information on the subject.
The questionnaire provided few answers as to whether procedures are followed, or how many attend instruction. We believe nonetheless that it provides important information about procedures and organisation in maternity institutions, and of what remains to be done in terms of measures to raise quality.
Conclusion
The guide Et trygt fødetilbud [A safe maternity service] has reportedly led to changes in Norwegian maternity care, but a good deal of work remains to be done with respect to procedures, unfilled positions and interdisciplinary instruction.
It is important for employers to know the extent to which the quality requirements are being met, to enable them to prepare remedial measures and subsequently assess the effect of the measures that are implemented.
- 1.
Faglige krav til fødeinstitusjoner. IK-2565. Oslo: Statens helsetilsyn, 1996. https://www.helsetilsynet.no/upload/Publikasjoner/utredningsserien/faglige_krav_fodeinstitusjoner_ik-2565.pdf (13.2.2016).
- 2.
St.meld. nr. 12 (2008-2009). En gledelig begivenhet. Om en sammenhengende svangerskaps-, fødsels- og barselomsorg.
https://www.regjeringen.no/no/dokumenter/stmeld-nr-12-2008-2009-/id545600/ (19.6.2017). - 3.
Et trygt fødetilbud – kvalitetskrav til fødselsomsorgen. IS-1877. Oslo: Helsedirektoratet, 2010.
https:// helsedirektoratet.no/Lists/Publikasjoner/Attachments/245/Et-trygt-fodetilbud-kvalitetskrav-til-fodselsomsorgenIS-1877.pdf (8.11.2016). - 6.
Svikt i samhandling, kommunikasjon og kompetanse i alvorlige hendelser… kunne det skjedd hos oss? Rapport fra Statens helsetilsyn 3/2014. http://www.helsetilsynet.no/no/Publikasjoner/Rapport-fra-Helsetilsynet/RapportHelsetilsynet-2014/Svikt-i-samhandling-kommunikasjon-og-kompetanse-i-alvorlige-hendelser-kunne-det-skjeddhos-oss/ (9.11.2016).
- 7.
Oppsummering av tilsynserfaring fra små fødeinstitusjoner. Statens helsetilsyn 5.5.2008. https:// www.helsetilsynet.no/no/Publikasjoner/Brev-hoeringsuttalelser/Utvalgte-brev-og-horingsuttalelser-tidligere-ar/Oppsummering-tilsynserfaringer-smaa-foedeavdelingene-under-500-foedsler-aar/ (18.11.2016).
- 8.
Uønskede hendelser knyttet til vikarbruk i spesialisthelsetjenesten. Kunnskapssenteret 28.10.2013. http://www.kunnskapssenteret.no/publikasjoner/uonskede-hendelser-knyttet-til-vikarbruk-i-spesialisthelsetjenesten (25.11.2016).
- 9.
Hodnett ED, Gates S, Hofmeyr GJ et al. Continuous support for women during childbirth. Cochrane Database Syst Rev 2013; 7: CD003766 [PubMed].. [PubMed]
- 11.
Neilson JP. Fetal electrocardiogram (ECG) for fetal monitoring during labour. Cochrane Database Syst Rev 2015; 12: CD000116. [PubMed]