Does the University of Tromsø – The Arctic University of Norway educate doctors to work in rural communities?
MAIN MESSAGE
Almost one out of three (30 %) GPs educated at the University of Tromsø – The Arctic University of Norway worked in a rural municipality compared with 19 % of all GPs in Norway
Doctors in health trusts, who had been educated at the University of Tromsø were mostly employed at the University Hospital of North Norway and staffed 53 % of positions for doctors there
Hospitals in Finnmark and Nordland were less frequently staffed by doctors educated at the University of Tromsø
The shortage of doctors in rural communities still presents a challenge nationally (1) and internationally (2–4). When the Storting resolved in 1968 to build the University of Tromsø (from 2013 the University of Tromsø – The Arctic University of Norway), the plans to offer medical studies in North Norway constituted a decisive argument. The main purpose of offering a new course of medical studies in Tromsø was to improve GP density and to raise health services and health conditions for the population of North Norway (Finnmark, Troms and Nordland) to the equivalent national standard.
With its visionary and innovative study model, developed under the leadership of Peter F. Hjort (1924 – 2011), the University of Tromsø was one of the first to provide clinical placements in rural communities during medical studies. Consequently, the model included collaboration with the health services all over North Norway (5). Throughout the fifth year of their studies, students received a considerable part of their clinical training through placement in local hospitals and in the municipal health services throughout the region. The first student cohort started in 1973, and the first doctors graduated in 1979.
There are two predominant hypotheses regarding what increases the likelihood of a doctor choosing to work outside the main conurbations: upbringing in a rural community and exposure to a rural community during their training. There is clear evidence from other countries that doctors who have grown up in rural communities are more likely to become doctors in these areas than those with an urban background (6–11). The effect of upbringing is stronger among young, unmarried doctors, and stronger if the individual comes from an attractive rural community (12).
However, in Norway this research has had a somewhat different focus. In the 1960s prior to the foundation of the University of Tromsø, Torstein Bertelsen (1923 – 2008) conducted studies showing that on the one hand, there is a tendency for doctors to return to the region where they grew up, and on the other hand that they tend to work at their place of study (13). Thus Bertelsen did not focus on rural communities as opposed to more central areas, but on the regions and counties. His findings were crucial for the decision to introduce a prioritised quota for admission to medical studies at the University of Tromsø for students from North Norway.
Studies of exposure to rural communities during medical studies have later shown how this leads to a greater tendency to work in these areas after graduation (14).
A particular problem in Tromsø at the start – which has later proved to be a constant challenge – was to recruit doctors and persuade them to remain in the smallest and most peripheral rural municipalities (1, 15). Studies on the recruitment effects of medical education in North Norway have focused so far on North Norway as a region.
Since the purpose of Tromsø's study model was to promote recruitment and a stable GP density throughout North Norway, a key question in this study is how successful this has been in relation to the health services in rural communities, not only in North Norway but also in other parts of the country.
Based on a data set that includes all cohorts of doctors educated in Tromsø from 1979 to 2012 inclusive, we wished to answer the following two questions: To what extent do GPs educated at the University of Tromsø work in rural municipalities in North Norway and in the rest of the country? To what extent do hospital doctors educated at the University of Tromsø work at university hospitals or smaller hospitals in North Norway and in the rest of the country?
Material and method
Altogether 96 % of doctors in Norway are members of the Norwegian Medical Association. The membership register is used, among other things, for descriptive and quality-promoting purposes. This study is based on de-identified data from the 1 611 practising doctors (as of 2013) who had graduated from the University of Tromsø in the period 1979 – 2012. The variable – place of work – as indicated in the register was used.
Foundation doctors are excluded from the data set (Fig. 1) since their place of work is temporary and does not necessarily reflect their own wishes. The distribution between the specialist health service and primary health care is given. The geographical presentation of how doctors educated at the University of Tromsø are distributed by county includes all practising doctors with the exception of foundation doctors.
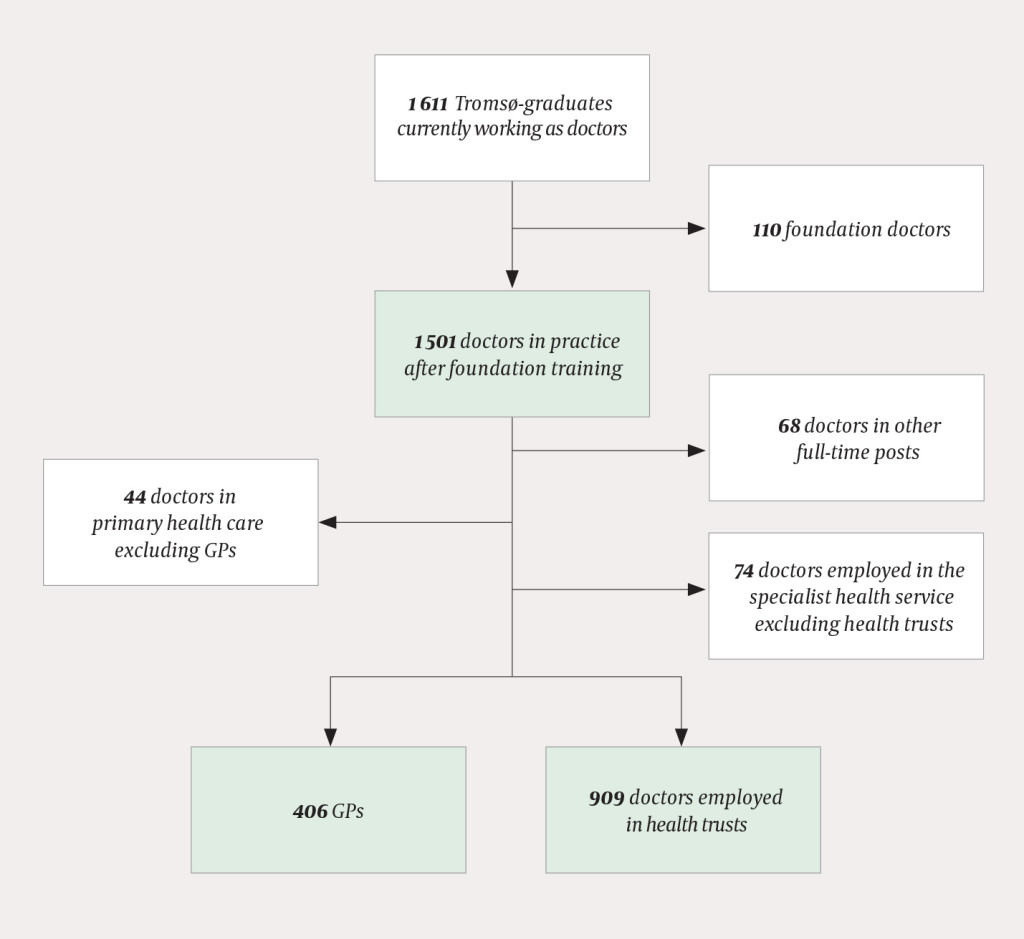
In the further analyses, the material was divided in two and limited to employees in the health trusts and GPs. The reason for this is the delimitation of information about doctors in Norway with which our data are compared. These data are independent of place of education. We have no sound data for distribution by municipality for all doctors working in primary health care, only for GPs (16). Secondly, we do not know the geographical distribution for all doctors working in the specialist health service, only for those working in health trusts (17). Thus the final study population consists of all GPs educated at the University of Tromsø and doctors employed in the health trusts who were still practising in 2013. The data were analysed using IBM SPSS Statistics 23 for Windows. We have not conducted statistical tests because the data set consists of the entire population and not just a sample.
To operationalise the difference between central areas and rural communities, we have used the centrality of the workplace municipality in the analysis of GPs, while in the case of doctors working in health trusts, there is a differentiation between university hospitals and other hospitals. The Institute for Studies of the Medical Profession (LEFO) has ensured that the information from the membership register has been approved for use in the study.
Division of municipalities
The centrality level of municipalities describes the opportunities for the population of a municipality to commute for work to one or several urban settlements (18). The municipalities are divided into four centrality levels (levels 0 – 3) by population, central functions and distance to an urban settlement. This means that the municipalities closest to the urban settlement are placed on the same level as the urban settlement. Municipalities on level 3 are regional centres in contrast to municipalities on level 0 that are the most remote. Rural communities in this study are understood as municipalities on level 0 or 1. Table 1 shows that 47 % of the municipalities in Norway are rural municipalities (level 0 and 1). Table 1 also shows that North Norway has a larger share of rural municipalities (82 %) than the rest of Norway (38 %).
Table 1
The percentage of municipalities on different levels of centrality in Norway and North Norway (section A) (18) compared with the distribution of centrality among GPs in North Norway versus the rest of Norway (section B) (16)
| Centrality |
A: Municipalities |
B: GPs |
||||
|---|---|---|---|---|---|---|
| North Norway |
Rest of Norway |
Total |
North Norway |
Rest of Norway |
Total % (n) |
|
| 0: Remote municipalities |
63.2 |
27.6 |
34.7 |
37.2 (182) |
8.7 (340) |
11.8 (522) |
| 1: Fairly remote municipalities |
18.4 |
10.3 |
12.1 |
19.8 (97) |
5.5 (216) |
7.1 (313) |
| 2: Fairly central municipalities |
14.9 |
19.1 |
18.4 |
28.6 (140) |
16.2 (634) |
17.6 (774) |
| 3: Central municipalities |
3.5 |
43.1 |
34.9 |
14.3 (70) |
69.6 (2 728) |
63.5 (2 798) |
| Total |
100 (n = 87) |
100 (n = 341) |
100 (n = 428) |
100 (489) |
100 (3 918) |
100 (4 407) |
University hospitals and other hospitals
Doctors in health trusts are divided according to whether their workplace is a university hospital or not. All local hospitals that belong to a university hospital including, for example, small local hospitals such as the University Hospital of North Norway Narvik and the University Hospital of North Norway Harstad, are included in this definition. This is because the comparison of data is organised so as not to distinguish between local hospitals in the same hospital trust that have different locations.
Results
A nationwide overview (Fig. 2) shows the place of work of doctors educated at the University of Tromsø who were still practising as of 2013.
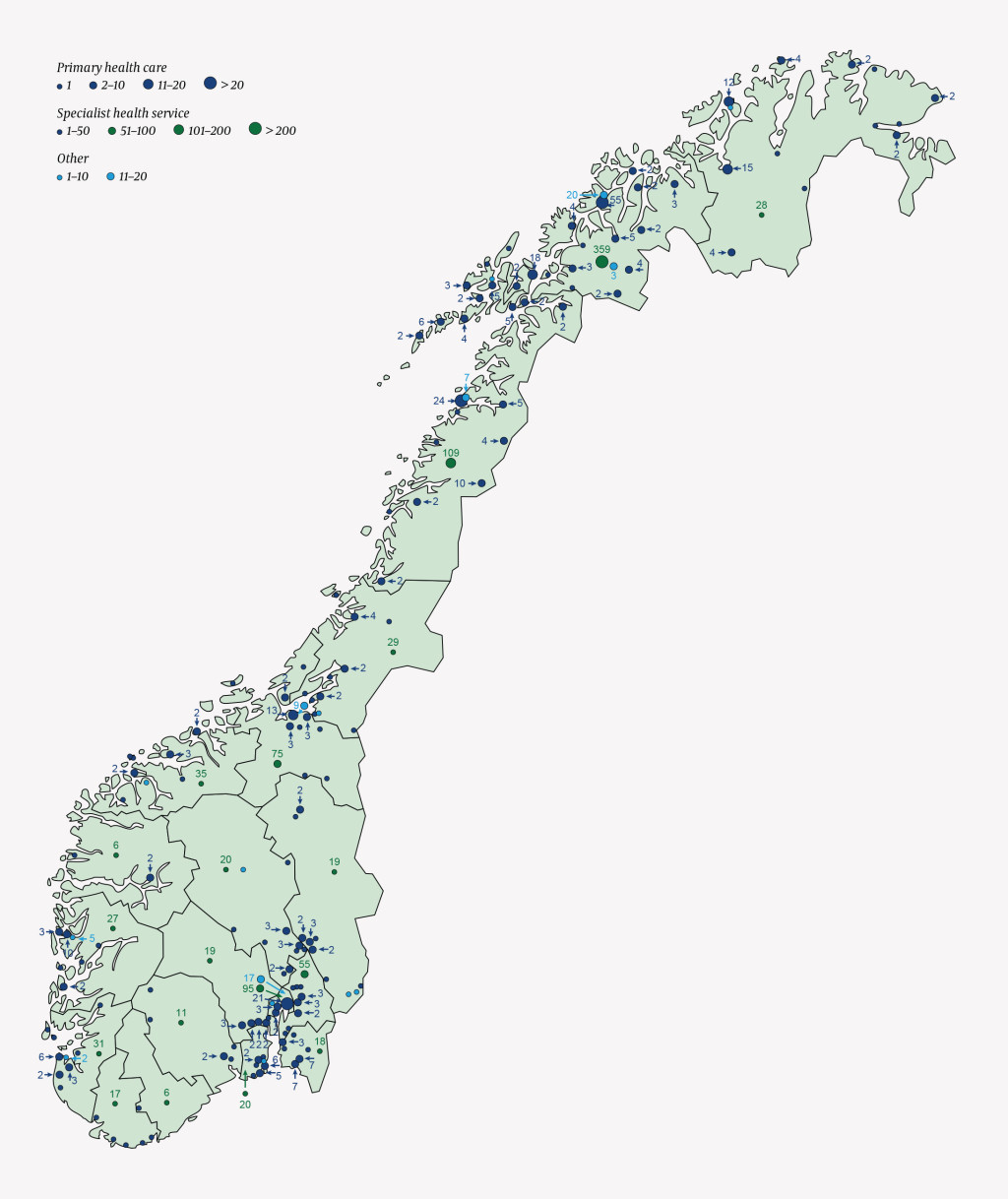
The further analyses are based on a data set consisting of 909 (69 %) doctors who worked in a health trust, and 30.9 % GPs (N = 1 315). Altogether 50.5 % of the GPs educated at the University of Tromsø and 45.8 % of doctors in health trusts who were educated at the University of Tromsø were men.
Recruitment of GPs to rural communities
Almost one out of three (30 %) of the GPs educated at the University of Tromsø worked in a rural municipality. In comparison, 19 % of all GPs in Norway worked in rural municipalities (Table 2).
Table 2
Workplace municipalities for GPs in Norway (Norwegian Directorate of Health 2013), and workplace municipalities for GPs educated at the University of Tromsø, in 2013. Distributed by centrality of workplace municipality (18)
| Level of centrality |
Percentage of all GPs in Norway (N = 4 407) |
Percentage of GPs educated at the University of Tromsø (N = 406) |
|---|---|---|
| O: Remote municipalities |
11.8 |
18.2 |
| 1: Fairly remote municipalities |
7.1 |
11.8 |
| Total rural municipalities |
18.9 |
30.0 |
| 2: Fairly central municipalities |
17.6 |
22.2 |
| 3: Central municipalities |
63.4 |
47.8 |
| Total central municipalities |
81.1 |
70.0 |
GPs educated at the University of Tromsø staffed 44 % of all GP positions in North Norway and 5 % of all GP positions in other parts of Norway. Moreover, doctors from the University of Tromsø staffed 34 % of GP positions in rural municipalities in North Norway, and 84 % of GP positions in the most central municipalities in the region (centrality level 3). This means that the more centrally a municipality is located in North Norway, the larger the share of GP positions staffed by doctors from the University of Tromsø (Table 3).
Table 3
Percentage of GPs educated at the University of Tromsø who staff GP positions in North Norway and in the rest of Norway in 2013, distributed by centrality level (18)
| North Norway |
Rest of Norway |
|||
|---|---|---|---|---|
| Number of GPs |
Percentage of graduates of the University of Tromsø who hold GP positions |
Number of GPs |
Percentage of graduates of the University of Tromsø who hold GP positions |
|
| 0: Remote municipalities |
182 |
33.5 |
340 |
3.8 |
| 1: Fairly remote municipalities |
97 |
35.1 |
216 |
6.5 |
| Total rural municipalities |
279 |
34.1 |
556 |
5.9 |
| 2: Fairly central municipalities |
140 |
42.9 |
634 |
4.7 |
| 3: Central municipalities |
70 |
84.3 |
2 728 |
5.0 |
| Total central municipalities |
210 |
56.7 |
3 362 |
4.9 |
| Total |
489 |
43.8 |
3918 |
4.9 |
No similar tendency was found for Norway excluding North Norway. Table 2 also showed that 119 GPs (56 %) educated at the University of Tromsø worked in central municipalities, as against 165 (86 %) in the rest of Norway. Thus those who moved south did not take on board the 'rural impact' of the University of Tromsø.
Out of all the GPs in Norway (N = 4 407), altogether 489 (11 %) were located in North Norway, and well over half of them (N = 279, 57 %) in rural municipalities (Table 3).
In the rest of Norway, a minority of GPs (556/3 918, 14 %) worked in rural municipalities.
Recruitment to hospitals
A larger share of doctors educated at the University of Tromsø (64 %) than the share of doctors in health trusts in Norway (56 %) worked at a university hospital. We found, therefore, no 'rural profile' for hospital doctors from the University of Tromsø when we look at the data set from a national perspective where we distinguish between university hospitals and other hospitals respectively.
Doctors educated at the University of Tromsø staffed 41 % of the positions in the health trusts in North Norway. This means that the University of Tromsø primarily educates hospital doctors for the area covered by the University Hospital of North Norway (Troms and Ofoten in the northern part of Nordland). For example, over half (53 %) of the doctors employed at the University Hospital of North Norway were educated at the University of Tromsø. Meanwhile doctors who had graduated from the University of Tromsø staffed the other hospitals in the region to a much lesser extent. This means that 26 – 28 % of the positions at Finnmark Hospital Trust and Nordland Hospital Trust and 14 % of the positions at Helgeland Hospital Trust were staffed by doctors educated at the University of Tromsø.
By way of comparison, only 424 (4 %) of doctors employed by health trusts in the rest of Norway were educated at the University of Tromsø. Nevertheless, 225 (53 %) of these worked at university hospitals. Corresponding figures for North Norway were 357 (74 %) out of 485 doctors.
Discussion
We found that many doctors educated at the University of Tromsø worked centrally in the North Norway region. They worked as GPs either in Tromsø and district, or in the specialist health service at the University Hospital of North Norway, whose activities are mainly based in Tromsø. We also found that in 2013, altogether 30 % of the Tromsø doctors worked in rural municipalities. The equivalent percentage for GPs in Norway as a whole was 19 %. We did not find a corresponding rural profile for doctors educated at the University of Tromsø who worked in health trusts (throughout Norway).
A strength of the article is that we possess data on all doctors educated at the University of Tromsø. Compared with all members of the Norwegian Medical Association, we found that the share of doctors educated at the University of Tromsø and employed in health trusts was of equal magnitude (17). In contrast, the share of GPs/district medical officers was larger (30 %) among those educated at the University of Tromsø compared with the country as a whole (27 %) (17). The exclusion of 186 doctors educated at the University of Tromsø who neither worked as GPs nor in a health trust (including private specialists) does not detract from our conclusions.
A weakness of the study is that our categorisation of hospitals was only twofold, and we cannot distinguish between large and small units within the same trust. The data we use as a reference standard contains only aggregated data about doctors educated at other universities, including universities abroad.
The results confirm findings from previous follow-up studies that have revealed that doctors tend to work in the region where they were educated (13), (20–23). Around half of all the doctors educated at the University of Tromsø worked in North Norway at the time of the survey. This applied to a greater degree to doctors who had grown up and attended school in North Norway, with three out of four doctors working in the region (19–22).
Labour market studies of various programmes of health and social studies confirm that both the place where you grow up and the place of study affect where you take a job (23). Over 90 % of those who grew up and studied in the same region later worked in this region. In comparison, between 50 – 60 % of those who had grown up in another region, worked in the region where they had studied (23). Our study confirms and further elucidates this picture by showing solid recruitment in the North Norway region as well as a regional centralisation.
We wondered why we did not observe the same rural profile among the hospital doctors as among the GPs. Even although the rural placement lasts longer than at other Norwegian study institutions, nevertheless the University Hospital of North Norway is the educational institution that medical students have longest and most continuous contact with throughout their programme of study (5, 24). This entails longer exposure and promotes relationship building. With regard to the sustainability of the programme of medical studies and the health service in North Norway, it is vital that the University Hospital of North Norway has strong appeal and is successful in recruitment. However, it may be problematic that the University of Tromsø does not educate more doctors for the local hospitals.
We do not know in which municipality the doctors in our study who graduated in the period 1979 – 2013 grew up. However, we do know that of those who were admitted to medical studies at the University of Tromsø in the years from 2006 – 2015, altogether 39 % had grown up in rural municipalities as against 11 % studying medicine at other Norwegian universities (25). We have no strong reason to believe that this has changed markedly between 1979 – 2013 and 2006 – 2015. It is therefore natural to interpret the results as supporting the hypothesis that growing up in a rural community influences the likelihood of practising as a doctor in such an area after graduation. Studies from other countries support this conclusion (6–11).
All Tromsø doctors had practice placements at local hospitals and GP surgeries throughout one consecutive year of study. This was originally a characteristic feature of medical studies in Tromsø, and it remains the case (5, 26). As a result, Tromsø doctors have overall more exposure to rural communities than doctors educated at other institutions in Norway or abroad. Therefore, it is natural to interpret the results as originating from the University of Tromsø's practice profile. Other studies of exposure to medical practice in rural communities in the course of one's education have shown that the longer the period of practice there, the greater the impact and the greater the interest in practising as a doctor in a rural community in the future (27).
A growing number of programmes of medical studies in Canada are attempting to augment recruitment to rural communities by establishing sub-departments at smaller locations in order to give students practical experience of working in a variety of conditions (2).
The new curriculum for the medical studies programme at the University of Tromsø that is currently being introduced (24) will extend the use of decentralised teaching. The most radical change is that 30 – 40 % of the students throughout their fifth and sixth year of study will have teaching, including clinical training, at hospitals and in the primary health service in Nordland and Finnmark (the Bodø and Finnmark model). Research on why students choose the University of Tromsø, why they choose a decentralised study model and their later career path will help to shed further light on the challenges involved in recruitment to rural communities.
Conclusion
Medical studies at the University of Tromsø – The Arctic University of Norway have contributed substantially to GP density in rural communities, and to solid recruitment to the University Hospital of North Norway.
- 2.
Ono T, Schoenstein M, Buchan J. Geographic imbalances in doctor supply and policy responses. OECD Health Working Papers, No. 69, 2014. OECD Publishing. 10.1787/5jz5sq5ls1wl-en (22.1.2015).[CrossRef]
- 3.
Wilson NW, Couper ID, De Vries E et al. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural Remote Health 2009; 9: 1060. [PubMed]
- 4.
Grobler L, Marais BJ, Mabunda SA. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas (Review). Cochrane Database of Systematic Reviews 2015, Issue 6. Art. No.:CD005314. http://www.thecochranelibrary.com (22.1.2015).
- 5.
Universitetet i Tromsø. Medisinsk studieplan. Tromsø/Oslo/Bergen: Universitetsforlaget, 1971.
- 7.
Rabinowitz HK, Diamond JJ, Gayle JA et al. Alternate career choices of medical students and their eventual specialty choice: a follow-up study. Fam Med 1998; 30: 695. [PubMed]
- 11.
Richards HM, Farmer J, Selvaraj S. Sustaining the rural primary healthcare workforce: survey of healthcare professionals in the Scottish Highlands. Rural Remote Health 2005; 5: 365. [PubMed]
- 13.
Bertelsen TI. Hvor kommer lægene fra og hvor blir de av? Tidsskr Nor Legeforen 1963; 83: 861 - 70.
- 15.
Andersen F, Herder O, Forsdahl A. Kommunelegetjenesten i Nord-Norge 1995-97. Tidsskr Nor Laegeforen 1999; 119: 1296 - 8. [PubMed]
- 16.
Helsedirektoratet 2013. Fastlegestatistikk. Fastlegepraksiser per desember 2013. https://helsedirektoratet.no/statistikk-og-analyse/fastlegestatistikk#fastlegestatistikk-2013(22.1.2015).
- 17.
Den norske legeforening. Yrkesaktive leger under 70 år i Norge fordelt på stilling per 8.7.2013. http://legeforeningen.no/Emner/Andre-emner/Legestatistikk (12.4.2016).
- 18.
Statistisk sentralbyrå. Standard for sentralitet. http://www.ssb.no/klass/#!/klassifikasjoner/128 (12.4.2016).
- 19.
Forsdahl A, Grundnes O, Eliassen H et al. Hvor blir Tromsø-legene av? Betydningen av landsdelstilhørighet og utdanningssted. Tidsskr Nor Laegeforen 1988; 108: 1225 - 30. [PubMed]
- 21.
Alexandersen Ø, Jørgensen E, Østerås J et al. Medisinerutdanningen i Tromsø–sikrer den legerekrutteringen til Nord-Norge? Tidsskr Nor Laegeforen 2004; 124: 2107 - 9. [PubMed]
- 23.
Gythfeldt K, Hagen K. Hva betyr høgskolene for rekruttering av arbeidskraft til egne regioner? Søkelys på arbeidslivet 03/2013. http://www.samfunnsforskning.no/Aktuelt/Nyhetsarkiv/Nytt-nummer-av-Soekelys-paaarbeidslivet15 (16.6.2017).
- 24.
Universitetet i Tromsø. Det helsevitenskapelige fakultet. Profesjonsstudiet i medisin. 2012-studieplanen. Tromsø: Universitetet i Tromsø, 2014.
- 25.
Abelsen B, Gaski M. Trenger vi opptakskvoter til medisinstudiet? Konferansesammendrag Den første nasjonale konferansen i helsetjenesteforskning 14.-15. mars 2017 i Trondheim. http://helsetjenesteforskning.org/konferansemars-2017/ (16.6.2017).
- 26.
Aaraas IJ. Legeutdanning i og for distriktene. Uniped 2016; 39: 293 - 303. [CrossRef]
- 27.
Eley DS, Synnott R, Baker PG et al. A decade of Australian rural clinical school graduates – where are they and why? Rural Remote Health 1937; 212: 12. [PubMed]