Norwegian studies have shown that 60 % of the age group 30 – 45 years report occupationally related health problems (1), that approximately half of all general-practice consultations with gainfully employed people are reported to have causes related to work (2), that as much as 30 – 40 % of all sickness absence may have work-related causes (3) and that 16 % of lung cancer cases in men are work-related and 22 % are possibly work-related (4). Nordic studies have estimated that 3 – 4 % of the total mortality in the population is work-related (5, 6), and that with no occupational exposure 20 % of lung cancer cases among Norwegian men could be avoided, as could 85 % of mesothelioma cases and 32 % of the cases of cancer in the nose and sinuses (7, 8).
A review study estimated that approximately 15 % of all cases of asthma in adults and 15 % of cases of COPD can be ascribed to occupational life (9). Reviews have also shown that conditions at work have an effect on musculoskeletal disorders (10), mental disorders (11) and cardiovascular diseases (12). This shows that working conditions have an effect on a number of groups of diseases that have a major impact on public health. At the same time, good working conditions may have a positive health effect.
Norway has five regional departments of occupational health. They are located at the university hospitals in Tromsø, Trondheim, Bergen and Oslo, as well as Telemark Hospital. Furthermore, there is an outpatient clinic for occupational medicine at the National Institute for Occupational Health (STAMI). These departments also employ occupational hygienists who possess special competence in identification and measurement of chemical and biological factors in the working environment.
The departments of occupational medicine examine associations between workplace exposure and illness, and provide advice on workplace measures that can prevent exacerbation of illnesses and emergence of new cases. In addition, people suffering from occupational diseases are provided with assistance in obtaining the financial compensation to which they are entitled, in the form of occupational injury benefit (from the Norwegian Labour and Welfare Administration, NAV) or occupational injury insurance (from the employer's insurance company).
At the examination, the diagnosis is established by the specialist in occupational medicine or a specialist in the organ affected, and the specialist in occupational medicine assesses a possible relationship to the patient's job by appraising a number of issues: is the clinical picture characteristic and in accordance with the possible effects of the exposure? Has the time and concentration of the exposure been sufficient? Is there a reasonable relationship between the timing of the exposure and the development of illness? Could the illness have other and more likely causes? Such an assessment may be time-consuming, and more detailed information on the exposure often needs to be collected and supplementary examinations undertaken before a conclusion can be drawn.
For the Norwegian Labour and Welfare Administration (NAV) to approve the illness as an occupational disease, the condition must be included on the list of conditions specified by the regulations to the National Insurance Act ('the occupational diseases list'), and its association with the patient's job must be deemed possible or likely. If NAV approves the condition as an occupational disease, the patient may receive special financial benefits that are additional to normal social benefits, as well as additional damages for pain and suffering, provided that the long-term disability amounts to at least 15 %. In addition, the patient may apply for financial compensation from the employer's insurance company, which may result in a considerably higher reimbursement sum.
To obtain a better overview of the examinations of patients at the hospital departments of occupational medicine and STAMI, and to reveal any changes in work-related exposure and illness over time, a joint, anonymous register of examinations was established in 2009.
Material and method
The population in this study consists of all those who were examined in a department of occupational medicine in Norway in the period 2010 – 2015. All variables were measured with the aid of a one-page registration form completed by the examining doctor after having assessed the patient (aarhusappendiks).
The variables include gender, age group, the referring agency, exposure factors (up to three pre-defined factors in prioritised order), occupation and industry (up to three pre-defined categories in prioritised order), occupational activity, social benefits, symptom organ (up to two pre-defined categories), diagnosis (ICD-10 code, main diagnosis and up to two secondary diagnoses), assessment of the association with work (likely, possible, not very likely/unlikely) and a report to the Labour Inspection Authority about work-related illness, if any. For variables with multiple response alternatives, only the first priority or main category was included.
Once the doctor has completed the form, the department makes an electronic record. STAMI receives and summarises the data annually. The processing of this data material has been undertaken with the aid of SPSS Statistics version 24.
Ethics
After consultation with the Regional Committee for Medical and Health Research Ethics and Statistics Norway, it was concluded that this anonymous register is not subject to any notification or licensing obligation.
Results
In the period 2010 – 2015, the departments received a total of 9 885 patient referrals. Of these, 997 referrals were rejected, because it was deemed that an occupational health assessment was irrelevant or unable to provide any new information, while 113 patients did not attend their scheduled examination. Altogether 8 775 patient examinations were registered. Descriptive data are shown in Tables 1 and 2.
Table 1
Patients assessed at the departments of occupational medicine in Norway in the period 2010–2015 (N = 8 775)
| Variable | Number | Proportion (%) |
|---|---|---|
| Gender |
|
|
| Man | 6 599 | 75 |
| Woman | 2 128 | 24 |
| Not stated | 48 | < 1 |
| Age (years) |
|
|
| < 30 | 631 | 7 |
| 30 – 49 | 2 613 | 30 |
| 50 – 69 | 4 609 | 53 |
| ≥ 70 | 892 | 10 |
| Not stated | 30 | < 1 |
| Referring agency |
|
|
| Company doctor | 817 | 9 |
| General practitioner | 2 649 | 30 |
| Private specialist | 323 | 4 |
| Hospital | 1 330 | 15 |
| NAV | 3 305 | 38 |
| Other | 275 | 3 |
| Not stated | 76 | < 1 |
| Social benefits |
|
|
| Sickness benefit (full/partial) | 1 408 | 16 |
| Rehabilitation/vocational rehabilitation/work assessment | 903 | 10 |
| Disability benefit (full/partial) | 1 166 | 13 |
| Association with work |
|
|
| Likely | 3 574 | 41 |
| Possible | 2 060 | 23 |
| Not very likely/unlikely | 2 809 | 32 |
| Not stated | 331 | 4 |
| Department |
|
|
| Tromsø | 795 | 9 |
| Trondheim | 1 645 | 19 |
| Bergen | 2 227 | 25 |
| Telemark | 1 762 | 20 |
| Oslo | 1 950 | 22 |
| STAMI | 396 | 5 |
Table 2
Exposure factors and illness in patients assessed at the departments of occupational medicine in Norway in the period 2010–15 (N = 8 775)
| Variable | Frequency | Proportion (%) |
|---|---|---|
| Most common industries |
|
|
| Manufacturing and mining | 2 613 | 30 |
| Building and construction | 1 439 | 16 |
| Health and social services | 785 | 9 |
| Retail trade | 791 | 9 |
| Transport and storage | 665 | 8 |
| Oil and gas extraction | 443 | 5 |
| Most common exposure factors |
|
|
| Irritants/allergens | 1 585 | 18 |
| Solvents | 1 326 | 15 |
| Toxic gases/fumes | 1 113 | 13 |
| Asbestos | 1 061 | 12 |
| Other inorganic dust (not asbestos) | 697 | 8 |
| Selected diagnoses |
|
|
| Asthma | 1 366 | 16 |
| COPD | 902 | 10 |
| Lung cancer | 1 119 | 13 |
| Toxic encephalopathy | 275 | 3 |
| Contact dermatitis | 268 | 3 |
The majority of those assessed were men (n = 6 599, 75 %), and most were in the age group 50 – 69 years (n = 4 609, 52 %). The most common referring agency was NAV (n = 3 305, 38 %). The number of patient referrals grew steadily from 2010 (n = 1 389) to 2015 (n = 1 678). The largest group of patients were assessed in Bergen (n = 2 227, 25 %) and the smallest at STAMI (n = 396, 5 %). The proportion of assessments that concluded with a likely association with work remained stable at around 40 %. As regards social benefits, altogether 16 % were receiving sickness benefit, 10 % were receiving work assessment allowance and 13 % disability benefit at the time of their examination.
Of the 12 industry categories in the register, manufacturing and mining was the most frequent (n = 2 613, 30 %). Work in the oil and gas extraction industry was most common in Bergen, where this industry accounted for 11 % of all cases. The most common exposure involved irritants/allergens (n = 1 585, 18 %), while ergonomic and psychosocial strains were rarely recorded as forms of exposure.
Some change in exposure took place from 2010 to 2015. While organic solvents were the most common form of exposure in 2010, irritants/allergens were most common from 2012 to 2015 (Figure 1).
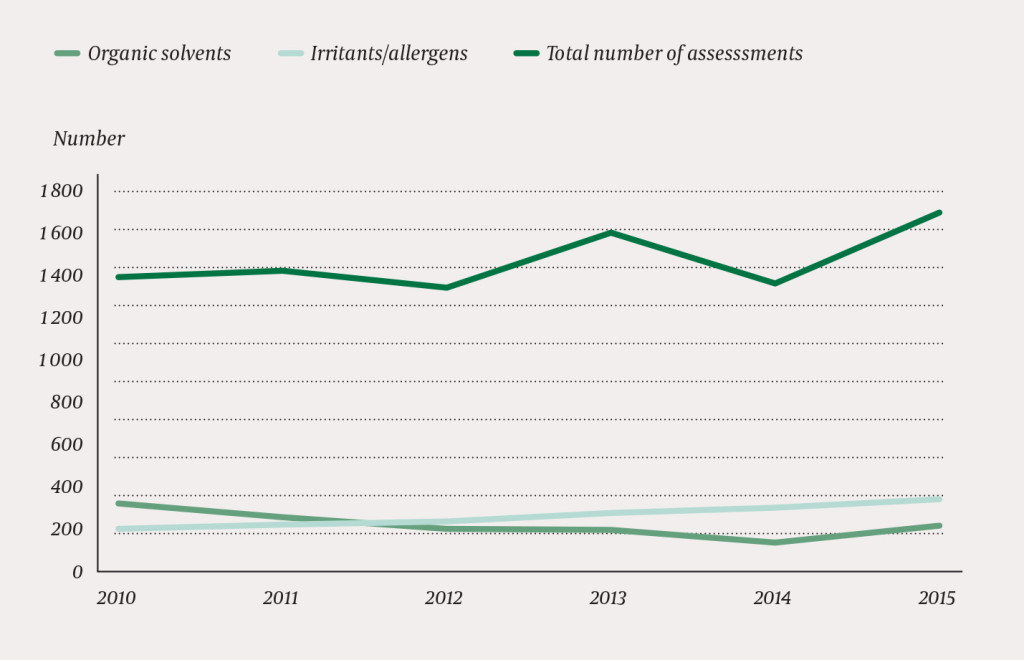
Exposure to solvents was clearly the most common form in 2010 (314/1 389 cases, 23 %), but was in third place in 2015 (201/1 678 cases, 12 %). Irritants/allergens were registered in 201/1 389 cases in 2010 (15 %) and in 346/1 678 cases in 2015 (21 %). The register showed that 35 % of all exposures had occurred in the patient's current workplace (i.e. the patient's workplace at the time of the consultation).
The most common symptom organs were the lungs/airways (n = 4 957, 57 %), followed by neurological disorders (n = 2 074, n = 24 %). Asthma was the most frequently recorded diagnosis (n = 1 366, 16 %). Chronic toxic encephalopathy (n = 275, 3 %) was recorded to a decreasing extent during the period (n = 67 in 2010 and n = 41 in 2015). Musculoskeletal afflictions and mental disorders were recorded in no more than 1 – 2 % of the cases.
We have data on reports to the Labour Inspection Authority on work-related illness only for 2015. The examining doctors reported 24 % of the cases in the context of the consultation, while in 22 % of the cases such a report had been submitted previously, for example by the referring doctor. In the remaining cases this type of report was not relevant (46 %) or had not been recorded on the form (8 %).
Discussion
Main findings
The most common exposures involved irritants/allergens (18 %) and organic solvents (15 %), and these factors were registered to an increasing and a somewhat decreasing extent respectively through the 2010 – 2015 period.
The most common symptom organs were the lungs/respiratory tract (57 %), with diagnoses of asthma, COPD and lung cancer. The proportion of cases that were deemed to have a likely or possible association with the patient's work amounted to 40 % and 23 % respectively.
Gender
The great majority of the patients assessed were men (75 %). This is most likely because male-dominated industries tend to have higher frequency of exposures that may cause traditional occupational diseases and result in occupational injury compensation.
Moreover, it is conceivable that women are underrepresented in the statistics, for example because cases of hand dermatitis, the frequency of which is likely to have increased in typically female occupations, are less frequently referred to departments of occupational medicine to be assessed for a relationship to the job situation.
Age
The relatively advanced age of the patients may be due to the fact that some work-related illnesses require a long exposure time or that there is a long latency period between the exposure and onset of illness. Long latency periods are observed especially in cases of asbestos-related cancers (lung cancer or malignant mesothelioma), where the exposure may have taken place 20 – 40 years previously. The use of asbestos has been banned in Norway since the 1980s, and the continuously high number of registrations may partly be ascribed to the long latency period, perhaps also to increased use of newer and better diagnostic imaging techniques.
As regards long exposure periods, this can be observed, for example, in cases of solvent-induced neurological disease. Norway has followed the practice of using the criterion recommended by public authorities of ten years of full-time exposure for concentrations at or above the limits stated in the regulations to the Working Environment Act on threshold values and limits (13).
Finally, the advanced age may be due to the fact that some decades ago, working conditions were poorer than they are now. Appropriate preventive measures have been implemented in many Norwegian enterprises, and it is thus conceivable that fewer young adults are affected by classical occupational diseases. The register showed, however, that 35 % of the exposures were related to the patients' current jobs. This indicates that the exposures are not only of a historical nature, although some exposures also lie in the past for those who have remained in the same job, and it may thus be relevant to implement measures to prevent an exacerbation in the patient as well as development of illness in others.
Exposure and illness
Musculoskeletal and mental disorders are among the most frequently self-reported occupational health problems (1, 4). This notwithstanding, these conditions account for a minor proportion of the illnesses assessed at the departments of occupational medicine. Similarly, ergonomic and psychosocial strains are rarely registered. The most likely explanation is that conditions caused by such strains over time are not acknowledged as occupational diseases in Norway.
Despite the increased knowledge about causal relationships between working conditions and illness, the list of occupational diseases has remained virtually unchanged since 1956. The preparation of a proposal for a new list was commissioned by the Ministry of Labour and Inclusion in 2008. It was proposed that certain musculoskeletal disorders, as well as post-traumatic stress disorder after traumatic events of a shorter or longer duration should be approved as occupational diseases (15). However, the proposal for the introduction of a new list of occupational diseases has not yet been adopted.
Skin diseases and hearing loss caused by noise are also common work-related illnesses that are rarely observed in the departments, even though they are found on the list of occupational diseases. Often, these illnesses will be assessed by the primary health services, i.e. the industrial health services, or by organ specialists in otorhinolaryngology and dermatology. Compared to COPD, cancer or injuries caused by solvents, for example, the relationship to the job will often be clearer and the degree of seriousness will be lower. Since the assessment register is based on data from the second-tier services in occupational medicine, it does not provide a complete overview of risk factors in Norwegian working life.
Change over time
Exposure to irritants/allergens was registered to a somewhat increasing extent over the period. The living conditions surveys on working environment undertaken by Statistics Norway show, however, that the proportion of respondents who report exposure to dust/smoke/gases and fumes at work has declined, and that self-reported work-related respiratory tract disorders was less prevalent in 2013 than 20 years previously (14). The increasing proportion of irritants/allergens in the register may possibly be due to better knowledge about the health risks of exposure, rather than an increasing degree of exposure to substances harmful to the respiratory tract in Norwegian workplaces.
There was a decline in registration of exposure to solvents. This may perhaps be an effect of targeted preventive efforts, such as replacement of solvent-based chemicals, more effective ventilation and increased use of protective equipment (16). Ever since the 1980s, the Labour Inspection Authority has focused on prevention of injuries from solvents; for example, this was one of the main goals in the inspectorate's chemicals campaign in 2003 – 06 (17).
A recently published article describes tendencies in the prevalence of occupational illnesses in European countries in the period 2000 – 2012 based on registry data (18). The results indicate that the prevalence of contact dermatitis and asthma, conditions for which the time between exposure and onset of illness is relatively short, is declining in most countries. With regard to noise-induced hearing loss and various musculoskeletal disorders, the tendencies varied somewhat.
Assessment of work-relatedness
Relatedness to the patient's job situation was assessed as likely or possible in 40 % and 23 % of the cases respectively. This percentage may vary according to the type of illnesses referred for assessment and therefore change over time, but this has not been observed so far. Moreover, it may vary if many referrals are rejected, for example because of long waiting periods, causing only those that are assumed to be 'most work-related' to be accepted for assessment.
Even though relatedness to the patient's job has been assessed as unlikely, the assessment may have been important in itself. An assessment is not only a matter of obtaining financial compensation. Many of the patients suffer from long-term and serious illness and have pondered on possible causal factors for years. A clarification will therefore be of major importance.
The capacity and waiting periods in the departments have varied over time, but have generally amounted to 1 – 3 months. Referrals to the departments are included in the waiting-list guarantee for the specialist health services. Capacity increased in the departments of occupational medicine following the extra allocation of earmarked funds from the Ministry of Labour and Social Affairs in 2008.
Reports to the Labour Inspection Authority
Only a small minority of those who are suspected to have an occupational illness need a comprehensive examination. On the other hand, all doctors are under a statutory obligation to report cases of suspected occupational illness to the Labour Inspection Authority. The authority receives somewhat less than 3 000 such reports annually, and the Register of Occupational Illnesses is based on these reports.
Although doctors are obligated to report cases of suspected occupational illness, there is significant underreporting, since fewer than 5 % of the doctors report to the Labour Inspection Authority (19). This problem was elucidated in a study of lung cancer in 2014. In men, 16 % and 22 % of the cases were deemed likely or possibly work-related respectively, while the reporting frequency form the health regions to the Labour Inspection Authority varied from 1.7 % to 5.1 % (4).
Costs to society
Of those who were assessed, altogether 16 % received sickness benefit, 10 % received work assessment allowance and 13 % disability benefit at the time of their examination. We assume that work-related illness was a key causal factor, but we have no data for this. A Norwegian study shows that as much as 30 – 40 % of all sickness absence may be due to work-related causes (3). For asthmatics who had been on sick leave for more than 16 days, it was found that fully 70 % suffered from work-related asthma (20).
Someone who suffers from a work-related illness will tend to have a greater need to stay away from the job that causes the illness when compared to someone with the same, but not work-related, illness (3). In 2016, SINTEF Technology and Society estimated that deaths, injuries, treatment, sickness absence, disability benefits and loss of quality of life due to work-related illness cost society NOK 30 billion annually (21). The Labour Inspection Authority, which undertakes approximately 18 000 inspections each year, sees a potential for better prevention in Norwegian workplaces (22).
Sources of error
Registrations were incomplete with regard to some variables. Even if some referrals and completed patient assessments have not been registered, we believe that no more than a few have slipped through the net. We have no figures for this, however, We are unable to find any reasons for systematic bias, and we therefore claim that the results are representative for the patients examined at the country's departments of occupational medicine.
Since the register is anonymous, single patients cannot be followed over time. Some have multiple registrations, since they have been assessed on more than one occasion. This may be because they have been referred by more than one agency (e.g. by both a general practitioner and NAV), or because there has been a call for a second opinion. The number of unique patients is therefore somewhat lower than the number of assessments.
Conclusion
Work-related illness entails major consequences for the health and quality of life of individuals. Additional to these are the costs to society. The most common exposure discovered in second-tier occupational health assessment in Norway involves irritants/allergens. Previously, solvents were the most common form of exposure, but this is registered to a declining extent. Manufacturing and mining are at the top of the list of industries, followed by building and construction. The majority of the patients have symptoms in their lungs/respiratory tract or in the nervous system.
The proportion of cases assessed as having a likely relationship to the patient's job situation remains stable at approximately 40 %. The register provides a good overview of the assessment of patients at the hospital departments and STAMI, including work-related exposures and illnesses and their changes over time, and can thus help target preventive efforts. Norwegian doctors should ensure that those who need such assessment are referred to the departments, both in order to prevent a further exacerbation of work-related illness and to ensure that patients with an occupational disease receive the compensation to which they are entitled.
We wish to thank all the departments of occupational medicine for their registration of data.
- 2.
Hilt B, Kvenild K, Stenersen H. Arbeidsrelaterte sykdommer i allmennpraksis. Tidsskr Nor Laegeforen 2003; 123: 2065 - 7 [PubMed].. [PubMed]
- 10.
Knardahl S, Veiersted KB, Medbø JI et al. Arbeid som årsak til muskel-skjelettlidelser: Kunnskapsstatus 2008. Oslo: Statens arbeidsmiljøinstitutt, 2008.
- 13.
Bast-Pettersen R, Grahnstedt S, Andorsen GS et al. Nevropsykologiske effekter etter eksponering for løsemidler. STAMI-rapport 2013 nr. 1. Oslo: Statens arbeidsmiljøinstitutt, 2013.
- 14.
Aagestad C, Tynes T, Sterud T et al. Faktabok om arbeidsmiljø og helse 2015. Status og utviklingstrekk. STAMIrapport 2015 nr. 3. Oslo: Statens arbeidsmiljøinstitutt, 2015.
- 15.
Norges Offentlige Utredninger. Yrkessykdommer. Yrkessykdomsutvalgets utredning av hvilke sykdommer som bør kunne godkjennes som yrkessykdom. NOU 2008: 11.
- 16.
Storstein J. Bedriftshelsetjenestens arbeid med løsemiddeleksponerte. Ramazzini 2006; 13: 6.
- 17.
Sluttrapport for Kjemikaliekampanjen 2003-2006. Trondheim: Direktoratet for Arbeidstilsynet, 2007.
- 18.
Working Group 2; Cost Action IS1002—Monitoring trends in Occupational Diseases and tracing new and Emerging Risks in a NETwork (MODERNET). Trends in incidence of occupational asthma, contact dermatitis, noise-induced hearing loss, carpal tunnel syndrome and upper limb musculoskeletal disorders in European countries from 2000 to 2012. Occup Environ Med 2015; 72: 294 - 303. [PubMed][CrossRef]
- 20.
Leira HL, Berg JA, Bratt U et al. Mye arbeidsrelatert sykdom blant astmatikere. Tidsskr Nor Laegeforen 2006; 126: 2367 - 9 [PubMed].. [PubMed]
- 21.
Hem K-G, Dahl Ø, Rohde T et al. Kostnader ved arbeidsrelaterte sykdommer og skader. SINTEF-rapport A27430. Oslo: SINTEF Teknologi og samfunn, 2016.
- 22.
Haarberg Ø, Lande LA, Samant Y et al. Rapport fra Register for Arbeidsrelatert sykdom. Oslo: Direktoratet for Arbeidstilsynet, 2015.