Stroke is one of the most frequent causes of death and the most common cause of severe disability (1). Around 15 000 people suffer from stroke each year (1). Most of these patients are elderly, and the incidence of stroke is expected to increase as the population ages (2).
It is estimated that about two million neurons are damaged each minute in a major untreated cerebral infarction (3). The use of intravenous thrombolysis to treat cerebral infarction is limited by the need to initiate treatment within 4.5 hours of symptom onset, with the effectiveness of treatment gradually decreasing within this time window (4) – (6). A maximum door-to-needle time of 40 minutes is a national quality indicator (7), and many hospitals have established their own algorithms and routines for patients admitted as «thrombolysis candidates». Nevertheless, only a minority of patients are treated with intravenous thrombolysis, primarily owing to prehospital delay (8) – (10). In 2015, several studies demonstrated beneficial effects of thrombectomy, but this too should be performed within a time window of six hours (11).
All patients with acute stroke should be admitted to hospital at once. Upon suspicion of acute stroke, the EMCC should be called immediately to ensure the fastest possible admission and evaluation for thrombolysis/thrombectomy. However, many patients do not call the EMCC directly, which can lead to thrombolytic therapy being delayed. If a patient with acute stroke contacts a general practitioner (GP)/Out-of-hours (OOH) services, this should lead to their prompt admission to hospital.
The aim of this study was to describe the prehospital path for patients with acute stroke, including how time was spent prior to arrival at the hospital, and differences between patients who contact the EMCC and those who contact the primary health care services (GP/OOH services). A further aim was to examine how health care professionals in the EMCC and in the primary health care services respond to being notified about a patient with stroke symptoms.
Material and method
This prospective observation study was part of a larger project on prehospital delay in cases of stroke, and on stroke awareness, conducted from 15 April 2009 to 1 April 2010 at the Stroke Unit, Department of Neurology, Akershus University Hospital. All patients in the catchment area (approximately 360 000 persons as of 1 January 2010) with possible stroke were admitted to the Department of Neurology irrespective of age.
All patients with a discharge diagnosis of cerebral infarction or intracerebral haemorrhage were included in the study (n = 440), as these conditions cannot be differentiated prior to hospitalisation and head CT. Patients with stroke imitators (other final diagnoses), transient symptoms (final diagnosis of transient ischaemic attack) or symptom duration of more than 24 hours prior to hospitalisation were excluded. Patients who attended the emergency department directly without contacting the health care service beforehand, and patients who had a stroke during a hospital stay were also excluded. Study inclusions and exclusions are shown in Fig. 1.
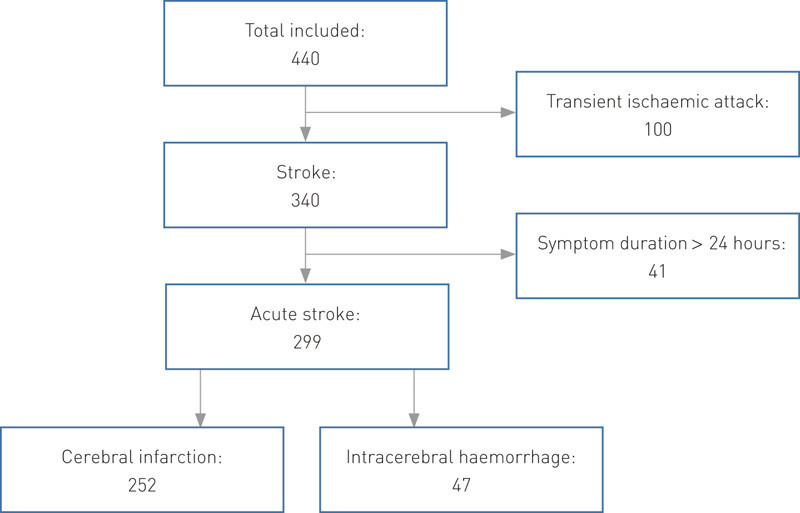
All patients and/or their relatives were interviewed within 72 hours of hospitalisation, and a structured questionnaire was completed. Electronic patient records were also reviewed and relevant data recorded.
Patient delay was defined as the time from symptom onset to first contact with the health care service. Prehospital delay was defined as the time from symptom onset to arrival at the emergency department. Contact with the health care service included telephone contact with the EMCC, telephone contact with the GP’s office/OOH services, and attendance at the GP’s office/OOH services. Information about previous stroke and heart disease was obtained from the electronic medical records. Neurological deficits were quantified using the Norwegian version of the National Institutes of Health Stroke Scale (NIHSS) (score 0 = no symptoms, maximum score 42) (12).
Statistics
Continuous data are presented as medians plus lower and upper quartiles as they were not normally distributed. Comparisons across groups were conducted using a Mann-Whitney U test. Categorical data are presented as absolute values and percentages, and the groups were compared using Pearson/Fisher’s exact chi-squared test. P-values < 0.05 were considered statistically significant. Statistical analyses were conducted using SPSS version 22 (IBM SPSS, Chicago, IL, USA).
Ethics
The project was judged by the Regional Committee for Medical and Health Research Ethics to be exempt from submission requirements. The project was approved by the local Data Protection Officer.
Results
A total of 299 patients were included in the study, of whom 252 had cerebral infarction and 47 had intracerebral haemorrhage. The median age was 75 years (65 – 82) and 145 (48.5 %) were women. In all, 191 (63.9 %) patients called the EMCC as their first contact with the health care service, while 61 (20.4 %) patients called the GP’s office/OOH services (36/25 respectively), and 47 (15.7 %) patients went directly to the GP’s office /OOH services (14/33 respectively) without prior telephone contact.
Of the 191 patients who called the EMCC, 179 (93.7 %) were transported directly to hospital by ambulance, whereas 12 (6.3 %) were asked to go to or were transported to the GP’s office/OOH services. Of these 12 patients, eight were subsequently taken to hospital by ambulance.
Of the 61 patients who telephoned the GP’s office or OOH services, 37 (60.7 %) were asked to attend in person to be assessed by a physician, whereas 24 (39.3 %) were transferred to the EMCC. Of the 37 patients who were asked to go to the GP’s office/OOH services, 18 were admitted via the EMCC, while 19 were taken to hospital by another mode of transport without the involvement of the EMCC.
Of the 96 patients who were assessed by a GP/OOH services physician (in person, as either first or second contact), 44 (45.8 %) were admitted to hospital by ambulance, while the remainder (54.2 %) travelled to hospital by another form of transport. The prehospital path is shown in detail in Fig. 2.
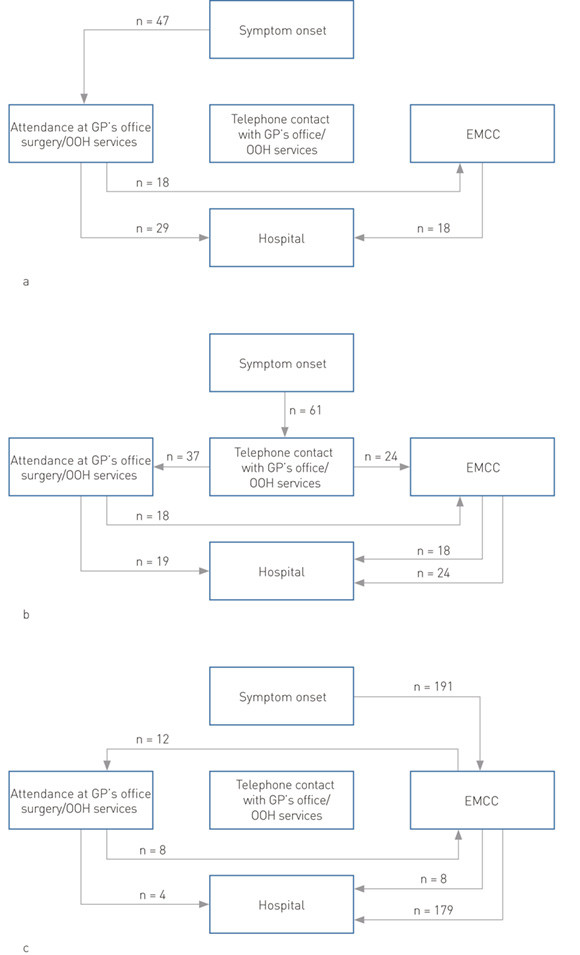
Table 1 summarises the results for all patients classified according to first medical contact (EMCC or GP/OOH services). The patients who called or went to the GP’s office/OOH services had significantly lower NIHSS scores (p = 0.001), significantly longer patient delay (< 0.001) and prehospital delay (p = 0.018), and a significantly lower thrombolysis rate (p = 0.003). There were no significant differences between the groups with respect to age, gender distribution, proportion with previous heart disease and proportion with previous stroke.
Table 1
Overview of patients classified on the basis of first medical contact – either the Emergency Medical Communication Centre (EMCC) or the general practitioner’s (GP’s) office/Out-of-hours (OOH) services. All patients were admitted to the Department of Neurology, Akershus University Hospital, with acute stroke in the period 15 April 2009 to 1 April 2010
|
| Total | EMCC | GP’s office/OOH services | P-value |
| Number (%) | 299 (100) | 191 (63.9) | 108 (36.1) |
|
| Age, years, median (lower and upper quartiles) | 75 (65 – 82) | 76 (67 – 82) | 73 (64 – 82) | 0.308 |
| Women (%) | 145 (48.5) | 90 (47.1) | 55 (50.9) | 0.527 |
| Living alone (%) | 133 (44.5) | 82 (42.9) | 51 (47.2) | 0.691 |
| Previous stroke (%) | 93 (31.1) | 66 (34.6) | 27 (25.0) | 0.086 |
| Previous heart disease (%) | 110 (36.8) | 77 (40.3) | 33 (30.6) | 0.093 |
| National Institutes of Health Stroke Scale score median (lower and upper quartiles) | 5 (2 – 12) | 7 (3 – 17) | 3 (1 – 5) | 0.001 |
| Arrival by ambulance (%) | 247 (82.6) | 187 (97.9) | 60 (55.6) | < 0.001 |
| Patient delay, minutes, median (lower and upper quartiles) | 66 (18 – 210) | 35 (10 – 120) | 172 (66 – 383) | < 0.001 |
| Transport delay, minutes, median (lower and upper quartiles) | 57 (40 – 89) | 46 (34 – 60) | 115 (66 – 226) | 0.023 |
| Prehospital delay, minutes, median (lower and upper quartiles) | 140 (69 – 362) | 83 (59 – 164) | 352 (188 – 636) | 0.018 |
| Cerebral infarction (%) | 252 (84.3) | 156 (81.7) | 96 (88.9) | 0.100 |
| Intravenous thrombolysis, number/number with cerebral infarction (%) | 22/252 (8.7) | 20/156 (12.8) | 2/96 (2.1) | 0.003 |
Discussion
This study revealed that of 299 patients with acute stroke, 63.9 % called the EMCC as their first contact with the health care service, and 93.7 % of these were transported by ambulance directly to hospital. Of those patients who telephoned the GP’s office or OOH services, 60.7 % were asked to go to the GP’s office/OOH services in person. In all, 45.8 % of patients who were assessed by their GP or by an OOH services physician were transported to hospital by ambulance. The patients whose first medical contact was with the primary health care services (telephone contact or attendance at the GP’s office/OOH services) had milder neurological deficits and longer patient delay than patients who called the EMCC. Approximately half of all patients who were asked to go to the GP’s office/OOH services after contacting the GP’s office/OOH services by telephone were admitted without the involvement of the EMCC.
The thrombolysis rate in cases of cerebral infarction is a national quality indicator, and the national average for Norway for the period May–August 2015 was 14.6 % (13). This indicator only includes patients up to 80 years of age. Three of the ten new national quality indicators published by the Norwegian Directorate of Health in February 2016 were related to cerebral infarction (14).
Even when hospitalisation is achieved within the appropriate time window, there are absolute and relative contraindications for intravenous thrombolysis, and the decision to treat is made on the basis of an overall assessment. Nevertheless, several studies show that prehospital delay is the most common reason for the low thrombolysis rate; that is, many patients arrive at hospital too late to be considered for intravenous thrombolysis (15) – (17). To address this, stroke awareness campaigns have targeted both the general public and specific populations (18) – (20). Studies show that such campaigns have a beneficial but short-lived effect, and that increased knowledge of stroke does not necessarily lead to long-term changes in behaviour/actions (21). The acronym «FAST» (Face, Arm, Speech, Time) has been employed in several English-speaking countries. In Norway, various acronyms have been used (22), and nationwide awareness campaigns have been proposed with and without acronyms. A recently published Norwegian study examined the effectiveness of a stroke awareness campaign in Western Norway. The study concluded that the campaign was effective for six months, judging by the thrombolysis rate and number of admissions for suspected stroke, but that the effect subsequently tapered off (23).
In the current study, nine out of ten patients who called the EMCC were taken by ambulance directly to hospital, whereas only four out of ten patients who contacted the primary health care services were transferred to the EMCC and admitted directly. This «detour» via the GP /OOH services causes unnecessary delay and greatly increases the risk that the patient will not be evaluated for intravenous thrombolysis or thrombectomy within the necessary time window. Patients who telephoned or attended the GP’s office/OOH services had lower NIHSS scores than patients who called the EMCC, but milder neurological deficits are not a contraindication for intravenous thrombolysis (6, 24), and the patient’s condition may subsequently deteriorate. However, specific symptoms were not recorded in this study; it is conceivable that a greater proportion of these patients had atypical symptoms and were therefore initially assessed at the GP’s office/OOH services because diagnoses other than stroke were considered more likely. In addition, these patients had longer patient delay than those who called the EMCC, which means that a greater proportion of these individuals could not have been considered for intravenous thrombolysis or thrombectomy anyway.
Stroke symptoms are in many ways more challenging than suspected coronary symptoms, due both to variability in symptoms and their severity, and also to the possibility of impaired cognition and communication (aphasia, dysarthria) or reduced self-awareness. Over 60 % of patients who contacted the GP’s office or OOH services were asked to attend in person, which led to unnecessary delay. One means of reducing this delay may be to focus on increased stroke-related education/training for health care professionals who represent the first medical contact for patients with possible acute stroke, as has also been proposed by Akuttutvalget [the emergency medicine committee] (25, 26). Such training should particularly target those who answer the telephone at the GPs offices and OOH services, usually medical secretaries/receptionists, nurses or medical students. There is also a need for stroke awareness campaigns aimed at the general public, as relatives are often the first to see the patient. Information can be made available through teaching in schools, in the waiting rooms of GPs offices, or as advertising campaigns on television and the internet, in magazines and newspapers, and possibly on milk cartons.
We did not examine the knowledge of health care professionals who encounter stroke patients in the acute phase, i.e. those who receive the first telephone call from a patient with acute stroke. One way of evaluating health care professionals’ knowledge and management of acute stroke is by using simulated patient case histories. In a study from the UK (27), GPs offices were called unannounced and presented with simulated patient case histories (graded easy, moderate or difficult), and their response recorded. Case histories with many symptoms were recognised as possible stroke and were referred to the EMCC, but this was not true for cases with fewer and atypical symptoms. In a US study (28), telephone operators at various hospitals were presented with a standardised stroke scenario and were asked to select one of four different responses, in addition to naming the most common symptoms of stroke. A total of 22 % advised the patient to contact their GP.
The current study has several weaknesses. Stroke imitators were not included, which means that sensitivity and specificity could not be determined. Whether it was the patient or a relative who contacted the health care service was also not recorded. The study was conducted in the period 2009 – 10, i.e. prior to publication of the Nasjonal faglig retningslinje for behandling og rehabilitering ved hjerneslag [National guidelines for treatment and rehabilitation after stroke] (1). In addition, stroke treatment is one of the target areas in the Norwegian Patient Safety Programme «In Safe Hands» (29), thus it is reasonable to assume that the situation may have changed as a result of greater focus on faster admission of patients with stroke. Nevertheless, we believe that many of the findings from this study continue to be relevant.
Conclusion
More than 90 % of patients with acute stroke who called the EMCC as their first medical contact were taken directly to hospital, whereas over 60 % of patients who contacted the GP’s office or OOH services were asked to attend in person, causing unnecessary delay. There is a need to focus on stroke awareness among both the general public and health care professionals.
The manuscript for this article was submitted prior to the launch of the national stroke campaign in Norway (28 October 2016); the campaign therefore does not feature in the discussion.
MAIN POINTS
Two out of three patients with acute stroke called the Emergency Medical Communication Centre (EMCC) as their first medical contact, and over 90 % of these patients were taken directly to hospital by ambulance
More than 60 % of patients who called their general practitioner’s (GP’s) office or Out-of-hours (OOH) services were asked to go to the GP’s surgery/OOH services in person
Patients who initially called and attended the GP’s office/OOH services had less severe neurological deficits and longer patient delay than those who called the EMCC, and significantly fewer of them received intravenous thrombolysis
- 1.
Nasjonal retningslinje for behandling og rehabilitering ved hjerneslag. Oslo: Helsedirektoratet, 2010.
- 2.
Scenario 2030 – Sykdomsutviklingen for eldre fram til 2030. Oslo: Statens helsetilsyn, 1999.
- 7.
Helsenorge.no. Trombolysebehandling av hjerneinfarkt innen 40 minutter. https://helsenorge.no/Kvalitetsindikatorer/behandling-av-sykdom-og-overlevelse/trombolysebehandling-etter-40-min (17.11.2016).
- 11.
Powers WJ, Derdeyn CP, Biller J et al. 2015 American Heart Association/American Stroke Association focused update of the 2013 guidelines for the early management of patients with acute ischemic stroke regarding endovascular treatment: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2015; 46: 3020 – 35. [PubMed] [CrossRef]
- 12.
NIHSS. NEL Nevrologi, 2013. http://nevro.legehandboka.no/skjema/skaringsskjema/nihss-33929.html (9.4.2016).
- 13.
Helsenorge.no. Trombolysebehandling ved blodpropp i hjernen. https://helsenorge.no/kvalitet-seksjon/Sider/Kvalitetsindikatorer-rapporter.aspx?kiid=Trombolysebehandling_ved_hjerneinfarkt (4.9.2016).
- 14.
Nye kvalitetsindikatorer viser variasjon i tjenestene: Oslo: Helsedirektoratet, 2016. https://helsedirektoratet.no/nyheter/nye-kvalitetsindikatorer-viser-variasjon-i-tjenestene (9.4.2016).
- 22.
Faiz KW, Sundseth A. Hvor ble det av tiden? Tidsskr Nor Legeforen 2013; 133: 1057. [PubMed]
- 25.
Norges offentlige utredninger. Først og fremst – et helhetlig system for håndtering av akutte sykdommer og skader utenfor sykehus. NOU 2015: 17. https://regjeringen.no/no/dokumenter/nou-2015-17/id2465765/ (23.4.2017).
- 26.
Lund CG, Ness E, Rørtveit S et al. For en bedre akuttmedisinsk tjeneste i Norge. Tidsskr Nor Legeforen 2016; 136: 383. [PubMed]
- 29.
Behandling av hjerneslag: Pasientsikkerhetsprogrammet I trygge hender. http://pasientsikkerhetsprogrammet.no/no/I+trygge+hender/Innsatsomr%C3%A5der/Behandling+av+hjerneslag.17.cms (20.9.2016).