Upper secondary school leaving celebrations and final exams – consultations in general practice and emergency care
In Norway, everyone who has completed basic schooling has a statutory right to a full-time, three-year course of upper secondary education. Most young people take advantage of this offer, and in 2015, over 90 % in the age group 16 – 18 participated in upper secondary education (1).
Celebrating the completion of upper secondary school – russefeiring – has long traditions in Norway. The normal practice is that you become a russ in the year you turn 19. Even though no more than 73 % of those who have commenced a course of upper-secondary education have completed this after five years (1), most young people participate in these celebrations the year they turn 19. For many, it means several weeks of celebrations largely outdoors, marked by a high intake of alcohol (2), both potential risk factors for illness and injury. Russefeiring is at its peak in the weeks prior to Norway’s Constitution Day on 17 May. Examinations for school leavers are held in the ensuing weeks, usually beginning on 19 May (3). Pupils receive examination grades as well as grades for overall achievement, and these count when pupils apply for admission to higher education.
Earlier studies have shown an increased incidence of injuries treated by the specialist health services (4) and increased use of antibiotics and cough medicine (5) among 19-year-olds in May. Outbreaks of meningococcal infections among russ have also been reported (6). Apart from this, we have little knowledge about the state of health of these pupils and their use of the health services.
In this study we examined 19-year-olds’ use of the general practitioner services in connection with russefeiring. We compared consultations in May with consultations in the other months of the year, and compared 19-year-olds with young people who were one year older or one year younger. We analysed consultations with regular GPs and emergency departments, and studied a sample of diagnostic groups more closely.
Material and Method
The study is based on data from the Directorate of Health’s system for the control and payment of reimbursements to health service providers (KUHR), which contains information about all patient contact with regular GPs and emergency departments. The population base per 1 January for 2012 – 15 is derived from Statistics Norway's website (7). Identifiable characteristics that could be traced to an individual were removed and the study therefore was exempt from notification to a regional medical research ethics committee.
The source data consisted of reimbursement claims from the general practitioner services for a four-year period (2012 – 15) for cohorts turning 18, 19 or 20 years during each of the relevant calendar years. The data set contained information about year of birth and sex, date of consultation, diagnostic codes in accordance with the International Classification of Primary Care 2 (ICPC-2), fee codes and type of practice (regular GP/emergency department). We included consultations with fee codes 2ad (daytime consultation with a GP), 2ak (consultation with a GP during the evening, night or at the weekend) and 2fk (consultation and emergency response to medical practice during out-of-hours services) (8). Telephone contact and house calls were not included.
We calculated age by subtracting the year of birth from the calendar year. We use the term «19-year-olds» for anyone who turned 19 during a specified calendar year, regardless of when they were born during the year. We categorised 18 and 19-year-olds in the same way. In the Norwegian school system, children start at school in the year they turn six, and with normal progression, by our definition the «russ» cohort will be composed of 19-year-olds.
For most consultations, only one diagnostic code was registered (87.2 %). We took all registered codes into account when grouping diagnoses into six different main categories: respiratory tract infections, general pain and musculoskeletal complaints, mental health problems, accidents and injuries, gastrointestinal complaints, and other conditions (e-tab 1). In addition, we checked each individual ICPC-2 code separately within the largest group (respiratory infections). The grouping was based on Statistics Norway’s classification (9).
Table 1
Allocation of ICPC-2 codes (International Classification of Primary Care 2) to six diagnostic groups used in analysis of consultations with a GP or the emergency department for young people aged 18 to 20
| Group 1 |
ICPC-2 codes |
| Respiratory tract infections, including ear infections |
R05, R09-R23, R71-R83, H71-H74 |
| General pain and musculoskeletal complaints, including joint and rheumatic problems |
L01, L08-L17, L83, L87,L92,L93, L02-L03, L84-L86, A01, L18-L19, L29, L07, L20, L88-L91, L94 |
| Mental illness or mental health problems |
P01-P99 |
| Accidents and injuries |
A80-A82, A84, A86, A88, B76-B77, D79-D80, F75-F79, H76-H79, L72-L81, L96, N79-N81, R87-R88, S12-S19, S80, U80, X82, Y80 |
| Gastrointestinal complaints |
D01-D12, D17-D21, D84-D87, D90, D92, D93 |
| Other conditions |
All other codes |
1 Groups based on Statistics Norway’s groups (9)
Statistical analyses
All analyses were performed using the Stata®14 statistical package (Statacorp, Texas). We presented the number of consultations per calendar month by cohort and year graphically. In addition, we used the Poisson regression model with the number of consultations per month as an outcome variable, and various combinations of year, month, sex, and cohort as explanatory variables. In the Poisson regression, we took into account the population in the different categories and the number of days in the month in question.
The results are presented as incidence rate ratio (IRR) with 95 % confidence interval (CI) with data from 19-year-olds in March as reference. The IRR therefore gives a measurement of the number of consultations for a given cohort in a given calendar month seen in relation to the number of consultations for 19-year-olds in March.
We chose 19-year-olds as the reference category to prevent any differences in the number of consultations based on age rather than calendar month from influencing the results. March was chosen because it is the month that is closest in time without being part of the most intense russefeiring while at the same time it is not a holiday month. In order to examine the impact of time, we also presented the number of consultations per week by year and cohort graphically.
Results
Altogether 1 690 139 consultations for 18 – 20-year-olds were registered in the period from 2012 – 15. The total number of consultations annually increased from 417 322 in 2012 to 434 524 in 2015 (an increase of 4.1 %), while the population base grew from 197 099 to 199 689 (an increase of 1.3 %).
The total number of consultations in May for 19-year-olds was higher than in the other months and higher than for the younger and older cohorts in May in all four years of the period studied (fig. 1). In May 2015, a total of 19 891 consultations were registered for 19-year-olds, while the corresponding figure for those who were one year younger or one year older was 11 627 and 12 200 respectively (fig 1). There was little difference between the relevant cohorts in other calendar months.
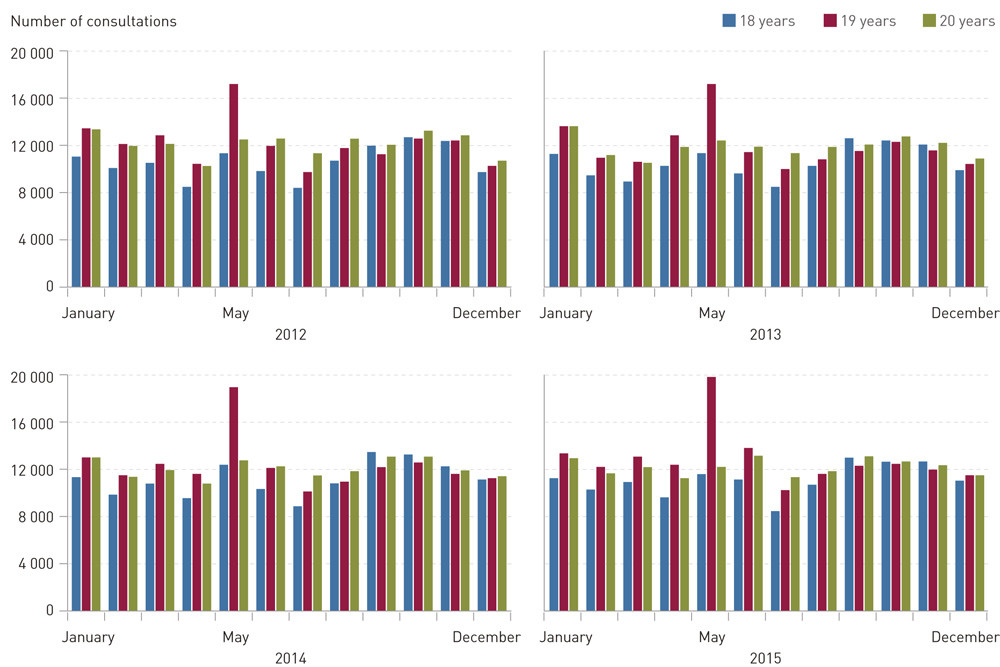
E-table 2 shows the monthly number of consultations per 1 000 inhabitants by cohort with the regular GP, the emergency department and for each diagnostic group, for 2015. The table shows a marked increase in both the number of regular GP consultations and in the number of consultations with the emergency department for 19-year-olds in May compared with 19-year-olds in other months and with cohorts who were one year younger or one year older, in the same month. The increase was most marked for the diagnostic group respiratory tract infections. For the diagnostic group accidents and injuries we also found a higher number of consultations for 19-year-olds than 18 and 20-year-olds in May, but here the total volume of consultations was considerably smaller. The years 2012 – 14 showed a similar pattern in terms of distributions and differences (data not shown).
Table 2
Number of consultations in 2015 with GPs and the accident and emergency department per month per 1000 inhabitants in age groups 18, 19 and 20 years
|
|
18 years N = 66 869 |
19 years N = 66 426 |
20 years N = 66 394 |
| GP, all codes |
|||
| March |
140 |
171 |
158 |
| April |
122 |
155 |
141 |
| May |
143 |
235 |
150 |
| June |
143 |
178 |
171 |
| Other1 |
143 |
152 |
154 |
| Emergency department, all codes |
|||
| March |
22 |
25 |
26 |
| April |
23 |
32 |
29 |
| May |
31 |
65 |
33 |
| June |
24 |
29 |
28 |
| Other1 |
25 |
28 |
29 |
| Respiratory tract infections 2, 3 |
|||
| March |
25 |
32 |
24 |
| April |
22 |
33 |
20 |
| May |
44 |
128 |
30 |
| June |
34 |
49 |
29 |
| Other1 |
29 |
27 |
24 |
| General pain and musculoskeletalcomplaints 3 |
|||
| March |
20 |
23 |
22 |
| April |
17 |
20 |
19 |
| May |
17 |
21 |
20 |
| June |
15 |
19 |
22 |
| Other1 |
19 |
20 |
21 |
| Mental health problems 3 |
|||
| March |
20 |
26 |
26 |
| April |
17 |
22 |
23 |
| May |
17 |
23 |
24 |
| June |
17 |
23 |
24 |
| Other1 |
19 |
23 |
25 |
| Accidents and injuries 3 |
|||
| March |
10 |
11 |
11 |
| April |
9 |
13 |
11 |
| May |
10 |
14 |
12 |
| June |
9 |
11 |
11 |
| Other1 |
11 |
11 |
11 |
| Gastrointestinal complaints 3 |
|||
| March |
9 |
12 |
12 |
| April |
8 |
10 |
11 |
| May |
8 |
10 |
11 |
| June |
7 |
9 |
11 |
| Other1 |
9 |
11 |
12 |
| Other conditions 3 |
|||
| March |
80 |
95 |
90 |
| April |
74 |
90 |
87 |
| May |
79 |
105 |
90 |
| June |
85 |
98 |
103 |
| Other1 |
83 |
90 |
93 |
1 Average for other months of the year
2 Including ear infections
3 See e-table 1 for details of grouping
For the entire period 2012 – 15 combined, the number of GP consultations for 19-year-olds in May compared with the number of consultations for 19-year-olds in March gave an incidence rate ratio of 1.40 (95 % CI 1.38 – 1.41) (fig. 2). Consultations with the emergency department doubled for 19-year-olds in May compared with 19-year-olds in March (IRR 2.07, 95 % CI 2.02 – 2.13). Consultations with the emergency department for 18-year-olds also showed a slightly higher incidence in May than for 19-year-olds in March, but this difference was far less than the corresponding difference between these months for 19-year-olds (fig. 2).
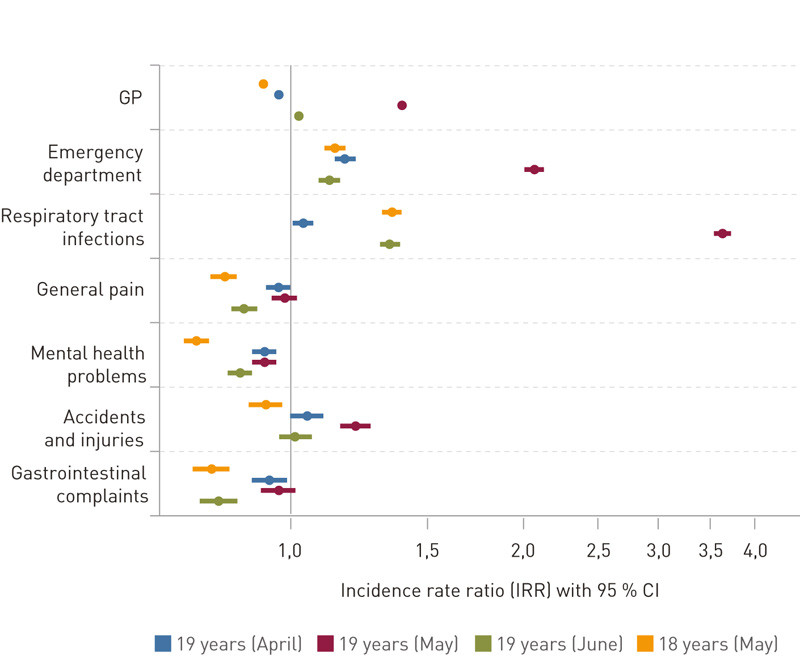
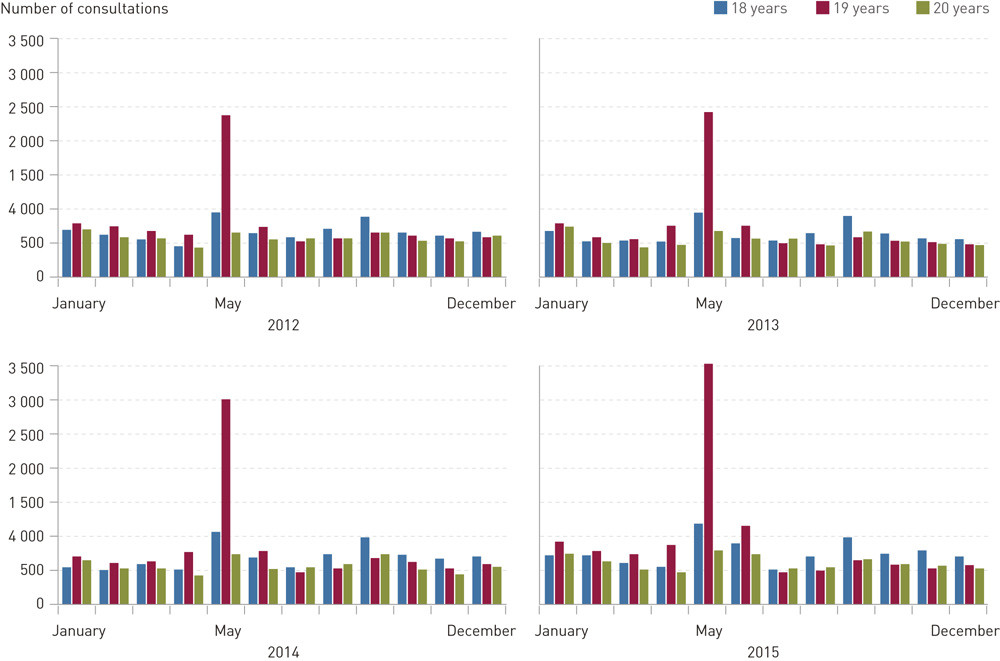
Among the diagnostic groups, respiratory tract infections clearly stood out – with the largest increase in the number of consultations in May for 19-year-olds (IRR 3.64, 95 % CI 3.55 – 3.73 compared with 19-year-olds in March). 18-year-olds also had more consultations in May than 19-year-olds in March, but the difference was not nearly as great. The number of consultations in the diagnostic group accidents and injuries was also higher among 19-year-olds in May (IRR 1.21, 95 % CI 1.16 – 1.27), while the total number of consultations with the diagnoses general pain, mental health problems and gastrointestinal complaints was somewhat less in May than in March for 19-year-olds.
We carried out corresponding analyses for each diagnostic code within the respiratory tract infections group. All codes clearly demonstrated a pattern of increase in May for 19-year-olds, with the exception of R80 Influenza, which showed a typical seasonal pattern with a greater number of consultations in the winter months (not shown). The greatest volume of consultations was for the diagnosis R74 Acute upper respiratory infection (e-fig 3). The incidence rate ratio for this diagnosis for 19-year-olds in May compared with 19-year-olds in March was 4.41 (95 % CI 4.22 – 4.60).
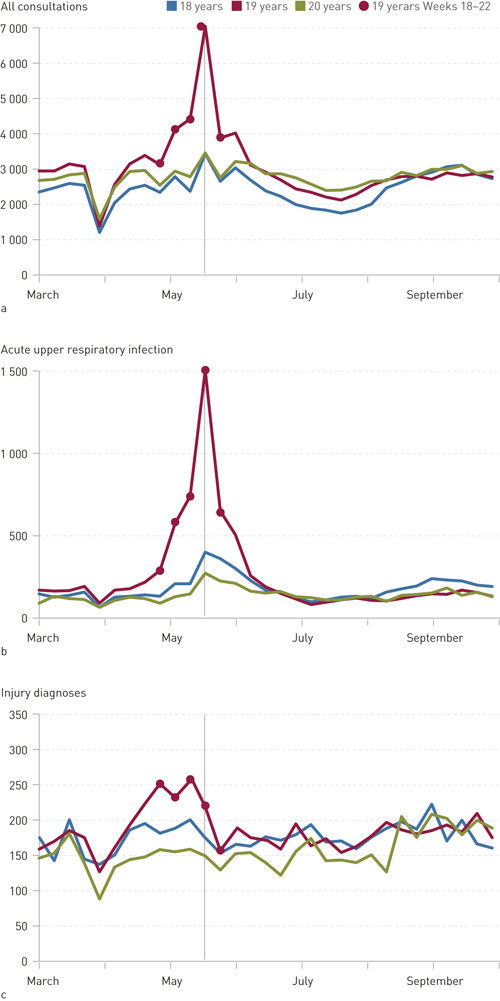
E-figure 4 shows the total number of consultations, the number of consultations with acute upper respiratory tract infections, and the number of consultations with an injury diagnosis for each week from March to October 2015. For 19-year-olds, there was an increase in the total number of consultations in weeks 19 and 20 (the period from 6 May to 17 May), a strong increase in the number of consultations in week 21 (18 to 24. May), followed by an ensuing decline (e‑fig 4a). Consultations for acute upper respiratory tract infections followed the same pattern (e-fig 4b). Most of the increase in injury diagnoses for 19-year-olds occurred in the weeks up to 17 May, with a sharp decline immediately after Constitution Day. However, the volume of consultations for accidents and injuries was low compared with infection diagnoses (e-fig 4c).
Discussion
All the years from 2012 to 2015 showed a higher number of consultations with regular GPs and emergency departments in May than in all other calendar months for 19-year-olds. We observed no such pattern for other cohorts, and for other calendar months than May, there were no striking differences between 19-year-olds and the cohorts immediately below and above. The single diagnosis acute upper respiratory tract infection showed an almost fourfold increase in consultations in May for 19-year-olds compared with March. We further found that the number of consultations for 19-year-olds was high in both the first and second half of May as regards both the total number of consultations and the single diagnosis acute upper respiratory tract infection. For injuries, however, we observed only an increase in the first half of May.
The study is based on data from the Directorate of Health’s system for the control and payment of reimbursements to health service providers – KUHR. This database is not organised as a health register. Importantly, the KUHR database is almost complete, in the sense that it contains data from all consultations where Norwegian GPs have claimed reimbursement.
We know little about diagnostic quality, but assume that there is variation among diagnoses. A study from Canadian general practice has shown good data quality for the diagnoses epilepsy, Parkinson’s disease and dementia, but more moderate results for chronic obstructive pulmonary disease and depression (10). An earlier Norwegian study (data from 1992 – 2008) showed that often the correct codes are not used in reporting (11). In our study, some of the uncertainty was reduced by combining diagnostic codes into large diagnostic groups. Youth Health Centres are not included in the source data, and for this reason we have been unable to capture all contact that would probably relate to sexual health and less serious mental problems.
Previous studies from the Norwegian Institute of Public Health have shown an increase in the use of antibiotics (5) and in the number of injuries treated by the specialist health service (4) in May for 19-year-olds. We assume that a large proportion of the increase in the use of antibiotics and in injuries, as well as the increase we now observe in the general practitioner services, can be associated with the russ period. The number of consultations for the russ cohort increased in the first half of May prior to the start of the examination period.
For most of those participating in these celebrations, May is nevertheless also examination time. Exam grades are important for further qualification for higher education and work, and illness during an examination that can be documented by a medical certificate gives an entitlement to take a new examination later (12). The strong increase in GP consultations also in the second half of May can probably be explained to some extent by a need for treatment for infections during examination time or to document an illness in order to secure examination rights. However, the data do not enable us to analyse the prevalence of medical certificates linked to exemption from exams.
The relative increase in consultations in May among 19-year-olds was greatest in relation to consultations with emergency departments, but the numerical increase was greatest for consultations with GPs. This concurs with the findings of a study on the influenza pandemic in 2009, in which the authors concluded that the general practitioner services were flexible, and could respond to increased need in the population (13).
Russ celebrations ahead of an important examination period are, to the best of our knowledge, a unique Norwegian tradition. Similar celebrations among adolescents and young adults in other countries are more often linked to the start of studies or take place during holiday periods (14, 15). Buddy scheme arrangements at Norwegian higher education institutions take place at the commencement of studies and are considered small-scale in comparison with russ celebrations (16, 17).
Suggestions have been put forward several times to move these celebrations to the post-examination period, or alternatively to move the examinations forward to take place before these celebrations. Last year a new committee was appointed to examine the reorganisation of the school year (18).
Conclusion
The cohort completing upper secondary education had a much greater number of consultations with the general practitioner services in May compared with the cohort below and above in all years covered by the study. The most frequent reason was respiratory tract infections. The increase began in the period before 17 May and persisted into the examination period.
We can probably explain the increased need for medical assistance during the russ period by a combination of a higher incidence of respiratory tract infections and a greater need for treatment and doctor’s certificates during the examination period.
MAIN MESSAGE
In May 2015, 19-year-olds had a total of 19 891 consultations in the general practitioner services, while the corresponding figure for 18-year-olds was 11 627, and for 20-year-olds 12 200.
Respiratory infections accounted for most of the increase, although injuries and accidents also played a part.
All years in the period between 2012 and 2015 showed an identical pattern.
- 1.
Statistisk sentralbyrå. Nøkkeltall for utdanning. www.ssb.no/utdanning/nokkeltall/utdanning (3.4.2017).
- 3.
Utdanningsdirektoratet. Kalender. https://www.udir.no/Kalender/Eksamen-og-prover/ (3.4.2017).
- 4.
Austdal LE, Strand MC, Vindenes V et al. Forekomst av skader i russetiden. Tidsskr Nor Legeforen 2015; 135: 648 – 52. [PubMed]
- 5.
Blix HS, Hjellvik V. Økt bruk av antibiotika blant 19-åringer i May. Tidsskr Nor Legeforen 2012; 132: 1084 – 8. [PubMed]
- 6.
Folkehelseinsituttet. Ungdom bør vurdere å vaksinere seg mot smittsom hjernehinnebetennelse. https://www.fhi.no/sv/smittsomme-sykdommer/hjernehinnebetennelse/ungdom-bor-vurdere-a-vaksinere-seg-mot-smittsom-hjernehinnebetennelse/ (3.4.2017).
- 7.
Statistisk sentralbyrå. Tabell 07459: Folkemengde, etter kjønn og ettårig alder. https://www.ssb.no/statistikkbanken/ (3.4.2017).
- 8.
Den norske legeforening. Normaltariffen. http://normaltariffen.legeforeningen.no/ (3.4.2017).
- 9.
Statistisk sentralbyrå. Allmennlegetjenesten, 2012. https://www.ssb.no/helse/statistikker/fastlegetj/aar/2013-09-18 (3.4.2017).
- 12.
Lovdata. Forskrift til opplæringslova. Kap. 4 – 5 § 3 – 35. https://lovdata.no/dokument/SF/forskrift/2006 – 06 – 23 – 724 (14.2.2017).
- 16.
Rimstad SLS, Selbekk AS, Robertson IE. Fadderuken og alkohol – unntakstilstand eller etablering av nye alkoholvaner? Rapport 2/2011. Stavanger: Kompetansesenter rus – region vest Stavanger, Rogaland A-senter, 2011.
- 17.
Stålesen E. Hvordan opplever studenter ved Universitetet i Agder forholdet til alkohol i fadderuken? Om fester, relasjoner og overskridelser. Masteravhandling. Kristiansand: Institutt for psykososial helse, Universitetet i Agder, 2015.
- 18.
Mellingsæter H. Skoleåret kan bli endret – nytt utvalg skal se på omorganisering. Aftenposten. 17.6.2016. www.aftenposten.no/norge/Skolearet-kan-bli-endret---nytt-utvalg-skal-se-pa-omorganisering-478751b.html (14.2.2017).